Lisbon Addictions 2017 Understanding Addiction A Health Inequalities

Lisbon Addictions 2017 Understanding Addiction: A Health Inequalities and Social Harms Perspective Dr Aileen O’Gorman University of the West of Scotland Aileen. OGorman@uws. ac. uk

This paper draws on a series of qualitative and ethnographic neighbourhood studies and analyses of drug trends and public policies in the UK, Scotland Ireland 2014

§ Estimated quarter of a billion people (5%) used drugs at least once in 2015 (UNODC: 2017). § Approximately one in ten (29. 5 m /0. 6%) designated with a drug use disorder and require treatment. § Who are the people whose drug use is problematised and why?

§ Global burden of disease and the concept of DALY (disabilityadjusted life years) flawed § focused on individual risk rather than the ecology of disease § exclude local context of poverty as a modifier of disease impact and the burden of disease on the poor. (King & Bertino, 2008) § strong links between poverty, deprivation, inequalities and problem drug use (SDF, 2007).

§ One way of unpicking this association is to focus on the socio -economic and political process that facilitate their disproportionate experience of drug-related harms among marginalised communities. § My research looks beyond the drug and individual drug users’ behaviour to the risk environment - the ‘physical, social, economic & policy contexts’ Rhodes (2002) – they inhabit

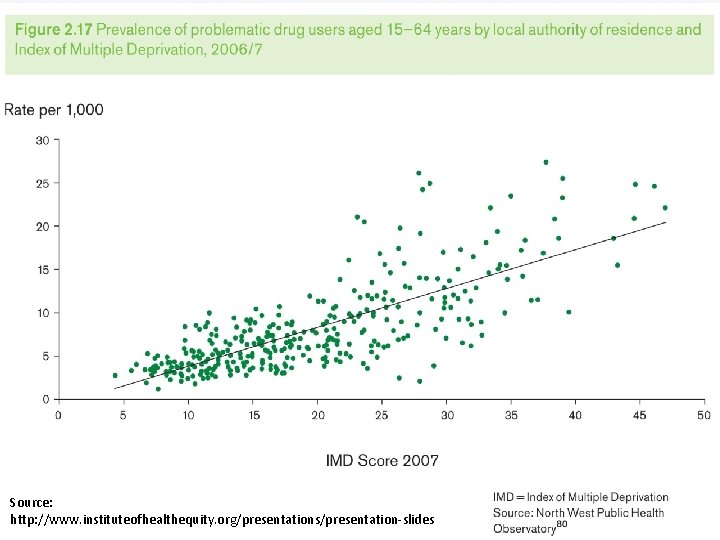
Source: http: //www. instituteofhealthequity. org/presentations/presentation-slides
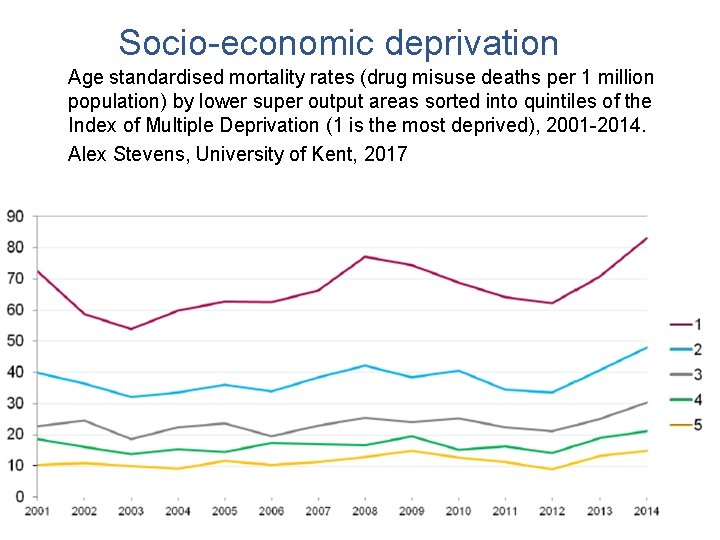
Socio-economic deprivation Age standardised mortality rates (drug misuse deaths per 1 million population) by lower super output areas sorted into quintiles of the Index of Multiple Deprivation (1 is the most deprived), 2001 -2014. Alex Stevens, University of Kent, 2017

§ Policy-related harms or ‘policy induced losses’: - the negative outcomes for people resulting from decisions taken, or not, by national and local government and statutory agencies. § A form of ‘structural violence’ by the state: - ‘the avoidable impairment of fundamental human needs’. (Galtung) § Intended or unintended consequences of policy or the outcomes of a politics of indifference?

What can ‘Health Inequalities’ teach us? § ‘Inequalities in health arise because of inequalities in society – in the conditions in which people are born, grow, live, work and age’ (Marmot, 2010). § an uneven distribution of risk factors … with the burden borne disproportionately by those in the lower socio-economic groups § The causes of health inequality are complex but they do not arise by chance. § The social determinants of health are largely the results of public policy.
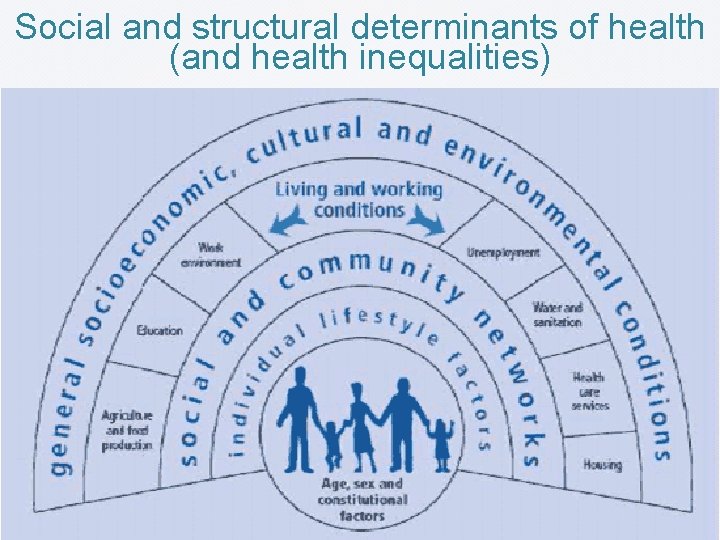
Social and structural determinants of health (and health inequalities)

§ General acceptance that inequalities in health arise out of inequalities in society which arise, largely, from public policy (Marmot, 2010) § Yet, little attention is paid to the role politics and policies play in shaping the macrosocial determinants of health and urban environments that produce and reproduce ill health and drug-related harms – the risk environment

Neo-liberal politics of austerity § Restructuring of the welfare state – cuts to education, housing, drug services, support services for marginalised comunities. § Increased welfare conditionality - ‘non-compliance’ = cessation of benefit § Change in disability supports – reassessment, regular reviews § Removal/reduction of welfare benefits to young people.

§ increasingly hostile drug policy environment § dominant public and political discourses individualise social and drug problems § framed as a ‘function of individual and cultural pathology’ and of ‘pharmacologically disordered citizens’. (Fraser & Moore, 2011) § focus on deficit model (Monaghan & Wincup, 2013) requires individual behavioural change § rather than policy deficits

Impact § In Scotland Ireland (where my research is based) we find concentrated areas of intense deprivation where inequalities in health, employment, education and access to services persist. § Individuals from deprived communities are more likely to experience morbidity and mortality from drug use. § For example, in Scotland, in the most deprived quintile drugrelated hospital admissions 14 times higher in the most deprived communities.

Number of drug-related general acute hospital stays in Scotland in 2015/6 by deprivation quintile.
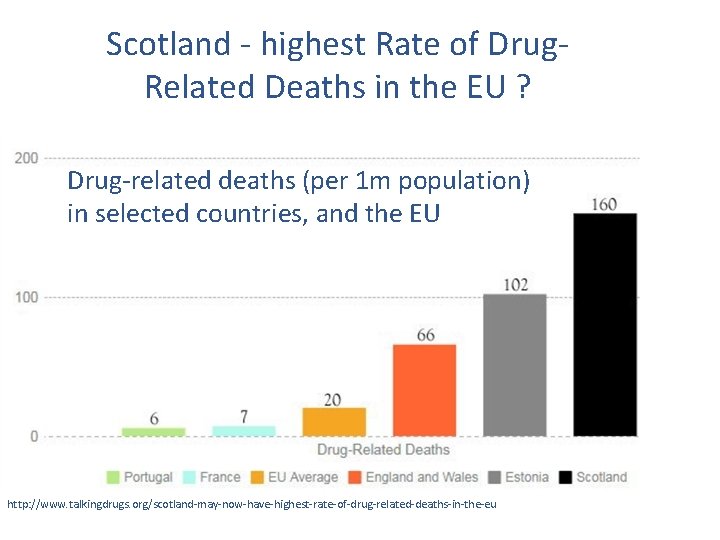
Scotland - highest Rate of Drug. Related Deaths in the EU ? Drug-related deaths (per 1 m population) in selected countries, and the EU http: //www. talkingdrugs. org/scotland-may-now-have-highest-rate-of-drug-related-deaths-in-the-eu

Scotland context of DRDs § Parkinson et al. (2016) identified now aging cohort at risk from the most deprived areas and who came to age in 1990 s exposed to the negative consequences of the changing social, economic and political contexts of the 1980 s (Thatherism and neo-liberalism) § recent exposure to a more ‘flexible’ labour market and greater conditionality and sanctions in the social security system increases the risk of DRDs

How do we move forward? § Responding to ‘problem’ drug use requires responding to the drivers of risk environments and the social and structural determinants of drug-related harms. § Consider the differential experience of drug-related harms with a focus on social justice and SDGs to address the disproportionate extent of drug-related harms experienced by those on the margins.
- Slides: 19