Liver Transplantation GENERAL PRINCIPLES Liver transplantation is treatment
















































- Slides: 79

Liver Transplantation

GENERAL PRINCIPLES Liver transplantation is treatment of choice for : Acute and chronic end-stage liver disease, Hepatomas Early cholangiocarcinoma Some liver-based metabolic disorders 11/1/2020 dr. yekehfallah phd of nursing 2015 2

Depending on the patient's condition and organ availability, options include: whole-organ deceased donor split-liver deceased donor living donor transplantation. 11/1/2020 dr. yekehfallah phd of nursing 2015 3

Liver transplantation currently affords patients a survival posttransplant of greater than 85% at 1 year and greater than 70% at 5 years. 11/1/2020 dr. yekehfallah phd of nursing 2015 4

Indications for Liver Transplantation in Adults: Etiologies of End-Stage Liver Disease 1. Fulminant Hepatic Failure 2. Alcoholic Liver Disease 3. Chronic Hepatitis C 4. Chronic Hepatitis B 5. Non-alcoholic steatohepatitis 6. Autoimmune Hepatitis 7. Primary Biliary Cirrhosis 8. Primary Sclerosing Cholangitis 9. Hepatic tumors 10. Metabolic and genetic disorders dr. yekehfallah phd of nursing 2015 11/1/2020 5

Indications for Liver Transplantation in Adults Presence of irreversible liver disease and a life expectancy of less than 12 months with no effective medical or surgical alternatives to transplantation Chronic liver disease that has progressed to the point of significant interference with the patient's ability to work or with his/her quality of life Progression of liver disease that will predictably result in mortality exceeding that of transplantation (85% one-year patient survival and 70% five-year survival) 11/1/2020 dr. yekehfallah phd of nursing 2015 6

Manifestations of End-Stage Liver Disease Progressive jaundice Intractable ascites Spontaneous bacterial peritonitis Hepatorenal Syndrome Encephalopathy Variceal bleeding Intractable pruritus Chronic fatigue (such as resulting in loss of gainful employment) Bleeding diathesis or coagulopathy 11/1/2020 dr. yekehfallah phd of nursing 2015 7

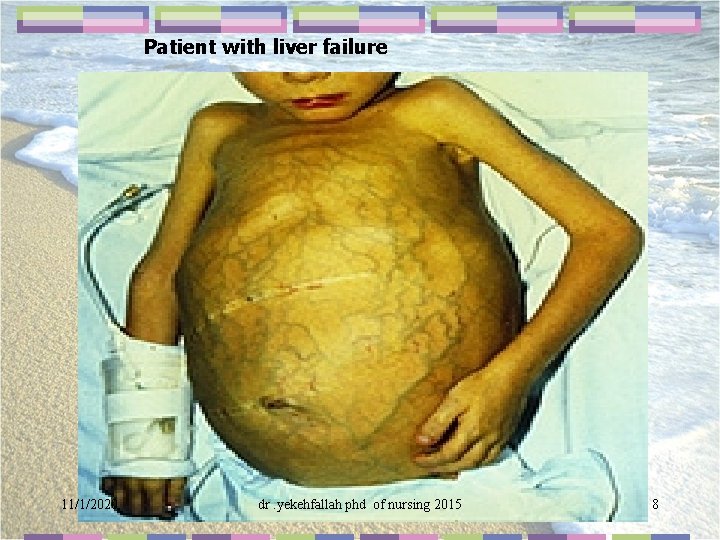
Patient with liver failure 11/1/2020 dr. yekehfallah phd of nursing 2015 8

Contraindications All Recipients Sepsis Recent extra-hepatic malignancy Irreversible cardiopulmonary disease Active substance abuse (HIV positive)Living donor recipients only Re-transplant Acute liver failure 11/1/2020 dr. yekehfallah phd of nursing 2015 9

11/1/2020 dr. yekehfallah phd of nursing 2015 10

CARE OF PATIENT DURING WAITING TIME Required a regular follow-up Every 2 to 4 weeks depending on severity of liver disease Routine US doppler, surveillance of oesophagal varices, management of ascites This follow-up can be done: • Directly by the transplant center • By the referring general physician or specialist • All therapeutic decisions should be made in accordance with the transplant physicians 11/1/2020 dr. yekehfallah phd of nursing 2015 11

Expanding The Donor Pool Age Hepatitis B/C organs High risk behavior History of malignancy Evaluate risk : benefit 11/1/2020 dr. yekehfallah phd of nursing 2015 12

Living Donor: Liver Transplantation Driven by: Expansion in number of patients requiring liver transplantation Shortage of deceased donor organs Increase in waiting list deaths 11/1/2020 dr. yekehfallah phd of nursing 2015 13

Living Donor Transplantation Recipient Advantages • Elective surgery • Scheduled (less uncertainty) • Avoid long waiting time Recipient Disadvantages • Increased technical complications • Arterial stenosis / thrombosis • Biliary leak / stricture 11/1/2020 dr. yekehfallah phd of nursing 2015 14

Living Donor Transplantation Donor Advantages • Emotional Gain Donor Disadvantages • • 11/1/2020 Psychological stress to donor and family Inconvenience / risk of evaluation process Operative mortality ( 1/150 liver) Major postoperative complications (2 -10%) Minor post operative complications (50%) Possible long term morbidity Unrecognized covert liver disease dr. yekehfallah phd of nursing 2015 15

Living Liver Donor Evaluation Donor Advocacy Team • Age < 55 yrs • Compatible blood group • History & physical • Routine labs • Ultrasound of liver • Volumetric analysis by MRA • R. lobe wt. = 1% recipient total wt 11/1/2020 dr. yekehfallah phd of nursing 2015 16

Living Donor Evaluation Decision to donate must be voluntary Informed consent Motivation to donate Behavioral and psychological health Donor recipient relationship Diversity issues 11/1/2020 dr. yekehfallah phd of nursing 2015 17

11/1/2020 dr. yekehfallah phd of nursing 2015 18

Preoperative management of complications associated with hepatic failure & cirrhosis Hepatic Encephalopathy Cerebral Edema Acute Renal Failure Infection & Sepsis Metabolic Derangements Malnutrition Coagulopathy Portal Hypertension 11/1/2020 dr. yekehfallah phd of nursing 2015 19

PRETRANSPLANT EVALUATION The pretransplant evaluation has several purposes and should be systematic, covering all organ systems to ensure that no major problems are overlooked. 11/1/2020 dr. yekehfallah phd of nursing 2015 20

PRETRANSPLANT EVALUATION A/Determine the etiology of liver disease and identify patients with decompensated liver cirrhosis: Spontaneous hepatic encephalopathy Refractory ascites Hepatorenal syndrome Hepatopulmonary syndrome Recurrent or refractory variceal bleeding Recurrent infections such as cholangitis or spontaneous bacterial peritonitis Intractable pruritus Severe malnutrition 11/1/2020 dr. yekehfallah phd of nursing 2015 21

PRETRANSPLANT EVALUATION B/Identify underlying medical problems that should be dealt with to optimize the candidate's overall condition before transplant C/Identify and address psychiatric, chemical dependency, and compliance issues and how they impact a potential candidate's appropriateness for, and timing of, transplant 11/1/2020 dr. yekehfallah phd of nursing 2015 22

PRETRANSPLANT EVALUATION D/Identify absolute contraindications: Active extrahepatic sepsis Extrahepatic malignancy Acquired immune deficiency syndrome Advanced cardiopulmonary disease E/For patients with hepatic malignancy, order preoperative imaging to detect extrahepatic spread 11/1/2020 dr. yekehfallah phd of nursing 2015 23

PRETRANSPLANT EVALUATION F/For acute (fulminant) liver failure (ALF) patients (generally more ill than those with chronic failure), refer them early to a transplant center 1/Poor prognostic indicators for spontaneous recovery from ALF: • • • Factor V level less than 30% p. H less than 7. 3 International normalized ratio (INR) greater than 6. 5 Stage 3 or 4 encephalopathy Lack of response to medical therapy within 24 to 48 hours 2/More severe hepatic parenchymal dysfunction, manifested by coagulopathy, hypoglycemia, and lactic acidosis 11/1/2020 dr. yekehfallah phd of nursing 2015 24

PRETRANSPLANT EVALUATION 3/More infectious complications 4/Higher incidence of renal failure 5/Higher incidence of cerebral edema and neurologic complications a/Some centers use intracranial pressure monitoring to monitor cerebral edema. b/Mannitol, hyperventilation, and thiopental have been used to prevent elevated intracranial pressure (>15 mm Hg). 6/Multiple-organ dysfunction syndrome 11/1/2020 dr. yekehfallah phd of nursing 2015 25

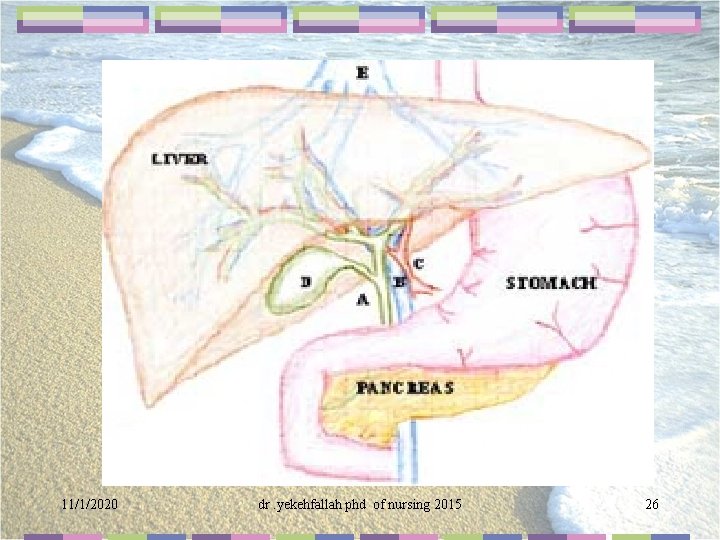
11/1/2020 dr. yekehfallah phd of nursing 2015 26

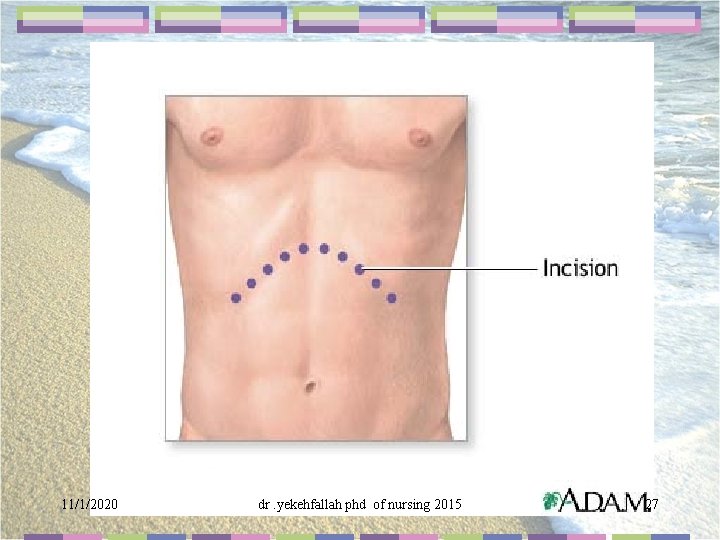
11/1/2020 dr. yekehfallah phd of nursing 2015 27

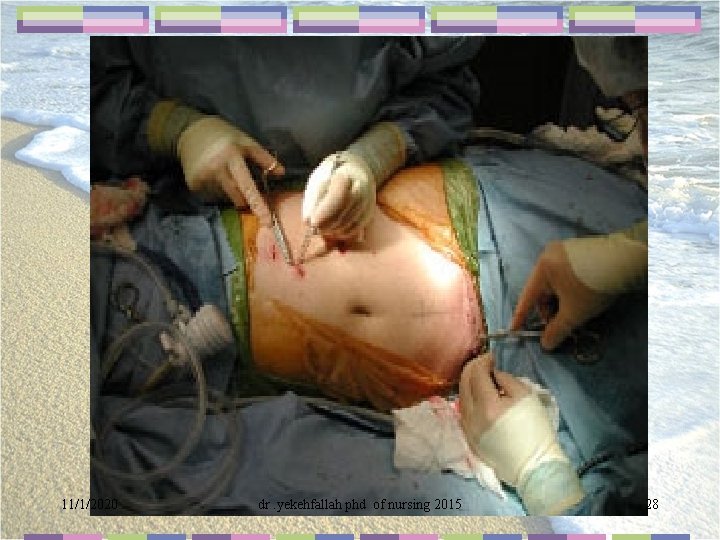
11/1/2020 dr. yekehfallah phd of nursing 2015 28

11/1/2020 dr. yekehfallah phd of nursing 2015 29

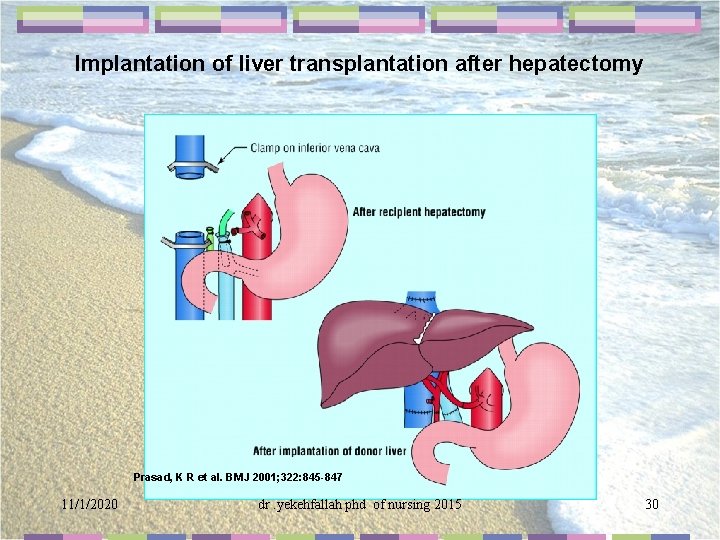
Implantation of liver transplantation after hepatectomy Prasad, K R et al. BMJ 2001; 322: 845 -847 11/1/2020 dr. yekehfallah phd of nursing 2015 30

11/1/2020 dr. yekehfallah phd of nursing 2015 31

11/1/2020 dr. yekehfallah phd of nursing 2015 32

11/1/2020 dr. yekehfallah phd of nursing 2015 33

11/1/2020 dr. yekehfallah phd of nursing 2015 34

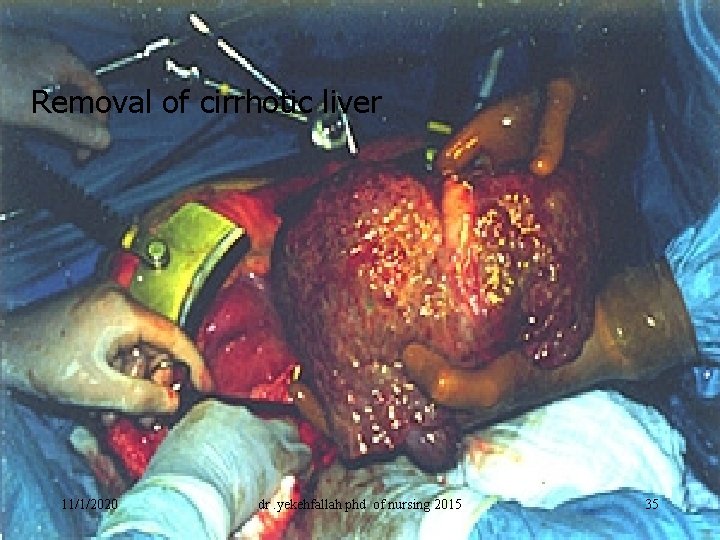
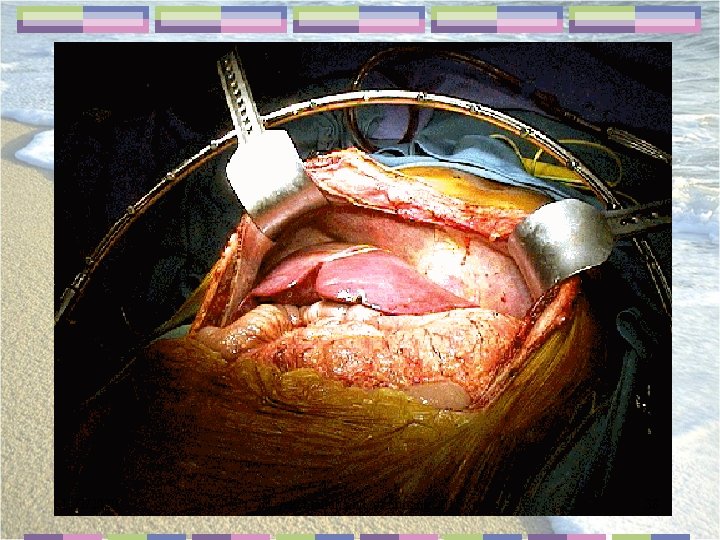
Removal of cirrhotic liver 11/1/2020 dr. yekehfallah phd of nursing 2015 35

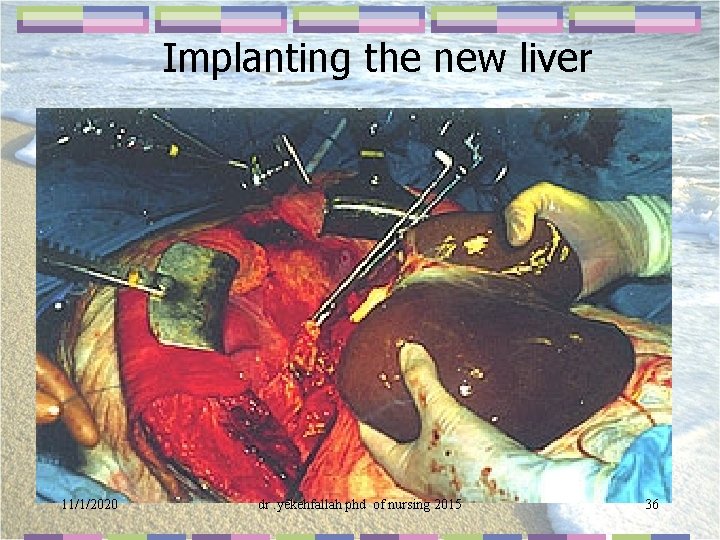
Implanting the new liver 11/1/2020 dr. yekehfallah phd of nursing 2015 36

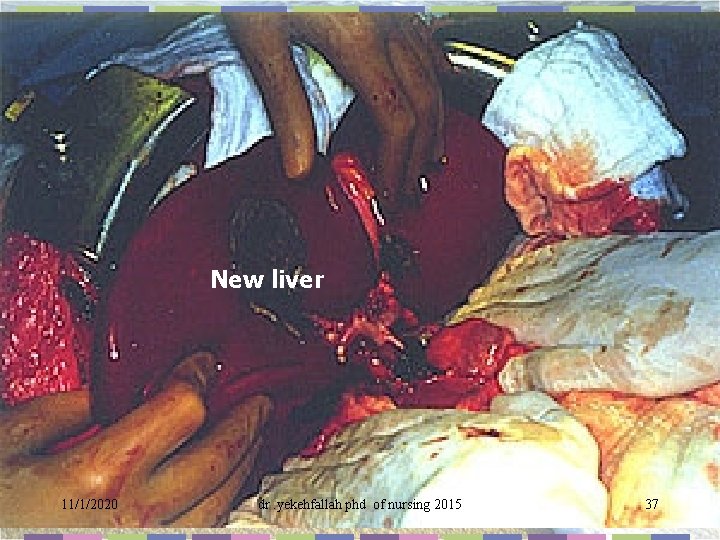
New liver 11/1/2020 dr. yekehfallah phd of nursing 2015 37

11/1/2020 dr. yekehfallah phd of nursing 2015 38

11/1/2020 dr. yekehfallah phd of nursing 2015 39

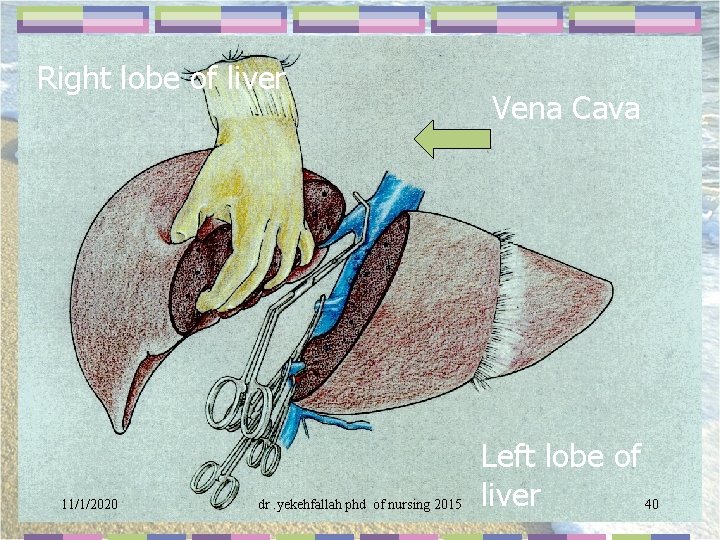
Right lobe of liver Vena Cava Left lobe of 11/1/2020 dr. yekehfallah phd of nursing 2015 liver 40

11/1/2020 dr. yekehfallah phd of nursing 2015 41

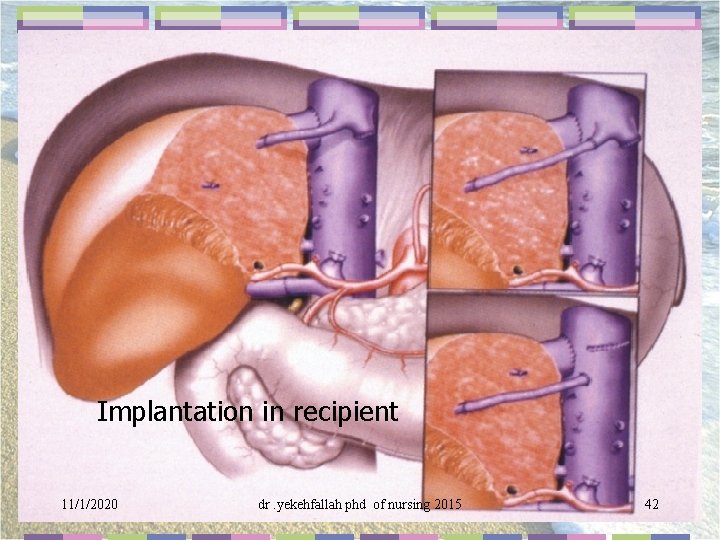
Implantation in recipient 11/1/2020 dr. yekehfallah phd of nursing 2015 42

11/1/2020 dr. yekehfallah phd of nursing 2015 43

11/1/2020 dr. yekehfallah phd of nursing 2015 44

11/1/2020 dr. yekehfallah phd of nursing 2015 45

11/1/2020 dr. yekehfallah phd of nursing 2015 46

INTRAOPERATIVE CARE A/ Venous and arterial monitoring catheters and large-volume infusion lines are placed in the operating room and can be a source of immediate morbidity (pneumothorax or hemothorax, pericardial tamponade, arterial pseudoaneurysm, air embolism) and hemorrhage in the coagulopathic patient. 11/1/2020 dr. yekehfallah phd of nursing 2015 47

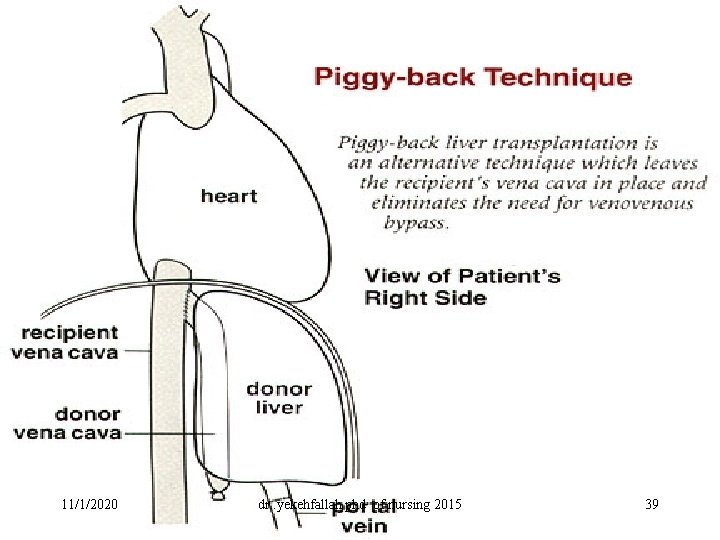
INTRAOPERATIVE CARE B/The transplant operation is divided into three phases: 1/Pre-anhepatic (mobilizing the recipient's diseased liver in preparation for its removal) 2/Anhepatic, characterized by coagulopathy and decreased venous return to the heart because of occlusion of the inferior vena cava and portal vein • Many centers routinely use a venous bypass system during this time. • After the native liver is removed, the donor liver is anastomosed to the appropriate structures to place the new liver in an orthotopic or piggyback (using a side-to-side cavoplasty technique) position. 3/Post-anhepatic, beginning after reperfusion. Hemodynamic instability on reperfusion can result in hypotension and serious arrhythmias due to acidosis, electrolyte abnormalities, air embolus, and cardiac strain. 11/1/2020 dr. yekehfallah phd of nursing 2015 48

Early Post-operative Management Extubate early Remove lines as soon as possible Immunosuppression Replace ascitic losses with albumin Avoid FFP unless • active bleeding • Invasive intervention is required 11/1/2020 dr. yekehfallah phd of nursing 2015 49

POSTOPERATIVE CARE The postoperative course can range from smooth to extremely complicated, depending mainly on the patient's preoperative status and the development of any complications. Initial posttransplant care should be in a critical care unit with continuous invasive hemodynamic monitoring and mechanical ventilation as needed. 11/1/2020 dr. yekehfallah phd of nursing 2015 50

11/1/2020 dr. yekehfallah phd of nursing 2015 51

POSTOPERATIVE CARE A/Stabilization and recovery of major organ systems functions B/Evaluation for continual improvement in graft function 1/Normalizing mental status 2/Normalizing coagulation profile 3/Resolution of hypoglycemia 4/Clearance of serum lactate 5/Serum transaminase levels usually rise during the first 24 to 48 hours secondary to reperfusion and preservation injury and then fall rapidly over the next 48 to 72 hours. Serum bilirubin and alkaline phosphatase levels may take several days longer to normalize. 11/1/2020 dr. yekehfallah phd of nursing 2015 52

POSTOPERATIVE CARE C/Provision of adequate immunosuppression D/Prevention along with vigilant monitoring for, and expeditious management of, complications in the immediate posttransplant period, to minimize morbidity and mortality 1/Avoid oversedation with benzodiazepines or morphine. 2/Avoid hypotension (systolic blood pressure below 100 mm Hg) to avoid renal dysfunction and graft thrombosis. Provision of adequate preload is paramount. 3/Limit central venous pressure to 8 to 12 cm H 2 O to • optimize portocaval pressure gradient and graft perfusion • minimize liver graft congestion/edema and bleeding risk from caval anastomoses 11/1/2020 dr. yekehfallah phd of nursing 2015 53

POSTOPERATIVE COMPLICATIONS A/Surgical complications 1/Hemorrhage. - Bleeding is common and can be compounded by deficits in coagulation factors, fibrinolysis, and platelet function. - Blood loss should be monitored by serial measurements of hemoglobin and detection of changes associated with acute hypovolemia (e. g. , decreased central venous pressure and urine output). If bleeding persists despite correction of coagulation deficiencies, surgical exploration is indicated 11/1/2020 dr. yekehfallah phd of nursing 2015 54

POSTOPERATIVE COMPLICATIONS 2/Vascular complications. The overall incidence of vascular complications is reported to be 8% to 12%. Thrombosis is the most common early event; stenosis and pseudoaneurysm formation occur later. Doppler ultrasound evaluation is the initial investigation of choice, with more than 90% sensitivity and specificity for thrombosis. a/Hepatic artery thrombosis (HAT) has a reported incidence of approximately 2% in adults and 10% in children. If detected early, up to 70% of grafts can be salvaged with urgent exploration, thrombectomy, or revision of the anastomosis. b/Thrombosis of the portal vein or hepatic veins is far less frequent. Liver dysfunction, tense ascites, and variceal bleeding can occur. If thrombosis is diagnosed early, operative thrombectomy and revision of the anastomosis may be successful. If thrombosis occurs late, liver function is frequently preserved because of the collateral veins; a retransplant is usually not necessary 11/1/2020 dr. yekehfallah phd of nursing 2015 55

POSTOPERATIVE COMPLICATIONS 3/Biliary complications occur in 15% to 35% of cases. a/Leak (early) • (1) Clinical symptoms: fever, abdominal pain, and peritoneal irritation. • (2) Diagnosis: Bilious output from surgical drains; ultrasound may demonstrate a • fluid collection; hepatobiliary scintigraphy (e. g. , HIDA [hepatobiliary iminodiacetic acid] scan) may demonstrate extravasation of radioactive tracer; cholangiography] or ERCP [endoscopic retrograde cholangiopancreatography]) (3) Management: Endoscopic stent placement and biloma drainage, or operative repair hepaticojejunostomy). b/Stricture (later) most common at the anastomotic site, likely related to local ischemia • (1) Clinical symptoms: cholangitis or cholestasis, or both • (2) Diagnosis: Ultrasound, magnetic resonance cholangiopancreatography, cholangiography • (3) Management: balloon dilatation or stent placement across the stricture, or both. 11/1/2020 dr. yekehfallah phd of nursing 2015 56

POSTOPERATIVE COMPLICATIONS 4/Wound complications a/Superficial wound infection, hematoma, and seroma (early) • (1) Diagnosis: drainage, increasing pain, erythema, fluctuance • (2) Management: (Re)incision and drainage, allowing for healing by secondary intention (serial open wound dressing changes) , antibiotics b/Incisional hernias (later), associated with malnutrition, attenuated fascia, and immunosuppression 11/1/2020 dr. yekehfallah phd of nursing 2015 57

POSTOPERATIVE COMPLICATIONS 5/Primary nonfunction a/Incidence: 3% to 5% b/Mortality rate is more than 80% without a retransplant c/Definition: poor or no hepatic function from the time of transplant d/Associated donor factors. • (1) Donor age greater than 49 years • (2) Macrosteatosis greater than 30% • (3) Donor intensive care unit stay greater than 3 days • (4) Cold ischemia time greater than 18 hours • (5) Reduced-size grafts e/Diagnosis: rule out HAT, severe preservation injury, accelerated acute rejection, and severe infection, because they can mimic primary nonfunction. The diagnosis is usually based on clinical parameters; graft biopsy may be helpful in some cases. f/Treatment • (1) Intravenous prostaglandin E 1 • (2) Early relisting for retransplantation 11/1/2020 dr. yekehfallah phd of nursing 2015 58

POSTOPERATIVE COMPLICATIONS B/Medical complications 1/Neurologic most commonly related to drugs or a poorly functioning graft • a/Symptoms: • (1) Decreased level of consciousness • (2) Seizures • (3) Focal neurologic deficits • b/Other neurologic complications: • • 11/1/2020 (1) Hypoxic ischemic encephalopathy (2) Central pontine myelinolysis (3) Cerebral edema (4) Intracranial hematomas dr. yekehfallah phd of nursing 2015 59

POSTOPERATIVE COMPLICATIONS 2/Pulmonary in up to 75% of recipients a/Noninfectious complications (first postoperative week): • (1) Pulmonary edema • (2) Pleural effusions • (3) Atelectasis • (4) Acute respiratory distress syndrome (ARDS) • (a) incidence less than 5%, but mortality greater than 80% • (b) most common when underlying bacterial infection is present, multiple transfusions, hypertension, aspiration, and antilymphocyte therapy b/Infectious complications (after the first week): • (1) Bacterial • (2) Fungal • (3) Viral 11/1/2020 dr. yekehfallah phd of nursing 2015 60

POSTOPERATIVE COMPLICATIONS 3/Renal affecting almost all liver recipients. Renal failure increases the mortality rate. Causes of renal failure: a/Pretransplant • (1) Hepatorenal syndrome • (2) Acute tubular necrosis b/Postoperative • (1) Hypovolemia • (2) Ischemic acute tubular necrosis • (3) Drug nephrotoxicity (calcineurin inhibitors) • (4) Preexisting subclinical or overt renal disease (e. g. , diabetic nephropathy, hepatitis , membranoproliferative glomerulonephritis) 11/1/2020 dr. yekehfallah phd of nursing 2015 61

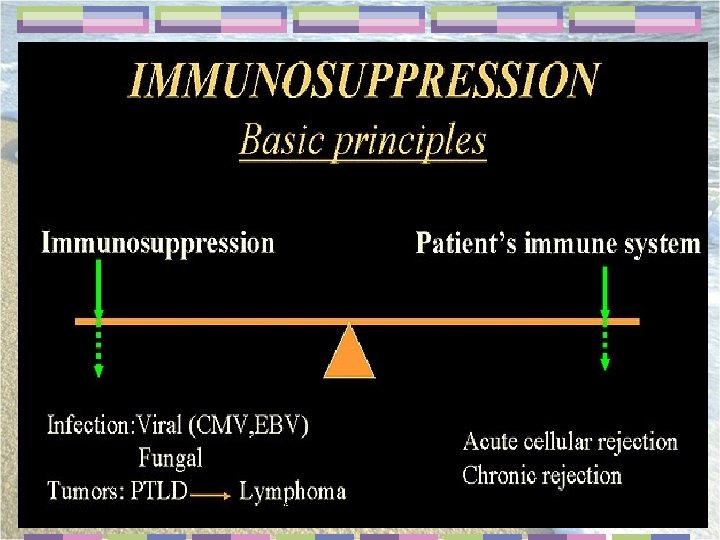
POSTOPERATIVE COMPLICATIONS 4/Immunosuppressive: a/Posttransplant diabetes b/Hyperlipidemia c/Viral and fungal infections d/Squamous and basal cell skin cancers and lymphoma 11/1/2020 dr. yekehfallah phd of nursing 2015 62

POSTOPERATIVE COMPLICATIONS 5/Recurrence of primary liver disease may require treatment and can significantly impact graft and patient survival a/Hepatitis B (Highly effective peritransplant and posttransplant longterm prophylaxis protocols that include lamivudine and/or hepatitis B immune globulin [HBIg] prevent hepatitis B recurrence. ) b/Hepatitis C (~20% cirrhosis rate from recurrent hepatitis C at 5 years posttransplant; no evidence-based recommendations on posttransplant treatment and efficacy of prophylaxis with pegylated interferon and ribavirin available) c/Autoimmune liver diseases (Recurrence rates of clinically significant autoimmune hepatitis, primary sclerosing cholangitis, and primary biliary cirrhosis are low and controversial; long-term posttransplant immunosuppression that includes steroids may offer theoretical [but not evidence-based] added benefits with regard to autoimmune disease recurrence prevention. ) 11/1/2020 dr. yekehfallah phd of nursing 2015 63

Post-operative complications & management of liver transplant patients Right pleural effusion • May affect ventilation, necessitating drainage. Hepatic edema secondary to aggressive resuscitation & increased intravascular volume. • Goal CVP 6 -10. Minimize increased hepatic vein pressures 11/1/2020 dr. yekehfallah phd of nursing 2015 64

Post-operative complications & management of liver transplant patients Renal failure • Elevation of creatinine & BUN observed in nearly all transplant patients secondary to ATN, hepatorenal syndrome. Usually self-limiting. May necessitate therapy with loop diuretics, renal replacement therapy. 11/1/2020 dr. yekehfallah phd of nursing 2015 65

Post-operative complications & management of liver transplant patients Electrolyte Derangements • Recovering graft increases demand for magnesium & phosphorous. • Transfusion of citrate rich blood products results in decreased serum magnesium & calcium. • Rapid correction of chronic hyponatremia with isotonic solution can have severe neurological consequence. Judicious use of hypotonic solutions with goal of serum Na 125 -130 advised. 11/1/2020 dr. yekehfallah phd of nursing 2015 66

Post-operative complications & management of liver transplant patients Thrombocytopenia • Preoperative portal hypertension results in splenomegaly & platelet sequestration. Generally improves as graft recovers. May necessitate replacement if bleeding is encountered or invasive procedures are planned. Splenectomy is rarely indicated. • Platelet dysfunction secondary to renal & hepatic failure may be improved acutely with DDAVP. 11/1/2020 dr. yekehfallah phd of nursing 2015 67

Post-operative complications & management of liver transplant patients Biliary leak • RUQ pain, fever, persistent elevation of bilirubin, liver enzymes. Biloma on CT. • Treated with endoscopic stent, percutaneous drainage. Possible surgical revision if duct is ischemic. Hepatic artery thrombosis • Persistent elevation or increasing liver enzymes, poor graft function. Diagnosed with U/S, CT angiography, MRA. • Treated with immediate revascularization. 11/1/2020 dr. yekehfallah phd of nursing 2015 68

Induction of Immunosuppression Triple therapy Initiated immediately following transplantation. • Calcineurin inhibitor (tacrolimus, cyclosporine) • anti-proliferative agent (mycophenolate) • corticosteroid taper. Agents vary according to etiology of liver disease • Thymoglobulin & Hb Ig utilized in hepatitis patients along with viral replication & to avoid coritocsteroid usage. 11/1/2020 dr. yekehfallah phd of nursing 2015 69

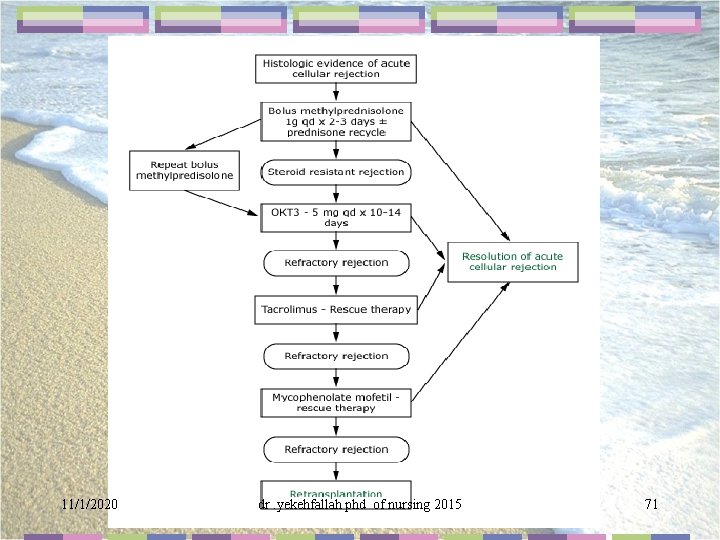
Allograft rejection Hyperacute rejection • Secondary to preformed Ab to graft antigen. • Extremely rare • Necessitates retransplantation. Acute Cellular Rejection • 70% of patients 5 to 14 days following transplant. • Heralded by fever, jaundice, elevation of liver enzymes. • Diagnosed by liver biopsy. Demonstrates endothelialitis & non-suppurative cholangitis. 11/1/2020 dr. yekehfallah phd of nursing 2015 70

11/1/2020 dr. yekehfallah phd of nursing 2015 71

11/1/2020 dr. yekehfallah phd of nursing 2015 72

Classification of Complications Graft dysfuntion or non-function Technical Immunological Infective Extrahepatic Drug effects Medical Recurrent Disease 11/1/2020 dr. yekehfallah phd of nursing 2015 73

Technical Complications Bleeding Hepatic artery thrombosis / stenosis Portal vein thrombosis / stenosis Biliary complications • Leak • Stricture • Sludge 11/1/2020 dr. yekehfallah phd of nursing 2015 74

Immunological Acute Rejection 5 -10 days post transplant but may occur at any time Clinical Elevated LFTS Liver Biopsy Portal tract inflammatory infiltrate Endothelialitis Destruction of biliary epithelium Treatment Steroids 11/1/2020 dr. yekehfallah phd of nursing 2015 75

Infective Bacterial < 15 days • Commonly lines /chest /urine Fungal > 15 days • • Prolonged hospitalization Broad spectrum antibiotics Re transplant Roux loop Viral > 4 weeks • CMV – recipients of CMV + organs 11/1/2020 dr. yekehfallah phd of nursing 2015 76

Extra-hepatic Cardiac failure / infarction Pulmonary Neurological Renal Endocrine • Diabetes (33%) Drug effects Recurrent disease 11/1/2020 dr. yekehfallah phd of nursing 2015 77

When to contact the transplant program: Sooner rather than later New medications Fever Abnormal liver functions tests Vomiting / diarrhea 11/1/2020 dr. yekehfallah phd of nursing 2015 78

? 11/1/2020 dr. yekehfallah phd of nursing 2015 79