Josep Vidal Alaball HCE OSTEOARTHRITIS Commonest condition to
Josep Vidal Alaball HCE

OSTEOARTHRITIS • Commonest condition to affect synovial joints • Single most important cause of locomotor disability • Previously considered a degenerative disease, inevitable consequence of ageing and trauma • Now viewed as a metabolically dynamic, essentially reparative process.
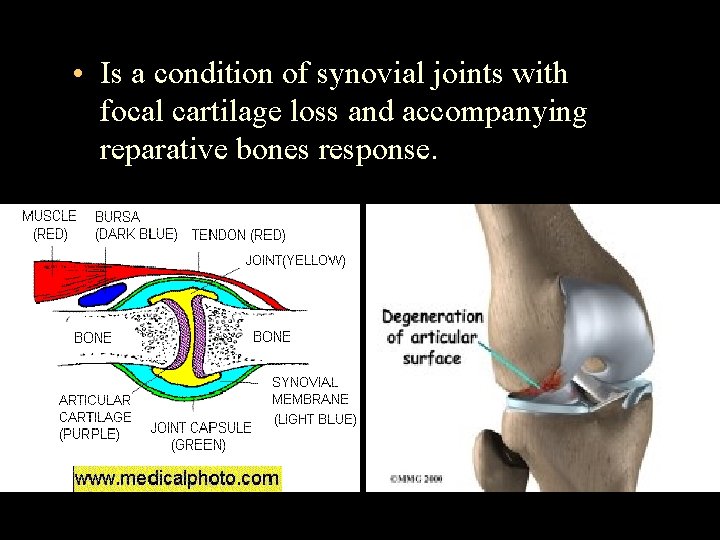
• Is a condition of synovial joints with focal cartilage loss and accompanying reparative bones response.

• In most cases this slow but metabolically active process keeps pace with various triggering insults and is non-progressive. • But sometimes it fails to compensate, resulting in joint failure. • Various extrinsic and intrinsic insults cause different patterns of arthritis, and multiple constitutional and environmental factors modify response and outcome.
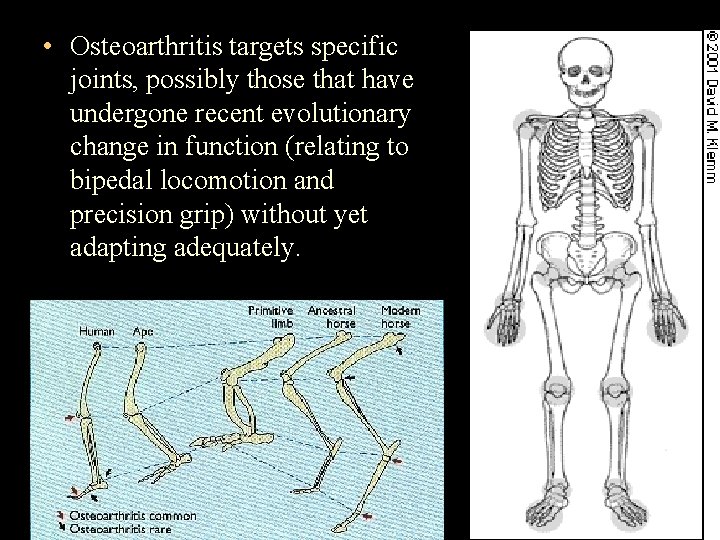
• Osteoarthritis targets specific joints, possibly those that have undergone recent evolutionary change in function (relating to bipedal locomotion and precision grip) without yet adapting adequately.

ASSESSMENT • For many plain radiograph remains the best means of assessment: – Evidence of cartilage loss (joint space narrowing) – Bone response (osteophytes and sclerosis) • There is often considerable discordance between structural change and clinical outcome
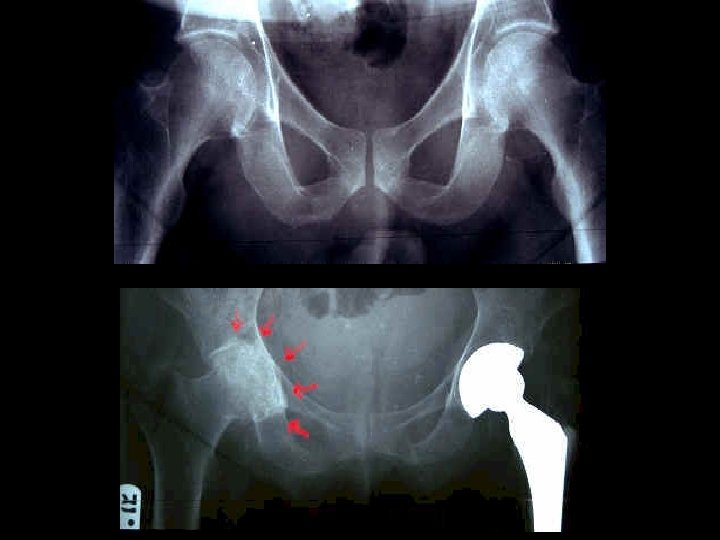
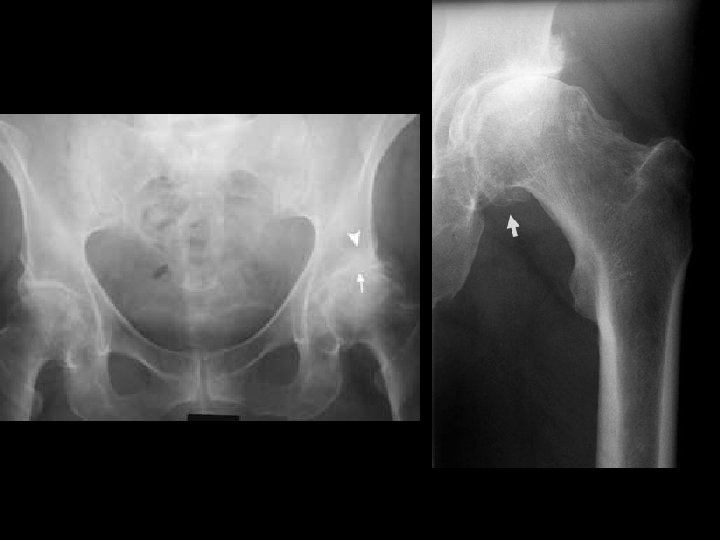
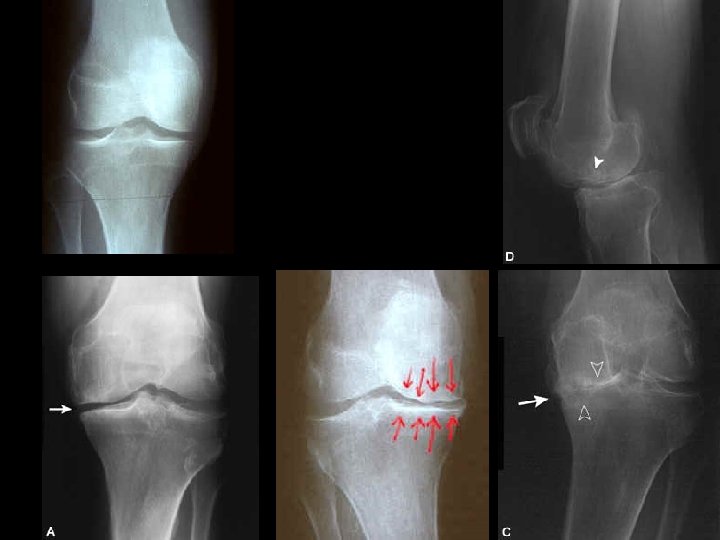

RISK FACTORS 1. AGE – NOT and inevitable consequence of ageing, BUT strongly related to age – Uncommon in people under 45 – Prevalence increases up to age 65, when al least 50% of people have RX evidence of OA in at least one joint group – May represent cumulative insult to the joint, possibly aggravated by decline in neuromuscular function

2. SEX – Pronounced FEMALE preponderance in – hands and knee 3. ETHNIC GROUP – Uncommon in Black and Asian populations – This seems to reflect genetic rather than cultural differences

4. INDIVIDUAL RISK FACTORS – Generalised factors • Obesity • Genetic factors • Female – Localised factors E. g. : • Meniscectomy • Instability • Dysplasia

TYPES OF OA 1. NODAL GENERALISED OA • Characterised by multiple Heberden´s nodes (distal interphalangeal joint) and Bouchard´s nodes (interphalangeal joint) • Symptoms usually starting around menopause • Aetiology unknown
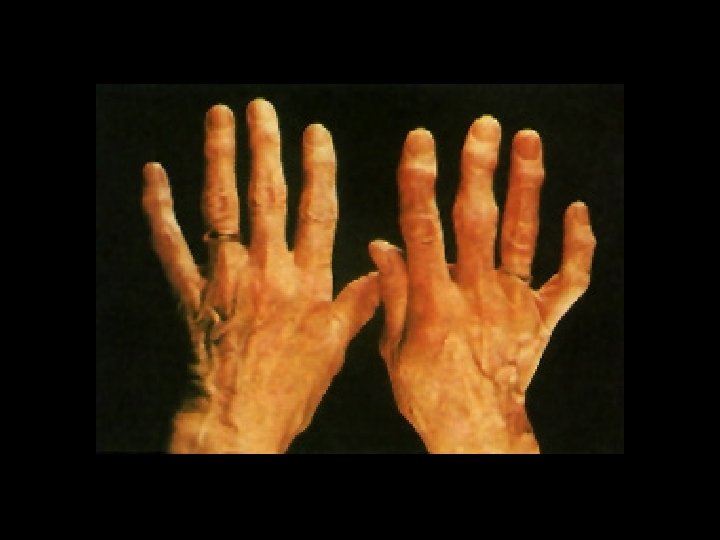

2. CRISTAL ASSOCIATED OA • Calcium crystals, notably calcium pyrophospate dyhidrate and apatite, may deposit in cartilage. • Predominantly in elderly women, affecting the knee

3. OA OF PREMATURE ONSET • Development of single joint OA after severe trauma is not uncommon • Premature onset in multiple joints may be a presenting feature of other conditions: – – – Haemochromatosis Ochronosis Acromegaly Thiemann’s disease Hereditary type II collagen defects Endemic OA

CLINICAL FEATURES • PAIN – Typically sharp pain on using the joint or dull ache which may occur at rest or during the night – Greatly influenced by personality, anxiety, depression and daily activity • GELLING OF JOINTS – Stiffness after immobility, morning stiffness lasting no more than 30 min. • FUNCTIONAL IMPAIRMENT

• • • CREPITUS BONY ENLARGEMENT DEFORMITY INSTABILITY SYNOVITIS MUSCLE WEAKNESS OR WASTING

THERAPEUTIC OPTIONS • Non-pharmacological treatment – Education (patient and spouse or family) – Social support (telephone contact) – Physiotherapy (aerobic exercises, muscle strengthening, and patellar strapping) – Occupational therapy (aids and appliances, joint protection) – Weight loss – Acupuncture – Transcutaneous electrical nerve stimulation (TENS)

• Pharmacological treatment – Simple analgesia – Non-steroidal anti-inflammatory drugs – COX-2 inhibitors (cyclo-oxygenase-2 selective non-steroidal anti-inflammatory drugs) – Topical (NSAID drugs, capsaicin) – Chondroprotective agents • Intra-articular treatment – Corticosteroids – Hyaluronans – Tidal irrigation

PATIENT EDUCATION • Trials contrasting education vs. effects of NSAIDs confirmed a significant beneficial effect on education in joint pain but not on disability. • Any member of the care team can provide education in several forms: literature, audiocassette, computer… • Emphasise weight reduction and exercise

SOCIAL SUPPORT • In OA of the knee controlled studies have shown that regular telephone contact from healthcare produces significant improvement in pain and function OCCUPATIONAL THERAPY • Walking aids, orthoses, splints

PHYSICAL THERAPY • Muscle strengthening programmes – Specific for certain joints – Shown to improve pain and disability in OA of the knee • TENS (transcutaneous electrical nerve stimulation) – Modest pain relief compared with placebo • Acupuncture

Changes in lifestyle for patients with OA • General measures – Maintain optimal weight – Encourage activity and regular general exercise – Maintain positive approach • Specific measures – Strengthening of local muscles – Use of appropriate footwear and walking aids – Pay attention to specific problems caused by disability (such as shopping, housework, and job)

ANALGESICS, NSAIDs, COX-2 i • PARACETAMOL – It is safe and effective – Slight benefit from addition of dextropropoxyphene • NSAIDs – More effective than placebo in reducing pain and improving function – Few studies have lasted longer than 2 years – No evidence they affect progression of OA

– Evidence that MISOPROSTOL and PPI reduce risk of upper GI injury – Cost utility of prophylactic use is controversial – Recommended to initiate NSAIDs only after consideration of side effects – Prescription should be reviewed every 6 months • COX-2 INHIBITORS – Published data remains scarce – Trials have shown similar efficacy to NSAIDs with GI toxicity comparable with placebo – Cost effective strategy for their use far from clear

Relative contraindications to starting treatment with NSAIDs * Gastrointestinal toxicity. Caution in: - Those aged >65 years - Patients with a history of peptic ulcer disease - Concomitant treatment with corticosteroids and anticoagulants - Smokers - Patients with cardiovascular disease - Heavy alcohol drinkers * Renal toxicity. Caution in: - Those aged >65 years - Patients with hypertension - Patients with congestive cardiac failure - Concomitant medication with ACE inhibitors and diuretics

TOPICAL TREATMENT • NSAIDs and CAPSAICIN – Strong evidence that they are effective and safe – Fewer side effects probably should be used more often – However substantial doubt as their superiority over simple rubefacients

INTRA-ARTICULAR THERAPY • CORTICOSTEROIDS – Use controversial in uncomplicated OA – Superior short term efficacy to intra-articular placebo – Benefits last 2 to 4 weeks – Indicated in patients with acute crystal associated synovitis and those unfit for or awaiting surgery – Potential for multiple injections to accelerate cartilage damage

• HYALURONIC ACID – In people with OA there is a reduced concentration of this acid – Trials suggest superior pain relief to placebo and equivalent to corticosteroids injections with greater duration of action • TIDAL IRRIGATION – Irrigation of knee joint with saline – Trials suggest some role in treatment of knee OA

CHONDROPROTECTIVE AGENTS • Clinical trials provide some justification for the use of CHONDROITIN and GLUCOSAMINE preparations but only for their analgesic or anti-inflammatory effects
SURGERY • JOINT REPLACEMENTS • ARTHROSCOPIC LAVAGE • OSTEOTOMY • ARTHRODESIS
THE END
- Slides: 33