Lecture DIGESTIVE SYSTEM INTESTINE LIVER PANCREAS Department of






- Slides: 45

Lecture DIGESTIVE SYSTEM INTESTINE LIVER PANCREAS Department of histology, cytology and embryology Kh. NMU part 2

Small intestine • Functions: • digestion – liver, pancreas, enterocytes • absorption – enterocytes • STRUCTURE: 4 membranes

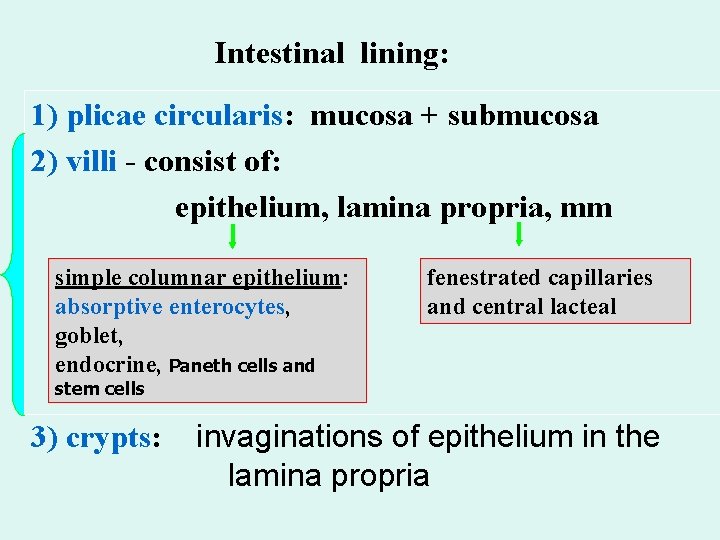
Intestinal lining: 1) plicae circularis: mucosa + submucosa 2) villi - consist of: epithelium, lamina propria, mm simple columnar epithelium: absorptive enterocytes, goblet, endocrine, Paneth cells and fenestrated capillaries and central lacteal stem cells 3) crypts: invaginations of epithelium in the lamina propria

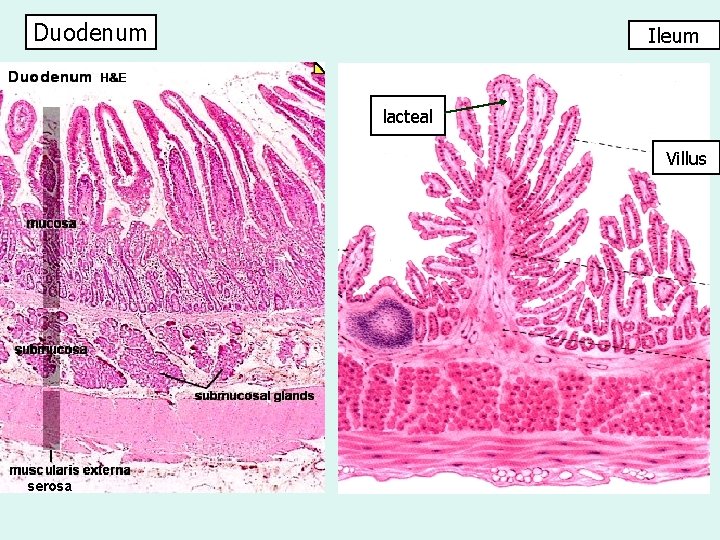
Duodenum Ileum lacteal Villus serosa

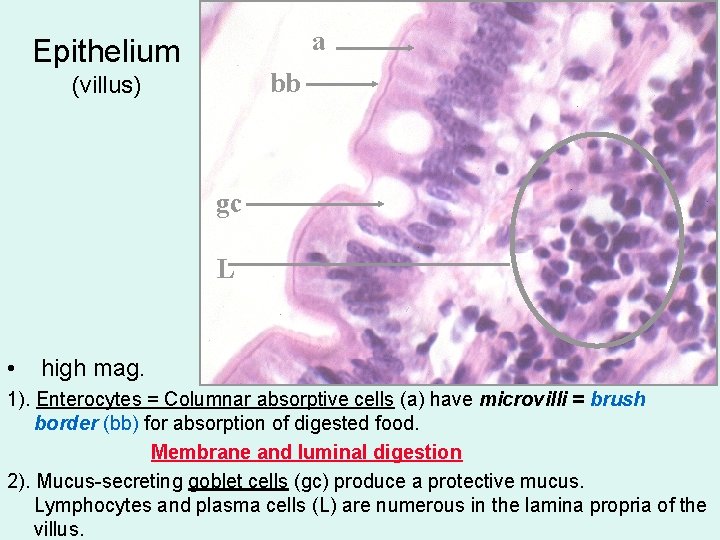
a Epithelium bb (villus) gc L • high mag. 1). Enterocytes = Columnar absorptive cells (a) have microvilli = brush border (bb) for absorption of digested food. Membrane and luminal digestion 2). Mucus-secreting goblet cells (gc) produce a protective mucus. Lymphocytes and plasma cells (L) are numerous in the lamina propria of the villus.

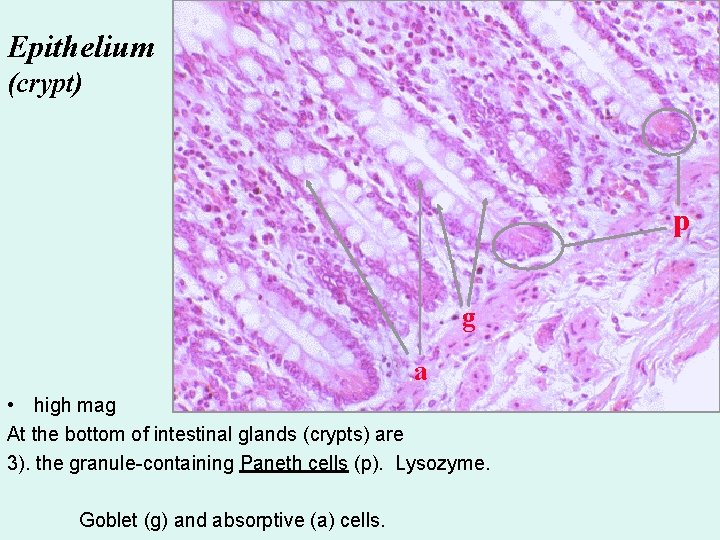
Epithelium (crypt) p g a • high mag At the bottom of intestinal glands (crypts) are 3). the granule-containing Paneth cells (p). Lysozyme. Goblet (g) and absorptive (a) cells.

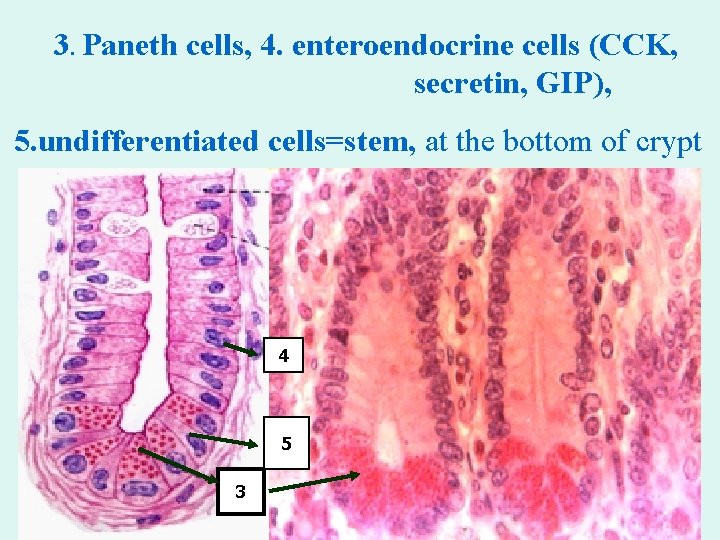
3. Paneth cells, 4. enteroendocrine cells (CCK, secretin, GIP), 5. undifferentiated cells=stem, at the bottom of crypt 4 5 3

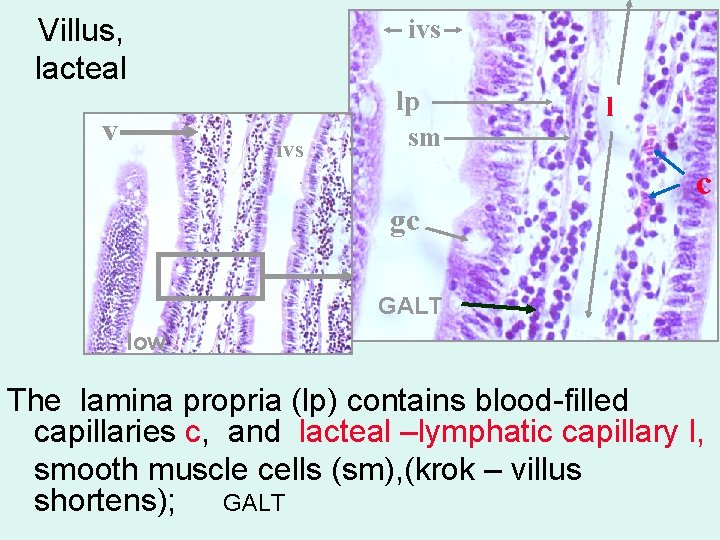
Villus, lacteal v ivs lp sm gc l c GALT low The lamina propria (lp) contains blood-filled capillaries c, and lacteal –lymphatic capillary l, smooth muscle cells (sm), (krok – villus shortens); GALT

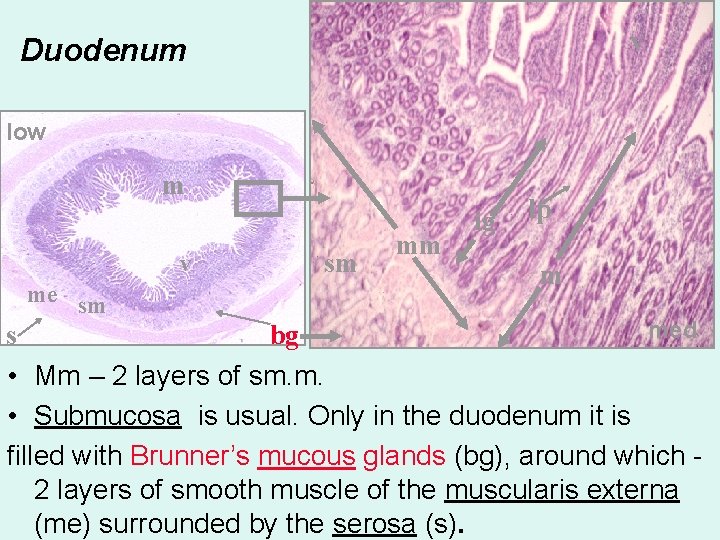
v Duodenum low m v me sm v sm mm ig lp m med s bg • Mm – 2 layers of sm. m. • Submucosa is usual. Only in the duodenum it is filled with Brunner’s mucous glands (bg), around which 2 layers of smooth muscle of the muscularis externa (me) surrounded by the serosa (s).

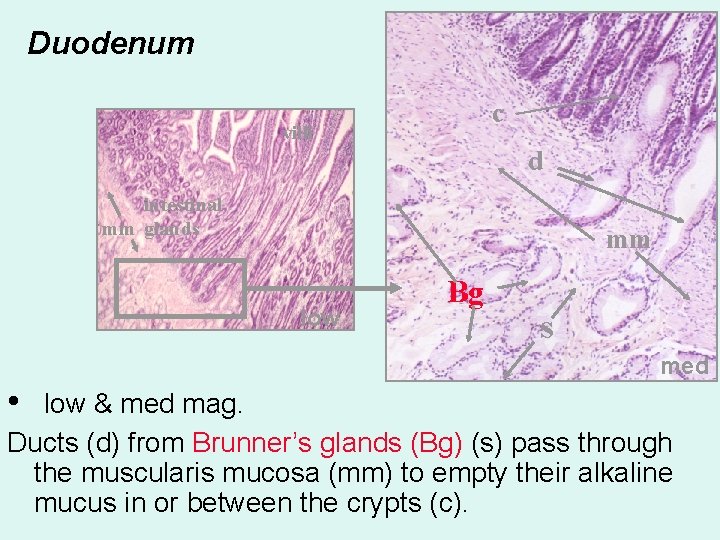
Duodenum c villi d intestinal mm glands mm low Bg s med • low & med mag. Ducts (d) from Brunner’s glands (Bg) (s) pass through the muscularis mucosa (mm) to empty their alkaline mucus in or between the crypts (c).

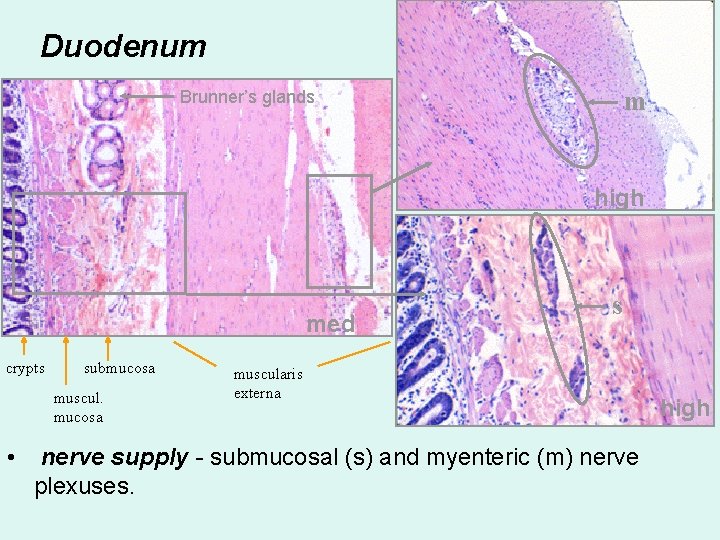
Duodenum m Brunner’s glands high med crypts submucosa muscul. mucosa • s muscularis externa nerve supply - submucosal (s) and myenteric (m) nerve plexuses. high

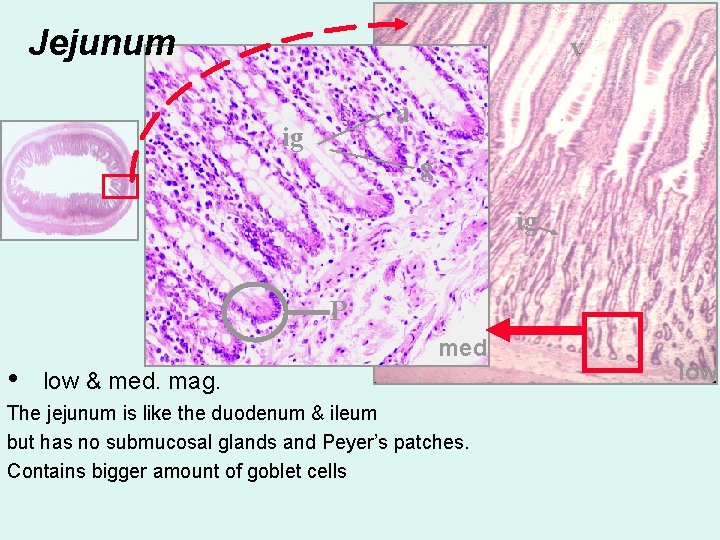
Jejunum v a ig g ig P • med low & med. mag. The jejunum is like the duodenum & ileum but has no submucosal glands and Peyer’s patches. Contains bigger amount of goblet cells low

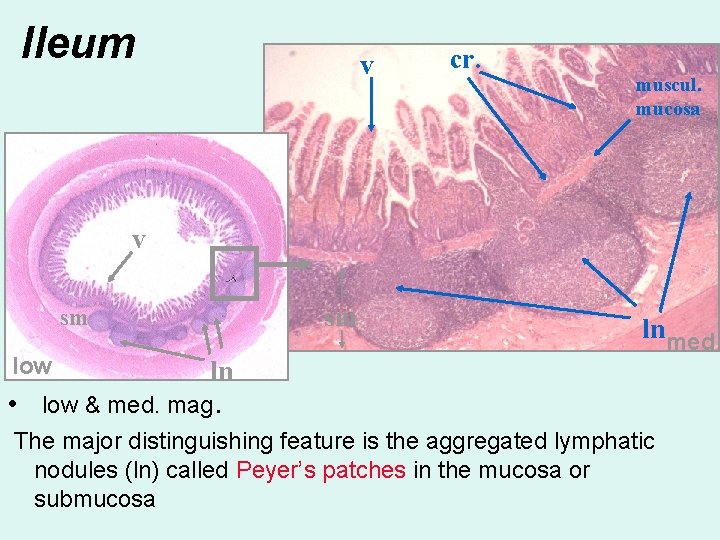
Ileum v cr. muscul. mucosa v sm sm low lnmed ln • low & med. mag. The major distinguishing feature is the aggregated lymphatic nodules (ln) called Peyer’s patches in the mucosa or submucosa

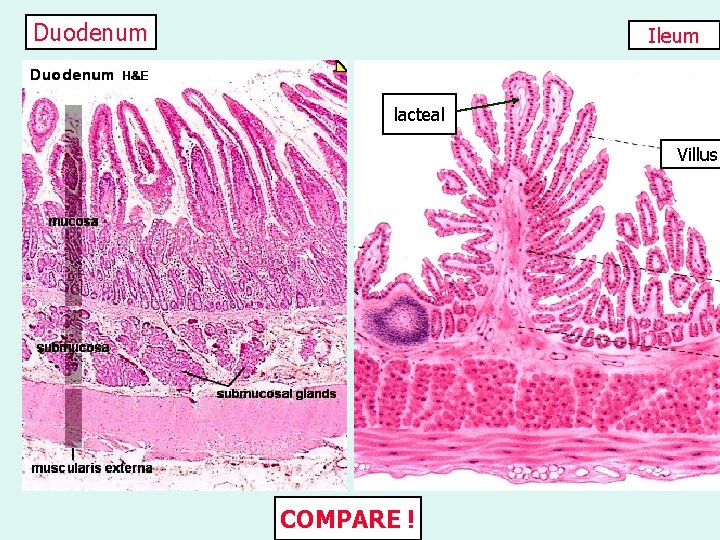
Duodenum Ileum lacteal Villus COMPARE !

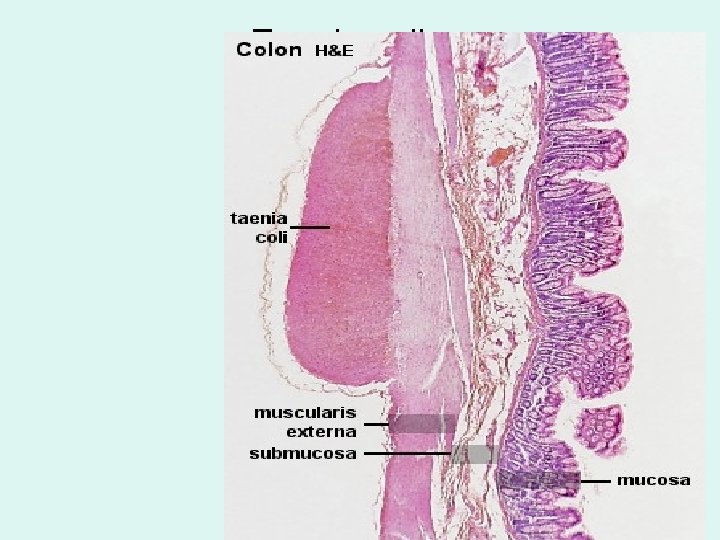
Large intestine (bowel) - general • Reabsorption of water, electrolytes, cellulous • Elimination of wastes • Inner lining - permanent internal folds of its mucosa & submucosa called plicae circulares and crypts. • Its mucosa lacks of villi. • The submucosa is usual • Circular & longitudinal smooth muscle form the muscularis externa. The inner circular layer is uniform but the outer longitudinal layer has 3 thicker bands, the taenia coli. • where the colon faces the abdominal cavity there is a serosa.

Taenia coli

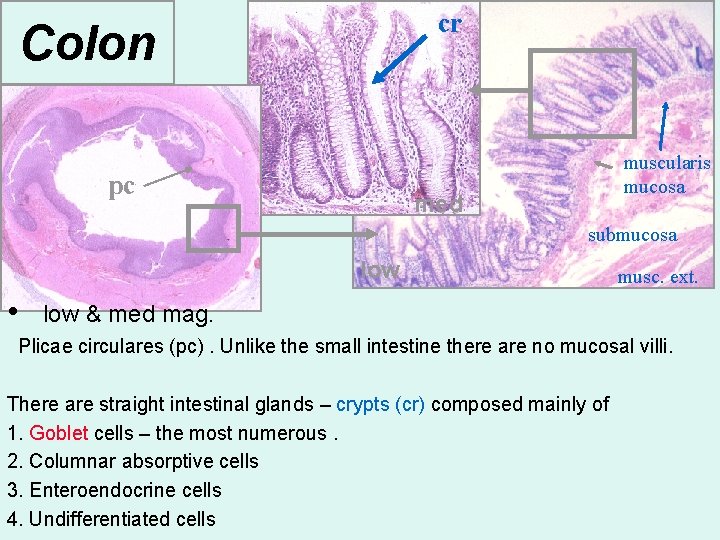
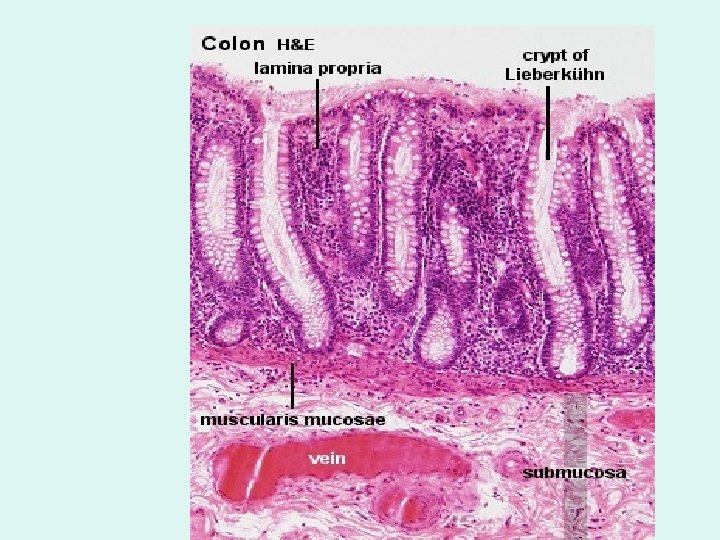
cr Colon pc muscularis mucosa med submucosa low • musc. ext. low & med mag. Plicae circulares (pc). Unlike the small intestine there are no mucosal villi. There are straight intestinal glands – crypts (cr) composed mainly of 1. Goblet cells – the most numerous. 2. Columnar absorptive cells 3. Enteroendocrine cells 4. Undifferentiated cells

High. Magn.

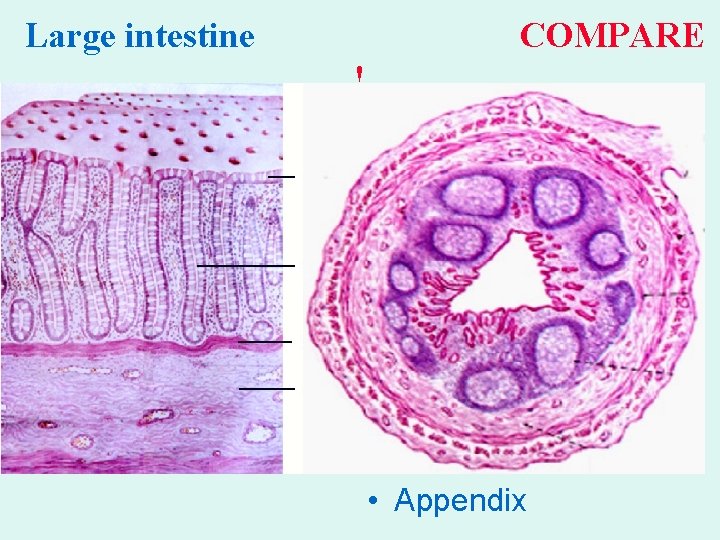
Large intestine COMPARE ! • Appendix

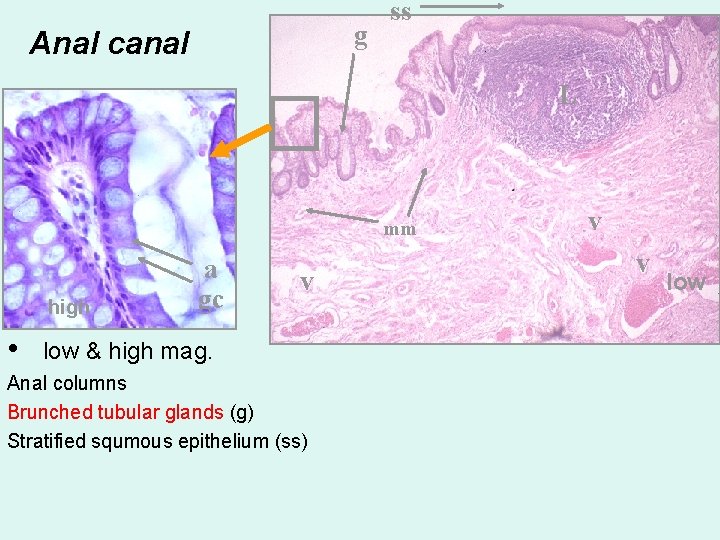
g Anal canal ss L ig high • a gc mm v low & high mag. Anal columns Brunched tubular glands (g) Stratified squmous epithelium (ss) v v low

Liver & Gall Bladder Liver has specific location – on the way of absorbed material, that is why has very original vasculature and functions

Functions: • • • Bile synthesis and secretion (emulsification) Excretion of bilirubin Protein synthesis Gluconeogenesis Storage Detoxification Protective Hemopoietic organ Endocrine

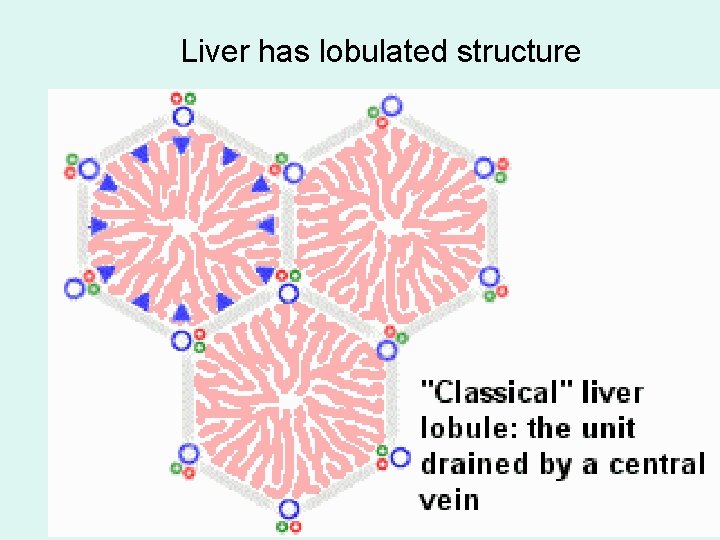
Liver has lobulated structure

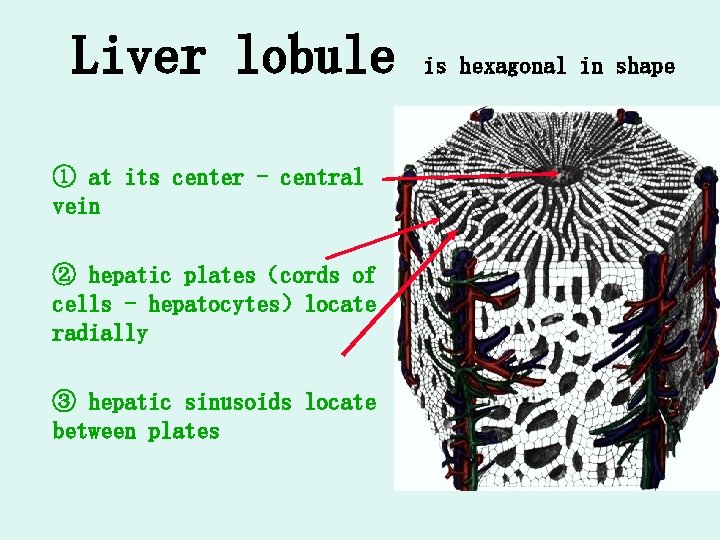
Liver lobule ① at its center - central vein ② hepatic plates(cords of cells - hepatocytes)locate radially ③ hepatic sinusoids locate between plates is hexagonal in shape

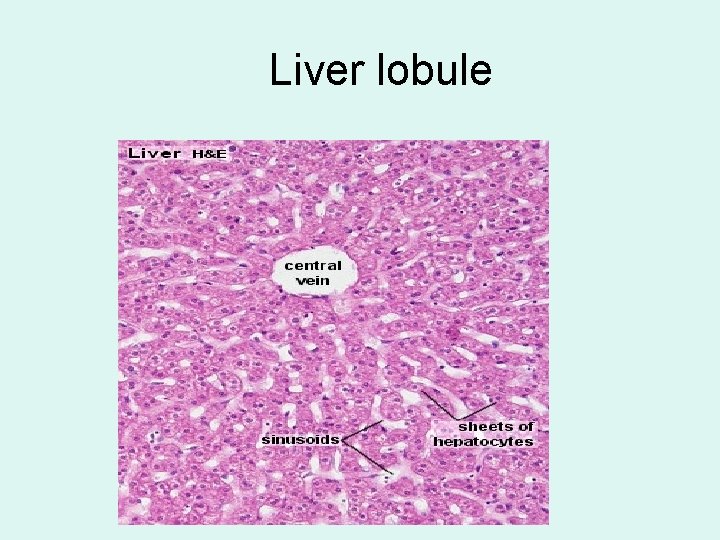
Liver lobule

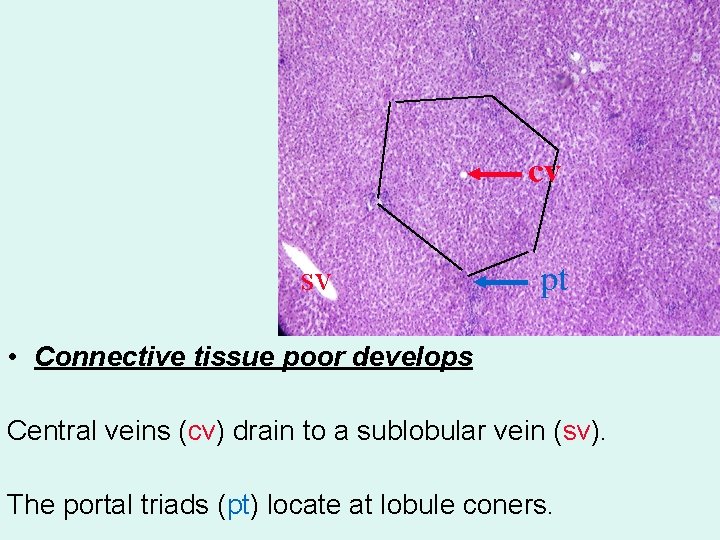
cv sv pt • Connective tissue poor develops Central veins (cv) drain to a sublobular vein (sv). The portal triads (pt) locate at lobule coners.

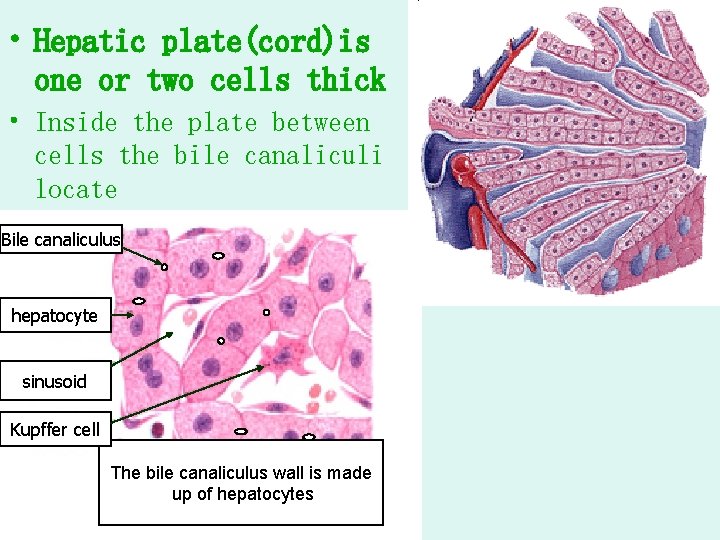
• Hepatic plate(cord)is one or two cells thick • Inside the plate between cells the bile canaliculi locate Bile canaliculus hepatocyte sinusoid Kupffer cell The bile canaliculus wall is made up of hepatocytes

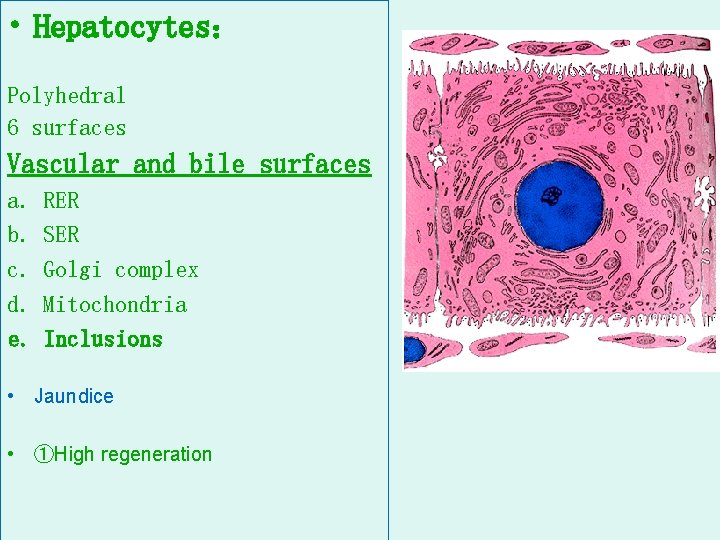
• Hepatocytes: Polyhedral 6 surfaces Vascular and bile surfaces a. b. c. d. e. RER SER Golgi complex Mitochondria Inclusions • Jaundice • ①High regeneration

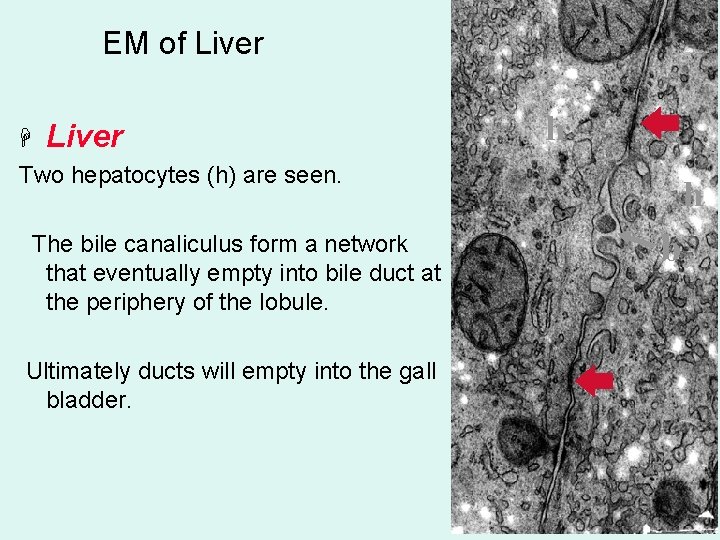
EM of Liver H Liver Two hepatocytes (h) are seen. The bile canaliculus form a network that eventually empty into bile duct at the periphery of the lobule. Ultimately ducts will empty into the gall bladder. h h b

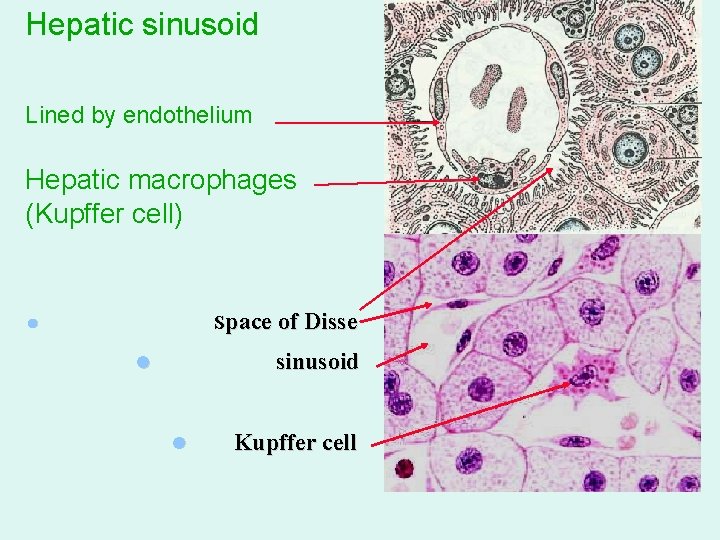
Hepatic sinusoid Lined by endothelium Hepatic macrophages (Kupffer cell) Space of Disse l sinusoid l l Kupffer cell

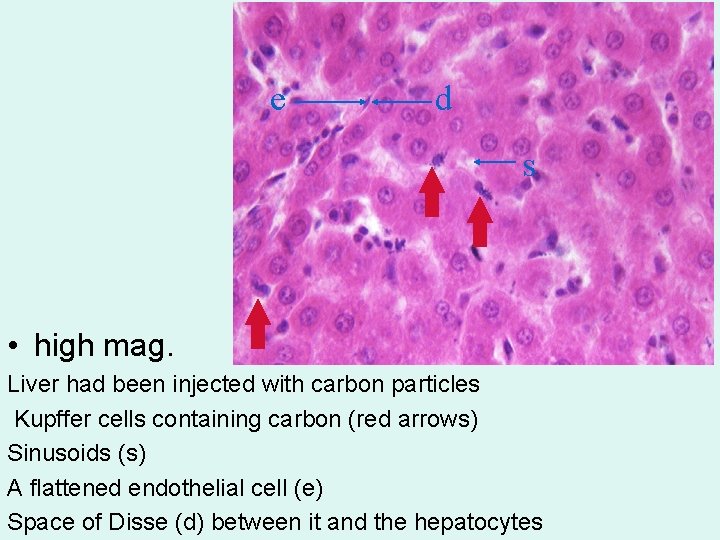
e d s • high mag. Liver had been injected with carbon particles Kupffer cells containing carbon (red arrows) Sinusoids (s) A flattened endothelial cell (e) Space of Disse (d) between it and the hepatocytes

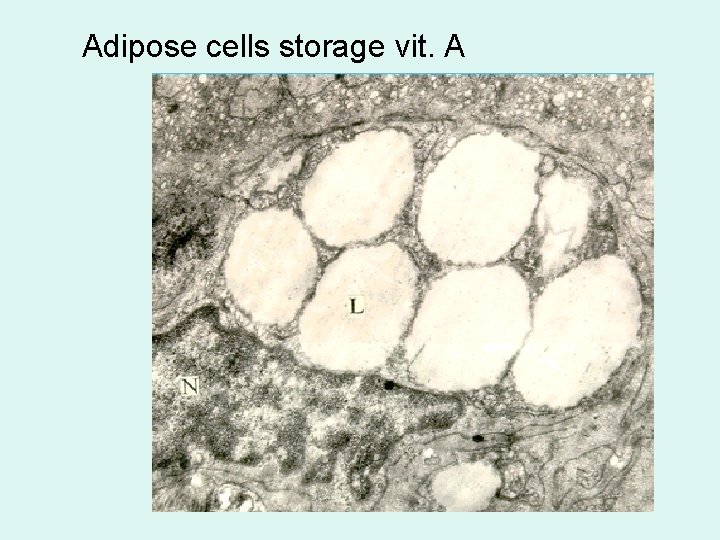
Adipose cells storage vit. A

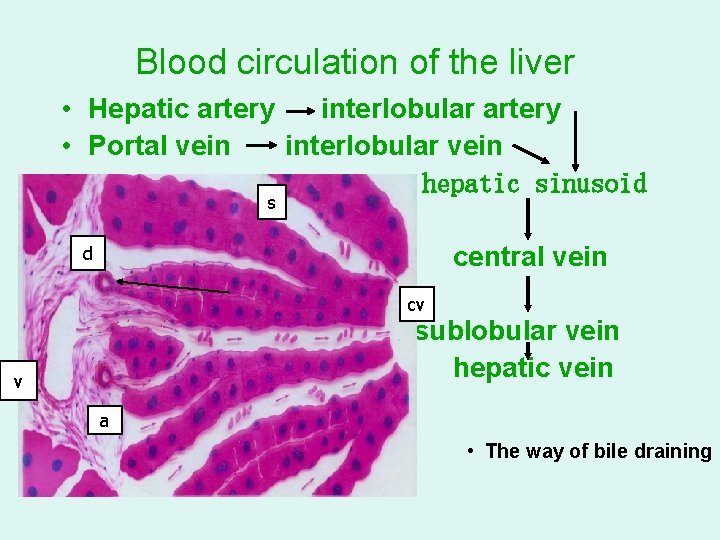
Blood circulation of the liver • Hepatic artery interlobular artery • Portal vein interlobular vein • hepatic sinusoid s v • d • cv • • central vein cv sublobular vein hepatic vein a • The way of bile draining

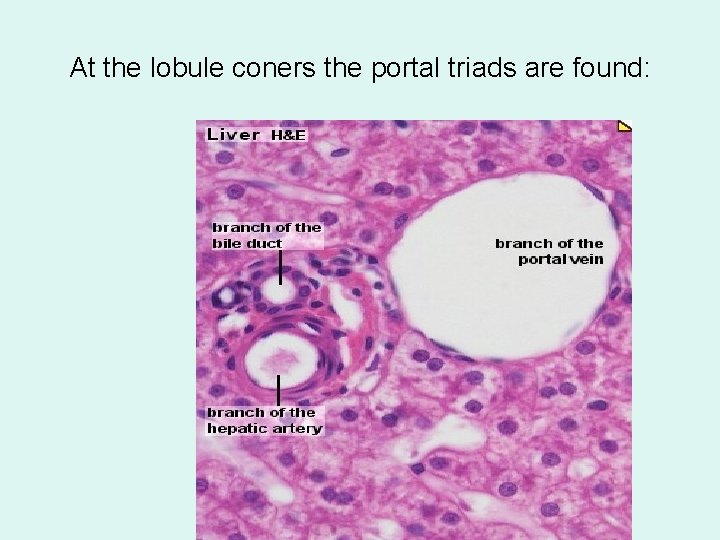
At the lobule coners the portal triads are found:

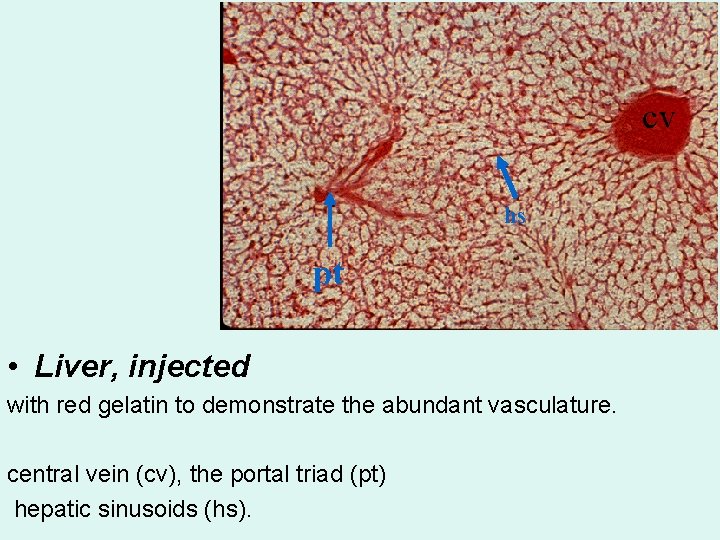
cv hs pt • Liver, injected with red gelatin to demonstrate the abundant vasculature. central vein (cv), the portal triad (pt) hepatic sinusoids (hs).

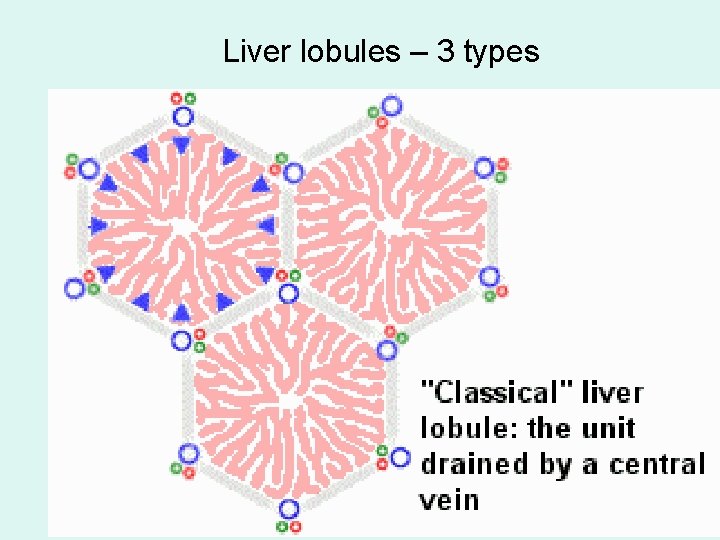
Liver lobules – 3 types

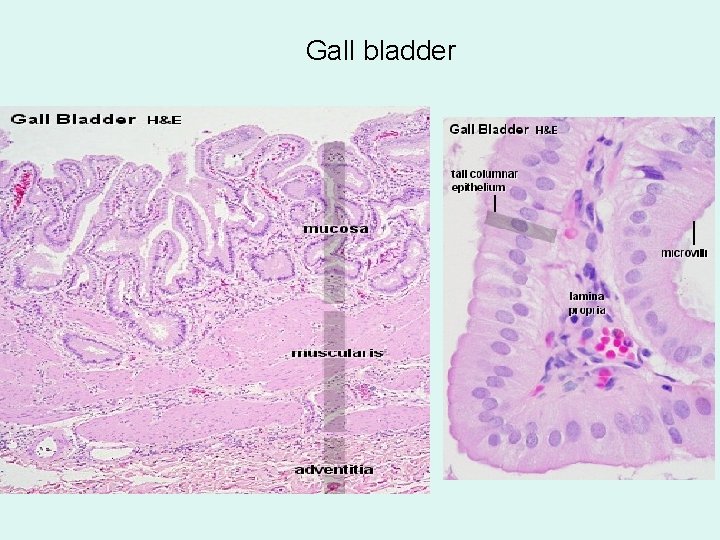
Gall bladder

Pancreas. Mixed gland • Functions: – Exocrine • • Trypsinogen, peptidase Amylase Lipase Deoxyribonuclease, ribonuclease – Endocrine

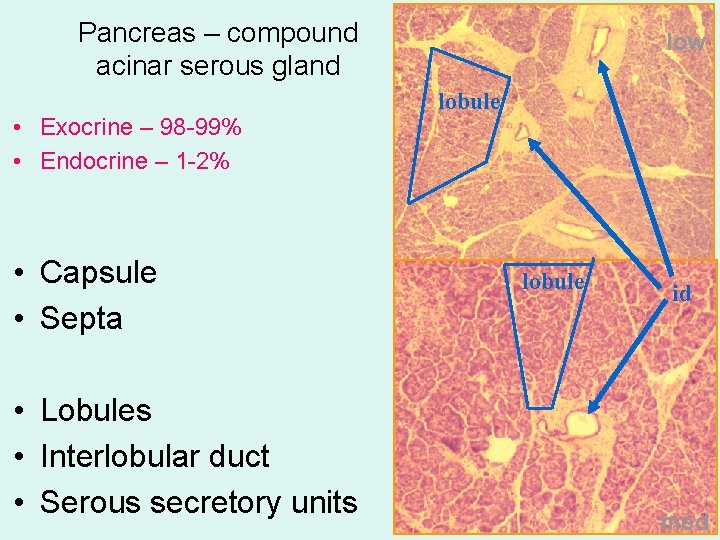
Pancreas – compound acinar serous gland • Exocrine – 98 -99% • Endocrine – 1 -2% • Capsule • Septa • Lobules • Interlobular duct • Serous secretory units low lobule id med

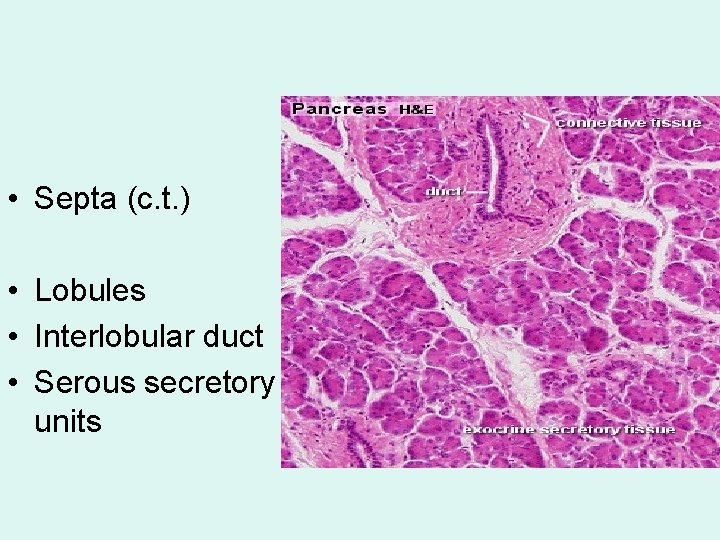
• Septa (c. t. ) • Lobules • Interlobular duct • Serous secretory units

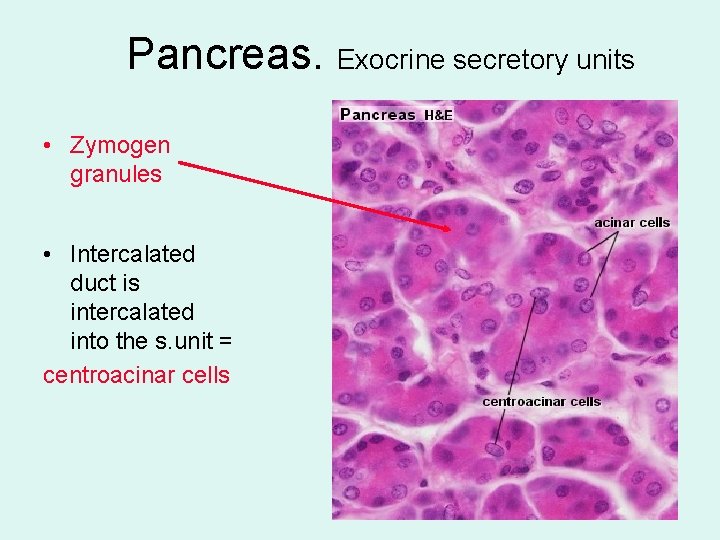
Pancreas. Exocrine secretory units • Zymogen granules • Intercalated duct is intercalated into the s. unit = centroacinar cells

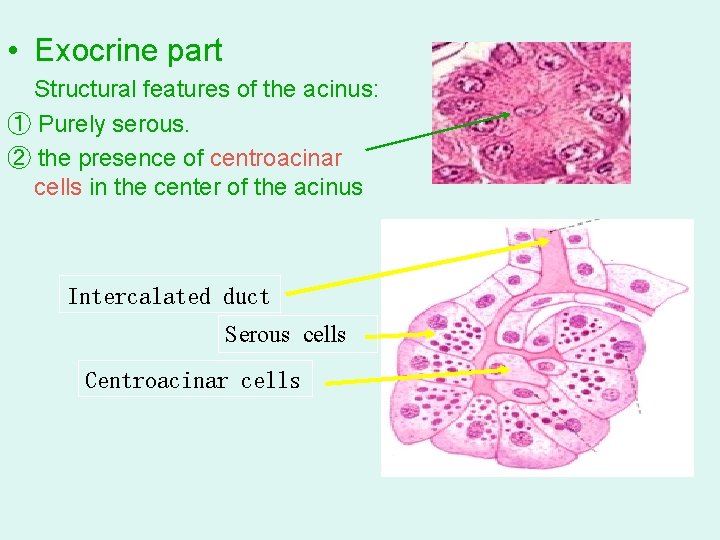
• Exocrine part Structural features of the acinus: ① Purely serous. ② the presence of centroacinar cells in the center of the acinus Intercalated duct Serous cells Centroacinar cells

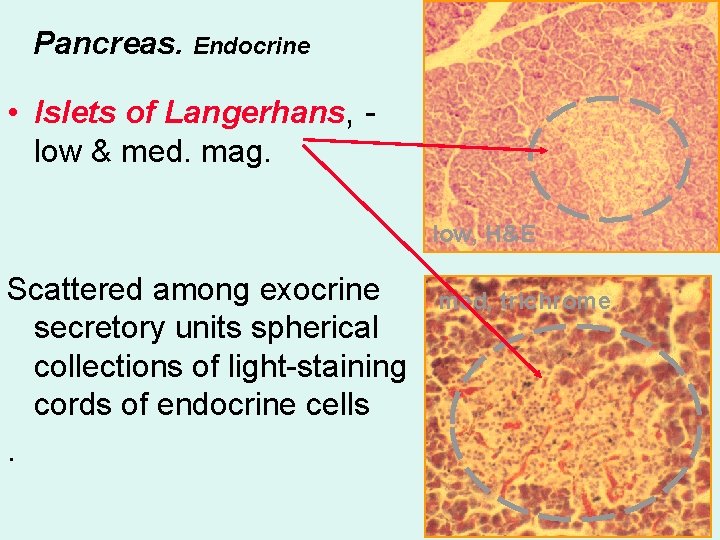
Pancreas. Endocrine • Islets of Langerhans, low & med. mag. low, H&E Scattered among exocrine secretory units spherical collections of light-staining cords of endocrine cells. med, trichrome

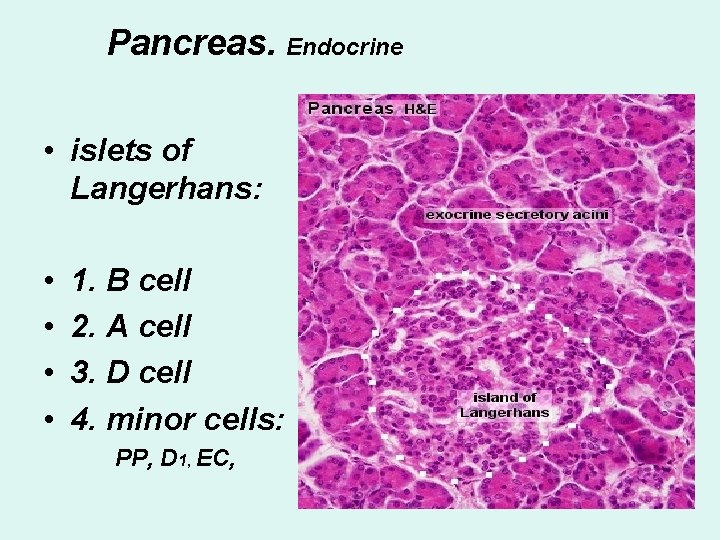
Pancreas. Endocrine • islets of Langerhans: • • 1. B cell 2. A cell 3. D cell 4. minor cells: PP, D 1, EC,

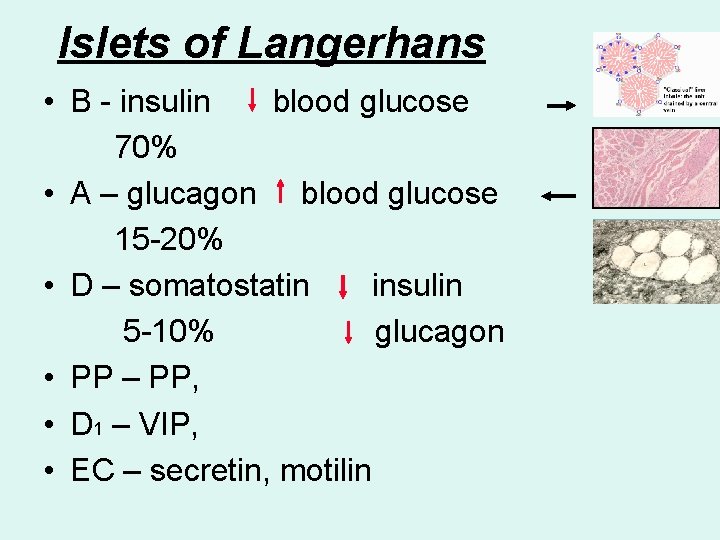
Islets of Langerhans • B - insulin blood glucose 70% • A – glucagon blood glucose 15 -20% • D – somatostatin insulin 5 -10% glucagon • PP – PP, • D 1 – VIP, • EC – secretin, motilin