Kentucky Primary Care Association MCO Panel About Anthem

Kentucky Primary Care Association MCO Panel

About Anthem Medicaid Members Providers Quality Covered Services Value Added Benefits 2

About the Outreach Team Since 2014, the Anthem Medicaid team can be found across the Commonwealth listening to members, interacting with providers and partnering with community-based organizations. 3

Community Involvement • State-wide partnerships with thousands of organizations • Support outreach efforts in every KY county • Sponsor hundreds of events, initiatives and programs state-wide • Health promotion activities in schools o o Dental Handwashing Nutrition Bullying prevention 4

Community Involvement Support Health Education and Research Health, Career, Safety and Resource Fairs Community Service Agencies-Fundraisers Homeless Shelters Recovery Homes Food Banks-Education and Volunteering Public Libraries-Children’s programming Public Medicaid Q&A sessions Health Departments-Councils, Coalitions, Collaborations Extension Offices-Community Baby Showers Re-Entry Councils-Addressing SDOH for Re-Entry Populations 5
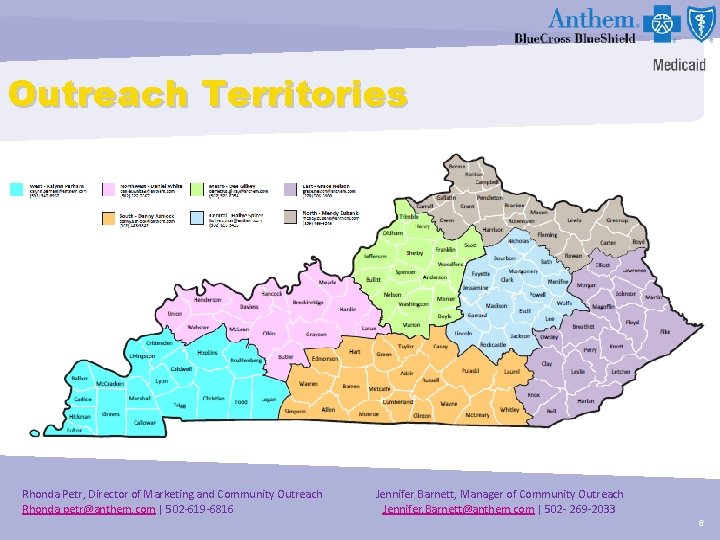
Outreach Territories Rhonda Petr, Director of Marketing and Community Outreach Rhonda. petr@anthem. com | 502 -619 -6816 Jennifer Barnett, Manager of Community Outreach Jennifer. Barnett@anthem. com | 502 - 269 -2033 6
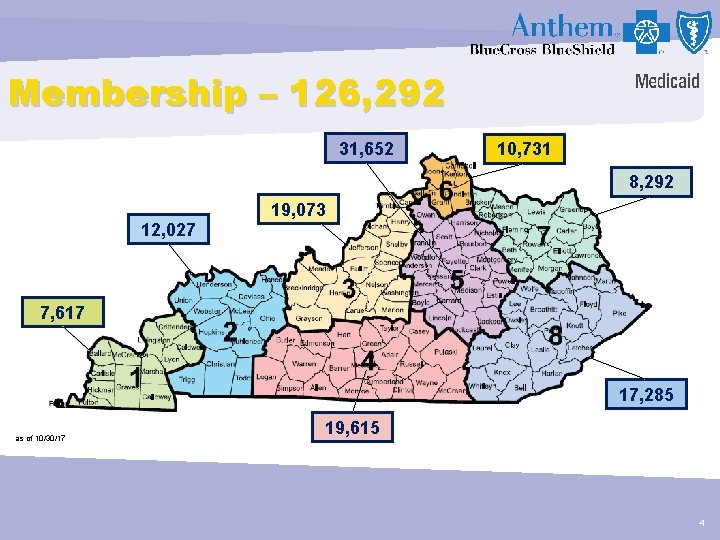
Membership – 126, 292 31, 652 10, 731 8, 292 12, 027 19, 073 7, 617 17, 285 as of 10/30/17 19, 615 4

Provider Network Anthem Medicaid has a very comprehensive, statewide network that includes over 20, 000 providers. The overall network composition is as follows: Region 1 – 1, 641 Region 2 – 2, 503 Region 3 – 10, 275 Hospitals 107 PCP’s Over 3, 600 Region 4 – 3, 855 Region 5 – 7, 999 Specialists Over 14, 000 BH Over 2, 000 Region 6 – 1, 693 Region 7 – 1, 903 Region 8 – 5, 024 5

Provider Incentives Provider Access and Quality Care Program (PAQCP) – targets PCPs with panels between 250 - 999 members. Provider Quality Incentive Program (PQIP) focuses on PCPs with panels over 1, 000 members Behavioral Health Quality Incentive Program (BHQIP) - targets Behavioral Health Providers (such as CMHCs, CSBs, and LMHA’s) 7

NCQA Accreditation Standards: Quality Improvement Member Connections Network Management Scored 100% of the available 50 points. Survey held March 27 -28, 2017 Member Rights & Responsibilities Credentialing Utilization Management 9

Covered Services • • Physician office visits No referrals required Inpatient & outpatient services Emergency services Home health Maternity services Chiropractic care Prescriptions 6

Pharmacy Care • Immunizations are NOW covered in Pharmacy’s in lieu of members visiting PCP • Drug Formulary can be found on the member website at: https: //fm. formularynavigator. com/FBO/4/Kent ucky_PDL_English. pdf 8

Enhanced Vision Services • Eyeglasses for Adults OR a credit for contacts ANNUALLY • Eyeglasses for children (up to two pair per year with EPSDT benefit) • Special needs eyeglasses for children (when medically necessary) • Vision screenings for all ages Eye. Quest is our vision vendor 12

Enhanced Dental Services • Reimbursement codes for missed appointments • Nitrous oxide for children when medically necessary • Services on multiple quadrants during one visit • Scaling and root-planing Denta. Quest is our vendor 13

Value Added Benefits • No Copays (for anything…) • Free Eyeglasses for ADULTS annually OR a credit towards contact lenses (Anthem is only MCO that offers that!) • Free sports physicals for kids • Free OTC medicines (with prescription) • Free crib or car seat for expectant mothers (attending 7 prenatal visits) • Free reloadable gift cards for prenatal rewards and well child visits • Free Smartphone with data, minutes AND unlimited texting 14

Success Story - Anna Member “Anna” recently switched to Anthem Medicaid. She had been: • Been experiencing multiple health issues including uncontrolled diabetes and renal failure • In and out of nursing and personal care facilities, had no independence • Having trouble filling prescriptions • Missing appointments because of transportation issues • Experiencing multiple ER visits and hospital admissions due to her uncontrolled health issues • Living with a friend and the situation was causing additional anxiety and depression • She was overwhelmed, inundated with issues and to make matter worse… • She did not have a reliable way to communicate with her health team 16

Success Story - Anna Anthem’s Case Managers worked with Anna over several months and assisted her by: • Placing her on formulary insulin prescription • Helping her obtain a glucose meter and supplies • Case Managers helped to work through a DCBS system-issue to remove an old primary insurance listing which was preventing her prescriptions from being properly filled • She was able to select a new, local PCP and dialysis center • She obtained a new smartphone to communicate with her physician and MCO • Eventually moved in with her aunt for a more stable & healthy environment 17

Success Story - Anna • Anna is now living with her aunt, is in control of her health conditions, is attending behavior therapy and working closely with her social worker and case manager. • She is keeping all of her doctor’s appointments, and has not had an ER visit or hospital admission in eight months! • She reports that she is now healthier, happier, and more independent! 18

18
- Slides: 19