Knowledge of radiation exposure in common radiological examinations


























- Slides: 33

Knowledge of radiation exposure in common radiological examinations amongst radiology department staff AL Chang, LH Cope, DH Keane, S Wood Presented by Dr AL Chang at Royal College of Radiologists Audit Meeting 18 May 2015

Disclosures • Work performed at Radiology department South Tyneside NHS Foundation Trust (STFT) • Current workplace – City Hospitals Sunderland NHS Foundation Trust 2

3

Background • The use of radiological investigations is an accepted part of medical practice justified in terms of clear clinical benefits to the patient, which should far outweigh the small radiation risks. • However even small radiation doses are not entirely without risk. A small fraction of the genetic mutations and malignant diseases that occur in the population can be attributed to background radiation 4

• The Ionising radiation (Medical Exposure) regulations 2000 and 2006 (IR(ME)R) impose a responsibility on imaging departments to ensure that all exposures to ionising radiation are justified, and that doses are optimized. Organizations and individuals using ionising radiation must comply with these regulations. 5

Background • • Information available on internet Heightened awareness of radiation exposure i. Refer available on intranet Only a third of clinicians receive training in radiation protection and the level of knowledge is low (Soye 2008) • On 1 April 2009, the Care Quality Commission (CQC) assumed responsibility from the Healthcare Commission for the inspection and enforcement for incidents in England under Ionising Radiation (Medical Exposure) Regulations 2000 6

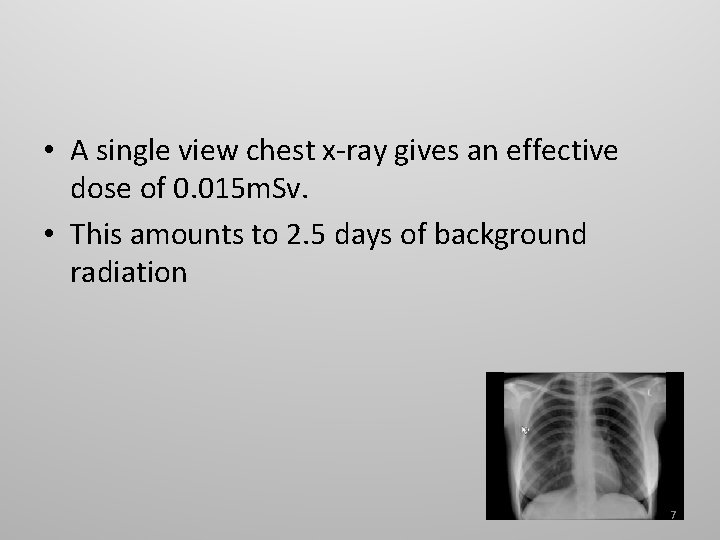
• A single view chest x-ray gives an effective dose of 0. 015 m. Sv. • This amounts to 2. 5 days of background radiation 7

THE STANDARD • All radiology department staff should have knowledge of the relevant radiation doses for common examinations Target • 50% awareness of dose estimation per chest xray equivalent 8

Process – Data collection • Standard questionnaire (14 questions) • To all staff in radiology department • Data collected over – First week November 2012 – First week April 2014 • Number distributed – 1 st round = 70 ; responders = 54 ( 77%) – 2 nd round = 60 ; responders = 38 ( 63%) 9

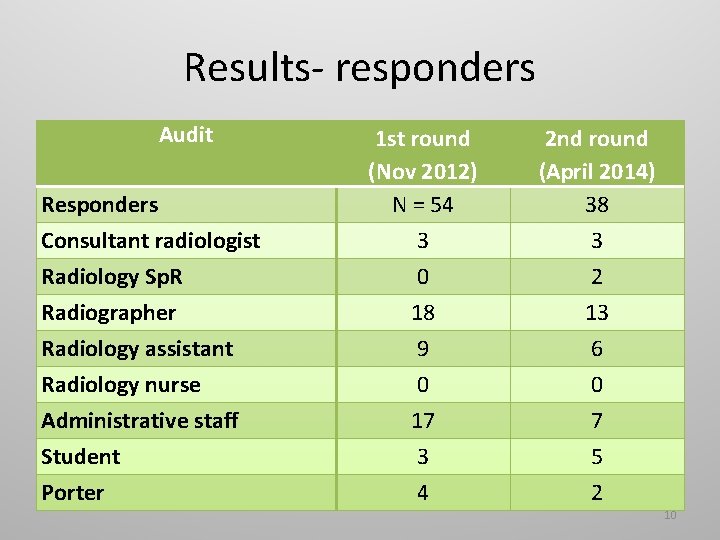
Results- responders Audit Responders Consultant radiologist Radiology Sp. R Radiographer Radiology assistant Radiology nurse Administrative staff Student Porter 1 st round (Nov 2012) N = 54 3 0 18 9 0 17 3 4 2 nd round (April 2014) 38 3 2 13 6 0 7 5 2 10

Introductory question • The IR(ME)R) regulations 2000 and 2006 impose a responsibility on imaging departments to ensure that exposures to the following imaging modalities are justified 1. 2. 3. 4. 5. 6. Plain x-rays Ultrasound scans Computed tomography imaging MRI scans Barium contrast studies All of the above 11

Introductory question • The IR(ME)R regulations 2000 and 2006 impose a responsibility on imaging departments to ensure that exposures to the following imaging modalities are justified 1. 2. 3. 4. 5. 6. Plain x-rays Ultrasound scans Computed tomography imaging MRI scans Barium contrast studies All of the above 12

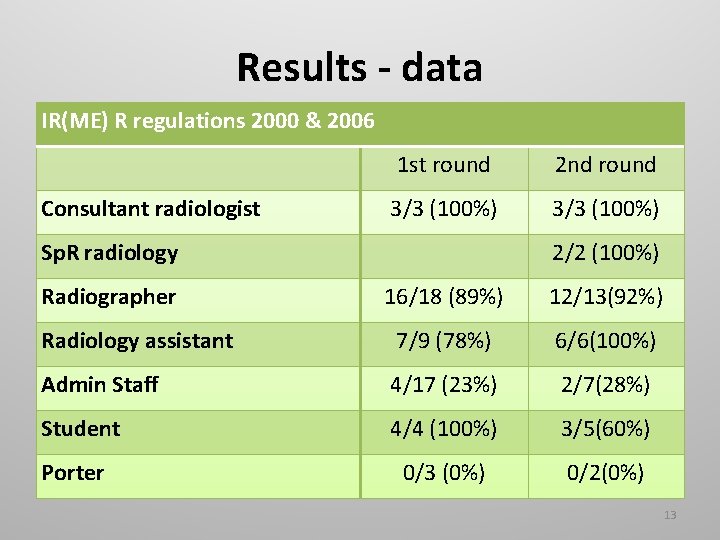
Results - data IR(ME) R regulations 2000 & 2006 Consultant radiologist 1 st round 2 nd round 3/3 (100%) Sp. R radiology Radiographer 2/2 (100%) 16/18 (89%) 12/13(92%) Radiology assistant 7/9 (78%) 6/6(100%) Admin Staff 4/17 (23%) 2/7(28%) Student 4/4 (100%) 3/5(60%) 0/3 (0%) 0/2(0%) Porter 13

Segment II of questionnaire What is the equivalent dose in ‘chest x-rays’ for the following examinations ? For example The equivalent dose from a single view pelvis x -ray is 20 chest x-rays 14

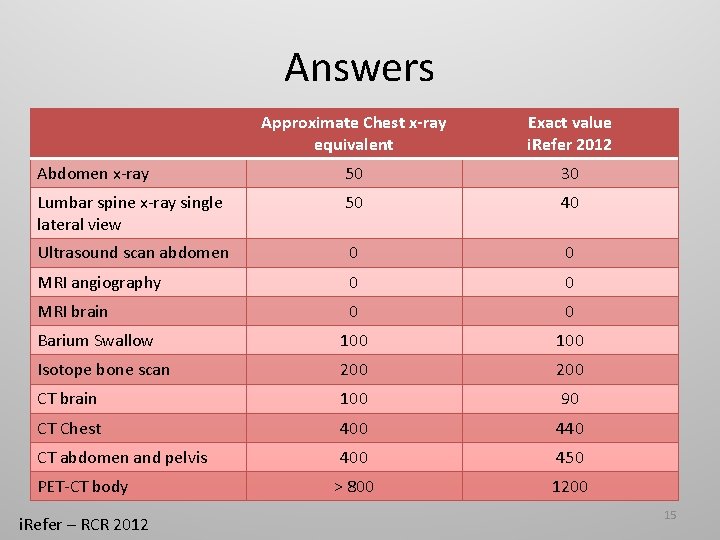
Answers Approximate Chest x-ray equivalent Exact value i. Refer 2012 Abdomen x-ray 50 30 Lumbar spine x-ray single lateral view 50 40 Ultrasound scan abdomen 0 0 MRI angiography 0 0 MRI brain 0 0 Barium Swallow 100 Isotope bone scan 200 CT brain 100 90 CT Chest 400 440 CT abdomen and pelvis 400 450 > 800 1200 PET-CT body i. Refer – RCR 2012 15

CT HEAD = approximate equivalent of 90 chest x-rays 16

What is the additional lifetime risk of inducing a fatal malignancy by performing …… CT chest abdomen and pelvis A Chest x-ray 1: 2 000 1: 1 000 17

Results 18

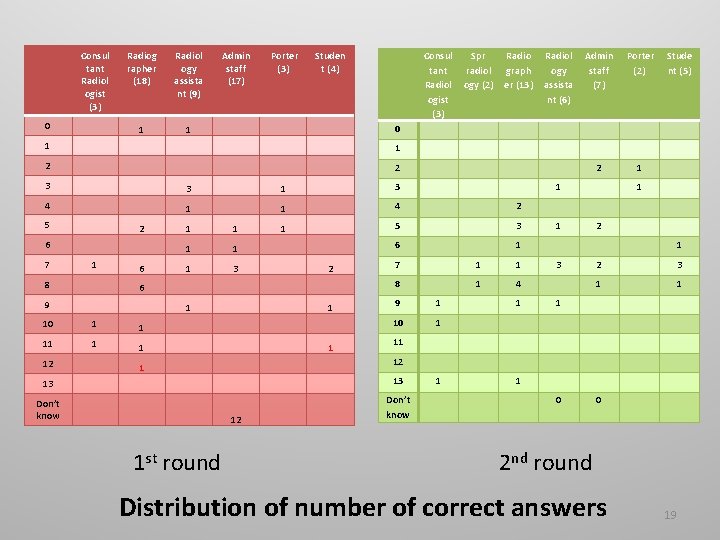
Consul tant Radiol ogist (3) 0 Radiog rapher (18) Radiol ogy assista nt (9) 1 1 Admin staff (17) Porter (3) Studen t (4) Consul tant Radiol ogist (3) Spr radiol ogy (2) Radio graph er (13) 1 2 2 3 3 1 3 4 1 1 4 2 1 5 3 6 1 2 6 7 1 8 6 1 1 3 1 10 1 1 1 12 1 2 6 9 1 1 Porter (2) 2 1 Stude nt (5) 1 7 1 1 8 1 4 9 1 10 1 1 2 1 3 2 3 1 11 12 1 13 13 Don’t know 12 1 st round Admin staff (7) 0 1 5 Radiol ogy assista nt (6) 1 1 0 0 2 nd round Distribution of number of correct answers 19

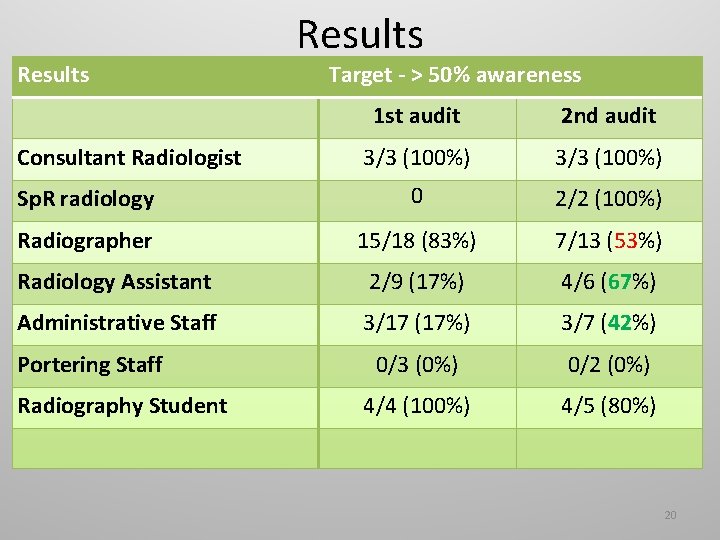
Results Target - > 50% awareness 1 st audit 2 nd audit 3/3 (100%) Sp. R radiology 0 2/2 (100%) Radiographer 15/18 (83%) 7/13 (53%) Radiology Assistant 2/9 (17%) 4/6 (67%) Administrative Staff 3/17 (17%) 3/7 (42%) 0/3 (0%) 0/2 (0%) 4/4 (100%) 4/5 (80%) Consultant Radiologist Portering Staff Radiography Student 20

Observations – first audit • Admin staff and porters are of the opinion that Ultrasound and MRI examination involve radiation exposure • 70% (12/17) of administrative staff respond ‘Don’t know’. • Radiography Students (4) have performed well – max being 11/13 • Highest mark (knowledge) by a radiographer (12/13) • 7/13 is average score amongst radiographers - 53% 21

Observations and Actions taken • Awareness of radiation exposure in common radiological examinations amongst staff working in radiology department is poor • 77% return of forms • Radiology nurses have not submitted form • Lunch time lectures ( x 4) on procedures undertaken in the department and on IR(ME)R 22

Observations – second round audit • Maximum score obtained by 1 consultant radiologist and radiographer • Radiology assistants – massive improvement in knowledge – 100% in the IR(ME)R questions and – 67% responders ( cf 17%) achieving > 50% score. – 1 Rad assistant scored 9/13 • Admin staff demonstrate some improved knowledge in radiation awareness: – No staff response of ‘Don’t know’. 23

Observations – second round • Radiographers – improve on the IR(ME)R question • (89% –> 92% correct) – decreased awareness of radiation equivalents • (83% -> 53% > 50% marks ) • Porters – very low awareness – no improvement. • Radiology nurses have not submitted forms 24

Further observations • Admin staff indicated that – MRI involved radiation (3) – CT head, CT abdomen involved radiation dose equivalent > 800 CXR (5) • Porters continue to believe that – MRI and US involved radiation – Barium swallow study involved no radiation. 25

Further observations • Students – indicate CT head and CT chest dose equivalents > 800 CXR – are aware that US & MRI involve NO radiation – are aware that PET-CT involves very large dose > 800 CXR (100%) • Overall knowledge of dose equivalent of CT head is poor (30% radiographers, 50% Sp. R) 26

Limitation • Reference - i. Refer (2012) for validation of radiation doses and chest x-ray equivalents. • However, these doses are relatively higher than STFT radiology in view of i. Dose in CT and Digital radiography. 27

Staff Responses • ‘Thank you for taking the time to inform us’ – Admin staff • ‘I now feel better equipped to answer patient questions’ – Radiology Assistant • ‘I am able to understand my job better’ – Radiology Assistant 28

Summary • Overall there is good interval improvement in awareness of radiation dose equivalents amongst radiology assistants and admin staff. • Staff feel valued 29

Recommendations and Action plan • Essential attendance at department lecture on procedures undertaken in the department and on radiation protection and Ionising (ME) regulations 2000 and 2006 to all staff • Although some staff are not directly involved in radiation exposure, it is essential they are aware of these procedures as they work in a radiation designated area 30

31

• My thanks to radiography student Sophie for distribution and collection of data sheets in radiology department in second audit cycle. • Any questions or suggestions 32

References 1. 2. 3. Soye & Paterson. A survey of awareness of radiation dose among health professionals in Northern Ireland. BJR 2008; 81: 725 -729. http: //bjr. birjournals. org/cgi/content/abstract/81/969/725 The Ionising Radiation (Medical Exposure) Regulations 2000. HMSO. http: //www. legislation. gov. uk/uksi/2000/1059/pdfs/uksi_200010 59_en. pdf i. Refer. Making the best use of clinical radiology 7 th Edition RCR 2012 www. rcr. ac. uk/content. aspx? pageid=995 33