Last Offices Care For Patients During The COVID
















- Slides: 30

Last Offices Care For Patients During The COVID - 19 Outbreak

Aims Last Offices • This is the last procedure a nurse performs for his/her patient. • This set of slides is to assist with the last offices procedure that is to be undertaken during the COVID 19 outbreak.

Privacy and Dignity During Last Offices • It is imperative that the deceased is treated with privacy, dignity and compassion throughout the process of last offices. • Remember to maintain privacy within the bedroom area. • This is a difficult procedure for nursing staff to undertake and only staff who are comfortable should take part. • The procedure should be led by a registered nurse. • Staff often find talking to the deceased, personalizes during the procedure.

Inform Relatives, Other Patients & Staff • Relatives that are with the deceased when they pass away may wish to spend some time with their relative alone. However, they must remain in full PPE and understand that they will need to isolate for 14 days following the visit. • If relatives are being informed over the telephone, remember that they may be distressed by the news (see next slide). • Any special wishes of the family to be carried out e. g. locks of hair collection. • Other patients and staff will need to be supported with the loss in a debrief.

Informing Relatives - Prepare yourself. Be familiar with clinical details. Be in a quiet place, no interruptions. Do you have support from a colleague? The telephone call should be made as soon as possible after the death. Clearly identify yourself, ask who you are speaking to and if they are with anyone else. Phrases such as “I have sad news” are helpful. Use clear language say “dead” or “died” not euphemisms like “passed away” or “expired. ” Be empathic and allow times for questions. Explain next steps. When call is finished look after yourself get support if appropriate.

Inform Relatives, Other Patients & Staff contd. - Staff should ensure that they inform: - Matron Service manager Operations Manager Consultant

Bereavement Support Bereavement support for anyone who needs it can be found here; • National bereavement support line – 0800 0246 121 • CRUSE bereavement care national helpline – 0808 1677 • NHS Bereavement Helpline 0800 2600 400 • The Spiritual Care Team as a source for support for people who are bereaved. Referral Number 0161 357 1769 • Trust bereavement practitioner – Paula Smith – paula. smith@gmmh. nhs. uk


Documentation • Paris notes – completion of individual plan of care for end of life • Datix completion • Death certificate/Notification of death – Is completed by a medic this need to detail the deceased’s COVID – 19 status, e. g. positive or pending results. This must be placed in the body bag or given to the funeral director. • Statement of intent – This goes with body to the funeral director • DNAR and a copy of the statement of intent - should be filed away by ward admin/clerk

Documentation Continued • Detained Patients – CQC statutory notification of death form must be completed and returned. Ward completes datix and informs MHA team end legal status. • For Restricted Patients – Same as above but for patient in hospital , RC must notify the Mo. J and provide reason for death if known. For patient subject to conditional discharge, the RC or social supervisor can provide this information. • If the deceased was subject to Deprivation of Liberty Safeguards authorization, the coroner will only need to be informed if the death was from unnatural causes or was unexpected. • Jewellery: Staff should ensure that, Prior to death ask the family/next of kin what jewellery they wish the deceased to continue wearing and record the information. Any rings must be taped into place.

Preparing for Last Offices Patients positive for COVID - 19 WITH NO aerosol generated procedures: Patients positive for COVID - 19 WITH aerosol generated procedures: Staff must don full level 2 PPE • Apron • Gloves • FFP 2 R mask Staff must don full level 3 PPE • Full suit • Gloves • FFP 3 R mask (only staff that have been fit tested)

Hand Hygiene • Hand hygiene is essential to reduce the transmission of infection in health and other care settings and is a critical element of standard infection control precautions (SICP’s). • Whilst carrying out the last office procedure, staff should ensure that they maintain proper hand hygiene • Hand hygiene must be performed immediately before and after every direct episode of contact with the deceased

Before performing hand hygiene: • Expose forearms (bare below the elbows); • Remove all hand wrist jewellery (a single, plain metal finger ring is permitted but should be removed (or moved up) during hand hygiene); • Ensure finger nails are clean, short and that artificial nails or nail products are not worn; • Cover all cuts or abrasions with a waterproof dressing.

Equipment required • • • Wound dressings Tape Gloves Aprons Absorbent pads/incontinence pad Any spigots that are required Orange clinical waste bags Washing equipment Towels Comb Shroud or sheets

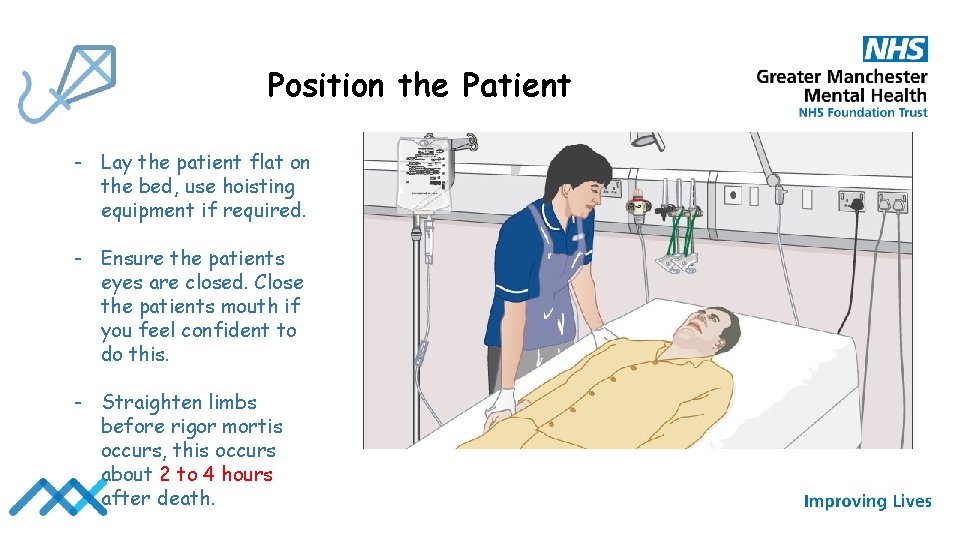
Position the Patient - Lay the patient flat on the bed, use hoisting equipment if required. - Ensure the patients eyes are closed. Close the patients mouth if you feel confident to do this. - Straighten limbs before rigor mortis occurs, this occurs about 2 to 4 hours after death.

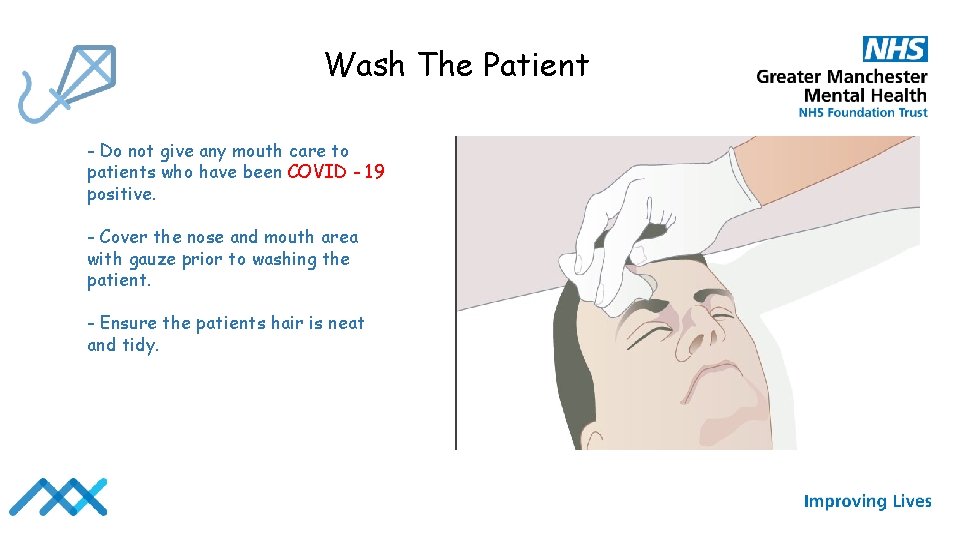
Wash The Patient - Do not give any mouth care to patients who have been COVID - 19 positive. - Cover the nose and mouth area with gauze prior to washing the patient. - Ensure the patients hair is neat and tidy.

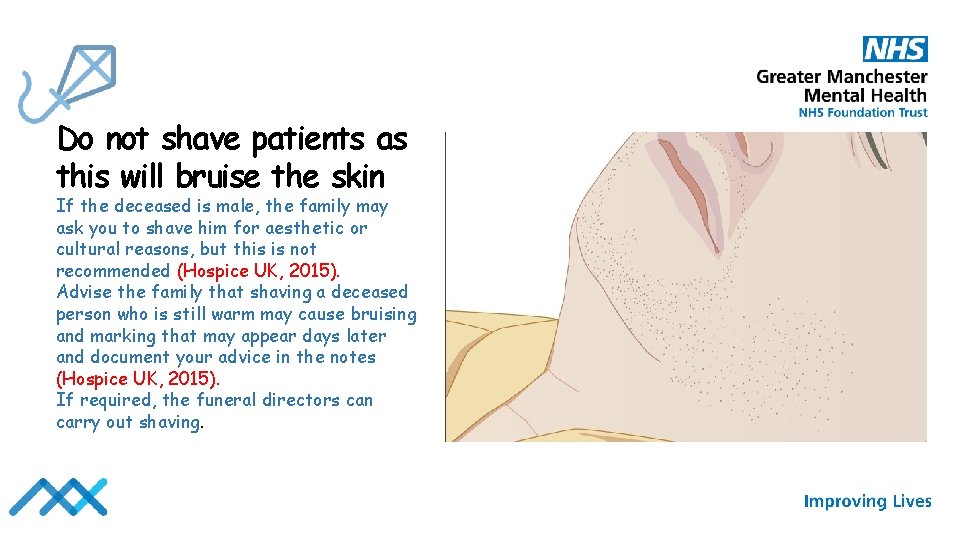
Do not shave patients as this will bruise the skin If the deceased is male, the family may ask you to shave him for aesthetic or cultural reasons, but this is not recommended (Hospice UK, 2015). Advise the family that shaving a deceased person who is still warm may cause bruising and marking that may appear days later and document your advice in the notes (Hospice UK, 2015). If required, the funeral directors can carry out shaving.

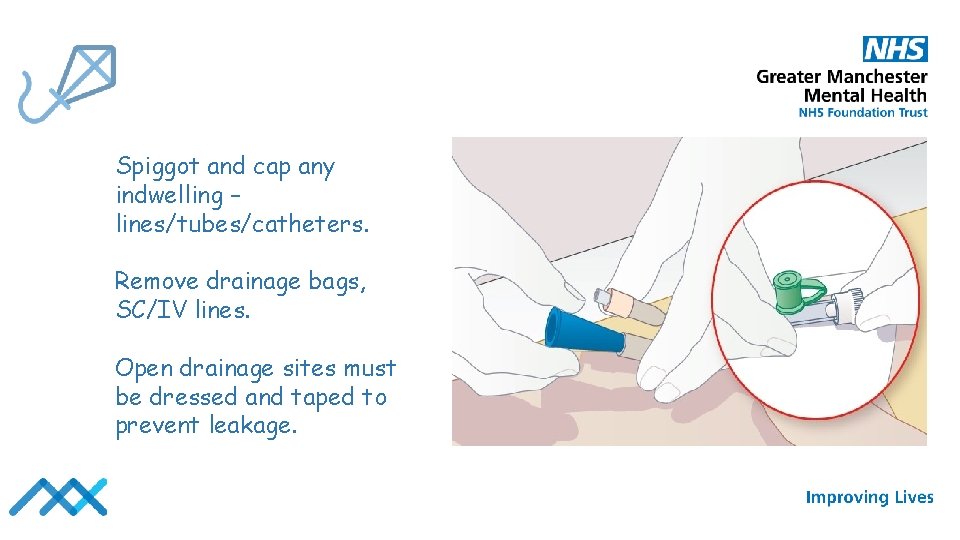
Spiggot and cap any indwelling – lines/tubes/catheters. Remove drainage bags, SC/IV lines. Open drainage sites must be dressed and taped to prevent leakage.

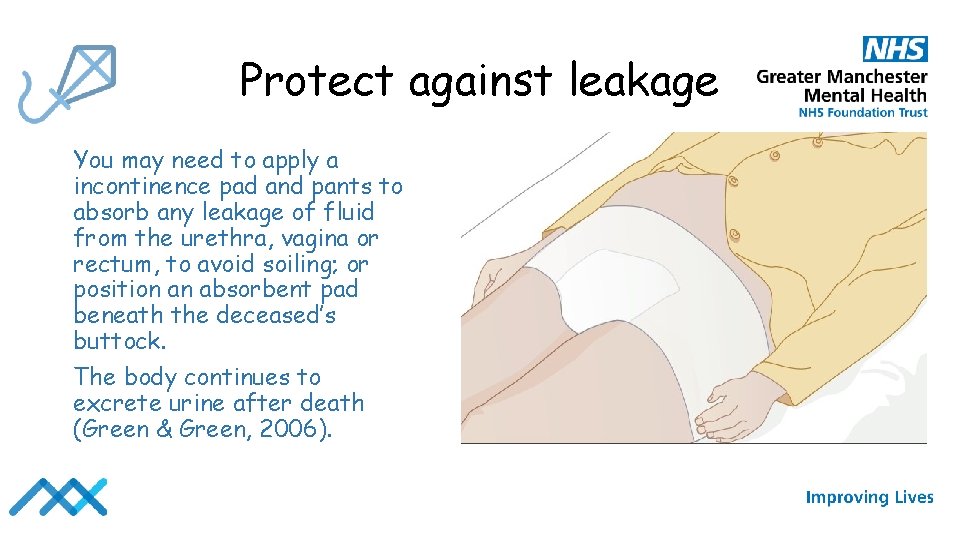
Protect against leakage You may need to apply a incontinence pad and pants to absorb any leakage of fluid from the urethra, vagina or rectum, to avoid soiling; or position an absorbent pad beneath the deceased’s buttock. The body continues to excrete urine after death (Green & Green, 2006).

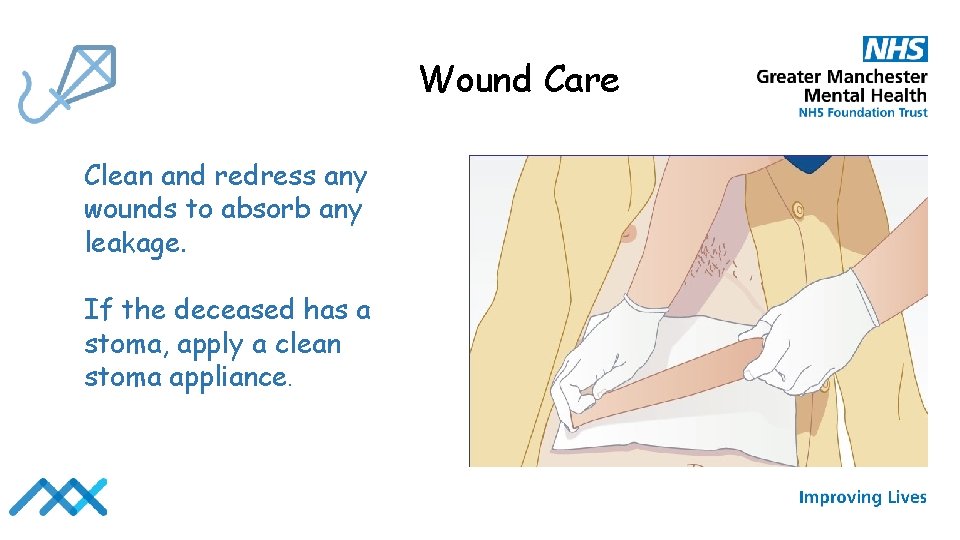
Wound Care Clean and redress any wounds to absorb any leakage. If the deceased has a stoma, apply a clean stoma appliance.

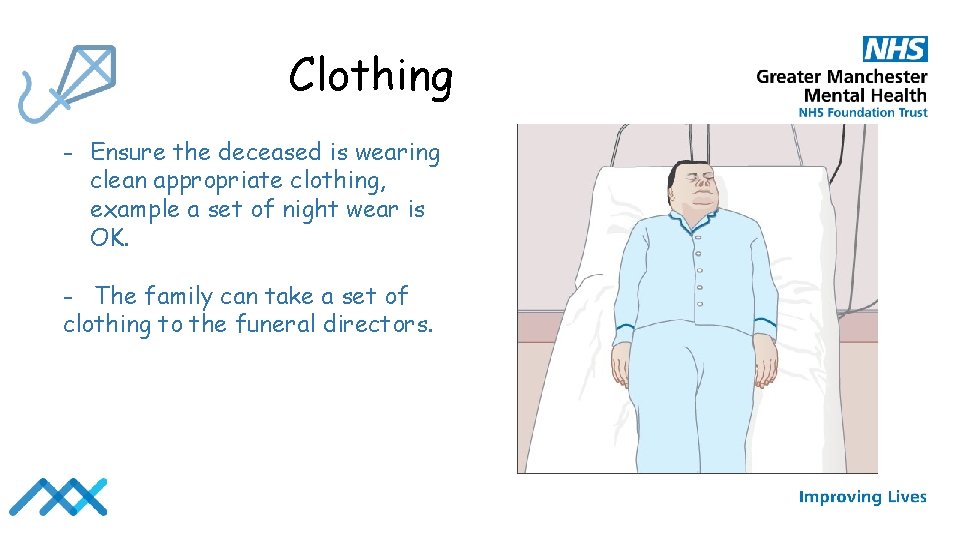
Clothing - Ensure the deceased is wearing clean appropriate clothing, example a set of night wear is OK. - The family can take a set of clothing to the funeral directors.

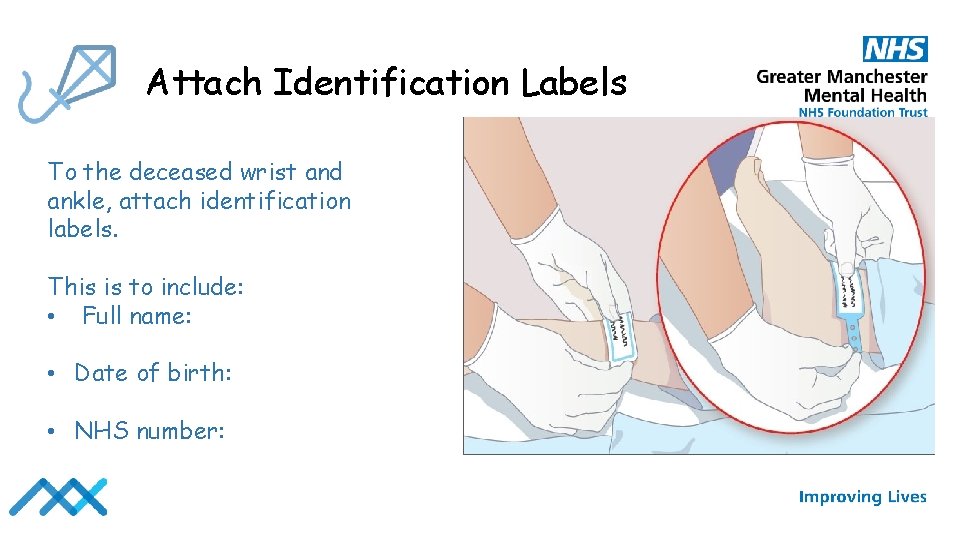
Attach Identification Labels To the deceased wrist and ankle, attach identification labels. This is to include: • Full name: • Date of birth: • NHS number:

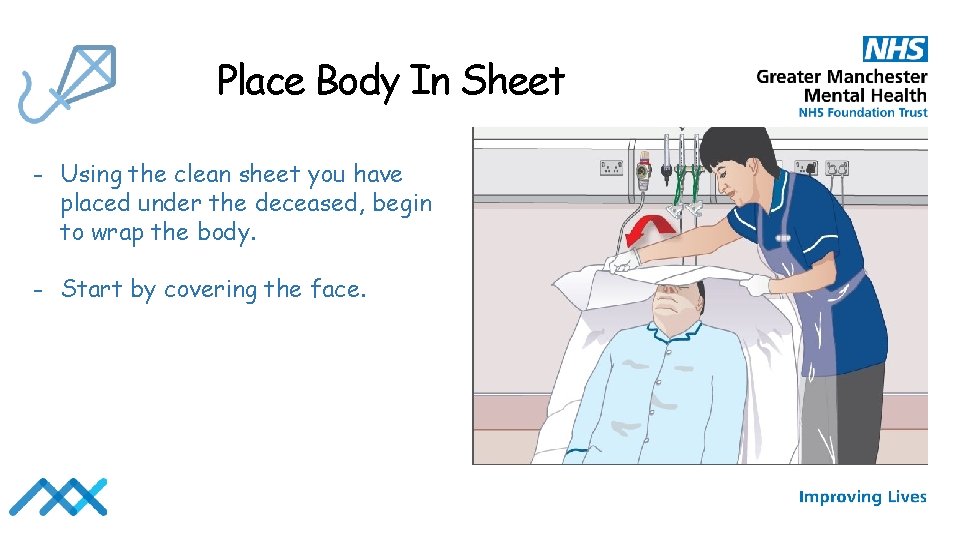
Place Body In Sheet - Using the clean sheet you have placed under the deceased, begin to wrap the body. - Start by covering the face.

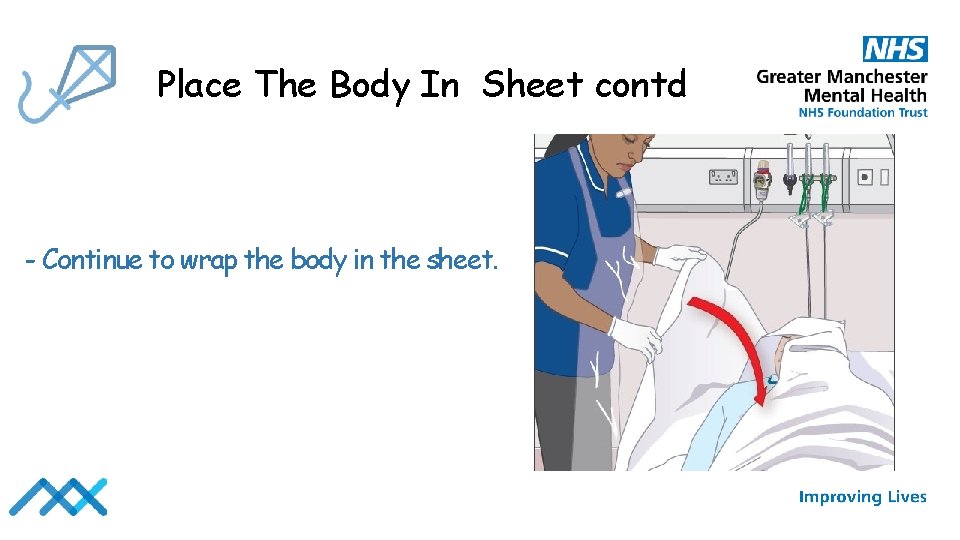
Place The Body In Sheet contd - Continue to wrap the body in the sheet.

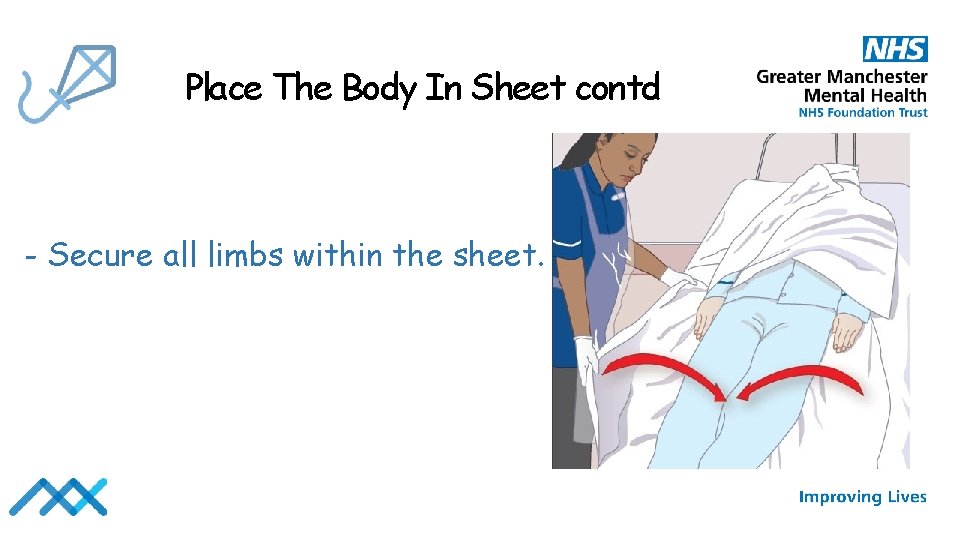
Place The Body In Sheet contd - Secure all limbs within the sheet.

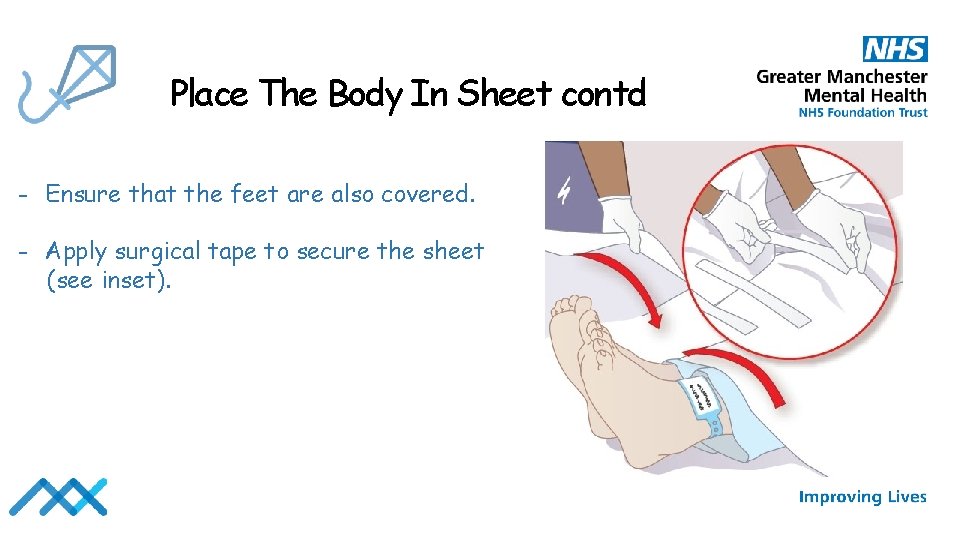
Place The Body In Sheet contd - Ensure that the feet are also covered. - Apply surgical tape to secure the sheet (see inset).

Funeral Directors - Prior to the deceased passing away the family will need to be asked about which funeral directors they wish to use. - Whilst waiting for the funeral directors ensure the body remains private from the rest of the ward. On attendance: - The funeral directors will bring two body bags to put the deceased in. - Please assist the funeral directors with the best way to remove the deceased form the building. Ensuring that other patients are not in the area.

Room Cleaning - After removal of the body, ensure to keep the room closed off. - Contact the heavy duty team to cleanse the room. - The room must be empty for two hours prior to the heavy duty cleaning team going in. - Once the heavy duty clean has taken place the room can be used again immediately.

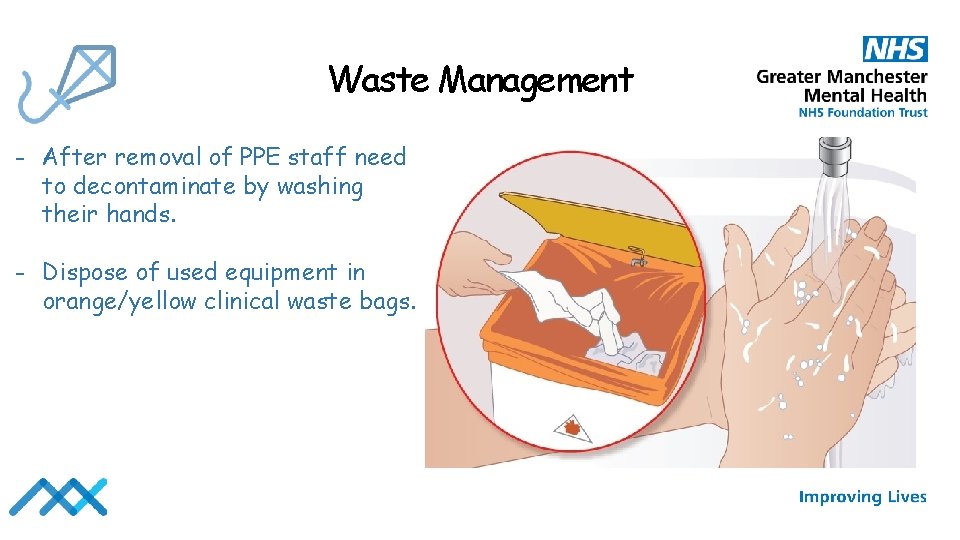
Waste Management - After removal of PPE staff need to decontaminate by washing their hands. - Dispose of used equipment in orange/yellow clinical waste bags.

Patient Property • If a patient has passed away in clothing that relatives wish to take home, then these must be washed at 60 degrees before they can be given to family. • Remember to document each item returned to the family.