LOCAL ANESTHETICS Dr Naila Abrar Learning Objectives After

LOCAL ANESTHETICS Dr. Naila Abrar

Learning Objectives After this session you should be able to: Ø define local anesthesia; Ø classify local anesthetics; Ø describe pharmacokinetic properties of commonly used local anesthetics; Ø describe the mechanism of action; Ø comprehend the structure-activity characteristics of local anesthetics; and Ø describe the toxicity of local anesthetics.

LOCAL ANESTHESIA DEFINITION Loss of sensory perception due blockade of sodium channels in neuronal cell membrane in a restricted/localized area of the body.
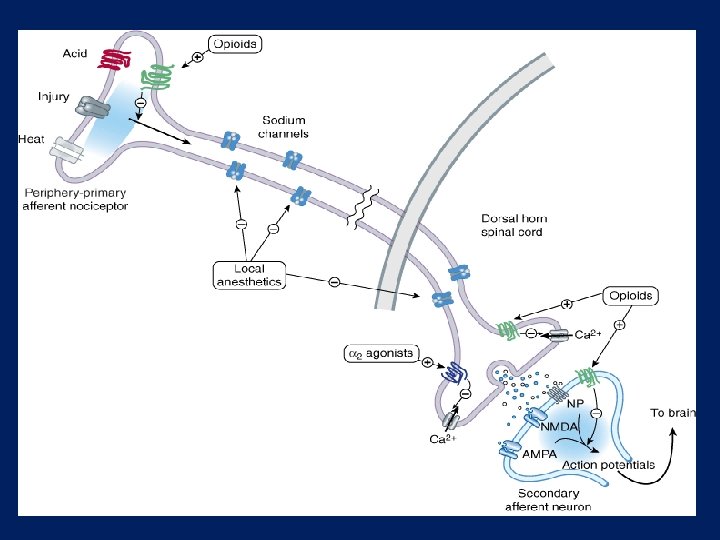

CHARACTERISTICS Ø Topical application or local injection Ø Peripheral nerves Ø Consciousness not altered Ø No amnesia Ø Vital functions not affected Ø No change in physiological functions Ø Recovery is spontaneous, predictable & without residual changes

CLASSIFICATION ACCORDING TO CHEMISTRY ESTERS v Cocaine v Procaine v Tetracaine v Benzocaine AMIDES v Lignocaine v Prilocaine v Mepivacaine v Bupivacaine v Ropivacaine

ACCORDING TO DURATION OF ACTION SHORT v Procaine, Chlorprocaine MEDIUM v Cocaine, Lidocaine, Mepivacaine, Prilocaine LONG v Tetracaine, Bupivacaine, Levobupivacaine, Ropivacaine

ACCORDING TO THERAPEUTIC USES SURFACE ANESTHESIA Ø Cocaine, lignocaine, tetracaine, benzocaine FEILD BLOCK & INFILTRATION ANESTHESIA Ø Procaine, lignocaine, bupivacaine NERVE BLOCK Ø Procaine, lignocaine, bupivacaine, tetracaine, ropivacaine SPINAL ANESTHESIA Ø Lignocaine, bupivacaine, tetracaine EPIDURAL ANESTHESIA Ø Lignocaine, bupivacaine OPHTHALMOLOGICAL ANESTHESIA Ø Proparacaine
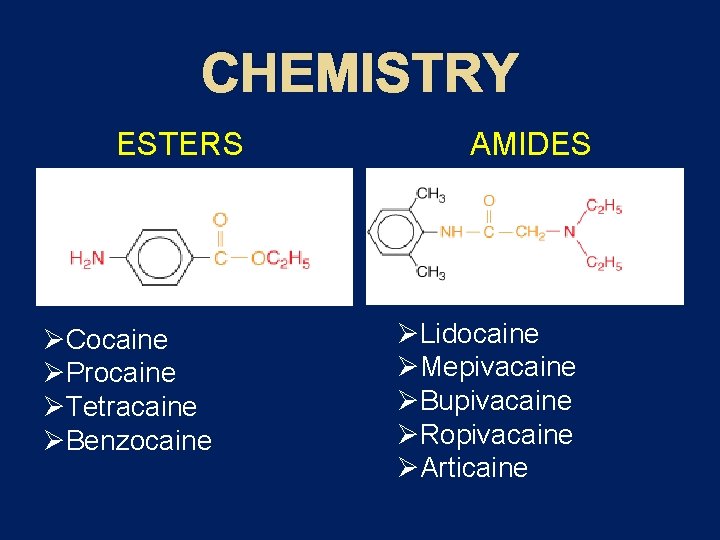
CHEMISTRY ESTERS ØCocaine ØProcaine ØTetracaine ØBenzocaine AMIDES ØLidocaine ØMepivacaine ØBupivacaine ØRopivacaine ØArticaine

PHARMACOKINETICS ABSORPTION Ø Dosage Ø Site of injection Termination of action Systemic effects intercostal>caudal>epidural>brachial>sciatic Ø Drug-tissue binding Ø Local tissue blood flow Ø Use of vasoconstrictors- epinephrine Ø Physiochemical properties of the drug

USE OF VASOCONSTRICTORS Ø EPINEPHRINE used Ø Blood supply limited Ø Absorption restricted Ø More time of contact-more pronounced effect Ø Delayed healing & tissue necrosis v a 2 receptors- decrease release of substance P- clonidine

DISTRIBUTION Ø Ø Ø Amides widely distributed Initial rapid distribution phase Slower distribution phase

METABOLISM & EXCRETION Ø Converted to more water soluble forms • liver- amides Prilocaine>lidocaine>mepivacaine>ropivacaine plasma- esters (butyrylcholinesterase) Toxicity of amide type increased in liver disease • Ø
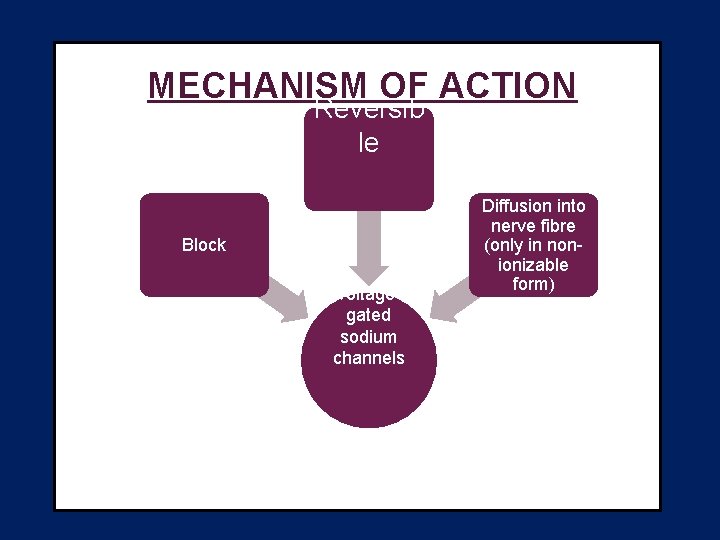
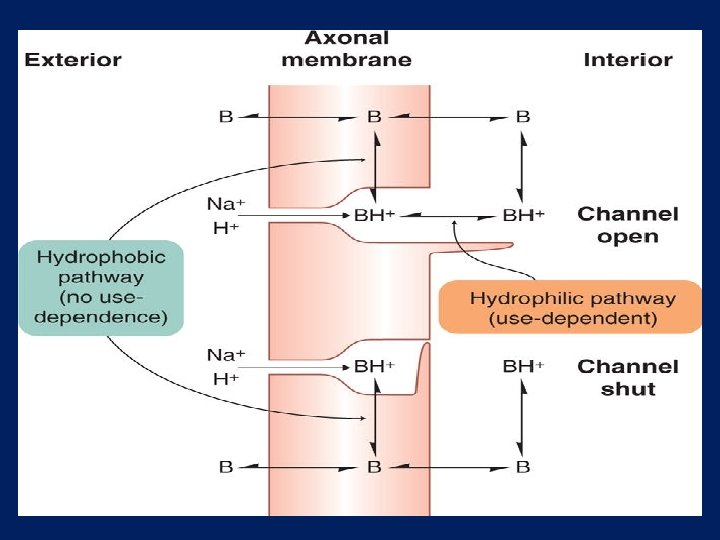
MECHANISM OF ACTION Reversib le Block voltagegated sodium channels Diffusion into nerve fibre (only in nonionizable form)
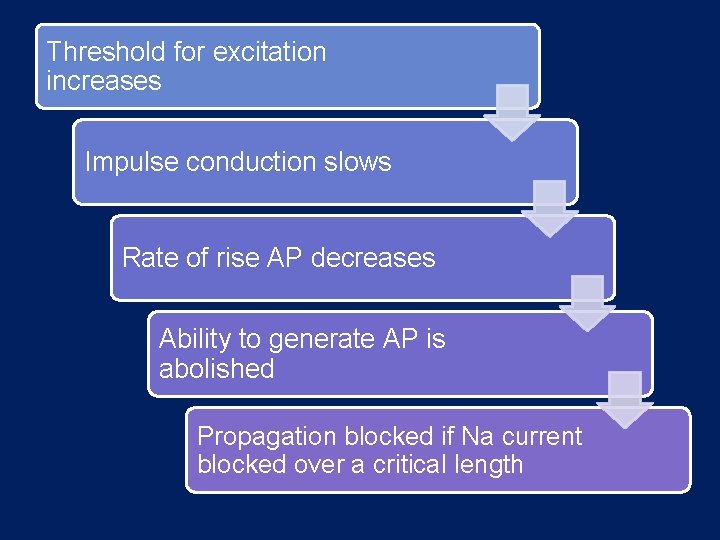
Threshold for excitation increases Impulse conduction slows Rate of rise AP decreases Ability to generate AP is abolished Propagation blocked if Na current blocked over a critical length
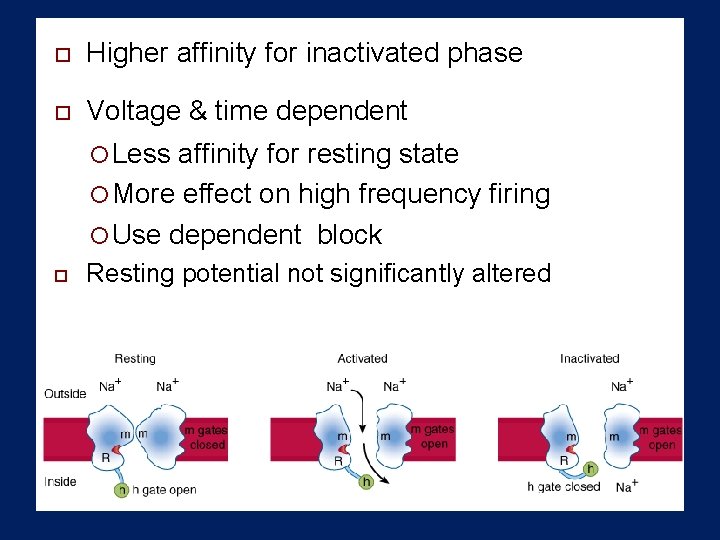
Higher affinity for inactivated phase Voltage & time dependent Less affinity for resting state More effect on high frequency firing Use dependent block Resting potential not significantly altered

Biological toxins-batrachotoxin, aconitine, scorpion venoms Bind to receptors within Na channel and prevent inactivation Prolonged influx of Na & depolarization Marine toxins tetrodotoxins & saxitoxin have effects similar to LA

FACTORS AFFECTING ACTION OF LOCAL ANESTHETICS LIPID SOLUBILITY p. Ka CARBON DIOXIDE HYDROPHOBIC NATURE TACHYPHYLAXIS

SUSCEPIBILITY OF NERVE FIBRES TO LOCAL ANESTHETICS Firing frequency Size State of myelination Fibre diameter Fibre position Pain sensation>temperature>touch>deep pressure> motor

TOXICITY 1. SYSTEMIC EFFECTS Ø Absorption from site of administration 2. DIRECT NEUROTOXICITY Ø Local effects when high concentrations are administered in close proximity to the spinal cord and other major nerve trunks

TOXICITY A. Ø Ø Ø CNS Circumoral & tongue numbness, metallic taste Nystagmus, muscle twitching, tonic-clonic convulsions Depression of cortical inhibitory pathwaysunopposed activity of excitatory neuronal pathways Generalized CNS depression Death due to respiratory failure

TOXICITY Adicular irri B. NEUROTOXICITY Ø More with chloroprocaine and lidocaine Ø Transient radicular irritation or neuropathic pain Ø Interference with axonal transport and disruption of calcium homeostasis

TOXICITY C. Ø CARDIOVASCULAR SYSTEM Direct effects on cardiac & smooth muscle membranes • • Ø v v Adicular irri Myocardial depression Arteriolar dilation-hypotension Indirect effects on ANS Bupivacaine is more cardiotoxic than othersslow idioventricular rhythm & broad QRS complexes Cocaine blocks norepinephrine reuptakevasoconstriction & hypertension, cardiac arrythmias

Adicular irri TOXICITY D. HEMATOLOGIC EFFECTS Ø Prilocaine – metabolite O-toluidine Ø An oxidizing agent converts Hb to met Hb

Adicular irri TOXICITY E. ALLERGIC REACTONS Ø Esters converted to p -aminobenzoic acid (PABA) derivatives

COCAINE Ø Sympathomimetic action Ø Potent vasoconstrictor Ø Cardiac stimulation Ø Marked pyrexia with overdose

BENZOCAINE Ø Low aqueous solubility Ø Topical local anesthetic – not absorbed Ø Relief of pain & irritation Ø Anesthesia of mucous membranes Ø PABA derivatives – antagonize effect of sulfonamides locally

LIDOCAINE(XYLOCAINE) Ø Most widely used Ø Effective by all routes but oral BA low Ø High 1 st pass metabolism Ø Fast onset, more intense & lasting effect Ø Alternative for ester allergic pts Ø Toxicity equal to procaine but more sedative than others

BUPIVACAINE Ø Not effective topically Ø Slower onset, longer acting Ø Unique property of sensory & motor dissociation Ø Popular for anesthesia during labor Ø More cardiotoxic

CLINICAL APPLICATION OF LOCAL ANESTHETICS SURFACE ANESTHESIA Ø Ear, eye, nose, throat, abraded skin Ø Only superficial layer Ø Soluble LA – rapid systemic absorption Ø Eutectic lidocaine/prilocaine – intact skin
CLINICAL APPLICATION OF LOCAL ANESTHETICS INFILTRATION ANESTHESIA Ø Dilute solution infiltrated under skin Ø Immediate onset & Do. A is short Ø Minor operations: incisions, excisions

CLINICAL APPLICATION OF LOCAL ANESTHETICS FIELD BLOCK or NERVE BLOCK Ø Injected around nerve trunk Ø Area distal to injection is anesthetized and paralyzed Ø Lidocaine Ø Bupivacaine for longer
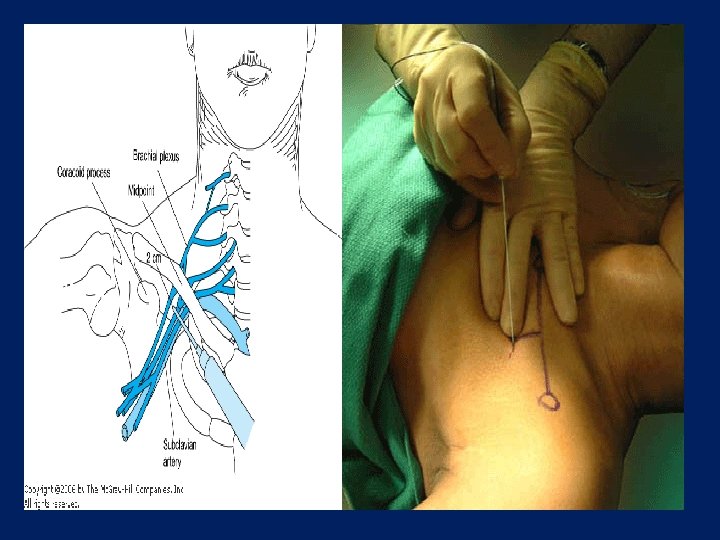
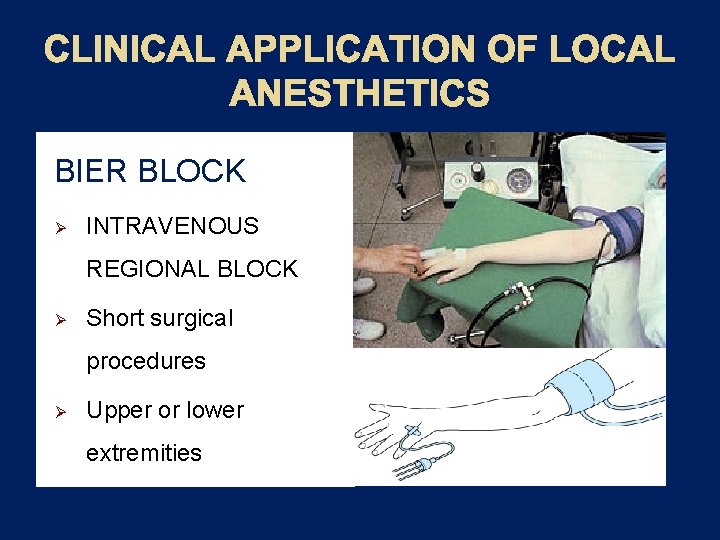
CLINICAL APPLICATION OF LOCAL ANESTHETICS BIER BLOCK Ø INTRAVENOUS REGIONAL BLOCK Ø Short surgical procedures Ø Upper or lower extremities

CLINICAL APPLICATION OF LOCAL ANESTHETICS SPINAL ANESTHESIA Ø Ø Subarachnoid space L 2 -3 or L 3 -4 – cauda equina Abdominal or pelvic surgery Effective analgesia & muscle relaxation Complications: respiratory paralysis, hypotension (sympathetic reflexes inhibited), headache, cauda equina syndrome, infection, neurotoxicity
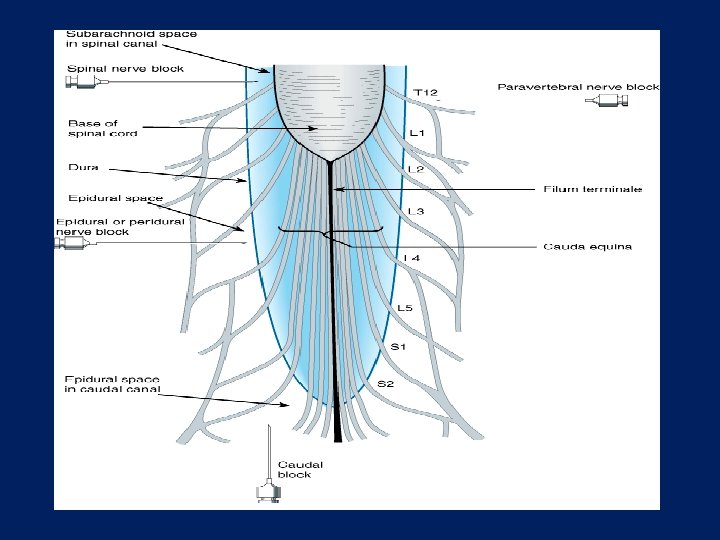
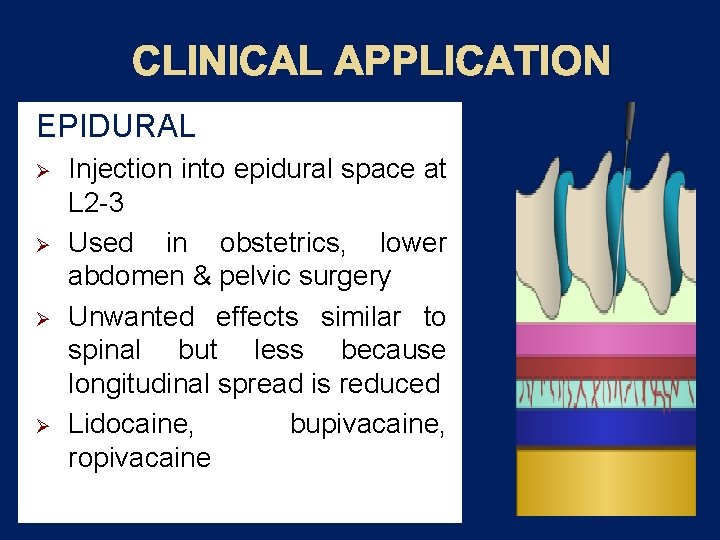
CLINICAL APPLICATION EPIDURAL Ø Ø Injection into epidural space at L 2 -3 Used in obstetrics, lower abdomen & pelvic surgery Unwanted effects similar to spinal but less because longitudinal spread is reduced Lidocaine, bupivacaine, ropivacaine
- Slides: 38