Learning from Neonatal Mortality Reviews Yorkshire and Humber

Learning from Neonatal Mortality Reviews Yorkshire and Humber Neonatal ODN Annual Conference 01/10/2020 Sunita Seal Yousef Gargani

We have a mortality problem! • • YHODN high mortality (MBRRACE) Mortality summit October 2019 Reduce preventable deaths 4 groups – Mortality Review, Thematic Analysis & Shared Learning – DCC & Thermal Care – Initial Respiratory Care – The Golden Hour

Mortality Review group • • Sunita Seal Kirsteen Mackay Joanna Preece Kathryn Johnson Aparna Manou Yousef Gargani Lisa Barker • • Karen White Joanna Hadley Sarah Simpson Susan Gibson Joyce Ayre Aoife Hurley Alex Lu

Current review process • Local mortality reviews (neonatal, perinatal) • PMRT • Network review – YHODN – South/North – Some thematic analysis • ? Standardised • ? Sharing learning outside of local unit
Aims Data collection – descriptive, qualitative Standardised review process Thematic analysis Strong learning Shared learning Actions (local and network)

Mortality data collection • YHODN high rates (MBRRACE data) • To understand why - more comprehensive analysis of deaths with more detail that Badger and MBRRACE offer required • Database? Demographic details plus details of circumstances of death including: Palliative care plan? Antenatal or postnatal? Reorientation of care Unexpected death Modifiable factors ( delivery and neonatal) PMRT

Standardised reviews – Driver diagrams • Quality of M&M discussions is variable • Are the right questions always asked? • If we want to share mortality themes and learning, we should be asking the same questions • Can driver diagrams be useful to target QI projects prospectively?
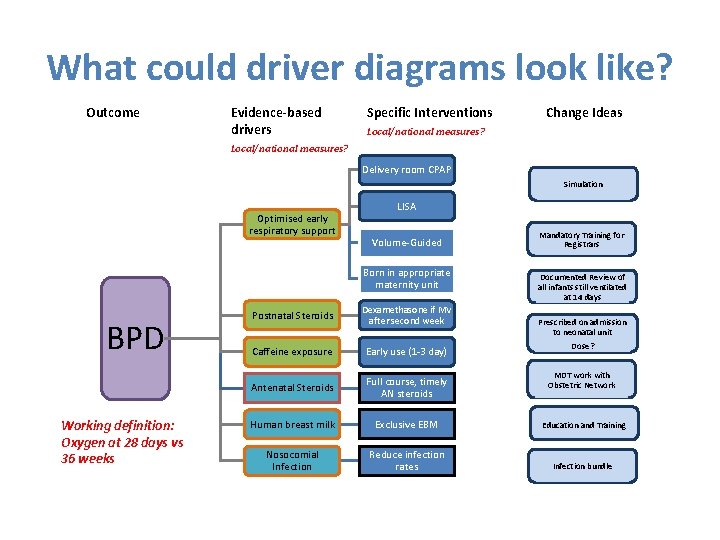
What could driver diagrams look like? Outcome Evidence-based drivers Specific Interventions Change Ideas Local/national measures? Delivery room CPAP Simulation Optimised early respiratory support LISA Volume-Guided Born in appropriate maternity unit BPD Working definition: Oxygen at 28 days vs 36 weeks Mandatory Training for Registrars Documented Review of all infants still ventilated at 14 days Postnatal Steroids Dexamethasone if MV after second week Caffeine exposure Early use (1 -3 day) Antenatal Steroids Full course, timely AN steroids Human breast milk Exclusive EBM Education and Training Nosocomial Infection Reduce infection rates Infection bundle Prescribed on admission to neonatal unit Dose? MDT work with Obstetric Network

How can they inform M&M discussion? • Infant who had severe BPD and/or died as a result: – – – – – Were they born in an appropriate unit? Did they receive full course of antenatal steroids? Did they receive delivery room CPAP? Did they receive early surfactant? How was their initial ventilation managed? Did they receive early caffeine? If ventilated after two weeks did they receive Dexamethasone? What milk did they receive? Did they have any late onset sepsis concerns? – Did they have a PDA? How was this managed? – Did they have chronic reflux/aspiration? How was this managed?

How can they be used to drive quality? • Identify aspects of care we should be measuring e. g. – % babies born in correct unit – % babies receiving full course of antenatal steroids – % babies receiving delivery room CPAP – % eligible babies receiving LISA – % babies having exclusive EBM • Then identify aspects that need improvement and generate change/QI
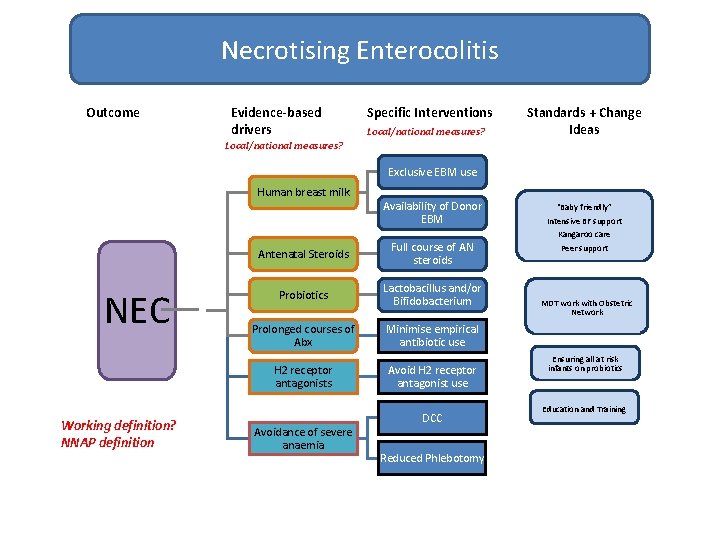
Necrotising Enterocolitis Outcome Evidence-based drivers Specific Interventions Local/national measures? Standards + Change Ideas Local/national measures? Exclusive EBM use Human breast milk NEC Working definition? NNAP definition Availability of Donor EBM Antenatal Steroids Full course of AN steroids Probiotics Lactobacillus and/or Bifidobacterium Prolonged courses of Abx Minimise empirical antibiotic use H 2 receptor antagonists Avoid H 2 receptor antagonist use Avoidance of severe anaemia DCC Reduced Phlebotomy “Baby friendly” Intensive BF support Kangaroo care Peer support MDT work with Obstetric Network Ensuring all at risk infants on probiotics Education and Training

Thematic analysis • Themes identified in the following broad areas: – – – – Antenatal communication & counselling Resuscitation - equipment availability & thermal control Early care on the NNU - particularly the golden hour Infection - timing of antibiotics in EOS End of life care - involvement of palliative care teams Documentation & communication Practical procedures eg Vascular access - correct positioning & security • Strong learning - feed into QI projects & guidelines

Shared learning • Key part of this project • Forum/network meetings • Local units – existent processes (huddles/social media/Neonatal Safety Champions/perinatal meetings) • Incorporate into teachings (simulations, STEPP, nursing study days) • Liaison with maternity - LMS safety groups and MATNEO SIN (Safety Improvement Network)

Summary • • • Improve the quality of reviews Identify trends in cause of death Driver diagrams will help Pan-ODN analysis of PMRT reviews Share learning widely Ongoing process with reports produced annually

Questions? Thank you!
- Slides: 16