Joint Hospital Surgical Ground Round April 2014 Hwang


















- Slides: 25

Joint Hospital Surgical Ground Round April 2014 Hwang Wan Wui Winston Queen Elizabeth Hospital

Presentation Outline Chicago Classification Scheme High Resolution Esophageal Pressure Topography Achalasia Presentation Investigation Treatment

Chicago Classification Scheme High Resolution Esophageal Pressure Topography Achalasia Presentation Investigation Treatment

The Chicago Classification Investigators in the Northwestern University in Chicago developed a new classification scheme to facilitate the diagnosis of esophageal motility disorders by interpretation of high resolution esophageal pressure topography (EPT) Esophageal pressure topography is a combination of high resolution manometry (HRM) and pressure topography

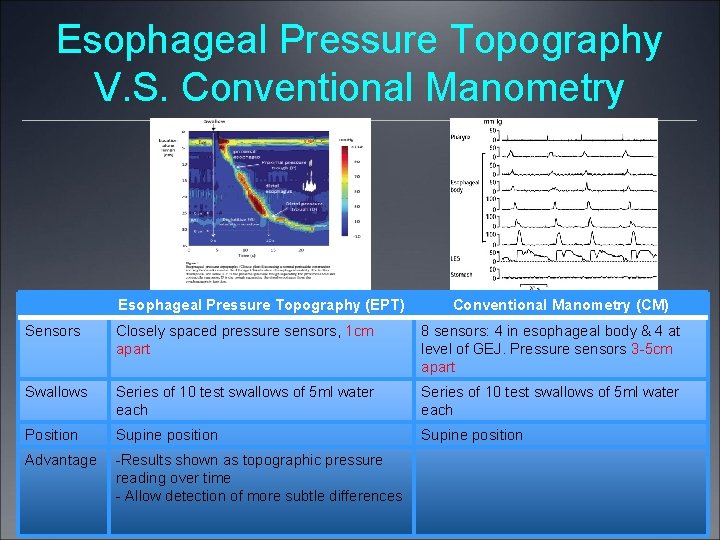
Esophageal Pressure Topography V. S. Conventional Manometry Esophageal Pressure Topography (EPT) Conventional Manometry (CM) Sensors Closely spaced pressure sensors, 1 cm apart 8 sensors: 4 in esophageal body & 4 at level of GEJ. Pressure sensors 3 -5 cm apart Swallows Series of 10 test swallows of 5 ml water each Position Supine position Advantage -Results shown as topographic pressure reading over time - Allow detection of more subtle differences

The Chicago Classification EPT Metrics Metric IRP Integrated Relaxation Pressure DCI Distal Contractile Integral CDP Contractile Deceleration Point Description Mean of the lowest EGJ pressure over 4 seconds measured in the ten-second window after deglutitive UES relaxation Volume (amplitude x duration x length) from proximal to distal pressure troughs Transition from peristaltic propagation to late phase of esophageal emptying (proceeds much more slowly) CFV Contractile Front Velocity Slope between the proximal pressure troughs and CDP DL Distal Latency Interval between UES relaxation and the CDP, duration of peristalsis Peristaltic Breaks Gaps of the peristaltic contraction between the UES and EGJ Each metric developed to characterize a specific feature of deglutitive esophageal function

Esophageal Pressure Topography V. S. Conventional Manometry Esophageal Motility EPT Characteristic CM LES Relaxation 1. Integrated Relaxation Pressure (IRP) <15 mm. Hg 1. LES relaxation <8 mm. Hg more than gastric pressure Peristaltic Propagation 2. Contractile Deceleration Point (CDP) No corresponding 3. Contractile Front Velocity (CFV) 2. Wave progression between pressure sensors 8 and 3 cm above the LES 4. Distal Latency (DL) No corresponding Contractile Vigor 5. Distal contractile Integral 3. Peristaltic amplitude (DCI) EPT allows more sophisticated interpretation of esophageal motility

The Chicago Classification IRP >= >= upper limit of of normal AND absent peristalsis YES Achalasia Type I: Classic Type II: Pan-esophageal pressurization Type III: Spastic NO IRP >= upper limit of normal AND some instances of intact or weak peristalsis NO YES IRP is normal BUT abnormalities in other metrics YES EGJ Outflow Obstruction Achalasia variant Mechanical obstruction Other Esophageal Motility Disorders Distal esophageal spasm Hypercontractile esophagus Absent peristalsis Nutcracker esophagus

Chicago Classification Scheme High Resolution Esophageal Pressure Topography Achalasia Presentation Investigation Treatment

Achalasia - Presentation Dysphagia both liquid and solid Regurgitation Chest pain Cough Aspiration pneumonia Weight loss

Achalasia - Investigations Barium Esophagogram Classical “bird’s beak” appearance Dilated esophageal body High Resolution Manometry Esophagogastroduodenoscopy Rule out pseudoachalasia Most common cause is malignancy infiltrating the EGJ

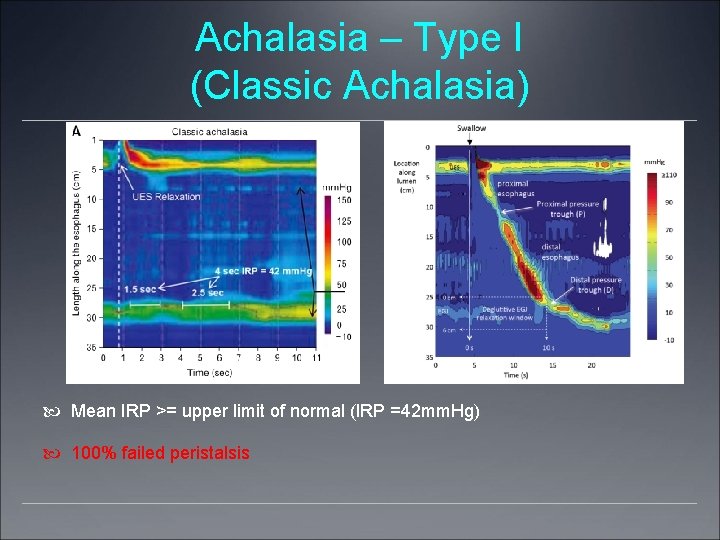
Achalasia – Type I (Classic Achalasia) Mean IRP >= upper limit of normal (IRP =42 mm. Hg) 100% failed peristalsis

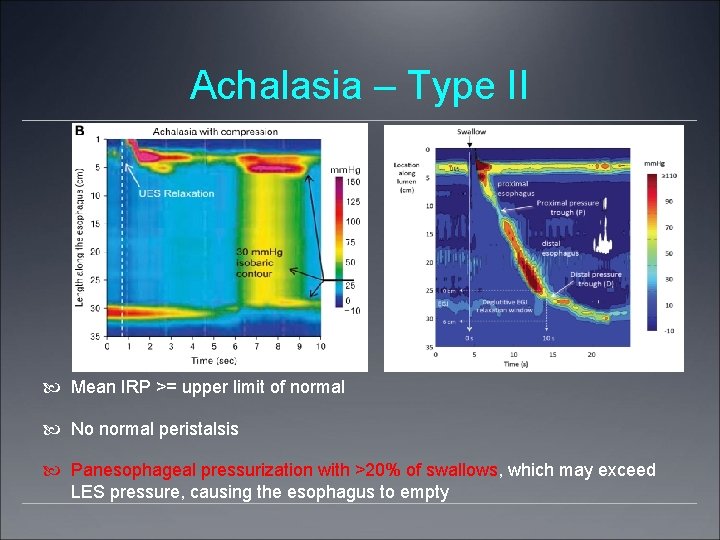
Achalasia – Type II Mean IRP >= upper limit of normal No normal peristalsis Panesophageal pressurization with >20% of swallows, which may exceed LES pressure, causing the esophagus to empty

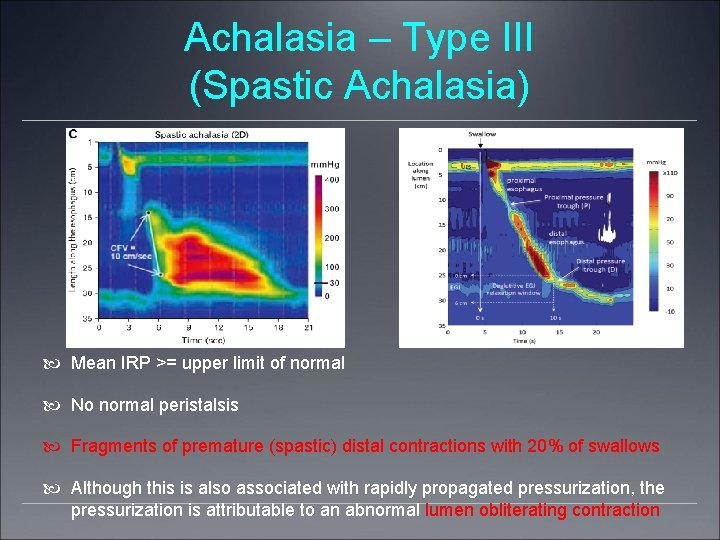
Achalasia – Type III (Spastic Achalasia) Mean IRP >= upper limit of normal No normal peristalsis Fragments of premature (spastic) distal contractions with 20% of swallows Although this is also associated with rapidly propagated pressurization, the pressurization is attributable to an abnormal lumen obliterating contraction

Achalasia Treatment Pharmacological Calcium channel blockers and nitrates short lived response side effects: headache, dizziness and pedal edema Botulin toxin injection prevents the release of acetylcholine at terminal nerve endings results last 6 -9 months. [1] Pharmacological therapies are less effective than endoscopic or surgical therapies [1] Pasricha PJ, Ravich WJ, Hendrix TR, Sostre S, Jones B, Kal- loo AN. Intrasphincteric botulinum toxin for the treatment of achalasia. N Engl J Med 1995; 332: 774 -778

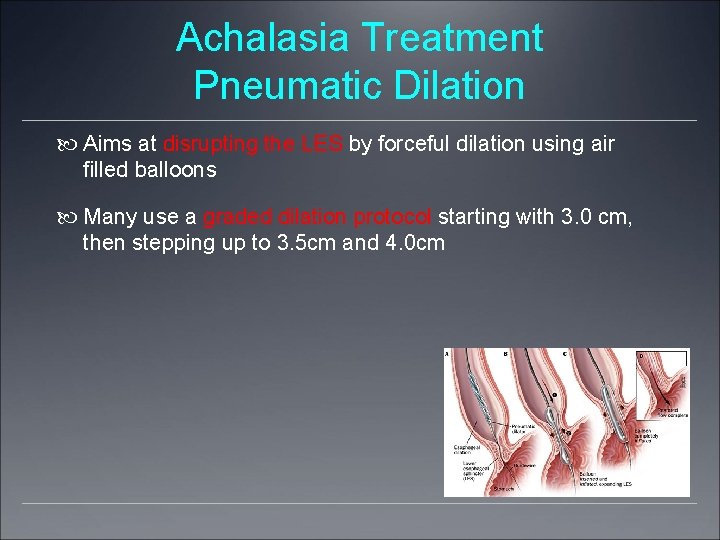
Achalasia Treatment Pneumatic Dilation Aims at disrupting the LES by forceful dilation using air filled balloons Many use a graded dilation protocol starting with 3. 0 cm, then stepping up to 3. 5 cm and 4. 0 cm

Achalasia Treatment Pneumatic Dilation Promising short term results Long term follow-up showed recurrence Author, Journal Study Design N No. of PD Results Eckardt VF, et al Gut 2004 [1] Prospective cohort 54 1 5 year remission rate 40% 10 year remission rate 36% Katsinelos P, et al Prospective World J Gastroenterol cohort 2005 [2] 39 1 -3 5 year remission 78% 10 year remission 61% 15 year remission 58. 3% [1] Eckardt VF, Gockel I, Bernhard G. Pneumatic dilation for achalasia: late results of a prospective follow up investigation. Gut 2004; 53: 629 -633 [2] Katsinelos P, Kountouras J, Paroutoglou G, Beltsis A, Zavos C, Papaziogas B, Mimidis K (2005) Long-term results of pneu- matic dilation for achalasia: a 15 years’ experience. World J Gastroenterol 11: 5701– 5705

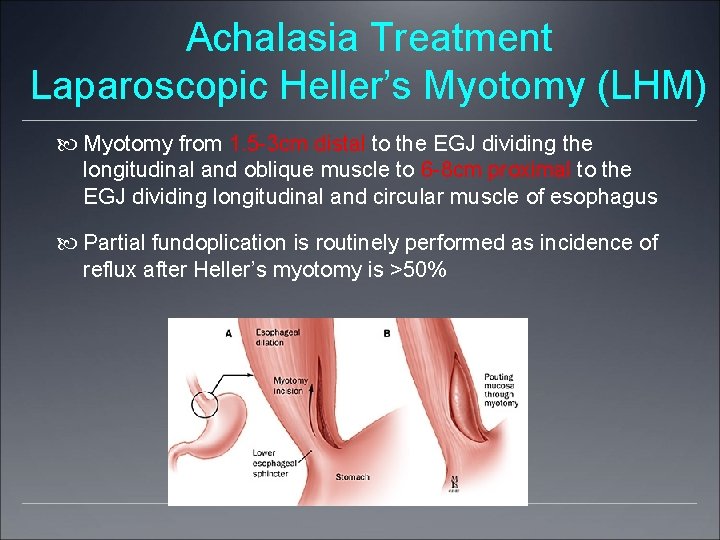
Achalasia Treatment Laparoscopic Heller’s Myotomy (LHM) Myotomy from 1. 5 -3 cm distal to the EGJ dividing the longitudinal and oblique muscle to 6 -8 cm proximal to the EGJ dividing longitudinal and circular muscle of esophagus Partial fundoplication is routinely performed as incidence of reflux after Heller’s myotomy is >50%

Achalasia Treatment Laparoscopic Heller’s Myotomy (LHM) LHM considered superior to pneumatic dilation and the first choice of treatment for achalasia Prospective trials have shown promising long term results of LHM A prospective trial in Italy followed up 6 years after laparoscopic Heller-Dor operation [1] Primary outcome was therapeutic success in terms of symptoms improvement At 6 years, 81. 7% of patients still have significant improvement in their symptoms [1] Costantini M, Zaninotto G, Guirroli E, et al. The laparoscopic Heller-Dor operation remains an effective treatment for esophageal achalasia at a minimum 6 -year follow-up. Surg Endosc 2005; 19: 345 -51

Achalasia Treatment Laparoscopic Heller’s Myotomy (LHM) Multicenter RCT published by European Achalasia Trial group in 2011 [1] Primary outcome was therapeutic success, measured by Eckardt score After 2 years of follow up, the study concluded LHM was not superior to pneumatic dilation Limitations: 2 year cohort study with no evidence on intermediate and long-term remission rates All patients in the PD group received 2 to 3 sessions of redilation [1] Boeckxstaens GE, Annese V, des Varannes SB, Chaussade S, Costantini M, Cuttitta A, Elizalde JI, Fumagalli U, Gaudric M, Rohof WO, Smout AJ, Tack J, Zwinderman AH, Zaninotto G, Busch OR. Pneumatic dilation versus laparoscopic Heller’ s myotomy for idiopathic achalasia. N Engl J Med 2011; 364: 1807 -1816

Achalasia Treatment in Different Subtypes Author Journal Study Type N Follow up Results Pandolfino JE, et al Gastroenterology 2008 [1] Retrospective cohort 213 3 years Salvador R, et al J Gastrointest. Surg 2010 [2] Prospective cohort 246 31 months - Treatment failure rates: -Type I 14. 6%; Type II 4. 7% ; Type III 30. 4% - Type II and LES resting pressure >30 mm. Hg were independent predictors of positive outcome Rohof WO, et al Gastroenterology 2013 [3] Multicenter RCT 176 2 years -Type II achalasia more likely to respond to any therapy -Type II (Botox 71%, pneumatic dilation 91%, Heller’s myotomy 100%) -Type I (56% overall) -Type III (29% overall) Treatment success rates: -Type I 81%; Type II 96%; Type III 66% Type II: success rate for PD was significantly higher than LHM [1] Pandolfino JE, Kwiatek MA, Nealis T, Bulsiewicz W, Post J, Kahrilas PJ. Achalasia: a new clinically relevant classification by high-resolution manometry. Gastroenterology 2008; 135: 1526 -1533. [2] Salvador R, Costantini M, Zaninotto G, et al. The preoperative manometric pattern predicts the outcome of surgical treatment for esophageal achalasia. J Gastrointest Surg 2010; 14: 1635– 1645 [3] Rohof WO, Salvador R, Annese V, et al. Outcomes of treatment for achalasia depend on manometric subtype. Gastroenterology 2013; 144: 718– 725

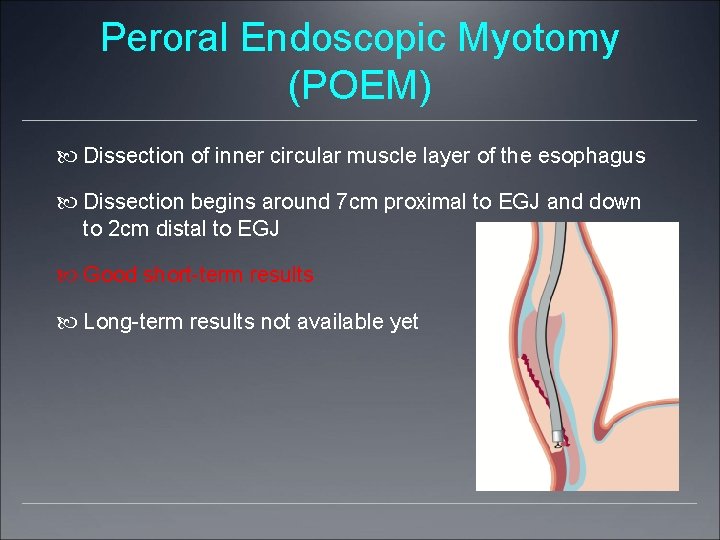
Peroral Endoscopic Myotomy (POEM) Dissection of inner circular muscle layer of the esophagus Dissection begins around 7 cm proximal to EGJ and down to 2 cm distal to EGJ Good short-term results Long-term results not available yet

Conclusion Pharmacological therapies are not recommended unless patient is not fit for endoscopic or surgical therapies Pneumatic dilation is the most effective nonsurgical treatment with promising short term results but high recurrence rate in the long term Laparoscopic Heller’s myotomy should be advocated for patients fit for surgery The Chicago Classification Scheme is providing a better classification for esophageal motility disorders. It has great impact on how we approach esophageal motility disorders, predict treatment outcomes and choose treatment options

Winston Hwang Queen Elizabeth Hospital

References Goldblum JR, Rice TW, Richter JE. Histopathologic features in esophagomyotomy specimens from patients with achala- sia. Gastroenterology 1996; 111: 648 -654 Richter JE. Achalasia – An Update. J Neurogastroenterol Motil. Jul 2010; 16(3): 232– 242 Boeckxstaens GE, etal. Achalasia. Lancet 2014; 383: 83 -93 Stefanidis D, et al. SAGES guidelines of the surgical treatment of esophageal achalasia. Surg Endosc 2012; 26: 296 -311