Kimberly K Kopp BSN RN CWOCN CFCN LEARNING

Kimberly K Kopp BSN, RN, CWOCN, CFCN

LEARNING OUTCOMES Participants will be able to:

§ Financial burden – § Year 2000 estimated at $19. 5 billion § $14. 2 billion incurred by community residents § $5. 3 billion by institutional residents. § $900 annually paid privately for pads § 25 million women affected by incontinence § 1 in 4 women over 18 report episodes of incontinence § On average, women wait 6. 5 years from the first time they experience symptoms until they obtain a diagnosis for their incontinence § 80% of those affected can be improved or cured with treatment § U. S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National Center for Health Statistics , Vital and Health Statistics, Prevalence of Incontinence Among Older Americans, Series 3, Number 36, June 2014 § National Association for Continence website

§ Need to be a Nurse Practitioner § Need expensive high tech equipment § Need to be able to do Urodynamics § Continence exam is too hard to pass § Already to busy don’t have time for Continence § I already take care of IAD so I am taking care of the incontinence issue

§Direct Patient Care – many opportunities §Bring new products to the facility to use §Resource person for staff §Help develop new protocols §Education of the staff and the public

§ CAUTI prevention § Prevention and Management of Incontinence Associated Dermatitis § High volume fecal output § Urinary incontinence § Staff education § Develop protocols for product usage § Product review § Teaching how to self catheterize § Assist patients with obtaining supplies for home

§ Assist with management of foley catheters § Suprapubic vs Urethral § Removal vs Long term placement § Obtaining UA’s § Develop simple management and education for staff as well as patient and families § Toileting programs § Chronic constipation § Dietary modifications § Containment products § Skin care

§ CMS mandates that facilities address § Avoidance of inappropriate catheter usage § Avoid inappropriate treatment of nonsymptomatic bacteriuria § Continence program for residents that have some ability to respond to cues to urinate § Bowel management regime to prevent constipation and impactions

§ Continence nurse can § Do basic baseline assessment of urinary / bowel system § Provide basic counseling to patients for § Dietary modifications § Pelvic floor exercises § Toileting programs § Clean intermittent catheterization procedure § Bladder control strategies § Containment options § Determine need for further referral

§ Women’s Health Events § Healthy U hospital educational event for public § Nursing staff § Always new nurses that need education § Education impacts the direct patient care § Primary care physicians § When to do a UA in long term catheterized patients § Management of those patients in the nursing homes § Treatment of women with chronic UTI’s § Antibiotics vs Vaginal estrogen

§ Report at huddle § 81 y/o male admitted to our Swing bed with CHF § Recent catheter placement in city due to acute renal failure and retention § Local physician wanted catheter changed to obtain urine specimen as WBC remained elevated § Urine had been bloody & bloody drainage around meatus § Nursing reports that catheter draining well

§Suggested use of a double balloon catheter to decrease irritation of bladder §Nurse not familiar with new double balloon catheter so offered to assist § 400 cc urine in bag at time of change but patient was uncomfortable and looked distended §Double balloon catheter inserted and immediately drained 1300 cc urine §Renal function improved, WBC normalized

§ 48 y/o female Physical therapy aide at CCMH § Complaint of frequency and urgency § Heard we had new incontinence equipment so got referral for treatment

§ Normal anatomy § Voiding every 30 -60 minutes during day § Up 4 -6 times a night § Had separate bedrooms at home § Didn’t want to take medication or have surgery

§ Initiated the biofeedback and electrical stimulation § Good pelvic floor strength § Education § Basic voiding anatomy and physiology § Urge suppression § Bladder retraining

§ In 6 weeks she was sleeping all night § Going 3 hours without voiding at work § Felt the best she had in years

§Impacts responsibilities at work §Fear of leaving home due to leakage §Embarrassment §Isolation §Stress in relationships §Depression §Desperate for help

§ 36 y/o female § Long standing urinary incontinence § 2 urologist, 2 surgeries, several urodynamic studies, medications § Willing to private pay for biofeedback and e stim due to desperation

§Assessment § Amazing pelvic floor strength § No consistent pattern to the incontinence § Wasn’t typical urge or stress § “normal” bowel routine § Had never been discussed with her §Solution § Added fiber to improve her normal bowel routine

§ 84 y/o female walks into office c/o incontinence § Totally incontinent § Never walked to bathroom to void § Rarely left home § Initial treatment § Bladder diary § Bladder retraining § Return appointment § Voiding every 2 hours § Going to visit grandchildren

§ 44 y/o female quad lived at home with assistance of home health care and private care givers § Repeated UTI’s and was receiving IV antibiotics every 6 weeks § Was so depressed and tired of feeling terrible she drove wheelchair down flight of stairs in suicide attempt

§ Introduced her to the option of the double balloon catheter by having her watch the video about the catheter § Has been using the double balloon catheter for 3 years now and has had only 1 -2 UTI’s/year that have been treated with oral antibiotics

§Diet and fluid intake §Bladder routine §Bowel routine

§ Prolapse § Fragile vaginal tissue § Squeeze fingers § Bladder distention § scan

§Patients aren’t asking for a miracle cure §They want someone to make their life more manageable §It really isn’t complicated or technical

§ 83 y/o active male §New indwelling catheter due to hematuria postop polyp removal couple days prior §Presented to the admissions department with complaints about the catheter
§Bilateral arm amputee of 50 years

§Tubing taped too tight was pulling §Are you having any other problems that I can help you with today? Response §I don’t want to bother you I know you are busy §I am having a little trouble emptying the leg bag

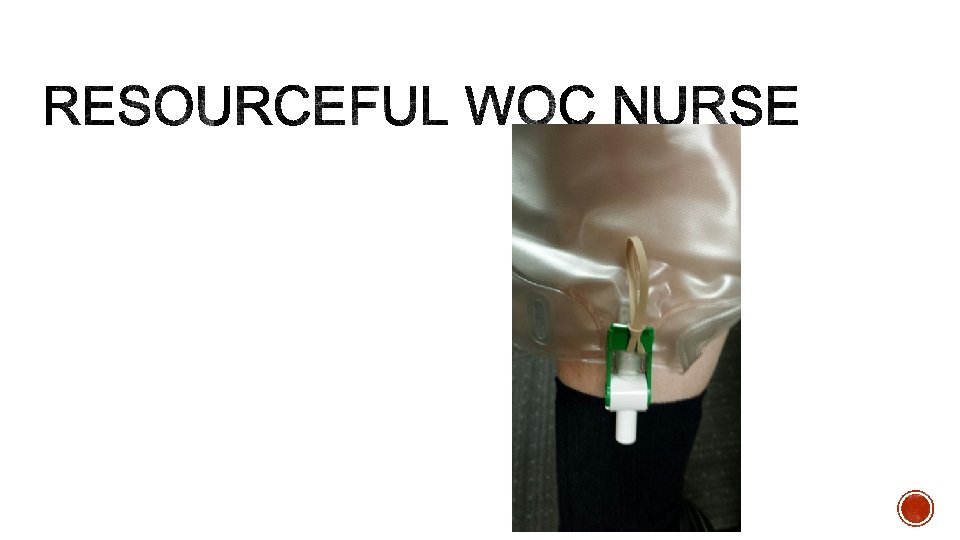
§ Cant get hook behind clamp to open drain § Need an extension on green handle


§ U. S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National Center for Health Statistics , Vital and Health Statistics, Prevalence of Incontinence Among Older Americans, Series 3, Number 36, June 2014 § National Association for Continence website

- Slides: 33