Kingdom of Bahrain Arabian Gulf University College of

Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Internal Medicine Notes Dermatology Prepared by: Ali Jassim Alhashli Based on: Kaplan Step 2 CK Internal Medicine
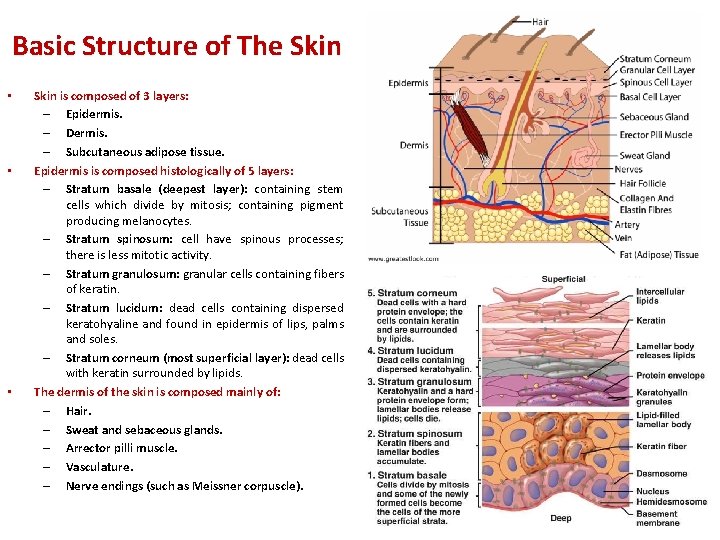
Basic Structure of The Skin • • • Skin is composed of 3 layers: – Epidermis. – Dermis. – Subcutaneous adipose tissue. Epidermis is composed histologically of 5 layers: – Stratum basale (deepest layer): containing stem cells which divide by mitosis; containing pigment producing melanocytes. – Stratum spinosum: cell have spinous processes; there is less mitotic activity. – Stratum granulosum: granular cells containing fibers of keratin. – Stratum lucidum: dead cells containing dispersed keratohyaline and found in epidermis of lips, palms and soles. – Stratum corneum (most superficial layer): dead cells with keratin surrounded by lipids. The dermis of the skin is composed mainly of: – Hair. – Sweat and sebaceous glands. – Arrector pilli muscle. – Vasculature. – Nerve endings (such as Meissner corpuscle).
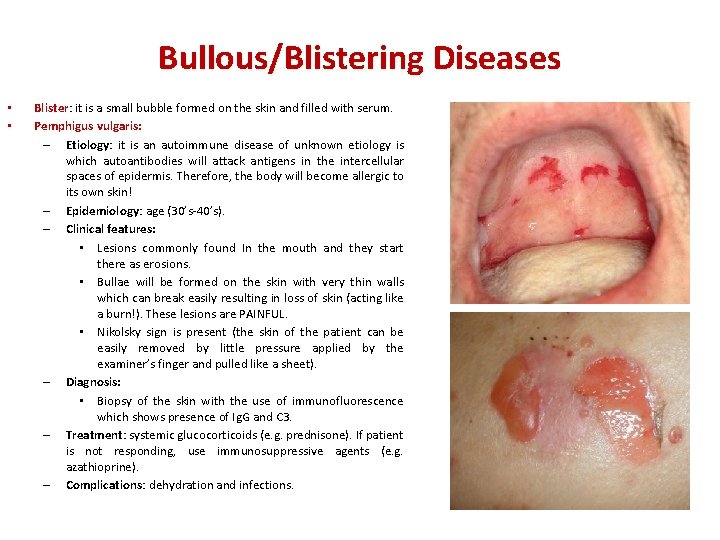
Bullous/Blistering Diseases • • Blister: Blister it is a small bubble formed on the skin and filled with serum. Pemphigus vulgaris: – Etiology: it is an autoimmune disease of unknown etiology is which autoantibodies will attack antigens in the intercellular spaces of epidermis. Therefore, the body will become allergic to its own skin! – Epidemiology: age (30’s-40’s). – Clinical features: • Lesions commonly found In the mouth and they start there as erosions. • Bullae will be formed on the skin with very thin walls which can break easily resulting in loss of skin (acting like a burn!). These lesions are PAINFUL. • Nikolsky sign is present (the skin of the patient can be easily removed by little pressure applied by the examiner’s finger and pulled like a sheet). – Diagnosis: • Biopsy of the skin with the use of immunofluorescence which shows presence of Ig. G and C 3. – Treatment: systemic glucocorticoids (e. g. prednisone). If patient is not responding, use immunosuppressive agents (e. g. azathioprine). – Complications: dehydration and infections.

Bullous/Blistering Diseases • Bullous pemphigoid: – Etiology: there antibodies directed against dermoepidermal junction causing separation of thick skin. This condition is more common than pemphigus vulgaris and is less serious. It can be induced by drugs such as: sulfa drugs, furosemide and penecillamine. – Epidemiology: age (70’s-80’s). – Clinical manifestations: • Oral lesions are rare. • Bullae are characterized by thick walls and they are much less likely to break (↓risk of dehydration and infections). – Diagnosis: • Skin biopsy with immunofluorescence showing antibodies to dermo-epidermal junction – Treatment: systemic steroids. TOPICAL steroids can be used when NO oral lesions are present.
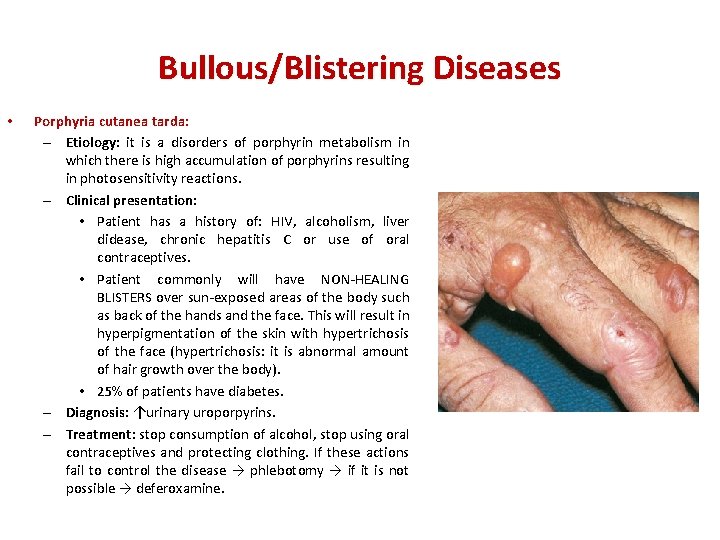
Bullous/Blistering Diseases • Porphyria cutanea tarda: – Etiology: it is a disorders of porphyrin metabolism in which there is high accumulation of porphyrins resulting in photosensitivity reactions. – Clinical presentation: • Patient has a history of: HIV, alcoholism, liver didease, chronic hepatitis C or use of oral contraceptives. • Patient commonly will have NON-HEALING BLISTERS over sun-exposed areas of the body such as back of the hands and the face. This will result in hyperpigmentation of the skin with hypertrichosis of the face (hypertrichosis: it is abnormal amount of hair growth over the body). • 25% of patients have diabetes. – Diagnosis: ↑urinary uroporpyrins. – Treatment: stop consumption of alcohol, stop using oral contraceptives and protecting clothing. If these actions fail to control the disease → phlebotomy → if it is not possible → deferoxamine.
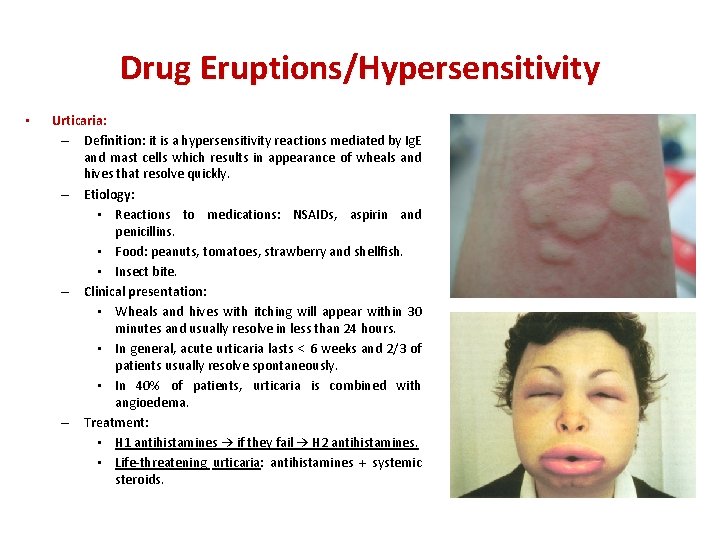
Drug Eruptions/Hypersensitivity • Urticaria: – Definition: it is a hypersensitivity reactions mediated by Ig. E and mast cells which results in appearance of wheals and hives that resolve quickly. – Etiology: • Reactions to medications: NSAIDs, aspirin and penicillins. • Food: peanuts, tomatoes, strawberry and shellfish. • Insect bite. – Clinical presentation: • Wheals and hives with itching will appear within 30 minutes and usually resolve in less than 24 hours. • In general, acute urticaria lasts < 6 weeks and 2/3 of patients usually resolve spontaneously. • In 40% of patients, urticaria is combined with angioedema. – Treatment: • H 1 antihistamines → if they fail → H 2 antihistamines. • Life-threatening urticaria: antihistamines + systemic steroids.
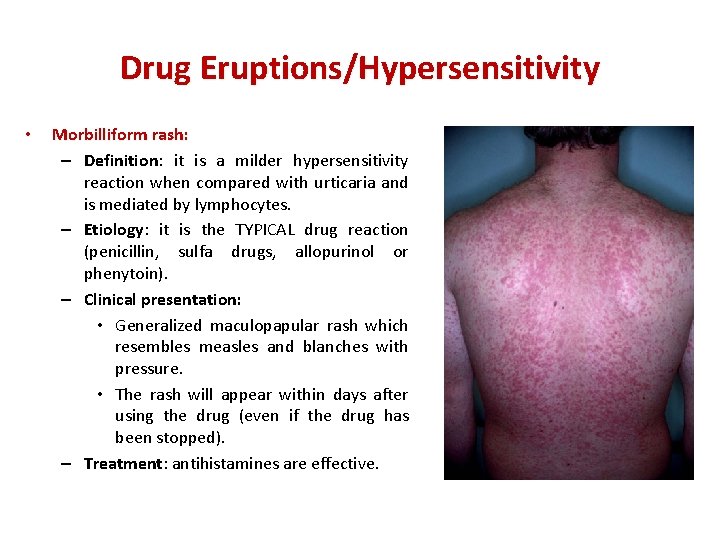
Drug Eruptions/Hypersensitivity • Morbilliform rash: – Definition: it is a milder hypersensitivity reaction when compared with urticaria and is mediated by lymphocytes. – Etiology: it is the TYPICAL drug reaction (penicillin, sulfa drugs, allopurinol or phenytoin). – Clinical presentation: • Generalized maculopapular rash which resembles measles and blanches with pressure. • The rash will appear within days after using the drug (even if the drug has been stopped). – Treatment: antihistamines are effective.

Drug Eruptions/Hypersensitivity • Erythema multiform: – Definition: it is a hypersensitivity reaction. – Etiology: • It occurs typically to infections (herpes simplex virus or Mycoplasma) • It can also occur in response to drugs (Penicillins, sulfa drugs and phenytoin). – Clinical manifestations: • Patients will have target-like lesion commonly on the palms and soles (the lesions have a central blister surrounded by an edematous ring). – Treatment: antihistamines + treating the underlying infection.
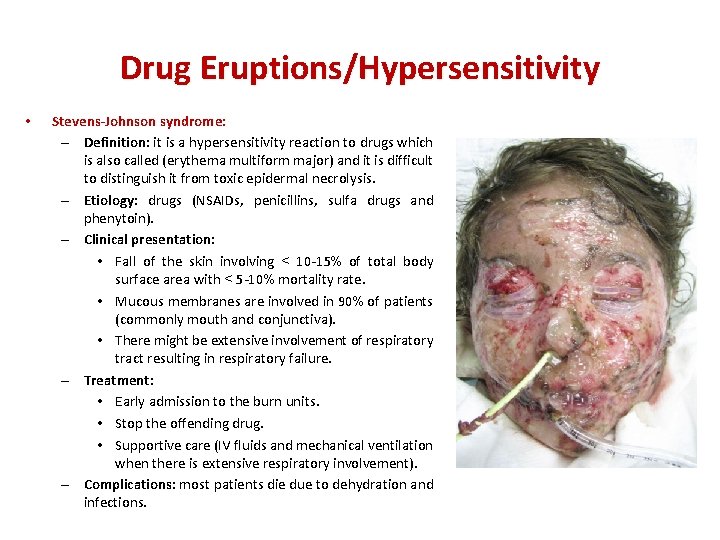
Drug Eruptions/Hypersensitivity • Stevens-Johnson syndrome: – Definition: it is a hypersensitivity reaction to drugs which is also called (erythema multiform major) and it is difficult to distinguish it from toxic epidermal necrolysis. – Etiology: drugs (NSAIDs, penicillins, sulfa drugs and phenytoin). – Clinical presentation: • Fall of the skin involving < 10 -15% of total body surface area with < 5 -10% mortality rate. • Mucous membranes are involved in 90% of patients (commonly mouth and conjunctiva). • There might be extensive involvement of respiratory tract resulting in respiratory failure. – Treatment: • Early admission to the burn units. • Stop the offending drug. • Supportive care (IV fluids and mechanical ventilation when there is extensive respiratory involvement). – Complications: most patients die due to dehydration and infections.
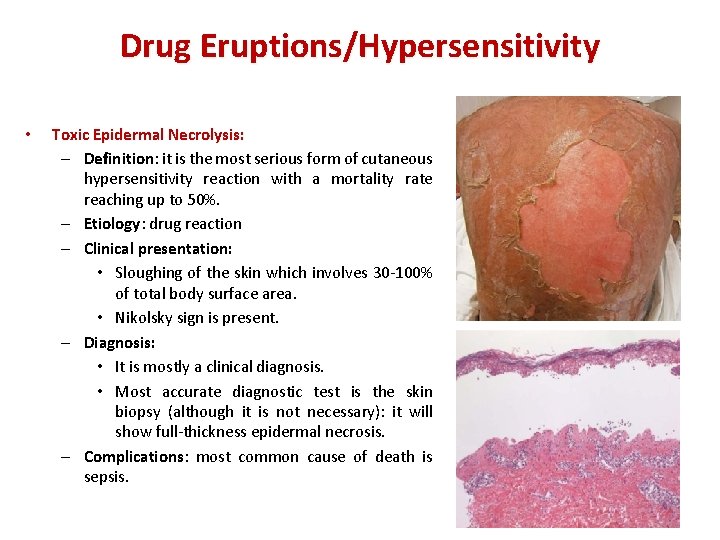
Drug Eruptions/Hypersensitivity • Toxic Epidermal Necrolysis: – Definition: it is the most serious form of cutaneous hypersensitivity reaction with a mortality rate reaching up to 50%. – Etiology: drug reaction – Clinical presentation: • Sloughing of the skin which involves 30 -100% of total body surface area. • Nikolsky sign is present. – Diagnosis: • It is mostly a clinical diagnosis. • Most accurate diagnostic test is the skin biopsy (although it is not necessary): it will show full-thickness epidermal necrosis. – Complications: most common cause of death is sepsis.
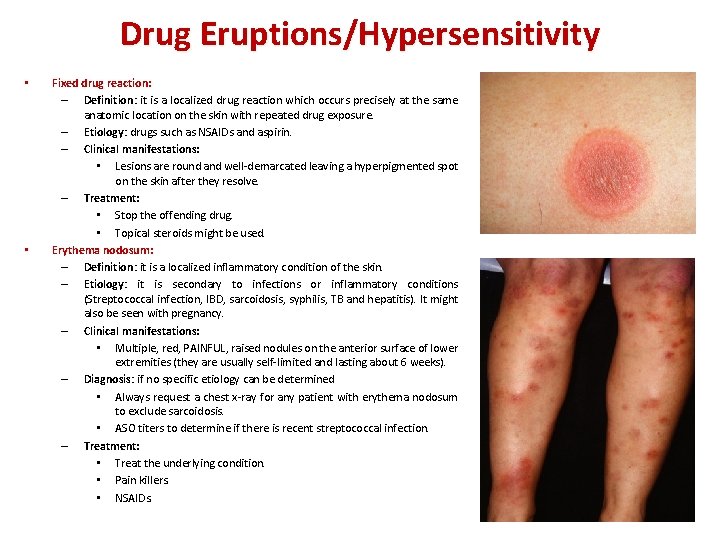
Drug Eruptions/Hypersensitivity • • Fixed drug reaction: – Definition: it is a localized drug reaction which occurs precisely at the same anatomic location on the skin with repeated drug exposure. – Etiology: drugs such as NSAIDs and aspirin. – Clinical manifestations: • Lesions are round and well-demarcated leaving a hyperpigmented spot on the skin after they resolve. – Treatment: • Stop the offending drug. • Topical steroids might be used. Erythema nodosum: – Definition: it is a localized inflammatory condition of the skin. – Etiology: it is secondary to infections or inflammatory conditions (Streptococcal infection, IBD, sarcoidosis, syphilis, TB and hepatitis). It might also be seen with pregnancy. – Clinical manifestations: • Multiple, red, PAINFUL, raised nodules on the anterior surface of lower extremities (they are usually self-limited and lasting about 6 weeks). – Diagnosis: if no specific etiology can be determined • Always request a chest x-ray for any patient with erythema nodosum to exclude sarcoidosis. • ASO titers to determine if there is recent streptococcal infection. – Treatment: • Treat the underlying condition. • Pain killers. • NSAIDs.
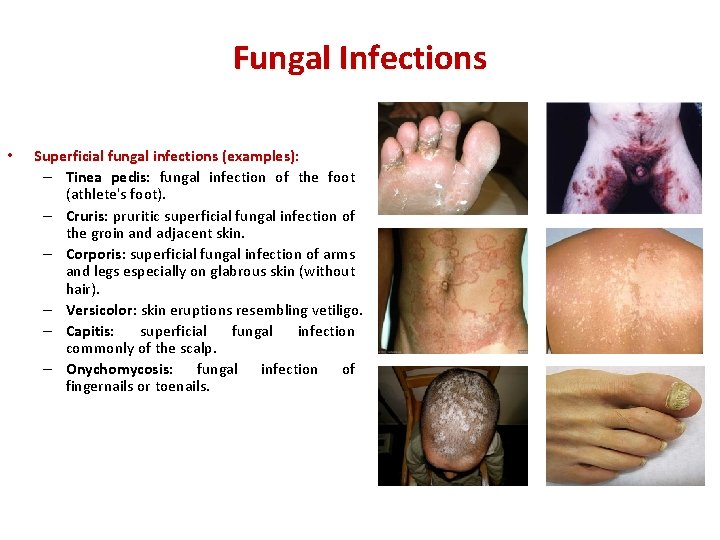
Fungal Infections • Superficial fungal infections (examples): – Tinea pedis: fungal infection of the foot (athlete's foot). – Cruris: pruritic superficial fungal infection of the groin and adjacent skin. – Corporis: superficial fungal infection of arms and legs especially on glabrous skin (without hair). – Versicolor: skin eruptions resembling vetiligo. – Capitis: superficial fungal infection commonly of the scalp. – Onychomycosis: fungal infection of fingernails or toenails.

Fungal Infections • • Superficial fungal infections: – Definition: they are referred to infections limited to the skin, hair or nails. – Diagnosis: • Diagnosis is mostly made clinically by (visual appearance). • Diagnosis can be confirmed with potassium hydroxide (KOH) test: by removing epithelial cells from the site of infection and adding KOH which dissolves epithelial cells but cannot dissolve the fungus thus revealing fungal hyphae. • Most accurate diagnostic test: culturing the fungus but it can take up to 6 weeks (which is not clinically practical). – Treatment: • Onychomycosis (nail infection) and tinea capitis (hair infection) must be treated with oral medications such as terbinafine. It is used 6 weeks for fingernails and 12 weeks for toenails. • Skin infections are treated with topical antifungals (azoles) such as ketoconazole, econazole and miconazole Tinea versicolor: – Definition: it is a superficial fungal infection of the skin which is characterized by the presence of multiple macules (usually asmptomatic) varying in color from white to brown. A macule is a flat, demarcated, discolored area of the skin < 1 cm. – Etiology: Malassezia furfur. – Clinical manifestations: white/brown macules that tend to merge together and are found on the chest, neck, abdomen or face. – Diagnosis: skin scrapings examined with 10% KOH showing fungal hyphae (spaghetti and meatballs pattern). – Treatment: topical ketoconazole or oral itraconazole (depending on amount of surface area involved).
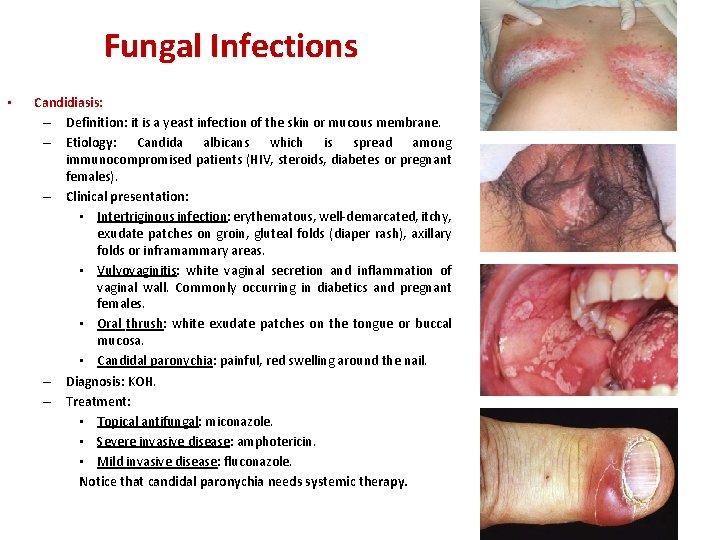
Fungal Infections • Candidiasis: – Definition: it is a yeast infection of the skin or mucous membrane. – Etiology: Candida albicans which is spread among immunocompromised patients (HIV, steroids, diabetes or pregnant females). – Clinical presentation: • Intertriginous infection: erythematous, well-demarcated, itchy, exudate patches on groin, gluteal folds (diaper rash), axillary folds or inframammary areas. • Vulvovaginitis: white vaginal secretion and inflammation of vaginal wall. Commonly occurring in diabetics and pregnant females. • Oral thrush: white exudate patches on the tongue or buccal mucosa. • Candidal paronychia: painful, red swelling around the nail. – Diagnosis: KOH. – Treatment: • Topical antifungal: miconazole. • Severe invasive disease: amphotericin. • Mild invasive disease: fluconazole. Notice that candidal paronychia needs systemic therapy.
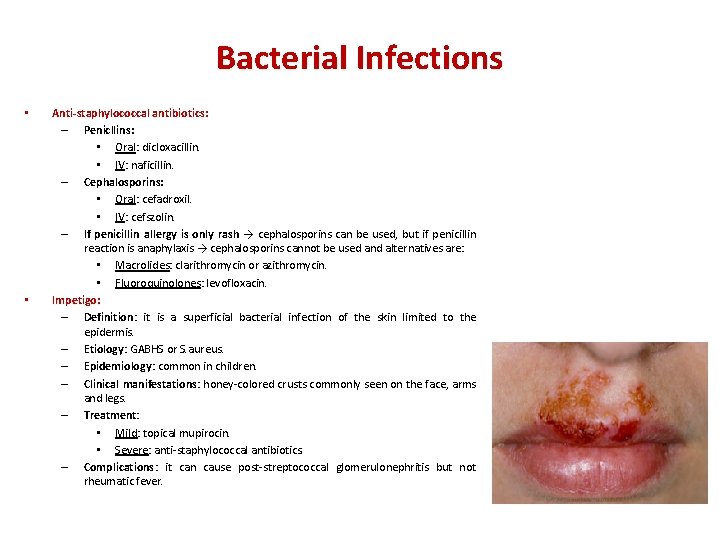
Bacterial Infections • • Anti-staphylococcal antibiotics: – Penicllins: • Oral: dicloxacillin. • IV: naficillin. – Cephalosporins: • Oral: cefadroxil. • IV: cefszolin. – If penicillin allergy is only rash → cephalosporins can be used, but if penicillin reaction is anaphylaxis → cephalosporins cannot be used and alternatives are: • Macrolides: clarithromycin or azithromycin. • Fluoroquinolones: levofloxacin. Impetigo: – Definition: it is a superficial bacterial infection of the skin limited to the epidermis. – Etiology: GABHS or S. aureus. – Epidemiology: common in children. – Clinical manifestations: honey-colored crusts commonly seen on the face, arms and legs. – Treatment: • Mild: topical mupirocin. • Severe: anti-staphylococcal antibiotics. – Complications: it can cause post-streptococcal glomerulonephritis but not rheumatic fever.
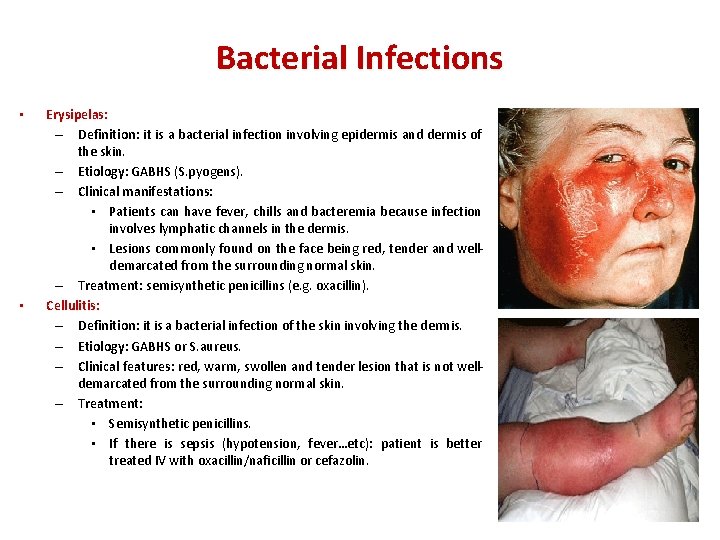
Bacterial Infections • • Erysipelas: – Definition: it is a bacterial infection involving epidermis and dermis of the skin. – Etiology: GABHS (S. pyogens). – Clinical manifestations: • Patients can have fever, chills and bacteremia because infection involves lymphatic channels in the dermis. • Lesions commonly found on the face being red, tender and welldemarcated from the surrounding normal skin. – Treatment: semisynthetic penicillins (e. g. oxacillin). Cellulitis: – Definition: it is a bacterial infection of the skin involving the dermis. – Etiology: GABHS or S. aureus. – Clinical features: red, warm, swollen and tender lesion that is not welldemarcated from the surrounding normal skin. – Treatment: • Semisynthetic penicillins. • If there is sepsis (hypotension, fever…etc): patient is better treated IV with oxacillin/naficillin or cefazolin.
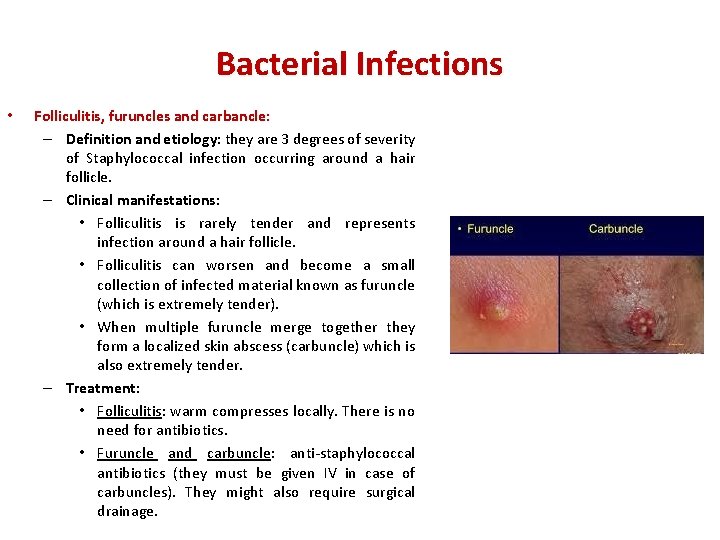
Bacterial Infections • Folliculitis, furuncles and carbancle: – Definition and etiology: they are 3 degrees of severity of Staphylococcal infection occurring around a hair follicle. – Clinical manifestations: • Folliculitis is rarely tender and represents infection around a hair follicle. • Folliculitis can worsen and become a small collection of infected material known as furuncle (which is extremely tender). • When multiple furuncle merge together they form a localized skin abscess (carbuncle) which is also extremely tender. – Treatment: • Folliculitis: warm compresses locally. There is no need for antibiotics. • Furuncle and carbuncle: anti-staphylococcal antibiotics (they must be given IV in case of carbuncles). They might also require surgical drainage.
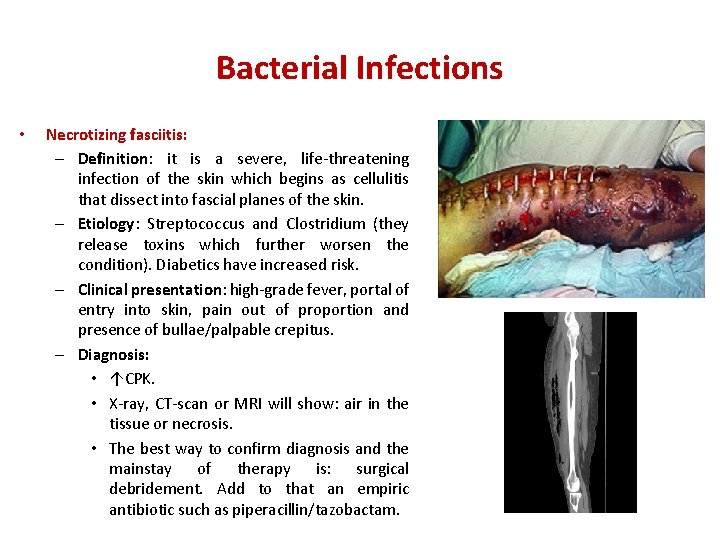
Bacterial Infections • Necrotizing fasciitis: – Definition: it is a severe, life-threatening infection of the skin which begins as cellulitis that dissect into fascial planes of the skin. – Etiology: Streptococcus and Clostridium (they release toxins which further worsen the condition). Diabetics have increased risk. – Clinical presentation: high-grade fever, portal of entry into skin, pain out of proportion and presence of bullae/palpable crepitus. – Diagnosis: • ↑CPK. • X-ray, CT-scan or MRI will show: air in the tissue or necrosis. • The best way to confirm diagnosis and the mainstay of therapy is: surgical debridement. Add to that an empiric antibiotic such as piperacillin/tazobactam.
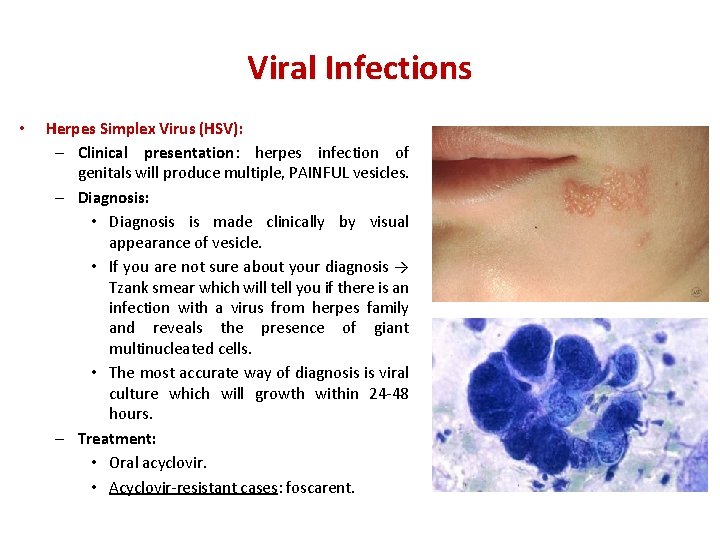
Viral Infections • Herpes Simplex Virus (HSV): – Clinical presentation: herpes infection of genitals will produce multiple, PAINFUL vesicles. – Diagnosis: • Diagnosis is made clinically by visual appearance of vesicle. • If you are not sure about your diagnosis → Tzank smear which will tell you if there is an infection with a virus from herpes family and reveals the presence of giant multinucleated cells. • The most accurate way of diagnosis is viral culture which will growth within 24 -48 hours. – Treatment: • Oral acyclovir. • Acyclovir-resistant cases: foscarent.
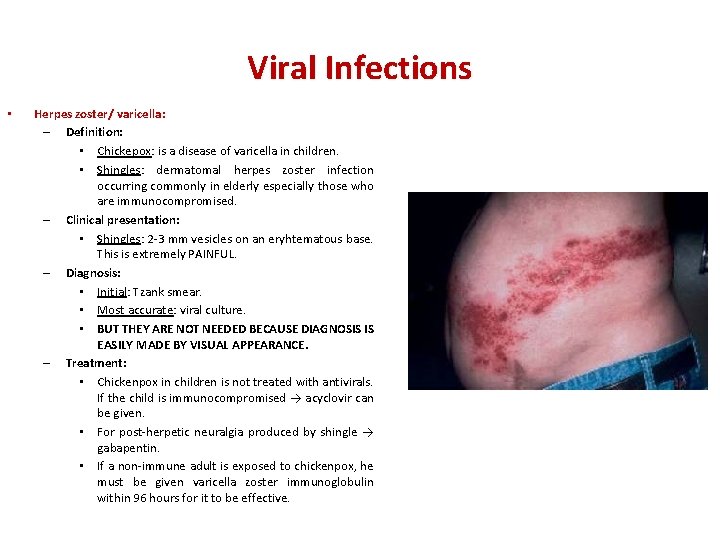
Viral Infections • Herpes zoster/ varicella: – Definition: • Chickepox: is a disease of varicella in children. • Shingles: dermatomal herpes zoster infection occurring commonly in elderly especially those who are immunocompromised. – Clinical presentation: • Shingles: 2 -3 mm vesicles on an eryhtematous base. This is extremely PAINFUL. – Diagnosis: • Initial: Tzank smear. • Most accurate: viral culture. • BUT THEY ARE NOT NEEDED BECAUSE DIAGNOSIS IS EASILY MADE BY VISUAL APPEARANCE. – Treatment: • Chickenpox in children is not treated with antivirals. If the child is immunocompromised → acyclovir can be given. • For post-herpetic neuralgia produced by shingle → gabapentin. • If a non-immune adult is exposed to chickenpox, he must be given varicella zoster immunoglobulin within 96 hours for it to be effective.
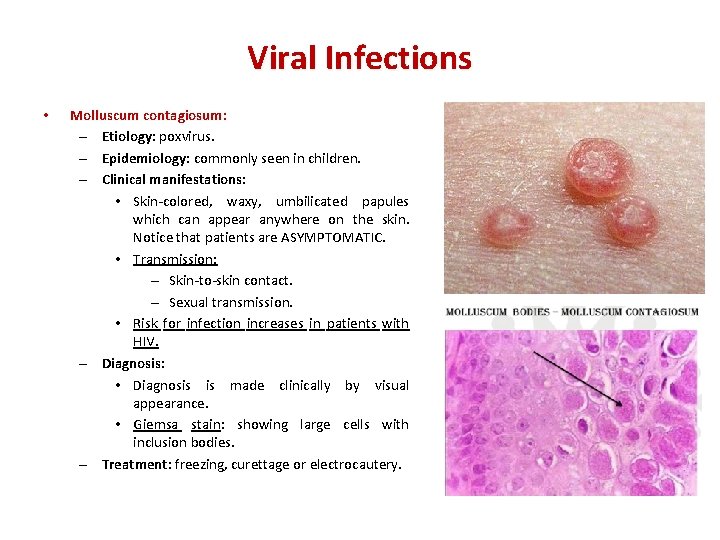
Viral Infections • Molluscum contagiosum: – Etiology: poxvirus. – Epidemiology: commonly seen in children. – Clinical manifestations: • Skin-colored, waxy, umbilicated papules which can appear anywhere on the skin. Notice that patients are ASYMPTOMATIC. • Transmission: – Skin-to-skin contact. – Sexual transmission. • Risk for infection increases in patients with HIV. – Diagnosis: • Diagnosis is made clinically by visual appearance. • Giemsa stain: showing large cells with inclusion bodies. – Treatment: freezing, curettage or electrocautery.

Parasitic Infections • Scabies: – Definition: it is a parasitic skin infection which is characterized by: • Superficial burrows. • Intense pruritus. • Secondary infections. – Etiology: female of Sarcoptes scabiei which burrows into the skin causing vesicular eruptions. It is transmitted by skin-toskin contact. – Clinical manifestations: • Superficial burrows commonly seen on web spaces if hands and feet. It can also produce pruritic lesions around penis, breast and axillary folds. It spares the head. – Diagnosis: • Usually clinically. • But can be confirmed by scraping out the organism after applying mineral oil into the superficial skin burrow. – Treatment: • Permethrin: it is a medication which is used against scabies and live. In addition, is is an insecticide.
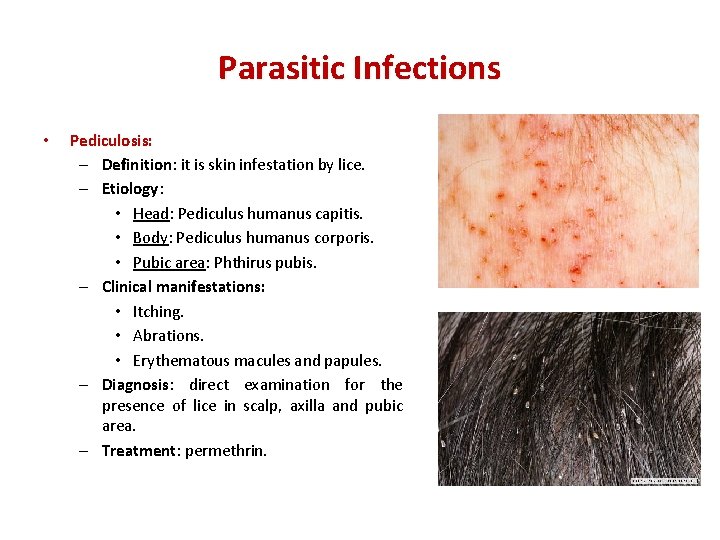
Parasitic Infections • Pediculosis: – Definition: it is skin infestation by lice. – Etiology: • Head: Pediculus humanus capitis. • Body: Pediculus humanus corporis. • Pubic area: Phthirus pubis. – Clinical manifestations: • Itching. • Abrations. • Erythematous macules and papules. – Diagnosis: direct examination for the presence of lice in scalp, axilla and pubic area. – Treatment: permethrin.

Toxin-Mediated Diseases • Toxic shock syndrome: – Etiology: it is a systemic reaction caused by toxin which is produced by Staphylococcus attached to a foreign body (tampon or surgical materials retained in the body). – Clinical manifestations/diagnosis: you need ≥ of the following criteria to diagnose toxic shock syndrome: • High-grade fever > 39 C. • Systolic blood pressure < 90 mm. Hg. • Desquamative skin rash. • Vomiting. • Involvement of mucous membranes (eyes, mouth or genitals). • Elevated bilirubin. • Platelet count < 100, 000. – Treatment: • Remove the source of infection. • IV fluid therapy (because patient is in shock). • Pressors (such as dopamine). • Antibiotics: – Methicillin-sensitive: clindamycin + oxacillin. – Methicillin-resistant (MRSA): vancomycin.
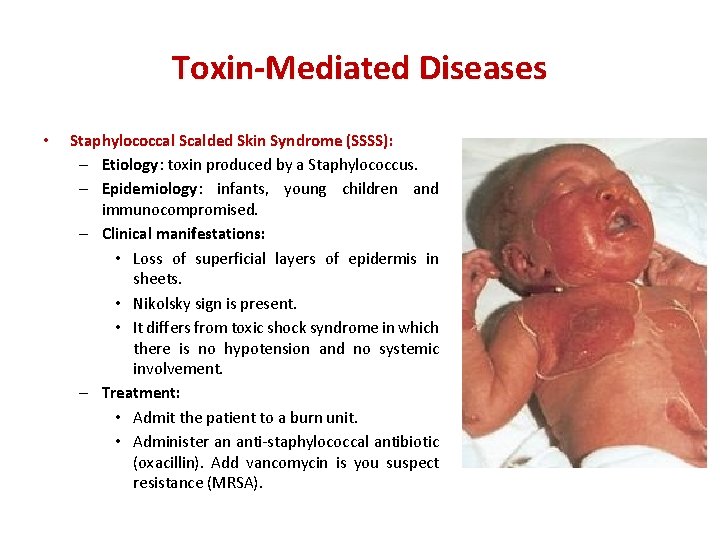
Toxin-Mediated Diseases • Staphylococcal Scalded Skin Syndrome (SSSS): – Etiology: toxin produced by a Staphylococcus. – Epidemiology: infants, young children and immunocompromised. – Clinical manifestations: • Loss of superficial layers of epidermis in sheets. • Nikolsky sign is present. • It differs from toxic shock syndrome in which there is no hypotension and no systemic involvement. – Treatment: • Admit the patient to a burn unit. • Administer an anti-staphylococcal antibiotic (oxacillin). Add vancomycin is you suspect resistance (MRSA).

Benign and Precancerous Lesions • • How to differentiate between benign and malignant skin lesions? – Benign skin lesions are characterized by the following: • They do not grow in size with time. • They have smooth, regular borders. • They are usually < 1 cm in diameter. • They have a homogenous color. – The most accurate method to differentiate between benign and malignant skin lesions is by skin biopsy. Seborrheic keratosis: – Definition: it is a benign skin condition which is commonly seen in elderly. – Clinical manifestations: hyperpigmented lesions with a “stuck-on’ appearance commonly found on the chest, back, shoulders and face. – Treatment: removal for cosmetic purposes by: • Liquid nitrogen. • Curettage.
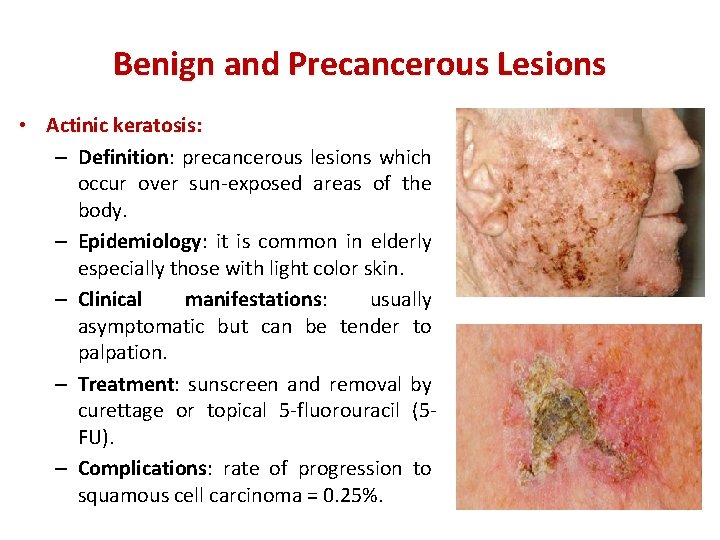
Benign and Precancerous Lesions • Actinic keratosis: – Definition: precancerous lesions which occur over sun-exposed areas of the body. – Epidemiology: it is common in elderly especially those with light color skin. – Clinical manifestations: usually asymptomatic but can be tender to palpation. – Treatment: sunscreen and removal by curettage or topical 5 -fluorouracil (5 FU). – Complications: rate of progression to squamous cell carcinoma = 0. 25%.

Malignant Diseases • Melanoma: – Definition: it is the most common skin malignancy accounting for 2/3 of cases. – Clinical manifestations: • Malignant lesions are characterized by the following: – They grow in size with time. – They have irregular borders. – Size > 1 cm in diameter. – Their color is not homogenous. • There are two types of melanoma: – Lentigo maligna melanoma: occurring over sun-exposed areas in elderly. – Acral-lentiginous melanoma: occurring in palms of hands, soles of feet or nail beds. – Diagnosis: • Full-thickness skin biopsy (why? ) → because depth of the lesion is the most important prognostic factor. – Treatment: excision. The size of margin of skin around melanoma which has to be removed is determined by the depth of melanoma: • Melanoma-in-situ: 0. 5 cm margin. • Melanoma < 1 mm depth: 1 cm margin. • Melanoma 1 -2 mm depth: 2 cm margin. • Melanoma > 2 mm depth: 3 cm margin.
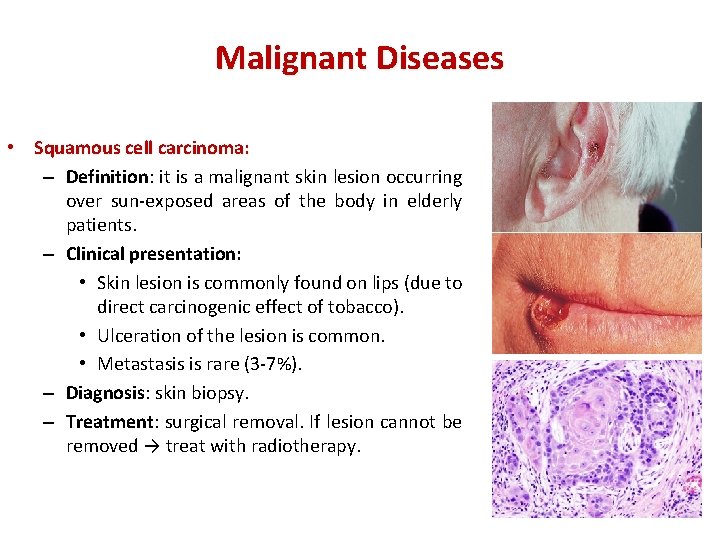
Malignant Diseases • Squamous cell carcinoma: – Definition: it is a malignant skin lesion occurring over sun-exposed areas of the body in elderly patients. – Clinical presentation: • Skin lesion is commonly found on lips (due to direct carcinogenic effect of tobacco). • Ulceration of the lesion is common. • Metastasis is rare (3 -7%). – Diagnosis: skin biopsy. – Treatment: surgical removal. If lesion cannot be removed → treat with radiotherapy.
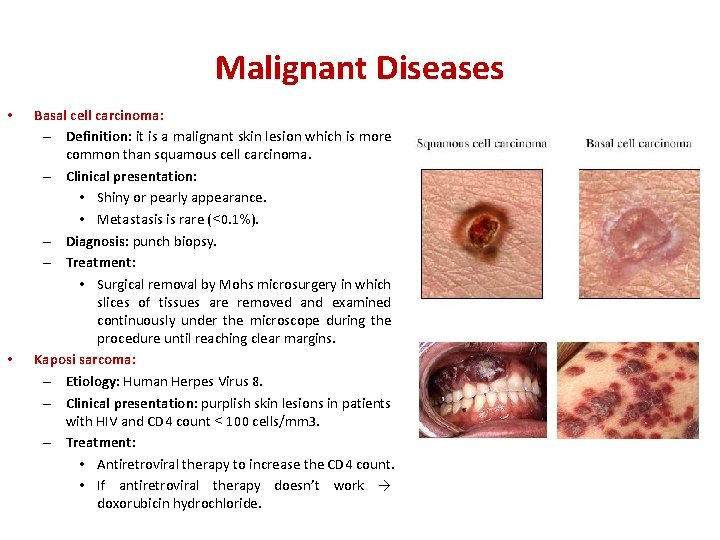
Malignant Diseases • • Basal cell carcinoma: – Definition: it is a malignant skin lesion which is more common than squamous cell carcinoma. – Clinical presentation: • Shiny or pearly appearance. • Metastasis is rare (<0. 1%). – Diagnosis: punch biopsy. – Treatment: • Surgical removal by Mohs microsurgery in which slices of tissues are removed and examined continuously under the microscope during the procedure until reaching clear margins. Kaposi sarcoma: – Etiology: Human Herpes Virus 8. – Clinical presentation: purplish skin lesions in patients with HIV and CD 4 count < 100 cells/mm 3. – Treatment: • Antiretroviral therapy to increase the CD 4 count. • If antiretroviral therapy doesn’t work → doxorubicin hydrochloride.
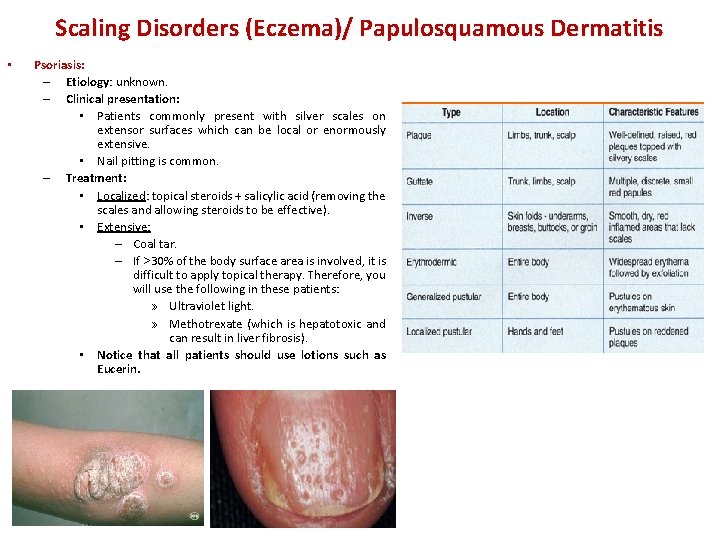
Scaling Disorders (Eczema)/ Papulosquamous Dermatitis • Psoriasis: – Etiology: unknown. – Clinical presentation: • Patients commonly present with silver scales on extensor surfaces which can be local or enormously extensive. • Nail pitting is common. – Treatment: • Localized: topical steroids + salicylic acid (removing the scales and allowing steroids to be effective). • Extensive: – Coal tar. – If >30% of the body surface area is involved, it is difficult to apply topical therapy. Therefore, you will use the following in these patients: » Ultraviolet light. » Methotrexate (which is hepatotoxic and can result in liver fibrosis). • Notice that all patients should use lotions such as Eucerin.
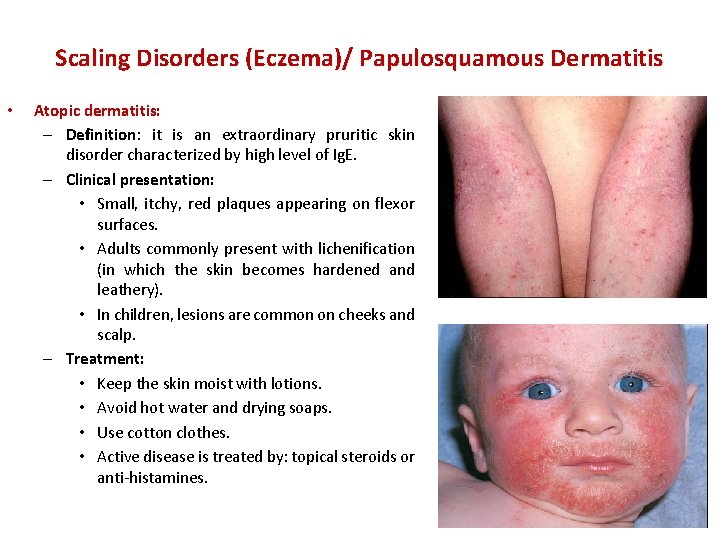
Scaling Disorders (Eczema)/ Papulosquamous Dermatitis • Atopic dermatitis: – Definition: it is an extraordinary pruritic skin disorder characterized by high level of Ig. E. – Clinical presentation: • Small, itchy, red plaques appearing on flexor surfaces. • Adults commonly present with lichenification (in which the skin becomes hardened and leathery). • In children, lesions are common on cheeks and scalp. – Treatment: • Keep the skin moist with lotions. • Avoid hot water and drying soaps. • Use cotton clothes. • Active disease is treated by: topical steroids or anti-histamines.
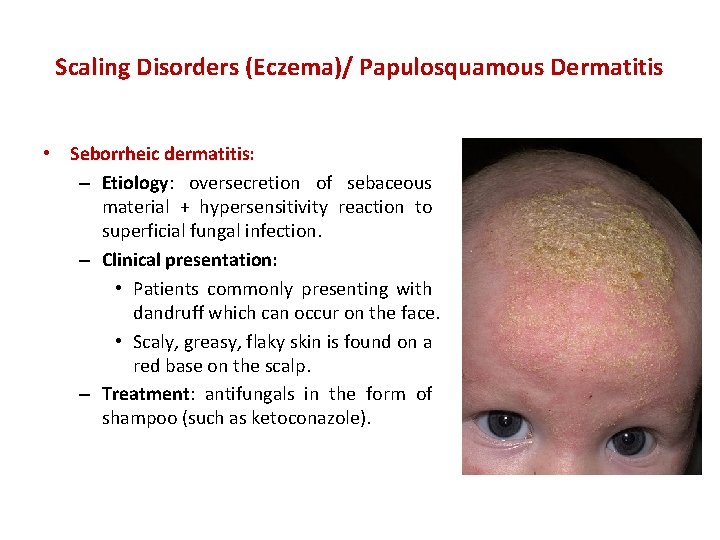
Scaling Disorders (Eczema)/ Papulosquamous Dermatitis • Seborrheic dermatitis: – Etiology: oversecretion of sebaceous material + hypersensitivity reaction to superficial fungal infection. – Clinical presentation: • Patients commonly presenting with dandruff which can occur on the face. • Scaly, greasy, flaky skin is found on a red base on the scalp. – Treatment: antifungals in the form of shampoo (such as ketoconazole).

Scaling Disorders (Eczema)/ Papulosquamous Dermatitis • • Stasis dermatitis: – Definition: it is hyperpigmentation of the skin due to accumulation of hemosiderin in the dermis. – Etiology: it occurs over a long period of time and is due to venous incompetence of lower extremities resulting in extravasation of blood in dermis. – Treatment: it cannot be reversed. Further progression can be prevented by elevation of the legs and lower extremity support hose. Contact dermatitis: – Etiology: it is a hypersensitivity reaction to: soaps, detergents, sunscreens, jewelry and latex. – Clinical presentation: lesions can appear as linear, streaked vesicles when caused by poison ivy. – Diagnosis: patch test (it determines whether a specific substance causes allergic inflammation of patient’s skin). – Treatment: • Determine the specific cause and avoid it. • Topical steroids and anti-histamines.

Scaling Disorders (Eczema)/ Papulosquamous Dermatitis • Pityriasis rosea: – Definition: it is a pruritic eruption which begins usually with a herald patch (in 80% of times). It is self-limited and resolves within 8 weeks without leaving a scar. – Clinical presentation: • Erythematous. • Salmon-colored. • Herald patch is present. • Looks like secondary syphilis. • Spares palms and soles. – Diagnosis: clinically but to make sure it is not secondary syphilis there will be negative VDRL/RPR. – Treatment: it is self-limited but very itchy lesions can be treated with topical steroids.
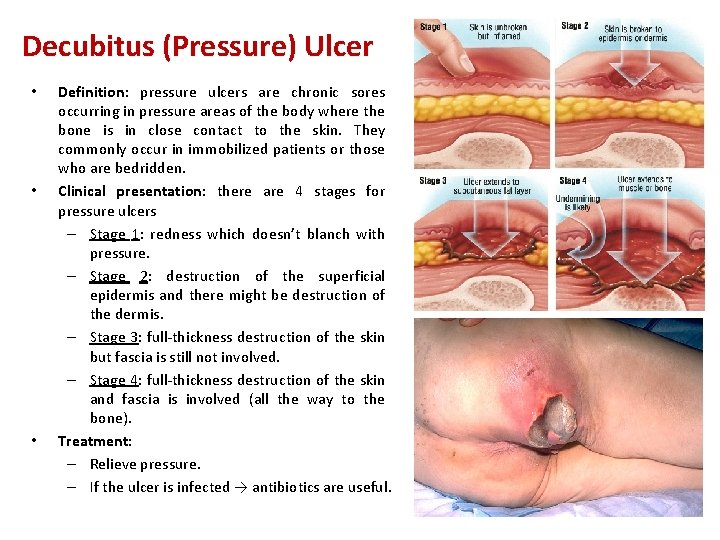
Decubitus (Pressure) Ulcer • • • Definition: pressure ulcers are chronic sores occurring in pressure areas of the body where the bone is in close contact to the skin. They commonly occur in immobilized patients or those who are bedridden. Clinical presentation: there are 4 stages for pressure ulcers – Stage 1: redness which doesn’t blanch with pressure. – Stage 2: destruction of the superficial epidermis and there might be destruction of the dermis. – Stage 3: full-thickness destruction of the skin but fascia is still not involved. – Stage 4: full-thickness destruction of the skin and fascia is involved (all the way to the bone). Treatment: – Relieve pressure. – If the ulcer is infected → antibiotics are useful.
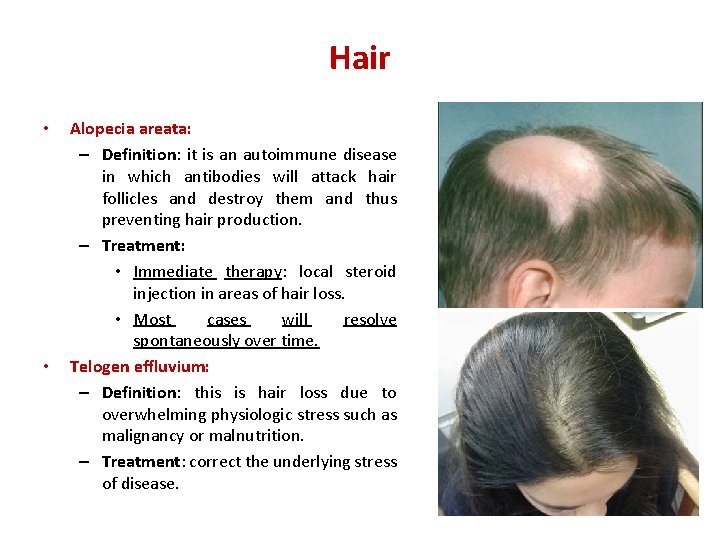
Hair • • Alopecia areata: – Definition: it is an autoimmune disease in which antibodies will attack hair follicles and destroy them and thus preventing hair production. – Treatment: • Immediate therapy: local steroid injection in areas of hair loss. • Most cases will resolve spontaneously over time. Telogen effluvium: – Definition: this is hair loss due to overwhelming physiologic stress such as malignancy or malnutrition. – Treatment: correct the underlying stress of disease.
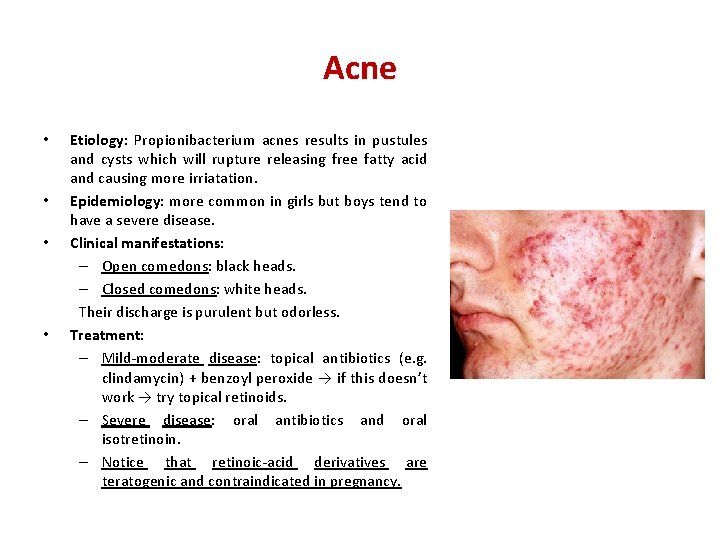
Acne • • Etiology: Propionibacterium acnes results in pustules and cysts which will rupture releasing free fatty acid and causing more irriatation. Epidemiology: more common in girls but boys tend to have a severe disease. Clinical manifestations: – Open comedons: black heads. – Closed comedons: white heads. Their discharge is purulent but odorless. Treatment: – Mild-moderate disease: topical antibiotics (e. g. clindamycin) + benzoyl peroxide → if this doesn’t work → try topical retinoids. – Severe disease: oral antibiotics and oral isotretinoin. – Notice that retinoic-acid derivatives are teratogenic and contraindicated in pregnancy.
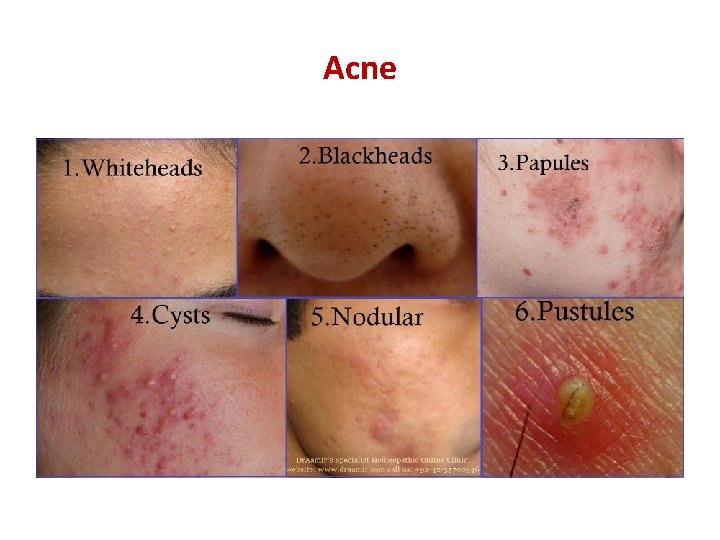
Acne
- Slides: 39