Kingdom of Bahrain Arabian Gulf University College of

Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences GI System – Review Problem (3) – Esophagus Ali Jassim Alhashli, BSc www. alhashli. com

Anatomy • • • It is a muscular tube of 25 cm length which begins at the level of lower border of C 6. It is divided into 3 parts: – Superior third: striated muscle only. – Middle third: striated + smooth muscles. – Inferior third: smooth muscle only. There are 3 main areas of narrowing (which can be detected by barium swallow): – At the level of cricopharyngeus muscle. – Where the left mainstem bronchus and aortic arch cross. – At the hiatus of diaphragm (at the level of T 10). Remember the vertebral levels at which the following traverse the diaphragm: v T 8 = Inferior Vena Cava (IVC). v T 10 = esophagus. v T 12 = aorta. There are 2 sphincters of the esophagus: – Upper Esophageal Sphincter (UES = formed by cricopharyngeus muscle): it prevents the passage of excess air into the stomach during breathing. – Lower Esophageal Sphincter (LES = physiological sphincter): it prevents the reflux of gastric contents into the esophagus. Histology: Histology non-keratinized stratified squamous epithelium.
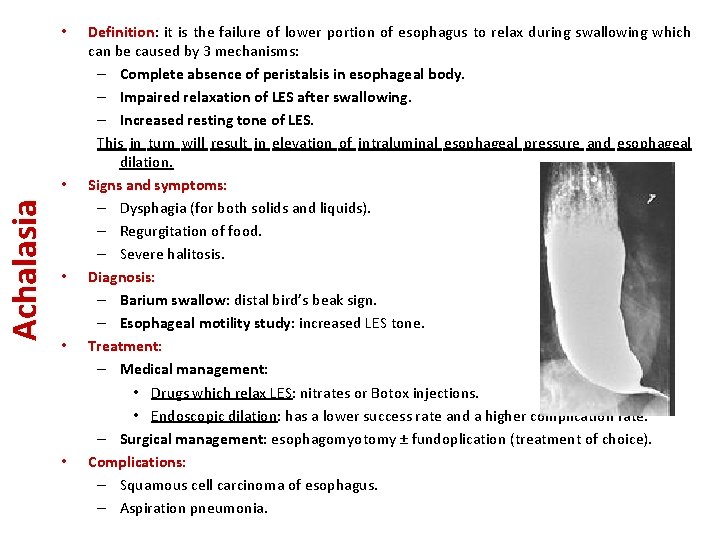
• Achalasia • • Definition: Definition it is the failure of lower portion of esophagus to relax during swallowing which can be caused by 3 mechanisms: – Complete absence of peristalsis in esophageal body. – Impaired relaxation of LES after swallowing. – Increased resting tone of LES. This in turn will result in elevation of intraluminal esophageal pressure and esophageal dilation. Signs and symptoms: – Dysphagia (for both solids and liquids). – Regurgitation of food. – Severe halitosis. Diagnosis: – Barium swallow: distal bird’s beak sign. – Esophageal motility study: increased LES tone. Treatment: – Medical management: • Drugs which relax LES: nitrates or Botox injections. • Endoscopic dilation: has a lower success rate and a higher complication rate. – Surgical management: esophagomyotomy ± fundoplication (treatment of choice). Complications: – Squamous cell carcinoma of esophagus. – Aspiration pneumonia.

Tracheo-esophageal Fistula • Tracheoesophageal (TE) fistula: – Definition: incomplete separation of esophagus and trachea. – Signs and symptoms: • Respiratory distress and chocking following the first feed. • Postprandial regurgitation. • Excess drooling and salivation. – There are 5 types of TE fistula: • Type-A: pure esophageal atresia. • Type-B: esophageal atresia with proximal TE fistula. • Type-C (most common): esophageal atresia with distal TE fistula. • Type-D: esophageal atresia with proximal and distal TE fistula. • Type-E: no esophageal atresia with TE fistula. – Diagnosis: • Inability to pass feeding tube. • CXR: tube coiled in upper esophagus. • AXR: presence of air in the stomach. If air is not present, this might indicate the presence of esophageal atresia without TE fistula. – Notice that TE fistula is associated with: • Polyhydramnios. • Pre-term birth. • Small for gestational age. – Treatment: • Decompression of the blind esophageal pouch with constant suction. • Prophylactic antibiotics (to prevent complications of aspiration). • Search for other anomalies (especially cardiac and renal). • Surgical repair: – Ligation of fistula and insertion of gastrostomy tube. – Anastomosis of the two ends of esophagus (jejunal or colonic grafts are used).
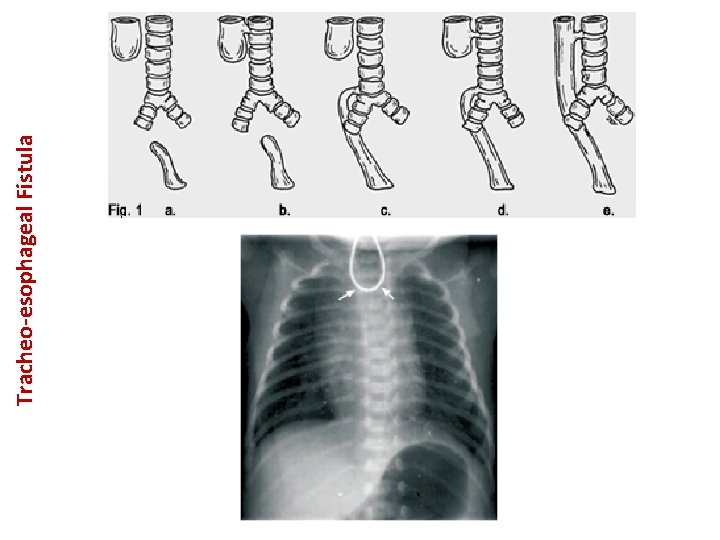
Tracheo-esophageal Fistula

Plummer-Vinson Syndrome and Esophagitis • • Plummer-Vinson Syndrome (PVS): – Epidemiology: middle-aged females. – Clinical presentation: • Iron-deficiency anemia. • Glossitis. • Esophageal web: which is a thin extension from esophageal mucosa made from squamous cells and occurs mostly in hypopharnyx producing dysphagia mostly to solids. – Diagnosis: barrium swallow. – Treatment: • Treat iron-deficiency anemia with ferrous sulfate. • Treat esophageal web with dilation procedures. Esophagitis: – Definition: infection/inflammation of the esophagus. – Etiology: • Candidal albicans in patients with: – HIV and CD 4 count < 200 cells/mm 3. – Diabetics. • Ingestions of medications or caustic substances. – Clinical manifestations: progressive odynophagia especially when swallowing food (why? ) → due to mechanical rub of food against the inflamed esophagus. – Diagnosis: • In HIV patients, assume it is Candida and start treatment with systemic anti-fungal (fluconazole). Regression of symptoms confirm your diagnosis. • Otherwise, do upper GI endoscopy with biopsy to determine the cause. • If esophagitis is caused by a medication or caustic substance → this will be determined from history.
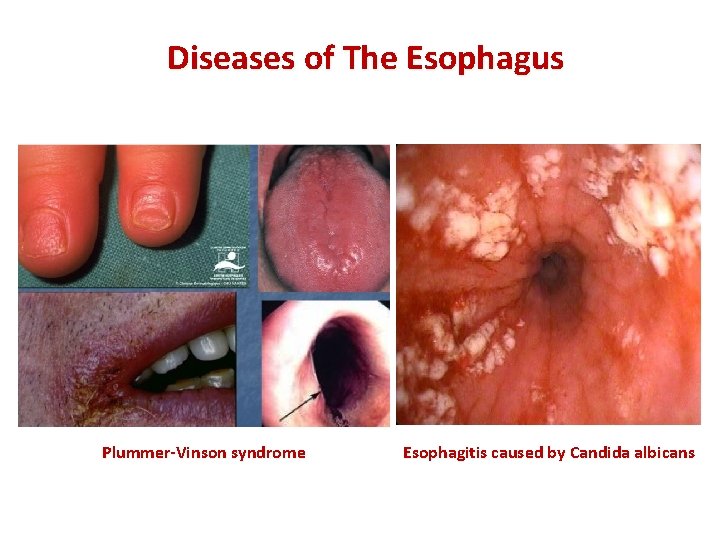
Diseases of The Esophagus Plummer-Vinson syndrome Esophagitis caused by Candida albicans

Zenker Diverticulum and Mallory-Weiss Syndrome • • Zenker diverticulum: – Definition: it is outpouching of posterior pharyngeal constrictor muscles at the back of the pharynx (simply: outpouching of posterior pharynx). – Clinical manifestations: • Dysphagia: inability to initiate swallowing because it is a proximal problem. • Halitosis (bad breath). • Patient waking up at night with undigested, regurgitated food on his pillow which has been eaten several day ago – Diagnosis: barrium swallow. Notice that endoscopy is contraindicated due to the high risk of perforation. – Treatment: surgical resection. Mallory-Weiss syndrome: – Etiology: non-transmural (not involving the whole wall) tears in lower esophagus due to repeated retching and vomiting (especially in alcoholics). – Clinical manifestations: • PAINLESS upper GI bleeding. • Melena (black stool) when amount of blood is > 100 ml. • Hematemesis: if there is continuous vomiting. – Diagnosis: upper GI endoscopy. – Treatment: • Most cases resolve spontaneously. • If there is severe bleeding: inject the area with epinephrine or perform cauterization.

Zenker Diverticulum and Mallory-Weiss Syndrome Mallory-Weiss syndrome

GERD and Barrett’s Esophagus • • Gastro-Esophageal Reflux Disease (GERD): – Definition: In GERD, there is a backflow of gastric content into the eophagus due to relaxation of LES. – Etiology: this can be idiopathic or precipitated by factors which are lowering LES pressure such as nicotine, alcohol, caffeine, chocolate, peppermint and anticholinergics. GERD occurs particularly when patient is lying down. – Clinical manifestations: epigastric pain/substernal chest pain, bad metal-like taste in the mouth, sore throat, coughing, wheezing and hoarsness. – Diagnosis: • Most accurate with 24 -hour p. H monitoring (usually not necessary when diagnosis is clear from clinical presentation of the patient). – Treatment: • If patient has MILD, INTERMITTENT symptoms → use H 2 -blockers (such as ranitidine). • Gold-standard therapy: PPIs (omeprazole). • In patients not responding to omeprazole → surgery to tighten LES (Nissen fundoplication). • Lifestyle modifications: avoid nicotine, alcohol, caffeine, spicy/fatty food and late night meal. Barrett’s esophagus: – Definition: it is a complication of long-standing GERD in which the normal squamous epithelium in distal esophagus will be changed to columnar epithelium and predisposing the patient to develop esophageal adenocarcinoma (0. 5% risk). – Diagnosis: • Patients with Barrett’s esophagus must undergoe endoscopy every 2 -3 years to exclude dysplasia or esophageal adenocarcinoma. • If there is low-grade dysplasia: you must repeat endoscopy in 3 -6 months to see if the dysplasia has progressed or resolved. • If there is high-grade dysplasia: patient must undergo surgical removal of the distal part of esophagus. – Treatment: PPIs (omeprazole).
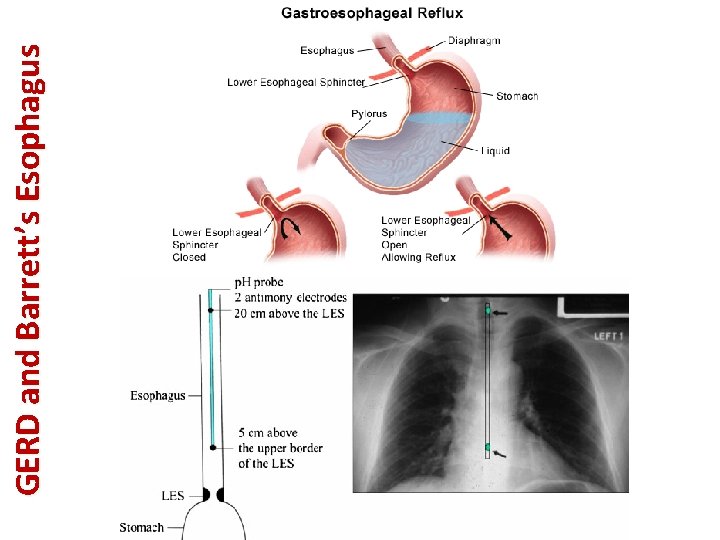
GERD and Barrett’s Esophagus
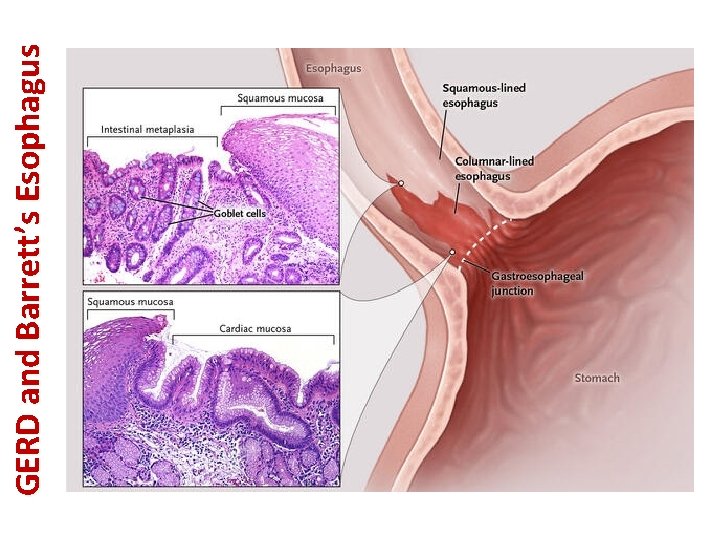
GERD and Barrett’s Esophagus
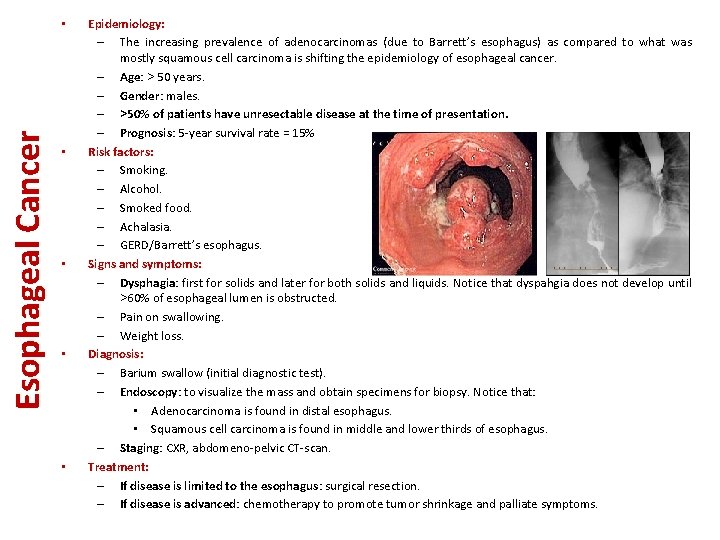
Esophageal Cancer • • • Epidemiology: – The increasing prevalence of adenocarcinomas (due to Barrett’s esophagus) as compared to what was mostly squamous cell carcinoma is shifting the epidemiology of esophageal cancer. – Age: > 50 years. – Gender: males. – >50% of patients have unresectable disease at the time of presentation. – Prognosis: 5 -year survival rate = 15% Risk factors: – Smoking. – Alcohol. – Smoked food. – Achalasia. – GERD/Barrett’s esophagus. Signs and symptoms: – Dysphagia: first for solids and later for both solids and liquids. Notice that dyspahgia does not develop until >60% of esophageal lumen is obstructed. – Pain on swallowing. – Weight loss. Diagnosis: – Barium swallow (initial diagnostic test). – Endoscopy: to visualize the mass and obtain specimens for biopsy. Notice that: • Adenocarcinoma is found in distal esophagus. • Squamous cell carcinoma is found in middle and lower thirds of esophagus. – Staging: CXR, abdomeno-pelvic CT-scan. Treatment: – If disease is limited to the esophagus: surgical resection. – If disease is advanced: chemotherapy to promote tumor shrinkage and palliate symptoms.
- Slides: 13

























