Local anesthetic All about local anesthetic LOCAL ANESTHESIA

Local anesthetic All about local anesthetic

LOCAL ANESTHESIA Professor Dr S. Mushtaq Gilani

Definition – Drugs that causes loss of sensation to pain in specific area of the body without loss of consciousness.

History Cocaine – Isolated by Niemann in 1860. –Introduced by koller In 1884 as topical optical anesthetic. Procaine – Synthesized by Einhorn in 1905. Lidocaine – Synthesized by Lofgren in 1943.

Ideal Criteria – Non irritating. – Water soluble. – Serializable. – Inexpensive. – Rapid onset of action.

Ideal Criteria – Should not produce permanent damage to the nerve tissue. – Potent. – Effective whichever route is given. – No post anesthetic side effect.

Classification (according to duration of action) – Short acting (30 to 60 minutes) Procaine (30 mins) Amethocaine (1 hour) – Intermediate acting (60 to 120 minutes) Lidocaine (1 -1. 5 hour) Pilocaine (2 hours) – Long acting (>2 hours) Bupivacaine (3 hours) Tetracaine
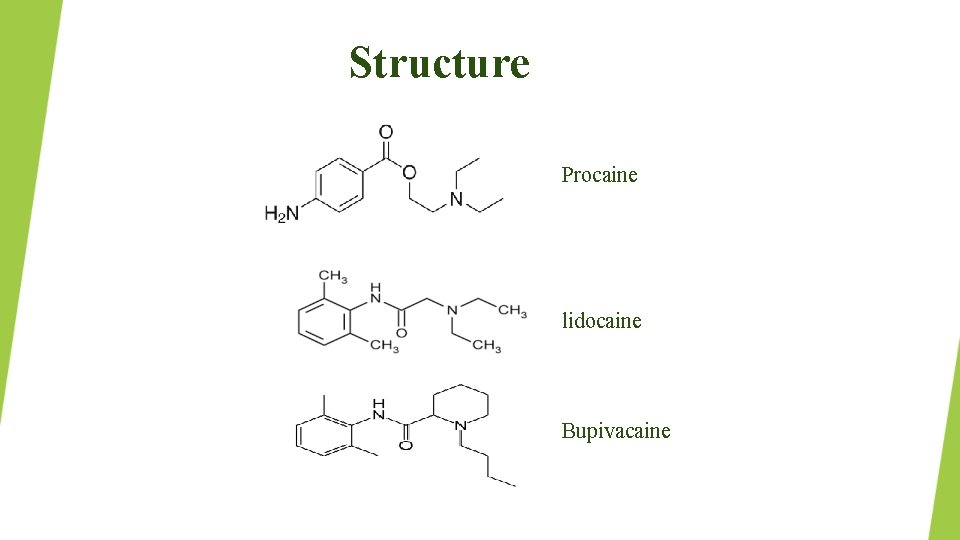
Structure Procaine lidocaine Bupivacaine

Classification(according to chemical structure) – Ester group Procaine Cocaine Benzocaine – Amide group Lidocaine Etidocaine
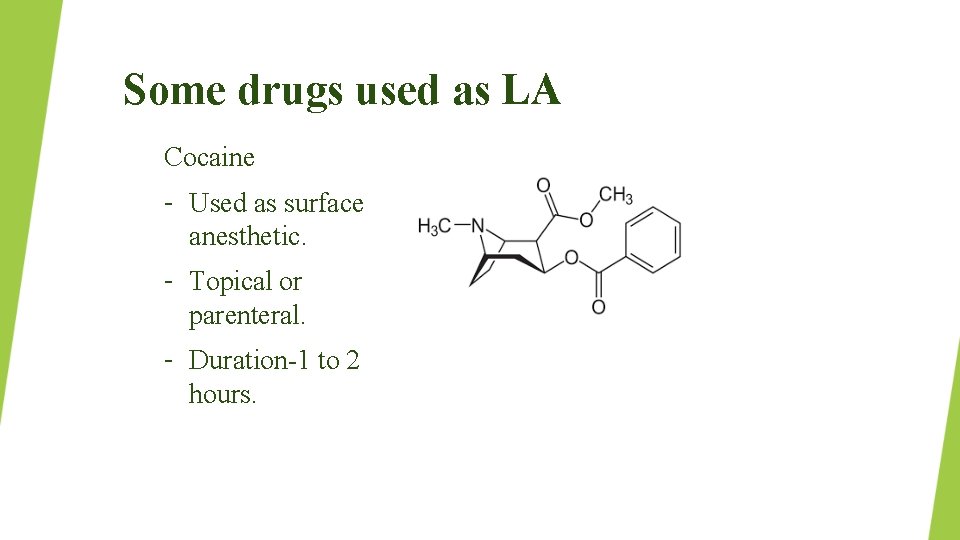
Some drugs used as LA Cocaine – Used as surface anesthetic. – Topical or parenteral. – Duration-1 to 2 hours.
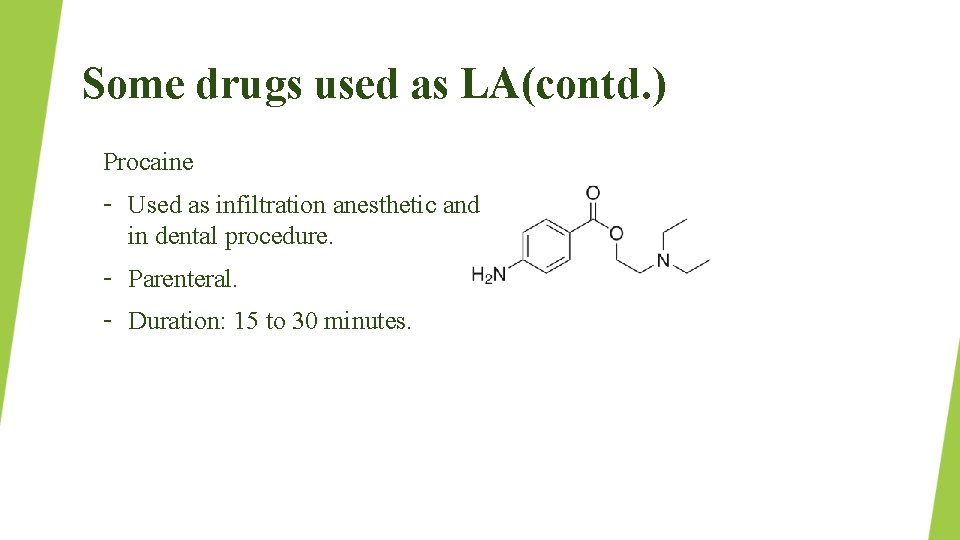
Some drugs used as LA(contd. ) Procaine – Used as infiltration anesthetic and in dental procedure. – Parenteral. – Duration: 15 to 30 minutes.

Some drugs used as LA(contd. ) Lidocaine – Used as epidural and spinal anesthetic. – Parenteral. – Duration: 30 to 60 mins.
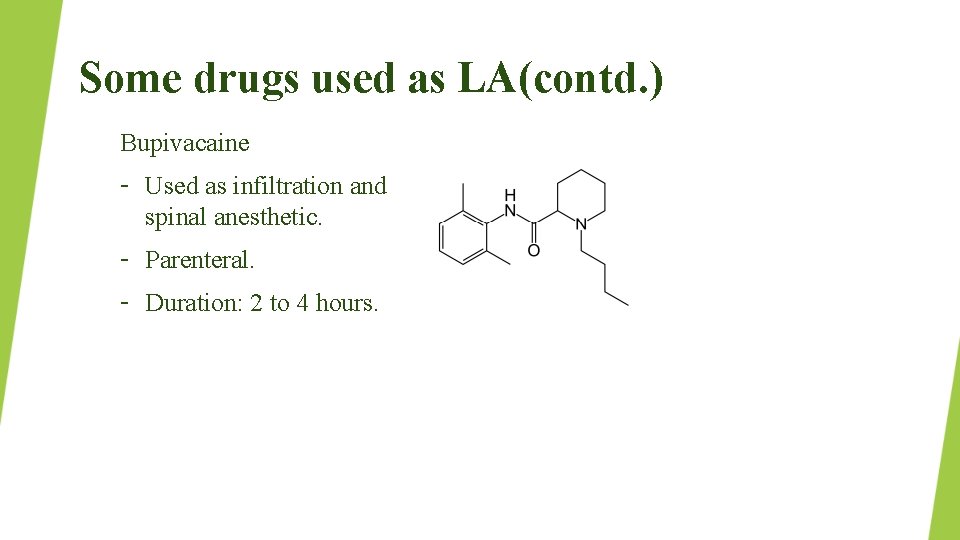
Some drugs used as LA(contd. ) Bupivacaine – Used as infiltration and spinal anesthetic. – Parenteral. – Duration: 2 to 4 hours.

Pharmacokinetics – Soluble surface anesthetics are rapidly absorbed from mucous membrane and abraded areas but absorption from intact skin is poor. – Rate of absorption depends on the blood flow to the area of application or injection. – Procaine is negligibly bound to plasma proteins, but amide local anesthetics are bound to plasma α 1 acid glycoprotein.

Pharmacokinetics (contd. ) – Amide linked LAs (lignocaine) are degraded macrosomes by dealkylaiton and hydrolysis. only in liver – Ester linked LAs (procaine) are rapidly hydrolyzed by plasma pseudo cholinesterase and remaining by esterase in the liver. – After oral ingestion both procaine and lignocaine have high first pass metabolism in the liver. Thus they are not effective orally for antiarrhythmic purpose.

Indications v LAs are used for Minor surgery Dental procedure Suturing small wounds Making an incision in a small area for removing superficial tissue sample for biopsy. During labor and delivery Gastrointestinal endoscopy Wart treatment Vasectomy Neonatal circumcision.

Adverse effect – Adverse effect may be classified as: – Those associated directly with blocking ion channels in cell membranes, such as cardiovascular and CNS toxicity. – Those due to other effects of drug or vehicle (mainly peripheral nerve complications). – Allergic reactions (often a mistaken diagnosis). – Mechanical or other effects of technique, such as needle trauma or introduction of infection. – Signs and symptoms of CNS toxicity include convulsions, followed by coma and respiratory depression.

Adverse effect(contd. ) – Adverse effect include Restlessness Dizziness Disorientation Light-headedness Rhythmical oscillation of the eyeballs Psychosis Slurred speech Slow heart rate Cardiac arrest

Contraindications – Local anesthetics are contraindicated in patient with known hypersensitivity, in the elderly, severe hemorrhage deformities, blood dyscrasias and hypertension.

Drug interactions Barbiturates may decrease activity of lidocaine. – Increased effects of lidocaine may occur if taken with beta blockers, cimetidine and quinidine. – – If lidocaine is used on a regular basis Its effectiveness may diminish when used with other medications.

Factors affecting the reaction of LA (lipid solubility) – All local anesthetics have weak bases. Increasing the lipid solubility leads to faster nerve penetration, block sodium channels, and speed up the onset of action. – The more tightly local anesthetics bind to the protein, the longer the duration of onset action. – Local anesthetics have two forms, ionized and nonionized. The nonionized form can cross the nerve membranes and block the sodium channels. – So, the more non ionized presented, the faster the onset action.

Factors affecting the reaction of LA (p. H influence) – Usually at range 7. 6 – 8. 9 – Decrease in p. H shifts equilibrium toward the ionized form, delaying the onset action. – Lower p. H, solution more acidic, gives slower onset of action

Factors affecting the reaction of LA (vasodilation) – Vasoconstrictor is a substance used to keep the anesthetic solution in place at a longer period and prolongs the action of the drug – vasoconstrictor delays the absorption which slows down the absorption into the bloodstream – Lower vasodilator activity of a local anesthetic leads to a slower absorption and longer duration of action – Vasoconstrictor used the naturally hormone called epinephrine (adrenaline). Epinephrine decreases vasodilator.

Routes of administration – There are five major routes for applying local anesthetics. These routes are summarized as follows: Topical Nerve block Infiltration Spinal Epidural

Topical anesthesia – Act as nerve blocking agent. E. g. , lidocaine. – This procedure can provide anesthesia on Skin and the mucus membrane of the rectum. Urethra and vagina. available in creams, ointments, aerosols, sprays, lotions, and jellies.

Nerve block anesthesia – Often a group of nerves, called a plexus or ganglion, that causes pain to a specific organ or body region can be blocked with the injection of medication into a specific area of the body. The injection of this nervenumbing substance is called a nerve block. – Affect the bundle of nerves serving the area to be operated upon. – This anesthesia used to block sensation in a limb or large area such as face.

How are nerve blocks used – Therapeutic nerve blocks are used to treat painful conditions. Such nerve blocks contain local anesthetic that can be used to control acute pain. – Diagnostic nerve blocks are used to determine sources of pain. These blocks typically contain an anesthetic with a known duration of relief. – Preemptive nerve blocks are meant to prevent subsequent pain from a procedure that can cause problems including phantom limb pain. – Nerve blocks can be used, in some cases, to avoid surgery.

Types of nerve block – Trigeminal nerve blocks (face) – Ophthalmic nerve block (eyelids and scalp) – Supraorbital nerve block (forehead) – Maxillary nerve block (upper jaw) – Sphenopalatine nerve block (nose and palate) – Cervical epidural, thoracic epidural, and lumbar epidural block (neck and back) – Cervical plexus block and cervical paravertebral block (shoulder and upper neck) – Brachial plexus block, elbow block, and wrist block – Subarachnoid block and celiac plexus block (abdomen and pelvis)

Local infiltration anesthesia – Uses for infiltrative anesthetics are as follows: – Blocks a specific group of nerves in a small area. – Subcutaneous infiltration (IV placement, superficial/shave biopsy, suturing) – Submucosal infiltration (dental procedures, laceration repairs) – Wound infiltration (postoperative pain control at incision site) – Intraarticular injections (postsurgical pain control, arthritic joint pain control) – Infiltrative nerve blocks (ankle block, scalp block, digit block)

Dosage administration guidelines – Lower concentrations of local anesthetics are typically used for infiltration anesthesia. – Variation in local anesthetic dose depends on the procedure, the degree of anesthesia required, and the individual patient's circumstances. – Reduced dosage is indicated in patients who are debilitated or acutely ill, in patients who are very young or very old, and in patients with liver disease, arteriosclerosis, or occlusive arterial disease.

Spinal anesthesia – In this anesthesia, an anesthetic agent is injected into the subarachnoid space through spinal needle. – Drugs affect large regional areas such as lower abdomen and leg.

Epidural anesthesia – It involves injection of the local anesthetic into the epidural (lumbar or caudal) space via a catheter that allows repeated infusions. – It absorb slowly in to the cerebrospinal fluid. – Used in labor and delivery.

Use of vasoconstrictor – Increase duration of action. – increase intensity of nerve block. – Decrease systemic toxicity.

Use of Vasoconstrictor – Added to the LA to delay absorption of the anesthetic from its injection site. – Administration of lidocaine 1% with epinephrine results in the same degree of blockade as that produce by lidocaine 2% with out vasoconstrictor.

Clinical Pharmacology of LA – Central nervous system central nervous system effects at low doses include sleepiness, light-headness, visual and auditory disturbances and restlessness. at higher concentrations nystagmus and muscular twitching may occur. - Cardiovascular system The cardiovascular effects of local anesthetics result partly from direct effects upon the cardiac and smooth muscle membranes and partly from indirect effects upon the autonomic nerves. Local anesthetics block cardiac sodium channels and thus depress abnormal cardiac pacemaker activity, excitability and conduction.

Clinical Pharmacology of LA – Blood The administration of large doses of prilocaine during regional anesthesia may lead to accumulation o the metabolite 0 -toluidine, an oxidizing agent capable of converting hemoglobin to methemoglobin that lead to pulmonary disease. - Allergic reaction The ester type local anesthetics are metabolized to p-aminobenzoic acid (PABA) derivatives. These metabolites are responsible for allergic reaction. amides are not metabolized to p-aminobenzoic acid that’s why no allergic reaction occur.

THANK YOU
- Slides: 37