Labour analgesia Dr S Parthasarathy MD DA DNB

Labour analgesia Dr. S. Parthasarathy MD. , DA. , DNB, MD (Acu), Dip. Diab. DCA, Dip. Software statistics, Ph. D(physiology) Mahatma Gandhi Medical College and Research Institute, Puducherry, India

But what is history ? ? • The era of obstetric anaesthesia began with James Young Simpson, when he administered ether to a woman with a deformed pelvis during childbirth. • His concept of “etherization of labour” was strongly condemned by critics • Religion condemned !!

• 1853, when John Snow administered chloroform to Britain’s Queen Victoria during the birth of her eighth child, Prince Leopold • In 1950 s – neuraxial techniques came into existence

• The International Association for the Study of Pain (IASP) declared 2007– 2008 as the • ’’Global Year against Pain in Women - Real Women, Real Pain. ” • Still only 60 % accept or opt for epidurals in UK !!

• What about India ? ?

Awareness of labour analgesia Not a single participant knew that the delivery is possible without suffering from labour pains; (1. 5%) were of the opinion that it was impossible; 196 (98%) did not know whether it is possible or not. An equal number had no idea about labour analgesia • 200 rural pregnant women • Anaesthesia, Pain & Intensive Care

• Do we need it ? ? • Is there a necessity? ?
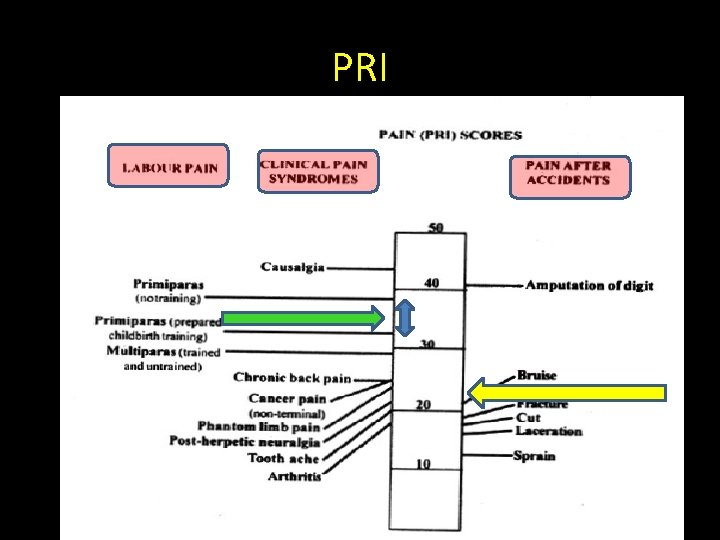
PRI
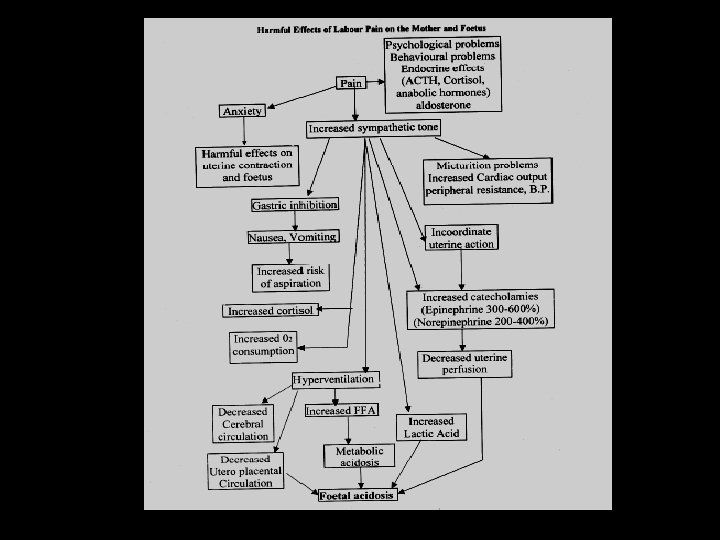

We need some form of labour analgesia • So we need it !!
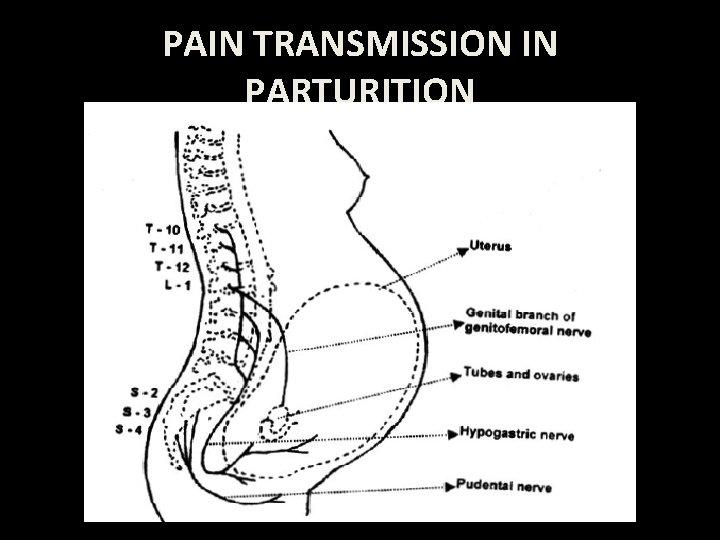
PAIN TRANSMISSION IN PARTURITION
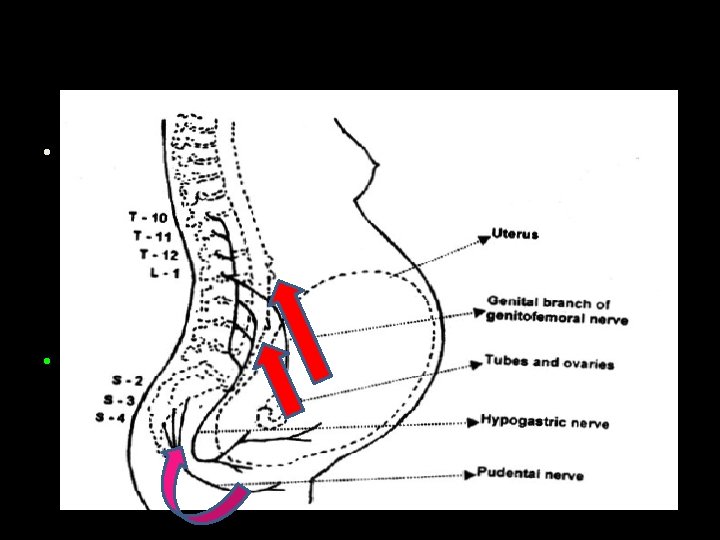
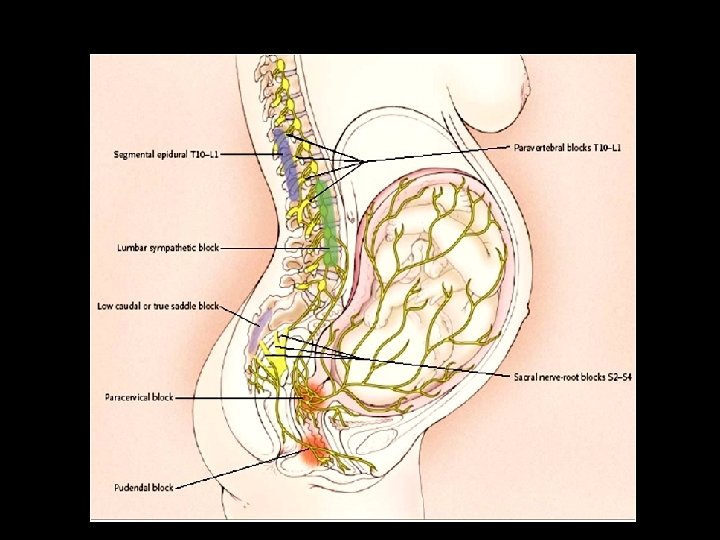
• Visceral afferent pain fibers from the uterus, cervix, and upper vagina form the cervical plexus and enter the spinal cord at the T 10–L 1 levels. The visceral afferent fibers also enter the sympathetic chain at L 2 and L 3 levels. • lower vagina, vulva, and perineum. signals are conveyed via the S 2–S 4 spinal nerve roots that form the pudendal nerve

Hence a contradiction • First stage ---- T 10 – L 3 • Second stage --- S 2, S 3, S 4

Now how to proceed • Give drugs – route ? ? Pharmacological • Something other than drugs Non pharmacological

Nonpharmacological

Non pharmacological Lamaze in 1958 The training starts from six weeks During labour Deep breath during contraction Relax Physician talks – electromyographic biofeedback with lamaze √ √ • Davidson hypnosis better than preparation alone • • •
• TENS • Four electrodes • Augustinson • 44% good relief 44 % acceptable 12 % nil
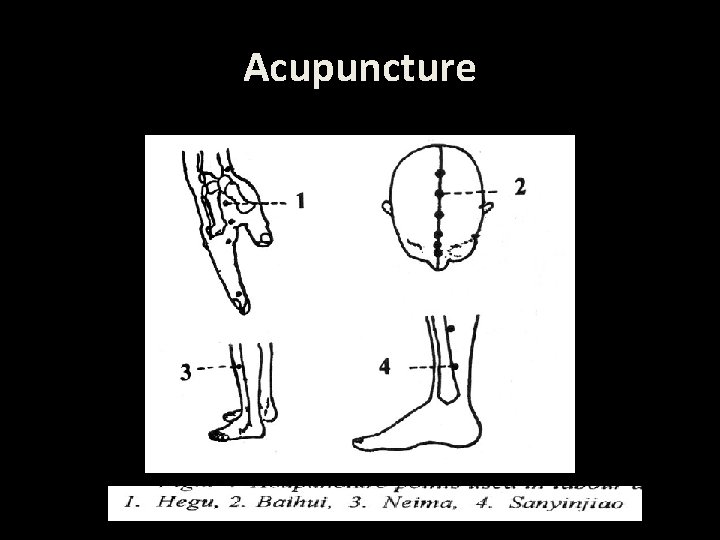
Acupuncture

Acupuncture • • Effective relief Contractions become more regularized Reduced oxytocin doses But wires Time Machinery Interference with fetal monitoring ? ?

Position • Vertical position • Squatting – no proper studies • Ambulating ? ? • Ambulating patients have shorter and less painful labour or vice versa ? ?
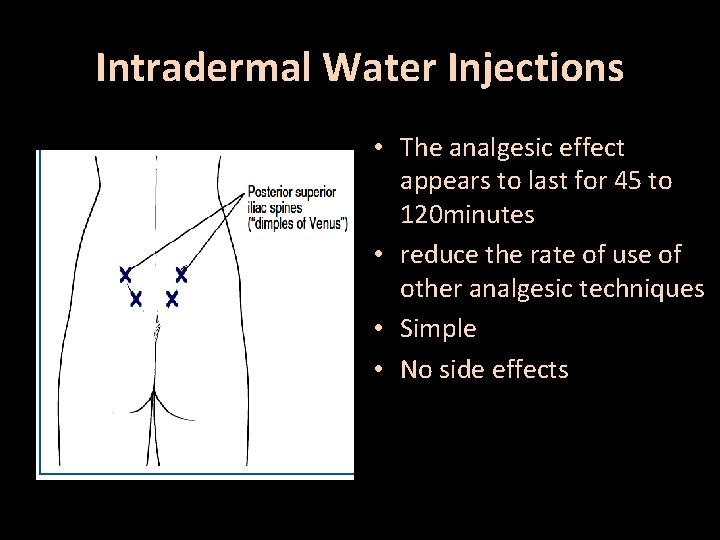
Intradermal Water Injections • The analgesic effect appears to last for 45 to 120 minutes • reduce the rate of use of other analgesic techniques • Simple • No side effects

Some one may criticize ? ? But no one stops a patient who is on intrathecal opioids to have hydrotherpay and intradermal water injection also Isnt it ? ?

Pharmacological • • Narcotics IM, SC or ( IV – more predictable, faster onset) Pethidine – 1947 The usual dose is 50 to 100 mg intramuscularly, which can be repeated every 4 hours. onset of analgesia occurs in 10 to 15 minutes, 45 minutes - reach peak effect. The duration -- 2 to 3 hours.

Other opioids • • Morphine Diamorphine Meptazinol Fentanyl , alfentanil, remifentanyl Tramadol Nalbuphine Butorphanol Pentazocine

Randomized studies • • Significant relief Easy to administer Staff can manage But studies reveal more percentage needed neonatal resuscitation ( morphine ? ? ) • PCA - √ - better in less dosage , more analgesia and less side effects ( especially fentanyl)
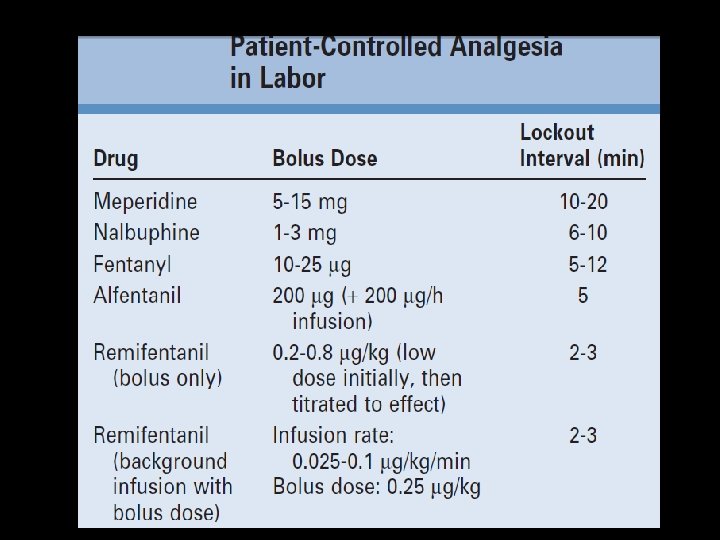

A lot of studies • epidural analgesia is superior to remifentanil PCA, they also postulated that high maternal satisfaction with intravenous PCA may be the result of factors other than the degree of analgesia produced • What ? Is it so ? ? • IV paracetomol • IV ketamine ( 0. 2 mg/Kg) – 25 mg IV during crowning !!

Benzodiazepines ? ? Analgesia ? ? Amnesia !!

INHALATIONAL ANALGESIA • • Nitrous oxide as premixed entonox 50 % Separates at 7 degress c Safety demand valve Inhales at each contraction Drowsy patient Stops Effective. Crosses but safe to neonate Equipment ? ? Resurgence of entonox !!

INHALATIONAL ANALGESIA • Inhaled methoxy flurane with the help of a cardiff inhaler was practiced with conc. of 0. 2 % • Enflurane 0. 5% MAC • Isoflurane _ ? Less uterine atony • Sevoflurane – 0. 7 MAC – good • Desflurane – cost and irritablity remains with efficiency less than nitrous oxide • Equipment, monitoring, aspiration risk , amnesia, timing ? ?

Evidence based medicine • Systemic pethidine • Remifentanyl PCA • All agents in carefully monitored doses

Neuraxial analgesia • • Spinal LA ? Opioids Continuous epidural CSEA Caudal Double catheter Continuous spinal Lumbar sympathetic , paracervical Pudendal ( nerve blocks )

Indications for epidural • • Pre eclampsia/hypertensive disease Prolonged labour Two or more babies in utero Anticipated instrumental delivery Diabetes Mellitus Breech presentation for vaginal delivery Significant respiratory disease

Contraindications • No CTG tracing or inadequate CTG tracing e. g. loss of contact • Declined by the woman • Inadequate midwifery staffing levels. & • Otherwise similar as for other epidurals

Epidural technique • Prepare , position , hydrate 500 ml of RL • Insert catheter – initiate dosage dilute local anaesthetics in 5 ml increments with lipid soluble opioid • TEST dose • Assess levels , monitor vitals • When ? ? • Effective contractions 4 cm dilation in primi
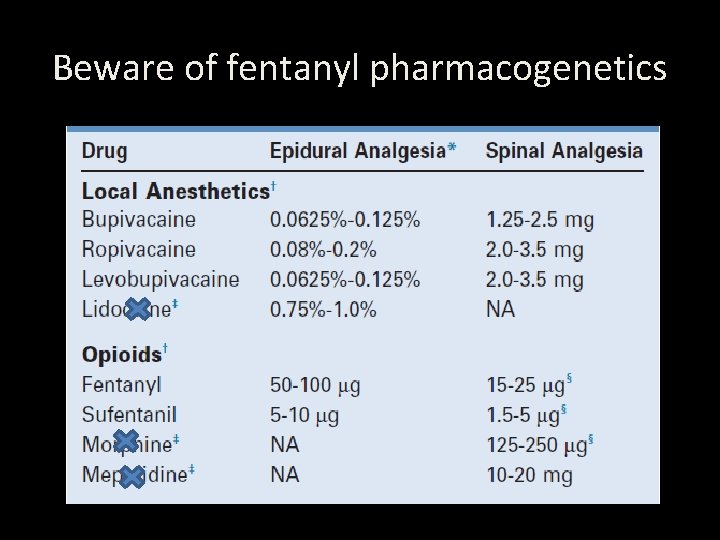
Beware of fentanyl pharmacogenetics

• Lidocaine, morphine, and meperidine are not commonly used for labor analgesia because of their short duration of action (lidocaine), long latency (morphine), and high incidence of nausea and vomiting (morphine and pethidine). Epidural block is the most effective and least depressant (pharmacologic option) allowing for an alert, participating mother

Opioids • • • Inadequate analgesics used alone Synergistic with local anesthetics Speedy onset of analgesia Improves quality of analgesia Permits use of very dilute LA solutions Help relieve persistent perineal pain and unblocked segments

I have initiated – maintain ? ?
? Intermittent boluses • Continuous infusion • PCEA

Intermittent • Epidural catch up phenomenon • Intermittent dose delayed • Severe pain • Influence the next dose

Infusion • Bupivacaine 10 ml /hour • Bupivacaine 12 ml/ hour with 2. 5 mic/ml fentanyl • Ropivacaine 10 ml of 0. 25 % • Levo bupi + fentanyl • Lignocaine 0. 75 %

Double catheter technique • Cleland • T 11 catheter 6 ml of dilute solution of LA • Caudal catheter - 5 ml for stage 2
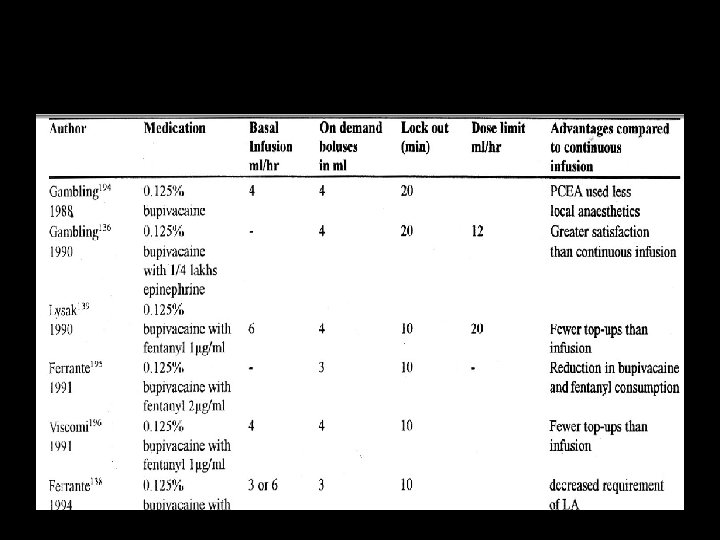
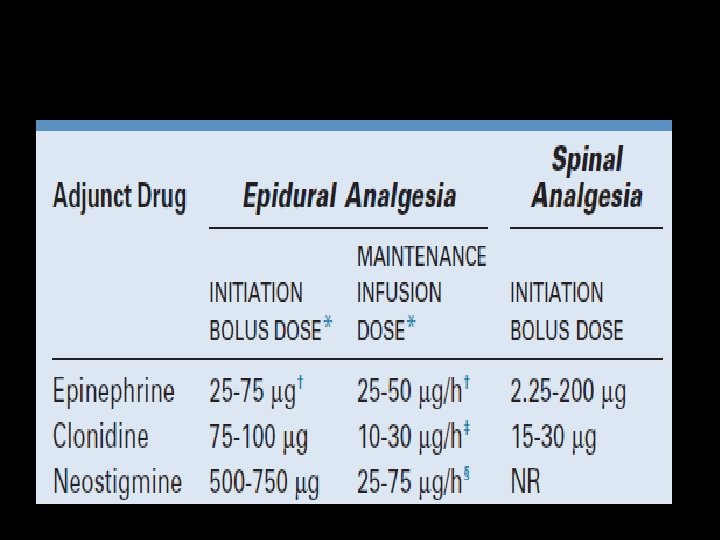

Any problem with epidural ? ?

2 – 20 rule • Problem with neuraxial anaesthesia • 2 hour – dystocia in first stage • 20 min dystocia in second stage

CSEA • CSEA as a routine and are indicated only in certain specific situations, • like very early stage of labour where local anaesthetics are avoided, • advanced stages of labour where rapid analgesia is desirable • difficult epidurals as CSEA reduces the failure rate of epidurals.

Computer integrated PCEA • Lim et al. reported another adaptation of the epidural delivery pump technology. Their centre has developed a computer-integrated PCEA (CI-PCEA) that controls background infusion rates depending on the previous hour’s demand boluses.

Walking epidural • THE IDEAL LABOUR ANALGESIC SHOULD GIVE A RESTED PARTURIENT THE ENERGY, STRENGTH AND SENSATION TO PERFORM EXPULSIVE EFFORTS AT THE TIME OF DELIVERY. • TO ACHIEVE THESE GOALS, RECENT DEVELOPMENTS HAVE FACILITATED MATERNAL AMBULATION WHILE RECEIVING EFFECTIVE REGIONAL ANALGESIA.

Why walk ? ? The upright posture helps shorten the duration of labour by walking Mothers who walk during labour had reduced duration and operative delivery rate. Weight of fetus would dilate the cervix Aorto caval compression ? ? • Vertical position !!

Walking epidural • • dilute local anaesthetics with opioids Motor block check No hypotension Supervised trial walk • Then allow

Spinal • • Bupivacaine 2. 5 mg with an opioid Faster onset Effective relief Prolong ? ? Motor block ? ? Hypotension and fetal effects ? ? Micro catheters

8 cm dilation. . Comes and gives what ? ?

Some doubts about epidurals

Increased rate of operative and instrumental delivery: Is epidural the cause ? ? • The Cochrane Database Systemic trials have emphasized that epidural analgesia had no statistically significant impact on the risk of caesarean section. • In two different metaanalyses of randomized trials, comparing patients with and without epidural, caesarean delivery was clearly not associated with epidural analgesia

Question 2 : Epidural taken early vs. late ? ? • • 4 – 5 cm no no 2 -3 cm no no 6 cm !! 4 -5 – once thought • there is no need to wait arbitrarily till the cervical dilation has reached 4– 5 cm, and endorsed a statement that “Maternal request is a sufficient indication for pain relief in labour. ” (ACOG guidelines )

Question 3 : Early vs. delayed pushing • The Pushing Early or Pushing Late with Epidural (PEOPLE) Study also supported delayed pushing for a better outcome

Withholding the epidural top-up in the second stage • No • Instrumental deliveries are not increased • But • Inadequate pain relief remains

Vaginal birth after caesarean and epidural • Task force guidelines 2007 jointly issued by the ASA and the Society of Obstetric Anaesthesiologists and Perinatologists (SOAP) recommend neuraxial techniques being offered to patients attempting vaginal birth after previous caesarean delivery • Do it early • Use it for post pain if needed

Epidural and breastfeeding • • • No impact No proper studies Go ahead Backache and epidural No significant change

Backache and epidural ? ? • In two recent randomized trials, there were no significant differences in the incidence of long-term back pain between women who received epidural pain relief and women who received other forms of pain relief

Epidural and baby • local anesthetics administered as components of epidural analgesia were sometimes associated with minor, transient effects on neonatal behavior • Intrathecal – very less effects • Beware of hypotension

Lumbar sympathetic block • 10 ml of 0. 5 % bupi with 1 in 2 lakh adrenaline each side for first stage followed by pudendal nerve block for second stage • Effective analgesia without hypotension and motor block • But technique ? ?
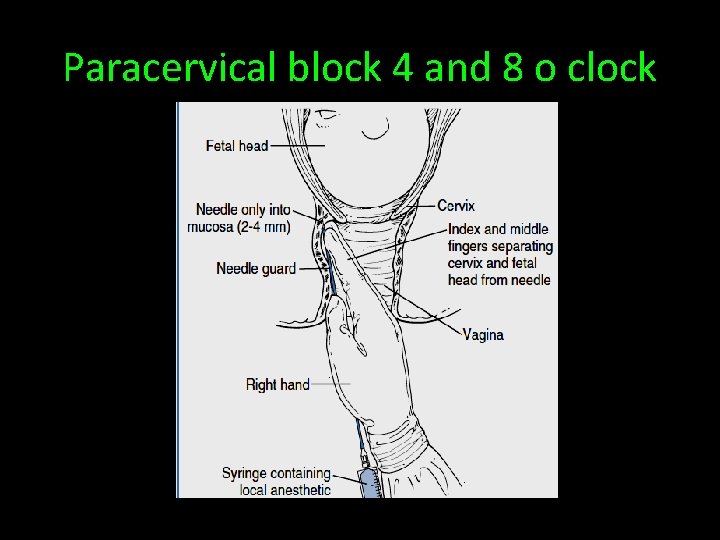
Paracervical block 4 and 8 o clock

PCB • The goal is to block transmission through the paracervicalganglion— • (Frankenhäuser’s ganglion)—which lies immediately lateral and posterior to the cervicouterine junction. • 50 - 75 % relief in primi first stage

Maternal complications

Fetal complications – bradycardia 110 or 120 !! // 0 - 70 % !! • • LA in the fetal scalp blood Uterine art. Constriction Stimulation of head Uterine activity • 5 – 10 minutes - betters without intervention.
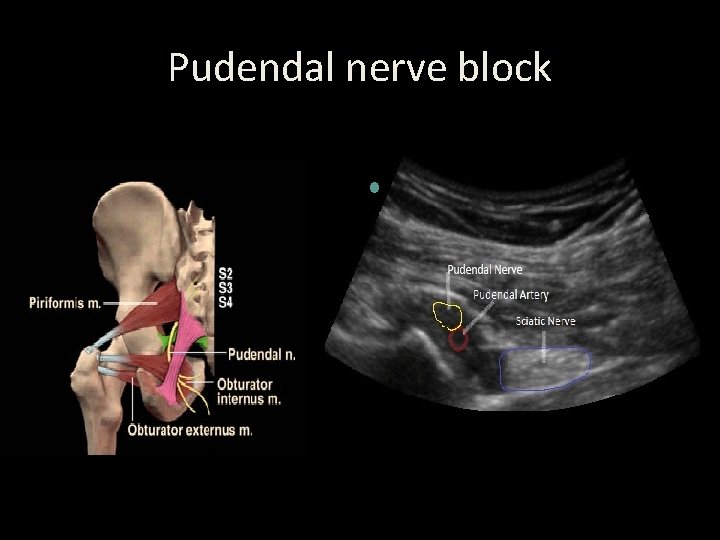
Pudendal nerve block
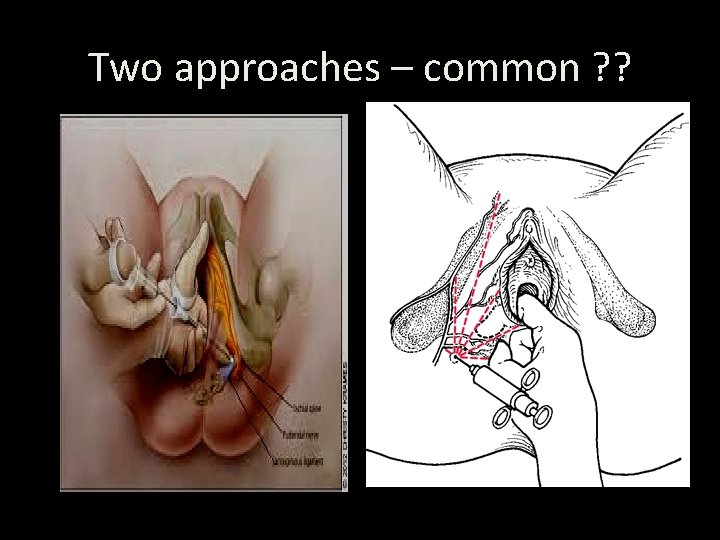
Two approaches – common ? ?

Iowa trumpet • Pudendal does nerve not block abolish sensation to the anterior part of the perineum, as the perineum is supplied by branches ilioinguinal of the and genitofemoral nerves.


Summary • • Labour analgesia – do we need ? Awareness Pathways Adverse effects of pain Techniques Lamaze Commonest opioid – Best technique


Appaa over !! – thank you all
- Slides: 77