July 2012 Webinar PDSA Sharing Month 1 Reporting

July 2012 Webinar • PDSA Sharing • Month 1 Reporting • CCI Practice: Byrnes Family Medicine

Testing on a Small Scale • Conduct the test with one provider in the office, or with one patient • Conduct the test over a short time period • Test the change with the members of the team that helped develop the plan • Test the change on a small group of volunteers • Minimize confusion, frustration until bugs are worked out, then spread

PDSA Sharing • Pre-visit planning: Eastbrook, Oyster Point, Green Hill • Use of diabetes template: Seneca • Population alerts: Warren, Corry, General Internal Medicine • Outreach for overdue patients: Manor, Mountville • Data capture/reporting: Hamilton Health • Patient education/Self management support: Oil Valley, Hamilton Health • Complication screening (feet, eyes, kidneys): Carlisle, Sandrowicz, Oyster Point

Super Strategies • Staff education/training • Staff meetings • Standing orders • Process auditing • Small, rapid PDSA cycles

PDSA Assistance, Reporting • Talk with your practice facilitator about your PDSAs – they are there to help you! • South Central – Sharon Adams 814 -344 -2222, sadams@scpa-ahec. org • North West – Patty Stubber 814 -217 -6029, pstubber@nwpaahec. org • Please fill out your entire PDSA worksheet, including what you’re learning (not just what you plan to do). • Submit your PDSA worksheets ongoing or with your monthly reports.
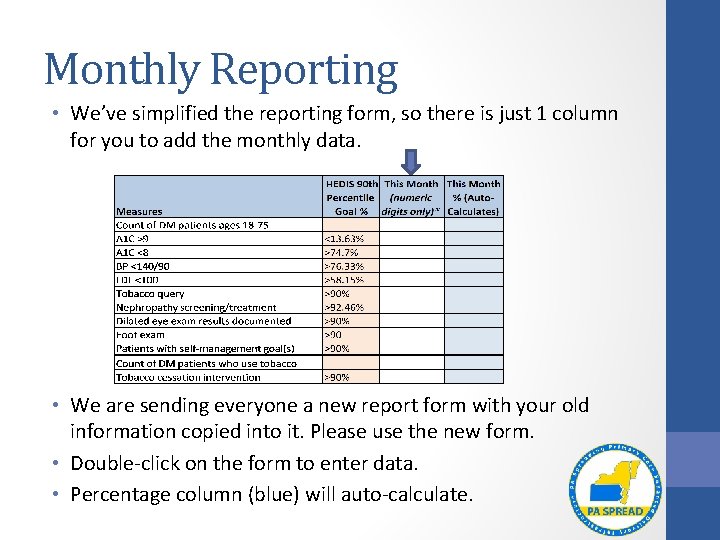

Monthly Reporting • We’ve simplified the reporting form, so there is just 1 column for you to add the monthly data. • We are sending everyone a new report form with your old information copied into it. Please use the new form. • Double-click on the form to enter data. • Percentage column (blue) will auto-calculate.
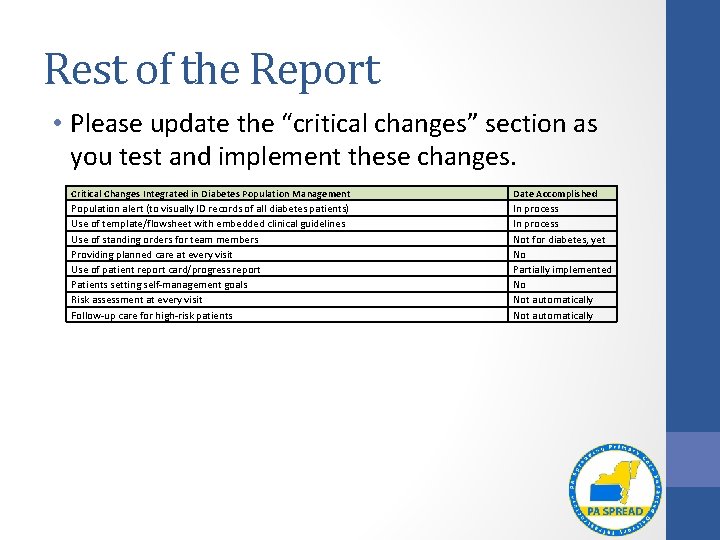

Rest of the Report • Please update the “critical changes” section as you test and implement these changes. Critical Changes Integrated in Diabetes Population Management Population alert (to visually ID records of all diabetes patients) Use of template/flowsheet with embedded clinical guidelines Use of standing orders for team members Providing planned care at every visit Use of patient report card/progress report Patients setting self-management goals Risk assessment at every visit Follow-up care for high-risk patients Date Accomplished In process Not for diabetes, yet No Partially implemented No Not automatically

Improvement Plan for Measures Not at Goal (keep typing in the boxes below to add lines as needed) Month Your PDSAs (what you planned, what you did, what you learned, how you refined or implemented) June 2012 We are working on the identification of all DM patients within the electronic record. Once this has been completed we will be meeting with providers and staff to educate them as to this ID. Since we have a flow chart already in place and a process in place to be prepared for the DM visit we will be measuring the compliance with a PDSA on the identification of the DM patient with a single provider and assistant. Improvement Plan for Measures Not at Goal (keep typing in the boxes below to add lines as needed) Month Your PDSAs (what you planned, what you did, what you learned, how you refined or implemented) June 2012 Created laminated list of measures, working off overdue and increased A 1 C list and calling and scheduling labs and appointments. Seeing patients 1 on 1 with A 1 C>15, now down to 10. 1 with diabetic educator. Staff/nursing meeting scheduled to discuss diabetic measures. In 2 weeks we will have staff meeting with doctors and team members to formulate additional plans. Staff seminar for nurses to discuss diabetic measures. Meeting with physician champion to discuss PDSA. Nurse will focus on calling patients 2 weeks out and gather data-observe for completed measures. PDSA worked with are physician schedules. Tracked two working days of their schedule. Put in orders, gave alerts. Measures met at 80% as this physician is very proactive in his approach to diabetes. Improvement Plan for Measures Not at Goal (keep typing in the boxes below to add lines as needed) Month Your PDSAs (what you planned, what you did, what you learned, how you refined or implemented) 1. June 2012 2. PDSA Cycle One – Creating Panel for Dr. A. William, and discovered that we can run reports on additional providers using two visit criteria. Registration is entering PCP and Doctor of Record as patients come in for visits. PDSA Cycle – Data Integrity and improving ability to create reports Lab data such as Hgb. A 1 c and LDL are readily available for review. Podiatry referrals are readily pulled for reports using Dr. Black as primary podiatrist. Ophthalmology referral data needs to be refined. Initially the report was created using Premier Eye Group as our primary indicator for eye consults. However, discovered after chart review, providers are using Ophthalmology consults as well Premier Eye Group. The report was refreshed and captured eye referrals using Dr. A. William’s panel. Another problem related to referrals – HHC has started a new referral process using the EMR. The referral consults will be marked completed once the actual reports are scanned into the EMR by HIS. Our referral numbers may be low until this process is perfected and all reports have arrived. Plan to monitor Unit Clerks using the Order Tracking Tab in the EMR. For the referrals without a completion date, the Unit Clerks are to call the patients to inquire if appointment was kept and the report needs to be sent from the referral office or if the patient requires rescheduling, Data Analyst reviewing ability to create reports for self- management goals. Clinical staff not using the Diabetic Goal Template consistently. Self- Management requires further investigation and planning for documentation of self- management goals. Assessment of smoking status is readily available and Medical Assistants assesses and documents upon rooming of patient. Assessment of Smoking intervention requires consensus on which areas of documentation to be PDSA Summary • It’s helpful to have a summary of the PDSAs you’ve been testing in the last part of the report.

Comments at the End • Feel free to add comments or questions at the end of the report. (Please date them. ) • Challenges you are facing. • Areas where you need support or resources. • Things you want to learn more about. Example: July 2012 1. Discussion concerning Self -Management goals and innovative ways to incorporate group visits. 2. Data integrity and creating reports remains a challenge for a number of measures but we are improving the quality of the reports.

Patient Centered Medical Home Building the System Mary Beth Byrnes, MSN, RN PA SPREAD PCMH Initiative July 26, 2012

Richard Byrnes, D. O. Family Practice n n n n Established 1974 Serving Upper Bucks & Montgomery Counties Suburban – Semi-Rural Patient Population 2100 97% English Speaking Caucasian Farming – Light Industry 7. 2% Community Unemployment Rate Staff – 1 RN (CNS), 2 MA, 1 CRNP (temporary)

PACCI – 2010 Why Participate in Initiative n n n Expert Guidance Challenge Financial q q q n No Cost Meaningful Use IBC – Incentive Payment Better Patient Outcomes
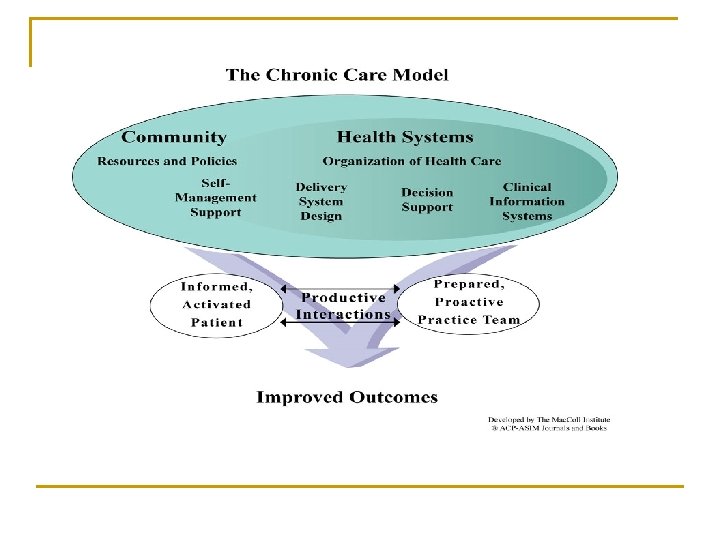

Decision Support n n n Clinical Guidelines Imbedded in EMR & Registry Stepped Care Protocol – Medications Standing Orders – Team Members q n n Risk Stratification – Identify highest risk patients Created a Care Management Process q q n Patient Centered Communication Proven Education Methods – Barrier to Care/Confidence Patient Support & Report Cards q n Labs, Eye Exam, Diabetic Education, Influenza & Pneumococcal Vaccinations, Mammograms, Colonoscopy Sharing Guidelines – Outcomes with Patients Patient Education Material & Resources

Delivery System Design n Planned Care at Every Visit q PDSA’s n n n q How to implement elements from Decision Support Written Policy for PDSA’s Implemented Job Descriptions related to the new policy Developed a Strategy n Mapped Office Visits

Delivery System Design Planned Care at Every Visit n n Formed Team & Identified Roles & Responsibilities Evaluated Method of Communication q n Self Management q q q n Report Card & Self Management Goals Readiness & Confidence Rulers Action Plan System to Identify & Document High Risk Patients q n Motivational Interviewing Techniques Develop Care Plan for Highest Risk Patients Huddles, Tag Team, Warm Hand Off
Delivery System Design Redefined Roles & Work Flows n Put more responsibility on staff q How to Read Charts n q n Removed any “Crutch” which blocked change Redefined Flow of Patient Visit - Mapping q q Team Effort Team Member Responsibilities n n n Written Policy Updated Job Descriptions Focused on Patient Education q n Tracking Tag Team Written Policy Based on Successful PDSA’s
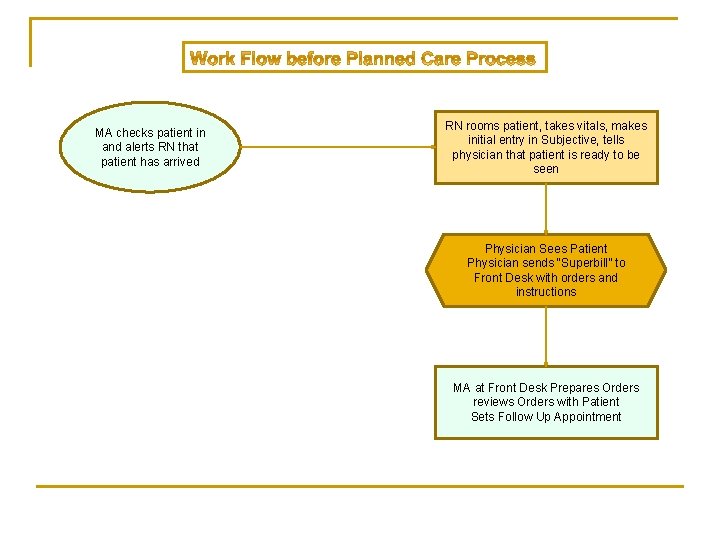
MA checks patient in and alerts RN that patient has arrived RN rooms patient, takes vitals, makes initial entry in Subjective, tells physician that patient is ready to be seen Physician Sees Patient Physician sends “Superbill” to Front Desk with orders and instructions MA at Front Desk Prepares Orders reviews Orders with Patient Sets Follow Up Appointment
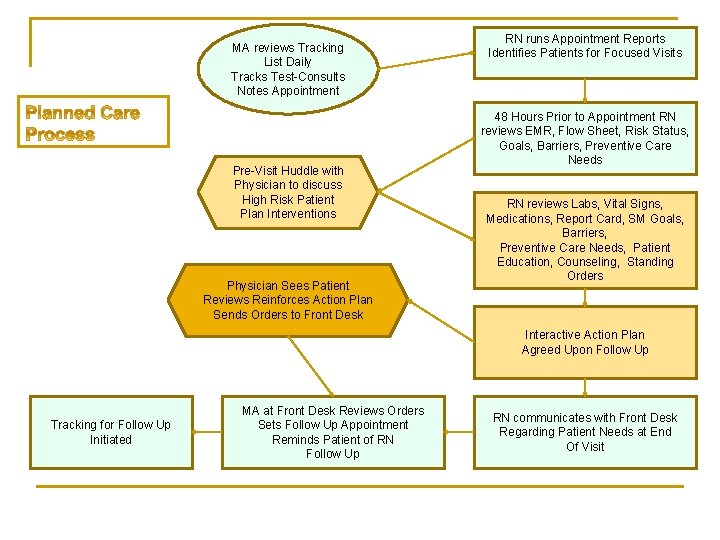
MA reviews Tracking List Daily Tracks Test-Consults Notes Appointment Pre-Visit Huddle with Physician to discuss High Risk Patient Plan Interventions Physician Sees Patient Reviews Reinforces Action Plan Sends Orders to Front Desk RN runs Appointment Reports Identifies Patients for Focused Visits 48 Hours Prior to Appointment RN reviews EMR, Flow Sheet, Risk Status, Goals, Barriers, Preventive Care Needs RN reviews Labs, Vital Signs, Medications, Report Card, SM Goals, Barriers, Preventive Care Needs, Patient Education, Counseling, Standing Orders Interactive Action Plan Agreed Upon Follow Up Tracking for Follow Up Initiated MA at Front Desk Reviews Orders Sets Follow Up Appointment Reminds Patient of RN Follow Up RN communicates with Front Desk Regarding Patient Needs at End Of Visit

Self-Management Support n n n Changed Method of Communication q Provider Self Assessment Patient Report Card q Clinical Measures Self Management Goals q Process Measures Identify Barriers to Goals & Readiness to Change Action Plan
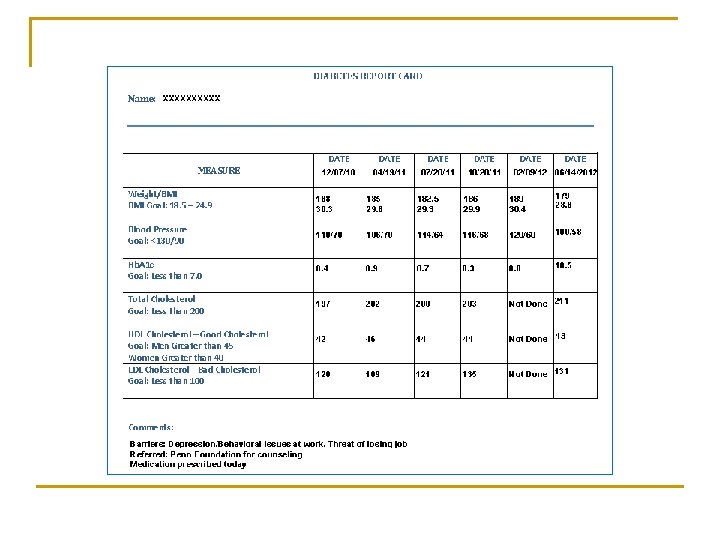
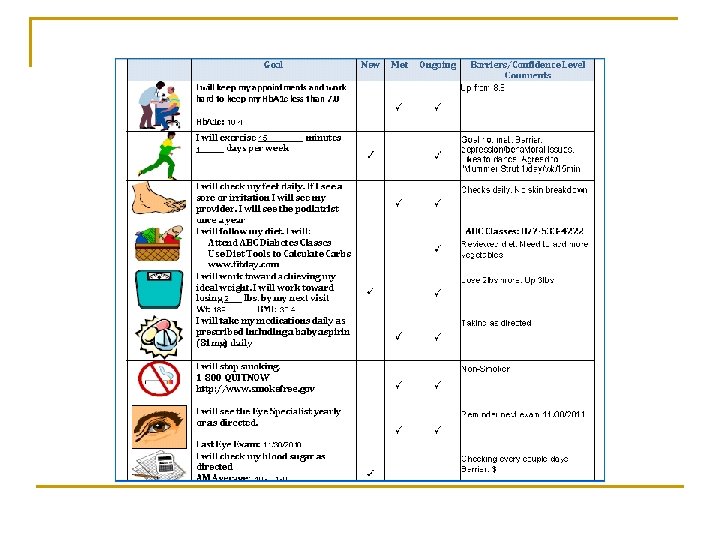

Impact of Self-Management Support n n n Improved Patient Outcomes Patients Taking Control Patients Increased Confidence q q n n n Spreading their Knowledge Improved Patient Satisfaction Improved Work Flow Improved Provider/Staff Satisfaction Development of Care Management Strategies q Developed Relationships with Insurance Carrier Care Managers and ABC Diabetes Education Program

Computer Information System The Tool n Goal q q Population Management Data Management Access and Continuity Monitor Performance
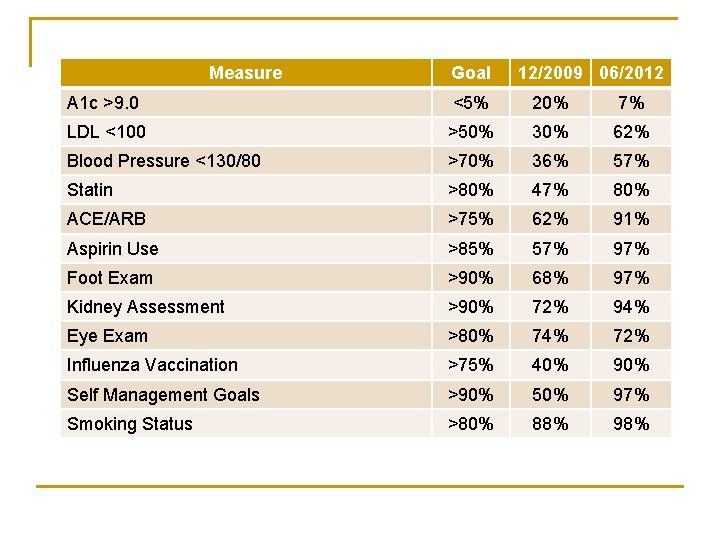
Measure Goal 12/2009 06/2012 A 1 c >9. 0 <5% 20% 7% LDL <100 >50% 30% 62% Blood Pressure <130/80 >70% 36% 57% Statin >80% 47% 80% ACE/ARB >75% 62% 91% Aspirin Use >85% 57% 97% Foot Exam >90% 68% 97% Kidney Assessment >90% 72% 94% Eye Exam >80% 74% 72% Influenza Vaccination >75% 40% 90% Self Management Goals >90% 50% 97% Smoking Status >80% 88% 98%

Advantage of Being a Small Practice n Small Practices can effect change faster than larger practices q n Less Inertia Change that occurs can result in improved patient outcomes that are consistent with improved patient outcomes in large practices

Questions?
- Slides: 27