LABORATORY ASSESMENT OF DM ANIK WIDIJANTI Clinical Pathology

LABORATORY ASSESMENT OF DM ANIK WIDIJANTI Clinical Pathology Department Saiful Anwar Hospital / Medical Faculty Brawijaya University MALANG

v. DM : Hyperglycemia because of deficient insulin secretion and / or abnormal insulin action v. USA : in 2002, 18, 2 million DM. v. Indonesia : prevalence DM increasing parallel with obesity. In 1981/1982 : 1. 5 - 1, 6 %. In 2001/2005 : 12. 5 - 14. 7 %

Type 1 DM Type 2 DM v. Destruction v. Secretory -cells v. Deficiency Insulin abs v. Gx acute defect insulin v. Insulin resistance v. Mixed Others Type DM v -cells defect v. Action defect v. Exocrine v. Endocrinopathy v. Drug induced v. Infections v. Others G. D. M DM in pregnancy
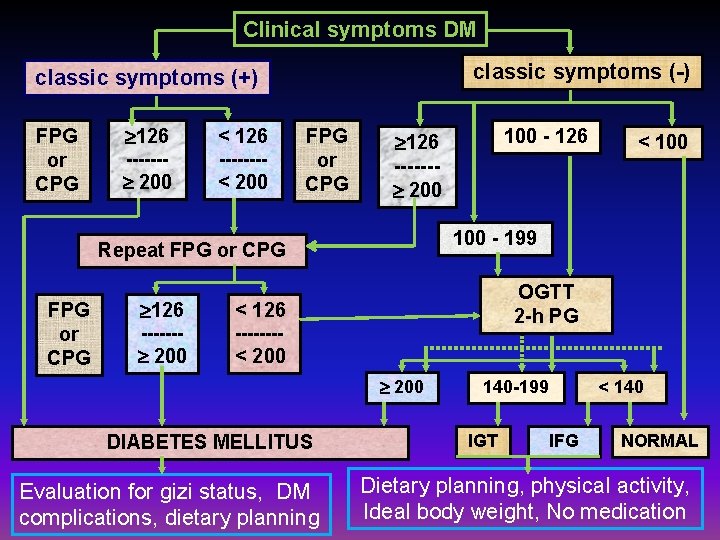
Clinical symptoms DM classic symptoms (-) classic symptoms (+) FPG or CPG 126 < 126 -------- 200 < 200 FPG or CPG 126 < 126 -------- 200 < 100 - 199 Repeat FPG or CPG 100 - 126 ------ 200 OGTT 2 -h PG < 200 DIABETES MELLITUS Evaluation for gizi status, DM complications, dietary planning 140 -199 IGT IFG < 140 NORMAL Dietary planning, physical activity, Ideal body weight, No medication
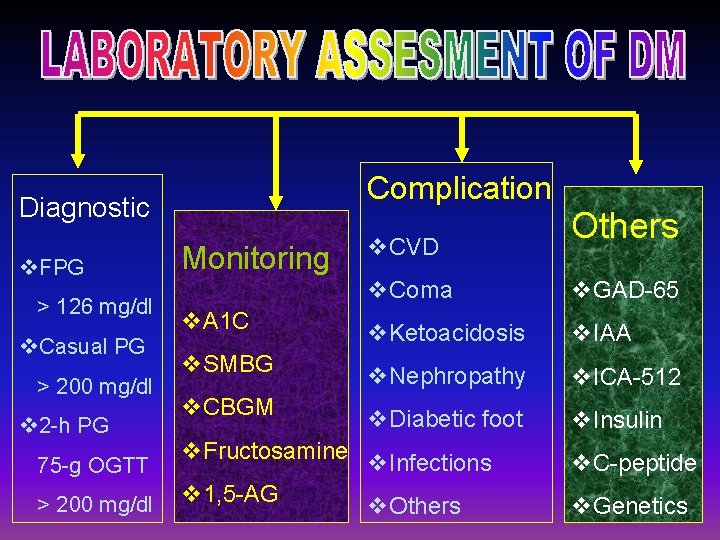
Complication Diagnostic v. FPG > 126 mg/dl v. Casual PG > 200 mg/dl v 2 -h PG 75 -g OGTT > 200 mg/dl Monitoring v. CVD Others v. Coma v. GAD-65 v. A 1 C v. Ketoacidosis v. IAA v. SMBG v. Nephropathy v. ICA-512 v. CBGM v. Diabetic foot v. Insulin v. Fructosamine v. Infections v 1, 5 -AG v. Others v. C-peptide v. Genetics
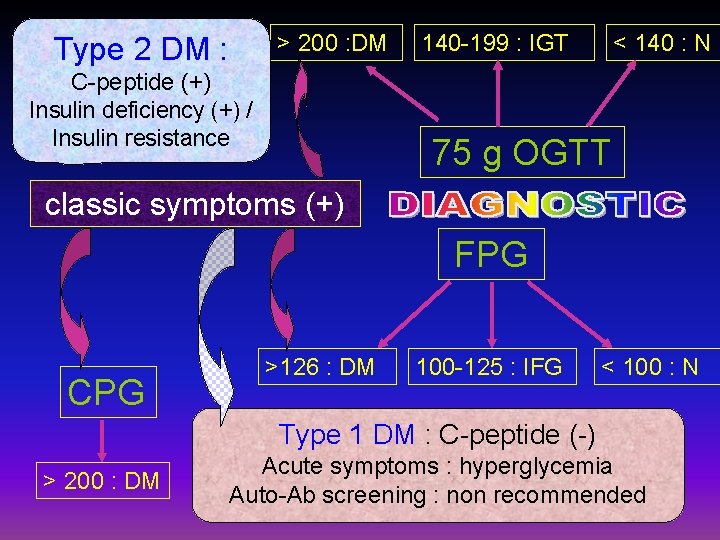
> 200 : DM Type 2 DM : C-peptide (+) Insulin deficiency (+) / Insulin resistance 140 -199 : IGT < 140 : N 75 g OGTT classic symptoms (+) FPG CPG >126 : DM 100 -125 : IFG < 100 : N Type 1 DM : C-peptide (-) > 200 : DM Acute symptoms : hyperglycemia Auto-Ab screening : non recommended

v 75 g OGTT more sensitive & specific than FPG v Poorly reproducible & difficult to perform in practice. v People who do not meet diagnostic criteria for DM by FPG, but would by the OGTT : A 1 C < 7. 0 % v OGTT not recommended for routine v Useful for further evaluation in whom DM is strongly suspected but normal FPG or IFG

Fasting PG : 8 -h 2 -h Plasma G Enzymatic not SMBG Enzymatic, not SMBG 75 -g glucose load + water ( maximum < 15 minute ) v. Normal v. I. F. G v. I. G. T v. D. M

v. Adults are BMI 25 kg/mm 2 + 1 ore more risk factors for DM v. Risk factors (-) : test begin no later than age 45 v. If normal, repeat testing at least at 3 -years v. Test either FPG or 2 -h 75 -g OGTT v. In pre-DM, treated other CVD risk factors

v Dx consistent with recommendations for adults v BMI 25 kg/mm 2 v Family history of type 2 DM in 1 st or 2 nd degree relative v Race / ethnicity v Insulin resistance or conditions associated v hypertension, dyslipidemia or PCOS v Maternal history of DM or GDM

v Screen GDM using risk factor analysis, use OGTT v Carry out GDM risk assessment at the 1 st prenatal visit v Screening / diagnosis at this stage of pregnancy use standard diagnostic testing of DM v Two approach may be followed for GDM screening at 2428 weeks v GDM should be screened for DM 6 -12 weeks post partum, & followed with screening for DM / pre-DM

v Screen GDM using risk factor analysis, use OGTT v Carry out GDM risk assessment at the 1 st prenatal visit v Screening / diagnosis at this stage of pregnancy use standard diagnostic testing of DM v Two approach may be followed for GDM screening at 2428 weeks v GDM should be screened for DM 6 -12 weeks post partum, & followed with screening for DM / pre-DM

v. Severe obese v. Prior history of GDM < or delivery of large for gestational-age infant v. Presence of glucosuria v. Diagnosis of PCOS v. Strongly family history of type 2 diabetes

Initial screening 50 -g OGTT 1 1 -h PG 130 mg/dl Identifies ~ 90 % GDM Two step approach 1 -h PG 140 mg/dl Identifies ~ 80 % GDM 100 -g OGTT 2 One step approach : high prevalence GDM 100 -g OGTT All woman at 24 -28 weeks gestation

Performed in the morning Overnight fast for at least 8 h GDM : 2 criteria Fasting : 95 mg/dl ( 5. 3 mmol/L ) 1 hour : 180 mg/dl ( 10. 0 mmol/L ) 2 hour : 155 mg/dl ( 8. 6 mmol/L ) 3 hour : 140 mg/dl ( 7. 8 mmol/L )
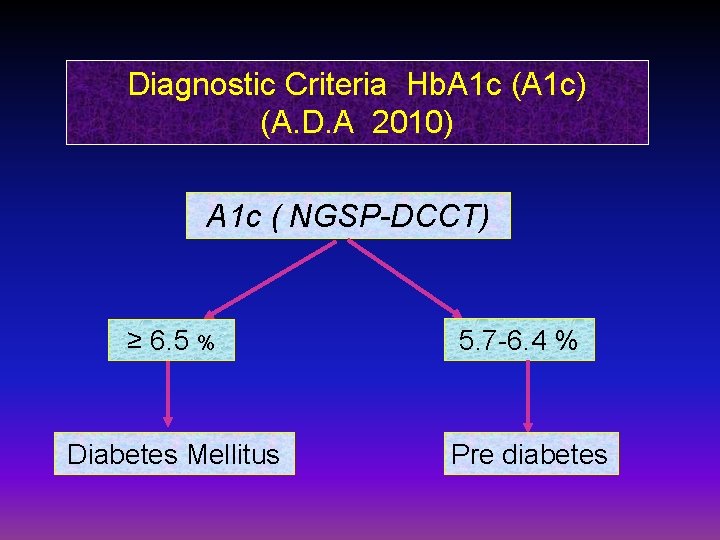
Diagnostic Criteria Hb. A 1 c (A 1 c) (A. D. A 2010) A 1 c ( NGSP-DCCT) ≥ 6. 5 % Diabetes Mellitus 5. 7 -6. 4 % Pre diabetes
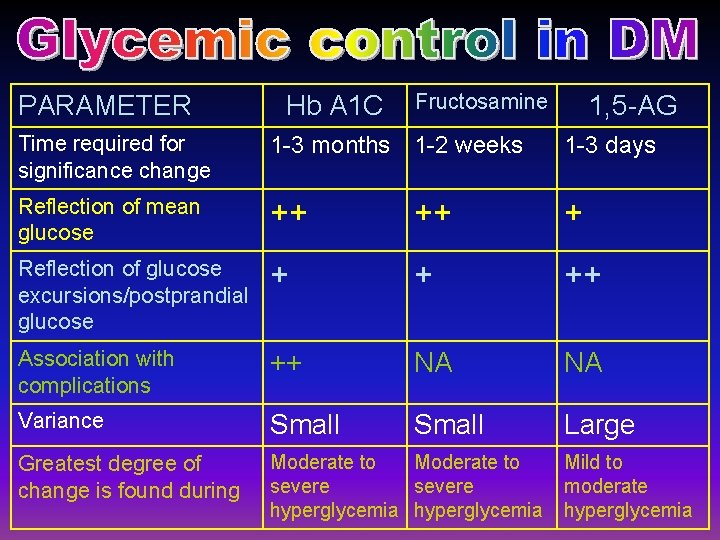
PARAMETER Hb A 1 C Fructosamine 1, 5 -AG Time required for significance change 1 -3 months 1 -2 weeks 1 -3 days Reflection of mean glucose ++ ++ + Reflection of glucose excursions/postprandial glucose + + ++ Association with complications ++ NA NA Variance Small Large Greatest degree of change is found during Moderate to severe hyperglycemia Mild to moderate hyperglycemia

v HPLC (reference) v Ion-Exchanges C : satisfactorily correlate with HPLC v Affinity binding C : little effect Hb variant. higher value than HPLC ( because measure total glycated Hb) v Electrophoresis and isoelectric focusing v Immunoassay : using monoclonal Ab exhibit excellent precision, Hb variant and carbamylated Hb are not detected. Correlate well with HPLC, but exhibit low value v Cassette based Immunoassay v Enzyme methods /Chemical analysis : total glycated Hb

v Hemoglobinopathy & Hb Variant → affect reliability test : altering glycation, abnormal peak on chromatography, RBC more prone to hemolysis v Transfusion, splenectomy, turnover RBC v Alcoholic chronic, opiate, iron deficiency, lead poisoning v Vitamin C and E can falsely lower level by inhibiting glycosylation, but vitamine C also increase levels for some assays v Carbamylated Hb in Uremia, Hyper-triglyceridemia, hyperbilirubinemia

v Measure of glycosilation of serum protein : interference by albumin levels→ reflecting glycemia over 1 -2 weeks v Whether fructosamine should be corrected for serum protein & albumin : controversial ? ? ? v Not affected by Hb variants, moderate to strong correlation With A 1 C → recommended for use in Hb pathy. Cheaper than A 1 C, a lack of consensus exists as to it clinical value v Alternative to A 1 C for estimating glycemic control, particularly where there are discrepancies SMBG and A 1 C and where short-term glycemic monitoring is desired

v Using serum sample & automatic equipment, has excellent batch analytical precision. v In carbonate buffer, fructosamine rearranges to the eneaminol form, which reduces NBT to a formasan. Absorbance at 530 nm is measured at two time points, and the absorbance change is proportional to concentrations of fructosamine v Hb > 100 mg/dl and bilirubine > 4 mg/dl interfere : → grossly hemolyzed and icteric samples should not be used v Vitamine C > 5 mg/dl : negative interfference

v Is validated marker of short-term glycemic control v Metabolically inert polyol that competes with glucose in the kidneys, otherwise stable levels of 1, 5 -AG are rapidly depleted as blood glucose levels exceed the renal threshold for glucosuria. v More accurately predicts rapid changes in glycemia than A 1 C & fructosamine. Can not use as an index for glycemic control in uremic patients. v More tightly associated with glucose fluctuations and postprandial glucose v 1, 5 -AG may offer complementary information to A 1 C

1. Measure fasting lipid profile at least annually. 2. In adults with low risk lipid value : LDL cholesterol < 100 mg/dl, HDL cholesterol > 50 mg/dl, Triglycerides < 150 mg/dl) → assessments may be repeated every 2 years

v Total Cholesterol : enzymatic colorimetric, accurate and easily automated v HDL Cholesterol : ultracentrifugation, precipitation, ion exchange chromatography, electrophoresis. v LDL-Cholesterol : Formula Fridewald (not valid in TG > 400 mg/dl) → direct immunoassay, electrophoresis v Triglyceride : enzymatic colorimetric, free glycerol enzymatic colorimetric, automated, good sensitivity, specifity, precision

v UAE annually in Type 1 DM (> 5 years), type 2 DM starting at diagnosis. v Microalbuminuria by measurement of albumin to creatinine ratio in a random urine v Serum creatinine at least annually in adults with DM regardless of the degree of UAE, should use to estimate GFR and stage CKD if present v Another's test : CBC, Urinalysis, cystatine-C

v Plasma Glucose (hypo or hyperglycemia) v Ketone bodies (blood or urine) particularly in type 1 DM : beta-hydroxyl butyric acid, aceto acetic acid, acetone. → colorimetric automated or dipstick v Blood gas analysis v Blood electrolyte analysis

v. Bacteria : direct smear, culture (Bactec or conventional) v. Mycobacterium tuberculosis : direct smear, culture v. CRP (acute phase reactant), CBC, urinalysis v. Sepsis / SIRS : Blood cultures, etc

v. Urinary keton v. Blood keton, Beta hydroxybutarate & others keton bodies v. Plasma Glukosa

Type 1 diabetes Type 2 diabetes C-peptide levels Very low or undetectable Detectable Prediabetes Auto antibodies (GAD 65, Auto antibodies absent ICA 512, IAA) maybe (testing not indicated) present Medication Therapy Insulin absolutely Oral agents necessary : multiple daily Insulin Commonly injection or insulin pump needed Therapy to None known prevent or Clinical trial in progress delay onset of diabetes Lifestyle (weight loss and physical activity ) Oral medications Clinical trial in progress
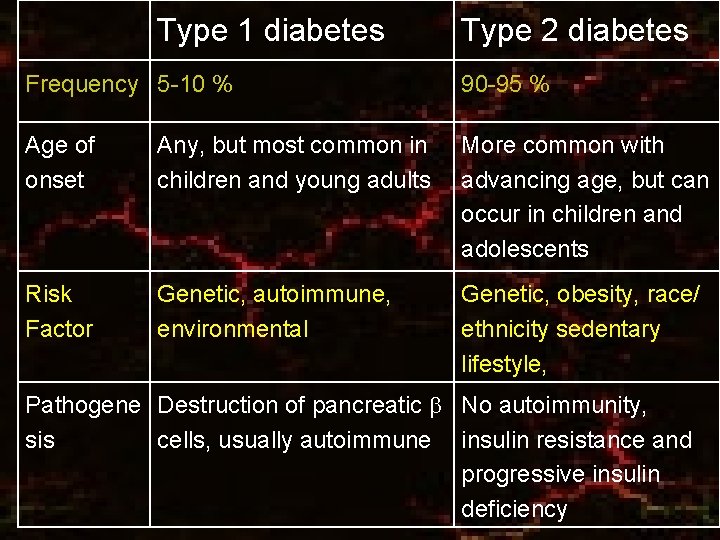
Type 1 diabetes Type 2 diabetes Frequency 5 -10 % 90 -95 % Age of onset Any, but most common in children and young adults More common with advancing age, but can occur in children and adolescents Risk Factor Genetic, autoimmune, environmental Genetic, obesity, race/ ethnicity sedentary lifestyle, Pathogene Destruction of pancreatic No autoimmunity, sis cells, usually autoimmune insulin resistance and progressive insulin deficiency

v Pro-insulin → insulin + C-peptide (equivocal) v Ratio C-peptide : insulin serum = 5 : 1 to 15 : 1, due primarily to hepatic clearance of insulin. v Half life C-peptide & pro-insulin 30 minute, but insulin 49 minute. → C-peptide more stabile v C-peptide levels : basal & pos glucagons stimulation v Assay : immunoassay → minor cross reactivity with proinsulin, in patients who have circulating Ab to insulin
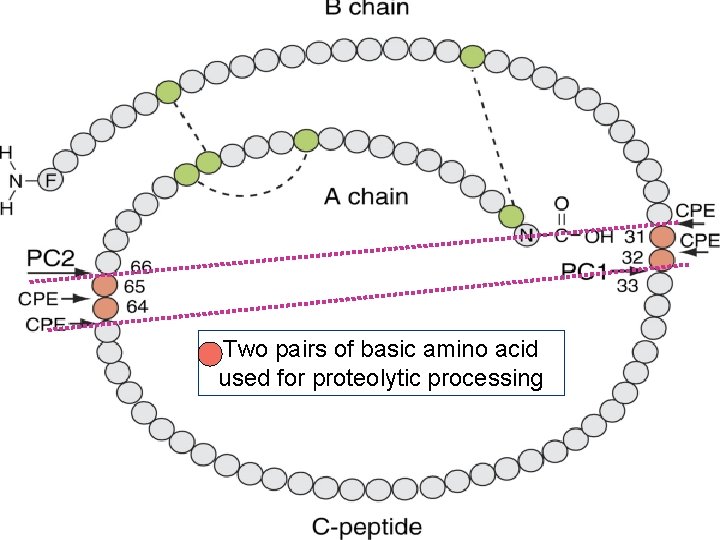
Two pairs of basic amino acid used for proteolytic processing

v. Insulin levels : fasting & 2 -h postprandial v. Wide variation in assay bias → standardization v. Performed for Insulin resistance A s s a y 1. RIA : cross reaction with pro-insulin & insulin exogenous, circulating anti insulin antibodies 2. Immuno enzymometric assay specific for insulin : interference from endogenous insulin & anti insulin Ab 3. Micro particle enzyme immunoassay (MEIA) : interference from endogenous insulin & anti insulin Ab

v GAD-65, IAA, ICA-512 v Antibodies (+) may help in DD type 1 DM from the others v Antibodies (-) does not exclude this diagnosis. v GAD-65 has the highest sensitivity (91 %) as a single screening marker for detecting multiple Antibodies v IAA : more common in young children who develop type 1 DM v GAD-65 more common in adults

v Cut off value for immune marker : not completely establish / standardized for clinical setting v No consensus as to what follow up testing should be undertaken when a positive autoantibody test v Incidence DM type 1 is low, testing of healthy individuals will identify only very small number (< 0. 5 %) who at that moment maybe pre-DM

v At diagnosis Type 1 DM : performed Anti TPO & Anti TG v Autoimmune thyroid : 17 -30 % in type 1 DM. v Thyroid Ab (+) : predictive of thyroid dysfunction Check TSH : If normal, rechecked every 12 years, or if patients develop thyroid dysfunction, thyromegaly, or abnormal growth rate.

SMBG v Insulin therapy : 3 or more times daily v inconvenience, physical discomfort & disability, along with expense v The procedure is complex for some patients, advances in technology, errors in technique v For accuracy & reproducibility : it is important to routine evaluate maintenance & standardization for each instrument by committee POCT especially in hospital

Point of care testing /P. O. C. T v Variation of methods, accuracy, presision v Interferen : temperature, humidity v Used good Calibrator v Strip Storage v Small Volume sample : Whole blood, serum or plasma v Simple & rapid v For Monitoring, not diagnostic

v Diagnostic test : FPG, 2 -h PG, OGTT v Monitoring : SMBG, A 1 C, Fructosamine, 1, 5 -AG v Complication : as indicated to clinical conditions v GAD-65, IAA, ICA-512 : Auto antibodies may help to DD Type 1 DM from others, it does not exclude diagnosis, not recommended for screening. v Each method had false positive and negative depend on sensitivity & specifity of the test

- Slides: 40