Lecture 4 1 2 3 4 5 Announcements

















- Slides: 27

Lecture 4 1. 2. 3. 4. 5. Announcements Email me if you did NOT receive a message from me last Friday. Black. Board kinda works but we will stay with our own site for now: www. uky. edu/~gcbrown/ent 561 Will try to get the lecture notes on sooner. No quiz on Thursday Online Reading: http: //www. crid. or. cr/digitalizacion/pdf/eng /doc 14606 -10. pdf

Epidemic Components • 1. The etiologic agent = microorganism that can cause disease. – Pathogenicity = its ability to cause disease; – Virulence = the severity of infection, expressed as: • morbidity = incidence of disease • mortality = death rate of the infection. • 2. The method of transmission = means by which the agent goes from the “source” to the host. We are only concerned with vectored pathogens here. • 3. The host – Depends on 3 things: – Accessibility – Susceptibility – Transmissibility

Most studies of arthropod-vectored disease study: • Time Trends – Four kinds – – • The secular trend - occurrence of disease over years The periodic trend – temporary change in a secular trend, The seasonal trend - seasonal changes in disease occurrence The epidemic occurrence of disease. Place Considerations – where the individual was when disease occurred; – where the individual was when he or she became infected; – where the vector became infected with the etiologic agent. • Infected Person – Individual characteristics: age, sex, occupation, personal habits, underlying disease, immunization history, etc. – Social characteristics: socioeconomic status, geographical distribution, public works & policies, disease rates in other group members

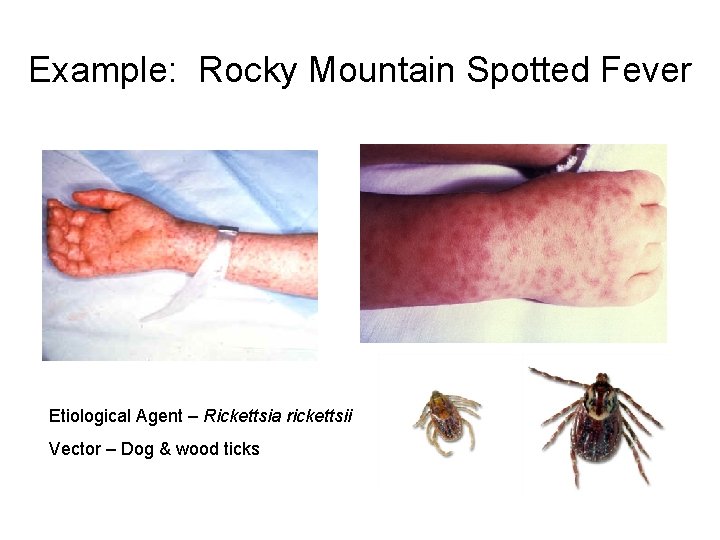
Example: Rocky Mountain Spotted Fever Etiological Agent – Rickettsia rickettsii Vector – Dog & wood ticks

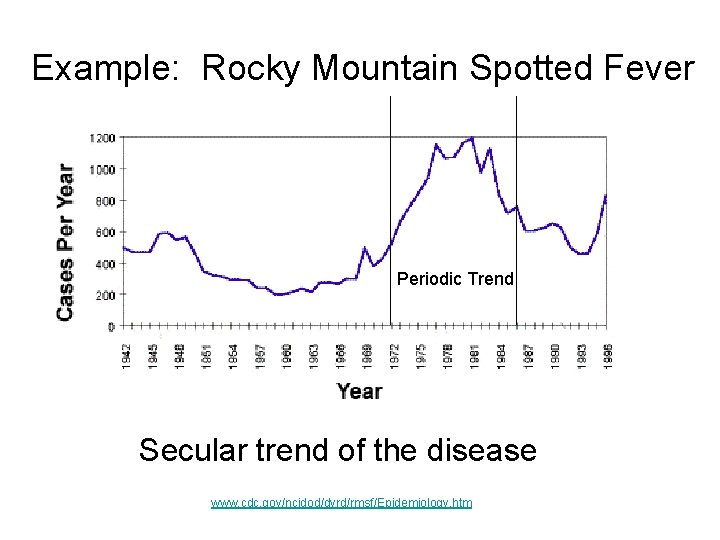
Example: Rocky Mountain Spotted Fever Periodic Trend Secular trend of the disease www. cdc. gov/ncidod/dvrd/rmsf/Epidemiology. htm

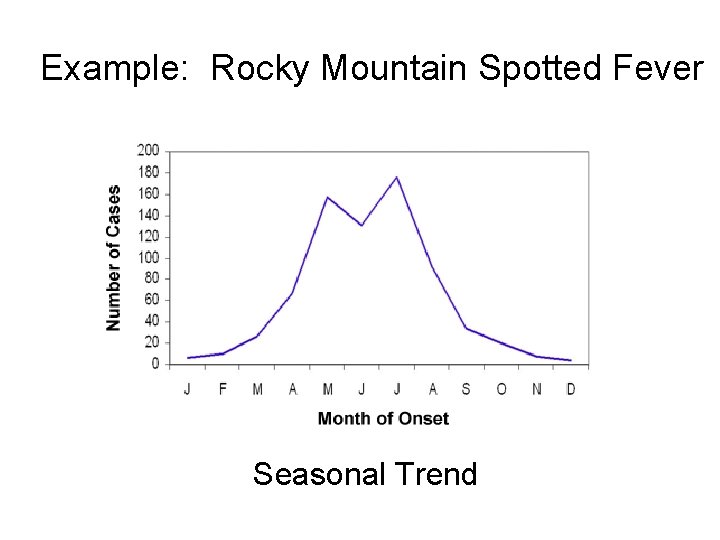
Example: Rocky Mountain Spotted Fever Seasonal Trend

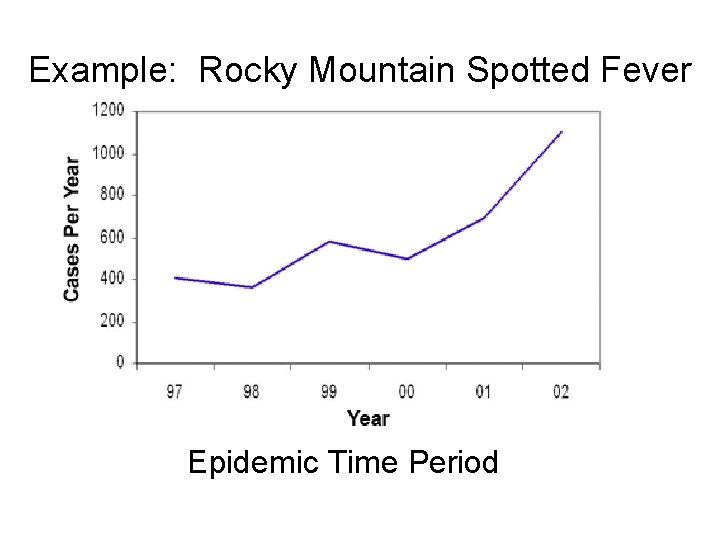
Example: Rocky Mountain Spotted Fever Epidemic Time Period

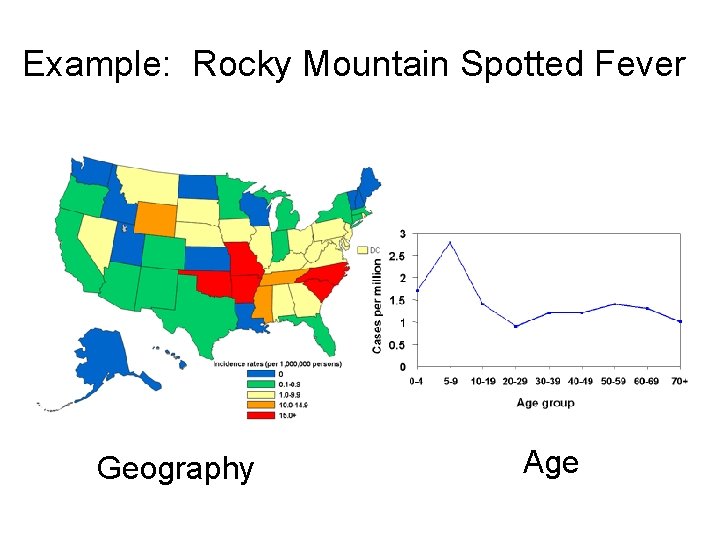
Example: Rocky Mountain Spotted Fever Geography Age

Parasite types in Medical Entomology • Micro vs macroparasites – Micro are microorganisms (viruses, bacteria, protozoa, etc. ). Macro are arthropods. • Ectoparasites vs endoparasites – – Ecto – parasitize from outside the host, infestation normally remains topical and peripheral – Endoparasites – parasitize from inside the host, Microparasites can produce systemic infestation. Disease is normally systemic. • Facultative vs. obligate – – Obligate are totally dependent on host. – Facultative have parasitic and free living forms.

Vectors and bloodfeeding • Most vectors are blood-feeders: – Normally the pathogen does not benefit the vector, detrimental effects sometimes occur. – The pathogen receives many benefits (acqusition, transport, re-insertion). – Principal problems for the pathogen from this system: • Must overcome ingestion by the vector (next slide) • Must be able to infect a new host from a small inoculum (slide following) • Totally dependent on the vector-host population dynamics and interaction.

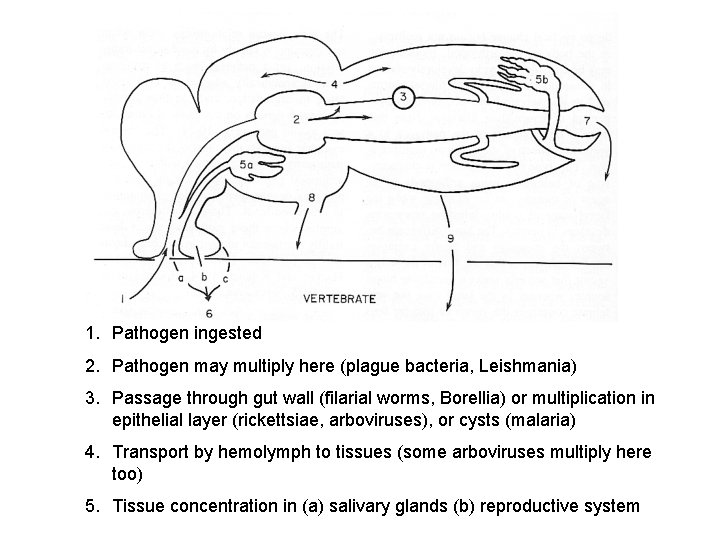
1. Pathogen ingested 2. Pathogen may multiply here (plague bacteria, Leishmania) 3. Passage through gut wall (filarial worms, Borellia) or multiplication in epithelial layer (rickettsiae, arboviruses), or cysts (malaria) 4. Transport by hemolymph to tissues (some arboviruses multiply here too) 5. Tissue concentration in (a) salivary glands (b) reproductive system

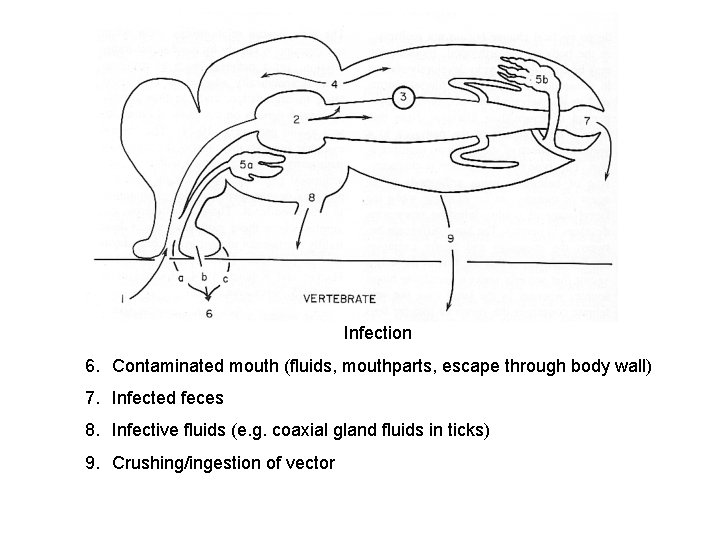
Infection 6. Contaminated mouth (fluids, mouthparts, escape through body wall) 7. Infected feces 8. Infective fluids (e. g. coaxial gland fluids in ticks) 9. Crushing/ingestion of vector

Definitive vs. Intermediate Hosts Definitive • Host in which gametocycte union occurs for the parasite. • AKA – Primary host Intermediate • Host in which asexual reproduction occurs for the parasite. • AKA – Secondary host; Alternate host

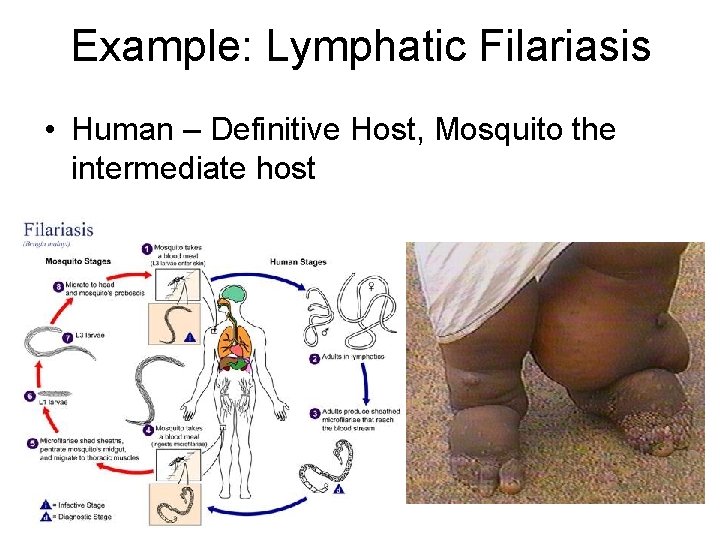
Example: Lymphatic Filariasis • Human – Definitive Host, Mosquito the intermediate host

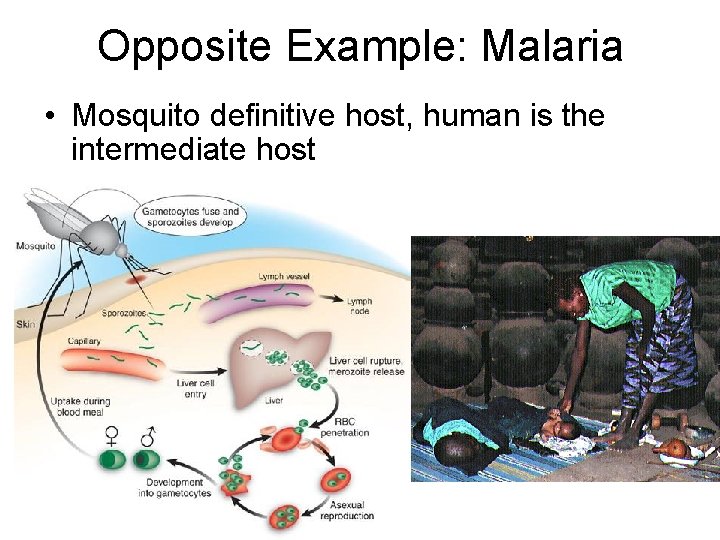
Opposite Example: Malaria • Mosquito definitive host, human is the intermediate host

More about hosts • accidental host one that accidentally harbors an organism that is not ordinarily parasitic in the particular species. • amplifying host one that increases parasite numbers &/or no. infectious vectors. Typically short-lived infections. • dead-end host the disease cannot be transmitted from the infected host to another animal. • predilection host the host preferred by a parasite. • reservoir host an animal (or species) that is infected by a parasite, and which serves as a source of infection for humans or another species. • transfer host, transport host one that is used until the appropriate definitive host is reached, but is not necessary to complete the life cycle of the parasite.

About Vectors – Host Selection • ‘phagic’ – feeds successfully; ‘philic’ – attracted to. • Anthropophagic – feed successfully on humans; Anthropophilic – attacks humans • Zoophagic – feed on vertebrates other than humans. Two big subsets – Mammalophagic – Ornithophagic

Modes of Transmission • Two main modes: – VERTICAL – vector to vector in subsequent life stages or generations – HORIZONTAL – passage of parasites between vectors and hosts

Vertical Transmission Subtypes • Transstadial – between subsequent life stages • Transgeneration – between subsequent generations (several methods) • Venereal – passage of parasites occurs between male and female during mating. Rare in vectors

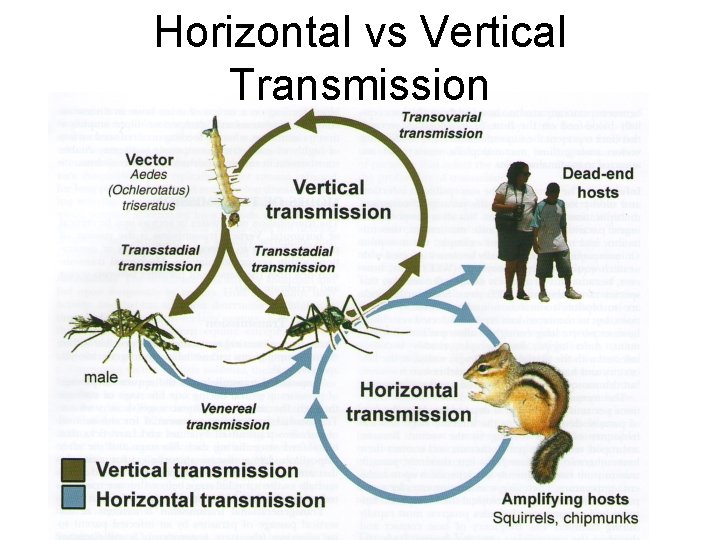
Horizontal vs Vertical Transmission

Compare Figs. 3. 3 & 3. 2 in your text 1. Which are the dead end hosts? 2. Where are the bridge vectors? 3. Where is the amplification cycle? 4. Where is the enzootic transmission cycle?

Interseasonal Maintenance • Most seasonal disease from arthropod-vectored pathogens in temperate zones require interseasonal maint. • Principal mechanisms: – Continued transmission – no seasonality, tropical diseases, disease of parasites that continuously live with hosts – Infected Vectors – most encephalitis viruses – Infected hosts – Reservoirs go dormant, parasite has a dormant stage in host. – No interseasonal maintenance – occasional local extinction • Migratory hosts • Weather fronts

Principles of Disease Vector Management • Surveillance – Vector, disease prevalence, pathogen burden • Prevention – Personal – Public • Control – Vector-based – Pathogen-based (pharmacologic)

Surveillance • Very good general section on this subject in your text: pp: 29 – 32

Prevention • Personal – Exclusion agents (clothing, screening, bed nets, sealing cracks/crevices, etc. ) – Chemical agents (repellents) – Private source controls – Sanitation & Personal Hygiene – Source Avoidance • Public – Public service announcements/education – Vector breeding site controls/sanitation – Disaster Management Planning READ: http: //www. crid. or. cr/digitalizacion/pdf/eng/doc 1460610. pdf

A Key Concept in DV Management is Risk • Most DV Management is Govt. Funded • They fund efforts in response to perceived risk • Risk = Cost of a Bad Outcome TIMES Probability of that Outcome Occurring

The main problem is there are multiple risks • Multiple “Bad Outcomes” including – Economic – Environmental – Social – Political • Each outcome has it’s own cost and probability • Major Complication: Disease risk is inversely correlated with vector control.