Late thrombotic events after BRS implantation a systematic

Late thrombotic events after BRS implantation: a systematic review and meta-analysis of randomised clinical trials COLLET Carlos 1, ASANO Taku 1, MIYAZAKY Yosuke 2, TENEKECIOGLU Erhan 2, KATAGUIRY Yuki 1, DE WINTER Robbert 1, CAPODANNO Davide 3, ONUMA Yoshinobu 2, SERRUYS Patrick W. 4 1. Academic Medical Center, University of Amsterdam, 2. Erasmus Medical Center, Rotterdam, 3. Ferrarotto Hospital, University of Catania 4. Imperial College of London

INTRODUCTION • Historically, the occurrence of stent thrombosis (ST) has jeopardized the safety of percutaneous coronary interventions (PCIs). • The use of dual antiplatelet therapy (DAPT), appropriate stent implantation techniques (i. e. post-dilatation with adequate stent expansion), and the advent of drug eluting stents (DES) have significantly reduced the rate of ischemic complication following PCI. • Focusing on long-term safety and efficacy, the concept of the bioresorbable scaffold was developed. Early scaffolding and very late resorption was aimed at maintaining efficacy and returning the treated region to the natural anatomical and physiological environment; this would translate into a clinical benefit at long-term follow-up.
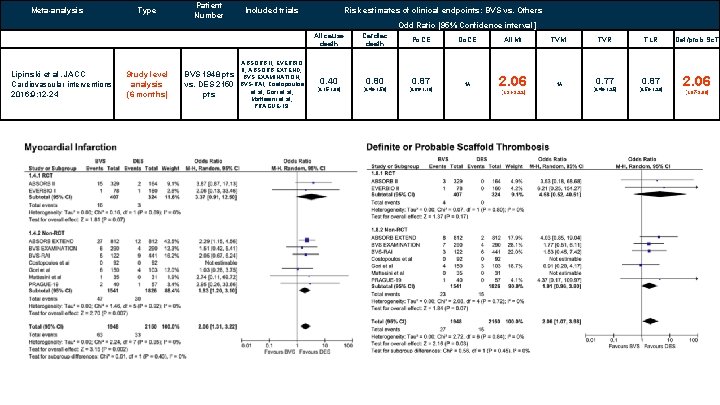
Meta-analysis Type Patient Number Included trials Risk estimates of clinical endpoints: BVS vs. Others Odd Ratio [95% Confidence interval] All cause death Lipinski et al. JACC Cardiovascular interventions 2016; 9: 12 -24 Study level analysis (6 months) BVS 1948 pts vs. DES 2150 pts ABSORB II, EVERBIO II, ABSORB EXTEND, BVS EXAMINATION, BVS-RAI, Costopoulos et al, Gori et al, Mattesini et al, PRAGUE-19. Cardiac death Po. CE Do. CE All MI TVMI NA 2. 06 NA 0. 40 0. 87 [0. 15 -1. 06] [0. 40 -1. 59] [0. 66 -1. 16] [1. 31 -3. 22] TVR TLR Def/prob Sc. T 0. 77 0. 87 [0. 48 -1. 25] [0. 59 -1. 28] 2. 06 [1. 07 -3. 98]
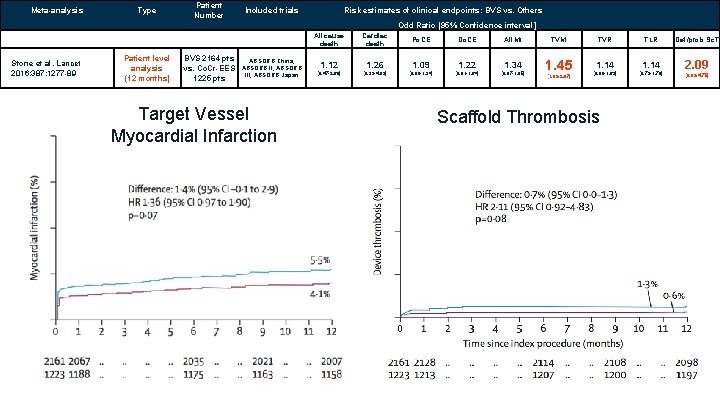
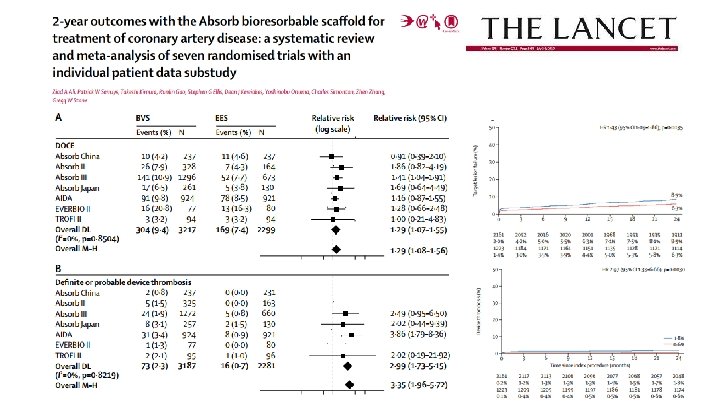
Meta-analysis Type Patient Number Included trials Risk estimates of clinical endpoints: BVS vs. Others Odd Ratio [95% Confidence interval] All cause death Stone et al. Lancet 2016; 387: 1277 -89 Patient level analysis (12 months) BVS 2164 pts vs. Co. Cr-EES 1225 pts ABSORB China, ABSORB III, ABSORB Japan Target Vessel Myocardial Infarction Cardiac death Po. CE Do. CE All MI TVMI 1. 45 1. 12 1. 26 1. 09 1. 22 1. 34 [0. 47 -2. 69] [0. 33 -4. 82] [0. 89 -1. 34] [0. 91 -1. 64] [0. 97 -1. 85] [1. 02 -2. 07] TVR TLR 1. 14 [0. 80 -1. 62] [0. 73 -1. 79] Scaffold Thrombosis Def/prob Sc. T 2. 09 [0. 92 -4. 75]

METHODS • Two independent reviewers searched MEDLINE/ Embase/ CENTRAL applying the search terms ‘bioresorbable’, ‘scaffold’ ‘everolimus-eluting stent(s)’, and ‘randomized trial’. • We included randomized clinical trials with patients who: (i) underwent PCI for obstructive coronary artery disease; (ii) had at least 24 months clinical followup; and (iii) underwent PCI with implantation of Absorb BVS. • The primary safety outcome of interest was to compare the risk of definite/ probable device thrombosis (DT) after BVS and EES implantation. The primary efficacy outcome of interest was the risk of TLF [cardiac death, TVMI, and ischaemia-driven target lesion revascularization (IDTLR)]. • Random-effect model.
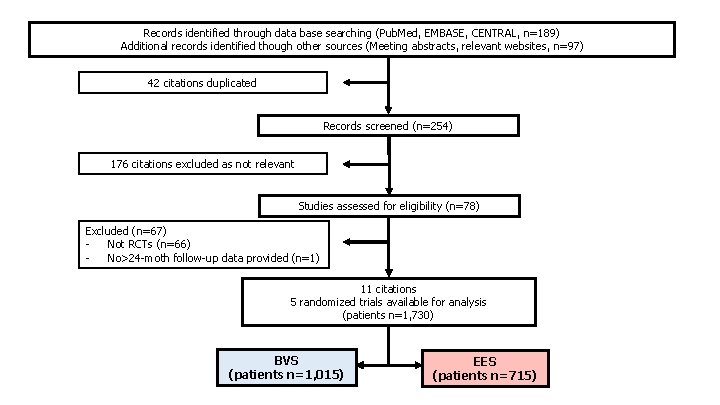
Records identified through data base searching (Pub. Med, EMBASE, CENTRAL, n=189) Additional records identified though other sources (Meeting abstracts, relevant websites, n=97) 42 citations duplicated Records screened (n=254) 176 citations excluded as not relevant Studies assessed for eligibility (n=78) Excluded (n=67) Not RCTs (n=66) No>24 -moth follow-up data provided (n=1) 11 citations 5 randomized trials available for analysis (patients n=1, 730) BVS (patients n=1, 015) EES (patients n=715)
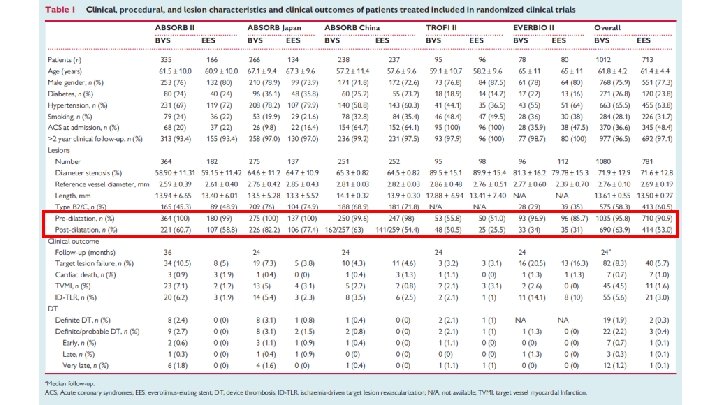
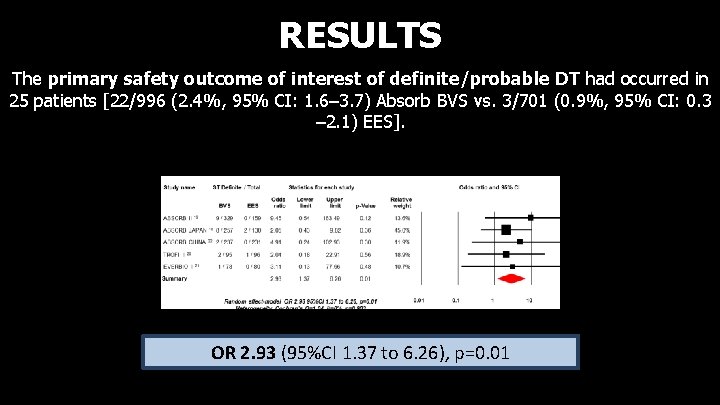
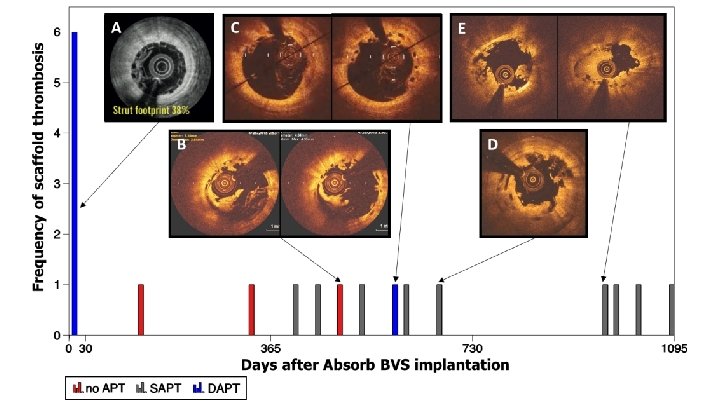
RESULTS The primary safety outcome of interest of definite/probable DT had occurred in 25 patients [22/996 (2. 4%, 95% CI: 1. 6– 3. 7) Absorb BVS vs. 3/701 (0. 9%, 95% CI: 0. 3 – 2. 1) EES]. OR 2. 93 (95%CI 1. 37 to 6. 26), p=0. 01
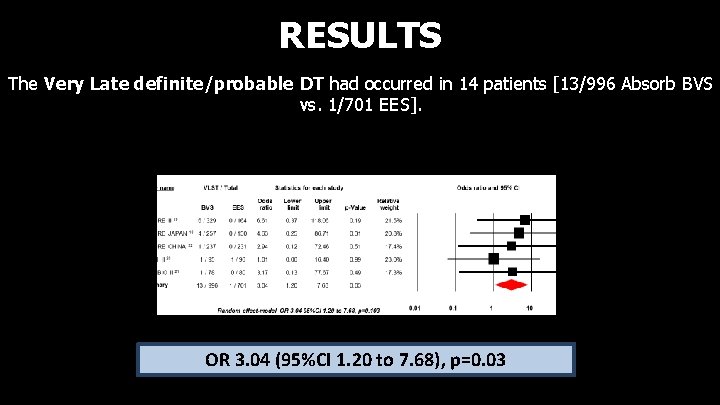
RESULTS The Very Late definite/probable DT had occurred in 14 patients [13/996 Absorb BVS vs. 1/701 EES]. OR 3. 04 (95%CI 1. 20 to 7. 68), p=0. 03
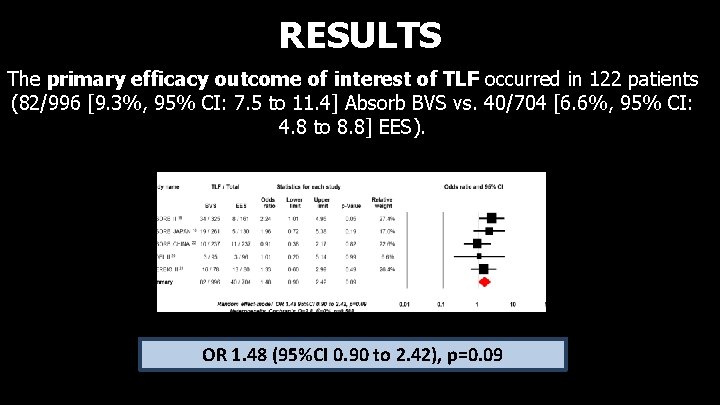
RESULTS The primary efficacy outcome of interest of TLF occurred in 122 patients (82/996 [9. 3%, 95% CI: 7. 5 to 11. 4] Absorb BVS vs. 40/704 [6. 6%, 95% CI: 4. 8 to 8. 8] EES). OR 1. 48 (95%CI 0. 90 to 2. 42), p=0. 09
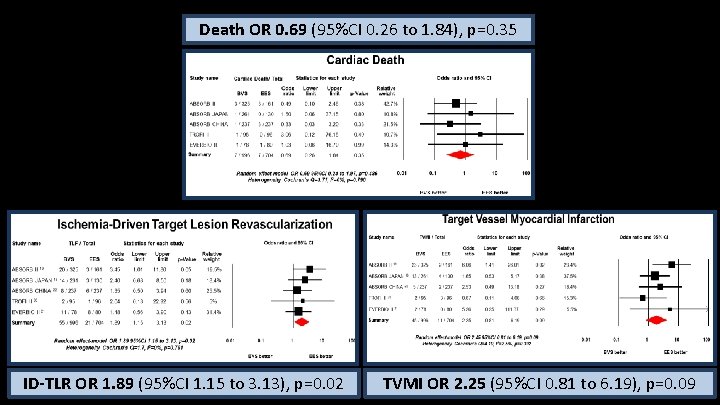
Death OR 0. 69 (95%CI 0. 26 to 1. 84), p=0. 35 ID-TLR OR 1. 89 (95%CI 1. 15 to 3. 13), p=0. 02 TVMI OR 2. 25 (95%CI 0. 81 to 6. 19), p=0. 09

Limitations • Lack of individual patient-level data. • The impact of intravascular imaging-guided PCI could not be assessed in this cohort, given the limited number of patients undergoing imaging-guided BVS implantation and the lack of prespecific intravascular ultrasound (IVUS)/OCT protocol for PCI guidance. • Even though we included all the studies available with long-term follow-up, the sample size of 1730 patients is still underpowered to detect differences in infrequent events such as DT

CONCLUSIONS • Compared with EES, the use of Absorb BVS was associated with a higher rate of DT and a trend towards higher risk of TLF driven by a higher risk of ID-TLR. • Very late scaffold thrombosis occurred in 1. 4% of the patients, the majority of these events occurred in the absence of DAPT.

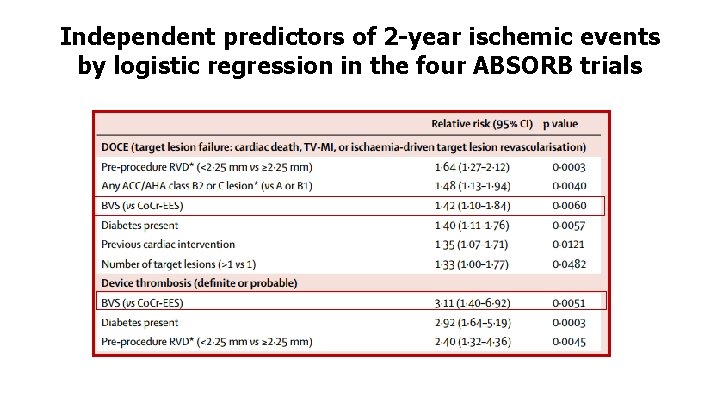
Independent predictors of 2 -year ischemic events by logistic regression in the four ABSORB trials
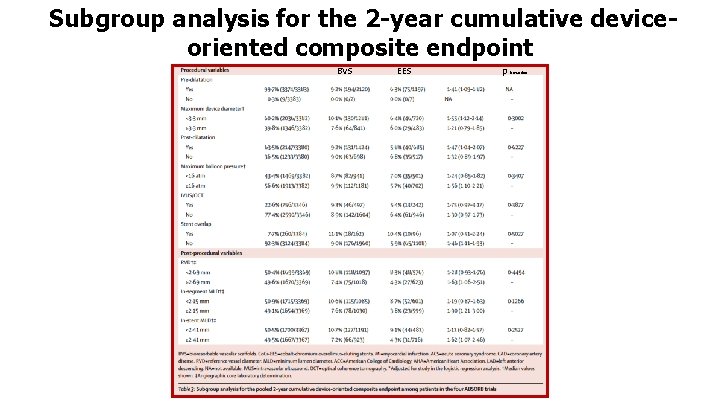
Subgroup analysis for the 2 -year cumulative deviceoriented composite endpoint BVS EES p interaction

Thank you
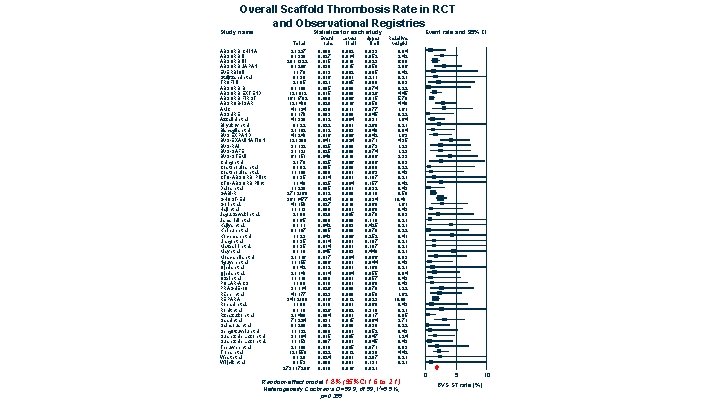
Overall Scaffold Thrombosis Rate in RCT and Observational Registries Study name Statistics for each study ABSORB CHINA ABSORB III ABSORB JAPAN EVERBIOII Stuijfzand et al TROFI II ABSORB B ABSORB EXTEND ABSORB FIRST ABSROB-ISAR AMC ASSURE Azzalini et al Biryukov et al Biscaglia et al BVS EXPAND BVS-EXAMINATION BVS-RAI BVS-SAFE BVS-STEMI Ching et al Costopoulos et al. CTO-ABSORB Pilot Dalos et al GABI-R GHOST-EU Gori et al. Haji et al Jaguszewski et al. Jamshidi et al Kajiya et al. Khripun et al Kochman et al Liang et al Mattesini et al. May et al Moscarella et al Nguyen et al Ojeda et al. Özel et al POLAR-ACS PRAGUE-19 Räber et al REPARA Robaei et al. Rohit et al Rzeszutko et al Saad et al Sainsous et al Sengottuvelu et al Suarez de Lezo et al. Teeuwen et al Trobs et al West et al Wójcik et al Total 2 / 237 9 / 329 20 / 1322 8 / 266 1 / 78 0 / 30 2 / 95 0 / 100 12 / 812 16 / 1702 12 / 419 4 / 134 0 / 170 4 / 339 0 / 22 2 / 162 4 / 249 12 / 290 3 / 122 3 / 121 6 / 151 2 / 79 0 / 92 1 / 108 0 / 35 1 / 40 1 / 220 27 / 2168 36 / 1477 4 / 150 1 / 113 2 / 98 0 / 65 0 / 11 0 / 107 1 / 23 0 / 35 0 / 10 2 / 116 1 / 155 0 / 42 2 / 140 1 / 119 1 / 98 3 / 114 4 / 177 34 / 2100 1 / 99 0 / 18 2 / 468 7 / 224 0 / 200 1 / 132 3 / 194 1 / 153 2 / 108 12 / 550 0 / 20 0 / 53 273 / 17296 Event rate 0. 008 0. 027 0. 015 0. 030 0. 013 0. 016 0. 021 0. 005 0. 015 0. 009 0. 029 0. 030 0. 003 0. 012 0. 022 0. 016 0. 041 0. 025 0. 040 0. 025 0. 009 0. 014 0. 025 0. 005 0. 012 0. 024 0. 027 0. 009 0. 020 0. 008 0. 042 0. 005 0. 043 0. 014 0. 045 0. 017 0. 006 0. 012 0. 014 0. 008 0. 010 0. 026 0. 023 0. 016 0. 010 0. 026 0. 004 0. 031 0. 002 0. 008 0. 015 0. 007 0. 019 0. 022 0. 024 0. 009 0. 018 Lower limit 0. 002 0. 014 0. 010 0. 015 0. 002 0. 001 0. 005 0. 000 0. 008 0. 006 0. 011 0. 000 0. 004 0. 001 0. 003 0. 006 0. 024 0. 008 0. 018 0. 006 0. 000 0. 001 0. 004 0. 001 0. 009 0. 018 0. 010 0. 001 0. 005 0. 000 0. 003 0. 000 0. 006 0. 001 0. 003 0. 004 0. 001 0. 009 0. 012 0. 001 0. 002 0. 001 0. 015 0. 000 0. 001 0. 005 0. 012 0. 001 0. 016 Upper limit 0. 033 0. 052 0. 023 0. 059 0. 085 0. 211 0. 080 0. 074 0. 026 0. 015 0. 050 0. 077 0. 045 0. 031 0. 268 0. 042 0. 071 0. 073 0. 074 0. 086 0. 096 0. 080 0. 063 0. 187 0. 157 0. 032 0. 018 0. 034 0. 069 0. 060 0. 078 0. 110 0. 425 0. 070 0. 252 0. 187 0. 448 0. 066 0. 044 0. 160 0. 055 0. 057 0. 069 0. 078 0. 059 0. 023 0. 068 0. 310 0. 017 0. 064 0. 038 0. 052 0. 047 0. 045 0. 071 0. 038 0. 287 0. 131 0. 021 Event rate and 95% CI Relative weight 0. 84 3. 42 6. 80 3. 06 0. 42 0. 21 0. 83 0. 22 4. 45 5. 70 4. 40 1. 61 0. 22 1. 64 0. 21 0. 84 1. 63 4. 35 1. 23 2. 33 0. 83 0. 22 0. 43 0. 21 0. 42 0. 43 8. 58 10. 43 1. 61 0. 43 0. 83 0. 21 0. 22 0. 41 0. 21 0. 83 0. 43 0. 21 0. 84 0. 43 1. 22 1. 62 10. 09 0. 43 0. 21 0. 85 2. 71 0. 22 0. 43 1. 24 0. 43 0. 83 4. 42 0. 21 Random-effect model 1. 8% (95%CI 1. 6 to 2. 1) Heterogeneity Cochran’s Q=59. 9, df 59, I 2=5. 5%, p=0. 355 0 5 BVS ST rate (%) 10
- Slides: 20