Kingston Hospital Grand Rounds Pediatric Brain Tumor Presenting

Kingston Hospital Grand Rounds Pediatric Brain Tumor Presenting as Dizziness & Otitis Media Moderator / ICU: Jeremy Barnett MD ED: Amy Gutman MD Neurology: Janet Tamai MD

Case Presentation ~ Chief Complaint • 8 yo male presents to the ED with the complaint of weakness and dizziness

Initial Presentation • 8 yo M, JS, presents at 0840 to room 19 via private vehicle • Nurse immediately came to Core 1 asking me to see patient rather than wait for 0900 MD • Patient laying limp on the stretcher, with mother at bedside. Maintaining airway, but clearly struggling to move & communicate • Mother states that he had been diagnosed with an ear infection, but today “was dizzy, couldn’t walk & was wobbly”

History of Present Illness • Mother reports 4 days ago child vomited once, dry heaving yesterday but otherwise acting / eating “normally” except for complaining of dizziness • Mother called PCP yesterday, who advised them to start antihistamines due to history of similar episodes with ear infections / congestion • Mother also called child’s neurologist / autism specialist who stated “don’t worry about JS’s symptoms”, but would see him in the office if he worsened • Last night child having difficulty walking, unable to stand unassisted, & unable to stand this am due to “dizziness”

Case Presentation ~ SHx, FHx, PMH • Social: • Non-smoking home • 2 nd grade • Family History • No pertinent family history • Allergies • NKDA • Medications • Risperdal, lorazepam • PMH • Full-term • Autism, OM

Review Of Systems (Per Mother) • General: Anxious, toxic, ill appearing & unable to communicate • HEENT: Ear “fullness”, nasal congestion, no visual complaints • Pulm: • CV: (-) SOB, DOE, PND (-) CP, palpitations • GI: (+) vomited once yesterday • Skin: (-) rashes, lesions
Physical Examination • General: • Awake & interactive. Appears “scared”, responds to staff, maintains airway • Vitals: • T 98. 3 oral, HR 98, Resp 16, Wt 35. 7 kg BP 124/71, Pulse Ox 100% ra • Skin: • Warm, dry, (-) rash, (-) temp differential • HEENT: • (-) swelling, tenderness, LAD, tongue deviation. TMs unremarkable • Pulm: • CTA AF BL, no distress • CV: • S 1 S 2 RRR (-) MRG • GI: • Soft NT ND (+) BSAQ • Neuro: • Mild right eye deviation which corrects to center. PERRLA at 3 mm = BL & briskly reactive; otherwise CN 2 -12 intact • LUE grip 3/5, LE BL 5/5 • (-) Babinski BL • Falls to left side when tries to ambulate • (+) vertical nystagmus BL 5 beat

What Is Your Differential? What Do You Want To Do Next?

Labs • CBC: Unremarkable • CMP: Unremarkable • Coags: Unremarkable • Urinalysis: • Cardiacs: Ordered, Not collected Unremarkable • ESR: Pending at time of transfer; slight elevation • Lactic Acid: 22 (elevated) • ED Lyme: Ordered, not sent
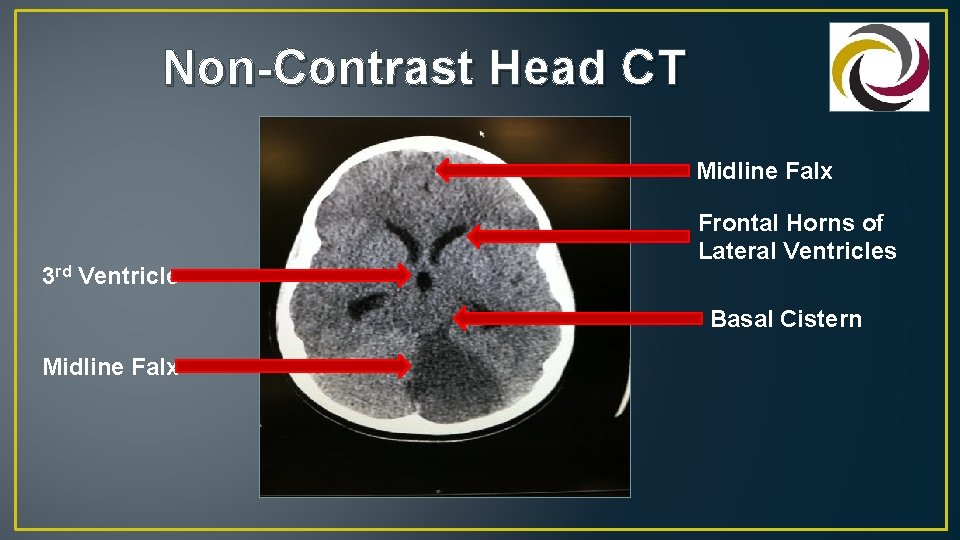
Non-Contrast Head CT Midline Falx 3 rd Ventricle Frontal Horns of Lateral Ventricles Basal Cistern Midline Falx
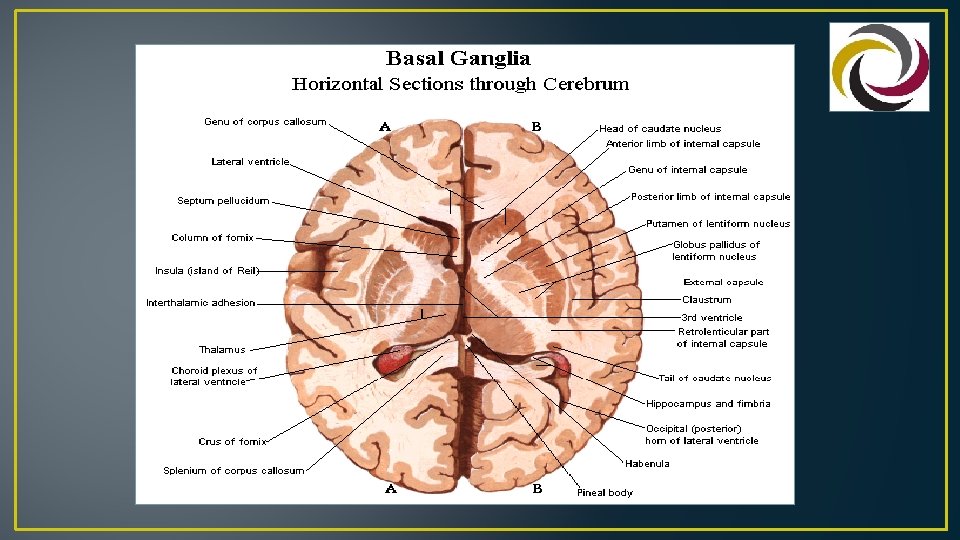
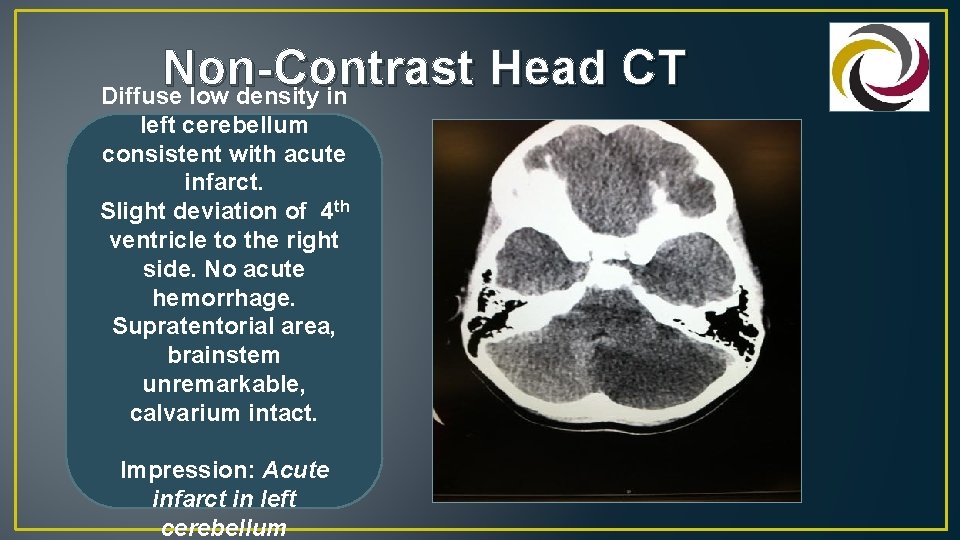
Non-Contrast Head CT Diffuse low density in left cerebellum consistent with acute infarct. Slight deviation of 4 th ventricle to the right side. No acute hemorrhage. Supratentorial area, brainstem unremarkable, calvarium intact. Impression: Acute infarct in left cerebellum

ED Course • Case discussed with Dr P, pediatric neurologist at Albany Medical Center who advised on acute ED management • Suspected underlying cerebellar mass due to CT appearance • Asked us to not wait for MRI, & rapidly transport • Interventions: • Oxygenation & airway protection • NS IVF pediatric bolus • Keppra 250 IV • Signal 9 transfer • Notified patient’s pediatric neurologist & pediatrician
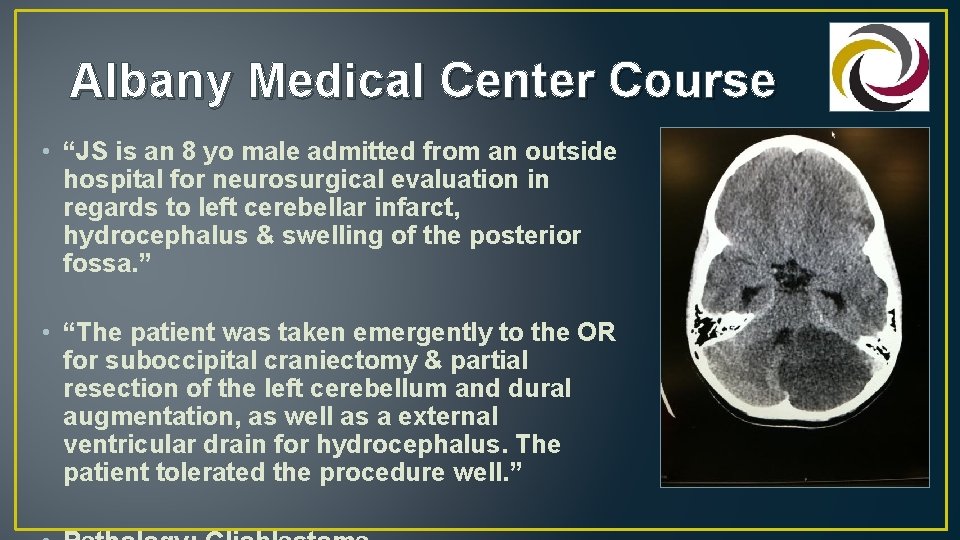
Albany Medical Center Course • “JS is an 8 yo male admitted from an outside hospital for neurosurgical evaluation in regards to left cerebellar infarct, hydrocephalus & swelling of the posterior fossa. ” • “The patient was taken emergently to the OR for suboccipital craniectomy & partial resection of the left cerebellum and dural augmentation, as well as a external ventricular drain for hydrocephalus. The patient tolerated the procedure well. ”
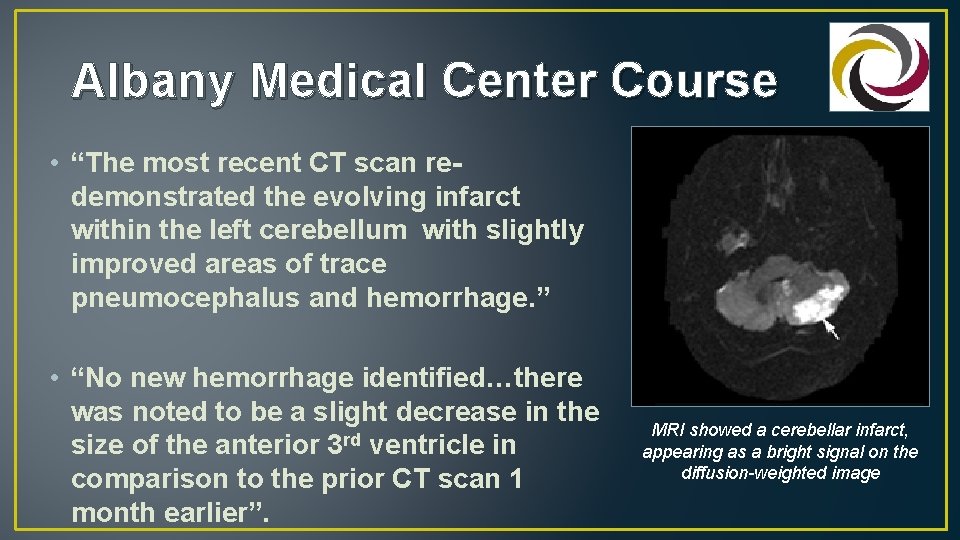
Albany Medical Center Course • “The most recent CT scan redemonstrated the evolving infarct within the left cerebellum with slightly improved areas of trace pneumocephalus and hemorrhage. ” • “No new hemorrhage identified…there was noted to be a slight decrease in the size of the anterior 3 rd ventricle in comparison to the prior CT scan 1 month earlier”. MRI showed a cerebellar infarct, appearing as a bright signal on the diffusion-weighted image

Vertigo Differential diagnosis in children

Vertigo • Definition: • A sensation of movement when there is none. Commonly a spinning sensation, but can be any type of movement • Need to differentiate between • “Dizziness” • Ataxia • Weakness • Confusion

Pediatric Dizziness & Vertigo • 1 st reported by Harrison in 1962 • Uncommon pediatric complaint • >560, 000 pediatric encounters over a 4 -year period showed prevalence of 0. 4% (dizziness), 0. 03% (peripheral vertigo), & 0. 02% (central vestibulopathy) • History & exam challenged by vocabulary, distractibility & compliance • Common impression that symptoms secondary to lack of coordination or behavioral • Remarkable compensation for vestibular deficits that in adults results in disequilibrium and / or ADL limitations

Essential History in the Dizzy Patient • True vertigo present? • PMH? • Onset pattern? • Medications? • Symptom duration? • Social? • Auditory symptoms? • Family? • Associated neurological symptoms? • Associated symptoms?
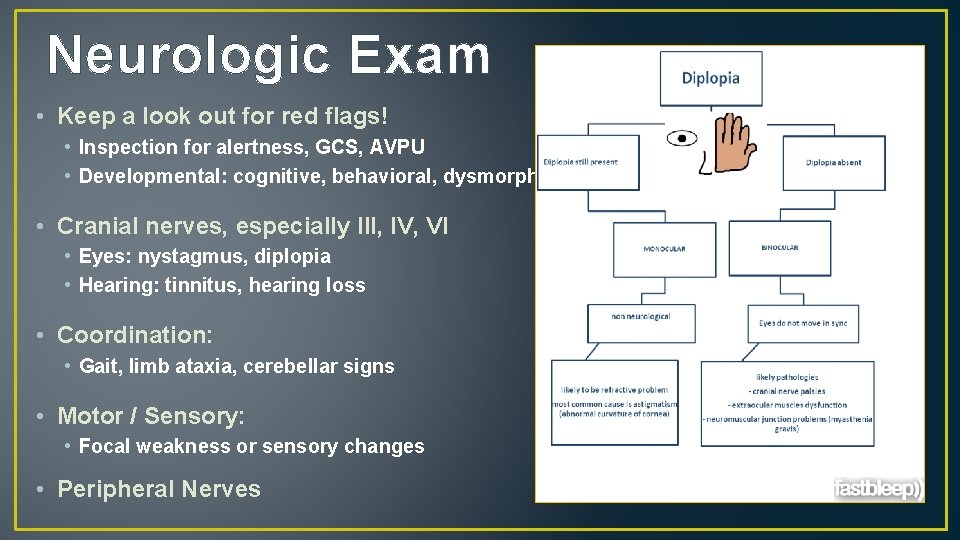
Neurologic Exam • Keep a look out for red flags! • Inspection for alertness, GCS, AVPU • Developmental: cognitive, behavioral, dysmorphia • Cranial nerves, especially III, IV, VI • Eyes: nystagmus, diplopia • Hearing: tinnitus, hearing loss • Coordination: • Gait, limb ataxia, cerebellar signs • Motor / Sensory: • Focal weakness or sensory changes • Peripheral Nerves
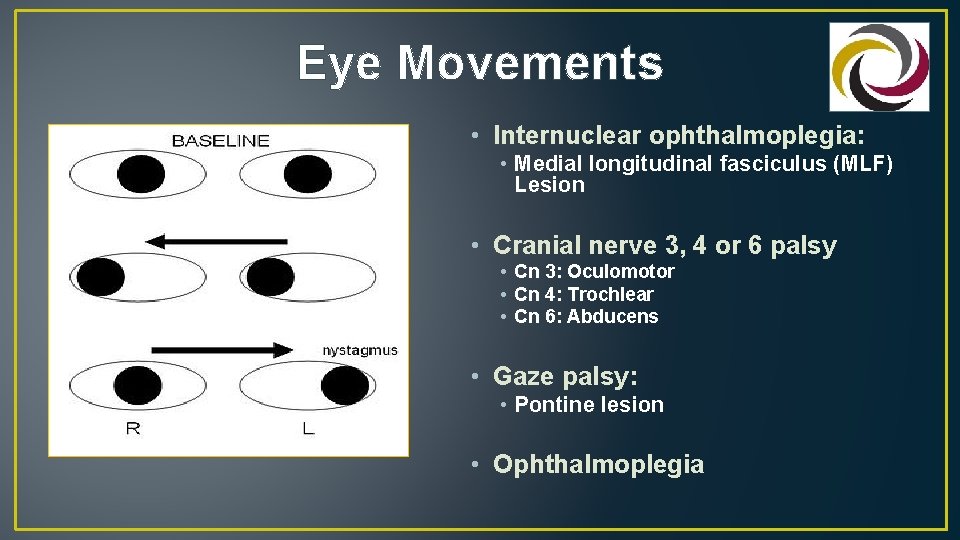
Eye Movements • Internuclear ophthalmoplegia: • Medial longitudinal fasciculus (MLF) Lesion • Cranial nerve 3, 4 or 6 palsy • Cn 3: Oculomotor • Cn 4: Trochlear • Cn 6: Abducens • Gaze palsy: • Pontine lesion • Ophthalmoplegia

Nystagmus • Fast uncontrollable eye movements • Vertical vs horizontal/rotatory nystagmus • Congenital nystagmus • Acquired • Brainstem lesion • Peripheral lesion • Other (i. e. medication)

Vertigo Differential Diagnosis • Migraine • Seizures • Aura • Infection • Peripheral: otitis media, labyrinthitis • Central: meningitis, encephalitis • Head trauma • Structural lesions • AVMs, Tumors, Arnold-Chiari • Drug overdose • i. e. NSAIDs, anticonvulsants • Benign paroxysmal vertigo of childhood - Recurrent vertigo, normal in between episodes, self limited after years • Benign paroxysmal positional vertigo • Rare in children • Stroke: • Hypercoagulable state, i. e. Sickle cell disease, genetic/inherited conditions, elevated homocysteine • Trauma (i. e. dissection) • Congenital heart disease
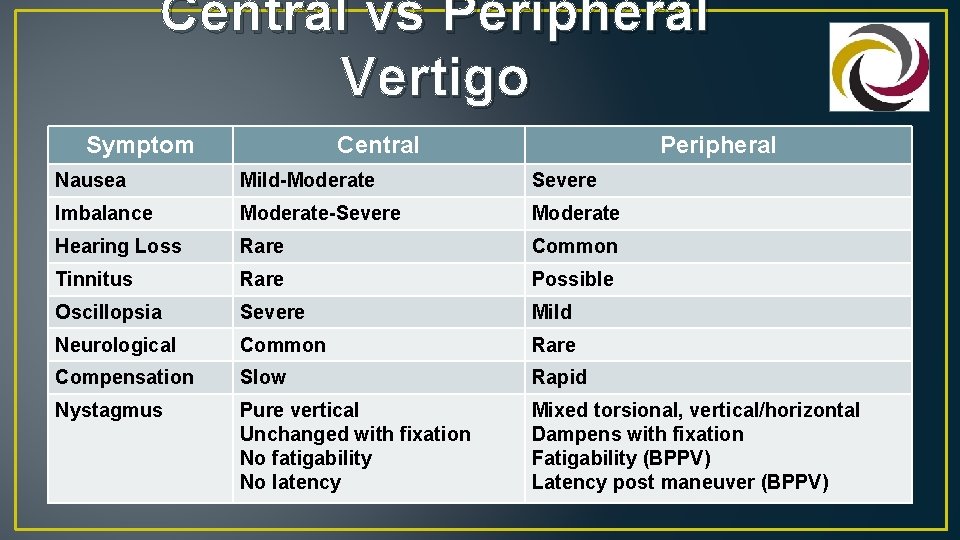
Central vs Peripheral Vertigo Symptom Central Peripheral Nausea Mild-Moderate Severe Imbalance Moderate-Severe Moderate Hearing Loss Rare Common Tinnitus Rare Possible Oscillopsia Severe Mild Neurological Common Rare Compensation Slow Rapid Nystagmus Pure vertical Unchanged with fixation No fatigability No latency Mixed torsional, vertical/horizontal Dampens with fixation Fatigability (BPPV) Latency post maneuver (BPPV)

Pediatric Vertigo Etiologies • Diversity of etiologies present with complaint of “vertigo” or “dizziness” • Detailed history & otoneurological exam essential • Most common etiology is migraine • Accompanies vertigo, but dominates clinical picture • Migraine in 35% of vertigo pediatric pts vs 6% adults • Though 10% children meet International Headache Society criteria for migraine, vestibular symptoms occur in about 25%
Migraine • Family history • Car sickness • Imaging normal • Can occur even in 1 -2 year olds, but difficult to diagnose until older • Symptoms • Throbbing head pain • Nausea, vomiting • Photophobia • Sonophobia • Visual aura • Focal symptoms • Vertigo
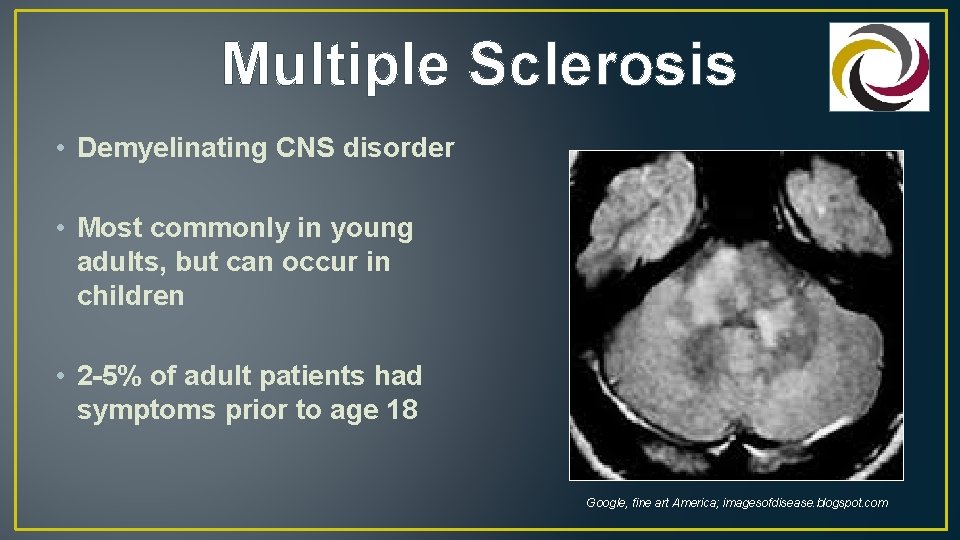
Multiple Sclerosis • Demyelinating CNS disorder • Most commonly in young adults, but can occur in children • 2 -5% of adult patients had symptoms prior to age 18 Google, fine art America; imagesofdisease. blogspot. com
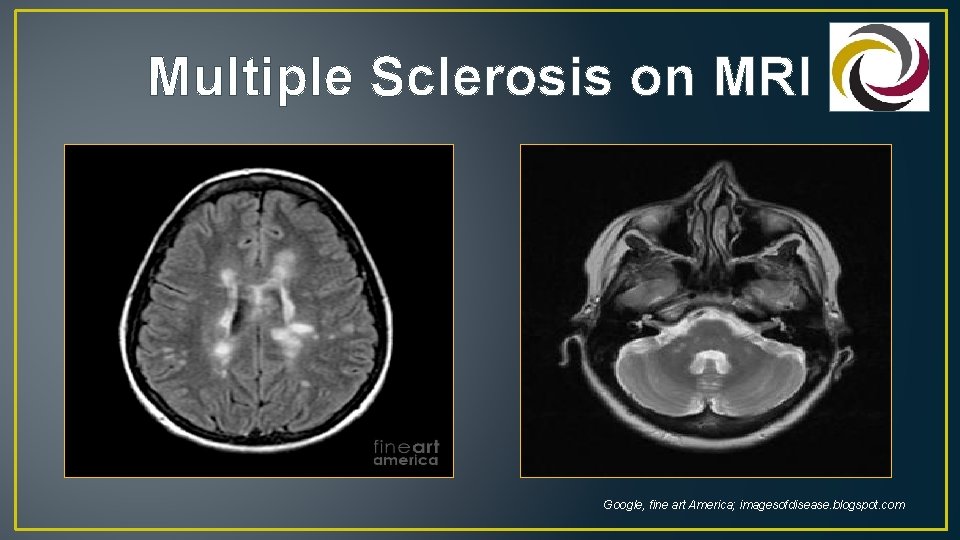
Multiple Sclerosis on MRI Google, fine art America; imagesofdisease. blogspot. com
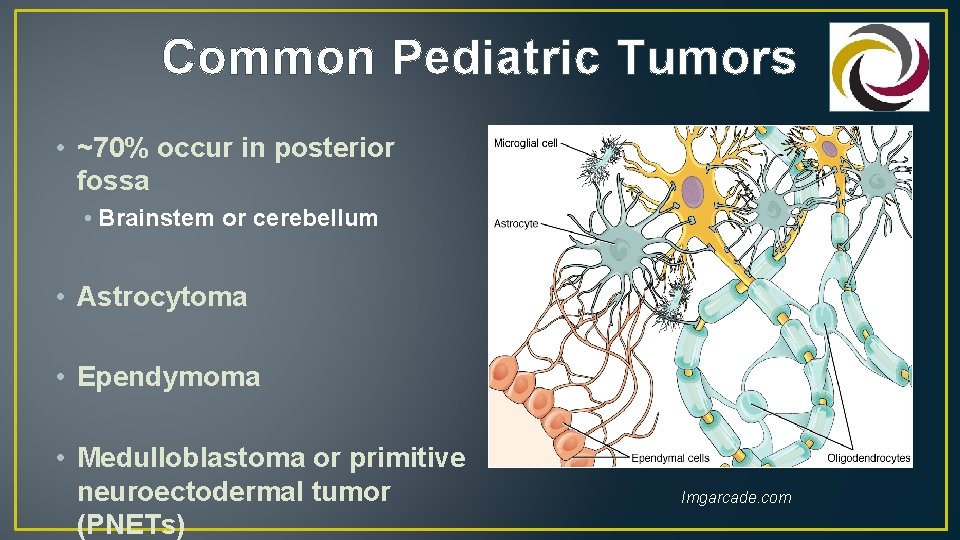
Common Pediatric Tumors • ~70% occur in posterior fossa • Brainstem or cerebellum • Astrocytoma • Ependymoma • Medulloblastoma or primitive neuroectodermal tumor (PNETs) Imgarcade. com
Cell Types • Three types of normal glial cells can produce tumors • Astrocytes produce astrocytomas (including glioblastomas) • Oligodendrocytes produce oligodendrogliomas • Ependymal cells produce ependymomas • Tumors that display a mixture of different cells are “mixed gliomas” Normal astrocytes comminfo. rutgers. edu

Pilocytic Astrocytoma (Juvenile Pilocytic Astrocytoma) • Most common Grade 1 astrocytomas • Typically do not spread • Considered “most benign” (noncancerous) of all the astrocytomas • Other Grade 1 astrocytomas: • Cerebellar astrocytoma • Desmoplastic infantile astrocytoma • Based on pathology Pathologyoutlines. com

Pilocytic Astrocytoma on MRI • Commonly see solid & cystic components Neuropathology-web. org

Diffuse Astrocytoma • Also called Low-Grade or Astrocytoma Grade II • Types: • Fibrillary • Gemistocytic • Protoplasmic • Tend to invade surrounding tissue and grow at a relatively slow rate • More common in the cerebral hemispheres
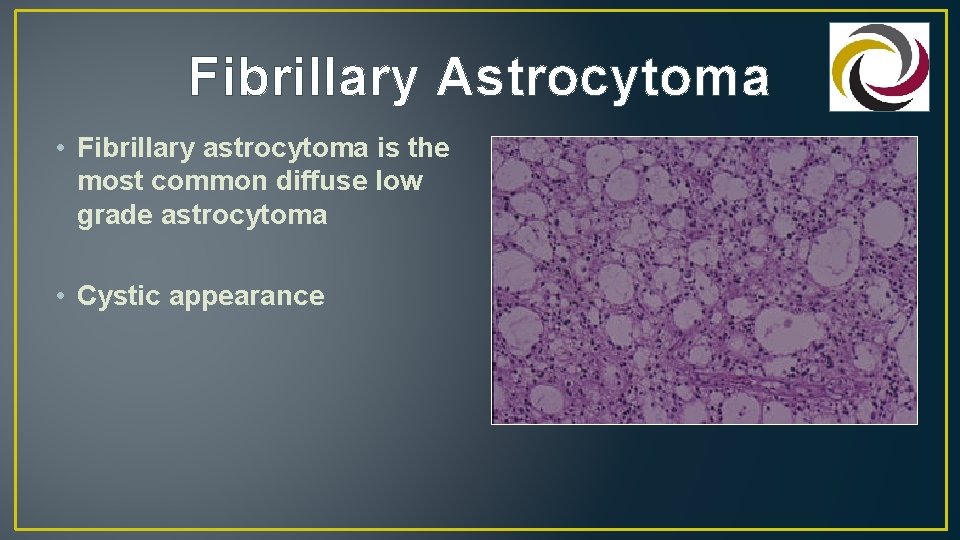
Fibrillary Astrocytoma • Fibrillary astrocytoma is the most common diffuse low grade astrocytoma • Cystic appearance
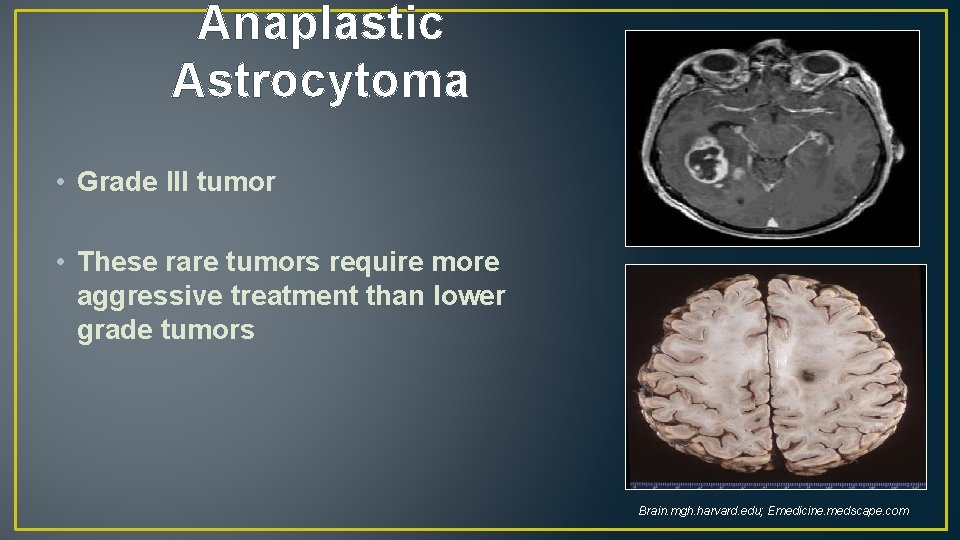
Anaplastic Astrocytoma • Grade III tumor • These rare tumors require more aggressive treatment than lower grade tumors Brain. mgh. harvard. edu; Emedicine. medscape. com

Grade IV Astrocytoma ~ Glioblastoma �Previously called “Glioblastoma Multiforme, ” “Grade IV Glioblastoma, ” and “GBM” • Two types of astrocytoma Grade IV • Primary, or de novo • Most common form, very aggressive • Secondary • Originate as a lower-grade tumor & evolve into a grade IV tumor Radiologyteacher. com
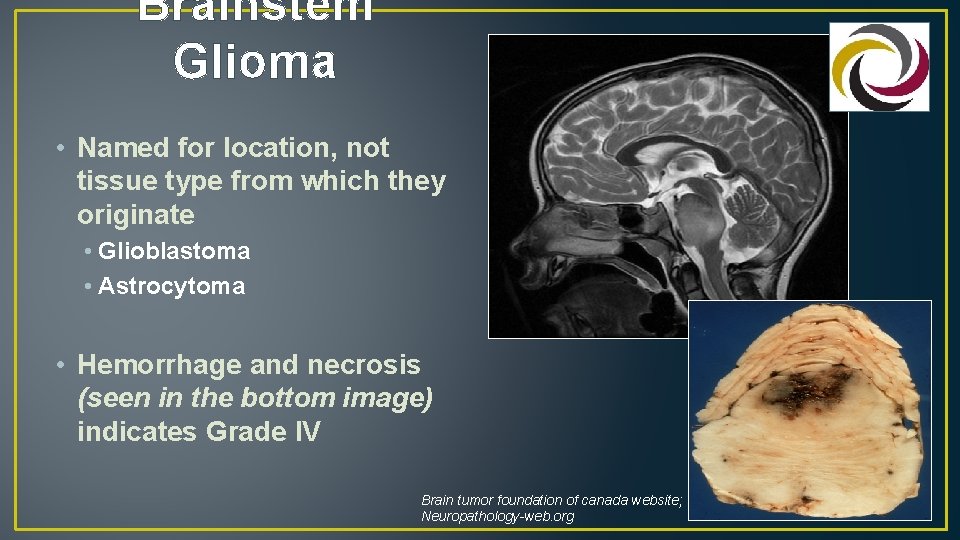
Brainstem Glioma • Named for location, not tissue type from which they originate • Glioblastoma • Astrocytoma • Hemorrhage and necrosis (seen in the bottom image) indicates Grade IV Brain tumor foundation of canada website; Neuropathology-web. org
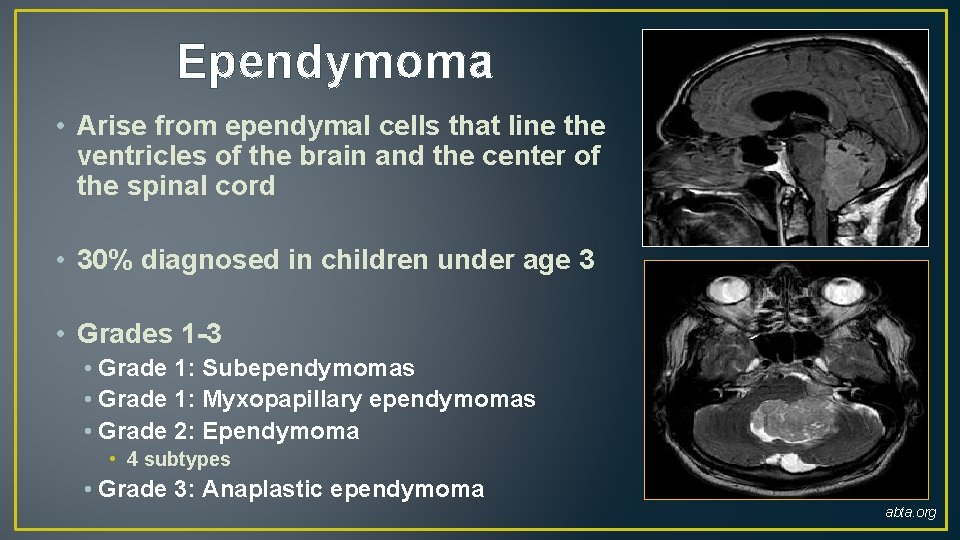
Ependymoma • Arise from ependymal cells that line the ventricles of the brain and the center of the spinal cord • 30% diagnosed in children under age 3 • Grades 1 -3 • Grade 1: Subependymomas • Grade 1: Myxopapillary ependymomas • Grade 2: Ependymoma • 4 subtypes • Grade 3: Anaplastic ependymoma abta. org

Medulloblastoma / Primitive Neuroectodermal Tumors (PNET) • Always located in the cerebellum • Unusual to spread outside brain & spinal cord • However, as CSF “seeding” common, need to image entire neuroaxis to identify drop metastasis and leptomeningeal spread • >70% of all pediatric medulloblastomas are diagnosed in children under age 10
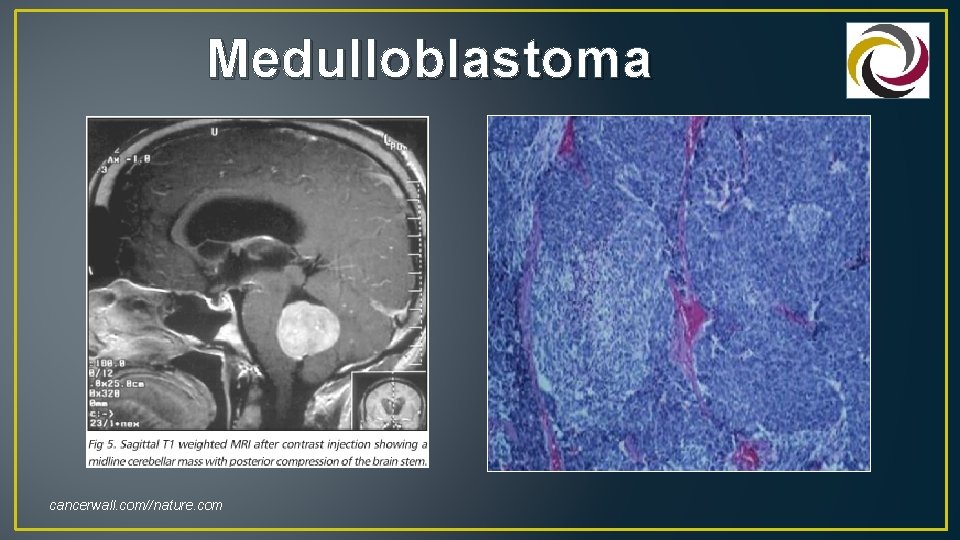
Medulloblastoma cancerwall. com//nature. com
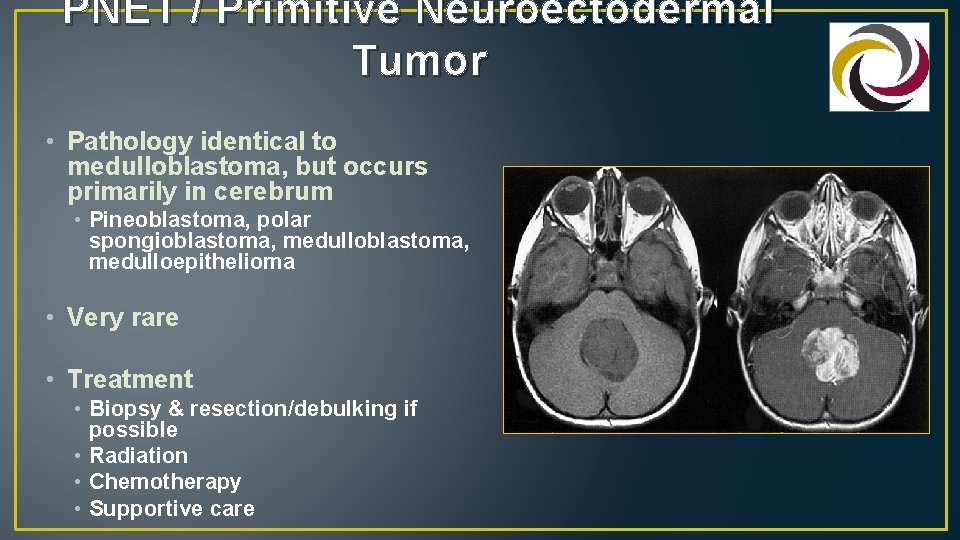
PNET / Primitive Neuroectodermal Tumor • Pathology identical to medulloblastoma, but occurs primarily in cerebrum • Pineoblastoma, polar spongioblastoma, medulloblastoma, medulloepithelioma • Very rare • Treatment • Biopsy & resection/debulking if possible • Radiation • Chemotherapy • Supportive care
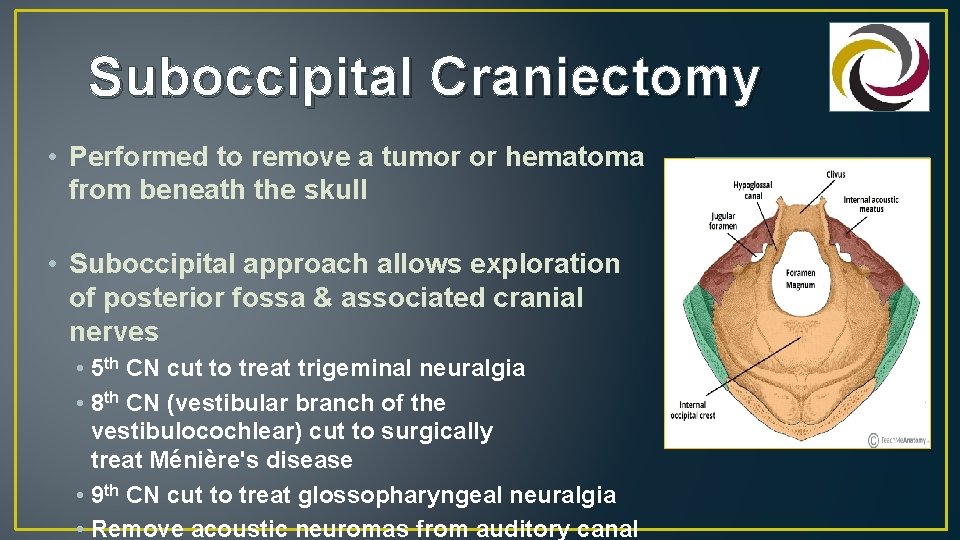
Suboccipital Craniectomy • Performed to remove a tumor or hematoma from beneath the skull • Suboccipital approach allows exploration of posterior fossa & associated cranial nerves • 5 th CN cut to treat trigeminal neuralgia • 8 th CN (vestibular branch of the vestibulocochlear) cut to surgically treat Ménière's disease • 9 th CN cut to treat glossopharyngeal neuralgia • Remove acoustic neuromas from auditory canal
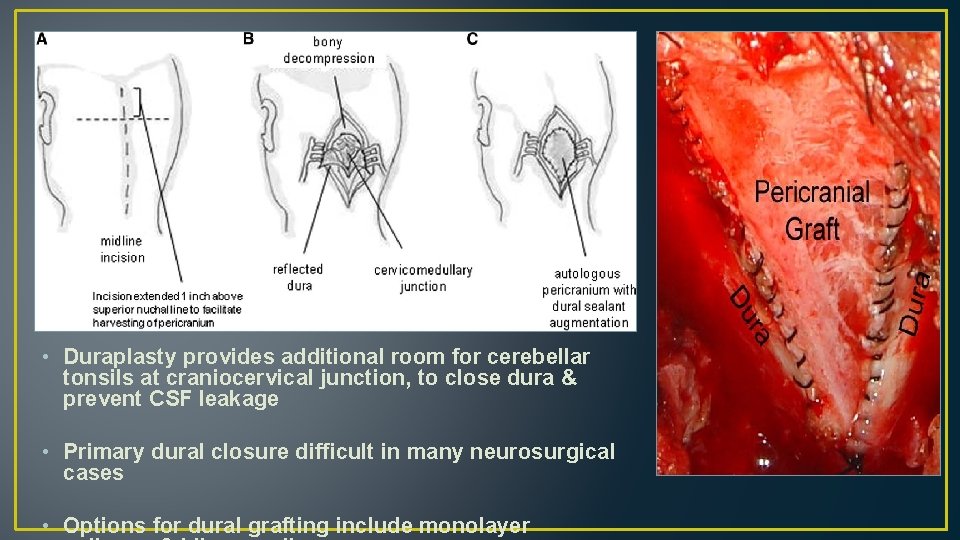
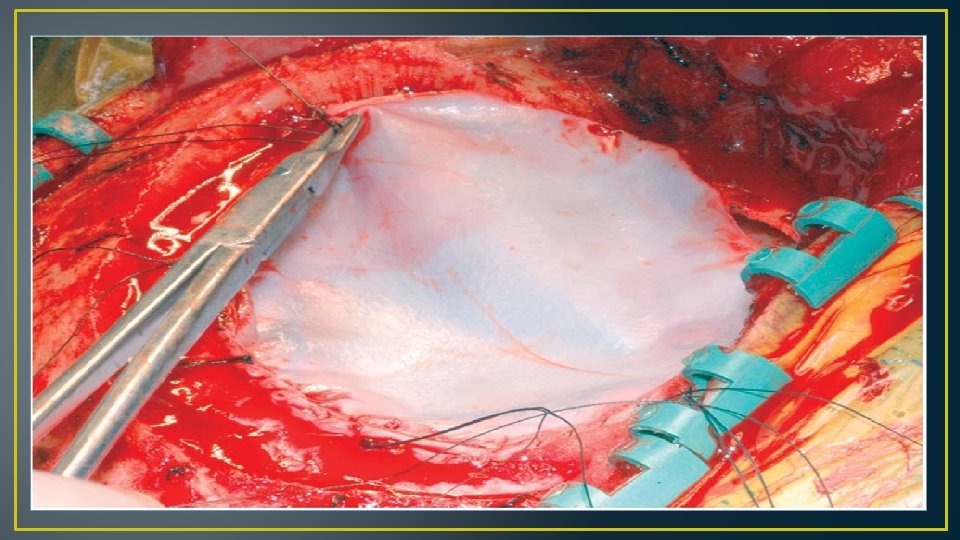
• Duraplasty provides additional room for cerebellar tonsils at craniocervical junction, to close dura & prevent CSF leakage • Primary dural closure difficult in many neurosurgical cases • Options for dural grafting include monolayer
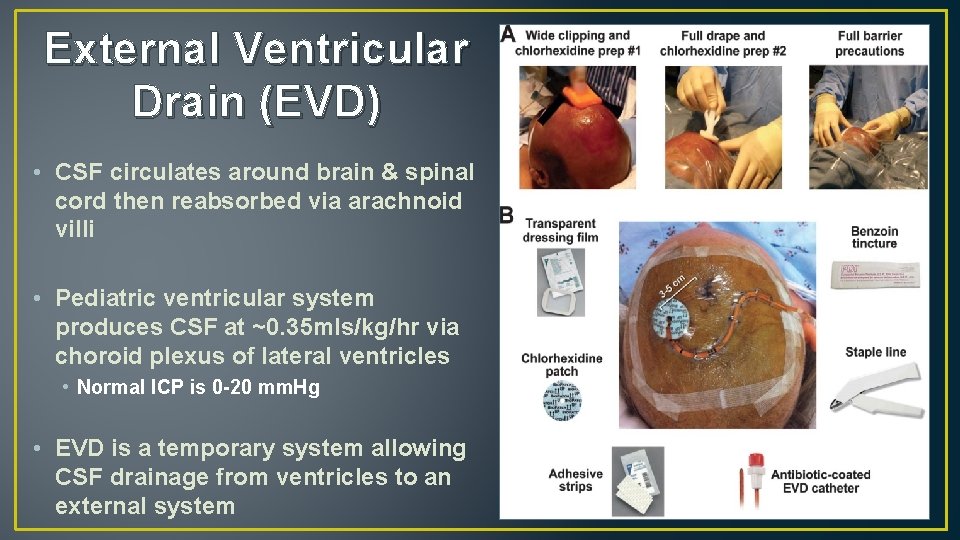
External Ventricular Drain (EVD) • CSF circulates around brain & spinal cord then reabsorbed via arachnoid villi • Pediatric ventricular system produces CSF at ~0. 35 mls/kg/hr via choroid plexus of lateral ventricles • Normal ICP is 0 -20 mm. Hg • EVD is a temporary system allowing CSF drainage from ventricles to an external system
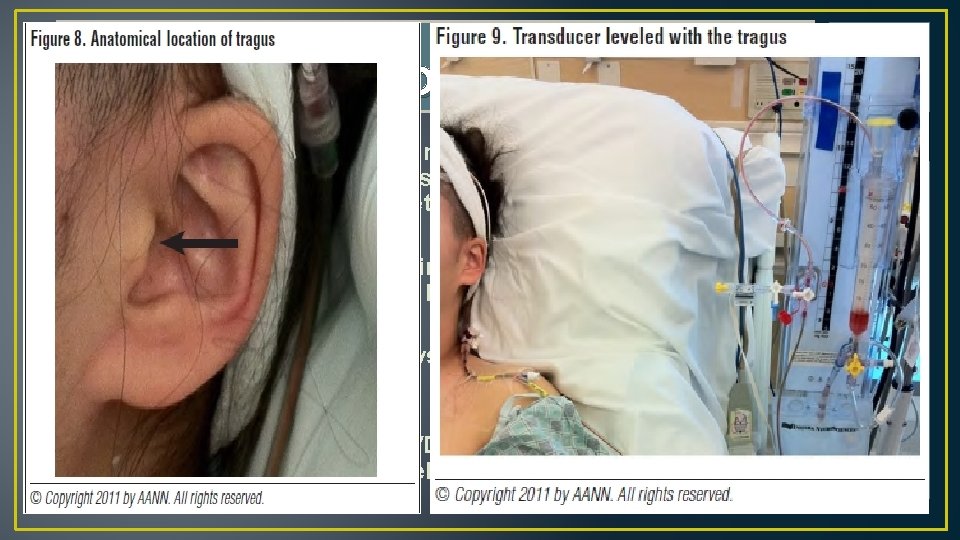
EVD Monitoring • EVD pressure transducer maintained at the same horizontal level as the ventricles for reliable interpretation • Laser level device should be in line with the patient's Foramen of Monro • If patient supine, level EVD system to the ear tragus • If the patient upright, level EVD to the mid sagittal line (between eyebrows)
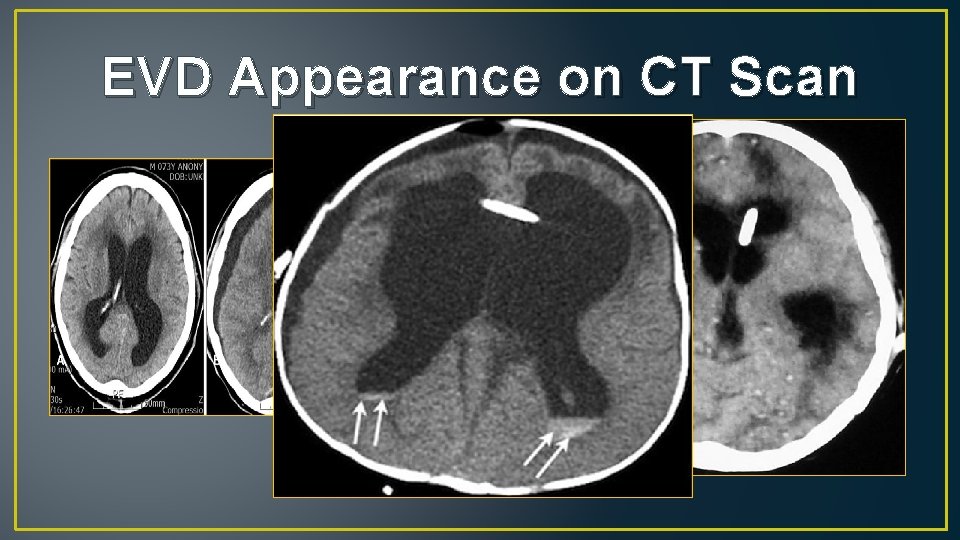
EVD Appearance on CT Scan

References • • • • • • Cohen-Kerem MR et al. Vertigo in Children and Adolescents: Characteristics and Outcome. Scientific. World. Journal. 2012; 2012: 109624. e. Pub 2012 Jan 3. Tintinelli. Emergency Medicine – A comprehensive Study Guide. “Pediatric Neurological Emergencies”. 2010. Up. To. Date. com. “Vertigo”, “Pediatric Dizziness”, “Pediatric Stroke” Yang WC, Chen CY, Wu KH, Wu HP. Acute onset of dizziness caused by a cavernous malformation lateral to the fourth ventricle: a case report. Pediatr Neonatol 2011 Apr; 52(2): 113 -6. Reed Group MDGuidelines. “Suboccipital Craniectomy”. 2013. Litvack ZN, West GA, Delashaw JB, Burchiel KJ, Anderson VC. Dural augmentation: part I-evaluation of collagen matrix allografts for dural defect after craniotomy. Neurosurgery. 2009 Nov; 65(5): 890 -7; discussion 897. Albanese, J; Leone M; Alliez JR; Kaya JM; Antonini F; Alliez B; Martin C (2003). "Decompressive craniectomy for severe traumatic brain injury: Evaluation of the effects at one year". Critical Care Medicine 31 (10): 2535– 2538. Hejazi, N; Witzmann A; Fae P. "Unilateral decompressive craniectomy for children with severe brain injury. Report of seven cases and review of the relevant literature". European Journal of Pediatrics 161 (2): 99– 104. Agannathan, J; Okonkwo DO; Dumont, AS. "Outcome following decompressive craniectomy in children with severe traumatic brain injury: a 10 -year single-center experience with long-term follow up". Journal of Neurosurgery Pediatrics. April 2007. 106 (4): 268– 275. Adelson. P. , et al. Intracranial pressure monitoring. Paediatric Critical Care. 4(3) (suppl. ): S 28 -S 30. 2003. Tippett N. Intracranial pressure (ICP) monitoring and extraventricular drains (EVD). Bayside Health, Alfred ICU: 1 -19. 2006. Photo Search: wikipedia, google, bing Muralidharan R. External ventricular drains: Management and complications. Surg Neurol Int. 2015 May 25; 6(Suppl 6): S 271 -4. Lau T, Reintjes S, Olivera R, van Loveren HR, Agazzi S. C-shaped Incision for Far-Lateral Suboccipital Approach: Anatomical Study and Clinical Correlation. J Neurol Surg B Skull Base. 2015 Mar; 76(2): 117 -21. Klimo P Jr, Nesvick CL, Broniscer A, Orr BA, Choudhri AF. Malignant brainstem tumors in children, excluding diffuse intrinsic pontine gliomas. J Neurosurg Pediatr. 2015 Oct 16: 1 -9. Hopkinsmedicine. org Medscape. com Klimo P Jr, Nesvick CL, Broniscer A, Orr BA, Choudhri AF. Malignant brainstem tumors in children, excluding diffuse intrinsic pontine gliomas. . J Neurosurg Pediatr. 2015 Oct 16: 1 -9. PDQ Pediatric Treatment Editorial Board. Childhood Central Nervous System Germ Cell Tumors Treatment (PDQ®): Health Professional Version. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute (US); 2002 -2015 Sep 24. Aghayan Golkashani H, Hatami H, Farzan A, Mohammadi HR, Nilipour Y, Khoddami M, Jadali F. Tumors of the Central Nervous System: An 18 -Year Retrospective Review in a Tertiary Pediatric. Referral Center. Iran J Child Neurol. 2015 Summer; 9(3): 24 -33. Assina R, Meleis AM, Cohen MA, Iqbal MO, Liu JK. Titanium mesh-assisted dural tenting for an expansile suboccipital cranioplasty in the treatment of Chiari 1 malformation. J Clin Neurosci. 2014 Sep; 21(9): 1641 -6. Robertson SC, Lennarson P, Hasan DM, Traynelis VC. Clinical course and surgical management of massive cerebral infarction. Neurosurgery. 2004 Jul; 55(1): 5561; discussion 61 -2.

Patient Follow-Up • EVD removed 2 weeks after initial surgery • As of 3 months after the initial presentation, patient with improved speech, motor function and ambulation • No evidence of metastatic spread • Weaned off TPN, tolerating po • Unclear if any long-term cognitive insults, but is able to ambulate & has regained strength on his left side

Summary • Pediatric brain tumor is a rare cause of dizziness, but needs to be considered if the history & exam suggestive of a significant or focal neurological deficit • A through history & physical exam is often a better diagnostic “tool” than any radiologic testing • Thank you for your attention today ~ any questions?
- Slides: 50