Karen You are assigned to work in labor


Karen You are assigned to work in labor and delivery today and are very excited. When you arrive at 7 am, the night shift nurse gives you a hand off. You will be taking care of Karen, a 26 yrold woman who arrived 15 minutes ago in early labor. She is currently in the bathroom, putting on her gown and leaving a urine specimen.

Karen Her history is as follows: She is 38 weeks gestation. Her antepartum course was complicated socially. Her husband was abusive and there is a court ordered certificate of protection, so he cannot visit her. Karen’s mother is with her and is very supportive.


Karen’s uterine contractions are mild , 30 -40 seconds every 5 -7 minutes. They started 5 hours ago and she called her primary care practitioner(PCP) who told her to come the hospital to get checked.

Karen has a birth plan that outlines what she would prefer during this experience. The nurse knows that a birth plan is a A. Legally binding document between the pt and the nurse. B. Contract that is voluntary between the pt and the nurse. C. Wish list that is abided by if possible between the pt and the nurse. D. Method of communication between the pt and the nurse.

Karen is in bed when you enter the room and her mother is in the chair. You introduce yourself and you can see Karen is very anxious. She is holding tight to the side rails. You quietly put your hand on her abdomen and wait for the next contraction.

The best nursing diagnosis for Karen in the latent phase is: A. Impaired mobility r/t labor as evidenced by voluntary bed rest. B. Low situational self esteem r/t domestic abuse evidenced by anxiety. C. Anxiety related to impending delivery as evidenced by a tight grip on the handrails. D. Powerlessness related to labor as evidenced by a tight grip on the handrails.

Karen seems to relax with your therapeutic touch. You explain to her that you are going to do a quick assessment and then you will take her history. First, you take her vital signs which are in normal limits.

Karen Ordering: Place the next assessment in priority order: _______ Perform a sterile vaginal exam (SVE) _______ Place her in lithotomy position _______Use litmus paper to check for rupture membranes _______Check fetal heart tones (FHT) _______Don sterile gloves _______Drape pt. _______Lubricate gloves

Karen is placed on a external monitor and is 2 cms dilated, 0 station and is 50% effaced. Her UCs are recording at 4 -7 minutes’ frequency lasting 30 -50 seconds. Litmus paper is negative for ruptured bag of waters.

What would be an appropriate intervention at this stage of labor? • • A. Teach patterned breathing? B. Offer her pain medication. C. Encourage her to get out of bed and walk. D. Apply sacral pressure.

Karen You explain to Karen and her mother that you are going to take her assessment history. The night nurse had already noted the date and time that Karen arrived. Next you ask her about her obstetrical history. She has been pregnant a total of 4 times. One pregnancy ended in a spontaneous abortion, another in an induced abortion, a third pg was premature twins who did not survive at 22 weeks.

Karen is considered a : G___ P___ T___ A___ L___

Karen You take Karen’s height and weight and ask her about her allergies. Karen tells you she is allergic to Penicillin and her mother confirms this. Karen relates that when she was younger she was given penicillin and broke out into urticaria all over.

Patients that are allergic to Penicillin should be given what category of antibiotics with caution? • • A. Cephalosporins B. Lincosamides C. Glycopeptides D. Aminoglycosides

Karen Next you ask Karen about the onset of labor. She states that it started approximately 5 hours ago but the UCs have become more regular in the past two hours. She had a small bloody show this morning and lost her mucous plug yesterday. Her prenatal records reveal that she is rubella immune and A+ blood type.

Karen denies use of alcohol but admits to smoking a half pack a day of cigarettes each day. You perform a head to toe assessment on Karen rates her pain as a 3 -4/10 pain scale with contractions.

Karen Social history indicates that Karen lives with her mother and will collect child support from her husband. She has not seen him in a month but is afraid that he will find out she is in the hospital and will try to come and see the baby.

A prudent step for the nurse to take in this situation is to: A. Call the local police and inform them of the situation. B. Call the nursery and tell them the situation so they can lock the doors. C. Let the hospital security know the situation. D. Lock the pt’s hospital door to prevent the husband from entering.

Karen While Karen is walking around you have a chance to review her prenatal records and found out she has Group B streptococcus +, (GBS+) so the next time she is due for her intermittent fetal monitoring strips to be run on the external monitor, you will tell her the treatment plan.

Karen Complications from an untreated GBS include: A. Endometriosis B. Mastitis C. Neonatal neurological syndrome D. Neonatal sepsis
Karen While you are explaining the treatment, you run a strip that looks like the following.

Karen How far apart are the contractions? ______________ You prepare to start an IV so that you can administer the antibiotics.

Karen The order the PCP reads: 1000 ml of D 5 W 1/2 NS at 130 ml/hr. The gtt factor is 15 gtts/ml. At how many gtts/min should you administer the IV? _________________

Karen In anticipation that a pt may need blood or blood by-products, what size angio catheter should you start the IV? A. 24 gauge 1 inch B. 22 -gauge 1. 5 inch C. 20 gauge 1 inch D. 18 gauge 1. 5 inch

Karen The antibiotic order is Clindamycin hydrochloride (Cleocin) 300 -mg IVPB (IV piggyback) in 50 ml of RL to run for 30 min. The nurse hangs the IVPB above the primary IV bag and regulates the gtts /min. At what level should the nurse set the gtts/min?

Karen After the IVPB is infused you assess Karen’s vital signs (VS) and the fetal heart rate (FHT) and encourage her to get OOB and walk. After 30 minutes of walking in the hall you hear Karen’s mother call you. Karen has spontaneously ruptured membranes and you escort her back to bed. The FHR is WNL, but the fluid discharge from Karen’s vagina is moderately meconium stained. She is now 4 -5 cms dilated and is getting very uncomfortable.

Karen The PCP had arrived and you explain to Karen and her mother that she is going to have to be confined to her bed now and that her membranes have ruptured and the fluid is green. The PCP puts in an intrauterine pressure catheter (IUPC) with a double lumen and an internal electrode.

The intrauterine pressure device is a device that assists with meconium stained amniotic fluid by: A. Installing cold fluid to dilute the meconium B. Extracting the meconium with mild suction C. Instilling warm fluid to dilute the meconium D. Extracting the fluid so the meconium solidifies. Fetal meconium is a sign of distress or post dates

Karen Meconium occurs because the fetus: A. Has weak abdominal muscles. B. Bears down in an attempt to move C. Releases adrenaline D. Does not release cortisol.

Karen After the amniotic infusion is started Karen gets increasingly more uncomfortable. The sterile vaginal exam reveals she is 6 cms dilated. What stage and phase of labor is Karen in? A. B. C. D. Stage 1: Phase 1 Stage 1: Phase 2 Stage 1: Phase 3 Stage 2

Karen What does the nurse expect Karen’s affect to be like at this point? A. Talkative B. Self-absorbed C. Irritable D. Content

Karen You discuss with Karen and her mother pain relief options, which include opioids such as butorphanol (Stadol), regional anesthesia (epidural), or breathing and relaxation techniques. Karen chooses to have an epidural so you notify the nurse anesthetist.

Karen Ordering: Place in order interventions to ready the pt for an epidural. ______Explain the procedure to the pt. ______Infuse a bolus dose of 1000 m. L of IV Fluid. ______Have the anesthesiologist obtain consent. ______Position in a spinal curved position. ______Coach through the procedure. ______Reposition without disrupting the catheter

Karen After the epidural you reposition the patient in bed. The best position for the client post epidural or spinal anesthesia is: A. Sitting up B. Lying flat C. Lying on side D. Semi Fowlers

Karen Select the common side effects of epidural anesthesia. A. High Blood Pressure B. Bladder distention C. Increased uterine contractibility D. Headaches E. Site infection

Karen Following the epidural the contractions began to slow down… 4 -7 min. a part. Since Karen’s contractions have slowed down, the PCP has decided to AUGMENT labor with oxytocin (Pitocin)

Karen The order reads to start pitocin at 2 m. U/min IVPB. The pitocin comes from the Pharmacy premixed (30 U in 500 ml bag) For how many ml/hr should you set the pump for? ___________________
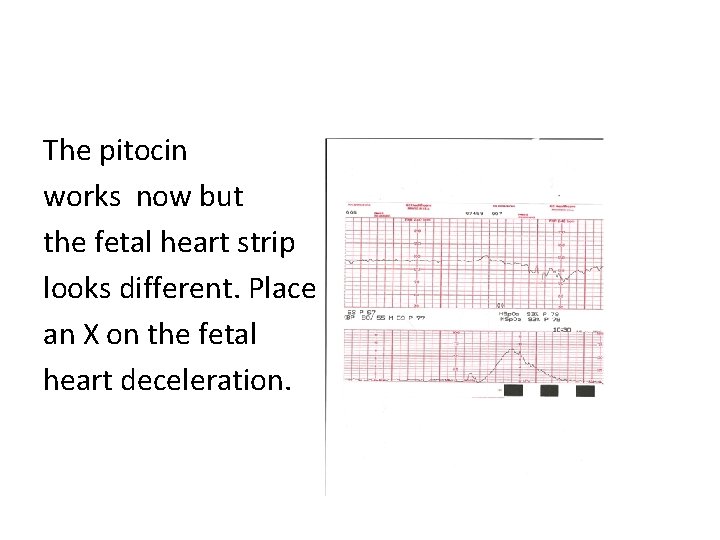
The pitocin works now but the fetal heart strip looks different. Place an X on the fetal heart deceleration.

Karen What type of deceleration is on the fetal monitor on last slide? A. Early B. Late C. Variable D. Sinusoidal

Karen Due to the deceleration noted on the fetal monitor, what should the nurse do first? A. Call the PCP. B. Stop the pitocin. C. Turn the pt. D. Give the pt oxygen.

Karen Once the deceleration is corrected, a sterile vaginal exam (SVE) is done and Karen is now fully dilated and 100% effaced.

What interventions should the nurse complete to get the pt who has an epidural anesthesia ready to push during the second stage of labor? (Check all that apply) Have her pant. A. Place her in lithotomy position. B. Check her bladder and catheterize if needed. C. Provide clean Pads under her perineum. D. Encourage her to verbalize her feeling. E. Get neonatal bed warmed and ready. F. Ask her mother to leave.

Karen does well pushing three times with each contraction. She is making slight progress with each contraction. The epidural drip is turned down by the nurse anesthetist so Karen can feel more the urge to push. After approximately 2 hours of pushing the fetal head is crowning. You call the PCP to come and you begin to prep Karen’s perineum front to back and set up the delivery instruments.

Karen What type of precautions are used in a delivery room? A. Standard B. Isolation C. Droplet D. Blood and body fluid

Karen The PCP holds her hand over the perineum and applies counter-pressure to prevent tearing. This maneuver is called ____________

Karen After three more pushes the fetal head is delivered over an intact perineum. You stop Karen from pushing and tell her to pant so the infant’s mouth can be suctioned out, and nose can be cleared and the PCP checks for nuchal cord.

Karen A nuchal cord is one that: A. Has a true knot. B. Is around the fetal head. C. Has a false knot. D. Is around the fetal shoulder

Karen Next the PCP applies downward pressure to assist the delivery of the anterior shoulder. After the anterior shoulder is the posterior shoulder slides out as does the entire body and legs of the infant. The PCP clamps the cord and Karen’s mom cuts the cord. The baby is placed on Karen’s abdomen and she immediately reaches for infant. The infant is a boy!

Karen The priority for the nurse once the infant’s airway is clear should be to : A. Promote bonding B. Conduct a physical exam C. Identify the infant and mother D. Prevent cold stress.

Karen The nurse places the infant on the warmed bed and assess him. He is acrocyanotic, his HR is 160, RR is 64 and he is flexed and pulls away from the nurses touch. She assigns him a one minute Apgar of_____

Karen After you take the vital signs, you do a quick physical assessment to make sure it is safe to keep the infant with Karen for a period of bonding. You weigh him and he is 5 pounds and 14 ounces and 19 inches long. While you are giving the infant his vitamin K and placing ID bands on him, the PCP is waiting for the last stage of labor to complete.

Karen The last stage of labor (stage 3) is from: A. The time the infant is crowning to the time of birth of the placenta. B. The time the infant is at 0 station to the time of the birth of the placenta. C. The time the infant’s cord is cut to the time of the birth of the placenta. D. The time the infant is fully delivered to the time the birth of the placenta.

Karen The four signs of placental separation are: (choose all that apply. ) A. The uterus becomes globular in shape. B. The uterus clamps down on the abdomen. C. The uterus rises in the abdomen. D. The umbilical cord lengthens. E. The cervix dilates to 4 cms F. There is a gush of blood.

Karen The nurse asked to adjust the Oxytocin (pitocin) to a post partum dose and shuts off the epidural drip. You increase the oxytocin (pitocin) to 100 m. U/min. (remember there is 30 U in 500 m. L bag) At how many m. L/hr will you set the pump? __________ml/hr

Put an X on the two spots where you should place Your hands to check the fundus after delivery.

Karen The infant is doubled wrapped with a stockinet on his head and is given to Karen to begin to breast feed which was the request from the birth plan.

Karen At 38 weeks gestation, Karen’s infant is only 5 pounds and 14 ounces. Name two risk factors from Karen’s history that may have contributed to a smaller infant. 1. _____ 2. _____
Karen
- Slides: 60