Living Your Best After Cancer Healthy Diet Choices

“Living Your Best After Cancer: Healthy Diet Choices” Wendy Demark-Wahnefried, Ph. D, RD, LDN • Professor, Duke University School of Nursing & Duke University Medical Center’s Dept. of Surgery • Nationally-recognized nutritionist with research focusing on the relationship between diet and cancer diagnosis and treatment • 2003 -2005—Director of the Cancer Prevention, Detection & Control Research Program at Duke Comprehensive Cancer Center • 2003—Named Susan G. Komen Professor of Survivorship

Living Your Best After Cancer: Healthy Diet Choices Wendy Demark-Wahnefried, Ph. D, RD, LDN Professor: School of Nursing & Dept. of Surgery Duke University Medical Center

Outline • How important is diet for the cancer survivor? • What dietary changes are the most helpful?
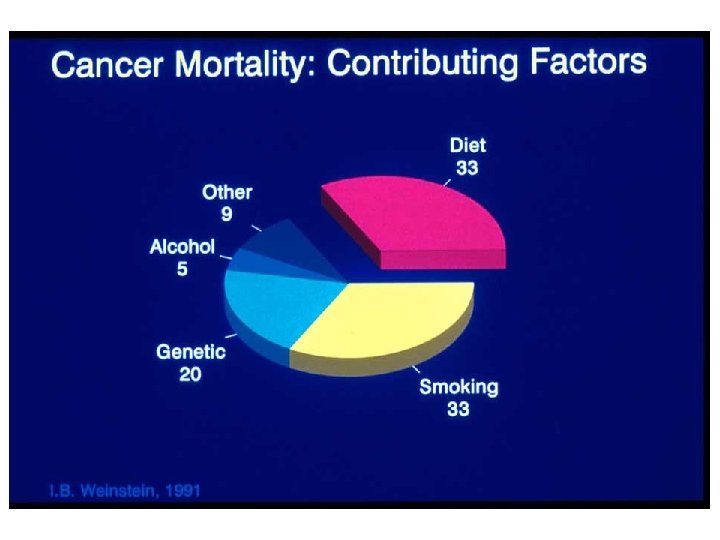


Striving for a Healthy Weight

Body Mass Index BMI = _ (Weight in Pounds) X 703 (Height in inches) x (Height in inches) If 25 or over: Overweight If 30 or over: Obese
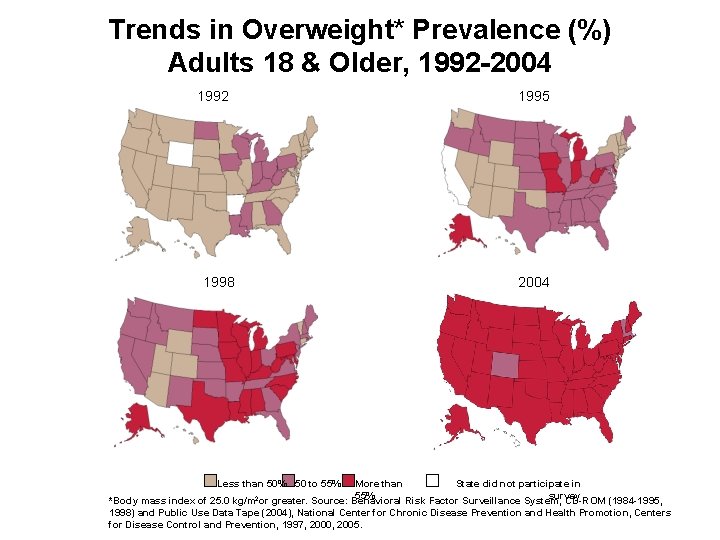
Trends in Overweight* Prevalence (%) Adults 18 & Older, 1992 -2004 1992 1998 1995 2004 Less than 50% 50 to 55% More than State did not participate in 55% survey *Body mass index of 25. 0 kg/m 2 or greater. Source: Behavioral Risk Factor Surveillance System, CD-ROM (1984 -1995, 1998) and Public Use Data Tape (2004), National Center for Chronic Disease Prevention and Health Promotion, Centers for Disease Control and Prevention, 1997, 2000, 2005.

Weight Management & Energy Balance Anorexia/Cachexia • Patients with select respiratory, G. I. & childhood cancers • Patients living with advanced cancer • Increasing weight to desired range important for recovery, well-being, functional status • Diet & exercise key roles +/pharmacotherapy Overweight/Obesity • Overweight a risk factor for cancers of endometrium, colon, esophagus, kidney, & breast(post-menopausal)– high proportion overweight (71% of breast/prostate survivors) • Overweight at dx poor prognostic indicator for cancer overall & cervical, esophageal, gastric, colorectal, uterine, pancreatic, hepatic, prostatic, biliary, renal, & breast cancers, & multiple myeloma & non. Hodgkin’s lymphoma • Weight gain common during & after treatment– linked with co-morbidity, functional decline & maybe recurrent/progressive CA
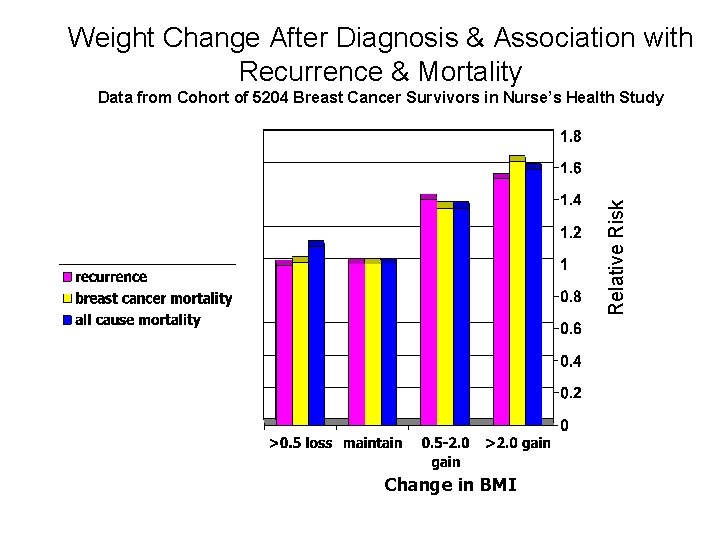
Weight Change After Diagnosis & Association with Recurrence & Mortality Relative Risk Data from Cohort of 5204 Breast Cancer Survivors in Nurse’s Health Study Change in BMI Kroenke et al. JCO 23: 1370 -8, 2005

• Maintain a healthful weight throughout life. • Balance caloric intake with physical activity • Lose weight if currently overweight or obese



Remember Portion Size Bagel 1980 vs. 2000 210 Calorie Difference 140 Calories 3” diam. 350 Calories 6” diam. French Fries 1980 vs. 2000 400 Calorie Difference 210 Calories 2. 4 oz. http: //www. cdc. gov/nccdphp/dnpa/obesity/trend/index. htm and http: //hin. nhlbi. nih. gov/oei_ss/menu. htm#sl 2 610 Calories 6. 9 oz.

Think Volumetrics Choose Lower Calorie Foods that Fill-you-up … 6 potato chips or 3 cups of popcorn

To date there are limited data showing a benefit of a healthful diet on cancer-related survival, however data show that cancer survivors who eat a plant-based diet have lower death rates from other diseases Compared with those who eat a Western diet Kroenke et al JCO 23: 9295 -303, 2005




Survivors and Supplements • No supplements have proven benefit on cancer-related outcomes, though some may reduce anxiety, etc. Herbal Miracle • Refer to responsible sources of information, i. e. , National Center for Complementary & Alternative Medicine (http: //nccam. nih. gov) • Rely on food as a source of nutrients 60 -89% of survivors take supplements 40 -50% begin additional supplements after diagnosis

A healthful body weight & healthy diet are important for the cancer survivor • Achieve/maintain a healthful weight • Consume a plant-based, nutrient-dense diet • Moderate alcohol intake • Seek local, regional or national programs that can provide support (i. e. , ACS, NCCAM, clinical trials, hospital-based or community initiatives.

Reach Out to ENhanc. E Wellness in Older Survivors (R 01 CA 106919) • Test the impact of a diet-exercise mailed material/telephone counseling program on weight loss & physical functioning in 640 prostate, colorectal & breast cancer survivors • 65+ years of age • 5+ years out from diagnosis • No progressive disease

Thank you!
- Slides: 23