Leveraging Health Information Technology to Improve Care Early









- Slides: 25

Leveraging Health Information Technology to Improve Care: Early Lessons from the ONC HITECH Programs Mat Kendall, MPH Director, Office of Provider Adoption Support (OPAS) Office of the National Coordinator for Health IT U. S. Department of Health & Human Services

Presentation Learning Objectives: • Overview of the Health Information Technology for Economic and Clinical Health Act (HITECH) • How ONC is Supporting Providers to Achieve Meaningful Use of Health IT • Who is Working To Achieve Meaningful Use and What Challenges They Are Facing • How Meaning Use of Health IT is Supporting Providers to Improve the Care They Deliver to Their Patients 10/26/2021 Office of the National Coordinator for Health Information Technology 1

HITECH: Catalyst for Transformation Ultimate Goals : Better Healthcare Paper Records Pre 2009 A system plagued by inefficiencies 10/26/2021 Better Health Reduced Costs HITECH Act Electronic Health Records 2009 EHR Incentive Program and 62 Regional Extension Centers 2014 Widespread adoption & meaningful use of EHRs Office of the National Coordinator for Health Information Technology 2

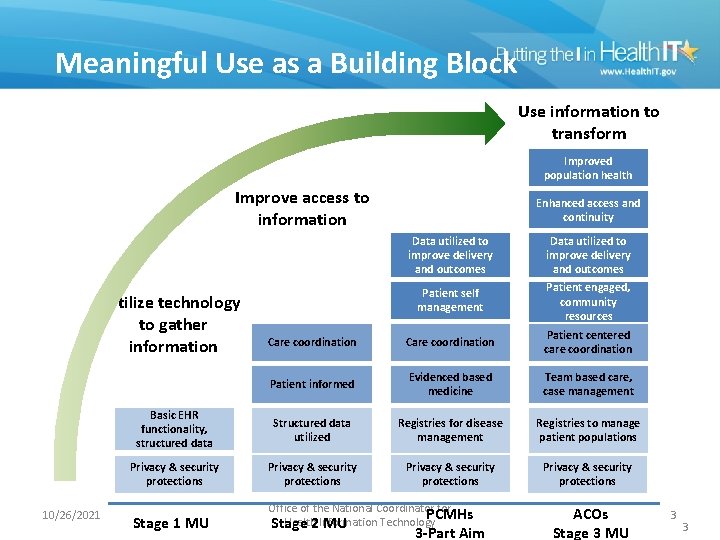
Meaningful Use as a Building Block Use information to transform Improved population health Improve access to information Data utilized to improve delivery and outcomes Patient self management Patient engaged, community resources Care coordination Patient centered care coordination Patient informed Evidenced based medicine Team based care, case management Basic EHR functionality, structured data Structured data utilized Registries for disease management Registries to manage patient populations Privacy & security protections Stage 1 MU Office of the National Coordinator for PCMHs Health 2 Information Technology Stage MU Utilize technology to gather information 10/26/2021 Enhanced access and continuity 3 -Part Aim ACOs Stage 3 MU 3 3

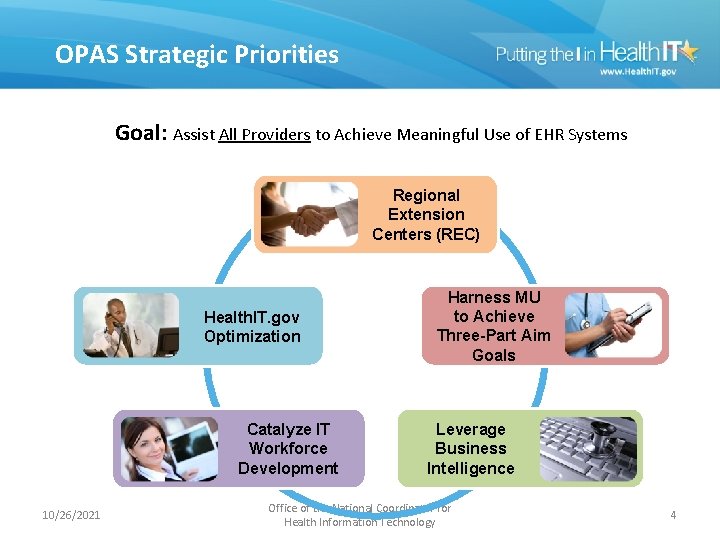
OPAS Strategic Priorities Goal: Assist All Providers to Achieve Meaningful Use of EHR Systems Regional Extension Centers (REC) Health. IT. gov Provider Adoption Optimization Services Catalyze IT Workforce Development 10/26/2021 Harness MU to Achieve Three-Part Aim Goals Leverage Business Intelligence Office of the National Coordinator for Health Information Technology 4

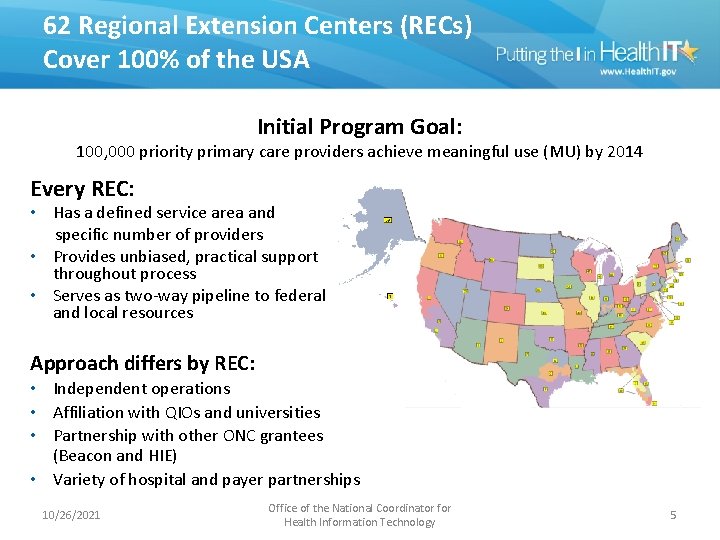
62 Regional Extension Centers (RECs) Cover 100% of the USA Initial Program Goal: 100, 000 priority primary care providers achieve meaningful use (MU) by 2014 Every REC: • Has a defined service area and specific number of providers • Provides unbiased, practical support throughout process • Serves as two-way pipeline to federal and local resources Approach differs by REC: • Independent operations • Affiliation with QIOs and universities • Partnership with other ONC grantees (Beacon and HIE) • Variety of hospital and payer partnerships 10/26/2021 Office of the National Coordinator for Health Information Technology 5

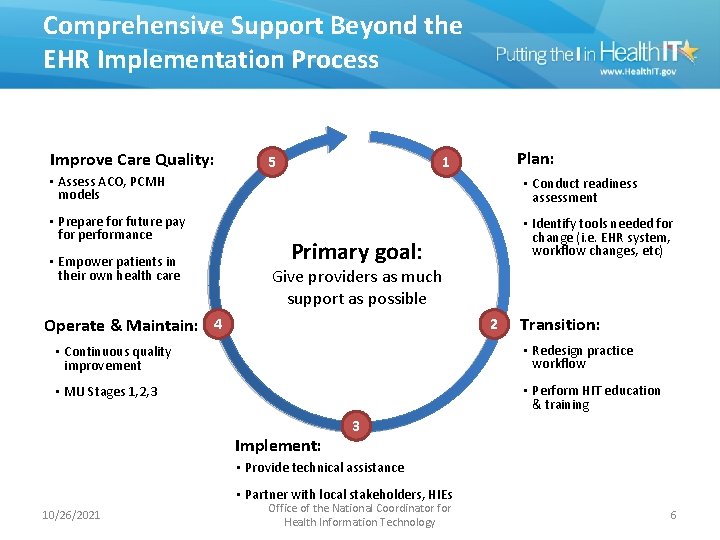
Comprehensive Support Beyond the EHR Implementation Process Improve Care Quality: 5 Plan: 1 • Assess ACO, PCMH models • Conduct readiness assessment • Prepare for future pay for performance • Identify tools needed for change (i. e. EHR system, workflow changes, etc) • Empower patients in their own health care Primary goal: Give providers as much support as possible Operate & Maintain: 4 2 Transition: • Continuous quality improvement • Redesign practice workflow • MU Stages 1, 2, 3 • Perform HIT education & training Implement: 3 • Provide technical assistance • Partner with local stakeholders, HIEs 10/26/2021 Office of the National Coordinator for Health Information Technology 6

Health IT Dashboard for the Medicare and Medicaid Electronic Health Record Incentive Programs http: //dashboard. healthit. gov/meaningfuluse • • Map & Dashboard Created by: Program Administered & Data Provided by: U. S. Department of Health and Human Services Office of the National Coordinator for Health Information Technology Centers for Medicare & Medicaid Services Office of Economic Analysis, Evaluation, and Modeling http: //dashboard. healthit. gov/meaningfuluse http: //dashboard. healthit. gov/ Email: ONCRequest@HHS. GOV 10/26/2021 Office of E-Health Standards and Services http: //dashboard. healthit. gov/meaningfuluse http: //www. cms. gov/Regulations-and-Guidance/Legislation/EHRIncentive. Programs Office of the National Coordinator for Health Information Technology 7

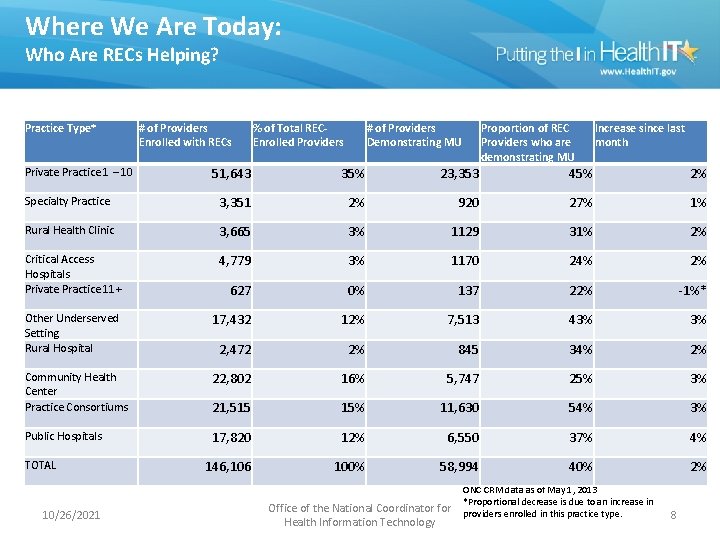
Where We Are Today: Who Are RECs Helping? Practice Type* # of Providers Enrolled with RECs % of Total RECEnrolled Providers # of Providers Demonstrating MU Proportion of REC Increase since last Providers who are month 131, 000 Priority Primary Care demonstrating MU 51, 643 35% Specialty Practice 3, 351 2% Rural Health Clinic 3, 665 3% Critical Access Hospitals Private Practice 11+ 4, 779 Private Practice 1 – 10 > 23, 353 Providers (PPCPs)45% are enrolled with 920 RECs 27% > 10, 000 specialists also enrolled 2% 1% 1129 31% 2% 3% 1170 24% 2% 627 0% 137 22% -1%* Other Underserved Setting Rural Hospital 17, 432 12% 7, 513 43% 3% 2, 472 2% 845 34% 2% Community Health Center Practice Consortiums 22, 802 16% 5, 747 25% 3% 21, 515 15% 11, 630 54% 3% Public Hospitals 17, 820 12% 6, 550 37% 4% 146, 106 100% 58, 994 40% 2% TOTAL 10/26/2021 Office of the National Coordinator for Health Information Technology ONC CRM data as of May 1, 2013 *Proportional decrease is due to an increase in providers enrolled in this practice type. 8

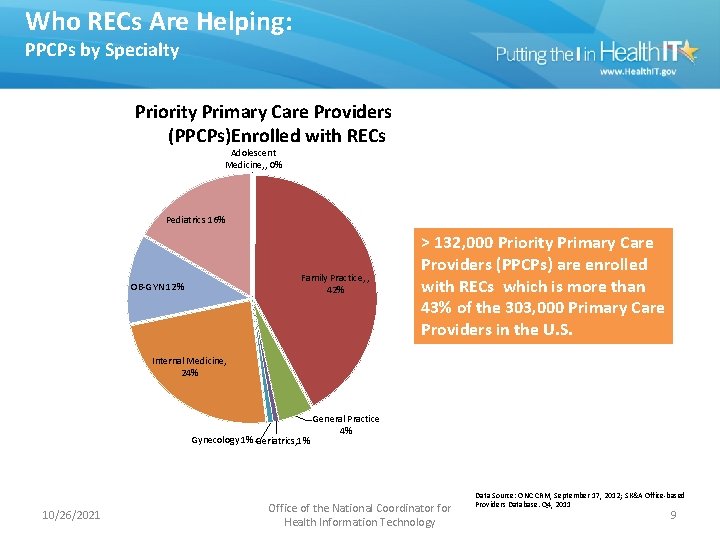
Who RECs Are Helping: PPCPs by Specialty Priority Primary Care Providers (PPCPs)Enrolled with RECs Adolescent Medicine, , 0% Pediatrics 16% Family Practice, , 42% OB-GYN 12% > 132, 000 Priority Primary Care Providers (PPCPs) are enrolled with RECs which is more than 43% of the 303, 000 Primary Care Providers in the U. S. Internal Medicine, 24% Gynecology 1% Geriatrics, 1% 10/26/2021 General Practice 4% Office of the National Coordinator for Health Information Technology Data Source: ONC CRM, September 17, 2012; SK&A Office-based Providers Database. Q 4, 2011 9

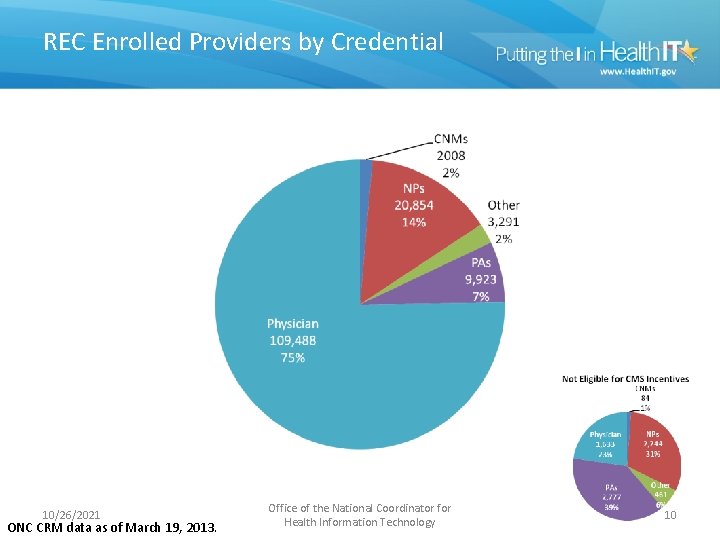
REC Enrolled Providers by Credential 10/26/2021 ONC CRM data as of March 19, 2013. Office of the National Coordinator for Health Information Technology 10

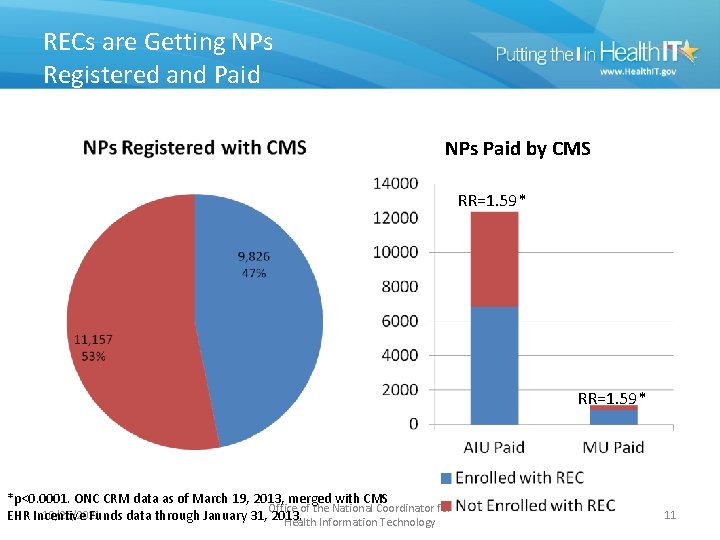
RECs are Getting NPs Registered and Paid NPs Paid by CMS RR=1. 59* *p<0. 0001. ONC CRM data as of March 19, 2013, merged with CMS Office of the National Coordinator for 10/26/2021 EHR Incentive Funds data through January 31, 2013. Health Information Technology 11

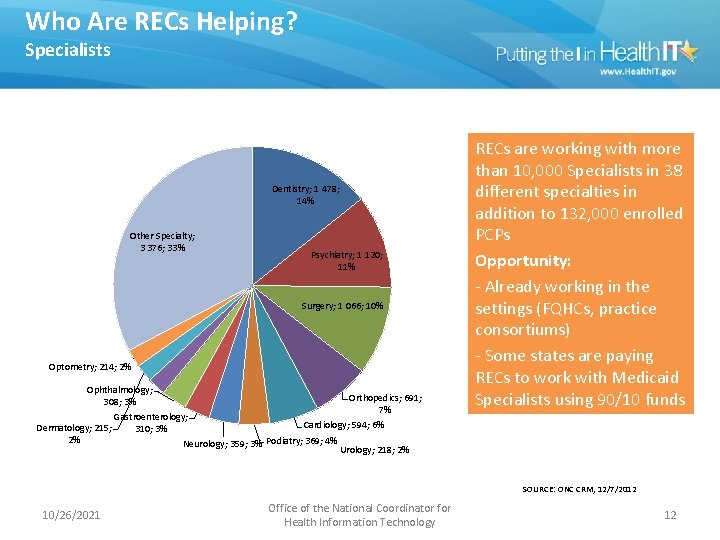
Who Are RECs Helping? Specialists Dentistry; 1 478; 14% Other Specialty; 3 376; 33% Psychiatry; 1 120; 11% Surgery; 1 066; 10% Optometry; 214; 2% Ophthalmology; Orthopedics; 691; 308; 3% 7% Gastroenterology; Cardiology; 594; 6% Dermatology; 215; 310; 3% 2% Podiatry; 369; 4% Neurology; 359; 3% Urology; 218; 2% RECs are working with more than 10, 000 Specialists in 38 different specialties in addition to 132, 000 enrolled PCPs Opportunity: - Already working in the settings (FQHCs, practice consortiums) - Some states are paying RECs to work with Medicaid Specialists using 90/10 funds SOURCE: ONC CRM, 12/7/2012 10/26/2021 Office of the National Coordinator for Health Information Technology 12

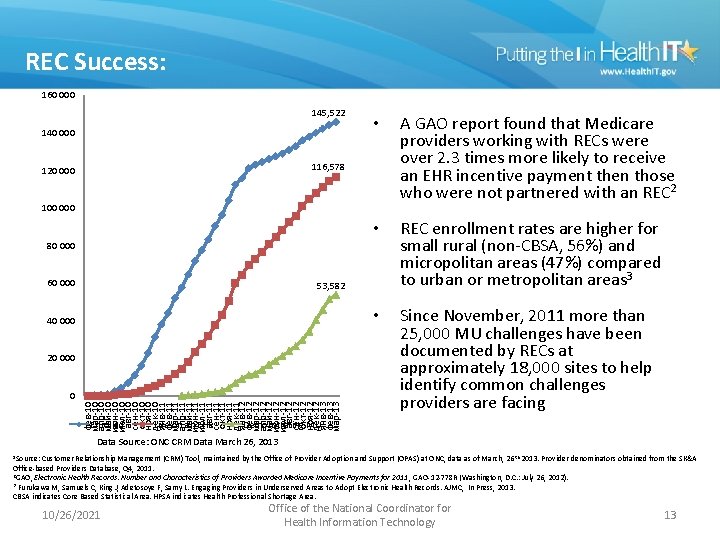
REC Success: 160 000 145, 522 140 000 • A GAO report found that Medicare providers working with RECs were over 2. 3 times more likely to receive an EHR incentive payment then those who were not partnered with an REC 2 • REC enrollment rates are higher for small rural (non-CBSA, 56%) and micropolitan areas (47%) compared to urban or metropolitan areas 3 • Since November, 2011 more than 25, 000 MU challenges have been documented by RECs at approximately 18, 000 sites to help identify common challenges providers are facing 116, 578 120 000 100 000 80 000 60 000 53, 582 40 000 20 000 фев-10 мар-10 апр-10 май-10 июн-10 июл-10 авг-10 сен-10 окт-10 ноя-10 дек-10 янв-11 фев-11 мар-11 апр-11 май-11 июн-11 июл-11 авг-11 сен-11 окт-11 ноя-11 дек-11 янв-12 фев-12 мар-12 апр-12 май-12 июн-12 июл-12 авг-12 сен-12 окт-12 ноя-12 дек-12 янв-13 фев-13 мар-13 0 Enrolled Live on an EHR Demonstrating MU Data Source: ONC CRM Data March 26, 2013 1 Source: Customer Relationship Management (CRM) Tool, maintained by the Office of Provider Adoption and Support (OPAS) at ONC, data as of March, 26 th 2013. Provider denominators obtained from the SK&A Office-based Providers Database, Q 4, 2011. 2 GAO, Electronic Health Records: Number and Characteristics of Providers Awarded Medicare Incentive Payments for 2011 , GAO-12 -778 R (Washington, D. C. : July 26, 2012). 3 Furukawa M, Samuels C, King J, Adetosoye F, Samy L. Engaging Providers in Underserved Areas to Adopt Electronic Health Records. AJMC, In Press, 2013. CBSA indicates Core Based Statistical Area. HPSA indicates Health Professional Shortage Area. 10/26/2021 Office of the National Coordinator for Health Information Technology 13

REC are also collecting specific practices level data on challenges that providers are experiencing Primary and Secondary Challenges Categories Being Tracked by RECs Practice Issues Vendor Issues Workflow adoption Upgrade Provider engagement Delays in implementation / installation Training Certification Reports slow / not available Vendor selection Administrative Financial Staffing Training / support materials inadequate/not available Lack of vendor support Technical Inaccurate reports and/or data Attestation Process Issues MU Measures Calculating patient volume Core CQMs Medicaid program not up yet Alternate Core CQMs Medicaid technical/ administrative Additional CQMs Medicare technical/ administrative Each of the Core / Menu Set measure Complete list of Challenges categories, tertiary Office of the including National Coordinator for categories and descriptions Health Information Technology of the categories, is available at healthit. gov/data. 10/26/2021 14

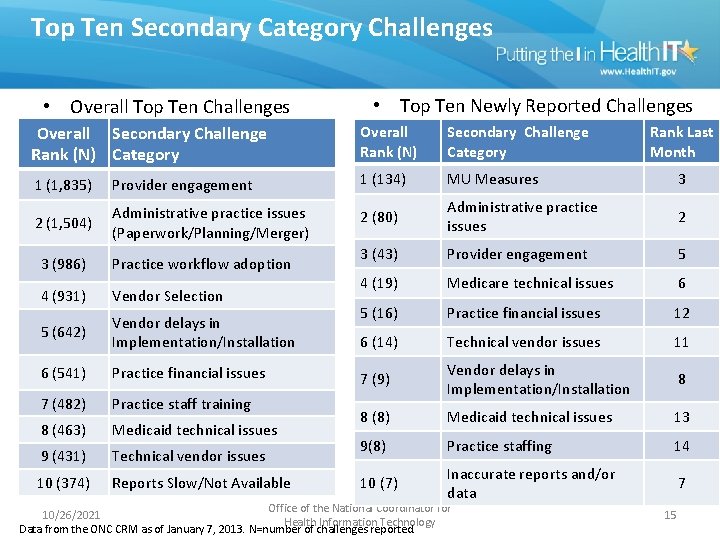
Top Ten Secondary Category Challenges • Overall Top Ten Challenges • Top Ten Newly Reported Challenges Overall Secondary Challenge Rank (N) Category Overall Rank (N) Secondary Challenge Category 1 (1, 835) Provider engagement 1 (134) MU Measures 3 2 (1, 504) Administrative practice issues (Paperwork/Planning/Merger) 2 (80) Administrative practice issues 2 3 (43) Provider engagement 5 4 (19) Medicare technical issues 6 5 (16) Practice financial issues 12 6 (14) Technical vendor issues 11 7 (9) Vendor delays in Implementation/Installation 8 8 (8) Medicaid technical issues 13 9(8) Practice staffing 14 10 (7) Inaccurate reports and/or data 7 3 (986) Practice workflow adoption 4 (931) Vendor Selection 5 (642) Vendor delays in Implementation/Installation 6 (541) Practice financial issues 7 (482) Practice staff training 8 (463) Medicaid technical issues 9 (431) Technical vendor issues 10 (374) Reports Slow/Not Available Office of the National Coordinator for 10/26/2021 Health Information Technology Data from the ONC CRM as of January 7, 2013. N=number of challenges reported. Rank Last Month 15

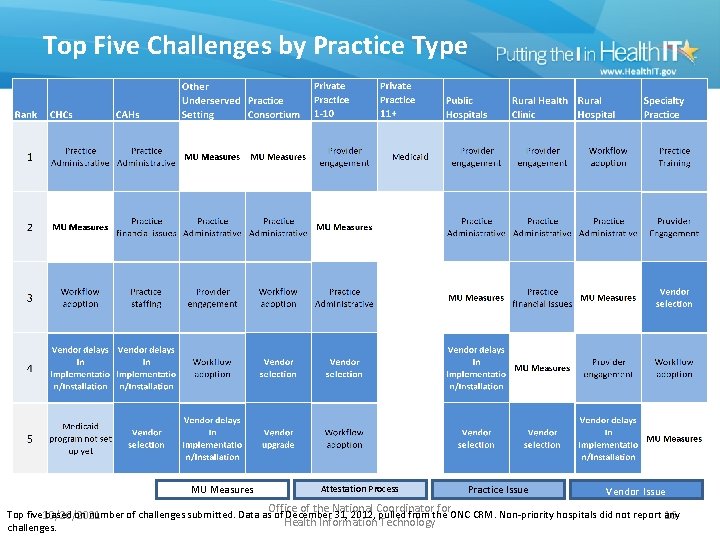
Top Five Challenges by Practice Type MU Measures Attestation Process Office of the National Coordinator for Practice Issue Vendor Issue Top five 10/26/2021 based on number of challenges submitted. Data as of December 31, 2012, pulled from the ONC CRM. Non-priority hospitals did not report any 16 Health Information Technology challenges.

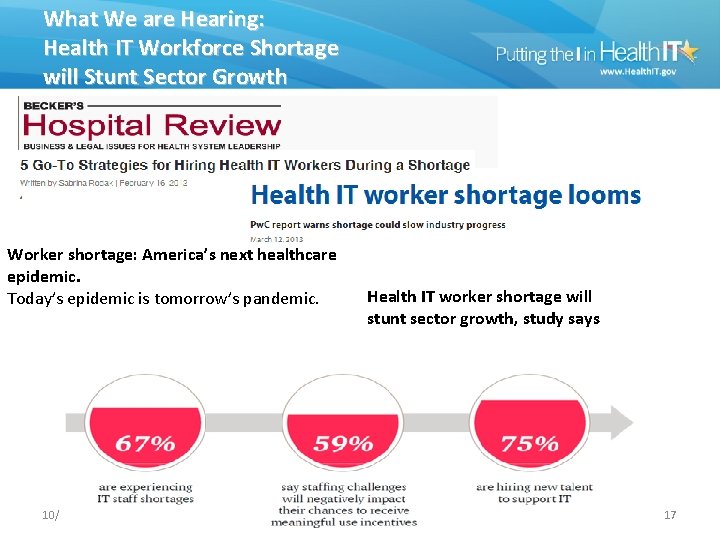
What We are Hearing: Health IT Workforce Shortage will Stunt Sector Growth Worker shortage: America’s next healthcare epidemic. Today’s epidemic is tomorrow’s pandemic. 10/26/2021 Health IT worker shortage will stunt sector growth, study says Office of the National Coordinator for Health Information Health ITTechnology 17

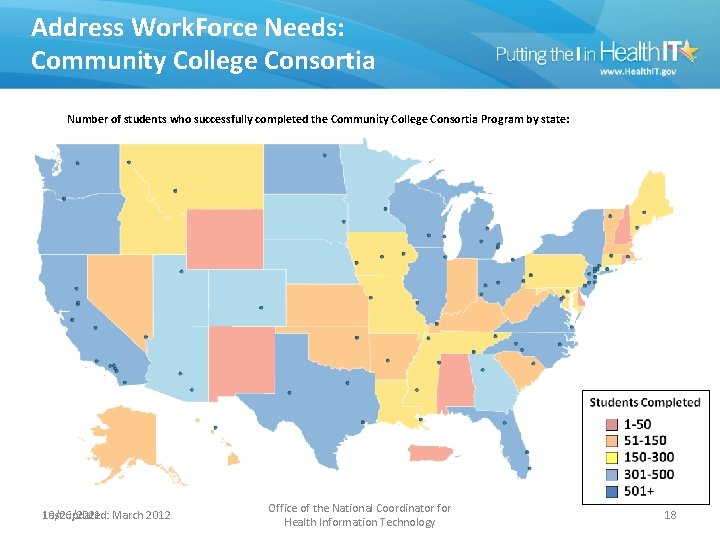
Address Work. Force Needs: Community College Consortia Number of students who successfully completed the Community College Consortia Program by state: 10/26/2021 Last updated: March 2012 Office of the National Coordinator for Health Information Technology 18

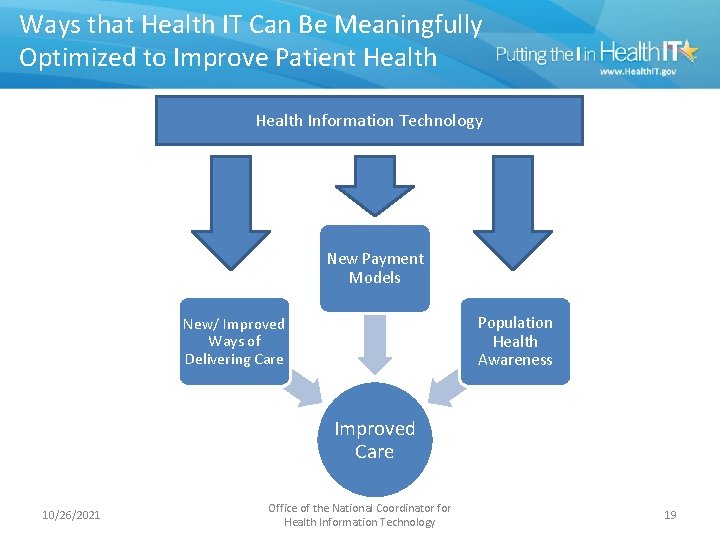
Ways that Health IT Can Be Meaningfully Optimized to Improve Patient Health Information Technology New Payment Models Population Health Awareness New/ Improved Ways of Delivering Care Improved Care 10/26/2021 Office of the National Coordinator for Health Information Technology 19

New/ Improved Ways of Delivering Care New Opportunity • New approaches to team based care • Open access scheduling • New/expanded roles for staff to assist with care coordination Medical Home Consumer Engagement • New ways of communicating/engaging patients (i. e. portals) • Teach patients about how they can be more active in their own care Health Information Exchange Privacy/Security 10/26/2021 New Needs: • Assistance with implementation and workflow redesign • Improved coordination/communication among external health care networks (specialist, nursing homes, etc. ) • Support for secure back up/recovery • Assistance in educating staff about how to protect data Office of the National Coordinator for Health Information Technology 20

New Payment Models New Opportunity New Needs: Shared Savings Programs • Cost/quality data analytics and risk management • Continuous quality improvement efforts aimed at improving quality/cost measures Comprehensive Primary Care Initiative Pioneer ACO Bundle Payments 10/26/2021 • Care management for at risk patients • Increased access to preventive care • Implement patient portals • Develop new payment arrangements that best improve care and generate savings for Medicare • Test concepts on a large scale • New approaches to billing and delivering care in different settings (Acute care hospital, Skilled nursing, etc. ) Office of the National Coordinator for Health Information Technology 21

Population Health Awareness New Opportunity National Quality Strategy New Needs: • Ensure Health IT is used to address most pressing health care challenges • Continuous quality improvement Million Hearts • Team approach to care management of patients who are at risk for heart disease • Increased access to preventive care Public Health Support • Support for new coordination around Immunizations and other public health priorities • Education for patients on how to access immunization data 10/26/2021 Office of the National Coordinator for Health Information Technology 22

Training for an Evolving Health IT Landscape Sound educational models need to be developed for different stages of training • Professional schools to select, support and train PCMH ready clinicians • Team work/interdisciplinary training • Life-long learning of key skills for all health care workers (IOM Report) • New education models on-line • New efforts to collect and disseminate curricula • Office of the National Coordinator for Health IT 23

Stay Connected, Communicate and Collaborate • Questions? Browse the ONC website at: health. IT. gov click the Facebook “Like” button to add us to your network • Contact us at: onc. request@hhs. gov • Subscribe, watch and share: Ø @ONC_Health. IT Ø http: //www. youtube. com/user/HHSONC Ø Health. IT and Electronic Health Records Ø http: //www. scribd. com/Health. IT/ Ø http: //www. flickr. com/photos/healthit Health. IT. gov/buzz-blog