LIVER Glucose Ketone bodies Glucose Fatty acids Glycerol
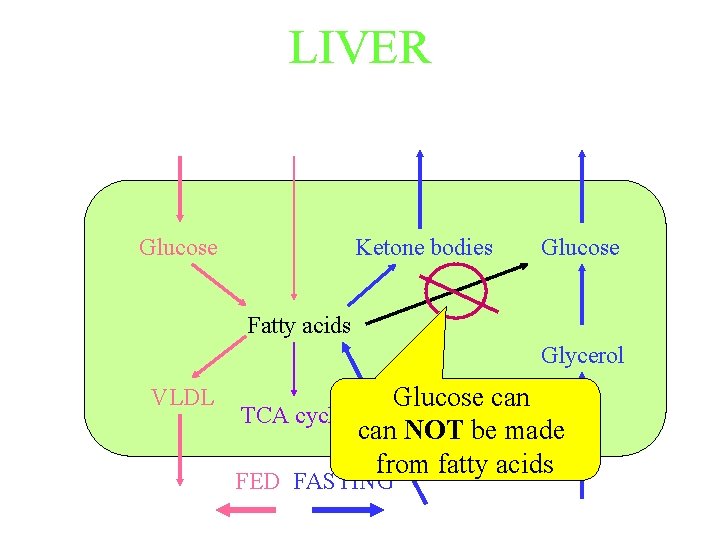
LIVER Glucose Ketone bodies Glucose Fatty acids Glycerol VLDL Glucose can TCA cycle can NOT be made from fatty acids FED FASTING
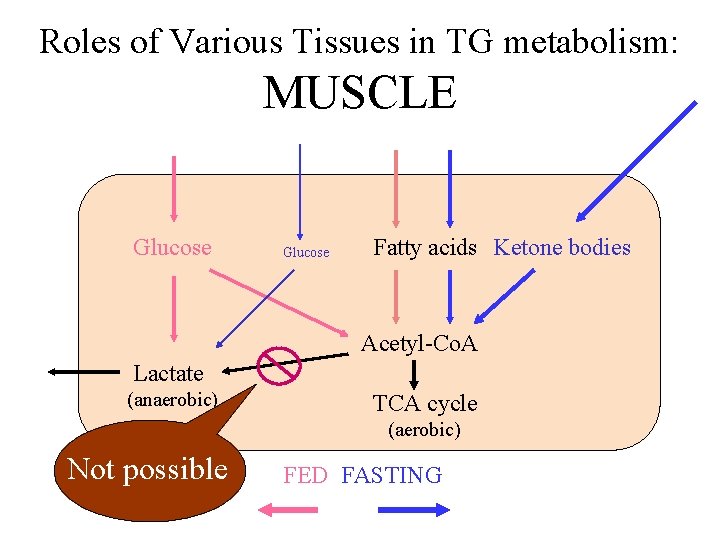
Roles of Various Tissues in TG metabolism: MUSCLE Glucose Fatty acids Ketone bodies Acetyl-Co. A Lactate (anaerobic) TCA cycle (aerobic) Not possible FED FASTING
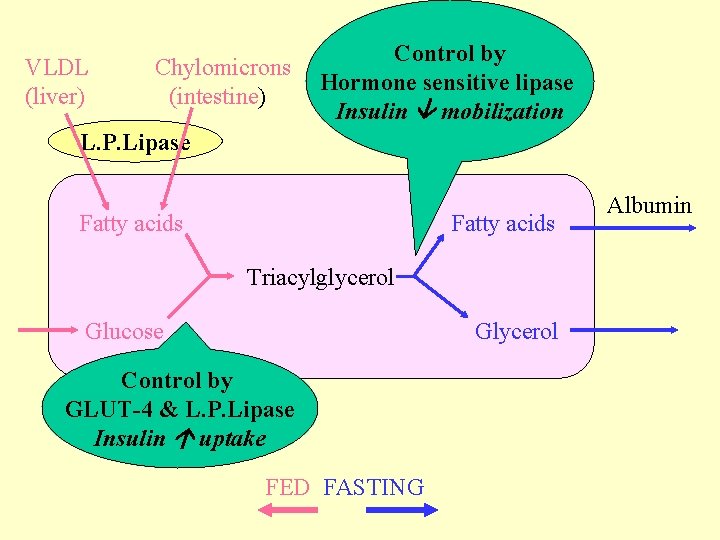
VLDL (liver) Chylomicrons (intestine) Control by Hormone sensitive lipase Insulin mobilization L. P. Lipase Fatty acids Triacylglycerol Glucose Glycerol Control by GLUT-4 & L. P. Lipase Insulin uptake FED FASTING Albumin

PPAR • Increased PPAR activity increases the amount of many adipocyte proteins as well as proteins in other tissues. • Thiazolidinediones (TZDs) increase the sensitivity of tissues to the effects of insulin; Type II diabetics have decreased insulin sensitivity. – TZDs work by increasing the activity of PPAR – The exact reason for the increased insulin sensitivity is not clear.
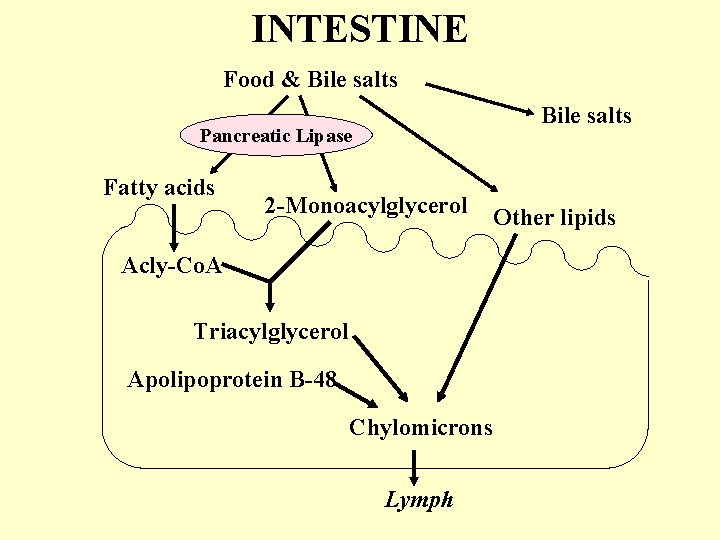
INTESTINE Food & Bile salts Pancreatic Lipase Fatty acids 2 -Monoacylglycerol Acly-Co. A Triacylglycerol Apolipoprotein B-48 Chylomicrons Lymph Other lipids
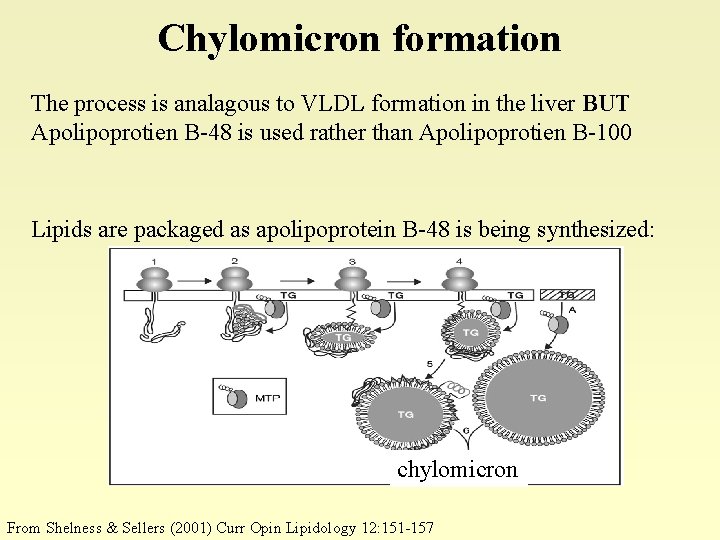
Chylomicron formation The process is analagous to VLDL formation in the liver BUT Apolipoprotien B-48 is used rather than Apolipoprotien B-100 Lipids are packaged as apolipoprotein B-48 is being synthesized: chylomicron From Shelness & Sellers (2001) Curr Opin Lipidology 12: 151 -157
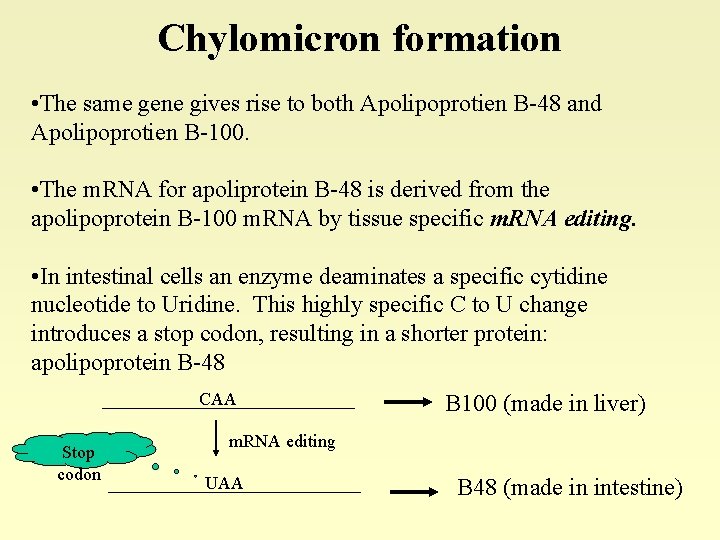
Chylomicron formation • The same gene gives rise to both Apolipoprotien B-48 and Apolipoprotien B-100. • The m. RNA for apoliprotein B-48 is derived from the apolipoprotein B-100 m. RNA by tissue specific m. RNA editing. • In intestinal cells an enzyme deaminates a specific cytidine nucleotide to Uridine. This highly specific C to U change introduces a stop codon, resulting in a shorter protein: apolipoprotein B-48 CAA Stop codon B 100 (made in liver) m. RNA editing UAA B 48 (made in intestine)
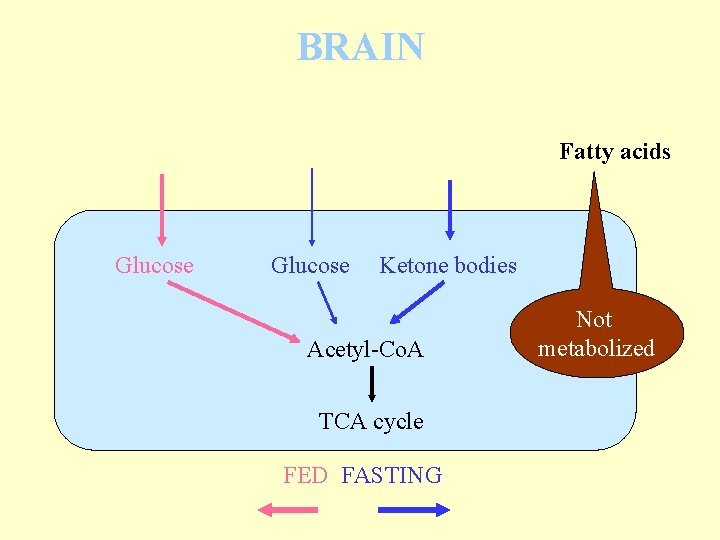
BRAIN Fatty acids Glucose Ketone bodies Acetyl-Co. A TCA cycle FED FASTING Not metabolized

Lipid Transport • Three Major Lipoprotein Pathways – Chylomicron pathway • Delivery of dietary lipid to tissues – VLDL • Delivery of lipid synthesized by liver to tissues – HDL • Cholesterol scavenger • Albumin – Transport of free fatty acids • Specialized Carriers – Some steroids – Some vitamins
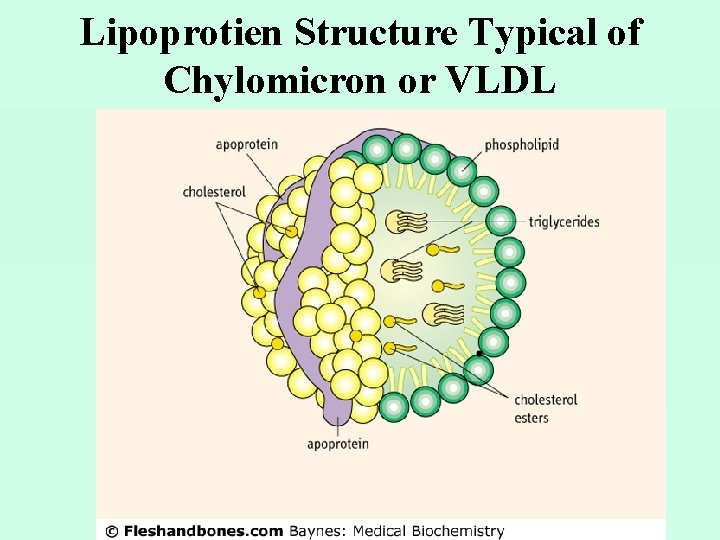
Lipoprotien Structure Typical of Chylomicron or VLDL

Lipid Transport • The term lipoprotein refers to a particle that contains lipid plus apolipoprotein. • The term apolipoprotein refers to a protein without the associated lipid. • Example: VLDL is a lipoprotein, and apolipoprotein B-100 is a protein component of VLDL

Lipid Transport • Important core apolipoproteins – Apolipoprotein B-100 • Liver - formation of VLDL – Apolipoprotien B-48 • Intestine - formation of chylomicrons • A shortened version of apolipoprotein B-100 shortened through RNA editing – Apolipoproteins A-I and A-II • Central protein component of HDL • Made in Liver and intestine
Lipid Transport • Apolipoproteins added extra-cellularly – Apolipoproteins C-I, C-III • C-II is required for the activation of lipoprotein lipase • C-III ia an antagonist of lipoprotein lipase • C-I is a modulator of cholesterol exchange – Apolipoprotein E • Involved in recognition and uptake of lipoproteins by the liver • Three common alleles (E 2, E 3, E 4) – E 2/E 2 is a risk factor for hyperlipoproteinemia – E 4 is a risk factor for Alzheimer Disease

VLDL Pathway

VLDL Liver Blood B-100 TG PL, Ch. E VLDL Cholesterol B-100 - Apolipoprotein B-100 TG - Triagylglycerol PL - Phospholipid Ch - Cholesterol Ch. E - Cholesterol ester
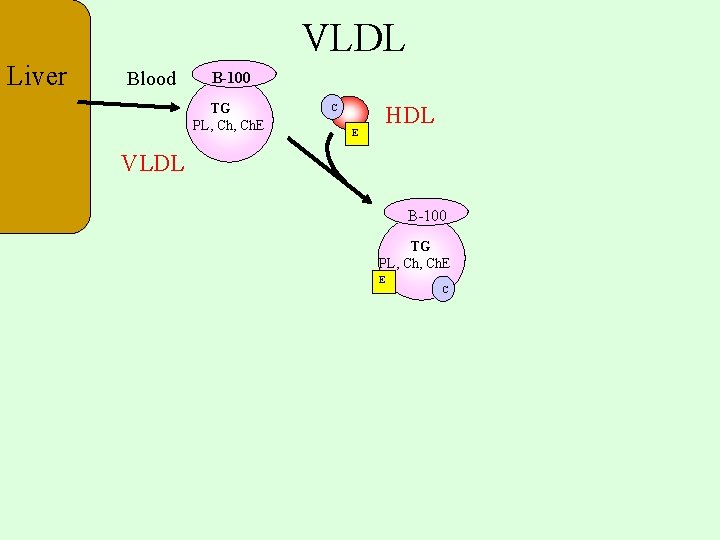
VLDL Liver Blood B-100 TG PL, Ch. E C E HDL VLDL B-100 TG PL, Ch. E E C
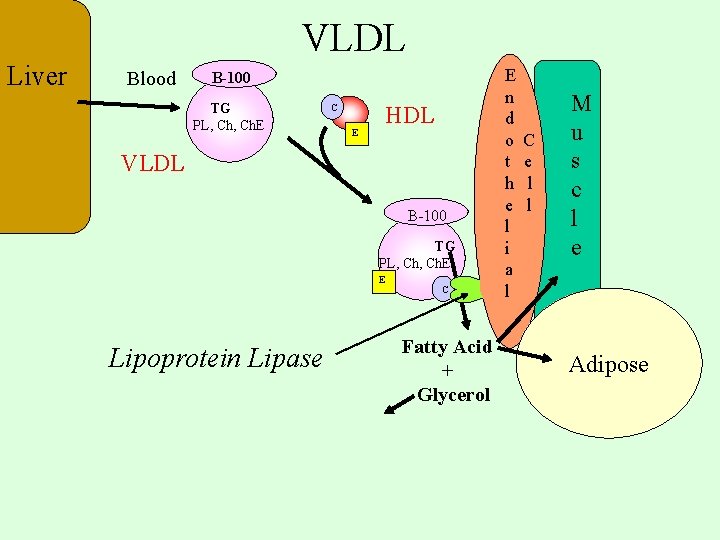
VLDL Liver Blood B-100 TG PL, Ch. E C E HDL VLDL B-100 TG PL, Ch. E E Lipoprotein Lipase C Fatty Acid + Glycerol E n d o t h e l i a l C e l l M u s c l e Adipose
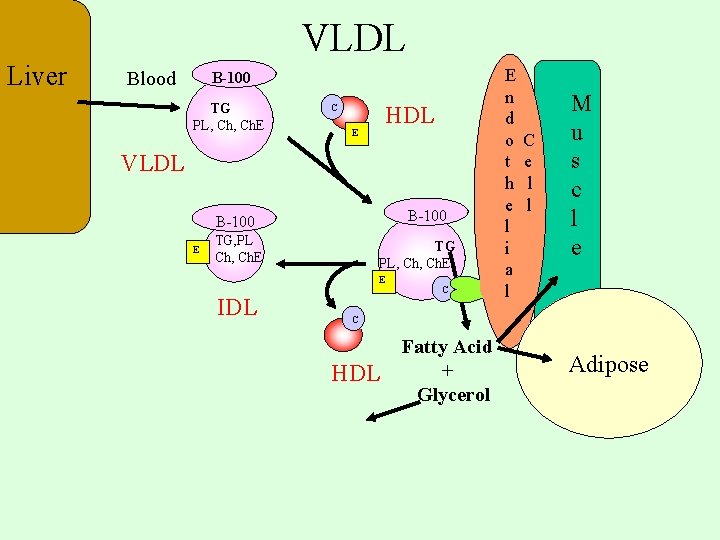
VLDL Liver Blood B-100 TG PL, Ch. E HDL C E VLDL B-100 E TG, PL Ch, Ch. E TG PL, Ch. E E IDL C E n d o t h e l i a l C e l l M u s c l e C HDL Fatty Acid + Glycerol Adipose
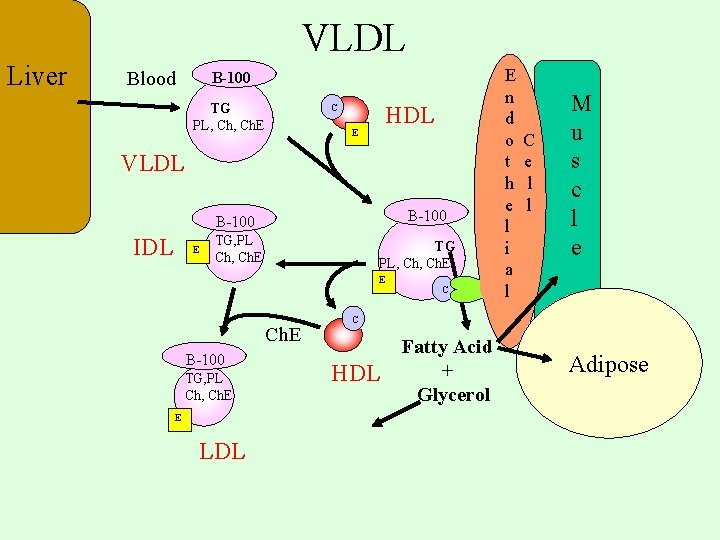
VLDL Liver Blood B-100 TG PL, Ch. E HDL C E VLDL B-100 IDL E TG, PL Ch, Ch. E TG PL, Ch. E E Ch. E B-100 TG, PL Ch, Ch. E E LDL C E n d o t h e l i a l C e l l M u s c l e C HDL Fatty Acid + Glycerol Adipose
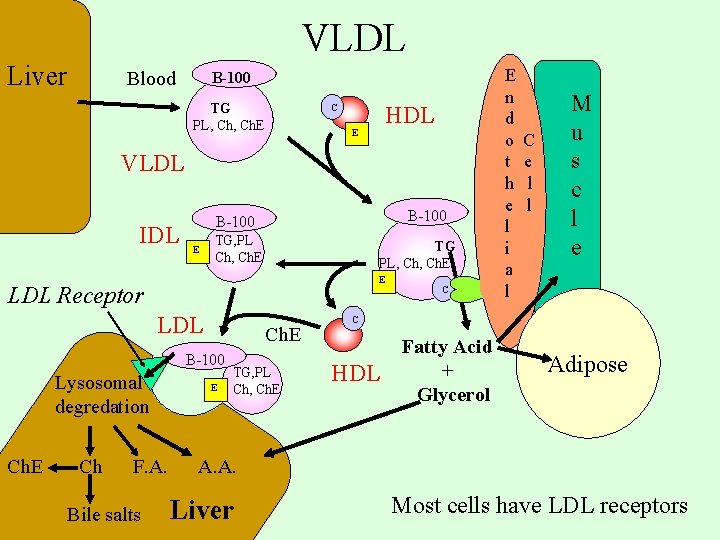
VLDL Liver Blood B-100 TG PL, Ch. E HDL C E VLDL IDL B-100 E TG, PL Ch, Ch. E TG PL, Ch. E E LDL Receptor LDL Ch. E B-100 Lysosomal degredation Ch. E Ch F. A. Bile salts E TG, PL Ch, Ch. E C E n d o t h e l i a l C e l l M u s c l e C HDL Fatty Acid + Glycerol Adipose A. A. Liver Most cells have LDL receptors
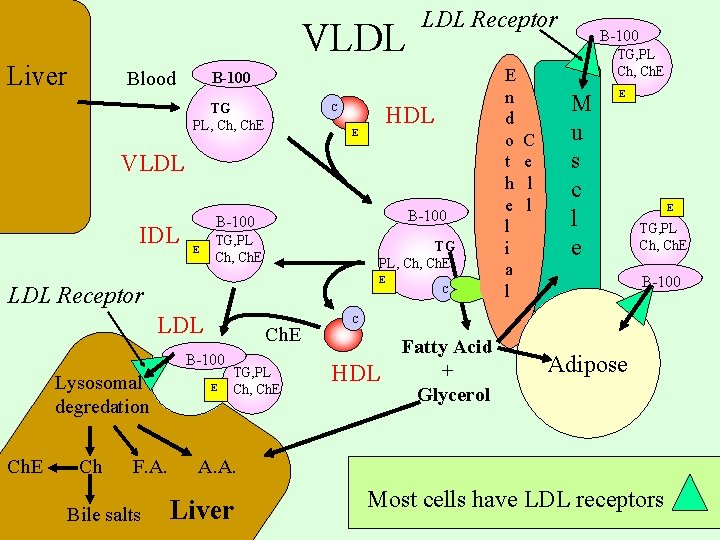
VLDL Liver Blood LDL Receptor B-100 TG PL, Ch. E HDL C E VLDL IDL B-100 E TG, PL Ch, Ch. E TG PL, Ch. E E LDL Receptor LDL Ch. E B-100 Lysosomal degredation Ch. E Ch F. A. Bile salts E TG, PL Ch, Ch. E C E n d o t h e l i a l B-100 TG, PL Ch, Ch. E C e l l M u s c l e E E TG, PL Ch, Ch. E B-100 C HDL Fatty Acid + Glycerol Adipose A. A. Liver Most cells have LDL receptors
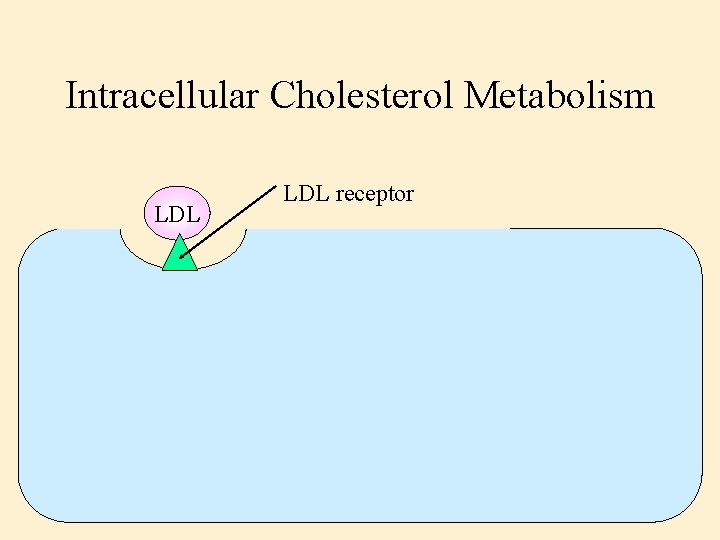
Intracellular Cholesterol Metabolism LDL receptor

Intracellular Cholesterol Metabolism Lysosome LDL
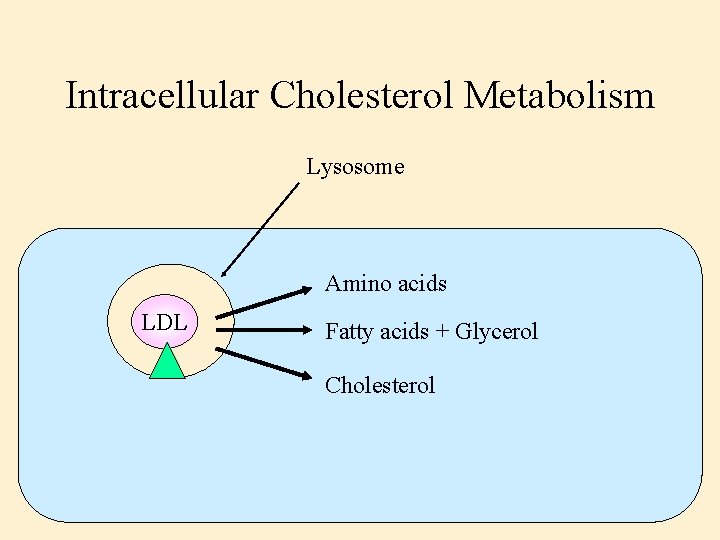
Intracellular Cholesterol Metabolism Lysosome Amino acids LDL Fatty acids + Glycerol Cholesterol
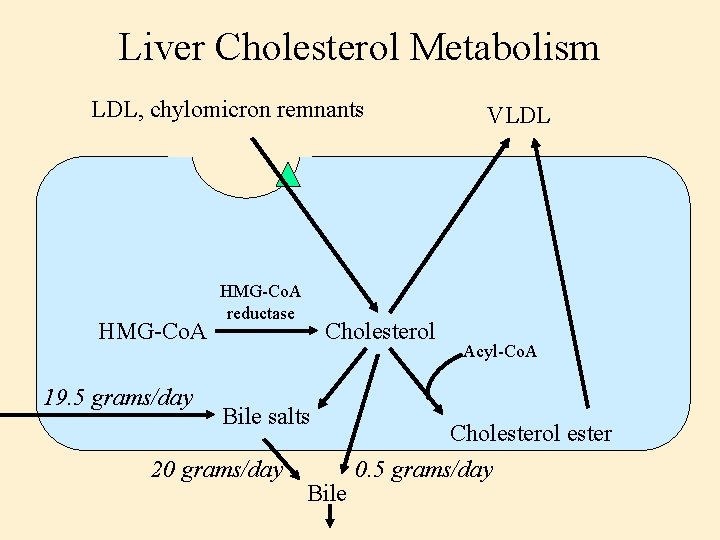
Liver Cholesterol Metabolism LDL, chylomicron remnants HMG-Co. A 19. 5 grams/day HMG-Co. A reductase Cholesterol Bile salts 20 grams/day Bile VLDL Acyl-Co. A Cholesterol ester 0. 5 grams/day
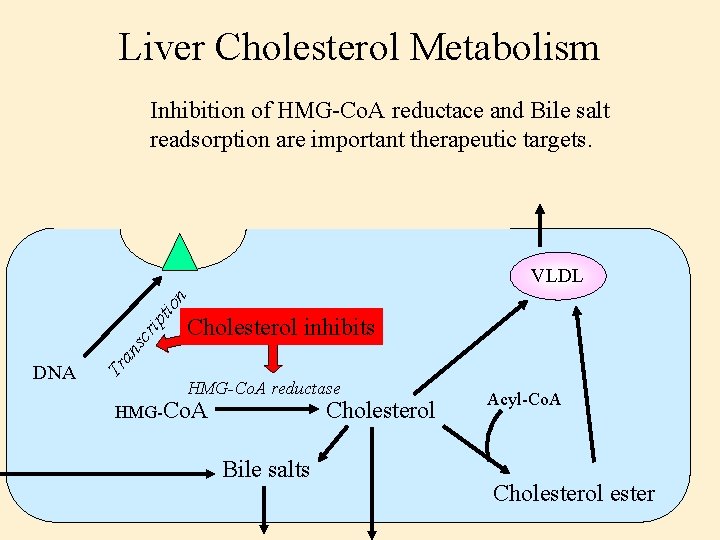
Liver Cholesterol Metabolism Inhibition of HMG-Co. A reductace and Bile salt readsorption are important therapeutic targets. Tr DNA Cholesterol inhibits an s cr ip tio n VLDL HMG-Co. A reductase HMG-Co. A Cholesterol Bile salts Acyl-Co. A Cholesterol ester
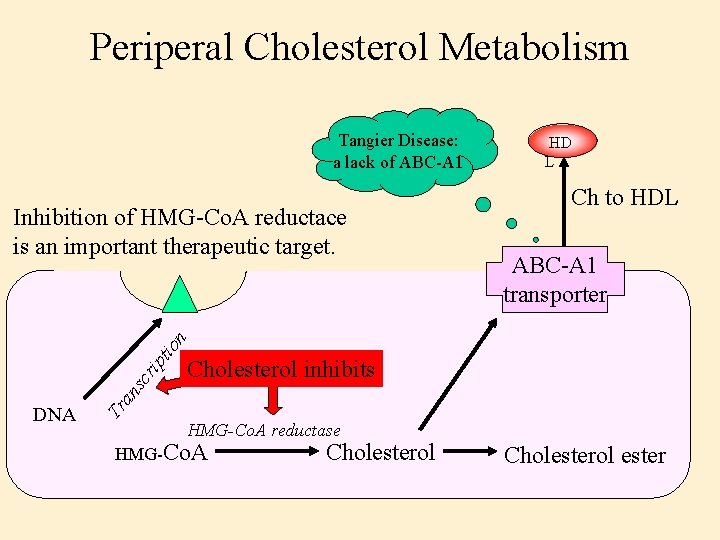
Periperal Cholesterol Metabolism Tangier Disease: a lack of ABC-A 1 Ch to HDL ABC-A 1 transporter Tr DNA Cholesterol inhibits an s cr ip tio n Inhibition of HMG-Co. A reductace is an important therapeutic target. HD L HMG-Co. A reductase HMG-Co. A Cholesterol ester
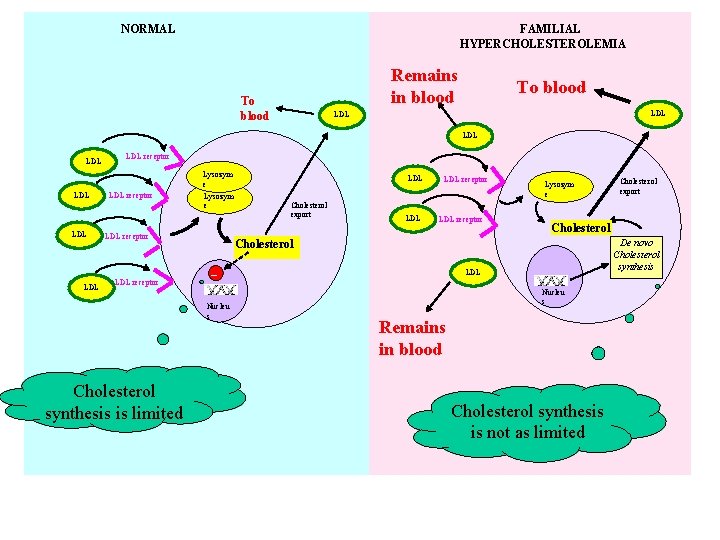
NORMAL FAMILIAL HYPERCHOLESTEROLEMIA Remains in blood To blood LDL LDL LDL receptor Lysozym e LDL receptor Cholesterol export LDL receptor Lysozym e - Cholesterol export Cholesterol De novo Cholesterol synthesis Cholesterol Nucleu s Cholesterol synthesis is limited LDL Nucleu s Remains in blood Cholesterol synthesis is not as limited

Chylomicron Pathway
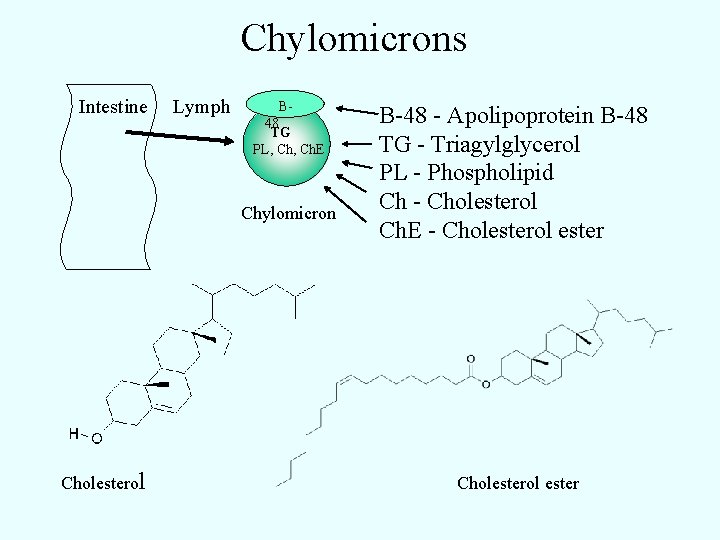
Chylomicrons Intestine Lymph B 48 TG PL, Ch. E Chylomicron Cholesterol B-48 - Apolipoprotein B-48 TG - Triagylglycerol PL - Phospholipid Ch - Cholesterol Ch. E - Cholesterol ester
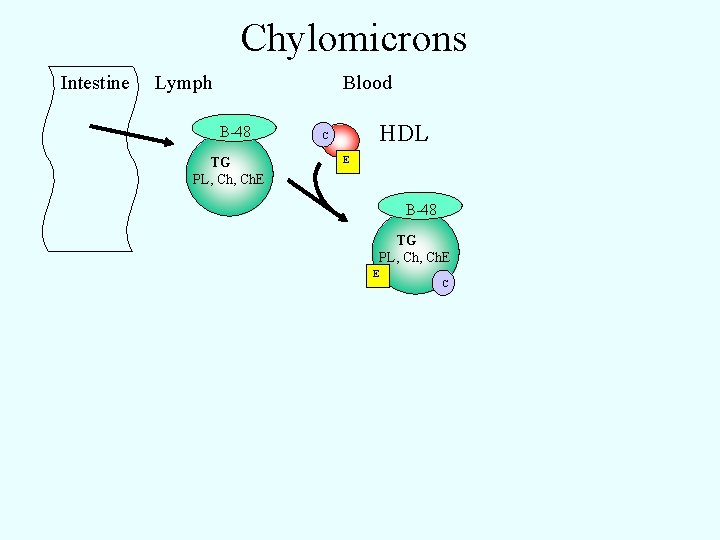
Chylomicrons Intestine Lymph Blood B-48 TG PL, Ch. E HDL C E B-48 TG PL, Ch. E E C
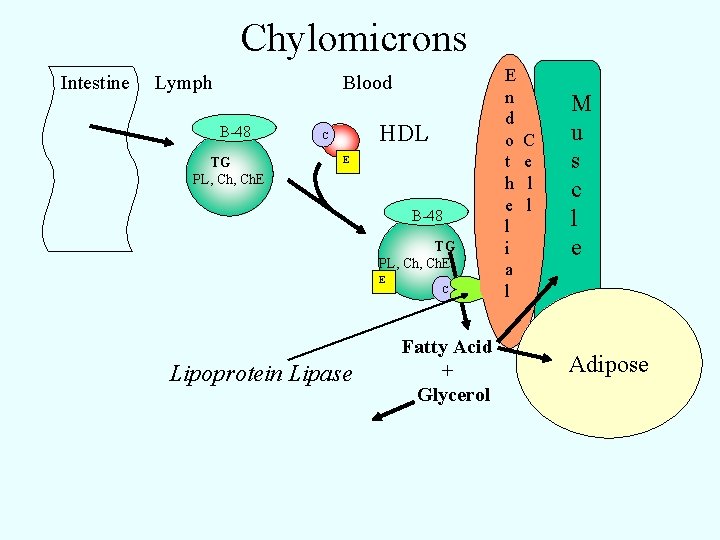
Chylomicrons Intestine Lymph Blood B-48 TG PL, Ch. E HDL C E B-48 TG PL, Ch. E E Lipoprotein Lipase C Fatty Acid + Glycerol E n d o t h e l i a l C e l l M u s c l e Adipose
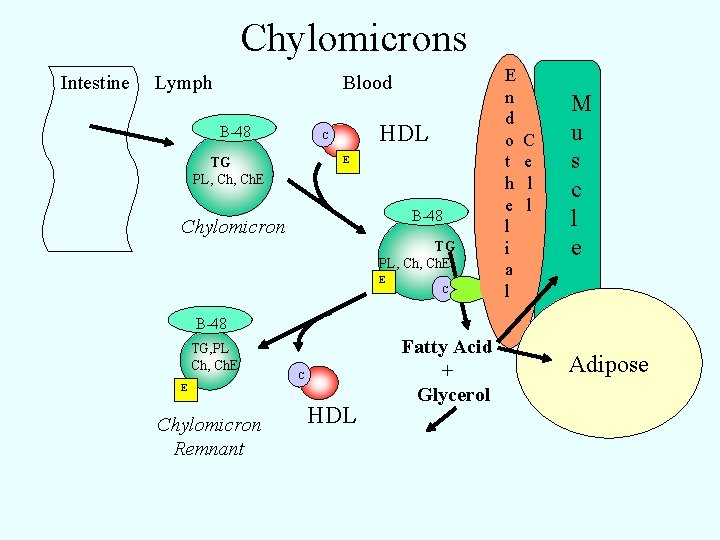
Chylomicrons Intestine Lymph Blood B-48 HDL C E TG PL, Ch. E B-48 Chylomicron TG PL, Ch. E E C E n d o t h e l i a l C e l l M u s c l e B-48 TG, PL Ch, Ch. E Chylomicron Remnant HDL Fatty Acid + Glycerol Adipose
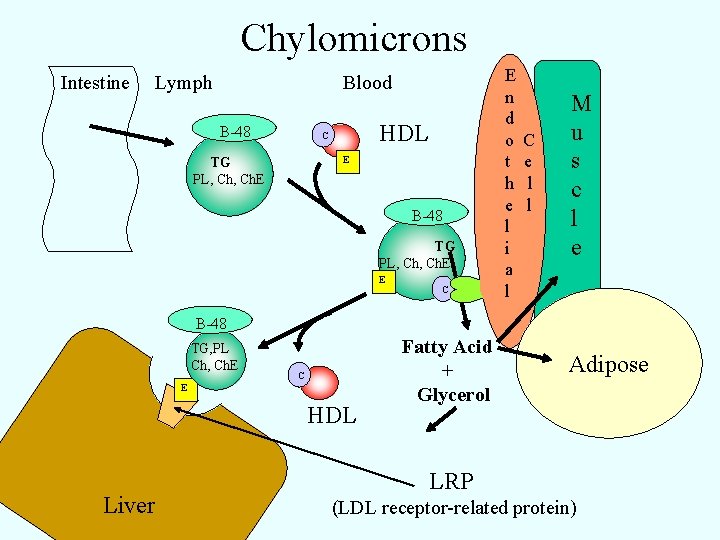
Chylomicrons Intestine Lymph Blood B-48 HDL C E TG PL, Ch. E B-48 TG PL, Ch. E E C E n d o t h e l i a l C e l l M u s c l e B-48 TG, PL Ch, Ch. E C E HDL Liver Fatty Acid + Glycerol Adipose LRP (LDL receptor-related protein)
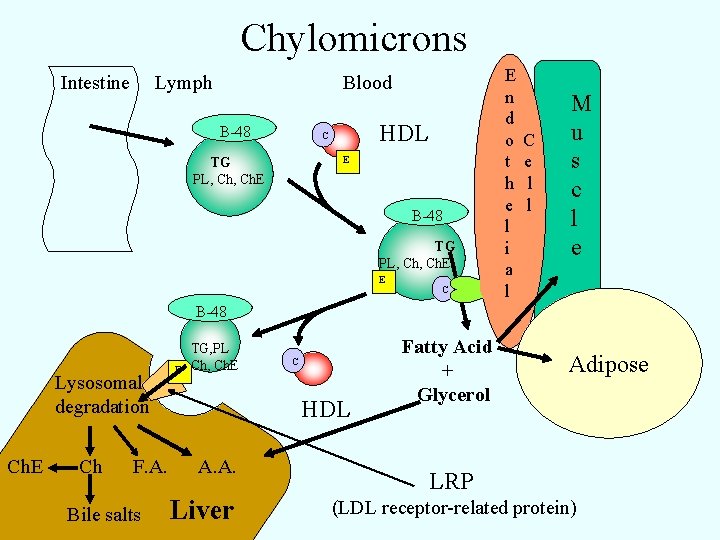
Chylomicrons Intestine Lymph Blood B-48 HDL C E TG PL, Ch. E B-48 TG PL, Ch. E E C E n d o t h e l i a l C e l l M u s c l e B-48 Lysosomal degradation Ch. E Ch F. A. Bile salts E TG, PL Ch, Ch. E C HDL A. A. Liver Fatty Acid + Glycerol Adipose LRP (LDL receptor-related protein)

HDL Pathway Reverse Cholesterol Transport Pathway
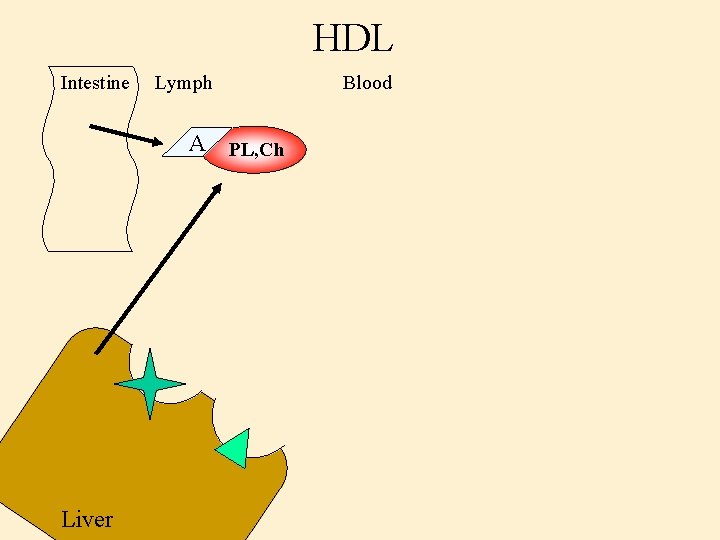
HDL Intestine Lymph A PL, Ch Liver Blood
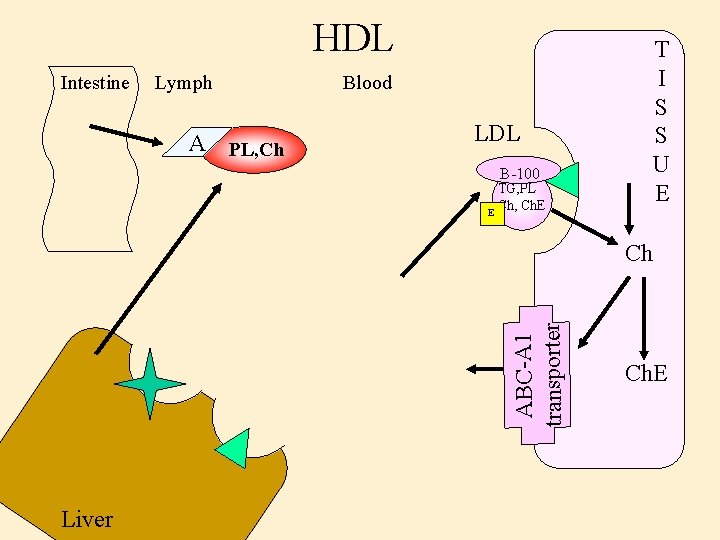
HDL Intestine Lymph A PL, Ch T I S S U E Blood LDL B-100 TG, PL Ch, Ch. E E ABC-A 1 transporter Ch Liver Ch. E
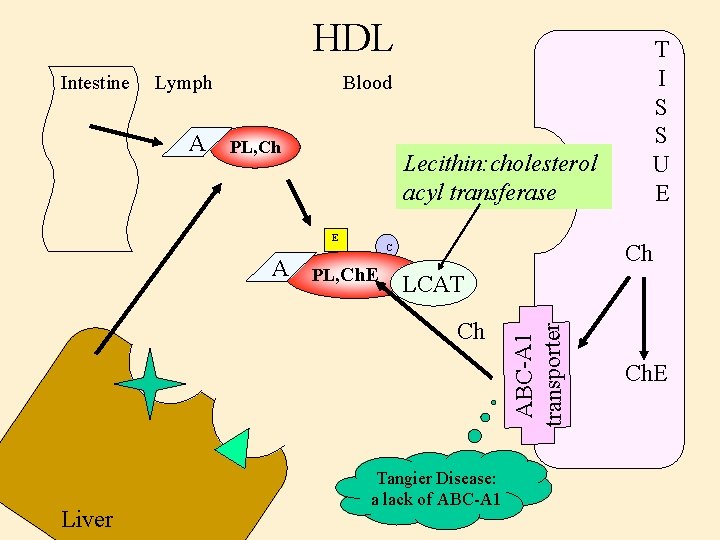
HDL Lymph A Blood PL, Ch Lecithin: cholesterol B-100 acyl transferase E A Ch C PL, Ch. E LCAT Ch Liver Tangier Disease: a lack of ABC-A 1 transporter Intestine T I S S U E Ch. E
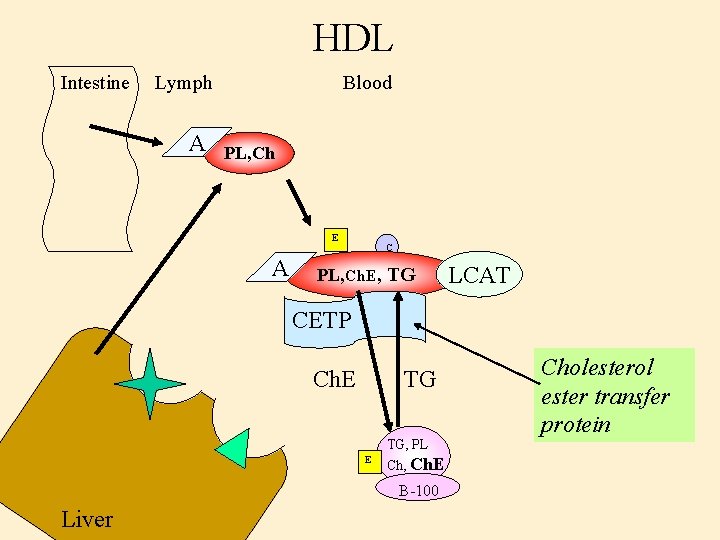
HDL Intestine Lymph A Blood PL, Ch E A C PL, Ch. E, TG LCAT CETP Ch. E TG, PL Ch, Ch. E B-100 Liver Cholesterol ester transfer protein
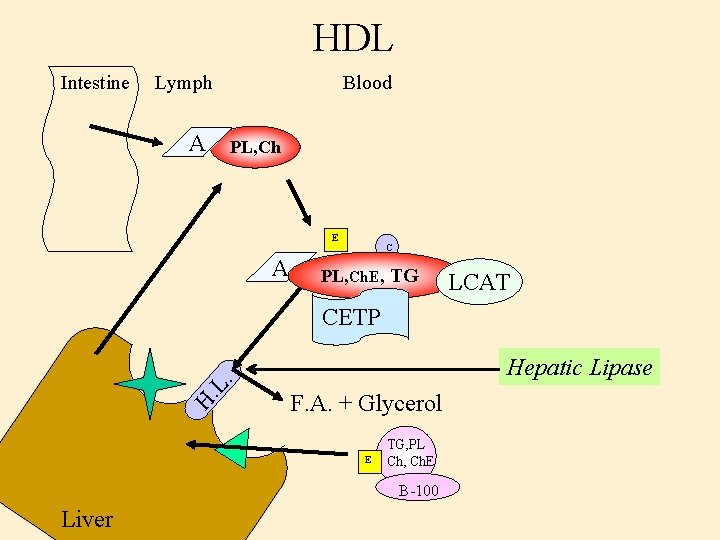
HDL Intestine Lymph A Blood PL, Ch E A C PL, Ch. E, TG LCAT H. L. CETP Hepatic Lipase F. A. + Glycerol E TG, PL Ch, Ch. E B-100 Liver
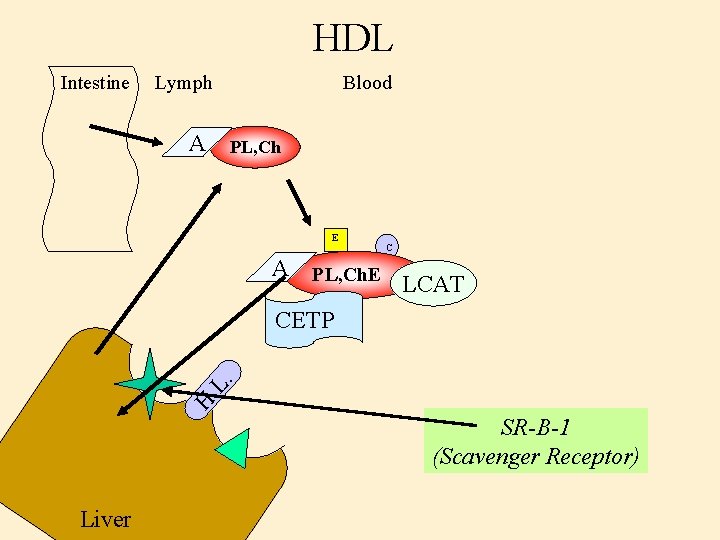
HDL Intestine Lymph A Blood PL, Ch E C A PL, Ch. E LCAT H. L. CETP SR-B-1 (Scavenger Receptor) Liver
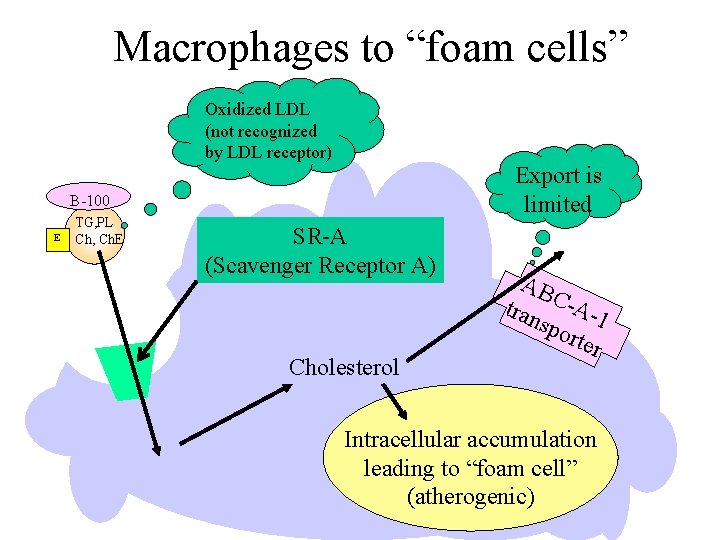
Macrophages to “foam cells” Oxidized LDL (not recognized by LDL receptor) Export is limited B-100 E TG, PL Ch, Ch. E SR-A (Scavenger Receptor A) Cholesterol AB tran C-A-1 spo rter Intracellular accumulation leading to “foam cell” (atherogenic)

Disorders of Lipid metabolism Type I diabetes: Very low insulin: cells act as if starving even though blood glucose is high. • Adipose: – Fatty acid mobilization up – Triacylglycerol synthesis is down • Liver: – Fatty acid synthesis is down (low glycolysis; low citrate) yet VLDL production is up. – Fatty acid oxidation is up – Ketone body formation is up: severe ketosis – Excess fatty acids go to VLDL formation: high blood lipid.

Dyslipidemias • Hypercholesterolemia – High LDL cholesterol • Hypertirgliceridemia – High blood triglycerides • Combined hyperlipidemia – High blood triglycerides and cholesterol • Hypoalphalipoproteinemia – Low HDL • Hypobetalipoproteinemia – Low VLDL & chylomicrons

Disorders of Lipid metabolism Type II diabetes: • Cells have a greatly reduced sensitivity to the effects of insulin • Molecular basis is poorly understood • Numerous hormones produced by adipocytes may play a role – Effects of obesity – PPAR modulates expression of important proteins

Disorders of Lipid metabolism Atheroschlerosis Important risk factors include: • High LDL/ HDL ratio • High concentration of small dense LDL particles – not efficiently taken up by liver – targets for oxidation – taken up by macrophage • Uptake of oxidized lipids by macrophages • Cholesterol processing by macrophages
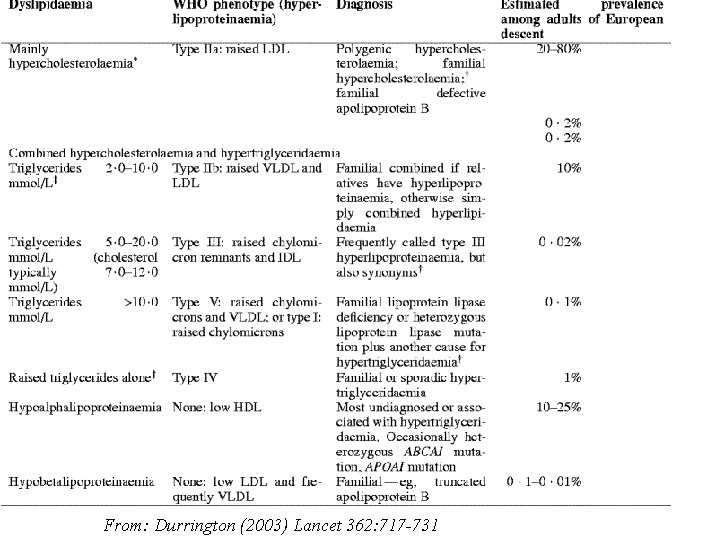
From: Durrington (2003) Lancet 362: 717 -731

Predisposing alleles and therapeutic targets: • Apolipoprotein B – VLDL/chylomicron metabolism • Apolipoproteins CII & CIII – rate of clearance of VLDL • Lipoprotein Lipase – Rate of clearance of VLDL • Apolipoprotein E – uptake of chylomicron remnants; LDL uptake – Three common Alleles • E 2/E 2 risk factor for hyperlipidemia • E 4 risk factor for Alzheimer

Predisposing alleles and therapeutic targets: • LDL receptor – Rate of clearance of LDL – Familial hypercholesteolemia • Apolipoprotein A 1 – low HDL • Cholesterol ester transfer protein (CETP) – HDL stability; LDL metabolism • ABC-A 1 protein – Cholesterol export from cells, particularly macrophage • PPARα PPARγ PPARδ
- Slides: 50