Labor and Delivery CAPT Mike Hughey MC USNR

Labor and Delivery CAPT Mike Hughey, MC, USNR Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide

Labor • Regular, frequent, leading to progressive cervical effacement and dilatation • Braxton-Hicks contractions – May be painful and regular, but usually are not – Do not lead to cervical change • Labor diagnosis usually made in retrospect. • Cause of labor is unknown Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 2

Latent Phase Labor • <4 cm dilated • Contractions may or may not be painful • Dilate very slowly • Can talk or laugh through contractions • May last days or longer • May be treated with sedation, hydration, ambulation, rest, or pitocin Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 3

Active Phase Labor • At least 4 cm dilated • Regular, frequent, usually painful contractions • Dilate at least 1. 2 -1. 5 cm/hr • Are not comfortable with talking or laughing during their contractions Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 4
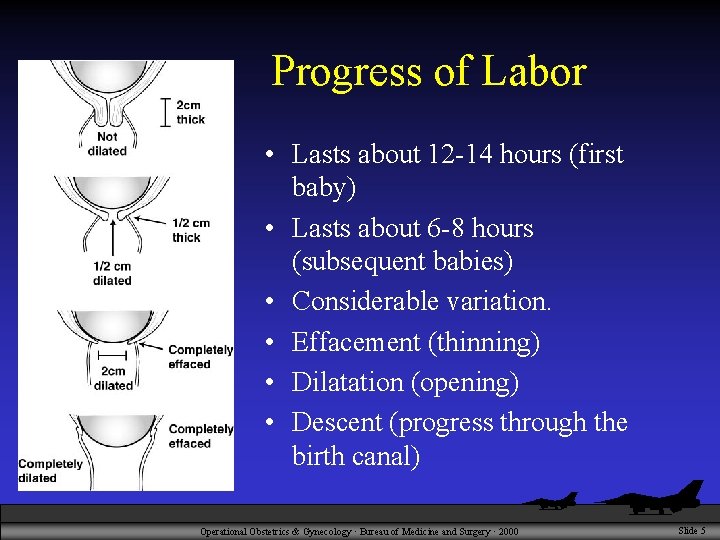
Progress of Labor • Lasts about 12 -14 hours (first baby) • Lasts about 6 -8 hours (subsequent babies) • Considerable variation. • Effacement (thinning) • Dilatation (opening) • Descent (progress through the birth canal) Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 5

Descent • Fetal head descends through the birth canal • Defined relative to the ischial spines • 0 station = top of head at the spines (fully engaged) • +2 station = 2 cm past (below) the ischial spines Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 6

Cardinal Movements of Labor • • Engagement (0 Station) Descent Flexion (fetal head flexed against the chest) Internal rotation (fetal head rotates from transverse to anterior • Extension (head extends with crowning) • External rotation (head returns to its’ transverse orientation) • Expulsion (shoulders and torso of the baby are delivered) Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 7
Watch a Delivery Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 8
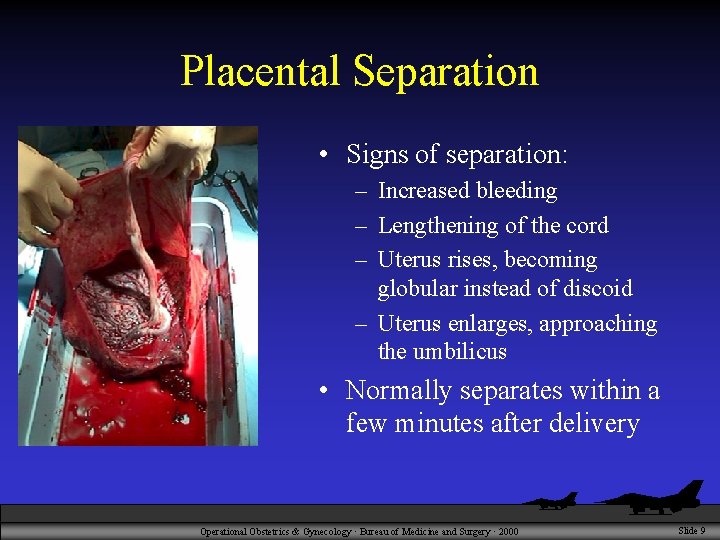
Placental Separation • Signs of separation: – Increased bleeding – Lengthening of the cord – Uterus rises, becoming globular instead of discoid – Uterus enlarges, approaching the umbilicus • Normally separates within a few minutes after delivery Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 9

Initial Labor Management • • Risk assessment Contractions: frequency, duration, onset Membranes: Ruptured, intact Status of cervix: dilatation, effacement, station • Position of the fetus: vertex, transverse lie, breech • Fetal status: fetal heart rate, EFM Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 10

Cervix • Dilatation: How far has the cervix opened (in cm) • Effacement: How thin is the cervix (in cm or %) Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 11

Status of Membranes • Nitrazine paper turns blue in the presence of alkaline amniotic fluid (“nitrazine positive”) • Vaginal secretions are nitrazine negative (yellow) because of their acidity • Pooling of amniotic fluid in the vaginal vault is a reliable sign Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 12
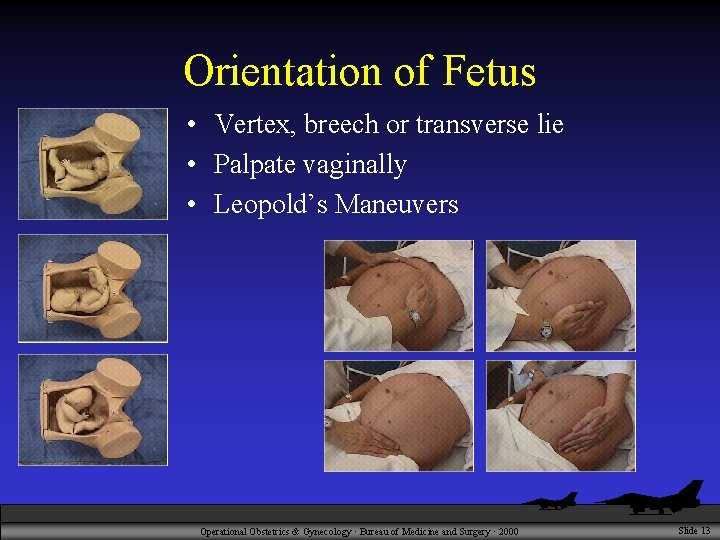
Orientation of Fetus • Vertex, breech or transverse lie • Palpate vaginally • Leopold’s Maneuvers Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 13

Management of Early Labor • Ambulation OK with intact membranes • If in bed, lie on one side or the other…not flat on her back • Check vital signs every 4 hours • NPO except ice chips or small sips of water Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 14

Monitor the Fetal Heart • During early labor, for low risk patients, note the fetal heart rate every 1 -2 hours. • During active labor, evaluate the fetal heart every 30 minutes • Normal FHR is 120 -160 BPM • Persistent tachycardia (>160) or bradycardia (<120, particularly <100) is of concern Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 15

Electronic Fetal Monitors • Continuously records the instantaneous fetal heart rate and uterine contractions • Patterns are of clinical significance. • Use in high-risk patients. • Use in low-risk patients optional Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 16
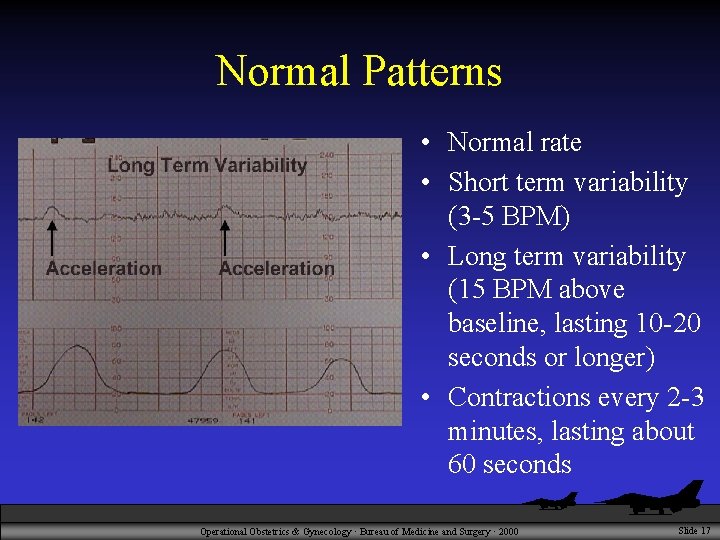
Normal Patterns • Normal rate • Short term variability (3 -5 BPM) • Long term variability (15 BPM above baseline, lasting 10 -20 seconds or longer) • Contractions every 2 -3 minutes, lasting about 60 seconds Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 17
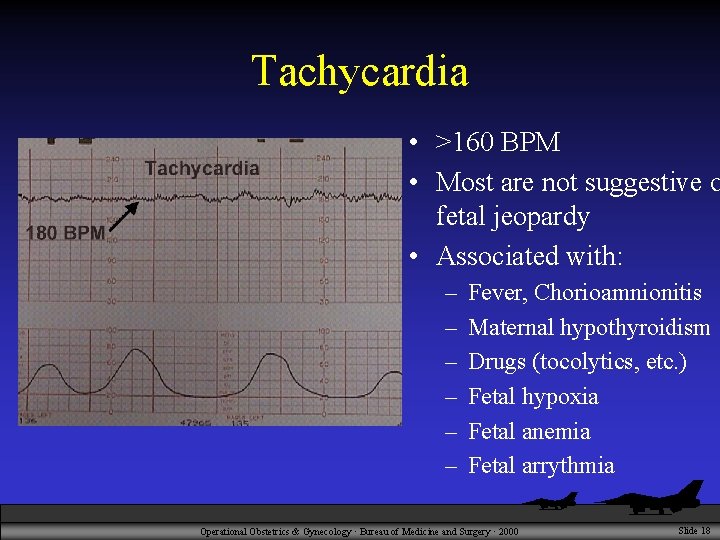
Tachycardia • >160 BPM • Most are not suggestive o fetal jeopardy • Associated with: – – – Fever, Chorioamnionitis Maternal hypothyroidism Drugs (tocolytics, etc. ) Fetal hypoxia Fetal anemia Fetal arrythmia Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 18
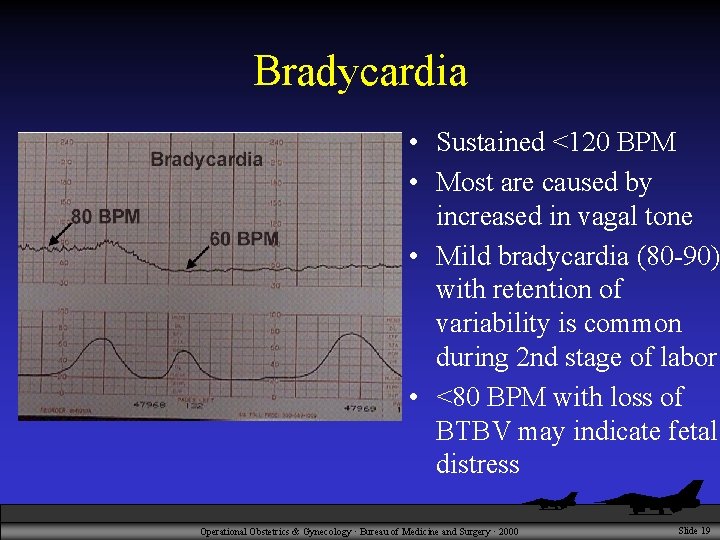
Bradycardia • Sustained <120 BPM • Most are caused by increased in vagal tone • Mild bradycardia (80 -90) with retention of variability is common during 2 nd stage of labor • <80 BPM with loss of BTBV may indicate fetal distress Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 19
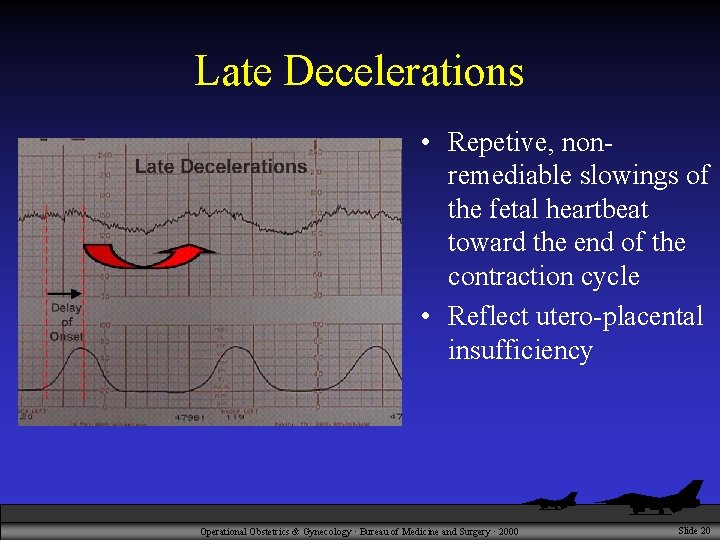
Late Decelerations • Repetive, nonremediable slowings of the fetal heartbeat toward the end of the contraction cycle • Reflect utero-placental insufficiency Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 20
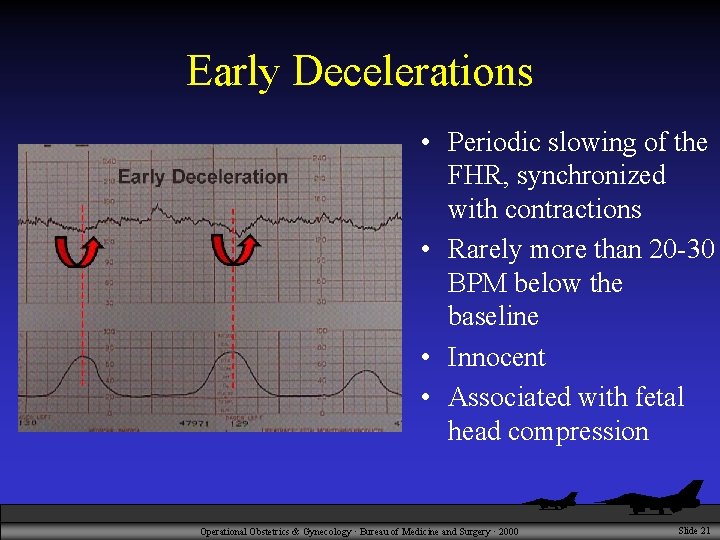
Early Decelerations • Periodic slowing of the FHR, synchronized with contractions • Rarely more than 20 -30 BPM below the baseline • Innocent • Associated with fetal head compression Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 21
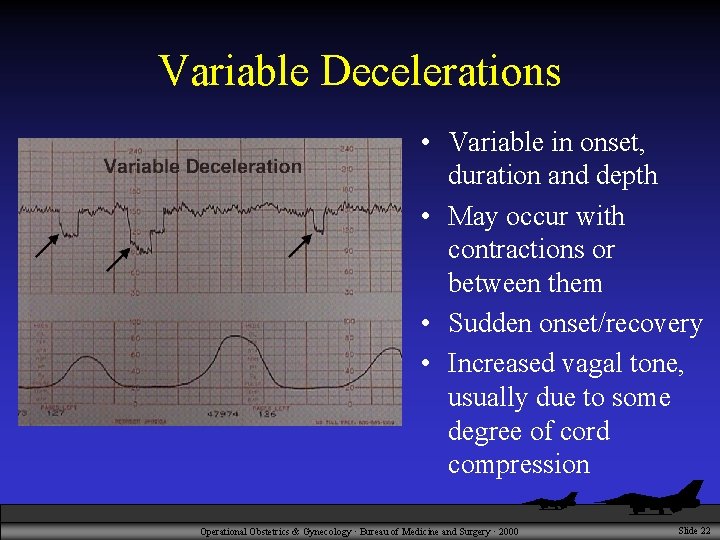
Variable Decelerations • Variable in onset, duration and depth • May occur with contractions or between them • Sudden onset/recovery • Increased vagal tone, usually due to some degree of cord compression Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 22
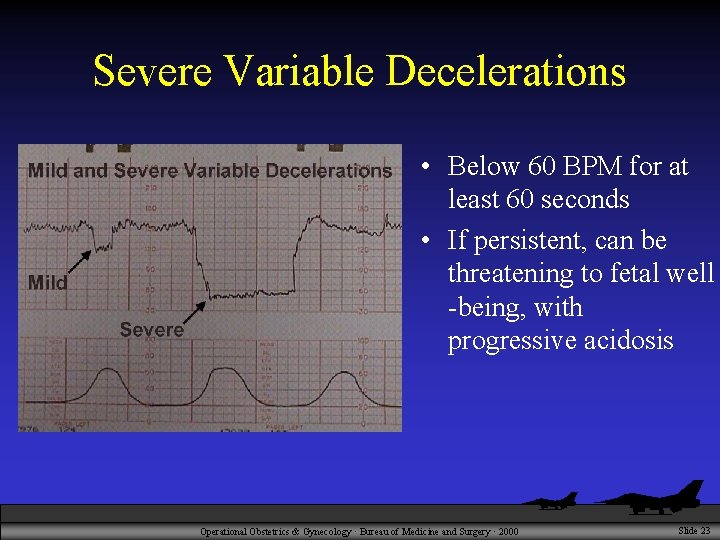
Severe Variable Decelerations • Below 60 BPM for at least 60 seconds • If persistent, can be threatening to fetal well -being, with progressive acidosis Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 23
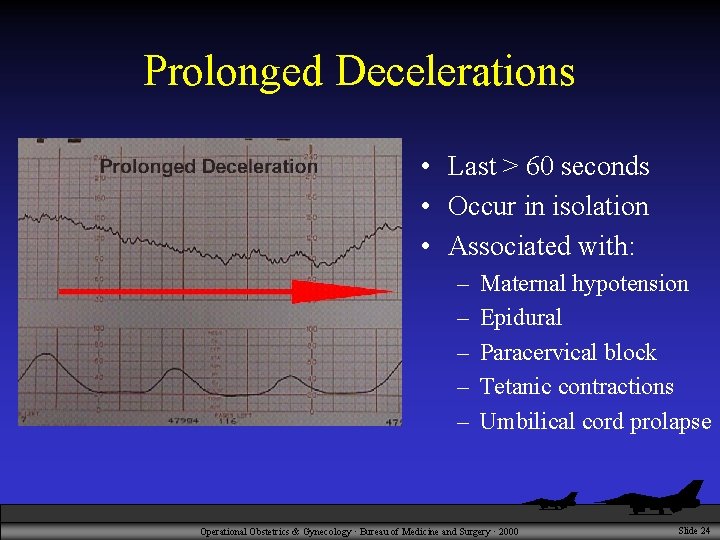
Prolonged Decelerations • Last > 60 seconds • Occur in isolation • Associated with: – – – Maternal hypotension Epidural Paracervical block Tetanic contractions Umbilical cord prolapse Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 24

Pain Relief • Narcotics • Continuous Lumbar Epidural • Paracervical Block • 50/50 nitrous/oxygen • Psychoprophylaxis (Lamaze breathing) • Hypnosis Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 25
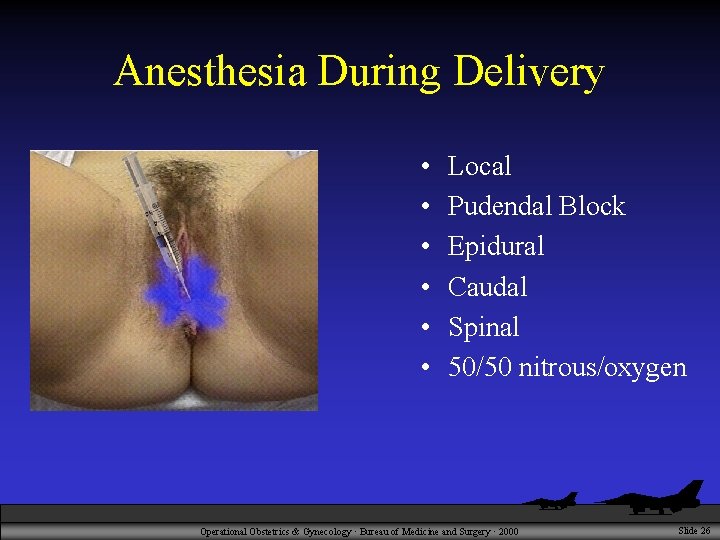
Anesthesia During Delivery • • • Local Pudendal Block Epidural Caudal Spinal 50/50 nitrous/oxygen Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 26
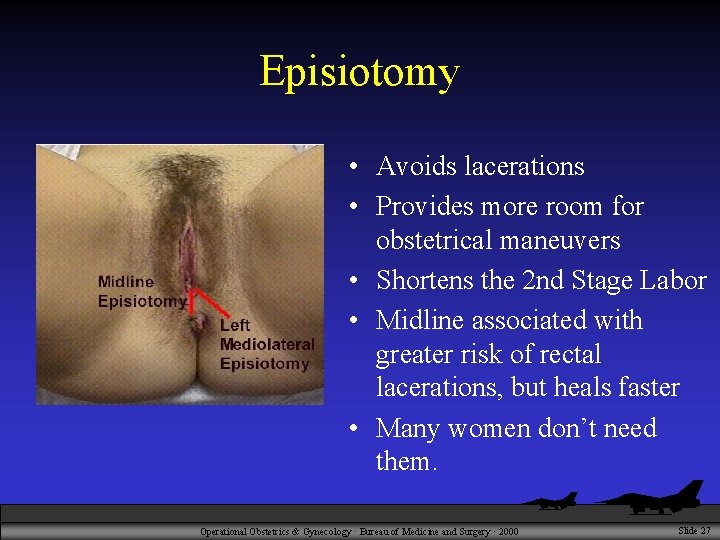
Episiotomy • Avoids lacerations • Provides more room for obstetrical maneuvers • Shortens the 2 nd Stage Labor • Midline associated with greater risk of rectal lacerations, but heals faster • Many women don’t need them. Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 27

Clamp and Cut the Cord • Clamp about an inch from the baby’s abdomen • Use any available instruments or usable material • Check the cord for 3 -vessels, 2 small arteries and one larger vein Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 28
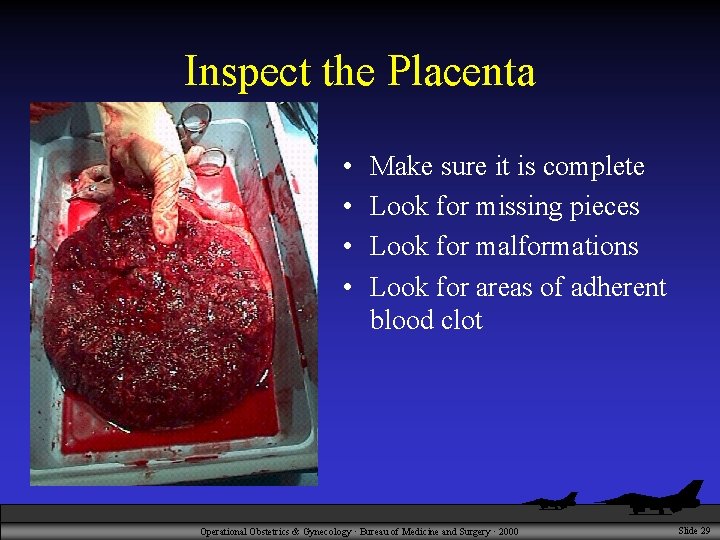
Inspect the Placenta • • Make sure it is complete Look for missing pieces Look for malformations Look for areas of adherent blood clot Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 29

Operational Obstetrics & Gynecology · Bureau of Medicine and Surgery · 2000 Slide 30
- Slides: 30