JOURNAL CLUB EVIDENCE BASED PRACTICE Clinical Practice Guidelines

JOURNAL CLUB: EVIDENCE BASED PRACTICE Clinical Practice Guidelines: The Diagnosis, Management, and Prevention of Bronchiolitis Margaret Thew

GUIDELINE APPLICATION • The bronchiolitis guideline is intended for children from 1 -23 months • Updated version released 2015 by American Academy of Pediatrics • The guideline offers recommendations ranked according to level of evidence and risk/benefit. • Key action of this guideline is the use of evidence-based approach to diagnosis, prevention, and management of bronchiolitis

POPULATION • Intended for children 1 -23 months of age • Excluded: • Children who are Immunocompromised. • Children with underlying respiratory disease. • Children with neuromuscular disease. • Children with congenital heart disease or known hemodynamic conditions. • Recurrent wheezing or risk of asthma.

DEFINITION • Bronchiolitis is commonly caused by a viral illness of the lower respiratory tract in infants. • It is characterized by acute inflammation, edema, and necrosis of the epithelial cells lining the small airways. • There is increased mucous production • Signs and Symptoms include; rhinitis, cough which may progress to tachypnea, wheezing, rales, use of accessory muscles, and/or nasal flaring. • Peak season December to March • Bronchiolitis is the most common cause for hospitalization among infants during the first 12 months.

RISKS • Bronchiolitis is the most common cause of hospitalization among infants during their first 12 months of life. • ~ 100, 000 admissions annually in the United States • The estimated cost of these admission is $1. 73 billion. • One estimate of hospitalization from the CDC was 5. 2 per 1000 children < 24 months (study timeline 200 -2005) • The largest age-specific hospitalization occurred between 30 -60 days of age at a rate of 25. 9/1000 children.

METHODS • A subcommittee was made up of; primary care physicians, pediatricians, family practice, ED, hospital medicine, pulmonologists, neonatal, peds infectious disease, a parent representative, and an epidemiologist trained in systemic reviews. • The evidence search and review included electronic database searches in The Cochrane Library, Ovid, CINAHL, EBSCO and Pubmed. • The search strategy included database searches reviewed by 1 of 4 members of the committee. The original evidence-based articles from 2003 were reviewed along with new evidence-based articles written from 2004 – 2014.

EVIDENCE-BASED APPROACH • The evidence-based approach reflect the quality of evidence and the balance of benefit and harm that is anticipated when the recommendation is followed. • This clinical practice guideline is not intended as a sole source of guidance in management of children with bronchiolitis only as a guide to support decision making. • These guidelines are reviewed every 5 years.

LEVELS OF RECOMMENDATIO N
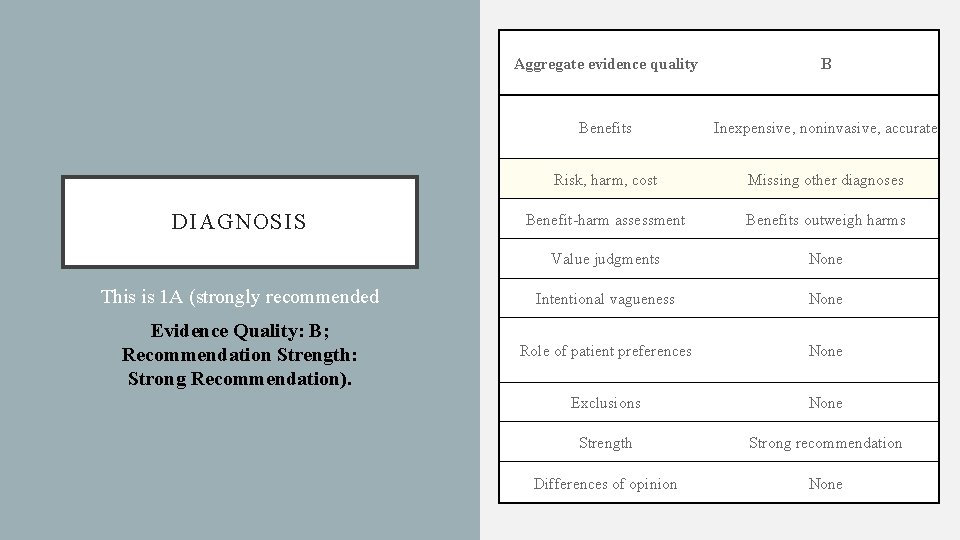

Aggregate evidence quality B Benefits Inexpensive, noninvasive, accurate Risk, harm, cost Missing other diagnoses Benefit-harm assessment Benefits outweigh harms Value judgments None This is 1 A (strongly recommended Intentional vagueness None Evidence Quality: B; Recommendation Strength: Strong Recommendation). Role of patient preferences None Exclusions None Strength Strong recommendation Differences of opinion None DIAGNOSIS

ASSESS RISK This is 1 B: Moderate recommendation Evidence Quality: B; Recommendation Strength: Moderate Recommendation
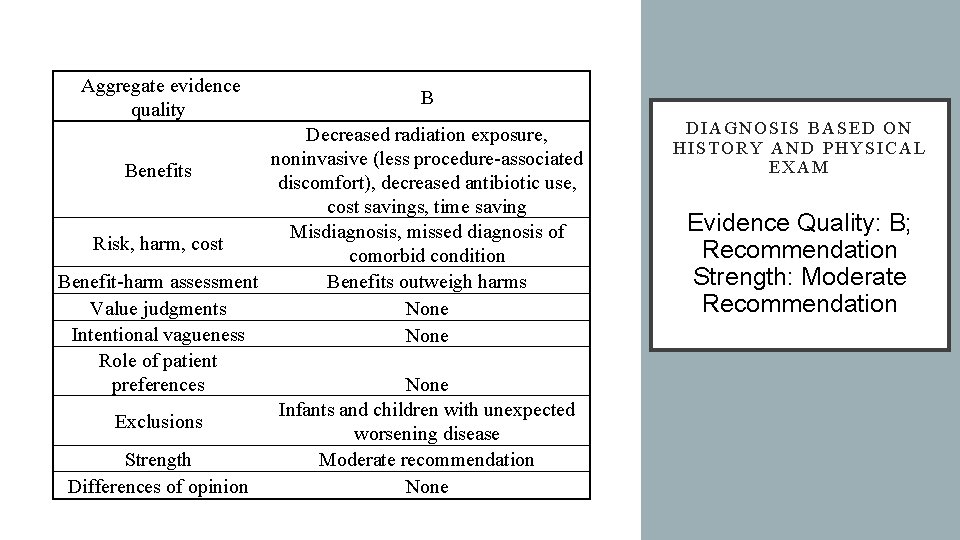

Aggregate evidence quality B Decreased radiation exposure, noninvasive (less procedure-associated Benefits discomfort), decreased antibiotic use, cost savings, time saving Misdiagnosis, missed diagnosis of Risk, harm, cost comorbid condition Benefit-harm assessment Benefits outweigh harms Value judgments None Intentional vagueness None Role of patient preferences None Infants and children with unexpected Exclusions worsening disease Strength Moderate recommendation Differences of opinion None DIAGNOSIS BASED ON HISTORY AND PHYSICAL EXAM Evidence Quality: B; Recommendation Strength: Moderate Recommendation
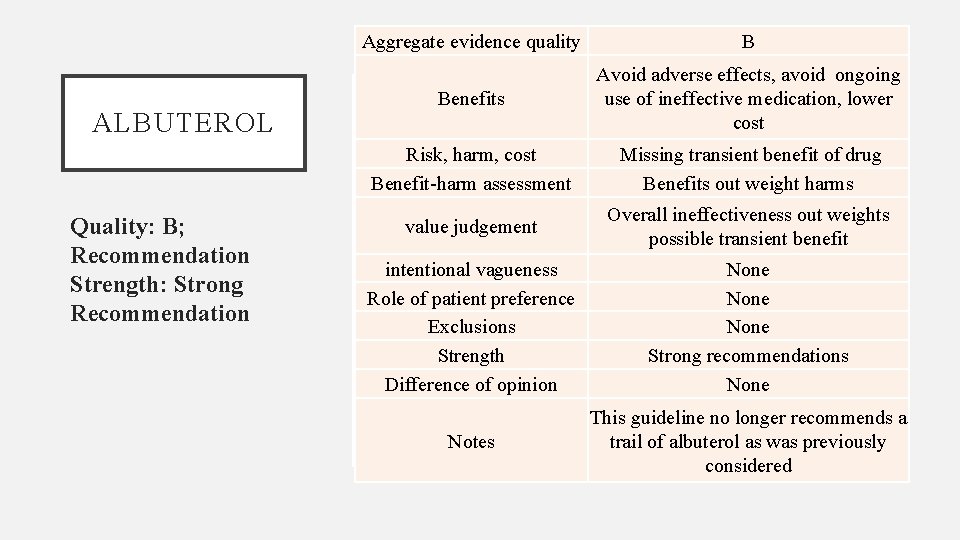

ALBUTEROL Quality: B; Recommendation Strength: Strong Recommendation Aggregate evidence quality B Benefits Avoid adverse effects, avoid ongoing use of ineffective medication, lower cost Risk, harm, cost Benefit-harm assessment Missing transient benefit of drug Benefits out weight harms value judgement Overall ineffectiveness out weights possible transient benefit intentional vagueness Role of patient preference Exclusions Strength Difference of opinion None Strong recommendations None Notes This guideline no longer recommends a trail of albuterol as was previously considered
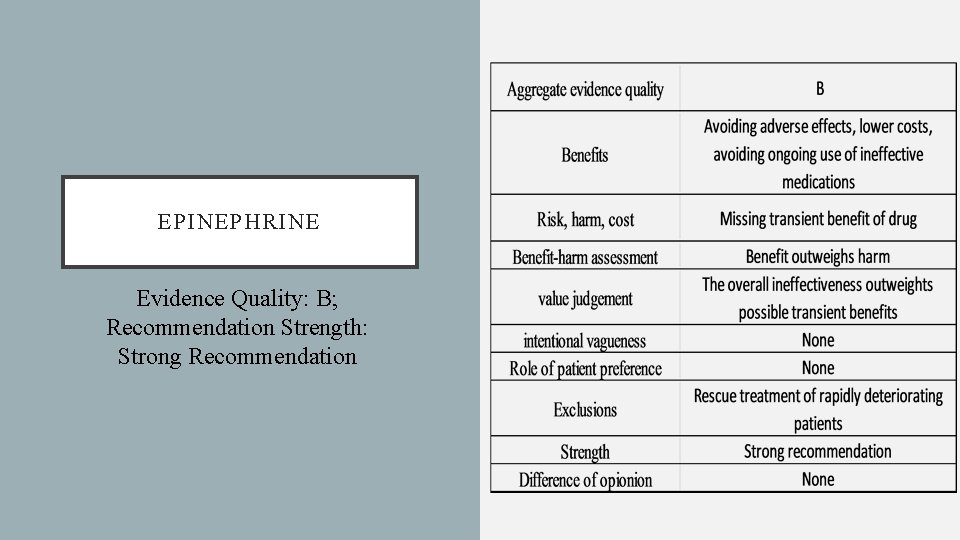

EPINEPHRINE Evidence Quality: B; Recommendation Strength: Strong Recommendation
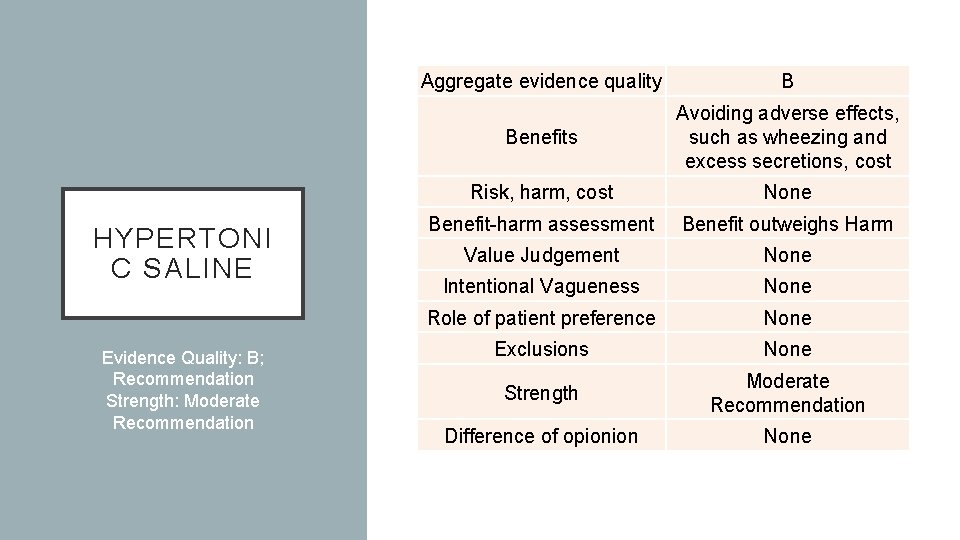
HYPERTONI C SALINE Evidence Quality: B; Recommendation Strength: Moderate Recommendation Aggregate evidence quality B Benefits Avoiding adverse effects, such as wheezing and excess secretions, cost Risk, harm, cost None Benefit-harm assessment Benefit outweighs Harm Value Judgement None Intentional Vagueness None Role of patient preference None Exclusions None Strength Moderate Recommendation Difference of opionion None
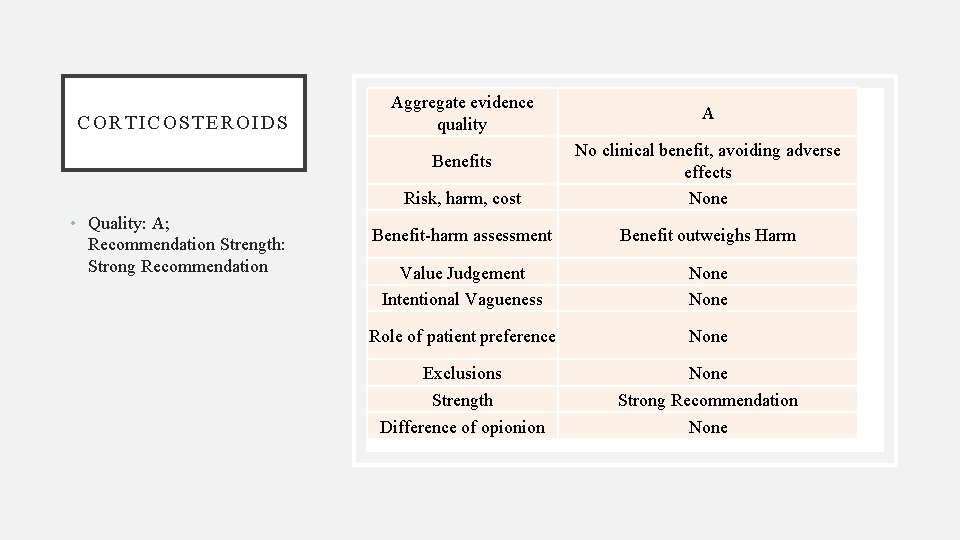

COR TICOSTEROIDS Aggregate evidence quality Risk, harm, cost No clinical benefit, avoiding adverse effects None Benefit-harm assessment Benefit outweighs Harm Value Judgement Intentional Vagueness None Role of patient preference None Exclusions Strength Difference of opionion None Strong Recommendation None Benefits • Quality: A; Recommendation Strength: Strong Recommendation A
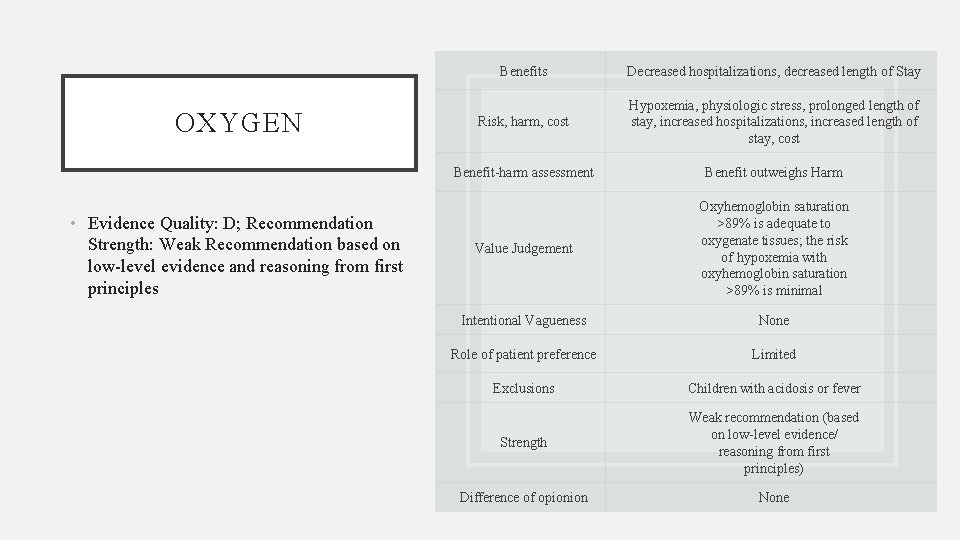

OXYGEN • Evidence Quality: D; Recommendation Strength: Weak Recommendation based on low-level evidence and reasoning from first principles Benefits Decreased hospitalizations, decreased length of Stay Risk, harm, cost Hypoxemia, physiologic stress, prolonged length of stay, increased hospitalizations, increased length of stay, cost Benefit-harm assessment Benefit outweighs Harm Value Judgement Oxyhemoglobin saturation >89% is adequate to oxygenate tissues; the risk of hypoxemia with oxyhemoglobin saturation >89% is minimal Intentional Vagueness None Role of patient preference Limited Exclusions Children with acidosis or fever Strength Weak recommendation (based on low-level evidence/ reasoning from first principles) Difference of opionion None
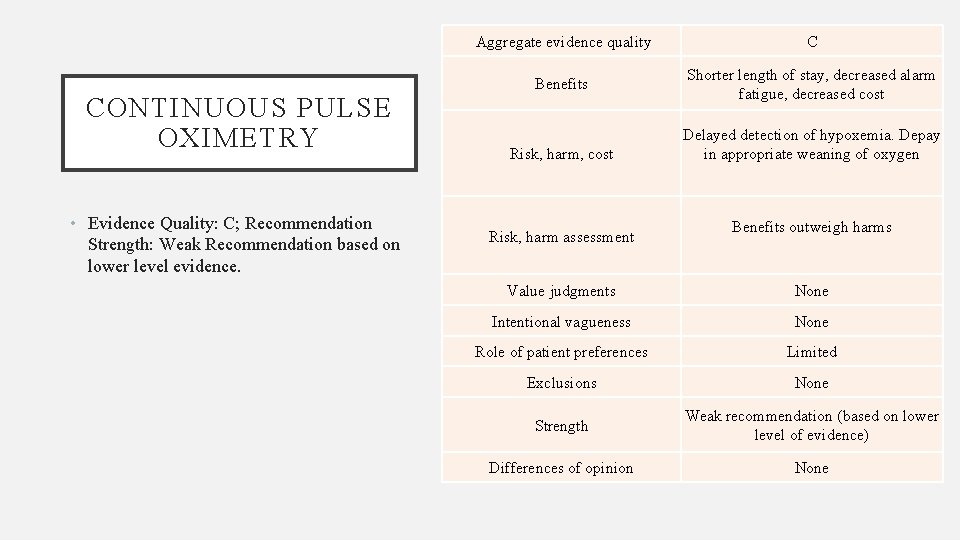
CONTINUOUS PULSE OXIMETRY • Evidence Quality: C; Recommendation Strength: Weak Recommendation based on lower level evidence. Aggregate evidence quality C Benefits Shorter length of stay, decreased alarm fatigue, decreased cost Risk, harm, cost Risk, harm assessment Delayed detection of hypoxemia. Depay in appropriate weaning of oxygen Benefits outweigh harms Value judgments None Intentional vagueness None Role of patient preferences Limited Exclusions None Strength Weak recommendation (based on lower level of evidence) Differences of opinion None
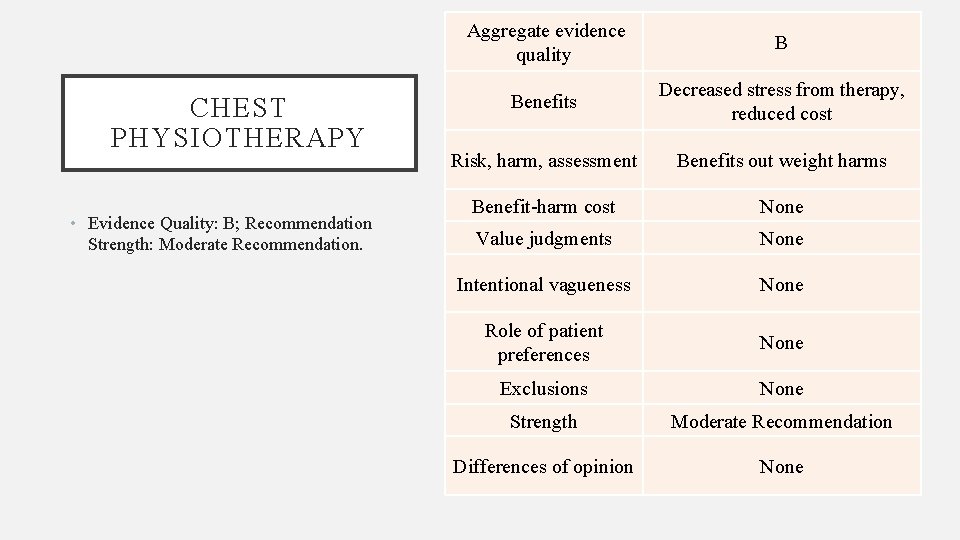
CHEST PHYSIOTHERAPY • Evidence Quality: B; Recommendation Strength: Moderate Recommendation. Aggregate evidence quality B Benefits Decreased stress from therapy, reduced cost Risk, harm, assessment Benefits out weight harms Benefit-harm cost None Value judgments None Intentional vagueness None Role of patient preferences None Exclusions None Strength Moderate Recommendation Differences of opinion None
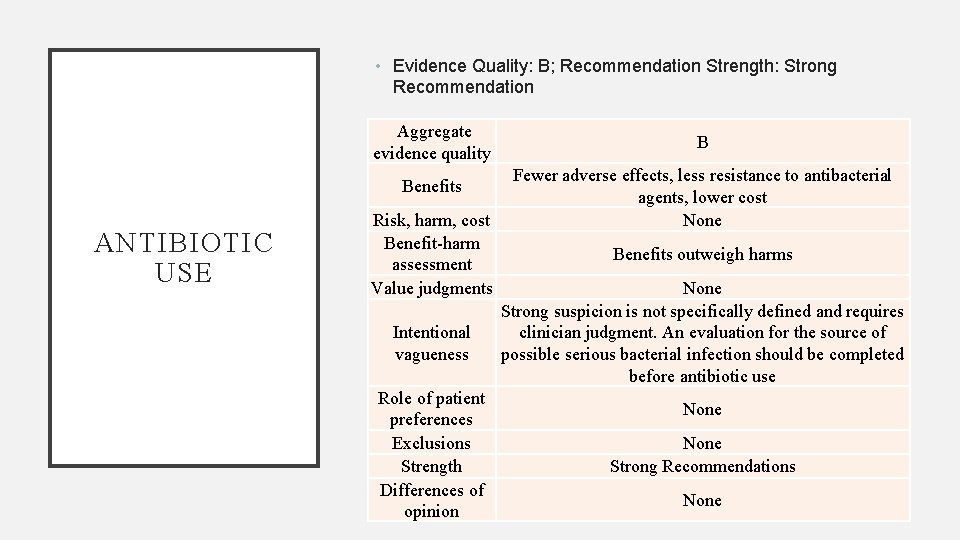
• Evidence Quality: B; Recommendation Strength: Strong Recommendation Aggregate evidence quality Benefits ANTIBIOTIC USE Risk, harm, cost Benefit-harm assessment Value judgments Intentional vagueness Role of patient preferences Exclusions Strength Differences of opinion B Fewer adverse effects, less resistance to antibacterial agents, lower cost None Benefits outweigh harms None Strong suspicion is not specifically defined and requires clinician judgment. An evaluation for the source of possible serious bacterial infection should be completed before antibiotic use None Strong Recommendations None
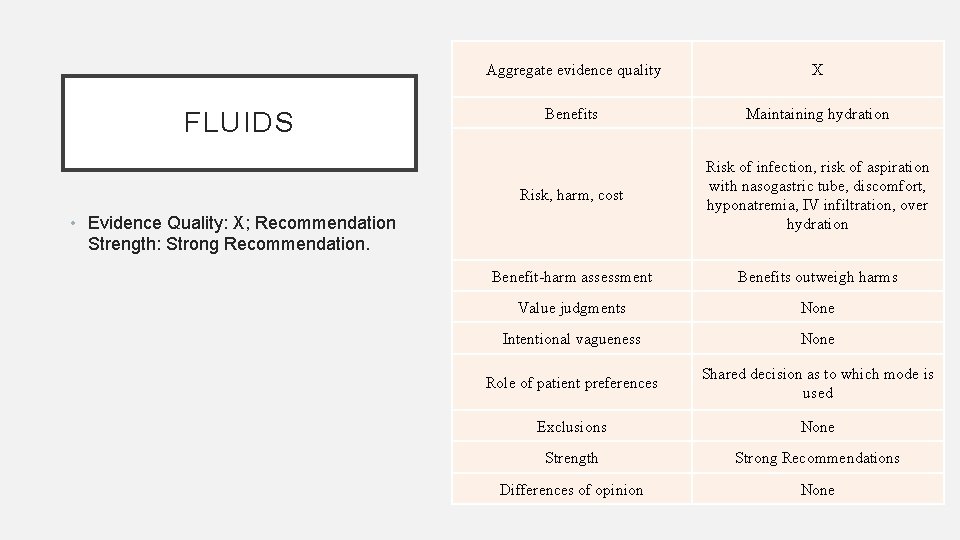
FLUIDS Aggregate evidence quality X Benefits Maintaining hydration Risk, harm, cost Risk of infection, risk of aspiration with nasogastric tube, discomfort, hyponatremia, IV infiltration, over hydration Benefit-harm assessment Benefits outweigh harms Value judgments None Intentional vagueness None Role of patient preferences Shared decision as to which mode is used Exclusions None Strength Strong Recommendations Differences of opinion None • Evidence Quality: X; Recommendation Strength: Strong Recommendation.

PALIVIZUMAB Evidence Quality: B; Recommendation Strength: Strong Recommendation. • No evidence suggests palivizumab is a costeffective measure to prevent recurrent wheezing in children. • Prophylaxis should not be administered to reduce recurrent wheezing in later years.
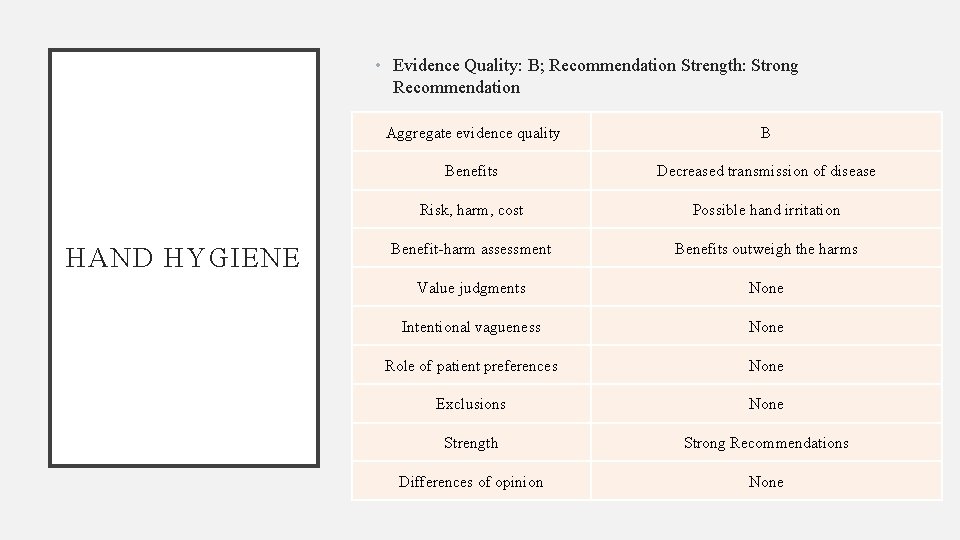
• Evidence Quality: B; Recommendation Strength: Strong Recommendation HAND HYGIENE Aggregate evidence quality B Benefits Decreased transmission of disease Risk, harm, cost Possible hand irritation Benefit-harm assessment Benefits outweigh the harms Value judgments None Intentional vagueness None Role of patient preferences None Exclusions None Strength Strong Recommendations Differences of opinion None
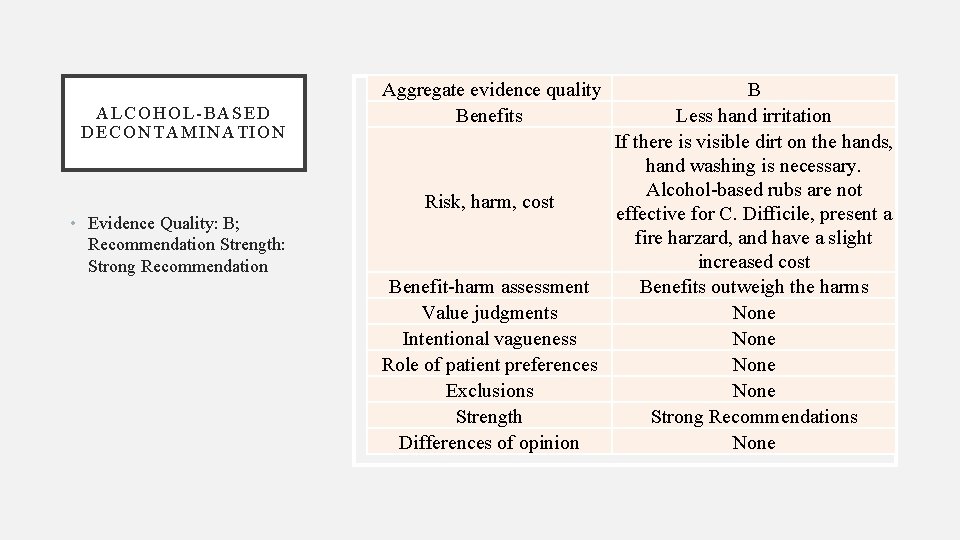
ALCOHOL-BASED DECONTAMINATION • Evidence Quality: B; Recommendation Strength: Strong Recommendation Aggregate evidence quality Benefits B Less hand irritation If there is visible dirt on the hands, hand washing is necessary. Alcohol-based rubs are not Risk, harm, cost effective for C. Difficile, present a fire harzard, and have a slight increased cost Benefit-harm assessment Benefits outweigh the harms Value judgments None Intentional vagueness None Role of patient preferences None Exclusions None Strength Strong Recommendations Differences of opinion None
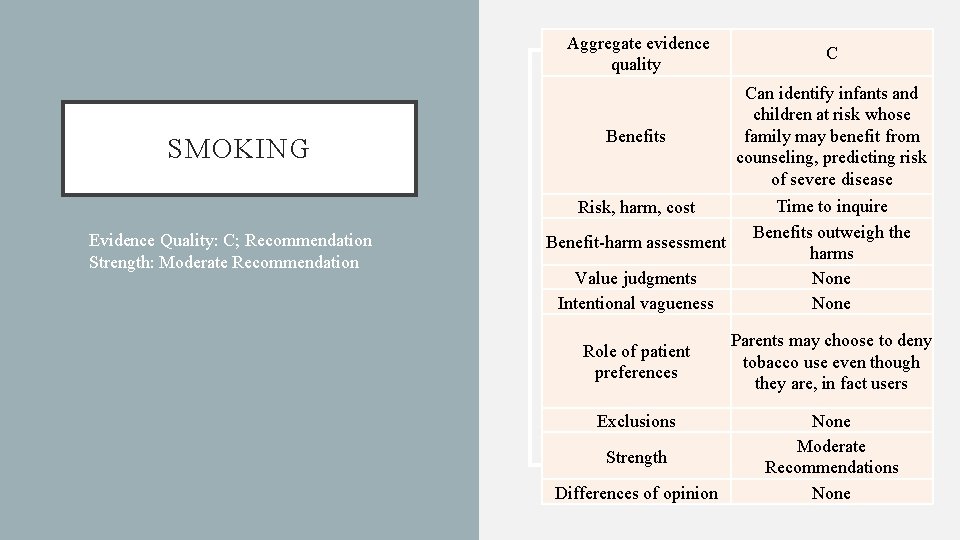
Aggregate evidence quality SMOKING • Evidence Quality: C; Recommendation Strength: Moderate Recommendation C Can identify infants and children at risk whose Benefits family may benefit from counseling, predicting risk of severe disease Time to inquire Risk, harm, cost Benefits outweigh the Benefit-harm assessment harms Value judgments None Intentional vagueness None Role of patient preferences Exclusions Strength Differences of opinion Parents may choose to deny tobacco use even though they are, in fact users None Moderate Recommendations None
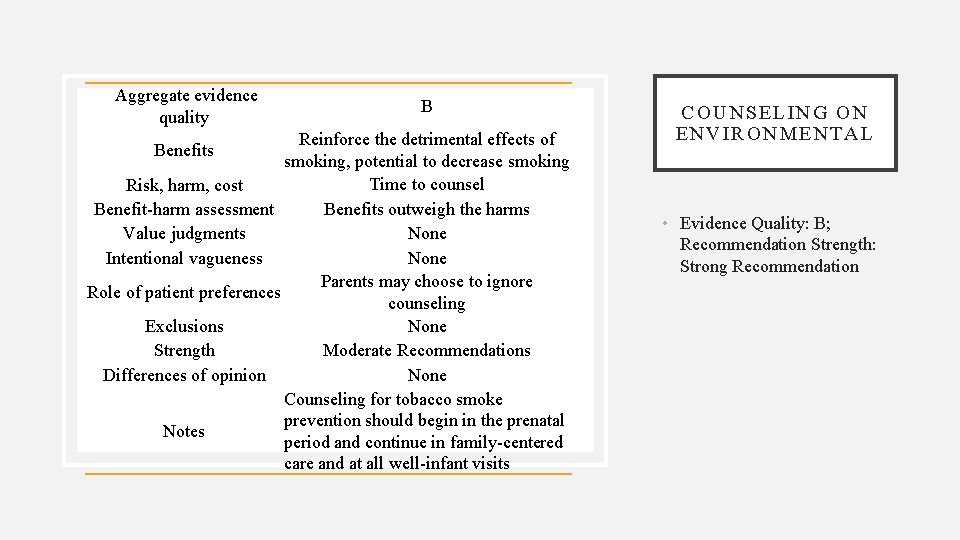

Aggregate evidence quality B Reinforce the detrimental effects of smoking, potential to decrease smoking Time to counsel Risk, harm, cost Benefit-harm assessment Benefits outweigh the harms Value judgments None Intentional vagueness None Parents may choose to ignore Role of patient preferences counseling Exclusions None Strength Moderate Recommendations Differences of opinion None Counseling for tobacco smoke prevention should begin in the prenatal Notes period and continue in family-centered care and at all well-infant visits Benefits COUNSELING ON ENV IRONMEN TAL • Evidence Quality: B; Recommendation Strength: Strong Recommendation
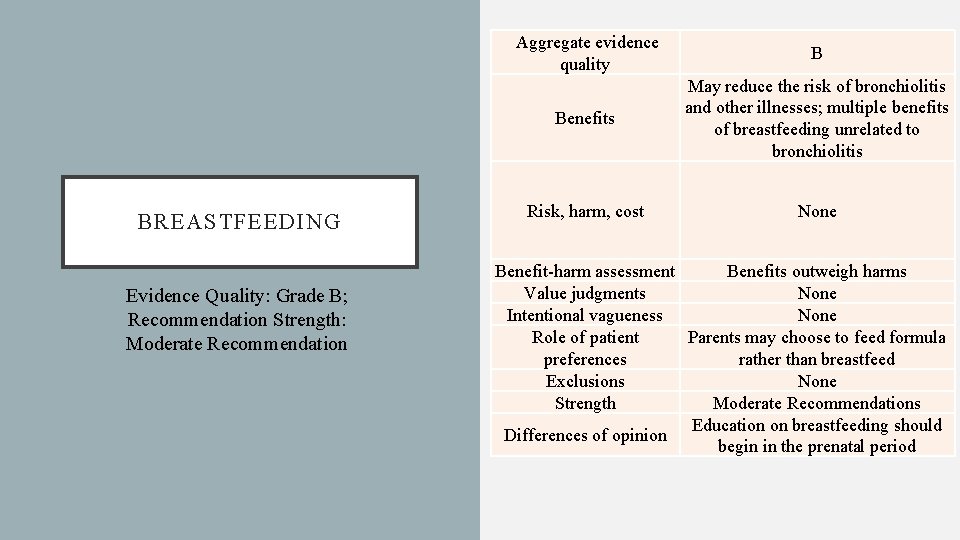
BREASTFEEDING Evidence Quality: Grade B; Recommendation Strength: Moderate Recommendation Aggregate evidence quality B Benefits May reduce the risk of bronchiolitis and other illnesses; multiple benefits of breastfeeding unrelated to bronchiolitis Risk, harm, cost None Benefit-harm assessment Benefits outweigh harms Value judgments None Intentional vagueness None Role of patient Parents may choose to feed formula preferences rather than breastfeed Exclusions None Strength Moderate Recommendations Education on breastfeeding should Differences of opinion begin in the prenatal period

FAMILY EDUCATION Evidence Quality: C; observational studies; Recommendation Strength; Moderate Recommendation Aggregate evidence quality C Benefits Decrease transmission of disease, benefits of breastfeeding promotion of judicious use of antibiotics, risks of infant lung damage attributable to tobacco smoke Risk, harm, cost Time to educate properly Benefit-harm assessment Benefits outweigh harms Value judgments None Personnel is not speifically defined but should include all people who enter a patient's room Intentional vagueness Role of patient preferences Exclusions None Strength Moderate Recommendations Differences of opinion None

• Better algorithms for predicting the course of illness • Impact of clinical score on patient outcomes • Evaluating different ethnic groups and varying response to treatments FUT URE RESEARCH NE EDS • Does epinephrine alone reduce admission in outpatient settings? • Additional studies on epinephrine in combination with dexamethasone or other corticosteroids • Hypertonic saline studies in the outpatient setting and in in hospitals with shorter LOS • More studies on nasogastric hydration • More studies on tonicity of intravenous fluids

• Incidence of true AOM in bronchiolitis by using 2013 guideline definition • More studies on deep suctioning and nasopharyngeal suctioning • Strategies for monitoring oxygen saturation • Use of home oxygen FUTURE RESEARCH NEEDS • Appropriate cutoff for use of oxygen in high altitude • Oxygen delivered by high-flow nasal cannula • RSV vaccine and antiviral agents • Use of palivizumab in special populations, such as cystic fibrosis, neuromuscular diseases, Down syndrome, immune deficiency • Emphasis on parent satisfaction/ patient-centered outcomes in all research (ie, not LOS as the only measure)

REFERENCE Ralston, S. L. , Lieberthal, A. S. , Meissner, C. , Alverson, J. E. , Baley, J. E. , Gadomski, A. m. , Johnson, D. W. , Light, M. J. , Maraqa, N. F. , Mendonca, E. A. , Phelan, K. J. , Zorc, J. J. , Stanko. Lopp, D. , Brown, M. A. , Nathanson, I. , Rosenblum, E. , Sayles, S. , and Hernandez-Cancio, S. (2014). Clinical practice guideline: The diagnosis, management, and prevention of bronchiolitis. Pediatrics. 134. e 1474 -1501.
- Slides: 30