Justification and benefit of adjuvant therapy in IVFICSI

Justification and benefit of adjuvant therapy in IVF/ICSI Prof. dr. sc. Miro Kasum Klinika za ženske bolesti i porode Petrova 13, Zagreb

Factors l Fetal – – Assisted hatching Preimplantation genetic screening l Maternal – – l Other methods – – Acupuncture Endometrial biopsy – – Aspirin Glucocorticoids Growth hormone Dehydroepiandrosterone Sildenafil Heparin Immnoglobulin Antibiotics

Assisted hatching (AH) l l l Before an embryo implants into the uterus it must hatch from the zona pellucida Definition: Artificial disruption (thinning) or making a small hole in the zona pellucida – Easier for hatching to occur Methods – Chemical – Mechanical – Laser
Indications and success rates l l l Older women > 37 years Poor embryo quality Thick zona pellucida Repeated failed IVF cycles – 3 or more ET without pregnancy > FSH levels l No evidence to recommend or determine any effect of AH on LBR l l Seif MM, Cochrane Database Syst Rev 2006 Improvement in CPR with AH means that a clinic with a success rate of 25% could anticipate improving the CPR to between 29% and 49% – Das S, Cochrane Database Syst Rev 2009
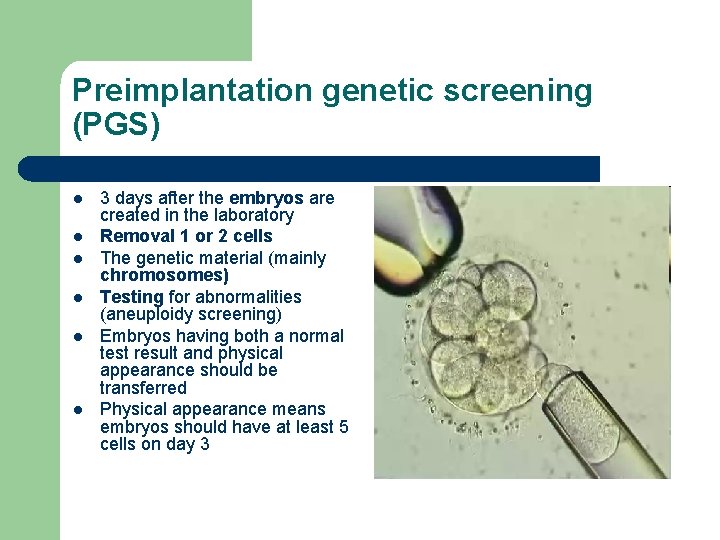
Preimplantation genetic screening (PGS) l l l 3 days after the embryos are created in the laboratory Removal 1 or 2 cells The genetic material (mainly chromosomes) Testing for abnormalities (aneuploidy screening) Embryos having both a normal test result and physical appearance should be transferred Physical appearance means embryos should have at least 5 cells on day 3

Indications and effectiveness l l A family history of genetic disorders Repeated unexplained miscarriages Advanced maternal age – > 35 years l l No evidence of a beneficial effect of PGS as currently applied on the LBR after IVF, but, for women of advanced maternal age PGS significantly lowers the LBR Technical drawbacks and chromosomal mosaicism underlie this inefficacy of PGS New approaches in the application of PGS should be evaluated carefully before their introduction into clinical practice l Mastenbroek S, HRU, 2011

Maternal factors and other methods l l l l Aspirin Glucocorticoids Growth hormone(GH) Dehydroepiadrosterone (DHEAS) Sildenafil Heparin Intravenous immunoglobulin (IVIg) Antibiotics l l Acupuncture Endometrial biopsy

Aspirin l Properties: – – l Arachidonic acid < Cyclooxigenase < Prostacyclin (PGI 2) << Thromboxane A 2 (TXA 2) Effects: – – – Vasodilatatory Anti-inflammatory Platelet aggregation inhibition

Aspirin following ET l l Aspirin 75 mg – Alternate days from the day of ETuntil 18 days after retrieval Evaluation: – Ovarian blood flow – Folliculogenesis – Ovarian responsiveness – Uterine vascularity and receptiveness l RCT of 1380 women – LBR l l 27% (with aspirin) 23% (without aspirin) – l Waldenstroem U, FS 2004 Low-dose aspirin does not improve IVF outcome and it cannot be recommended for routine clinical use – Revelli A, FS 2008; Duvan CL, JARG 2006; Fratarelli JL, FS 2008; Gelbaya TA, HRU 2007

Glucocorticoids l Immunomodulators – > Intra uterine environment – > Implantation rate – < NK cells < Cytokines < Endometrial inflammation – – Boomsma CM, Cochrane Database Syst Rev 2007 – Tetsuka M, JCEM 1997 – Miell JP, JE 1993 – l l > Ovarian response to gonadotrophins Dexametasone – – – => enzyme 11 -beta hydroxysteroid dehxdrogenase type 1 => Directly influence follicular development => Indirectly by increasing serum GH, IGF-1, and consequently follicular fluid IGF-1 levels

Glucocorticoids and success rates l l 1 mg dexamethone 10 mg prednisolone l > Implantation rate – l > Pregnancy rate – l 16. 3 vs. 11. 6% (NS) 26. 9 vs. 17. 2% (NS) < Cancellation rate – 2, 8 vs. 12, 4% (SS) – Keay SD, HR 2001 l > Pregnancy rate – Borderline (SS) – Boomsma CM, Cochrane Database Syst Rev 2007

Growth hormone (GH) l l > Intraovarian IGF-I Addition of IGF-I to gonadotrophins – l > Gonadotrophin action in granulosa cells in poor responders – – l Demonstration in animal and human studies Augmentation of the activity of aromatase Increase of E 2 -17 beta, P 4, LH-r Augmentation of follicular development Increase of oocyte maturation Hypothesis for the introduction of GH to enhance ovarian steroidogenesis and follicular develpoment and the ovarian response acting sinergistically with FSH – Yoshimura Y, BR 1996, Suikarri AM, FS 1996

GH during ovulation induction l l Mostly studied poor responders 4 -12 IU of GH – l sc l > Retrieved oocytes – l Starting on the day of ovarian stimulation with gonadotrophins 7. 5 vs. 3. 5 (p< 0. 001) > PR – 60% l l No significant differences – l Ibrahim ZH, FS 1991 Number of follicles and oocytes, gonadotrophin dose, cancellation, PR No support for the use of GH as adjuvant th l Suikkari AM, FS 1996, Shaker A, FS 1992, Kotarba D, Cochrane Library , 2002

Dehydroepiandrosterone (DHEAS) l l l Primarily adrenocortical reticularis zone origin In high amounts during reproductive life Progressive decline with age Speculation that HRT in the elderly may have ageretardant effects Essential sustrate for steroidogenesis – – < DHEAS => < testosterone, < E 2 -17 beta > DHEAS (oral supplementation) => > IGF-I l Orentreich N, JCEM 1984, Mc. Natty KP, S 1979, Casson PR, HR, 2000

DHEAS before ovulation induction l Mostly studied – – l l l Women with diminished ovarian reserve Repeated IVF failures Oral supplementation 75 mg daily 2 – 4 months before ovulation induction with gonadotrophins l > E 2 -17 beta l l > IGF-I l l l Particularly 35 -40 years l l Trott E, FS, 1996 > CPR < Dose of gonadotrophins – l Casson PR, E, 1998 > Outcome in CC resistency l l Casson PR, HR 2000 Barad D, HR 2006 May augment ovulation induction Beneficially affect oocyte and embryo quality and PR

Sildenafil l A potent c. GMP-specific phosphobodies-terase 5 inhibitor – Its selective inhibition of c. GMP catabolism in cavernous smooth muscle tissue augments penile erection l – Fagelman E, U, 2001 Vaginal sildenefil improves uterine artey blood flow and sonographic endometrial appearence l Sher G, HR 2000

Sildenafil during ovarian stimulation l l 7 days of sildeneafil – > Uterine artery blood flow The combination of sildenafil and estradiol valarate – >Uterine artery blood flow – > Endometrial thickeness l Sher G, HR 2000 Vaginal route for 3 to 10 days – > 2 previous > IVF failures l > PR (SS) – < Endometrial thickness l > 9 mm – Sher G, FS 2002 Promising studies * l l The addition of silldenefil to an estrogen supplemented regimen Previously failed to achieve an endometrial thickness greater than 8 mm – – No increase in endometrial thickness No increase in blood flow l l Check JH, HR 2000 Sildenefil has not demostrated a definitive role

Heparin l Treatment of choice – l l Recurrent pregnancy loss due to a. PL antibodies Heparins are involved in activities anticoagulation and adhesion of the blastocyst to the endometrial epithelium and subsequent invasion a. PL may be responsible – – < Phospholipid adhesion molecules of trophoblast < h. CG release < Trophoblast invasiveness < Trophoblast differentiation in vitro l Fiedler K, EJMR 2004, Di Sormone N, AR 2000
Heparin and success rates l Assumption – – l l < Immunological status < Embryo implantation at least one a. PL Heparin 5000 IU, Aspirin 100 mg daily NO significant difference in PR those treated and those receiving placebo – Quenby S, FS 2005, Stern C, FS 2003 Seropositive women – – Seropositive women in IVF – l l > 3 IVF failures at least 1 thrombophilic defect Enoxaparin (Low molecular weight heparin), 40 mg daily > CR, > PR, > LBR/ placebo l l l 20, 9% vs. 6, 1% 31% vs. 9, 6% 23, 8% vs. 2, 8% l Qublasn H, HF 2008

Immunoglobulin (Ig. G) l l Indications – > Embryo failure – > Recurrent miscarriage l > Inappropriate immune response l > Proinflammatory cytokines Preparations of Ig. G contain – All humoral Ig. G antibodies – Normally in the plasma of blood donors l Effects of Ig. G: – – l < Proinflammatory citokynes > Antinflammatory cytokines < NK cells < Pathological antibodies Dose: – 500 mg iv / kg before ET l l Carp HJ, CRAI 2005 Coulam CB, EP 2000

Ig. G before ET l No improve in PR l l Stephenson MD, FS 2000 > LBR (SS), meta analysis, 3 RCT l l > PR (56% vs. 9%) l l l No benefit l Balasch J, FS 1996 Clark DA, JARG 2006 Coulam CB, EP 2000 > Outcomes in specific group of IVF patients with positive APA l Sher G, AJRI 1996

Antibiotics l Vaginal antisepsis, negative effect – l Bacterial vaginosis, negative effect – – – l l < Quality of the oocytes and the embryos < H 2 O 2 producing lactobacilli < CR > EPL Bacterial contamination of the ET catheter tip Significant negative effect – – – < CR < ZP > Endometritis l > Cytokines, > Macrophages, > Prostaglandins, > Leukocytes l Salim R, HR 2002; Spandorfer S, JRM 2001; Moore DE, FS 2001

Controversial role of antibiotics l l Ceftriaxone + metronidazole At oocyte recovery – – Reduction of bacteria on the transfer catheter clip (78, 4%) > CR l – l l 41, 3% vs. 18, 7% – Egbase PE, Lancet 1999 Amoxycillin + clavulanic acid 1 g/1, 25, RCT At oocyte recovery + 6 days > Pregnancy loss rate – l 21, 6 % vs. 9, 3% > CPR l l l 33, 3% vs. 20, 8% (p=9, 15) Not recommend this antibiotic prescription * Ensure maximum catheter sterility * l Peikrishvili R, JGOBR 2004
Acupuncture l l l Used in China for centuries to regulate the female reproductive system Recent popularity in the western world 3 potential mechanisms – – – > Neurotransmiters, Gn. RH, FSH, E 2, “O” > Uterine blood flow < Endogenous opioids l Cho ZS, PNAC 1998

Beneficial effects of acupuncture l Timing of administration: – – – During ovarian stimulation At oocyte recovery At ET and afterward l l A number of systemic reviews and meta-analysis have been conducted on its efectiveness as an adjuvant treatment Ng EH, BJOG 2008 > CPR, > LBR l l l Manheimer E, BMJ 2008 > PR – l l > CPR, > LBR El-Toukhy T, BJOG 2008 > LBR Placebo effect and small sample size cannot be excluded * Not recommended as a routine use procedure * l Cheong YC, Cochrane database Syst Rev 2008
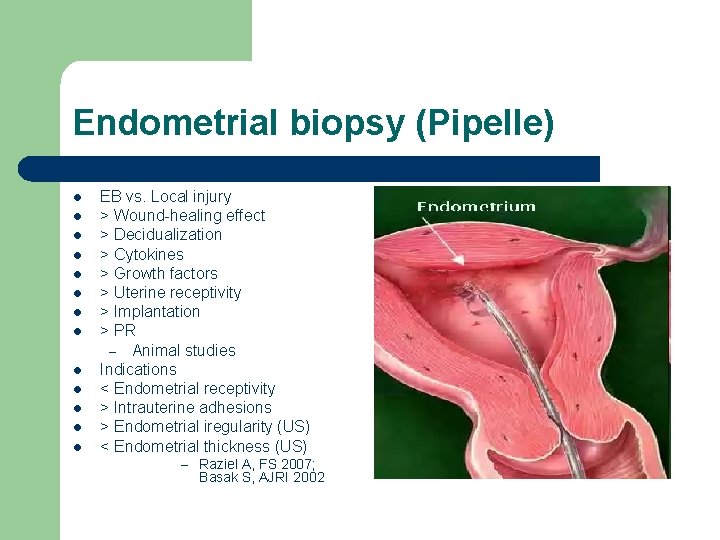
Endometrial biopsy (Pipelle) l l l l EB vs. Local injury > Wound-healing effect > Decidualization > Cytokines > Growth factors > Uterine receptivity > Implantation > PR – Animal studies Indications < Endometrial receptivity > Intrauterine adhesions > Endometrial iregularity (US) < Endometrial thickness (US) – Raziel A, FS 2007; Basak S, AJRI 2002

Benefits of scratching (EB) l l On days 10 -13 and 20 -24 of previous cycle > genes encoding membrane proteins important during implantation – Kalma Y, FS 2009 l l l > CR – 27, 7% vs. 14, 2% > CPR – 66, 7% vs. 30. 3% > LBR – 48, 9% vs. 22. 5% – Barash A, FS 2003 l > CR following excision of polyp or thickened endometrium – Li R, FS 2008 l > CR, > CPR, > LBR – Zhou L FS 2008 l l l Results are promising Prospective controlled studies are still needed to confirme the procedure Validitation in a large randomized study may lead to the routine performance of EB in conjuction with IVF

Conclusions l l l The expense, time, stres and frustration felt by physicians and 15% of couples with difficulties in conceiving are searcing for new drugs and tecnologies that will increase succes rates However, progress has been limited because none of the available adjuvant treatments has a clear advantage If the embryos are genetically abnormal, no maternal adjuvant therapy will improve the pregnancy rate l l l Some of therapies may prove efficacious in subgroups of patients Treatment often needs to be “tailor -made” to suit the individual patient Low molecular weight heparine may be effective against antiphospholipid antibodies, other than LE and ACA EB may benefit patients with thin and nonresponsive endometrium Ig may benefit patients with high NK cell numbers, or enhanced killing activity
- Slides: 28