Knowledge and basic practice in prevention and treatment

Knowledge and basic practice in prevention and treatment of Acute Respiratory Infection caused by Coronavirus (COVID-19) Training materials for final year healthcare students 03/2020

Learning goals 1. Presentation of the biological, the epidemiological and the clinical characteristics of the pathogen (SARS-Co. V 2); 2. Presentation of measures to prevent and control COVID -19 for individuals and the communities; 3. Supporting health facilities in implementing measures to control COVID-19; 4. Participating in assisting the reception, triaging and taking care of patients.

Lesson 1. SARS-Co. V-2: biological, epidemiological and clinical characteristics Training materials for final year healthcare students 03/2020

General introduction • Emerging infectious diseases by novel strains of virus are the new challenges to Public Health worldwide • Some recent viral epidemic – 2002: Severe acute respiratory syndrome caused by corona virus (SARS-Co. V) – 2009: H 1 N 1 flu – 2012: Acute respiratory infection syndrome caused by Middle East corona virus (MERS-Co. V) – 2019: Acute respiratory infection syndrome due to new strain of corona virus (SARS-Co. V-2)

The biological characteristics of SARS-Co. V-2 • A new strain of the coronavirus that has not been previously identified. • Today, there are six other known strains of Corona virus that can infect humans

The biological characteristics of SARS-Co. V-2 • Belong to Betacoronavirus, SARS virus causes disease in civets, mice, transmitting to humans and MERS-Co. V causes diseases in bats, transmitting to camels and humans. • SARS-Co. V-2 is from bats and wild animals which transmitting to humans. This is an enveloped virus, a circular or oval virus particle, usually having polyhedron shape with a diameter of 60140 nm. . • Genetic characteristics are different from SARS and MER-Co. V, similar to 85% SARS genes • SARS Co. V-2 is present in the respiratory tract for 96 hours and takes 6 days to isolate and cultured in Vero E 6 and Huh -7 cell lines.

The biological characteristics of SARS-Co. V-2 • SARS-Co. V-2 survives in the body for about 4 weeks from the time of entry. • In the environment, SARS-Co. V-2 is very susceptible to light, ultraviolet rays and high temperature. • In cold, moist environment, on metal surfaces, SARS-Co. V-2 can last for 1 -3 days.

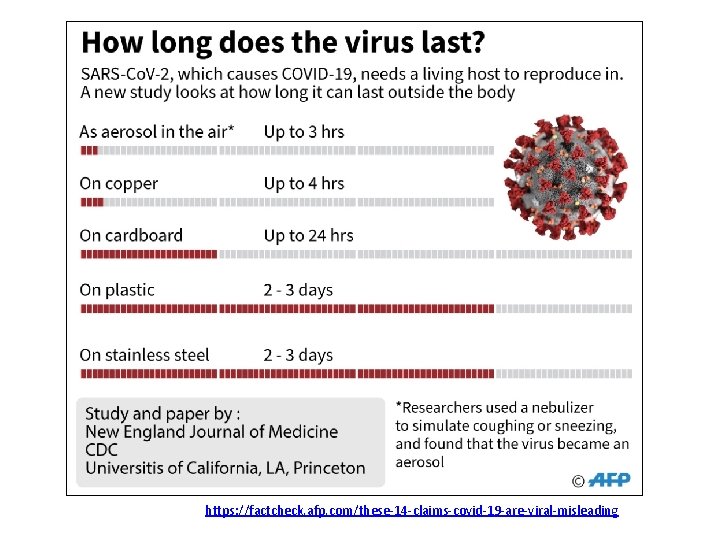
https: //factcheck. afp. com/these-14 -claims-covid-19 -are-viral-misleading

Clicker Question Imagine that a patient who is positive for SARSCo. V-2 coughed in a hospital room. On which of the following surfaces would SARS-Co. V-2 be most likely to stay infectious for more than 2 days? 1) A cardboard box 2) A copper table 3) A stainless steel table 4) In the air
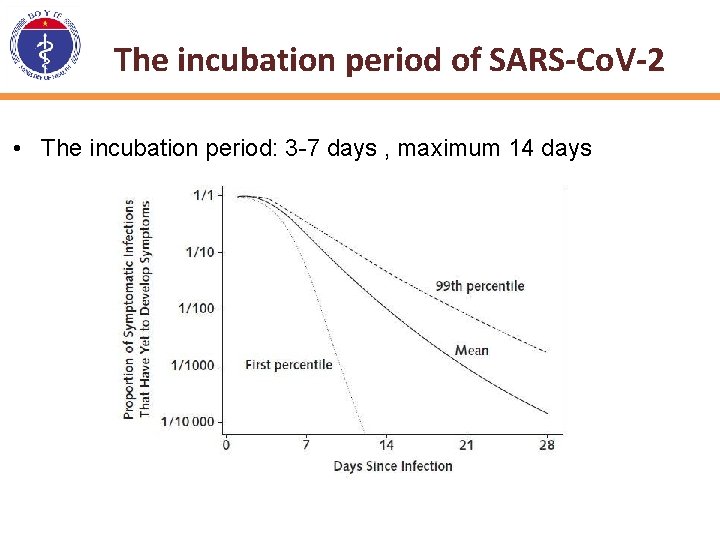
The incubation period of SARS-Co. V-2 • The incubation period: 3 -7 days , maximum 14 days
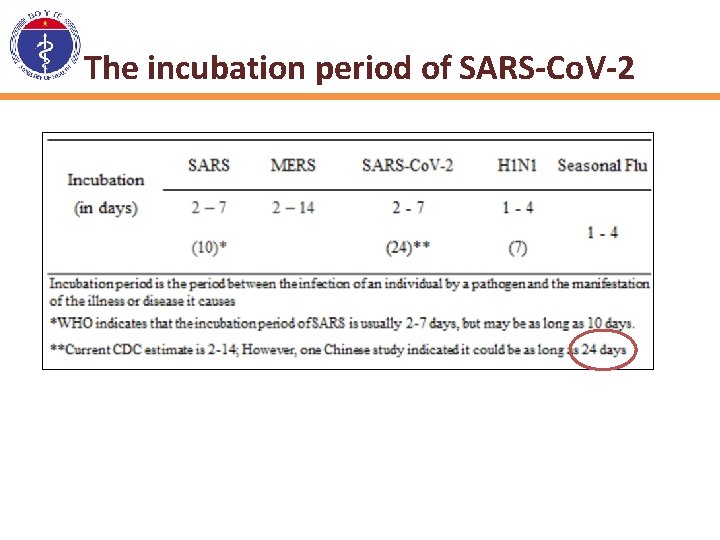

The incubation period of SARS-Co. V-2
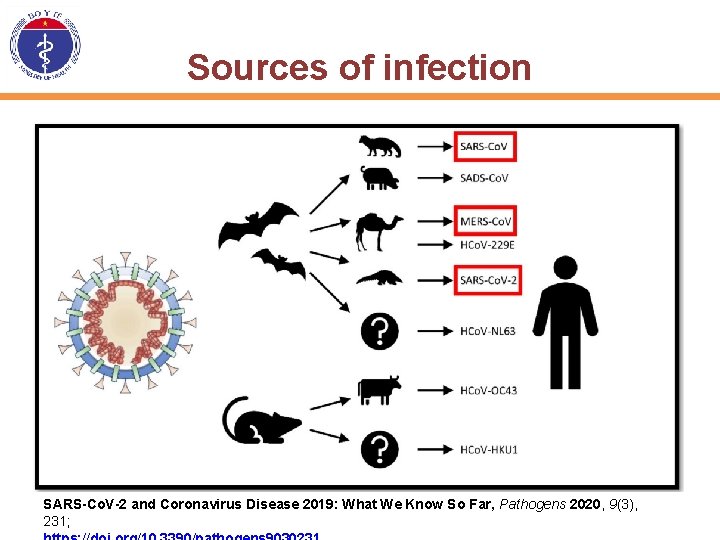
Sources of infection SARS-Co. V-2 and Coronavirus Disease 2019: What We Know So Far, Pathogens 2020, 9(3), 231;
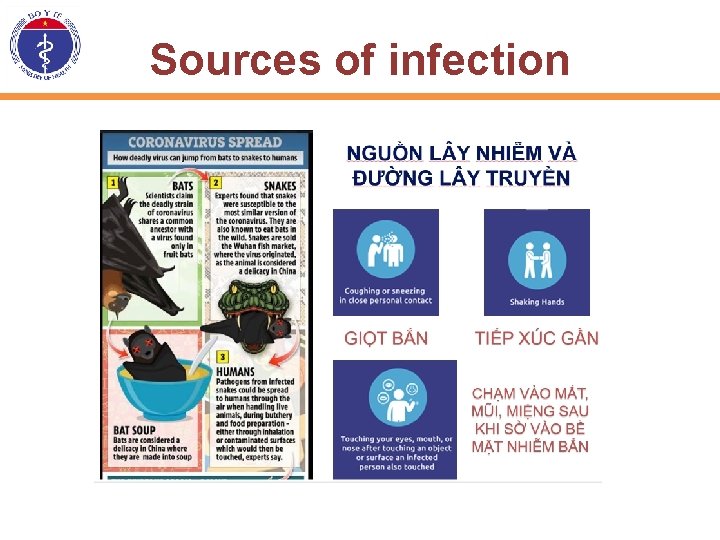
Sources of infection
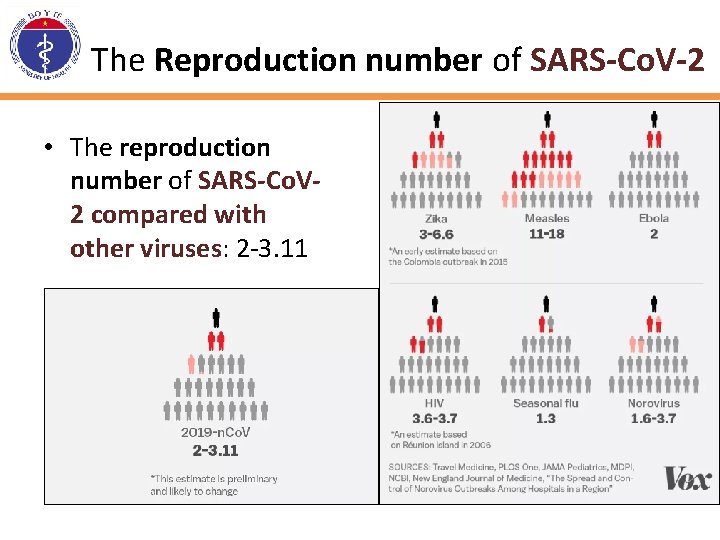
The Reproduction number of SARS-Co. V-2 • The reproduction number of SARS-Co. V 2 compared with other viruses: 2 -3. 11
Epidemiological characteristics of COVID-19
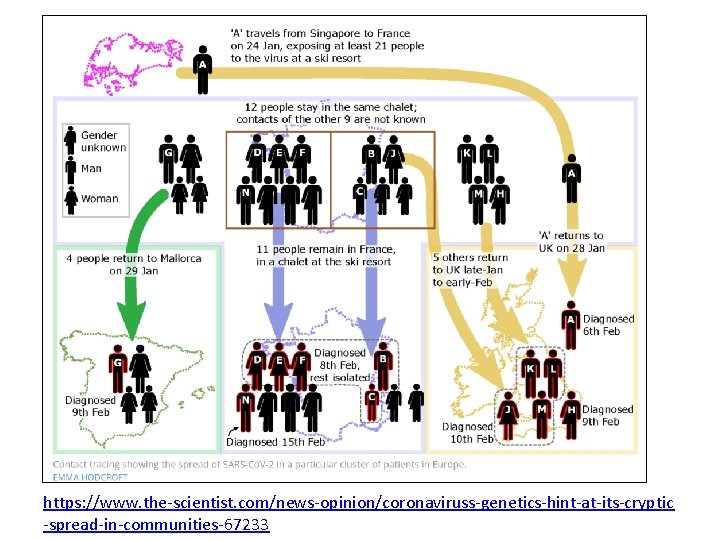
https: //www. the-scientist. com/news-opinion/coronaviruss-genetics-hint-at-its-cryptic -spread-in-communities-67233

Clicker Question Which of the following is a correct statement about the incubation period of SARS-Co. V-2? 1) The SARS-Co. V-2 incubation period is the period between infection and appearance of symptoms 2) The SARS-Co. V-2 incubation period is the period between infection and the start of infectiousness 3) The SARS-Co. V-2 incubation period is always 5 days or less in humans 4) The SARS-Co. V-2 incubation period is always more than 5 days in humans

Epidemiological characteristics of COVID-19 https: //experience. arcgis. com/experience/685 d 0 ace 521648 f 8 a 5 beeeee 1 b 9125 cd

Situation of COVID-19 in Vietnam • The first case of COVID-19 in Vietnam was a Chinese from Wuhan who was discovered on January 23, 2020. • The second person is the son of the first case, who is living in Vietnam

Situation of COVID-19 in Vietnam • At 22: 00 on 06/03/2019, Hanoi has confirmed the first case of Covid-19 in the city, also the 17 th case of Vietnam after more than 20 days of not detecting new case in Vietnam, even at the used-to-be " epicenter " of Vietnam which is Vinh Phuc province.
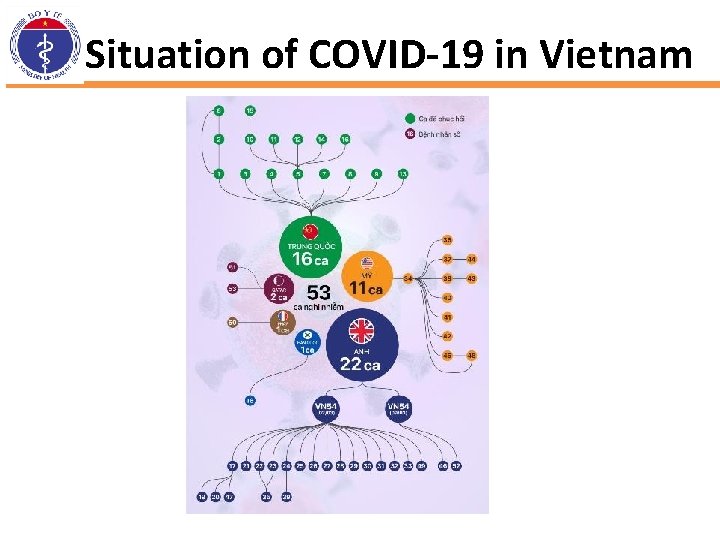
Situation of COVID-19 in Vietnam
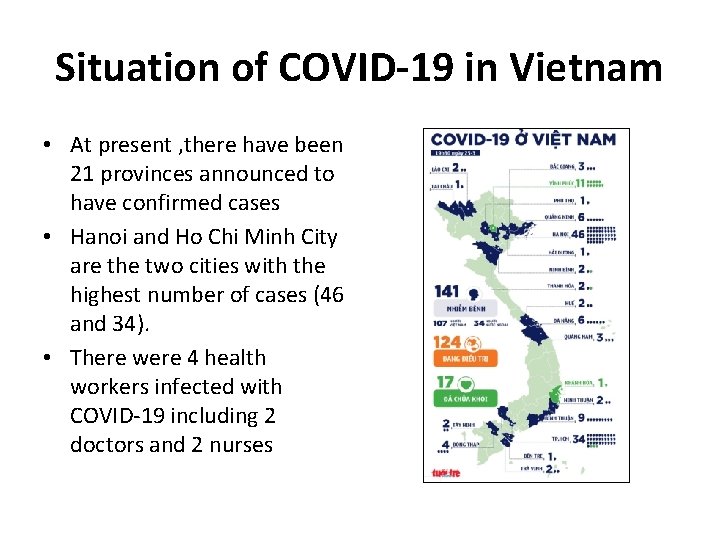
Situation of COVID-19 in Vietnam • At present , there have been 21 provinces announced to have confirmed cases • Hanoi and Ho Chi Minh City are the two cities with the highest number of cases (46 and 34). • There were 4 health workers infected with COVID-19 including 2 doctors and 2 nurses
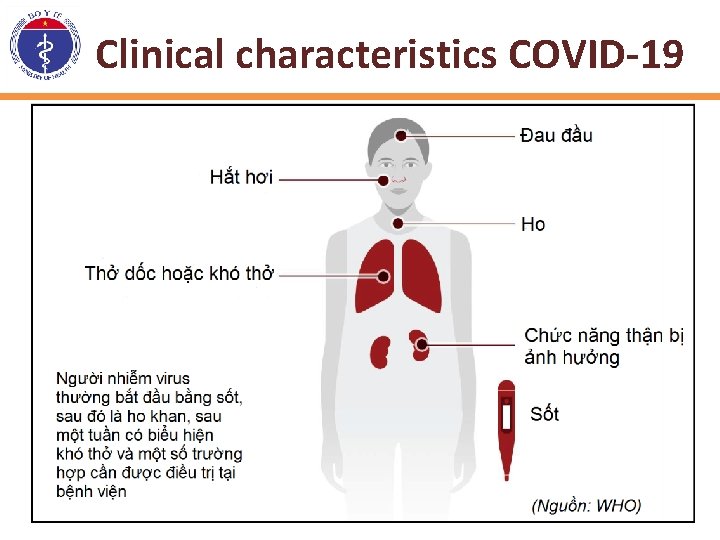
Clinical characteristics COVID-19

Clinical characteristics COVID-19 • Older adults and those with many underlying medical conditions (such as hypertension, cardiovascular disorders, diabetes, liver disorders and respiratory illnesses) may be at higher risk for developing serious symptoms.
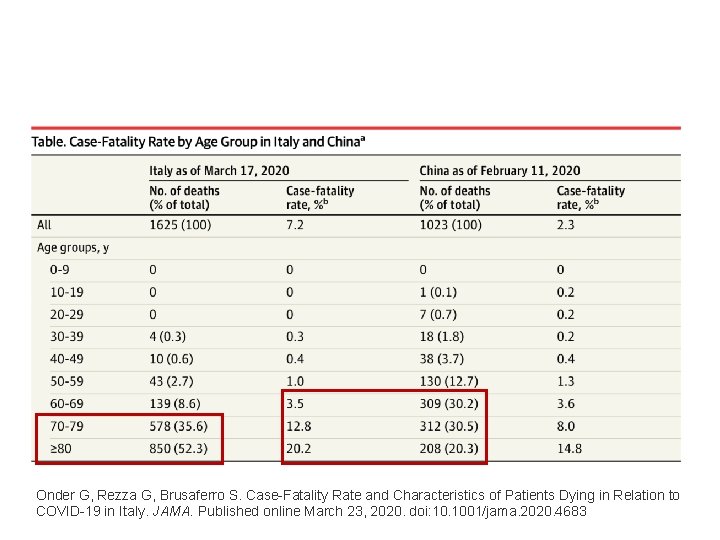
Onder G, Rezza G, Brusaferro S. Case-Fatality Rate and Characteristics of Patients Dying in Relation to COVID-19 in Italy. JAMA. Published online March 23, 2020. doi: 10. 1001/jama. 2020. 4683

Clicker Question Which of the following statements is best supported by the SARS-Co. V-2 epidemiological data you just saw? 1) SARS-Co. V-2 has a lower infection rate in people below age 60 than in people above age 60. 2) SARS-Co. V-2 has a higher infection rate in people below age 60 than in people above age 60. 3) SARS-Co. V-2 has a lower case fatality rate in people below age 60 than in people above age 60. 4) SARS-Co. V-2 has a higher case fatality rate in people below age 60 than in people above age 60.

Lesson 2. COVID-19 prevention measures for individuals and communities Training materials for final year healthcare students 03/2020

6 COMMON PREVENTION MEASURES Avoid close contact Avoid touching your eyes, nose and mouth Stay home when you are sick and get medical care Cover your cough or sneeze Clean surfaces with disinfectants Wash your hands often with soap and water

HOUSEHOLD SURFACES OFTEN CONTAMINATED WITH PATHOGENS

HOUSEHOLD SURFACES OFTEN CONTAMINATED WITH PATHOGENS

HOUSEHOLD SURFACES OFTEN CONTAMINATED WITH PATHOGENS

PERSONAL PREVENTION MEASURES • Wash your hands often with soap or a proper antiseptic solution (wash your hands for at least 20 seconds and the disinfectant solution contains at least 60% alcohol) • Clean contact surfaces frequently • Avoid crowded people • Avoid close contact with people who have respiratory symptoms (flu-like symptoms) • Regularly update news about the disease situation from official sources • Ministry of Health Hotlines:

PREVENTION MEASURES At school and workplace: • Wash your hands often • Regularly clean contact surfaces in classrooms and workplace During transport: • Wash your hands often • Keep a distance of at least 1 m from the person nearby • Follow the instructions of the relevant institutions and local authorities

PREVENTION MEASURES When you have symptoms such as sore throat, dry cough, sneezing, fever, and pain, you should: • Cough or sneeze to your elbow or tissue papers, then dispose the paper immediately and wash your hands. • If you feel unwell, stay at home and call your doctor or local health care center. • If you experience progressive shortness of breath, call your doctor and seek immediate care. • If there are signs of illness and you stay home, you need to eat and sleep separately from other people in the house, and use separate utensils such as glasses, dishes, etc.

HAND WASHING Routine handwashing protocol Notes: Wash your hands with soap and water when visibly soiled. Wash your hands for at least 30 seconds, repeat step 2, 3, 4, 5 at least 5 times

HOW TO WEAR MASK PROPERLY Wear surgical mask properly u Single se Surgical mask should be used once only Do not reuse single-use surgical mask Wear mask so that the colored side (blue/gray) facing outward Cover both your nose and mouth, press the metallic strip to fit your nose WHO NEED TO WEAR CLOTH MASK Healthy people, without respiratory symptoms such as fever, cough, shortness of breath, runny nose… When wearing mask, must not touch the outside of the mask When removing the mask, pull only the elastic straps to take off the mask, do not touch the outside face. Dispose the mask right away to a trash bin with a lid Wash your hands with soap and water, or use alcohol-based handrub after removing the mask WHEN TO WEAR CLOTH MASK When travel to crowded areas, such bus stations, train stations, markets, supermarkets, walking streets…

PRINCIPLES OF TREATMENT OF COVID-19 • Suspect cases must be hospitalized for confirmation testing. • All cases require isolation. • Symptomatic treatment, improving the physical condition and critical care when needed are important. • There are no specific vaccines and drugs yet.

GENERAL TREATMENT OF COVID-19 • Bed rest • Patient room should be well ventilated, preferably with a disinfection system. • Nose and throat hygiene, keep warm • Symptomatic treatment: Antipyretic, cough suppressant; drink enough water; fluid, electrolyte and nutrition balance; and improve physical condition. • Counseling, psychological support. • Closely monitor vital signs, detect respiratory failure, circulatory failure. • Severe patients must be treated at ICU.

Clicker Question A person finds out that they are positive for SARS-Co. V-2 even though they currently do not have symptoms. What preventative actions should they take to avoid transmitting their infection to other people? 1) Wear a mask, wash hands regularly, and take anti-SARSCo. V-2 drugs daily 2) Wear a mask, avoid close contact with other people, and take anti-SARS-Co. V-2 drugs daily 3) Wash hands regularly, avoid close contact with other people, and take anti-SARS-Co. V-2 drugs daily 4) Wear a mask, wash hands regularly, and avoid close contact with other people

Implementing Isolation to Prevent COVID 19 (Decree 963/QĐ-BYT on 18/3/2020)

SUSPECT CASE A patient with one of the following symptoms: fever, cough, shortness of breath or pneumonia, AND one of the following epidemiological factors : 1. A history of travel to or residence in another countries, territories reporting community transmission of COVID-19 disease (according to WHO reports) during the 14 days after entry into Vietnam.

SUSPECT CASE A patient with one of the following symptoms: fever, cough, shortness of breath or pneumonia, AND one of the following epidemiological factors : 2. A history of travel to or residence in a location inside Vietnam with an outbreak of COVID-19 disease during the 14 days prior to symptom onset Pasteur Institutes and CDCs update the outbreak location lists daily within their administrative regions, and report to General Department of Preventive Medicine to announce to all local health centers.

SUSPECT CASE A patient with one of the following symptoms: fever, cough, shortness of breath or pneumonia, AND one of the following epidemiological factors : 3. Having been in contact with a confirmed or suspect COVID-19 case in the last 14 days prior to symptom onset

CONFIRMED CASE • Is a suspect case or any persons with a positive confirmation test result of SARS-Co. V-2 infection performed by laboratories authorized by the Ministry of Health. (As of now, there are 22 laboratories authorized by Ministry of Health)

CLOSE CONTACT A close contact is a person who has a contact within 2 meters with a confirmed case or a suspect case during the illness phase, including: 1. Who lives in the same household, same house with confirmed case or suspect case during the illness phase. 2. Who works in the same working group or stays in the same workplace room with confirmed cases or suspected cases during the disease period. 3. Who belongs to a same group: traveling, business trips, playing, parties, meetings. . . with confirmed cases or suspected cases during the disease period.

CLOSE CONTACT A close contact is a person who has a contact within 2 meters with a confirmed case or a suspect case during the illness phase, including: 4. Who sits in the same row and within two rows of seats (front and rear) on the same means of transport (ships, cars, airplanes, ships. . . ) of a confirmed case or a suspect case during illness phase. In some specific cases, depending on the results of epidemiological investigations, the health authority will decide to expand the list of close contacts amongst passengers traveling in the vehicle.

CLOSE CONTACT A close contact is a person who has a contact within 2 meters with a confirmed case or a suspect case during the illness phase, including: 5. Who has had close face-to-face contact with a confirmed or suspect case during an illness phase in any other situations.
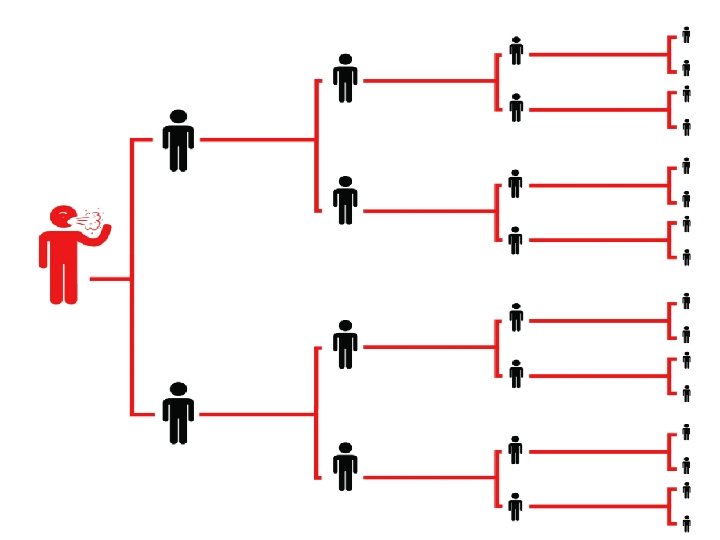
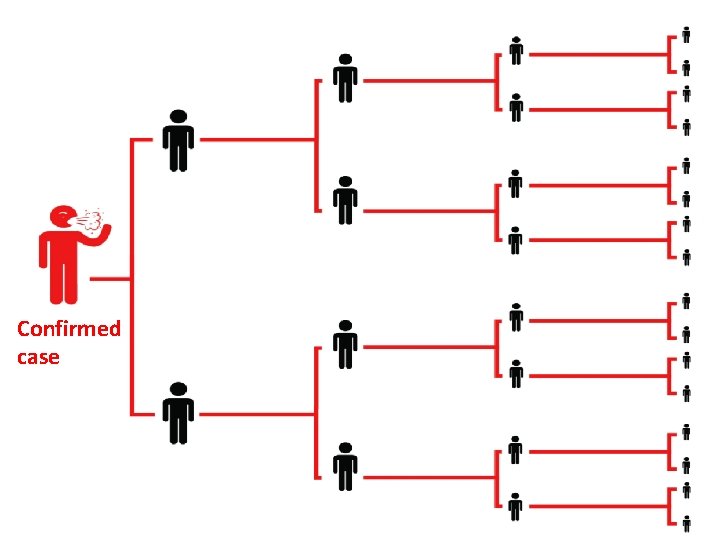
Confirmed case
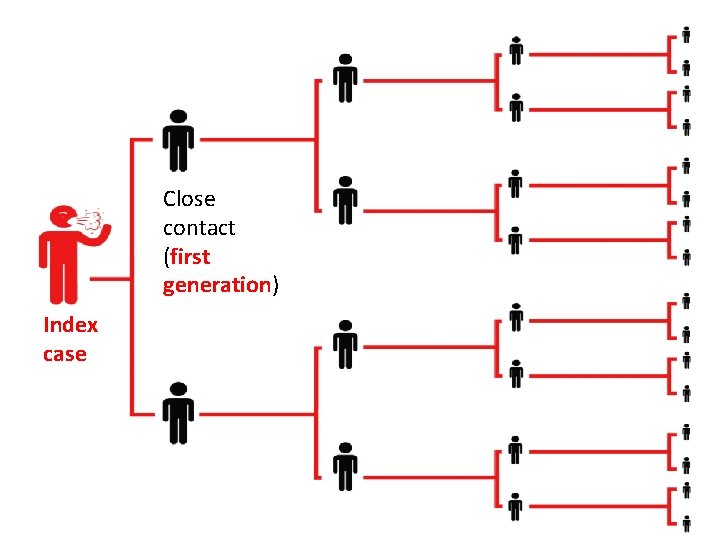
Close contact (first generation) Index case
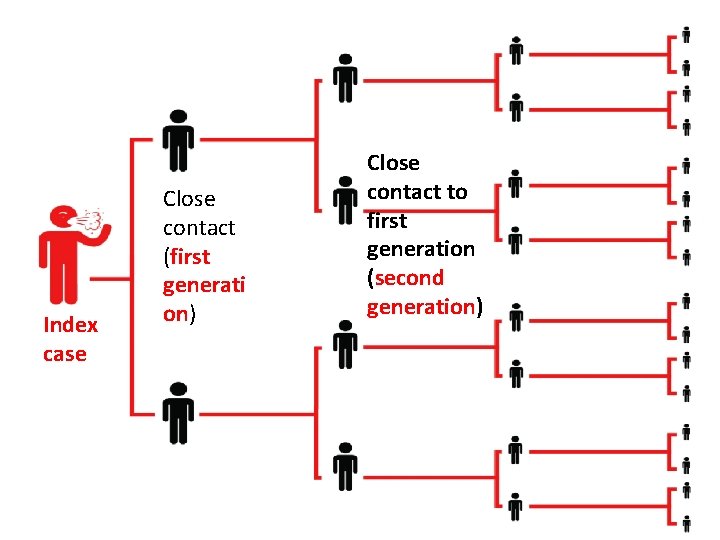
Index case Close contact (first generati on) Close contact to first generation (second generation)

Clicker Question According to the criteria we just discussed, which of the following people best fits the definition of a “suspected case” for COVID-19? 1) A patient who developed a cough 2 days ago and returned 10 days ago from a holiday in a province of Vietnam that currently has a COVID-19 outbreak. 2) A patient who developed a cough 2 days ago and returned 20 days ago from a holiday in a province of Vietnam that currently has a COVID-19 outbreak. 3) A patient who developed diarrhea 2 days ago and is currently living in an apartment with their brother who tested positive for SARS-Co. V-2 10 days ago. 4) A patient who developed diarrhea 2 days ago and is currently living in an apartment with their brother who tested positive for SARS-Co. V-2 20 days ago.

Management of confirmed cases • Strict isolation and treatment at medical facilities, minimize complications and deaths. • Limit patient referrals to avoid spreading unless beyond the current facility’s capacity. • Treat according to the guidance of the Ministry of Health. • Isolate until the patient is cured and discharged.

Management of close contacts of a confirmed case (Round 1 contact) 1. Investigate, review, make a list of all people in close contact with the confirmed case to record information about home address, place of residence, personal phone number; names and phone numbers of family members when needed to communicate. 2. 3. Isolate at health facilities for 14 days from the last exposure to the confirmed case. In cases where health facilities do not have adequate isolation space, people living in the same households, in the same house with the confirmed case shall be prioritized to be isolated at health facilities, other close contacts shall be isolated at Concentrated isolation facility reserved for close contacts. 3. Obtain specimen for SARS-Co. V-2 test.

Management of close contacts of a confirmed case (Round 1 contact) Obtain specimen for SARS-Co. V-2 test. • If the test result is positive for SARS-Co. V-2, treat as a confirmed case. • If the test result is negative for SARS-Co. V-2, continue isolation, daily health monitoring (measurement of body temperature, detection of symptoms) at health facilities or concentrated isolation facilities for 14 days from the last exposure to the confirmed case. During the monitoring process, if symptoms of suspected disease appear, continue to sample SARS-Co. V-2 samples. • If no suspected symptoms appear, the isolation end after 14 days from the last exposure to the confirmed case

Management of close contacts of a close contact (Round 2 contact) Home self-isolation and instruction on how to selfprevent the disease and monitor health while waiting for test results of first-round contacts: • If the test result of the first-round contact is positive for SARS-Co. V-2, the isolation level of the secondperson contact should be upgraded to the first-round contact. • If the test result of the first-round contact is negative for SARS-Co. V-2, the second-round contact isolation is ended.

Clicker Question A patient was just confirmed to be positive for SARS-Co. V-2. You do tracing to find their first and second round contacts. Which of the following answers is the best description of how you should manage these contacts? 1) 2) 3) 4) Isolate first round contacts in a health facility, notify second round contacts that they may be infected, and do a SARS-Co. V-2 test on all first and second round contacts Isolate first round contacts in a health facility, notify second round contacts that they may be infected, and do a SARS-Co. V-2 test on all first round contacts Isolate first round contacts in a health facility, isolate second round contacts at home, and do a SARS-Co. V-2 test on all first and second round contacts Isolate first round contacts in a health facility, isolate second round contacts at home, and do a SARS-Co. V-2 test on all first round contacts

Management of suspect cases Have the patient wear a mask and transfer to a treatment facility separated from the treatment area for confirmed case. Depending on the result of the SARS-Co. V-2 test, the case should be managed as follows: - If the suspect case is positive for SARS-Co. V-2, then transfer the patient to treatment and isolation area as a confirmed case. - If the suspect case is negative for SARS-Co. V-2, the patient should be transferred to a separate area exclusively designated for patients with a negative test result. .

Management of suspect cases If symptoms resolve after 14 days from the last exposure to the infection source, the patient will be discharged from the hospital. If the patient still has symptoms after 14 days from the last exposure to the infection source, a second sample will be collected; if the second result is still negative for SARS-Co. V-2, the patient will be transferred to another area and treated like other common diseases.

Management of close contacts of a suspect case Home self-isolation and instruction on how to self-prevent the disease and monitor health while waiting for test results of the suspect case: - If the test result of the suspect case is positive for SARS-Co. V-2, upgrade the isolation level of these people to first round contacts. - If the test result of the suspect case is negative for SARS-Co. V-2, the isolation of the close contact of the suspect case is ended.

ISOLATION AT HOME OR AT RESIDENCE Medical isolation at home, at place of residence: private house; apartment; collective housing; dormitories for schools, industrial parks and enterprises; hotel rooms, motels, inns and guest rooms of agencies and units.

ROOM REQUIREMENTS ON ISOLATION AT HOME • It is best to stay in a private room, if there is no private room, the bed of the isolated person should be at least 2 meters away from the beds of other family members or in the same residence, and away from the common areas. • Ensuring good ventilation, do not use air conditioning, cleaning regularly, limiting furniture in the room. • If possible, choose a room at the end of the block, at the end of the wind, away from crowded areas. • Having toilets, hand soap, clean water. • Having trash cans with lids.

IMPLEMENTATION TO ISOLATE AT HOME • People's Committees of communes, wards where there are isolated people • Management board / managers / owners of apartments, dormitories, hotels, motels, hostels • Medical staff • People are isolated • Members of the household, residence

THINGS FOR INDIVIDUALS TO DO WHEN ISOLATED AT HOME • Complying with self-quarantine at the place of residence or at home within the isolated time limit and have a commitment with local authorities (Sample attached). • Take your own temperature and monitor your health daily. Record measurement results and general health status on the daily health monitoring sheet. Notify health staff of commune level about the results of their temperature measurements and health status everyday • Immediately notify the commune health worker assigned to monitor as soon as having one of the symptoms: fever, cough, sore throat, shortness of breath. • Restricting going out of private rooms, limiting direct contact with family members from home or places of residence as well as others;

THINGS FOR INDIVIDUALS TO DO WHEN ISOLATED AT HOME • Do not leave the place of residence or home during the isolation period. • Take personal hygiene measures, wear masks, regularly wash hands with soap and clean water or other disinfectant solution. Do not share personal belongings: bowls, chopsticks, spoons, cups, toothbrushes, towels, etc. • Collecting used masks, towels, tissues from nose and mouth into separate garbage bags for disposal according to regulations. • Do not eat together, do not sleep with other family members, at the same lodging, or accommodation. • Make sure to have adequate nutrients, drink enough water, physical activities, gentle exercise on the spot.

ISOLATION AT CONCENTRATED ISOLATION FACILITIES Medical isolation at concentrated isolation establishments under the 2007 Law on Prevention of Infectious Diseases • Army and police barracks; • School dormitories; • Residential areas of factories and enterprises; • New apartment buildings have not been put into use; • Hotels, motels, guest houses, resorts, . . . • Schools; • Commune health facilities; • Other areas may be used as isolation facilities.

REQUIREMENTS FOR CONCENTRATED ISOLATION FACILITIES • Ensuring essential living conditions: electricity, water, toilet area, bathroom. • Ensuring good ventilation. • Ensure security and safety. • Ensure fire prevention. • It is best to be separate from residential areas or have separate fences. • Convenient for traveling, transporting isolated people, providing logistics and transporting waste for processing. • If possible, providing television and internet for each isolated room.

ESTABLISHING CONCENTRATED ISOLATION FACILITIES 1. Decision on establishment of isolation facilities 2. Arrangement and organization in isolation facilities 3. Organization of isolation: 1. Provincial People's Committee 2. Steering Committee for prevention and control of COVID 19 in provinces and cities 3. Isolated facilities 4. Managers and owners of facilities are used as concentrated isolation areas 5. Healthcare workers and staff of isolated facility 6. People are isolated

THINGS FOR INDIVIDUALS TO DO WHEN ISOLATED IN CONCENTRATED ISOLATION FACILITIES • Complying with medical isolation according to regulations of isolation facilities and committing to follow medical isolation measures (the attached form). • Executing personal hygiene measures, wearing masks, washing hands with soap or other antiseptic solution regularly. Do not spit • Being measured of body temperature at least 2 times (morning, afternoon) a day and practicing health self-monitor daily. • Notifying healthcare personnel assigned to follow up as soon as having one of the suspected symptoms: fever or cough, sore throat, difficulty breathing.

THINGS FOR INDIVIDUALS TO DO WHEN ISOLATED IN CONCENTRATED ISOLATION FACILITIES • Restricting going out of the isolation room and restricting direct contact with other people in the isolation area, everyday • Do not gather to talk, do not gather to eat, do not organize games in the room, the corridor, in the yard in the isolation section. • Washing personal items such as clothes, dishes, glasses with soap or regular detergent. • Do not share personal items such as mugs, cups, bowls, chopsticks, spoons, towels, toothbrushes. . .

THINGS FOR INDIVIDUALS TO DO WHEN ISOLATED IN CONCENTRATED ISOLATION FACILITIES • Ensuring adequate nutritional intakes, drinking enough water, light exercising, gentle physical activities on the spot. • Collecting used masks, napkins, tissues touched nose and mouth into infectious waste containers. • Collect other domestic waste into household waste bins.

NOTICES FOR CONCENTRATED ISOLATION FACILITIES • Prevention of infection to officials and employees in isolation establishments • Handling when detecting cases of confirmed or suspect COVID-19 in isolation facilities (under the guidance of Decision 878 / QĐ-BYT dated 12/3/2020) • Complete the task of a concentrated isolation facility

Clicker Question Which of the following answers is the best description of actions that should be taken by individuals isolated at home AND individuals isolated in a concentrated isolation facility? 1) 2) 3) 4) Stay isolated in a room that is well-ventilated and air-conditioned, wash items regularly and avoid sharing them with others, monitor temperature and symptoms regularly, and report suspected COVID-19 symptoms to the appropriate health worker Stay isolated in a room that is well-ventilated and not air-conditioned, wash items regularly and avoid sharing them with others, monitor temperature and symptoms regularly, and report suspected COVID-19 symptoms to the appropriate health worker Stay isolated in a room that is well-ventilated and air-conditioned, engage in gentle exercises with other individuals under isolation, monitor temperature and symptoms regularly, and report suspected COVID-19 symptoms to the appropriate health worker Stay isolated in a room that is well-ventilated and not air-conditioned, engage in gentle exercises with other individuals under isolation, monitor temperature and symptoms regularly, and report suspected COVID-19 symptoms to the appropriate health worker

Lesson 3. Sampling, Storage And Transporting Of Suspected SARS-Co. V-2 Specimens Training materials for final year healthcare students 03/2020

Main topic 1. 2. 3. 4. 5. Specimens Time to collect specimens The process of donning and doffing PPE Methods of collecting specimens Preservation, packaging and transport of specimens to the laboratory 6. Biosecurity in preservation, packaging and transportation of specimens

Specimens • Note: Must be trained in biosafety before collecting samples • There must be respiratory samples, blood samples may be added • Upper respiratory tract specimens: - Oropharyngeal fluid - Oral rinse fluid • Lower respiratory tract specimens: - Sputum - Alveolar, endotracheal, pleural fluid - Tissues of the lungs, bronchi, alveoli • Whole blood specimen (3 -5 ml)
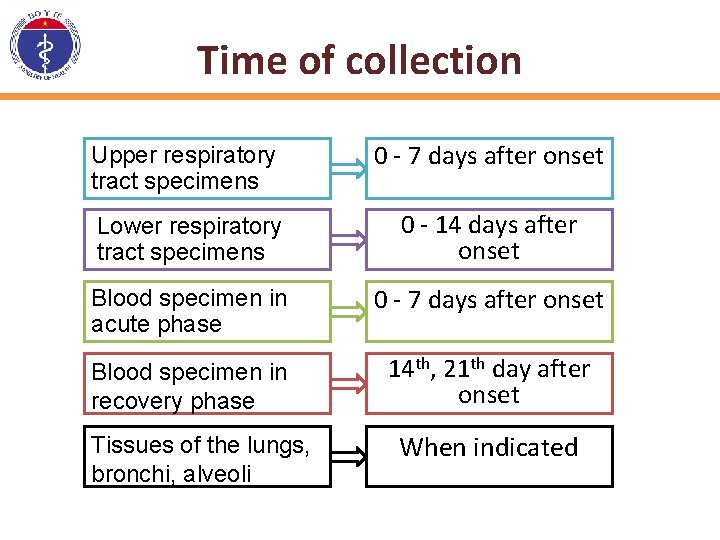
Time of collection Upper respiratory tract specimens 0 - 7 days after onset Lower respiratory tract specimens 0 - 14 days after onset Blood specimen in acute phase 0 - 7 days after onset Blood specimen in recovery phase 14 th, 21 th day after onset Tissues of the lungs, bronchi, alveoli When indicated

Specimen collection – Preparing equipment • Sterile swab with soft and hard • handle; • • Tongue depressor; • • 15 ml pyramid centrifuge tube, • containing 2 -3 ml transport • medium; • • Plastic vial (50 ml Falcon tube) or nylon bag for packaging the • specimen; • Sterile bandages and gauze; • • Alcohol wipe, writing pen. . . ; Personal protective equipment Eye protection glasses; Gloves; Respirator (N 95, . . . ); 10 ml sterile syringe; Sterile collection tubes (with or without anticoagulant); Arm strap, cotton swab, alcohol. . . ; Sample storage flask.

Procedure to don PPE Step 1: Hand hygiene. Step 2: Wear boots / shoe covers. Step 3: Wear pants and gown (wear an apron if indicated). Step 4: Wear a mask. Step 5: Wear glasses Step 6: Wear a hood that covers hair, head, ears, and mask strap. • Step 7: Wear a face shield or goggles (if having strap, must be outside of the hood) • • •

Procedure to doff PPE (1) Separate gown, pants and hood • Step 1: Remove gloves. When removing, turning gloves inside out, discard in the waste container. If an apron is used, removing the apron, undoing the lower tie first and then the upper tie, turning the apron inside out, and discard in the waste container. • Step 2: Hand hygiene. • Step 3: Remove the gown, turning the gown inside out and discard in the waste container. • Step 4: Hand hygiene.

Procedure to doff PPE (2) • Step 5: Removing shoes and boots or shoe covers at the same time, turn the inside of the pants out, discard in the waste container. If wearing boots, place the boots in a bucket with disinfectant solution. • Step 6: Hand hygiene. • Step 7: Removing goggles or face shield. • Step 8: Hand hygiene. • Step 9: Removing hood by running your hand inside the hood. • Step 10: Removing mask (hold the strap behind the head or behind the ear). • Step 11: Hand hygiene.

Procedure to doff PPE (3) Coveralls with hood, pants and tops • Step 1: Remove gloves. When removing, turning gloves inside out, discard in the waste container. If an apron is used, removing the apron, undoing the lower tie first and then the upper tie, turning the apron inside out, and discard in the waste container. • Step 2: Hand hygiene. • Step 3: Removing goggles or face shield. • Step 4: Hand hygiene. • Step 5: Remove hoods, tops, pants. When removing, turning the coverall inside out and discard in the waste collection bin. • Step 6: Hand hygiene.

Procedure to doff PPE (4) Coveralls with hood, pants and tops • Step 7: Removing boots or shoe covers at the same time, turn the inside of the pants out, discard in the waste container. If wearing boots, place the boots in a bucket with disinfectant solution. • Removing goggles or face shield. • Step 8: Hand hygiene. • Step 9: Removing mask (hold the strap behind the head or behind the ear). • Step 10: Hand hygiene.
Procedure to don / doff PPE Wearing surgical masks • Remove the mask strap, do not touch the mask, discard in the waste collection bin • Hand hygiene

Wearing respirator (N 95) • Hand hygiene • Opening the package, place the mask on the palm of the hand, the metal edge hugging the nose bridge, facing forward, let the strap drop freely under the hand • Place the mask under the chin, the nose cover up • Pull the upper strap over the head and place it on the occipital area, above the ears. Pull the lower strap over the head and place it at the back of the neck, under the ears. Notice not to overlap two straps behind the head • Check and adjust the strap if twisted • Place the tip of the index fingers of the two hands at the tip of the nose, pressing the nose cover so that the mask fits the nose • Check for fitting of mask (inhale / exhale - create negative pressure) Removing respirator: • Removing the lower strap by holding the strap behind the head, then removing the top strap over the head, do not let your hand touch the mask when removing. • Hand hygiene

Clicker Question A healthcare worker has just collected a SARS-Co. V-2 specimen from a patient and is currently wearing PPE that includes a separate hood, gown, and pants. Which answer describes the correct order for doffing their PPE? 1) Remove gloves and perform hand hygiene, Remove gown and perform hand hygiene, Remove shoe/boot/shoe covers and perform hand hygiene, Remove goggles/face shield and perform hand hygiene, Remove hood, Remove mask and perform hand hygiene 2) Remove gloves and perform hand hygiene, Remove goggles/face shield and perform hand hygiene, Remove hood, Remove mask and perform hand hygiene, Remove shoe/boot/shoe covers and perform hand hygiene, Remove gown and perform hand hygiene 3) Remove gloves and perform hand hygiene, Remove goggles/face shield and perform hand hygiene, Remove hood, Remove mask and perform hand hygiene, Remove gown and perform hand hygiene, Remove shoe/boot/shoe covers and perform hand hygiene 4) Remove gloves and perform hand hygiene, Remove gown and perform hand hygiene, Remove goggles/face shield and perform hand hygiene, Remove hood, Remove mask and perform hand hygiene, Remove shoe/boot/shoe covers and perform hand hygiene
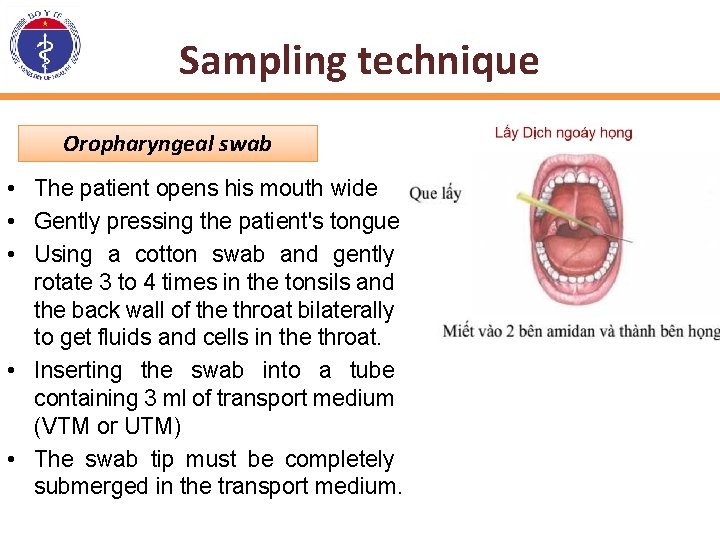
Sampling technique Oropharyngeal swab • The patient opens his mouth wide • Gently pressing the patient's tongue • Using a cotton swab and gently rotate 3 to 4 times in the tonsils and the back wall of the throat bilaterally to get fluids and cells in the throat. • Inserting the swab into a tube containing 3 ml of transport medium (VTM or UTM) • The swab tip must be completely submerged in the transport medium.
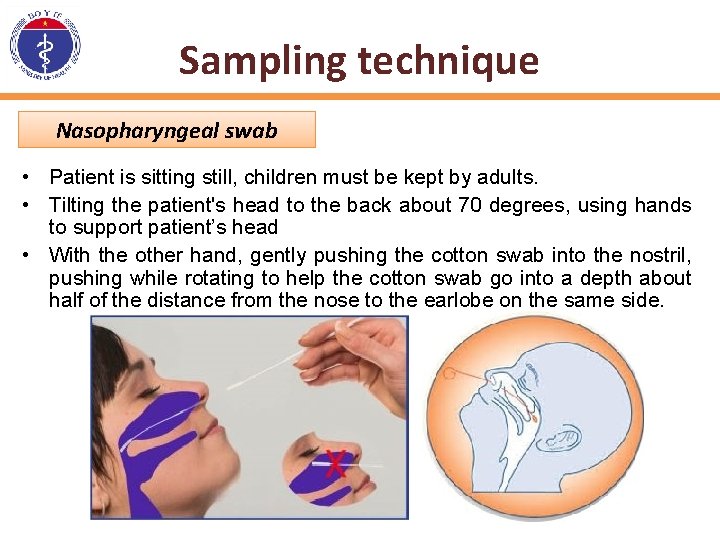
Sampling technique Nasopharyngeal swab • Patient is sitting still, children must be kept by adults. • Tilting the patient's head to the back about 70 degrees, using hands to support patient’s head • With the other hand, gently pushing the cotton swab into the nostril, pushing while rotating to help the cotton swab go into a depth about half of the distance from the nose to the earlobe on the same side.

Sampling technique Nasopharyngeal swab • Holding the swab at the sampling site for 5 seconds • Slowly rotating and removing the cotton swab • Placing the tip of the cotton swab in the specimen container containing the transporting medium, breaking the swab handle to have a suitable length • Closing the lid, tightening, wrapping with paraffin paper • Storing the samples in a temperature of 2 -8 ° C before transferring to the laboratory. • If the specimen is not transported to the laboratory within 72 hours must be stored at -70 ° C and then must be kept frozen during transport to the lab

Sampling technique Oral rinse fluid • Patients gargle with 10 ml of rinsing solution (normal saline). • Rinsing fluid is collected into a beaker or petri dish and diluted in a ratio of 1: 2 in a virus storage medium. Endotracheal tube fluid • Patients are intubated • Using a suction tube, placing in the endotracheal tube and use syringe to obtain fluid. • Put the fluid into a tube containing viral storage medium.

Sampling technique Blood specimen • Using a sterile needle and syringe, take 3 -5 ml of venous blood, transfer into a container (containing EDTA anticoagulant for whole blood sample), storage at 4 ° C for 24 hours.

Sampling technique Notice • Labelling with name, age, address, type of specimen, date of sample collection on the sample container. • Lower respiratory specimens (endotracheal, alveolar, pleural fluid) must be coordinated with clinicians during the collection of patient samples.

Disinfecting of sampling area • PPE: put in a special plastic bag used for medical waste that is able to withstand high temperatures, along with infected equipment (using new gloves and masks). • Tie and using dry wet at 120 ° C / 30 minutes before discarded with other medical waste or can be burned in waste incinerators at district hospital. • Hand washing with soap and disinfecting with chloramine 0. 1% of all tools and sampling areas; thermos for transporting specimens to the laboratory.

Specimen storage • Shipping as soon as possible, within 48 hours: storing at 2 -8 ° C, and transfer to laboratory. • Shipping after 48 hours: storing at -70 ° C • Do not store in the freezer compartment of the refrigerator or -20 ° C. • Whole blood specimens can be stored at 2 -8 ° C for 5 days.

Specimen packaging • Specimens must be carefully packed in 3 protective layers (WHO) while transporting • Tightening the specimen tube cap, wrap with paraffin paper (if any), wrap each tube with absorbent paper. • Putting the tube in the shipping bag (or bottle with a tight lid). • Wrapping the specimen bag with absorbent paper or cotton dampening with disinfectant (chloramine B. . . ), or placing the specimen pack in the second nylon bag and tying the bag. • The records of specimens are packed together into a final nylon bag, tied tightly, transferred to a cold thermos, outside with the logo printed on (logo: biological specimens, not to be flipped reverse – following World Health Organization’s regulations) when shipping.

Specimen transport • Lab units receiving samples must be from the list of laboratories allowed to test new strains of corona virus (SARS-Co. V-2) according to the regulations of the Ministry of Health. • Notifying the lab of the delivery date and expected time of arrival of the specimen • Specimens are transported to the testing room by road or airway as soon as possible. • Avoid spilling or breaking the tube samples during transport. • Specimens should be stored at 4 ° C when transported to the laboratory, avoiding the thawing process many times that could reduce the quality of the specimens.

Clicker Question Which statement about collecting a nasopharyngeal swab is correct? 1) The sample site should be swabbed with a cotton swab for 5 seconds, the cotton swab should be submerged in the tube of transport medium for 5 seconds before you discard the full swab, and the tube of transport medium should be stored at -20 °C during transport. 2) The sample site should be swabbed with a cotton swab for 5 seconds, the cotton swab should be submerged in the tube of transport medium and the end should be broken off so the lid can be sealed, and the tube of transport medium should be stored at -20 °C during transport. 3) The sample site should be swabbed with a cotton swab for 5 seconds, the cotton swab should be submerged in the tube of transport medium for 5 seconds before you discard the full swab, and the tube of transport medium should be stored at 2 -8°C during transport. 4) The sample site should be swabbed with a cotton swab for 5 seconds, the cotton swab should be submerged in the tube of transport medium and the end should be broken off so the lid can be sealed, and the tube of transport medium should be stored at 2 -8 °C during transport.

Lesson 4: Management And Treatment Of Confirmed And Suspected Cases Of COVID-19 At Medical Facilities Training materials for final year healthcare students 03/2020

Main topics 1. 2. 3. 4. Patient triage Suspected and confirmed case triage General care and monitoring measures Discharge criteria

Patient triage Triaging on clinical manifestation a) Upper respiratory tract infection b) Mild pneumonia c) Severe pneumonia d) ARDS • Milde ARDS: 200 mm. Hg < P/F ≤ 300 mm. Hg (with PEEP or CPAP ≥ 5 cm H 2 O). • Moderate ARDS: 100 mm. Hg <P/F ≤ 200 mm. Hg (with PEEP ≥ 5 cm. H 2 O). • Severe ARDS: P/F ≤ 100 mm. Hg (with PEEP ≥ 5 cm. H 2 O) e) Sepsis f) Septic shock

General care, monitoring and treatment measures (1) 1. 2. 3. 4. 5. 6. 7. Bed rest. Patient’s room should be well ventilated. Air filtration systems or other disinfection prevention methods, such as ultraviolet lamps (if available) could be applied. Keeping pharyngeal and oral hygiene, moisturizing the nose with normal saline solution, rinsing the mouth and mouth with the usual oral rinse solutions. Keeping body warm. Drinking enough water, maintaining fluid and electrolyte balance. Being cautious when giving intravenous fluid for pneumonia patients with no sign of shock. Ensuring nutrition and improving fitness. For critically ill patients, following the nutrition guidelines issued by the Vietnam Association of Emergency Critical Care Medicine and Medical Toxicology. Using antipyretic agents if having high fever, paracetamol can be used at doses of 10 -15 mg / kg / time, not to exceed 60 mg / kg / day for children and no more than 2 grams / day for adults.

General care, monitoring and treatment measures (2) 8. 9. 10. 11. 12. 13. Relieving cough with common cough suppressants if needed. Providing assessment, treatment and prognosis of other chronic conditions (if any). Providing counseling, psychological support, encouraging patients. Closely monitoring the vital signs, detecting signs of severe disease progression such as respiratory failure, circulatory failure for timely interventions. Providing adequate and timely laboratory tests and routine investigations depending on the patient's condition for diagnosis, prognosis, and follow-up. At the treatment facilities, there must be a set of minimum equipment for emergency care: oxygen saturation monitor machine, oxygen supply system / tank, supplemental oxygen devices (nasal cannula, simple face masks, non-rebreather masks with reservoir bag), bag valve masks (ambu bag), and endotracheal intubation equipment with different sizes suitable for all ages.

General care, monitoring and treatment measures Mild - Moderate • Fowler’s position, open airway • Oxygen cannula nasal Severe • CPAP, high flow nasal oxygen , Bi. PAP • Contraindications for NCPAP, Bi. PAP: patients with hemodynamic disorder, multiorgan failure, disorders of consciousness • No improvement after 1 h intubation Critical - ARDS • Required intubation • ARDS: Protective lung ventilation Target p. H >= 7. 20 Severe ARDS, considering prone ventilation > 12 h/day Moderate – severe ARDS : high PEEP • Sedation / muscle relaxant? • Fluid balance

Other treatment measures ü Antibiotics ü Antiviral drug ü Systemic Corticosteroids ü Extra corporeal dialysis ü Intravenous Immunoglobulin ü Interferon ü Respiratory rehabilitation

Discharge criteria Discharge when – No fever for at least 3 days – Good condition, normal vital signs, normal lab tests – 2 negative specimen samples for SARS-Co. V-2 Post-discharge follow-up – Monitor body temperature 2 times / day – If temperature > 38 o. C for 2 consecutive measures / other abnormalities contact health facilities

Clicker Question You are treating a COVID-19 patient who has mild pneumonia. Which of the following is the best action to treat them? 1) Keep the patient in a cold, air-conditioned room 2) Limit the amount of water that the patient drinks 3) Ensure that the patient receives adequate nutrition 4) Avoid having conversations with the patient

One Minute Paper Today we discussed COVID-19 epidemiology and clinical characteristics, protocols for managing suspected cases, and protocols for managing and treating confirmed cases. What questions do you still have? Please write them down so you can ask your instructor later or remember to look up their answers later.

Thank you!
- Slides: 110