Kawasaki Disease By Luke May What is Kawasaki

Kawasaki Disease By Luke May

What is Kawasaki disease? • Acute systemic vasculitis • Inflammation of arteries • Named for Dr. Tomisaku Kawasaki (19252020) • Japanese pediatrician who first described disease • Children <5 years old (usually) • Can have very serious cardiovascular effects • Potentially difficult diagnosis • Clear, effective treatment + good outcomes

Signs and Symptoms • Extreme immune response (inflammatory): o Fever- 5+ days, typically present o Rash- especially groin o Red/bloodshot eyes o Red/swollen hands and feet o Red/cracked lips and “strawberry” tongue o Swollen Lymph nodes o Variety of additional symptoms (diarrhea, cough, joint pain)
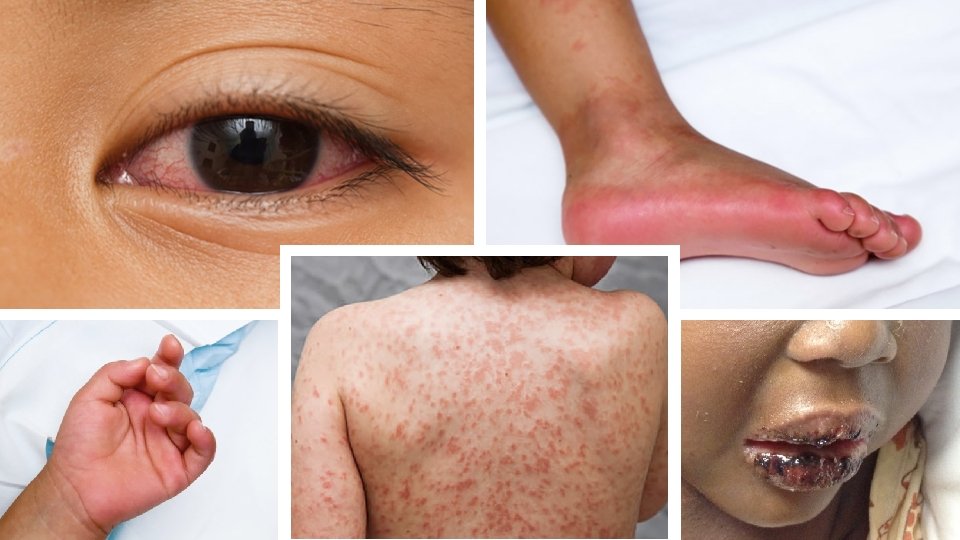

Cause • Unknown • Genetic Component? o Most prevalent in Asian/Pacific Islander populations • Environmental? o Peaks in January-March in U. S. o Unknown spore/bacteria?
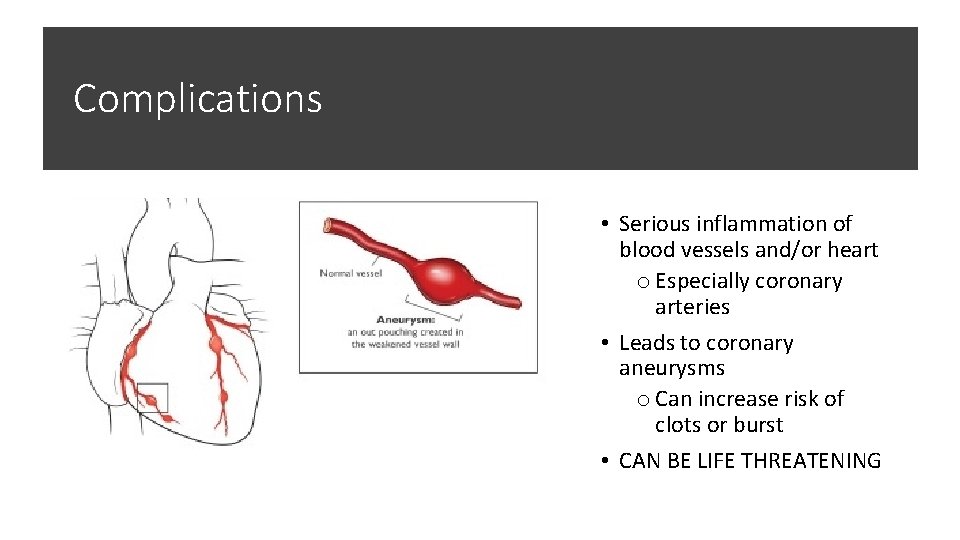
Complications • Serious inflammation of blood vessels and/or heart o Especially coronary arteries • Leads to coronary aneurysms o Can increase risk of clots or burst • CAN BE LIFE THREATENING

Typical Diagnosis • No specific, definitive test • Heavily relies on physical exam, clinical history, presenting signs/symptoms • Typical Tests • Blood, urine- check for inflammation/rule out other conditions • Echocardiogram- observes abnormal heart functions • Two types • Complete= fever + 4/5 symptoms (most common) • Incomplete= fever + 2 or 3/5 symptoms • Specialist referrals • Infectious disease, cardiology, rheumatology

Differential Diagnosis • May be difficult in practice • Not all core symptoms necessarily present (patients differ) • Can look like other inflammatory diseases • Pain, redness, swelling, heat • No specific test • Other Possible conditions: • Toxic shock syndrome • Stevens-Johnson syndrome • Streptococcal scarlet fever

Treatment • Optimally within first 10 days • Specific treatments: • Intravenous immunoglobulin (IVIG)typically one dose • Aspirin • Ongoing care: • Depends on severity • Low impact: • Infrequent risk assessment/counseling • High impact: • medications • physical activity restrictions • relatively frequent diagnostics/imaging
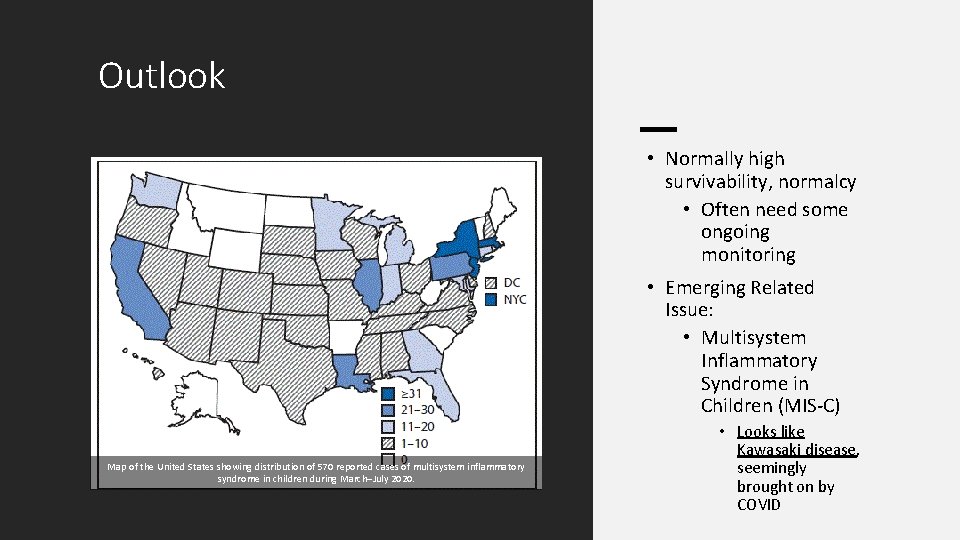
Outlook • Normally high survivability, normalcy • Often need some ongoing monitoring • Emerging Related Issue: • Multisystem Inflammatory Syndrome in Children (MIS-C) Map of the United States showing distribution of 570 reported cases of multisystem inflammatory syndrome in children during March–July 2020. • Looks like Kawasaki disease, seemingly brought on by COVID

• American Academy of Pediatrics. (2020, May 13). Kawasaki disease in infants & young children. Healthychildren. org. https: //www. healthychildren. org/English/healthissues/conditions/heart/Pages/Kawasaki-Disease. aspx References (APA) • Bacher, Renée. (June 18, 2020). Tomisaku Kawasaki, pediatrician who discovered disease that bears his name, dies at 95. The Rheumatologist. https: //www. the-rheumatologist. org/article/tomisaku-kawasakipediatrician-who-discovered-disease-that-bears-his-name-dies-at-95/ • Godfred-Cato S, Bryant B, Leung J, et al. (2020, August 14). COVID-19– Associated Multisystem Inflammatory Syndrome in Children — United States, March–July 2020. MMWR Morbidity and Mortality Weekly Report. 69(32): 1074– 1080. DOI: http: //dx. doi. org/10. 15585/mmwr. mm 6932 e 2 • Mayo Clinic. (2020, June 11). Kawasaki disease. https: //www. mayoclinic. org/diseases-conditions/kawasakidisease/symptoms-causes/syc-20354598 • Saguil, A. , Fargo, M. V. , & Grogan, S. P. (2015). Diagnosis and Management of Kawasaki Disease. American Family Physician, 91(6), 365 -371. http: //ezaccess. libraries. psu. edu/login? url=https: //wwwproquestcom. ezaccess. libraries. psu. edu/docview/2454242692? accountid=13158
- Slides: 11