JOURNAL CLUB PRESENTATION on Barriers of Drug Adherence

JOURNAL CLUB PRESENTATION on Barriers of Drug Adherence among Patients with Epilepsy: In Tertiary Care Hospital, South India. Presenter: Anjna Kumari BS 18 MHNS 001

Barriers of Drug Adherence among Patients with Epilepsy: In Tertiary Care Hospital, South India. � Author Name: Ancy M Das , Lakshmi Ramaoorthy, Sunil Narayan, Vaibhav Wadwekar � Journal � Name: Journal of Caring Sciences Volume: 7 � Year: Dec. 2018 � Website: http: //journals. tbzmed. ac. ir/JCS content

INTRODUCTION v. Epilepsy is one of the common neurological disorders which is featured by abnormal movement; may occur with or without loss of consciousness. v. However, epilepsy is a hidden disorder like an iceberg, and many cases go unconveyed.

�All over the world, misconceptions, fright and negative public attitudes toward this most prevalent neurological disorder results in discrimination, isolation and widespread social rejection of epileptic patients. �There may be more than 40 billion epileptics. �In India, the prevalence rate of epilepsy is 5 -10 per 1000 population. �It's with two major types; generalized or partial. Cont. .

OBJECTIVE �To assess the adherence pattern to antiepileptic regimen, among patients with epilepsy. �To identify the clinical and patientrelated factors contributing as barriers.

Research Methodology �Research Approach: Quantitative study �Research Design: Non – experimental design( cross – sectional study) �Study Setting : Tertiary care hospital in South India. �Population: Epileptic patient(18 -65 years)

�Sample Size: 100 Epilepsy patient. �Sampling Technique: convenient sampling technique.

Inclusion & Exclusion Criteria Inclusion Criteria: v Patients diagnosed with epilepsy. v Willing to participate and taking antiepileptic medications for at least one year. Exclusion Criteria v The patients who are below 18 years of age. v Patients who have mental retardation and severe physical impairments. v Who were less than one year of anti-epileptic treatment were excluded from the study.

Tools Used For The Study �Sociodemoghraphic �Clinical data sheet. Variable. �Self prepared questioner. (Knowledge, attitude and believe questioner) �MMAS (Morisky Medication Adherence Scale).

Tools Used For The Study � Morisky Medication Adherence Scale (MMAS) was used to assess the adherence pattern to antiepileptic regimen which includes eight items. � MMAS is a standardized 8 item questionnaire with seven Yes/No questions. � All yes response scored as 1, No response as Zero

One question answered on a 5 -point Likert scale � A: Never/Rarely � B: Once in a while � C: Sometimes � D: Usually � E: All the time All B-E response were scored as 1(one) A (Never/Rarely) response scored as zero as per tool.

Scoring And Interpretation According to the scoring system for the MMAS, � 0 = High adherence � 1 to 2 = Medium adherence � And more than 2 = Low adherence. Patients who had a score of 0 to 2 were considered adherent and more than 2 as non-adherent.

Interpretation � Assessment of the Patient related factors such as lifestyle, social support and patient prescriber relationship was done with the help of Rating Scale. � Assessment of the Behavioral factors such as knowledge, belief and attitude was assessed by using self-prepared questionnaire consisting of 30 questions.
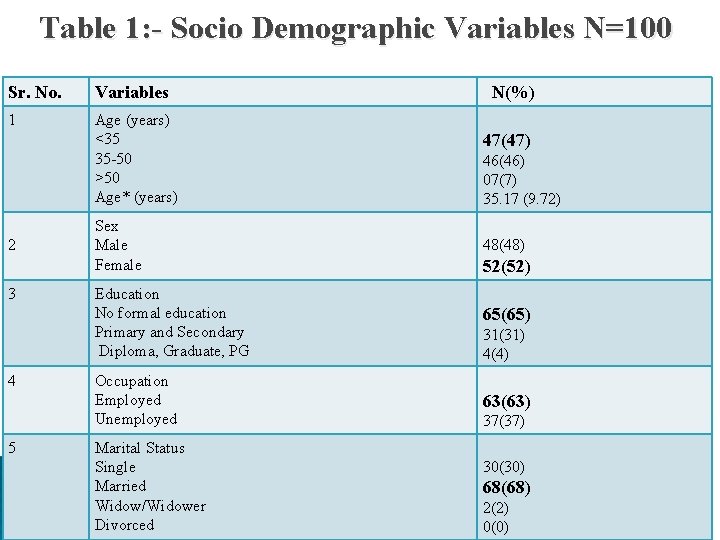
Table 1: - Socio Demographic Variables N=100 Sr. No. Variables 1 Age (years) <35 35 -50 >50 Age* (years) 2 3 4 5 Sex Male Female Education No formal education Primary and Secondary Diploma, Graduate, PG Occupation Employed Unemployed Marital Status Single Married Widow/Widower Divorced N(%) 47(47) 46(46) 07(7) 35. 17 (9. 72) 48(48) 52(52) 65(65) 31(31) 4(4) 63(63) 37(37) 30(30) 68(68) 2(2) 0(0)
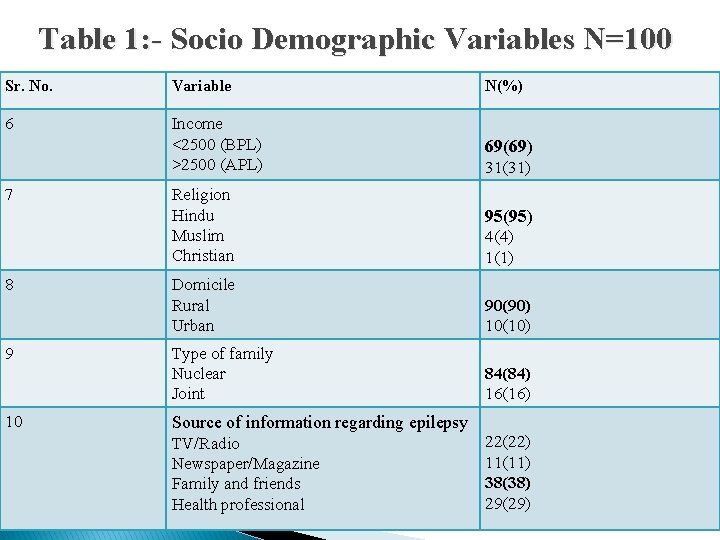
Table 1: - Socio Demographic Variables N=100 Sr. No. Variable N(%) 6 Income <2500 (BPL) >2500 (APL) 69(69) 7 8 9 10 Religion Hindu Muslim Christian 31(31) 95(95) 4(4) 1(1) Domicile Rural Urban 90(90) 10(10) Type of family Nuclear Joint 84(84) 16(16) Source of information regarding epilepsy TV/Radio Newspaper/Magazine Family and friends Health professional 22(22) 11(11) 38(38) 29(29)
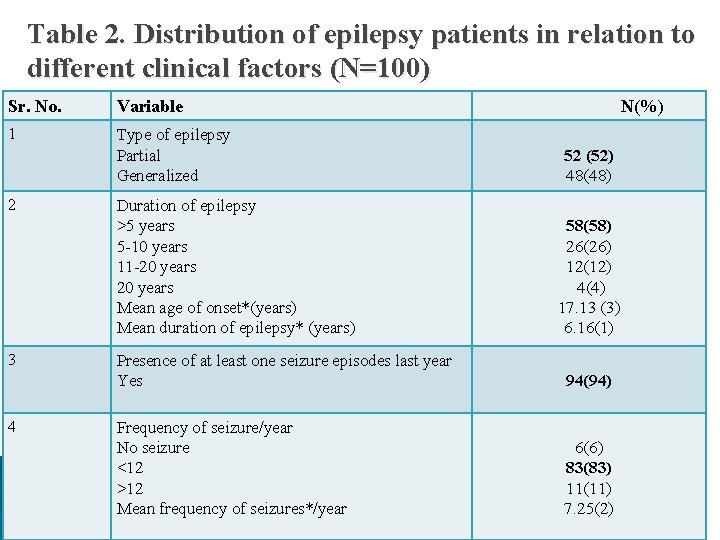
Table 2. Distribution of epilepsy patients in relation to different clinical factors (N=100) Sr. No. Variable 1 Type of epilepsy Partial Generalized 2 3 4 Duration of epilepsy >5 years 5 -10 years 11 -20 years Mean age of onset*(years) Mean duration of epilepsy* (years) N(%) 52 (52) 48(48) 58(58) 26(26) 12(12) 4(4) 17. 13 (3) 6. 16(1) Presence of at least one seizure episodes last year Yes 94(94) Frequency of seizure/year No seizure <12 >12 Mean frequency of seizures*/year 6(6) 83(83) 11(11) 7. 25(2)
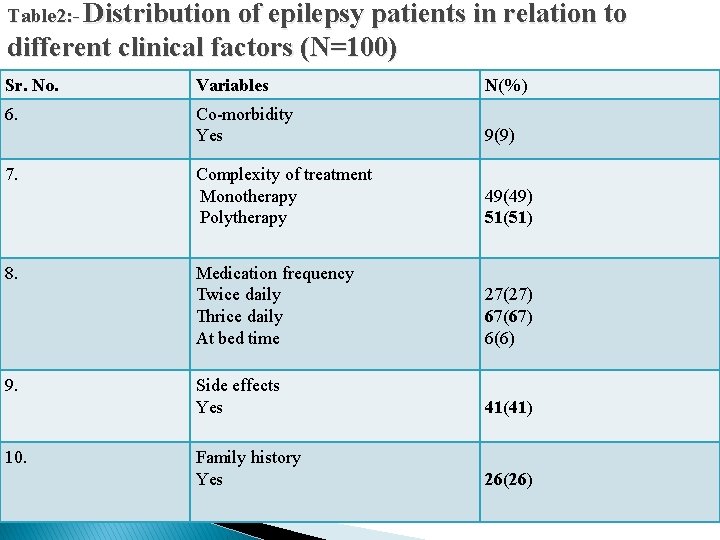
Table 2: - Distribution of epilepsy patients in relation to different clinical factors (N=100) Sr. No. Variables N(%) 6. Co-morbidity Yes 9(9) Complexity of treatment Monotherapy Polytherapy 49(49) 51(51) Medication frequency Twice daily Thrice daily At bed time 27(27) 67(67) 6(6) Side effects Yes 41(41) Family history Yes 26(26) 7. 8. 9. 10.
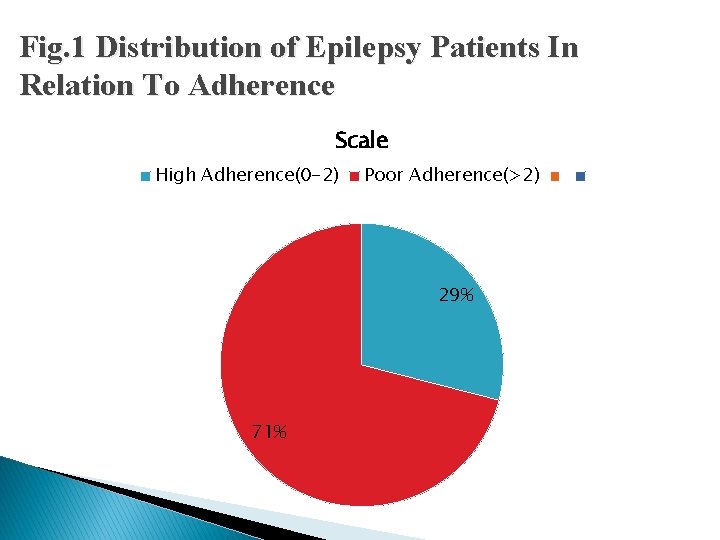
Fig. 1 Distribution of Epilepsy Patients In Relation To Adherence Scale High Adherence(0 -2) Poor Adherence(>2) 29% 71%
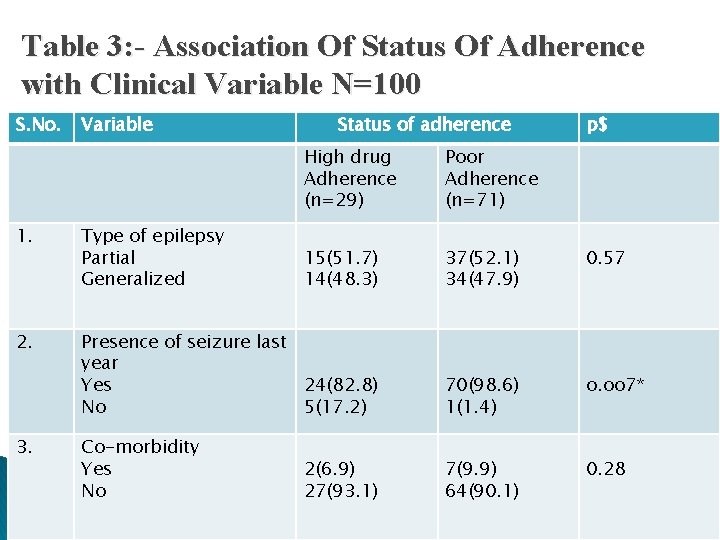
Table 3: - Association Of Status Of Adherence with Clinical Variable N=100 S. No. Variable Status of adherence High drug Adherence (n=29) Poor Adherence (n=71) p$ 1. Type of epilepsy Partial Generalized 15(51. 7) 14(48. 3) 37(52. 1) 34(47. 9) 0. 57 2. Presence of seizure last year Yes 24(82. 8) No 5(17. 2) 70(98. 6) 1(1. 4) o. oo 7* Co-morbidity Yes No 7(9. 9) 64(90. 1) 0. 28 3. 2(6. 9) 27(93. 1)
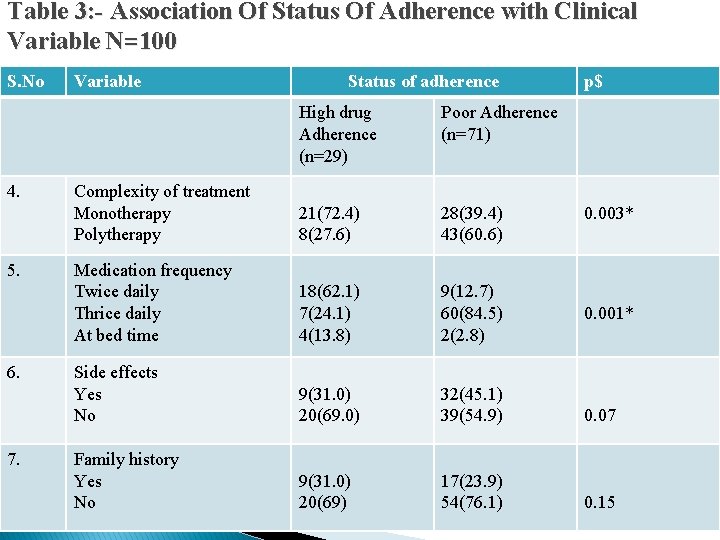
Table 3: - Association Of Status Of Adherence with Clinical Variable N=100 S. No 4. 5. 6. 7. Variable Status of adherence p$ High drug Adherence (n=29) Poor Adherence (n=71) Complexity of treatment Monotherapy Polytherapy 21(72. 4) 8(27. 6) 28(39. 4) 43(60. 6) Medication frequency Twice daily Thrice daily At bed time 18(62. 1) 7(24. 1) 4(13. 8) 9(12. 7) 60(84. 5) 2(2. 8) Side effects Yes No 9(31. 0) 20(69. 0) 32(45. 1) 39(54. 9) 0. 07 Family history Yes No 9(31. 0) 20(69) 17(23. 9) 54(76. 1) 0. 15 0. 003* 0. 001*

Table 4: -Comparison of status of adherence in relation to the behavioral factors N=100 Variable Status of adherence High drug adherence (n=29) Mean (SD) Lifestyle Social support Patient prescriber relationship 30. 03 (3. 94) 8. 21 (1. 37) 13. 28 (1. 9) Statistical indicators$ Poor drug adherence (n=71) Mean (SD) 25. 85 (3. 92) 8. 01 (1. 27) 13. 30 (1. 39) $Independent student t- test, *significance at p<0. 05 0. 0001* 0. 5 0. 95

Table 5: -Comparison of status of adherence in relation to the patient related factors N=100 Variable Knowledge Belief Attitude Status Of Adherence High drug adherence Poor drug adherence (n=29) Mean (SD) (n=71) Mean (SD) 13. 07( 4. 32) 3. 79 (1. 82) 2. 76 (1. 40) 8. 39 (3. 70) 3. 46 (1. 39) 2. 70 (1. 16) $Independent student t test, *significance at p<0. 05 p$ 0. 0001* 0. 33 0. 84

Summary � 100 patients, majority (71) of patients were not adherent to the antiepileptic treatment. � 49 patients were on monotherapy had more adherent, than 51 patient who were on polytherapy � It shows that as the number of drugs increases, adherence decreases.

Limitation of the study � Study was conducted only one hospital i. e. Tertiary Care Hospital. � Study was used in 100 epilepsy patients in an Outpatient unit of tertiary care center.

Drawback of the study �Study adopted convenient Sampling, hence the study results may not be generalized in larger extent. �The results were based on patient’s recall of facts which sometime biased. �Small sample size was used for conducted a study.

Conclusion � Systematically and orderly planned health information will be very much beneficial for patients with epilepsy. � This study adopted convenient Sampling, hence the study results may not be generalized in larger extent. � Also the results were based on patient’s recall of facts which sometime biased.

References…. . 1. Easthall C, Song F, Bhattacharya D. A meta-analysis of cognitive-based behaviour change techniques as interventions to improve medication adherence. BMJ Open 2013; 3 (8): Pii: e 002749. doi: 10. 1136/bmjopen 2013002749. 2. Jones RM, Butler JA, Thomas VA, Peveler RC, Prevett M. Adherence to treatment in patients with epilepsy: associations with seizure control and illness beliefs. Seizure 2006; 15 (7): 504– 8. doi: 10. 1016/j. seizure. 2006. 003 3. Liu J, Liu Z, Ding H, Yang X. Adherence to treatment and influencing factors in a sample of Chinese epilepsy patients. Epileptic Disord 2013; 15 (3): 289– 94. doi: 10. 1684/epd. 2013. 0588 4. Nakhutina L, Gonzalez JS, Margolis SA, Spada A, Grant A. Adherence to antiepileptic drugs and beliefs about medication among predominantly ethnic minority patients with epilepsy. Epilepsy Behav 2011; 22 (3): 584– 5. doi: 10. 1016/j. yebeh. 2011. 08. 007 6. Beerendrakumar N, Ramamoorthy L, Haridasan S. Dietary and Fluid Regime Adherence in Chronic Kidney Disease Patients. J Caring Sci. 2018; 7(1): 17 -20. Published 2018 Mar 1. doi: 10. 15171/jcs. 2018. 003 7. Gabr WM, Shams ME. Adherence to medication among outpatient adolescents with epilepsy. Saudi Pharm J 2015; 23 (1): 33 -40. doi: 10. 1016/j. jsps. 2014. 05. 003

- Slides: 28