Kent Saylor MD October 11 2017 MUHC Health

Kent Saylor, MD October 11, 2017 MUHC Health Equity Symposium INDIGENOUS HEALTH CARE ACCESS – THE ROUTE AHEAD

Recognition of territory

Goals for today At the end of this session learners will: Have a better understanding of the needs for more Indigenous health care providers Have a better understanding of the gap in the number of Indigenous health care providers Have a better understanding of what can be done in academic institutions and health care institutions

Who am I? Pediatrician Northern and Native Child Health Program – MCH Director – Indigenous Health Curriculum Director – Indigenous Health Professions Program Mohawk Nation

Definition An “Indigenous” person is defined as a someone who is either: First Nations Inuit Métis The terms “Indigenous” & “Aboriginal” are synonymous
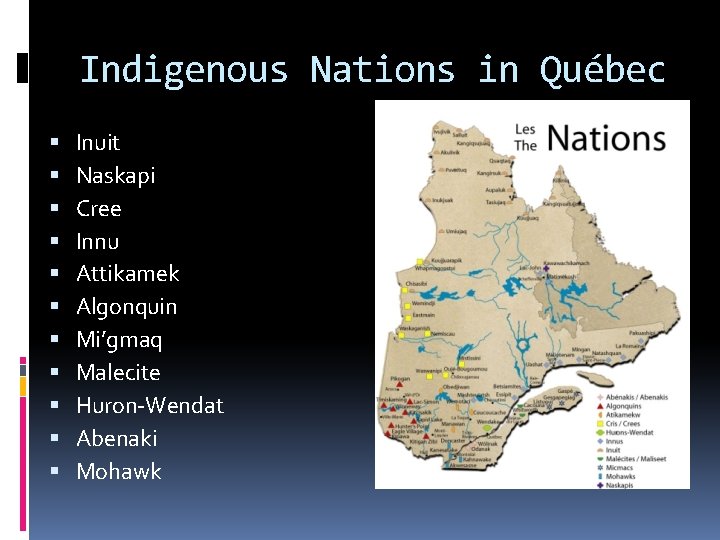
Indigenous Nations in Québec Inuit Naskapi Cree Innu Attikamek Algonquin Mi’gmaq Malecite Huron-Wendat Abenaki Mohawk

Numerous health discrepancies Lower life expectancy Higher infant mortality Medical conditions Diabetes Cancer Infectious disease Bronchiolitis Many others

Factors contributing to health disparities • ACCESS TO CARE, EVEN BASIC PRIMARY CARE, IS DIFFICULT AND ACCESS TO SPECIALIST CARE VERY LIMITED • MANY HEALTH CARE PROFESSIONALS WORK SHORT TERM • LESS KNOWLEDGE OF INDIGENOUS PEOPLES’ CULTURE, HEALTH ISSUES • LANGUAGE BARRIERS WHICH OPTIMAL • SOCIAL DETERMINANTS OF HEALTH • VERY FEW INDIGENOUS HEALTH CARE PROVIDERS • IN QUEBEC: EST. 12 OUT 20, 000 DOCTORS ARE INDIGENOUS MAKES CARE LESS THAN

Many solutions are beyond the reach of health care but. . . Health care professional training schools and health care institutions have a significant role to play Until now we have not made significant efforts to address the health needs on Indigenous peoples
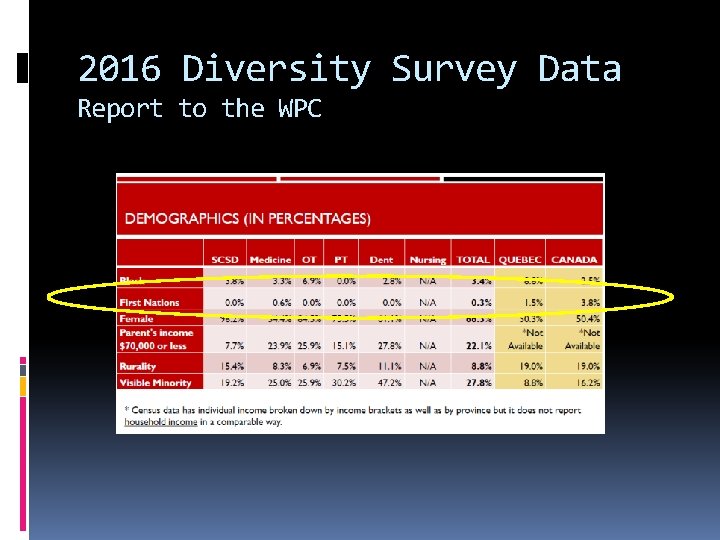
2016 Diversity Survey Data Report to the WPC

Truth and Reconciliation Commission Call to action #23 We call upon all levels of government to: Increase the number of Aboriginal professionals working in the health-care field ii. Ensure the retention of Aboriginal health-care providers in Aboriginal communities iii. Provide cultural competency training for all healthcare professionals i. Truth and Reconciliation Commission of Canada: Calls to action; 2015

Truth and Reconciliation Commission Call to action #24 We call upon medical and nursing schools in Canada to require all students to take a course dealing with Aboriginal health issues, including the history and legacy of residential schools, the United Nations Declaration on the Rights of Indigenous Peoples, Treaties and Aboriginal rights, and Indigenous teachings and practices. This will require skills-based training in intercultural competency, conflict resolution, human rights, and anti-racism.

Experience at Mc. Gill university
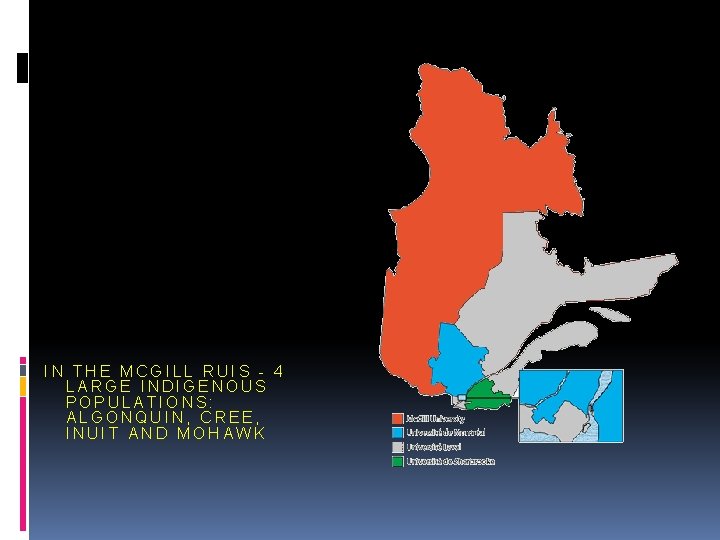
INDIGENOUS POPULATION IN CANADA - ESTIMATED 1. 4 MILLION (~4%) INDIGENOUS PEOPLE IN CANADA FIRST NATIONS, MÉTIS AND INUIT ACCOUNT FOR 60%, 33%, AND 4%, RESPECTIVELY. 3% MIXED BACKGROUNDS (STATS CAN) IN QUEBEC ~1. 8% ARE INDIGENOUS IN THE MCGILL RUIS - 4 LARGE INDIGENOUS POPULATIONS: ALGONQUIN, CREE, INUIT AND MOHAWK

Message from Indigenous Partners We need more Indigenous health care providers – not just doctors Our children lose interest in science/math at an early age Mature students interested in health careers need help and guidance getting back to school All health care professionals need to learn about Indigenous peoples

Realization We need a comprehensive program to address the lack of Indigenous health care providers, not just physicians We need to address cultural safety training for all future health care providers

A new program is born The Indigenous Health Professions Program (IHPP) Mc. Gill – Faculty of Medicine

Partners Mc. Gill partners CSD, Medicine, Nursing, PT/OT Dentistry, Nutrition and SW Indigenous partners within our region Algonquin, Cree, Inuit and Mohawk Current Mc. Gill students Indigenous and non-Indigenous

IHPP Objectives 1. CREATE A CENTRALIZED LOCATION FOR ALL MATTERS DEALING WITH INDIGENOUS PEOPLES’ HEALTH TRAINING AND TEACHING AT MCGILL 2. INCREASE THE NUMBER OF INDIGENOUS HEALTH CARE PROFESSIONAL STUDENTS AT MCGILL 3. INCREASE THE TOTAL NUMBER OF INDIGENOUS HEALTH CARE PROFESSIONALS IN QUEBEC/CANADA 4. STIMULATE THE CREATION OF INDIGENOUS CURRICULA AT ALL HEALTH PROFESSIONS SCHOOLS AT MCGILL 5. CREATE A WELCOMING ENVIRONMENT FOR INDIGENOUS STUDENTS IN THE HEALTH PROFESSIONS AT MCGILL

IHPP Program – Indigenous Student Education Trajectory Early Exposure Transitioning Applying Retention & completion Professional Development

Activities Outreach worker to visit communities, schools etc. Summer science camp – Eagle Spirit Science Futures Bridge programs with CEGEPS and Universities Pre-admission workshops


For current Indigenous students Welcoming Dinner Elder in residence Tutoring and mentoring programs Informal gatherings

Welcoming Dinner 2017

Future plans Plans to reach mature students Plans to introduce topics on Indigenous health at all the schools Establish trust with Indigenous partners

5 -10 YEAR VISION Long term Goals • At least 2% of graduates from health professional programs will be Indigenous • Indigenous health curriculum taught at all schools • Mc. Gill is seen as a leader in Quebec in training Indigenous health care professionals • Facilitate the hiring of more Indigenous staff

Beyond students How can we bring about positive change in our health care institutions?

Everyone working in health care is part of the solution! Reception Maintenance Porter Technicians Physician/Nurse Administrator

Truth and Reconciliation Commission Call to action #23 We call upon all levels of government to: Increase the number of Aboriginal professionals working in the health-care field ii. Ensure the retention of Aboriginal health-care providers in Aboriginal communities iii. Provide cultural competency training for all healthcare professionals i. Truth and Reconciliation Commission of Canada: Calls to action; 2015

Cultural safety

Cultural safety training Need to establish cultural safety training for all staff who have contact with patients Important for all cultures but the needs for Indigenous clients are unique Historical factors Social determinants of health Stereotypes

We are trying to avoid this tragedy

Conclusions We have a responsibility to actively recruit and train more Indigenous health care professionals We have a responsibility to train all future health care providers about the realities regarding the health of Indigenous peoples We must do better at educating current health care providers regarding cultural safety

Niá: wen Merci Thank you Questions?
- Slides: 34