Judicious Use of Anticoagulation A CaseBased Approach Michael

Judicious Use of Anticoagulation: A Case-Based Approach Michael B. Streiff, MD, FACP Associate Professor of Medicine and Pathology Division of Hematology Medical Director, Johns Hopkins Anticoagulation Management Service and Outpatient Clinics

Disclosures • Research Funding – Bristol-Myers Squibb – NIH/NHLBI • Consulting – – – Sanofi-aventis Eisai, Inc. Daiichi-Sankyo Janssen Healthcare Bi. O 2 • Speaking Honoraria – Sanofi-aventis – Ortho-Mc. Neil • Educational Grants – Sanofi-Aventis – Covidien

Anticoagulation for pregnancy loss • 32 year old woman with 2 previous first trimester pregnancy losses asks about LMWH to prevent miscarriages. You advise her to – Start therapeutic dose LMWH – Start prophylactic dose LMWH + Aspirin 100 mg – Start no antenatal prophylaxis

LMWH does not improve pregnancy outcomes: The ALIFE Study 364 women with at least 2 pregnancy losses Placebo (N=121) Completed Study (N=103) Aspirin 80 mg (N=120) Completed Study (N=97) Aspirin 80 mg + Nadroparin 2850 IU (N=123) Completed Study (N=99) Kaandorp S et al. NEJM 2010
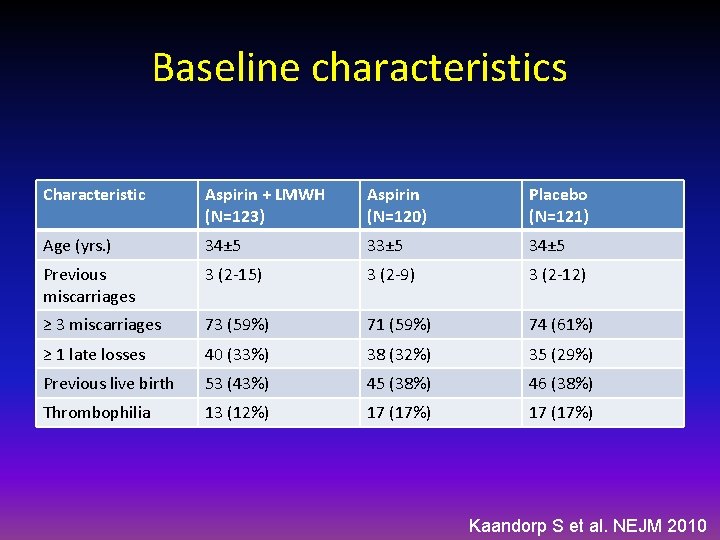
Baseline characteristics Characteristic Aspirin + LMWH (N=123) Aspirin (N=120) Placebo (N=121) Age (yrs. ) 34± 5 33± 5 34± 5 Previous miscarriages 3 (2 -15) 3 (2 -9) 3 (2 -12) ≥ 3 miscarriages 73 (59%) 71 (59%) 74 (61%) ≥ 1 late losses 40 (33%) 38 (32%) 35 (29%) Previous live birth 53 (43%) 45 (38%) 46 (38%) Thrombophilia 13 (12%) 17 (17%) Kaandorp S et al. NEJM 2010
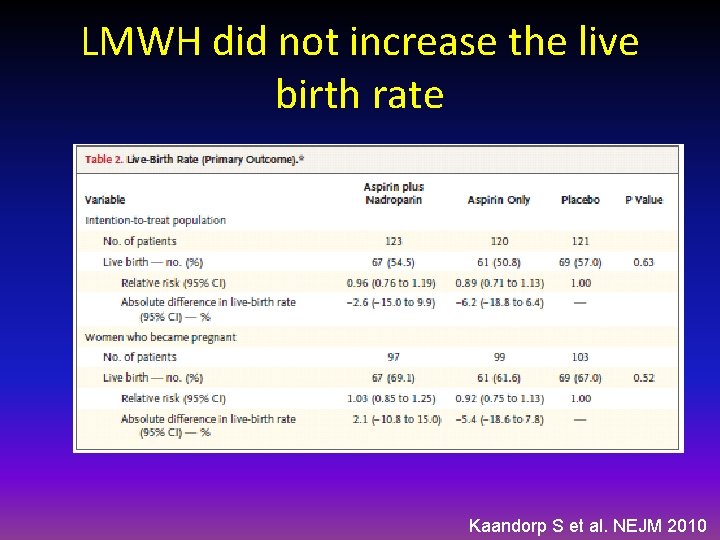

LMWH did not increase the live birth rate Kaandorp S et al. NEJM 2010
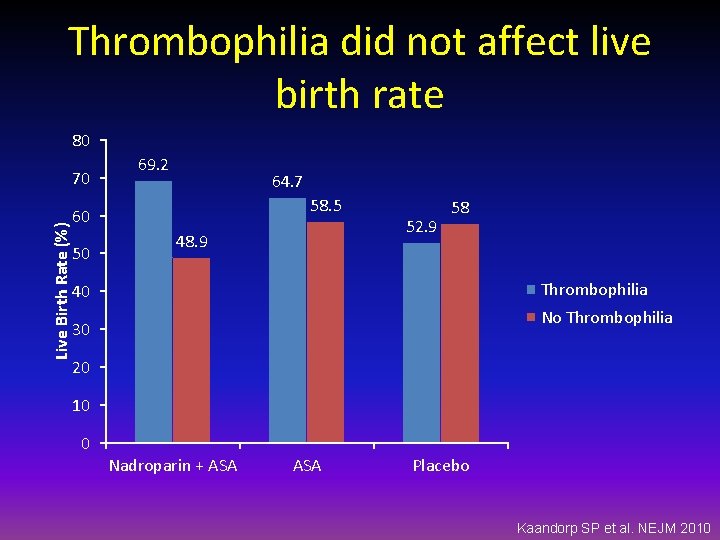
Thrombophilia did not affect live birth rate 80 Live Birth Rate (%) 70 69. 2 64. 7 58. 5 60 50 48. 9 52. 9 58 Thrombophilia 40 No Thrombophilia 30 20 10 0 Nadroparin + ASA Placebo Kaandorp SP et al. NEJM 2010

Anticoagulation does not prevent early pregnancy loss Surveillance alone 25 Adverse Events (%) • Open-label RCT of enox 40 mg/d + ASA 75 mg vs. surveillance alone • PMHx ≥ 2 losses 24 weeks or less • Begin 7 weeks gestation or less • Conclusion. Prophylactic AC does not improve pregnancy outcomes 20 20 22 Enox 40 + ASA N=294 15. 6 16 15 10 5 0 Pregnancy loss Bleeding Clark P et al. Blood 2010

Heparin + Aspirin reduces pregnancy loss in Antiphospholipid Syndrome Aspirin (N=163) UFH/LMWH + ASA (N=171) 80 70 Live Births (%) • Metanalysis of 5 RCTs of UFH/LMWH + aspirin versus aspirin • Regimens- UFH 500020000 units + aspirin 75 -81 mg and LMWH 5000 + aspirin 75 -81 mg • Conclusion- UFH/LMWH + ASA improves live birth rates 60 74. 3 RR 1. 3 55. 8 50 40 30 20 10 0 Live Birth Mak A et al. Rheumatol 2010

Anticoagulation- Less or More? • A 65 year old man with a St Jude aortic valve is scheduled to undergo a prostatectomy for cancer. When should he resume full-dose anticoagulation? – 12 hours post-op – 24 hours post-op – 36 hours post-op – 72 hours post-op
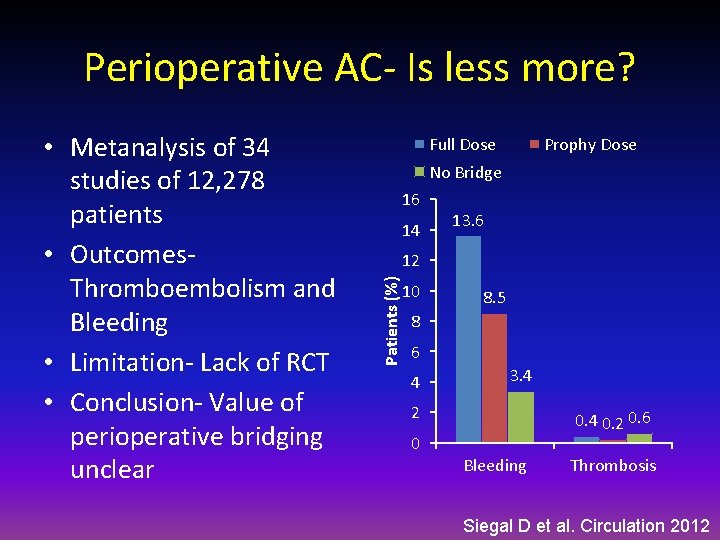
Perioperative AC- Is less more? Full Dose Prophy Dose No Bridge 16 14 13. 6 12 Patients (%) • Metanalysis of 34 studies of 12, 278 patients • Outcomes. Thromboembolism and Bleeding • Limitation- Lack of RCT • Conclusion- Value of perioperative bridging unclear 10 8. 5 8 6 4 3. 4 2 0 0. 4 0. 2 0. 6 Bleeding Thrombosis Siegal D et al. Circulation 2012
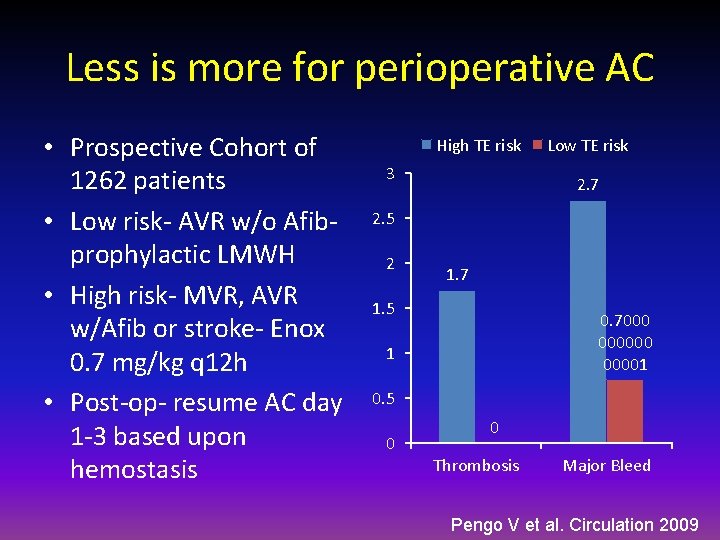
Less is more for perioperative AC • Prospective Cohort of 1262 patients • Low risk- AVR w/o Afibprophylactic LMWH • High risk- MVR, AVR w/Afib or stroke- Enox 0. 7 mg/kg q 12 h • Post-op- resume AC day 1 -3 based upon hemostasis High TE risk 3 Low TE risk 2. 7 2. 5 2 1. 7 1. 5 0. 7000 00001 1 0. 5 0 0 Thrombosis Major Bleed Pengo V et al. Circulation 2009

Thromboembolism Risk Stratification Thromboembolic Risk Atrial Fibrillation Mechanical Valve High CHADS 2 score 5 or 6 Any Mitral valve Older valve (Cagedball, Tilting disk) Recent stroke/TIA Recent (within 3 mos. ) VTE Severe thrombophilia Intermediate CHADS 2 score 3 or 4 Bileaflet Aortic valve + TE risk factors VTE within 3 -12 mos. Recurrent VTE, Active Cancer Non-severe thrombophilia Low CHADS 2 score 0 -2 VTE > 12 mos. Bileaflet Aortic valve w/o TE risk factors Venous Thromboembolism TE risk factors= A fib, Cardiac failure, HTN, DM, Age > 75, Stroke/TIA Douketis JD Blood 2011

Bleeding Risk Assessment Low Bleeding Risk Procedures High Bleeding Risk Procedures Cholecystectomy Abdominal hysterectomy GI Endoscopy ± biopsy or stent Pacemaker insertion, EP testing Dental extractions Carpal tunnel repair Dilatation/currettage Skin Cancer excision Abdominal hernia Hydrocele repair Cataract surgery Bronchoscopy ± biopsy Central Venous Catheter removal Skin, Thyroid, Breast, Lymph node biopsy Cardiac surgery Abdominal aneurysm repair Neurosurgery Urologic surgery Head and Neck surgery Hip/knee replacement Back surgery Kidney biopsy Polypectomy/sphincterotomy Transurethral prostate resection General surgery Vascular surgery Any major surgery (> 45 minutes) Spyropoulos AC and Douketis JD Blood 2012
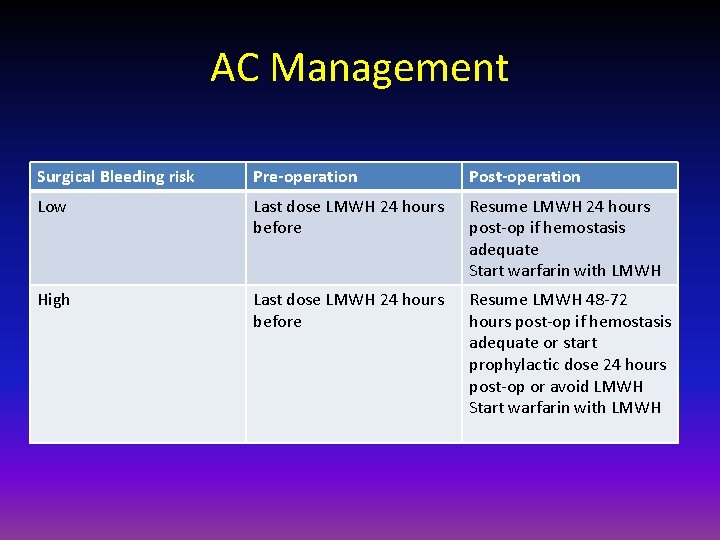
AC Management Surgical Bleeding risk Pre-operation Post-operation Low Last dose LMWH 24 hours before Resume LMWH 24 hours post-op if hemostasis adequate Start warfarin with LMWH High Last dose LMWH 24 hours before Resume LMWH 48 -72 hours post-op if hemostasis adequate or start prophylactic dose 24 hours post-op or avoid LMWH Start warfarin with LMWH

Anticoagulation for VTE • 65 year old man develops a right femoralpopliteal vein DVT 1 week after right knee replacement. A thrombophilia evaluation reveals he is heterozygous for the factor V Leiden mutation. How long should he be treated? – 6 weeks – 3 months – 12 months – Indefinite

Anticoagulation for VTE • 48 year old man presents with progressive dyspnea over 1 week and left leg discomfort. CT angiogram identifies bilateral PE. Duplex study finds a left leg DVT. No VTE risk factors are identified. How long should he be treated? – 3 months – 6 months – 12 months – Indefinite
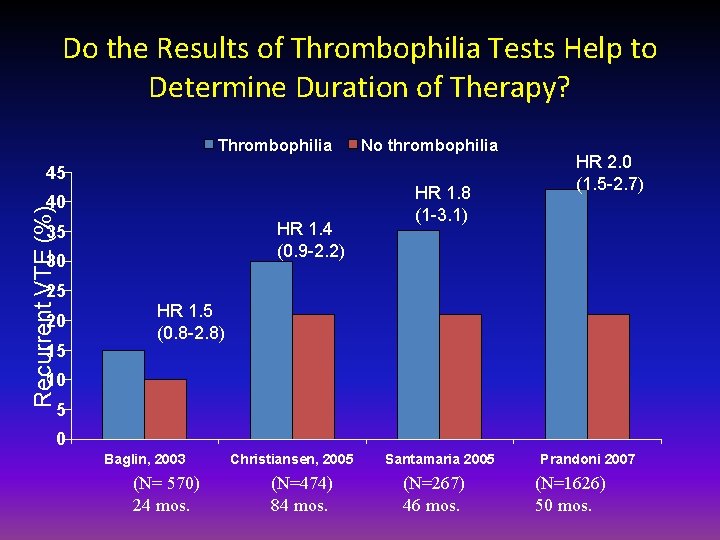
Do the Results of Thrombophilia Tests Help to Determine Duration of Therapy? Thrombophilia 45 Recurrent VTE (%) 40 HR 1. 4 (0. 9 -2. 2) 35 30 25 20 15 No thrombophilia HR 1. 8 (1 -3. 1) HR 2. 0 (1. 5 -2. 7) HR 1. 5 (0. 8 -2. 8) 10 5 0 Baglin, 2003 (N= 570) 24 mos. Christiansen, 2005 (N=474) 84 mos. Santamaria 2005 (N=267) 46 mos. Prandoni 2007 (N=1626) 50 mos.

Thrombophilia-Assessing the risk • High risk thrombophilia – Antithrombin deficiency - 1. 8 % per year (95% CI 1. 1 -2. 6%) – Protein C deficiency - 1. 5% per year (1. 1 -2. 1%) – Protein S deficiency - 1. 9% per year (1. 3 -2. 6%) • Moderate risk thrombophilia – Factor V Leiden - 0. 5% per year (0. 4 -0. 6%) – Prothrombin gene mutation - 0. 3% per year (0. 2 -0. 5%) – Factor VIII - 0. 5% per year (0. 4 -0. 5%) • Low risk thrombophilia – Factor IX - 0. 1% per year (0. 02 -0. 2%) – Factor XI - 0. 2% per year (0. 06 -0. 6%) – Hyperhomocysteinemia – 0. 1% per year (0. 05 -0. 3%) Lijfering WM et al. Blood 2009
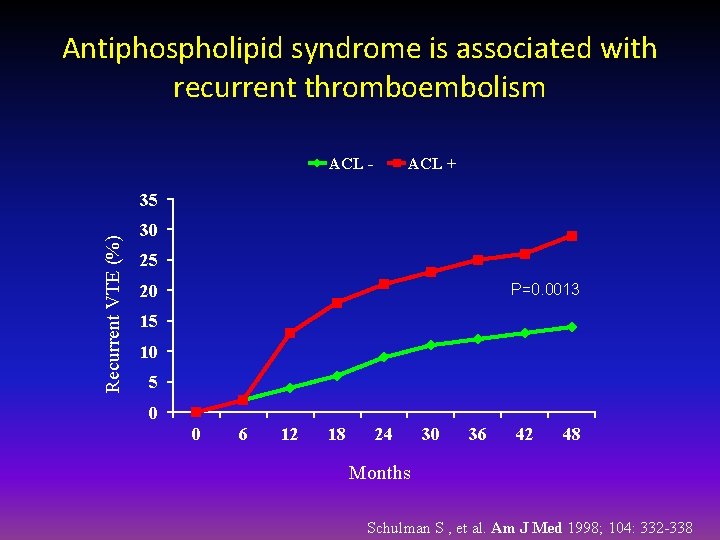
Antiphospholipid syndrome is associated with recurrent thromboembolism ACL - ACL + Recurrent VTE (%) 35 30 25 P=0. 0013 20 15 10 5 0 0 6 12 18 24 30 36 42 48 Months Schulman S , et al. Am J Med 1998; 104: 332 -338
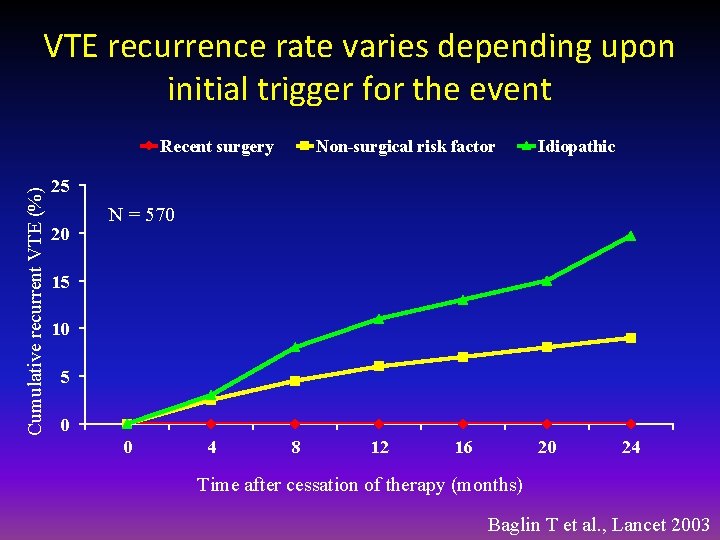
VTE recurrence rate varies depending upon initial trigger for the event Cumulative recurrent VTE (%) Recent surgery Non-surgical risk factor Idiopathic 25 20 N = 570 15 10 5 0 0 4 8 12 16 20 24 Time after cessation of therapy (months) Baglin T et al. , Lancet 2003

7. 4 8 7 6 5 4 3 2 1 0 4. 2 c th i pa io No n- su rg Id ica lt lt rig ge ge r r 0. 7000 00001 rg Su • Systematic review of prospective cohort studies and RCTs • 15 Studies • 5159 Subjects • Follow up- 3 -96 months • Conclusion- Setting of thrombosis strongly influences recurrence rate Recurrent VTE (% per pat. -yr) VTE Setting influences recurrence risk Iorio A et al. Arch Intern Med 2010
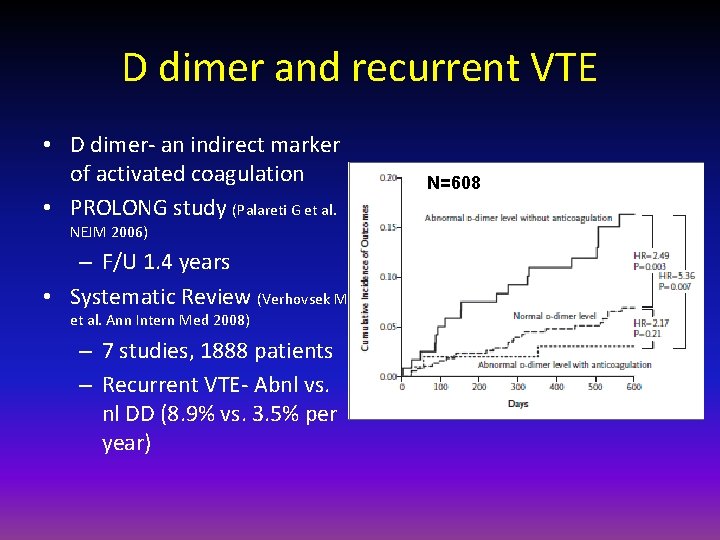
D dimer and recurrent VTE • D dimer- an indirect marker of activated coagulation • PROLONG study (Palareti G et al. NEJM 2006) – F/U 1. 4 years • Systematic Review (Verhovsek M et al. Ann Intern Med 2008) – 7 studies, 1888 patients – Recurrent VTE- Abnl vs. nl DD (8. 9% vs. 3. 5% per year) N=608
How do we identify the low risk patient with idiopathic VTE? • Prospective cohort study of 665 patients with idiopathic VTE – Enrolled at 12 centers, 4 countries prior to DC of warfarin after 5 -7 months of therapy – Information of 76 laboratory and clinical variables associated with VTE were collected – Multivariate analysis used to develop clinical prediction rule for recurrent VTE • Results – F/U population 600/665 (90%) – Mean F/U -18 months (1 -47 mos. ) – Annual risk of recurrent VTE 9. 3% per year (7. 7%-11. 3%) • Men 13. 7% (10. 8%-17%) • Women 5. 5% (3. 7%-7. 8%) Rodger MA, et al. CMAJ 2008; 179(5): 417 -26
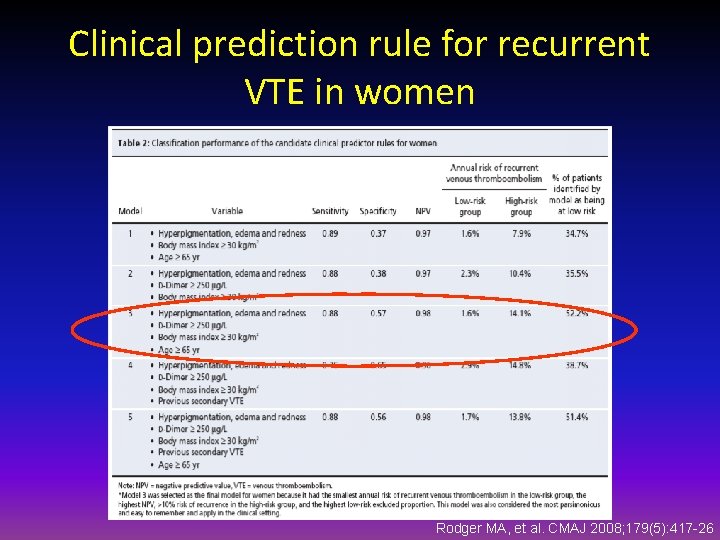
Clinical prediction rule for recurrent VTE in women Rodger MA, et al. CMAJ 2008; 179(5): 417 -26
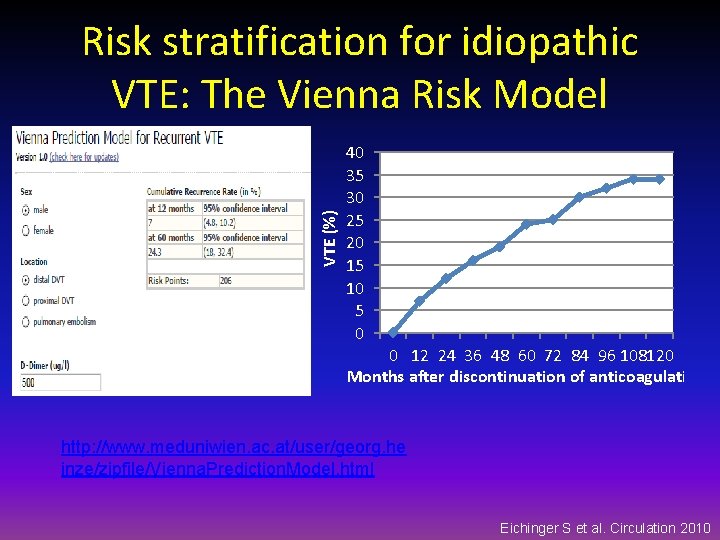
VTE (%) Risk stratification for idiopathic VTE: The Vienna Risk Model 40 35 30 25 20 15 10 5 0 0 12 24 36 48 60 72 84 96 108120 Months after discontinuation of anticoagulation http: //www. meduniwien. ac. at/user/georg. he inze/zipfile/Vienna. Prediction. Model. html Eichinger S et al. Circulation 2010

Indefinite Anticoagulation: Weighing the risks Thrombosis Bleeding
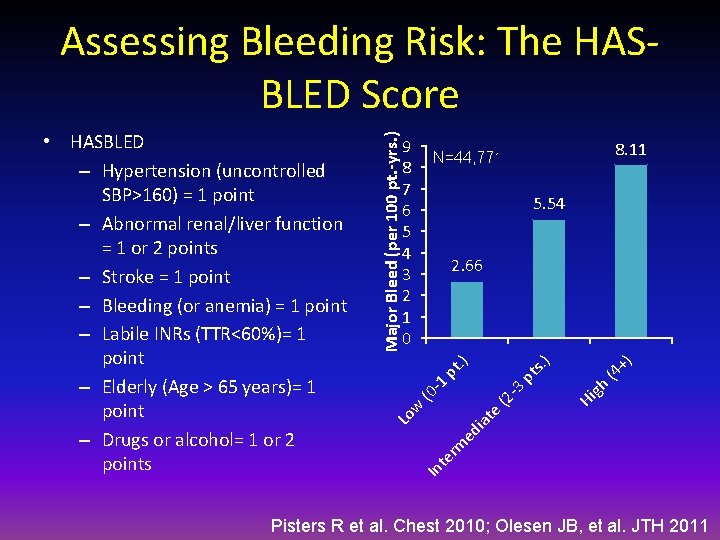
9 8 7 6 5 4 3 2 1 0 8. 11 N=44, 771 5. 54 ) (4 + gh Hi te w (2 - (0 3 -1 pt pt s. ) 2. 66 In te rm ed ia Lo • HASBLED – Hypertension (uncontrolled SBP>160) = 1 point – Abnormal renal/liver function = 1 or 2 points – Stroke = 1 point – Bleeding (or anemia) = 1 point – Labile INRs (TTR<60%)= 1 point – Elderly (Age > 65 years)= 1 point – Drugs or alcohol= 1 or 2 points Major Bleed (per 100 pt. -yrs. ) Assessing Bleeding Risk: The HASBLED Score Pisters R et al. Chest 2010; Olesen JB, et al. JTH 2011

Central Venous Catheter Prophylaxis • 67 year old man has just had a right subclavian Hickman CVC placed for chemotherapy for recently diagnosed NHL. What should be used for CVC thrombosis prophylaxis? – Warfarin 1 mg daily – Enoxaparin 40 mg daily – Dalteparin 5000 units daily – No prophylaxis necessary
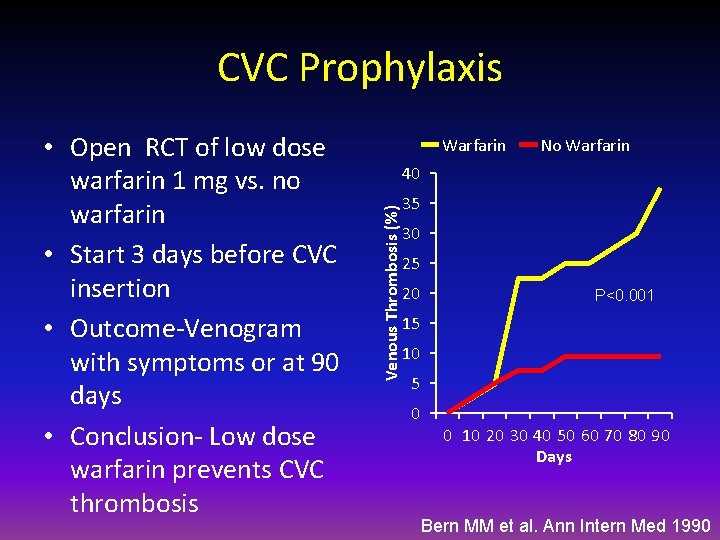
CVC Prophylaxis Warfarin No Warfarin 40 Venous Thrombosis (%) • Open RCT of low dose warfarin 1 mg vs. no warfarin • Start 3 days before CVC insertion • Outcome-Venogram with symptoms or at 90 days • Conclusion- Low dose warfarin prevents CVC thrombosis 35 30 25 20 P<0. 001 15 10 5 0 0 10 20 30 40 50 60 70 80 90 Days Bern MM et al. Ann Intern Med 1990
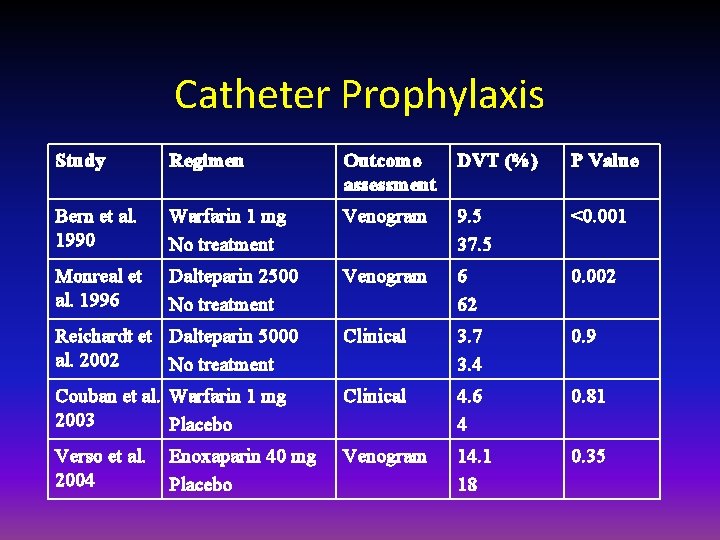

Catheter Prophylaxis Study Regimen Outcome assessment DVT (%) P Value Bern et al. 1990 Warfarin 1 mg No treatment Venogram 9. 5 37. 5 <0. 001 Monreal et al. 1996 Dalteparin 2500 No treatment Venogram 6 62 0. 002 Reichardt et Dalteparin 5000 al. 2002 No treatment Clinical 3. 7 3. 4 0. 9 Couban et al. Warfarin 1 mg 2003 Placebo Clinical 4. 6 4 0. 81 Verso et al. 2004 Venogram 14. 1 18 0. 35 Enoxaparin 40 mg Placebo
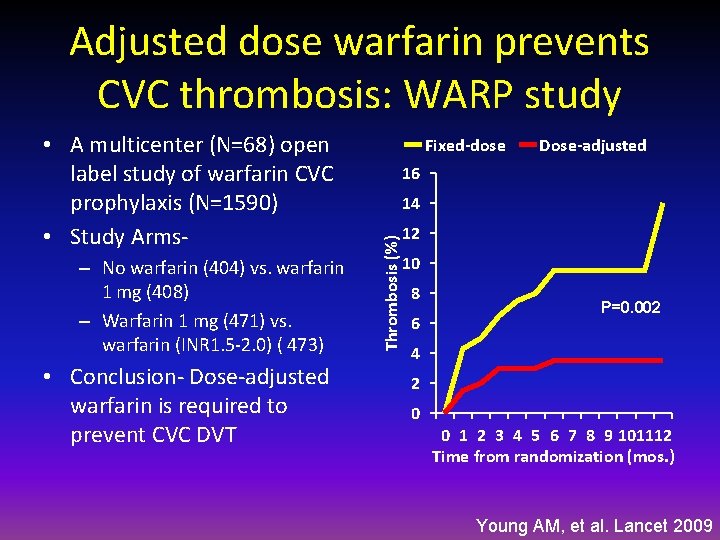
Adjusted dose warfarin prevents CVC thrombosis: WARP study – No warfarin (404) vs. warfarin 1 mg (408) – Warfarin 1 mg (471) vs. warfarin (INR 1. 5 -2. 0) ( 473) • Conclusion- Dose-adjusted warfarin is required to prevent CVC DVT Fixed-dose Dose-adjusted 16 14 Thrombosis (%) • A multicenter (N=68) open label study of warfarin CVC prophylaxis (N=1590) • Study Arms- 12 10 8 6 P=0. 002 4 2 0 0 1 2 3 4 5 6 7 8 9 101112 Time from randomization (mos. ) Young AM, et al. Lancet 2009

Elevated INR- Less vitamin K is more • 70 year old man taking warfarin for atrial fibrillation has an INR of 7. He does not have any signs of bleeding. What should you do? – Hold warfarin and administer vitamin K 2. 5 mg po – Hold warfarin and administer vitamin K 2. 5 mg IV – Hold warfarin and recheck INR in 1 -2 days – Hold warfarin and administer Vitamin K 2. 5 mg and 3 units of FFP
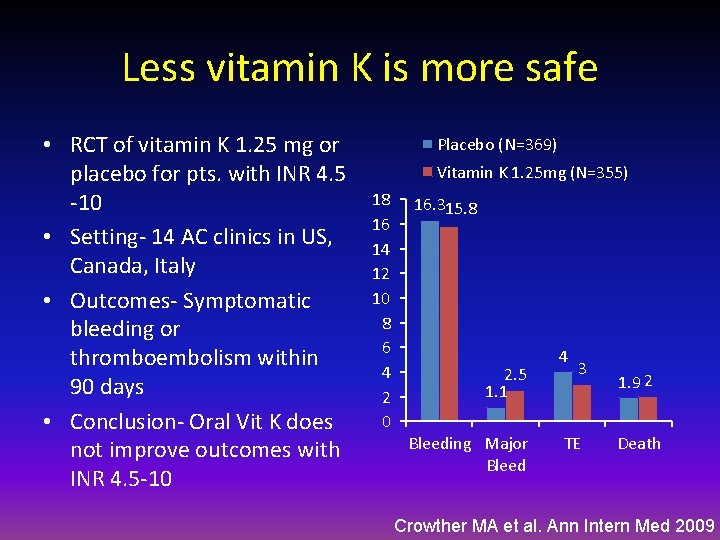
Less vitamin K is more safe • RCT of vitamin K 1. 25 mg or placebo for pts. with INR 4. 5 -10 • Setting- 14 AC clinics in US, Canada, Italy • Outcomes- Symptomatic bleeding or thromboembolism within 90 days • Conclusion- Oral Vit K does not improve outcomes with INR 4. 5 -10 Placebo (N=369) Vitamin K 1. 25 mg (N=355) 18 16 14 12 10 8 6 4 2 0 16. 315. 8 2. 5 1. 1 Bleeding Major Bleed 4 3 TE 1. 9 2 Death Crowther MA et al. Ann Intern Med 2009

Is less is more? • 72 year old man with atrial fibrillation who has been on warfarin 5 mg daily for 3 months. Today his INR is 1. 8. No reason identified. What should you do with his warfarin dose? – Increase his dose to 7. 5 mg MWF, 5 mg ROW (21% dose increase), recheck 1 week – Increase his dose to 7. 5 mg daily (50% dose increase), recheck 1 week – Increase his dose to 7. 5 mg W, 5 mg ROW (7% dose increase, recheck 1 week – Continue same dose, recheck 1 week
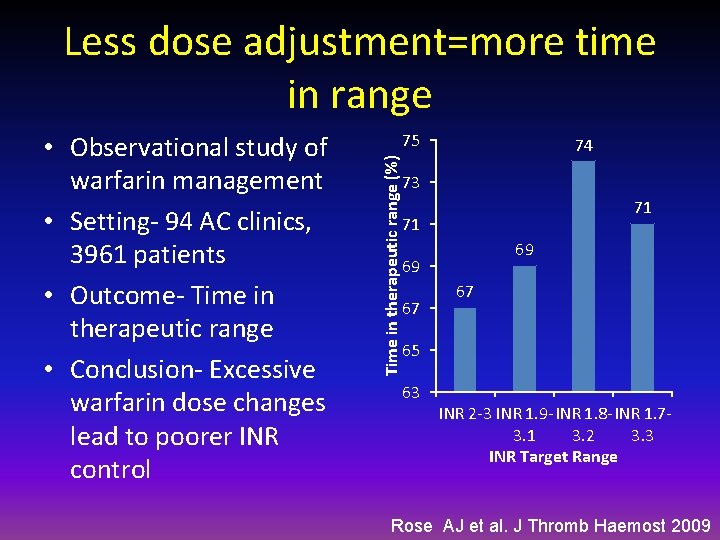
Less dose adjustment=more time in range 75 Time in therapeutic range (%) • Observational study of warfarin management • Setting- 94 AC clinics, 3961 patients • Outcome- Time in therapeutic range • Conclusion- Excessive warfarin dose changes lead to poorer INR control 74 73 71 71 69 69 67 67 65 63 INR 2 -3 INR 1. 9 - INR 1. 8 - INR 1. 73. 1 3. 2 3. 3 INR Target Range Rose AJ et al. J Thromb Haemost 2009

Is less LMWH more? • A 65 year old man with an atrial fibrillation (CHADS 2 score 3) who has been on warfarin for 4 months has an INR of 1. 5. Your nurse asks you for advice. You suggest… – LMWH + warfarin dose increase – Warfarin dose increase only
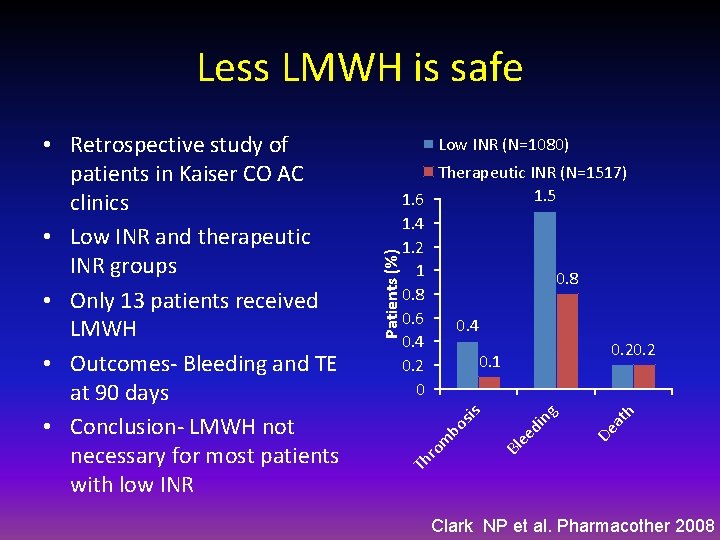
Less LMWH is safe Low INR (N=1080) at h De g in Bl ee d om bo sis Therapeutic INR (N=1517) 1. 5 1. 6 1. 4 1. 2 1 0. 8 0. 6 0. 4 0. 2 0. 1 0. 2 0 Th r Patients (%) • Retrospective study of patients in Kaiser CO AC clinics • Low INR and therapeutic INR groups • Only 13 patients received LMWH • Outcomes- Bleeding and TE at 90 days • Conclusion- LMWH not necessary for most patients with low INR Clark NP et al. Pharmacother 2008

Conclusions • Anticoagulation is not indicated for recurrent early pregnancy loss except perhaps APS • Therapeutic AC should be used sparingly in the post-operative period • Setting rather than presence of thrombophilia dictates duration of therapy • Risk stratification models can help determine the risk of recurrent VTE and bleeding in patients with idiopathic VTE • Central venous catheter prophylaxis remains of unproven benefit • Studies continue to optimize warfarin management

Questions ?
- Slides: 40