La maladie de Barth vu travers lexprience franaise

La maladie de Barth – vu à travers l’expérience française Jean Donadieu Hôpital Trousseau – Registre des neutropénies

3 ans d’engagement • Automne 2011 • Printemps 2012 - mise en place de l’étude : Etat de l’art • A need for a global approach • Agreement between Reference centers : Mitochondriopathy / Hear disease/ Immune deficiency • The french SCN registry offered an infrastructure • A resident is available for a semester • Patient’ association is sponsoring the study • • Summer 2012: data collection and analysis End 2012 – Early 2013: Publication /// Sept 2013 – working party – with Bristol group 2014 : guidelines in French / National consultation for Barth‘ patients in Paris

Barth syndrome: the challenge • Rare… extremely rare • Scattered • Multi systemic • Chronic disease • Not a single expert in France

Barth syndrome/ france • Existing competences – – Cardiologists Geneticians Biochemists Networks – national plan for rare diseases • • Reference center for cardiac defect Reference center for mitochondriopathies Reference center for immune deficiency Learning society for pediatric immuno hematology and for pediatric cardiology – Registry for chronic neutropenia • a parent’s association

Method • Observational, longitudinal, retrospective, multicentric survey • Patients: o o who lived in France Diagnosed between 1983 and 2012 Complete diagnosis: TAZ Mutation Presumptive: Cardiopathy and Neutropenia and * X-linked * Cardiolipid profile

Identification of cases • French SCN registry • Networks from learning society - Société d’hématologie et immunologie pédiatrique - Société de Cardiologie pédiatrique et congénitale Networks of centre of refernces Genetic laboratories (n=2) Biochemistry / Necker Request to pathologists in charge of Sudden death program o Patients’ association o Administrative data base: Death certificate / Organ transplantation / Discharge records

Data collection • ON SITE • Medical file / CBC / Echocardiography • Definition: Date of diagnosis = date of first symptoms • Diagnosis Echocardiography: the first within 3 months after date of diagnosis

Results - Logistic • Death certificate, Discharge records, Heart transplantation data base: No data ! • International Classification of Disease: neglects Bt. HS ! • A complex medical networks – 22 patients – 27 centers – 70 physicians

Demography: 22 patients 16 families o o Gender : 21 male 1 female (XO) Familial history : 2/3 Median age At diagnosis = 3. 1 weeks (p 25: 0 -p 75: 6, 2) Diagnosis first symptoms o o o o Cardiomyopathy = 16 patients (73%) Infection = 4 patients (18 %) Failure to thrive 1 Hypoglycemia at birth No Metabolic coma IUGR= 7 patients (32%) Diagnosis o o 18 Complete diagnosis TAZ mutated 4 Presumptive o o 3 siblings 1 Biochemistry profile

Epidemiology o Incidence at birth = 1. 5/million of birth (IC 95%: 0. 6 – 2. 3) (or 1 / 700 000 birth) o Between 0 and 3 new cases/ year expected in France (850 000 birth/year) o Prevalence is difficult to extrapolate. Probably no more than 30 cases living in France / 60 millions inhabitants o About 200 cases in EU ?

Genetic • TAZ mutations: in 15 families out 16 • Among 13 mothers evaluated: – 9 carriers – 1 had proven somatic mosaicism
Hematological features o Initial o o o 1. 3 G/L ANC value : (p 25: 0. 6 - p 75: 2. 9) 4 patients with ANC ≤ 0. 5 G/L Follow up : 8 CBC per patient o Median ANC : o o o 0. 98 G/L (p 25: 0. 69 – p 75: 12. 1) 16 patients (72%) ANC ≤ 0, 5 G/L at least ONCE 2 patients (9%) médian ANC ≤ 0, 5 G/L Bone marrow : Rarely performed (n=2 )Myeloid maturation arrest
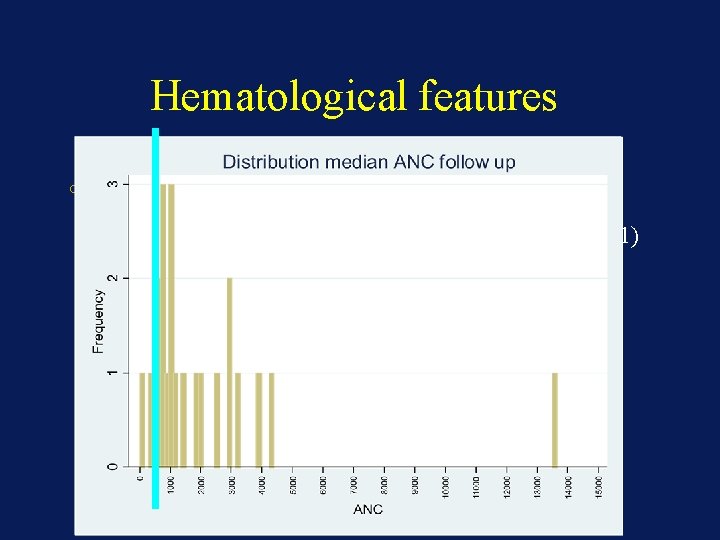
Hematological features o Follow up : 8 CBC per patient o Median ANC : o o 0. 98 G/L (p 25: 0. 69 – p 75: 12. 1) 16 patients (72%) ANC ≤ 0, 5 G/L at least ONCE 2 patients (9%) médian ANC ≤ 0, 5 G/L
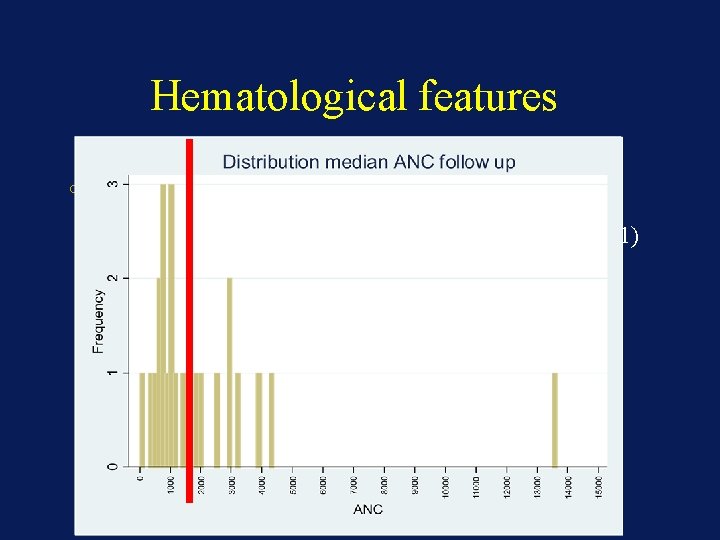
Hematological features o Follow up : 8 CBC per patient o Median ANC : o o 0. 98 G/L (p 25: 0. 69 – p 75: 12. 1) 16 patients (72%) ANC ≤ 0, 5 G/L at least ONCE 2 patients (9%) médian ANC ≤ 0, 5 G/L

Hematological features o Initial o o o ANC value : 1. 3 G/L (p 25: 0. 6 - p 75: 2. 9) 4 patients with ANC ≤ 0. 5 G/L Follow up : 8 CBC per patient o Median ANC : o o o 0. 98 G/L (p 25: 0. 69 – p 75: 12. 1) 16 patients (72%) ANC ≤ 0, 5 G/L at least ONCE 2 patients (9%) médian ANC ≤ 0, 5 G/L Bone marrow : Rarely performed (n=2 )Myeloid maturation arrest • Heterogeneous usually NOT A DEEP NEUTROPENIA

Infections • 94 infectious events, – 10 severe in 5 patients (23%). • Median age at first severe infection was 3. 7 months (range: 0. 2– 30. 7 months). – 84 mild infections. • Recurrent stomatitis was observed in 1 patient • Mild infections are associated to heart failure

Heart – 91 % (n=20) with a symptomatic cardiomyopathy • 1 : never (till age of 12 years) • 1 dyed very early – septic shok / autospy revealed no cardiopathy – 54 hospitalisations for heart failure • 16 patients (73%) needed inotropic support, • 14 (64%) needed invasive ventilation • 11 (50%) were treated with both inotropic agents and invasive ventilation at least once – 4 on cardiac transplant list / 2 heart transplant – 9 death related to cardiomyopathy

Echocardiography/ Diagnosis data • 11 patients with valuable information – 6 dilated cardiomyopathy (DCM) and hypertrophy cardiomyopathy (HCM) – 2 had DCM only – 1 had HCM only
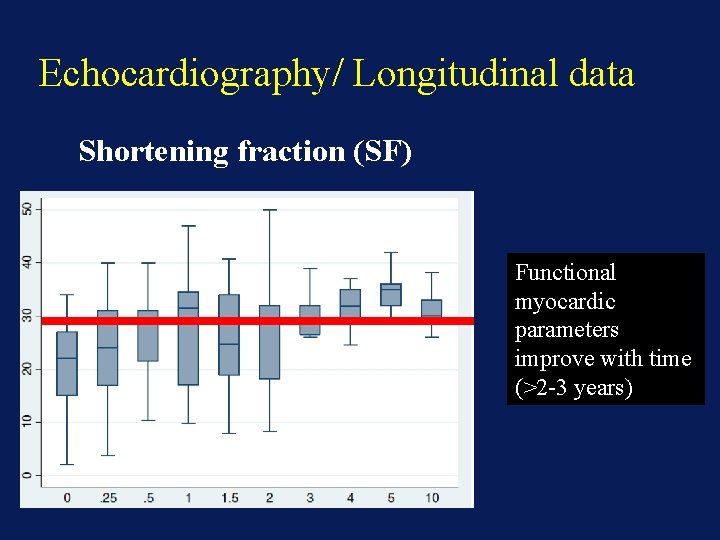
Echocardiography/ Longitudinal data Shortening fraction (SF) Functional myocardic parameters improve with time (>2 -3 years)
Electro cardiography • Repolarisation abnormalities in 77 % of patients • QTc: 440 ms (p 25: 420 – p 75: 466) • No arythmia observed

Other results – Age at walk : 19 months ( p 25: 18 – p 75: 21, 8) – Failure to thrive: - 50% weight < 3 SD - 50% height – 3 SD o Aciduria 3 – méthylglutaconic = 50% at diagnosis
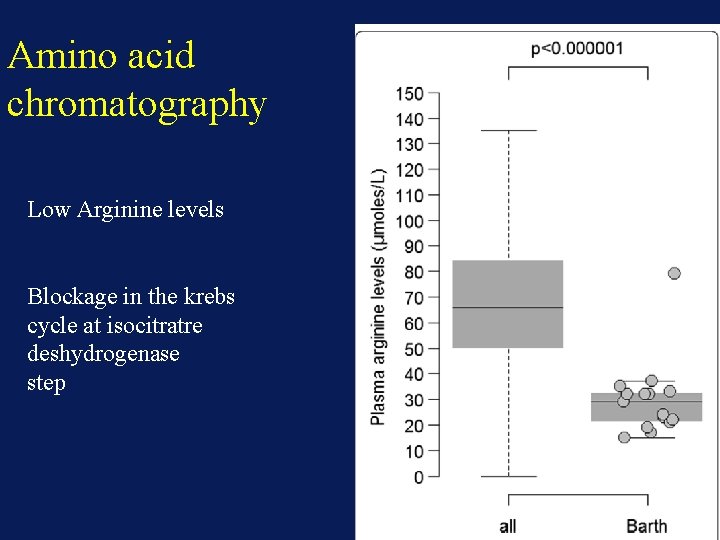
Amino acid chromatography Low Arginine levels Blockage in the krebs cycle at isocitratre deshydrogenase step
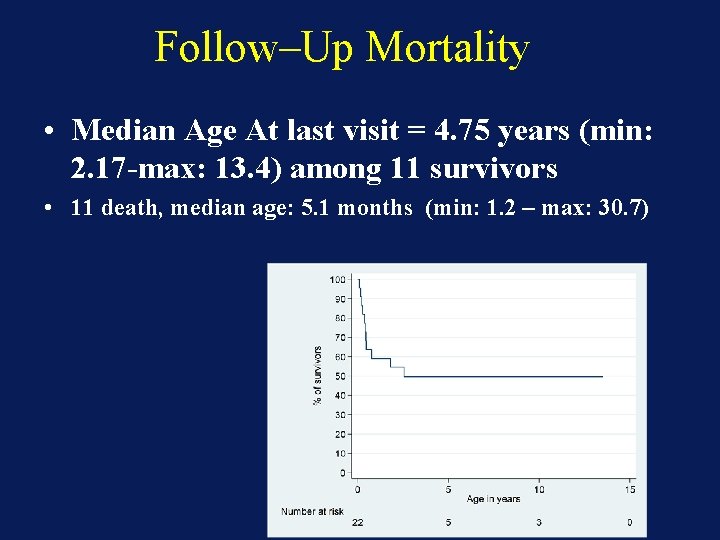
Follow–Up Mortality • Median Age At last visit = 4. 75 years (min: 2. 17 -max: 13. 4) among 11 survivors • 11 death, median age: 5. 1 months (min: 1. 2 – max: 30. 7)
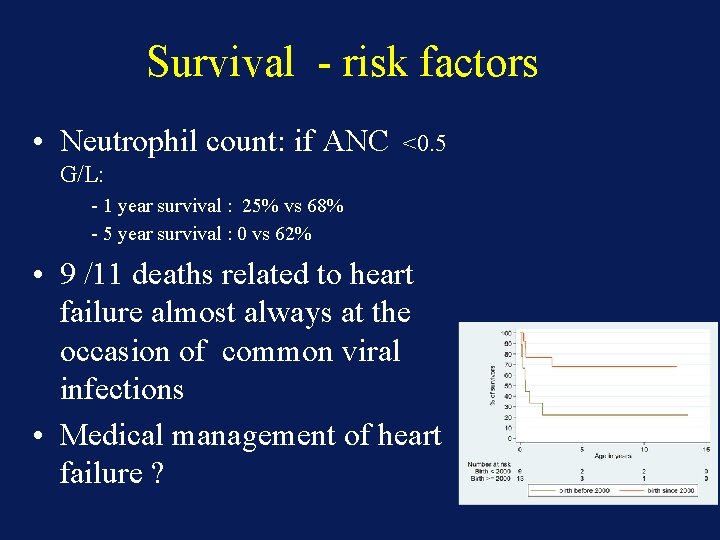
Survival - risk factors • Neutrophil count: if ANC <0. 5 G/L: - 1 year survival : 25% vs 68% - 5 year survival : 0 vs 62% • 9 /11 deaths related to heart failure almost always at the occasion of common viral infections • Medical management of heart failure ?


Conclusion of our study • BTHS exists in France !

Conclusion for the diagnosis • Not so easy ! • The diagnosis has mainly to be considered in boys with very early heart failure • Do not excluded quickly the diagnosis of BTHS ! • Neonatalogist and general pediatricians Has to be involved in the diagnosis/ detection of cases

Conclusions. . • No room for a randomized trial • The best approach: – The 2 first years are determinant ! – Guidelines • For physicians and general pediatricians • IV Ig for BTHS babies before age of 2 ? • Diet with arginine support ? – To maintain a network BUT also to set up a central expert center for the long term follow up. – To participate to cooperative studies – at international or EU levels – To stimulate basic science research / Data collection/ bio bank ?


Acknowledgement • The french barth association

Thanks • The physicians of the networks • Barth Working party in France – – – – – Charlotte Rigaud Anne-Sophie Lebre Renaud Touraine Chris Ottolenghi Allel Chabli Philippe Charron, Marlene Rio Pascale De Lonlay Damien Bonnet • L’équipe registre – B Beaupain – Students • C Rigaud, • S Cohen • Les laboratoires de génétiques – Pitié C Bellanné Chantelot – CHU Dijon B Aral L Faivre – Necker AS Lebbre • • • Laboratoire CERMIT F Bachelerie Laboratoire Hémato CHU toulouse E Delabesse M Pasquet E rare: Neutro Net C Klein K Boztug Whim ther net : R Badolato Grants : Inserm Invs ANR neutro Net Whimthernet/ Amgen / Chugai / AS st quentin fallavier / Ceredih / Barth France
- Slides: 31