Lesson 15 The Digestive System 1 Chapter 24




- Slides: 22

Lesson # 15 The Digestive System 1 Chapter 24 Objectives: 1 - To explain the functions of the digestive system. 2 - To describe the structure of the parietal and visceral peritoneum. 3 - To describe the functional histology of the digestive tract. 4 - To explaining how food travels through the alimentary canal. 5 - To explain the mechanisms that control the digestive function.

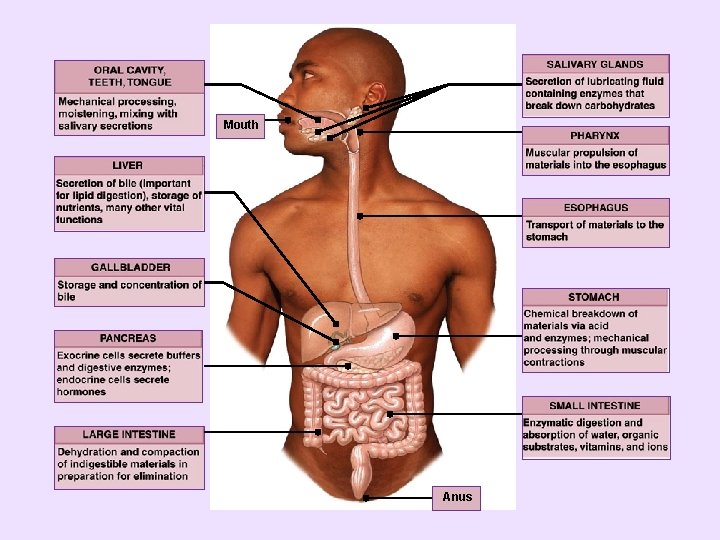
Functions of the Digestive System 1 - Ingestion: It occurs when materials enter the digestive tract via the mouth. 2 - Mechanical processing: It is the crushing and shearing that make materials easier to propel along the digestive tract. 3 - Digestion: It is the chemical breakdown of food into small organic fragments for absorption by the digestive epithelium. 4 - Secretion: It is the release of water, acids, enzymes, buffers, and salts epithelium of the digestive tract and by the glandular organs. by the 5 - Absorption: It is the movement of organic substrates, electrolytes, vitamins, and water across the digestive epithelium into interstitial fluid of the digestive tract. 6 - Excretion: It is the removal of waste products from the body fluids.

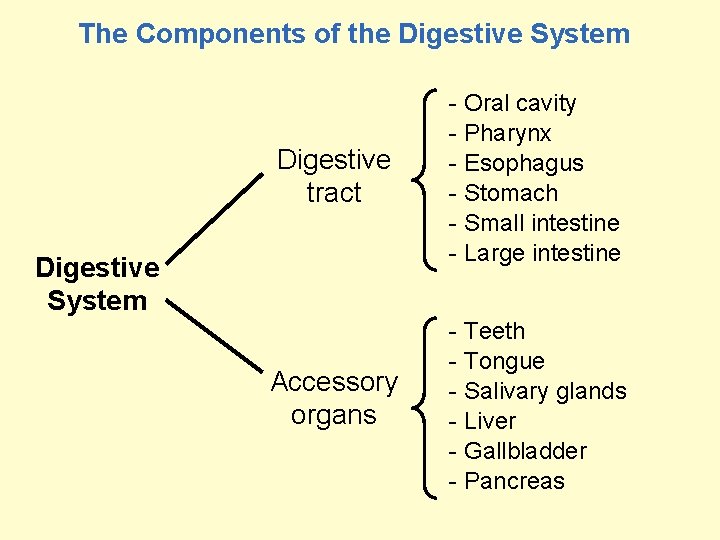
The Components of the Digestive System Digestive tract - Oral cavity - Pharynx - Esophagus - Stomach - Small intestine - Large intestine Accessory organs - Teeth - Tongue - Salivary glands - Liver - Gallbladder - Pancreas Digestive System

Mouth Anus

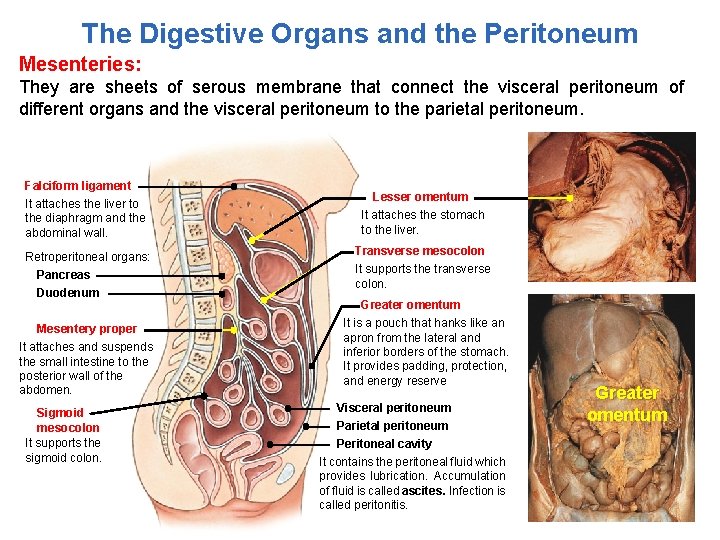
The Digestive Organs and the Peritoneum Mesenteries: They are sheets of serous membrane that connect the visceral peritoneum of different organs and the visceral peritoneum to the parietal peritoneum. Falciform ligament It attaches the liver to the diaphragm and the abdominal wall. Retroperitoneal organs: Pancreas Duodenum Mesentery proper It attaches and suspends the small intestine to the posterior wall of the abdomen. Sigmoid mesocolon It supports the sigmoid colon. Lesser omentum It attaches the stomach to the liver. Transverse mesocolon It supports the transverse colon. Greater omentum It is a pouch that hanks like an apron from the lateral and inferior borders of the stomach. It provides padding, protection, and energy reserve Visceral peritoneum Parietal peritoneum Peritoneal cavity It contains the peritoneal fluid which provides lubrication. Accumulation of fluid is called ascites. Infection is called peritonitis. Greater omentum

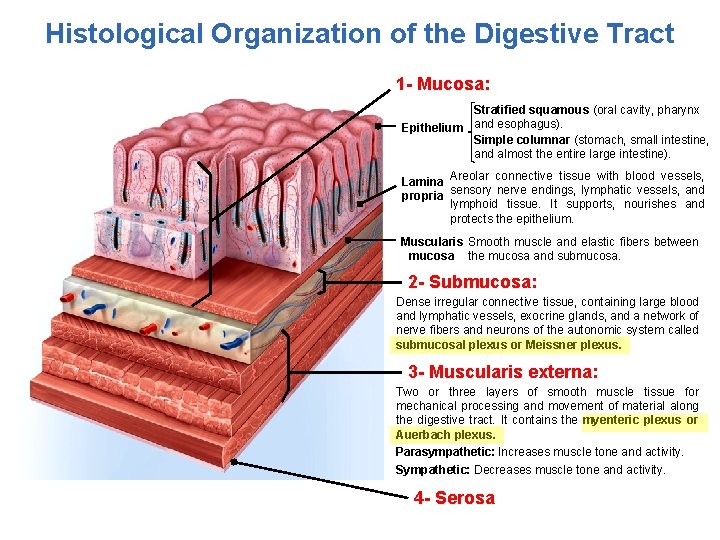
Histological Organization of the Digestive Tract 1 - Mucosa: Stratified squamous (oral cavity, pharynx Epithelium and esophagus). Simple columnar (stomach, small intestine, and almost the entire large intestine). Lamina Areolar connective tissue with blood vessels, propria sensory nerve endings, lymphatic vessels, and lymphoid tissue. It supports, nourishes and protects the epithelium. Muscularis Smooth muscle and elastic fibers between mucosa the mucosa and submucosa. 2 - Submucosa: Dense irregular connective tissue, containing large blood and lymphatic vessels, exocrine glands, and a network of nerve fibers and neurons of the autonomic system called submucosal plexus or Meissner plexus. 3 - Muscularis externa: Two or three layers of smooth muscle tissue for mechanical processing and movement of material along the digestive tract. It contains the myenteric plexus or Auerbach plexus. Parasympathetic: Increases muscle tone and activity. Sympathetic: Decreases muscle tone and activity. 4 - Serosa

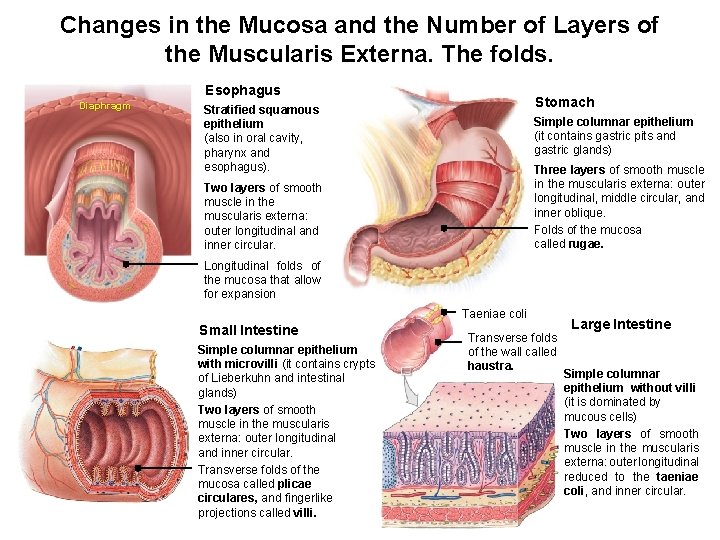
Changes in the Mucosa and the Number of Layers of the Muscularis Externa. The folds. Esophagus Diaphragm Stomach Stratified squamous epithelium (also in oral cavity, pharynx and esophagus). Simple columnar epithelium (it contains gastric pits and gastric glands) Three layers of smooth muscle in the muscularis externa: outer longitudinal, middle circular, and inner oblique. Folds of the mucosa called rugae. Two layers of smooth muscle in the muscularis externa: outer longitudinal and inner circular. Longitudinal folds of the mucosa that allow for expansion Taeniae coli Small Intestine Simple columnar epithelium with microvilli (it contains crypts of Lieberkuhn and intestinal glands) Two layers of smooth muscle in the muscularis externa: outer longitudinal and inner circular. Transverse folds of the mucosa called plicae circulares, and fingerlike projections called villi. Transverse folds of the wall called haustra. Large Intestine Simple columnar epithelium without villi (it is dominated by mucous cells) Two layers of smooth muscle in the muscularis externa: outer longitudinal reduced to the taeniae coli, and inner circular.

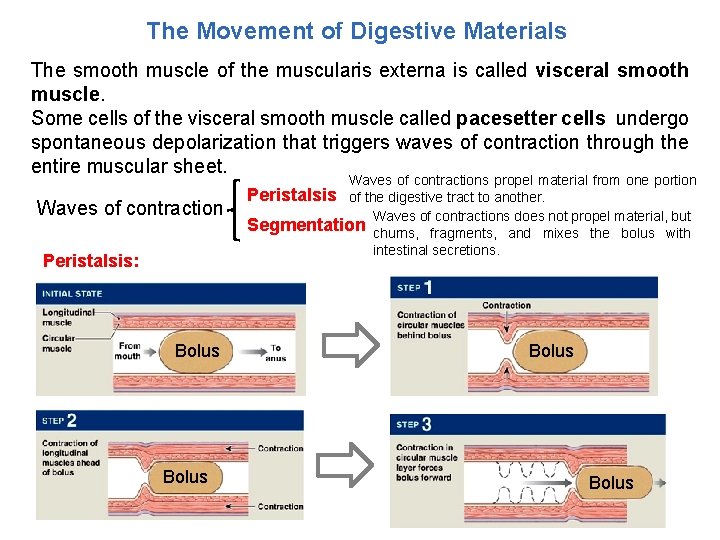
The Movement of Digestive Materials The smooth muscle of the muscularis externa is called visceral smooth muscle. Some cells of the visceral smooth muscle called pacesetter cells undergo spontaneous depolarization that triggers waves of contraction through the entire muscular sheet. Waves of contraction Peristalsis: Bolus Waves of contractions propel material from one portion Peristalsis of the digestive tract to another. Waves of contractions does not propel material, but Segmentation churns, fragments, and mixes the bolus with intestinal secretions. Bolus

Control of Digestive Functions 1 - Local Factors 2 - Neural Mechanisms a- Short reflexes b- Long reflexes 3 - Hormonal Mechanisms 1 - Local Factors Prostaglandins, histamine, and other chemicals released into interstitial fluid, may affect adjacent cells within small segment of digestive tract, coordinating response to changing conditions (variations in local p. H, chemical, or physical stimuli). Local factors affect only a portion of tract.

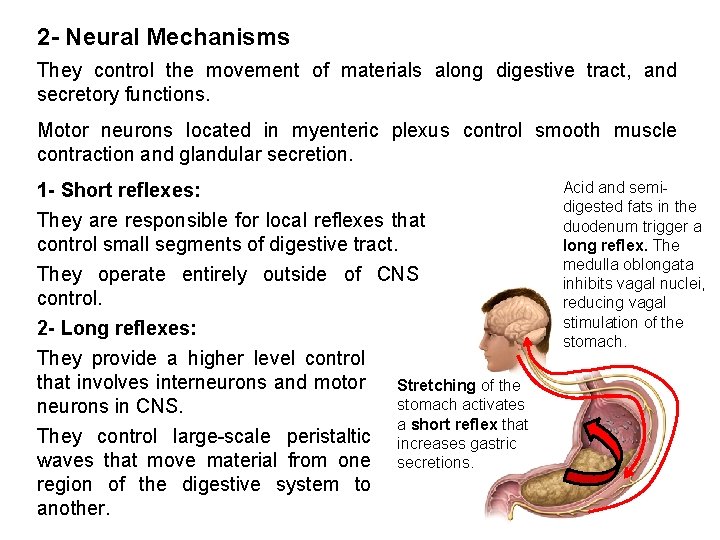
2 - Neural Mechanisms They control the movement of materials along digestive tract, and secretory functions. Motor neurons located in myenteric plexus control smooth muscle contraction and glandular secretion. 1 - Short reflexes: They are responsible for local reflexes that control small segments of digestive tract. They operate entirely outside of CNS control. 2 - Long reflexes: They provide a higher level control that involves interneurons and motor Stretching of the stomach activates neurons in CNS. a short reflex that They control large-scale peristaltic increases gastric waves that move material from one secretions. region of the digestive system to another. Acid and semidigested fats in the duodenum trigger a long reflex. The medulla oblongata inhibits vagal nuclei, reducing vagal stimulation of the stomach.

3 - Hormonal Mechanisms At least 18 peptide hormones affect most aspects of digestive function and some of them also affect activities of other systems. The hormones gastrin, secretin, and enteroendocrine cells in the digestive tract. other; are produced by They reach target organs after distribution in bloodstream. Ex: Chyme also stimulates duodenal enteroendocrine cells to release secretin and cholecystokinin (CCK) that suppress gastric secretion and motility.

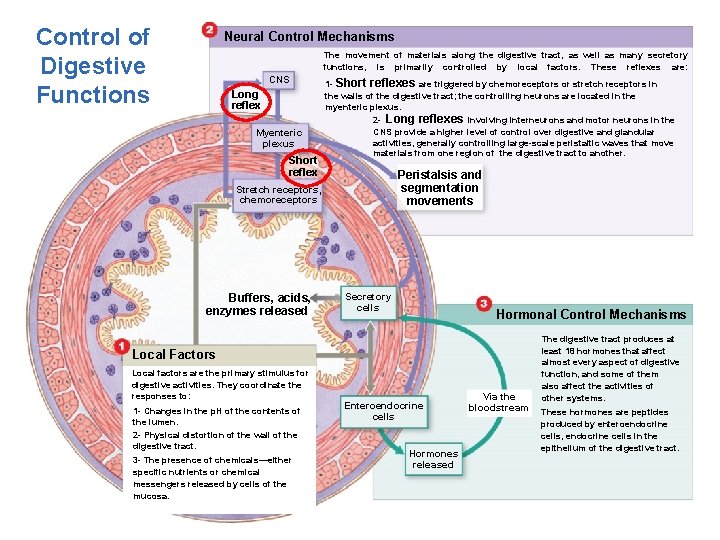
Control of Digestive Functions Neural Control Mechanisms The movement of materials along the digestive tract, as well as many secretory functions, is primarily controlled by local factors. These reflexes are: CNS Long reflex Myenteric plexus Short reflex 1 - Short reflexes are triggered by chemoreceptors or stretch receptors in the walls of the digestive tract; the controlling neurons are located in the myenteric plexus. 2 - Long reflexes involving interneurons and motor neurons in the CNS provide a higher level of control over digestive and glandular activities, generally controlling large-scale peristaltic waves that move materials from one region of the digestive tract to another. Peristalsis and segmentation movements Stretch receptors, chemoreceptors Buffers, acids, enzymes released Secretory cells Hormonal Control Mechanisms Local Factors Local factors are the primary stimulus for digestive activities. They coordinate the responses to: 1 - Changes in the p. H of the contents of the lumen. 2 - Physical distortion of the wall of the digestive tract. 3 - The presence of chemicals—either specific nutrients or chemical messengers released by cells of the mucosa. Enteroendocrine cells Hormones released Via the bloodstream The digestive tract produces at least 18 hormones that affect almost every aspect of digestive function, and some of them also affect the activities of other systems. These hormones are peptides produced by enteroendocrine cells, endocrine cells in the epithelium of the digestive tract.

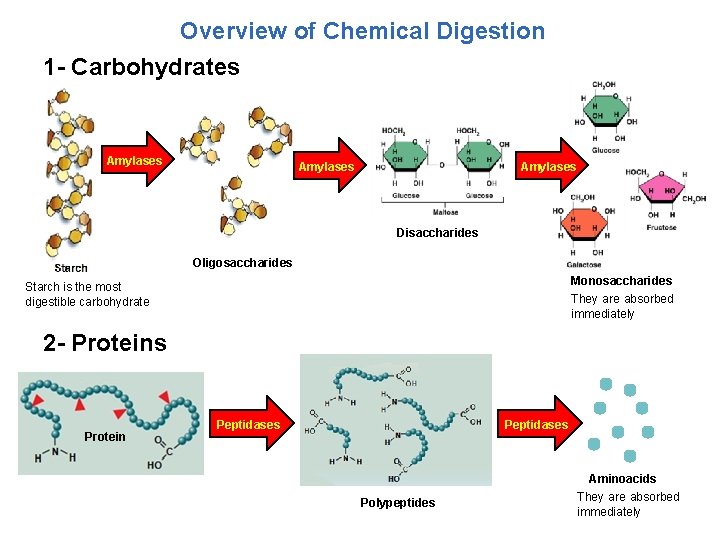
Overview of Chemical Digestion 1 - Carbohydrates Amylases Disaccharides Oligosaccharides Monosaccharides They are absorbed immediately Starch is the most digestible carbohydrate 2 - Proteins Protein Peptidases Polypeptides Aminoacids They are absorbed immediately

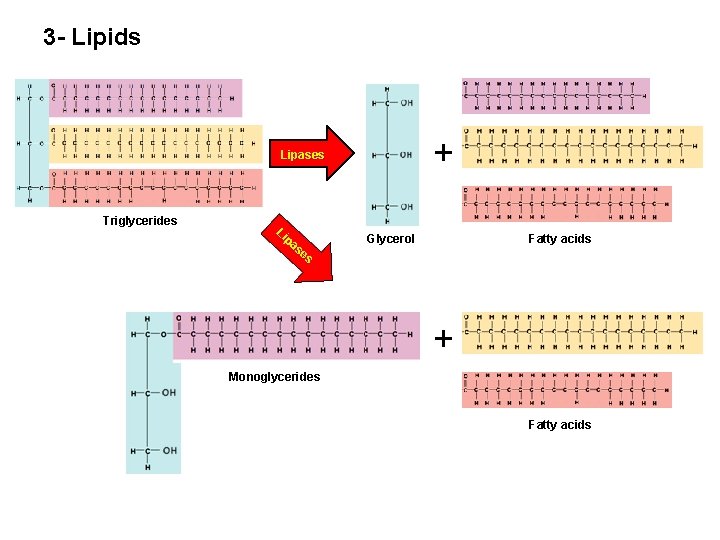
3 - Lipids + Lipases Triglycerides Li pa se s Glycerol Fatty acids + Monoglycerides Fatty acids

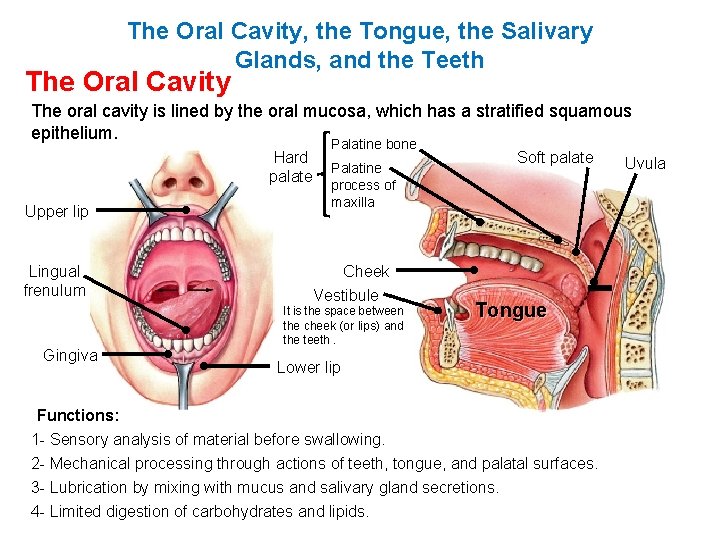
The Oral Cavity, the Tongue, the Salivary Glands, and the Teeth The Oral Cavity The oral cavity is lined by the oral mucosa, which has a stratified squamous epithelium. Hard palate Upper lip Lingual frenulum Palatine bone Palatine process of maxilla Cheek Vestibule It is the space between the cheek (or lips) and the teeth. Gingiva Soft palate Tongue Lower lip Functions: 1 - Sensory analysis of material before swallowing. 2 - Mechanical processing through actions of teeth, tongue, and palatal surfaces. 3 - Lubrication by mixing with mucus and salivary gland secretions. 4 - Limited digestion of carbohydrates and lipids. Uvula

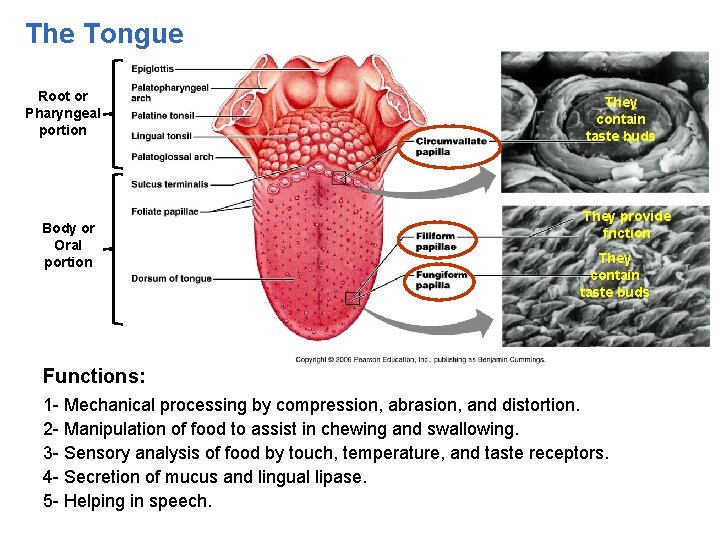
The Tongue Root or Pharyngeal portion Body or Oral portion They contain taste buds They provide friction They contain taste buds Functions: 1 - Mechanical processing by compression, abrasion, and distortion. 2 - Manipulation of food to assist in chewing and swallowing. 3 - Sensory analysis of food by touch, temperature, and taste receptors. 4 - Secretion of mucus and lingual lipase. 5 - Helping in speech.

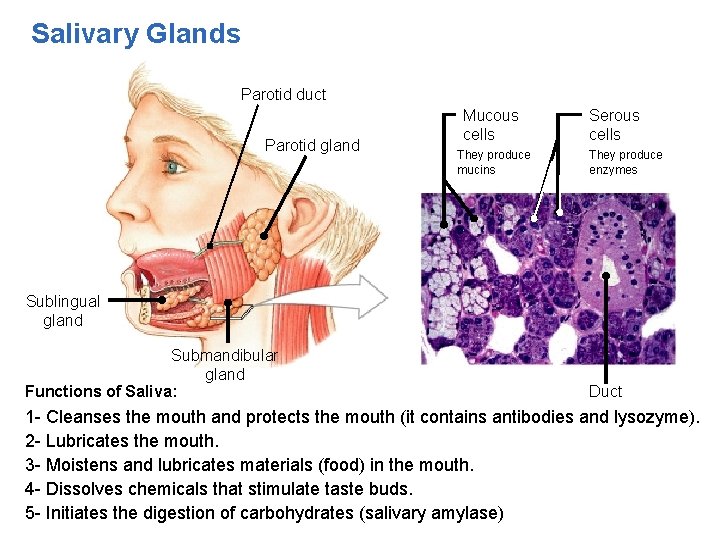
Salivary Glands Parotid duct Parotid gland Mucous cells They produce mucins Serous cells They produce enzymes Sublingual gland Submandibular gland Functions of Saliva: Duct 1 - Cleanses the mouth and protects the mouth (it contains antibodies and lysozyme). 2 - Lubricates the mouth. 3 - Moistens and lubricates materials (food) in the mouth. 4 - Dissolves chemicals that stimulate taste buds. 5 - Initiates the digestion of carbohydrates (salivary amylase)

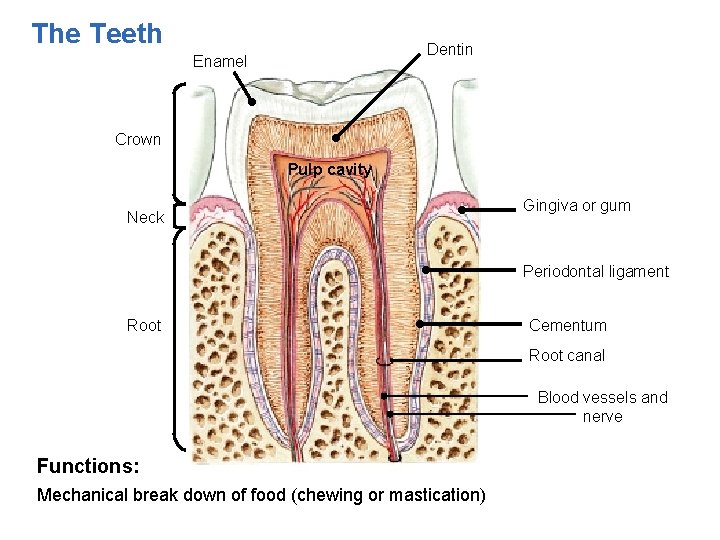
The Teeth Dentin Enamel Crown Pulp cavity Neck Gingiva or gum Periodontal ligament Root Cementum Root canal Blood vessels and nerve Functions: Mechanical break down of food (chewing or mastication)

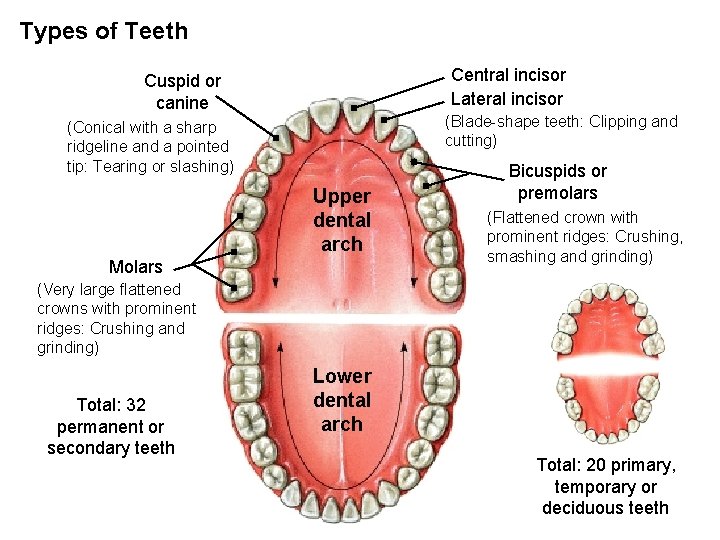
Types of Teeth Central incisor Lateral incisor Cuspid or canine (Blade-shape teeth: Clipping and cutting) (Conical with a sharp ridgeline and a pointed tip: Tearing or slashing) Upper dental arch Molars Bicuspids or premolars (Flattened crown with prominent ridges: Crushing, smashing and grinding) (Very large flattened crowns with prominent ridges: Crushing and grinding) Total: 32 permanent or secondary teeth Lower dental arch Total: 20 primary, temporary or deciduous teeth

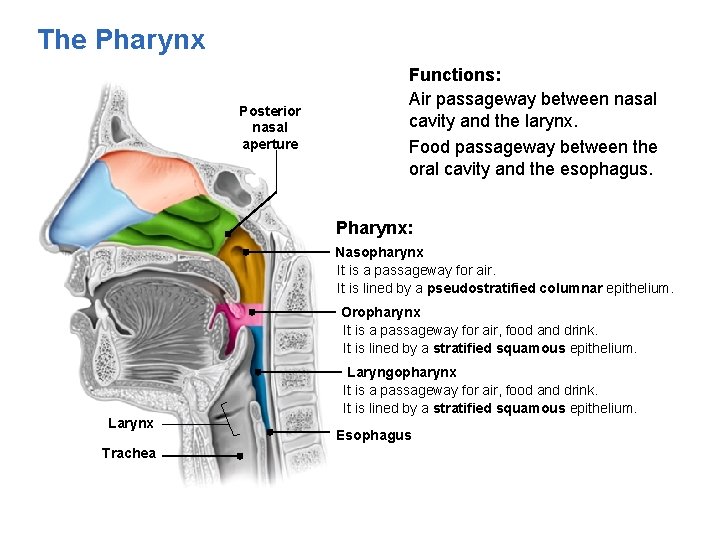
The Pharynx Posterior nasal aperture Functions: Air passageway between nasal cavity and the larynx. Food passageway between the oral cavity and the esophagus. Pharynx: Nasopharynx It is a passageway for air. It is lined by a pseudostratified columnar epithelium. Oropharynx It is a passageway for air, food and drink. It is lined by a stratified squamous epithelium. Larynx Trachea Laryngopharynx It is a passageway for air, food and drink. It is lined by a stratified squamous epithelium. Esophagus

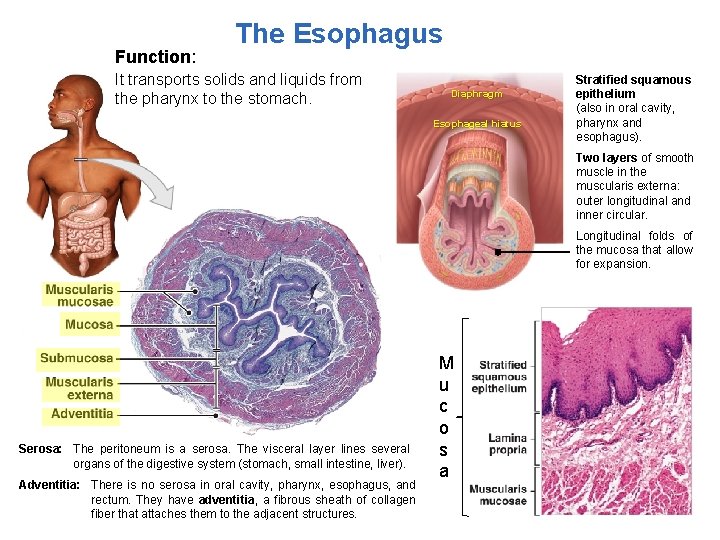
Function: The Esophagus It transports solids and liquids from the pharynx to the stomach. Diaphragm Esophageal hiatus Stratified squamous epithelium (also in oral cavity, pharynx and esophagus). Two layers of smooth muscle in the muscularis externa: outer longitudinal and inner circular. Longitudinal folds of the mucosa that allow for expansion. Serosa: The peritoneum is a serosa. The visceral layer lines several organs of the digestive system (stomach, small intestine, liver). Adventitia: There is no serosa in oral cavity, pharynx, esophagus, and rectum. They have adventitia, a fibrous sheath of collagen fiber that attaches them to the adjacent structures. M u c o s a

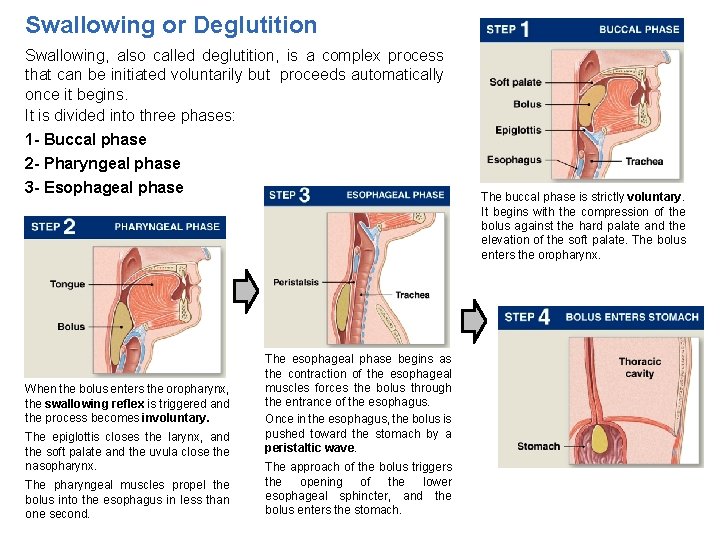
Swallowing or Deglutition Swallowing, also called deglutition, is a complex process that can be initiated voluntarily but proceeds automatically once it begins. It is divided into three phases: 1 - Buccal phase 2 - Pharyngeal phase 3 - Esophageal phase When the bolus enters the oropharynx, the swallowing reflex is triggered and the process becomes involuntary. The epiglottis closes the larynx, and the soft palate and the uvula close the nasopharynx. The pharyngeal muscles propel the bolus into the esophagus in less than one second. The buccal phase is strictly voluntary. It begins with the compression of the bolus against the hard palate and the elevation of the soft palate. The bolus enters the oropharynx. The esophageal phase begins as the contraction of the esophageal muscles forces the bolus through the entrance of the esophagus. Once in the esophagus, the bolus is pushed toward the stomach by a peristaltic wave. The approach of the bolus triggers the opening of the lower esophageal sphincter, and the bolus enters the stomach.