JMP Using to Develop and Execute an Administrative
- Slides: 2

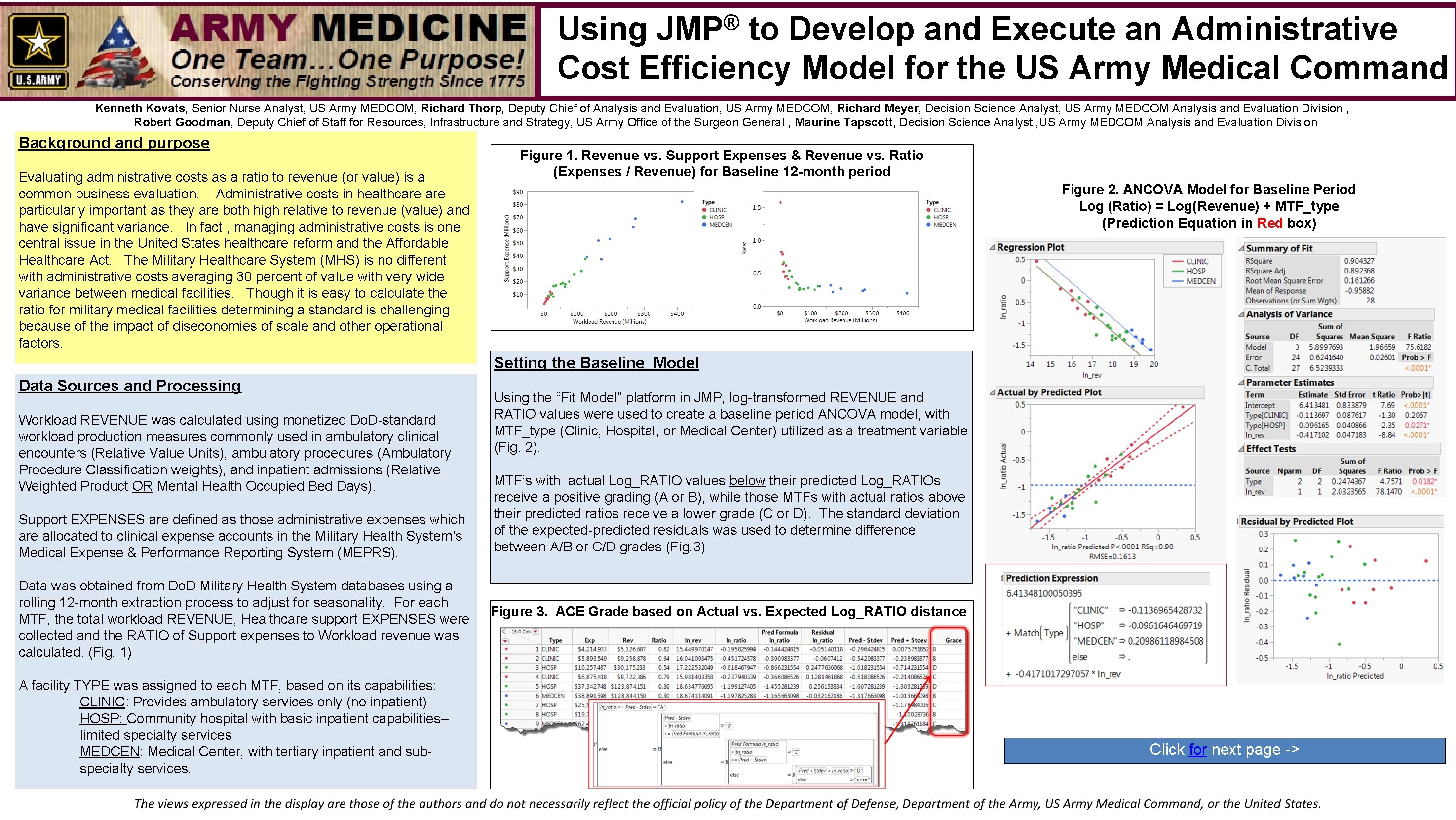
® JMP Using to Develop and Execute an Administrative Cost Efficiency Model for the US Army Medical Command Kenneth Kovats, Senior Nurse Analyst, US Army MEDCOM, Richard Thorp, Deputy Chief of Analysis and Evaluation, US Army MEDCOM, Richard Meyer, Decision Science Analyst, US Army MEDCOM Analysis and Evaluation Division , Robert Goodman, Deputy Chief of Staff for Resources, Infrastructure and Strategy, US Army Office of the Surgeon General , Maurine Tapscott, Decision Science Analyst , US Army MEDCOM Analysis and Evaluation Division Background and purpose Evaluating administrative costs as a ratio to revenue (or value) is a common business evaluation. Administrative costs in healthcare particularly important as they are both high relative to revenue (value) and have significant variance. In fact , managing administrative costs is one central issue in the United States healthcare reform and the Affordable Healthcare Act. The Military Healthcare System (MHS) is no different with administrative costs averaging 30 percent of value with very wide variance between medical facilities. Though it is easy to calculate the ratio for military medical facilities determining a standard is challenging because of the impact of diseconomies of scale and other operational factors. Figure 1. Revenue vs. Support Expenses & Revenue vs. Ratio (Expenses / Revenue) for Baseline 12 -month period Figure 2. ANCOVA Model for Baseline Period Log (Ratio) = Log(Revenue) + MTF_type (Prediction Equation in Red box) Setting the Baseline Model Data Sources and Processing Workload REVENUE was calculated using monetized Do. D-standard workload production measures commonly used in ambulatory clinical encounters (Relative Value Units), ambulatory procedures (Ambulatory Procedure Classification weights), and inpatient admissions (Relative Weighted Product OR Mental Health Occupied Bed Days). Support EXPENSES are defined as those administrative expenses which are allocated to clinical expense accounts in the Military Health System’s Medical Expense & Performance Reporting System (MEPRS). Data was obtained from Do. D Military Health System databases using a rolling 12 -month extraction process to adjust for seasonality. For each MTF, the total workload REVENUE, Healthcare support EXPENSES were collected and the RATIO of Support expenses to Workload revenue was calculated. (Fig. 1) A facility TYPE was assigned to each MTF, based on its capabilities: CLINIC: Provides ambulatory services only (no inpatient) HOSP: Community hospital with basic inpatient capabilities– limited specialty services MEDCEN: Medical Center, with tertiary inpatient and subspecialty services. Using the “Fit Model” platform in JMP, log-transformed REVENUE and RATIO values were used to create a baseline period ANCOVA model, with MTF_type (Clinic, Hospital, or Medical Center) utilized as a treatment variable (Fig. 2). MTF’s with actual Log_RATIO values below their predicted Log_RATIOs receive a positive grading (A or B), while those MTFs with actual ratios above their predicted ratios receive a lower grade (C or D). The standard deviation of the expected-predicted residuals was used to determine difference between A/B or C/D grades (Fig. 3) Figure 3. ACE Grade based on Actual vs. Expected Log_RATIO distance Click for next page ->

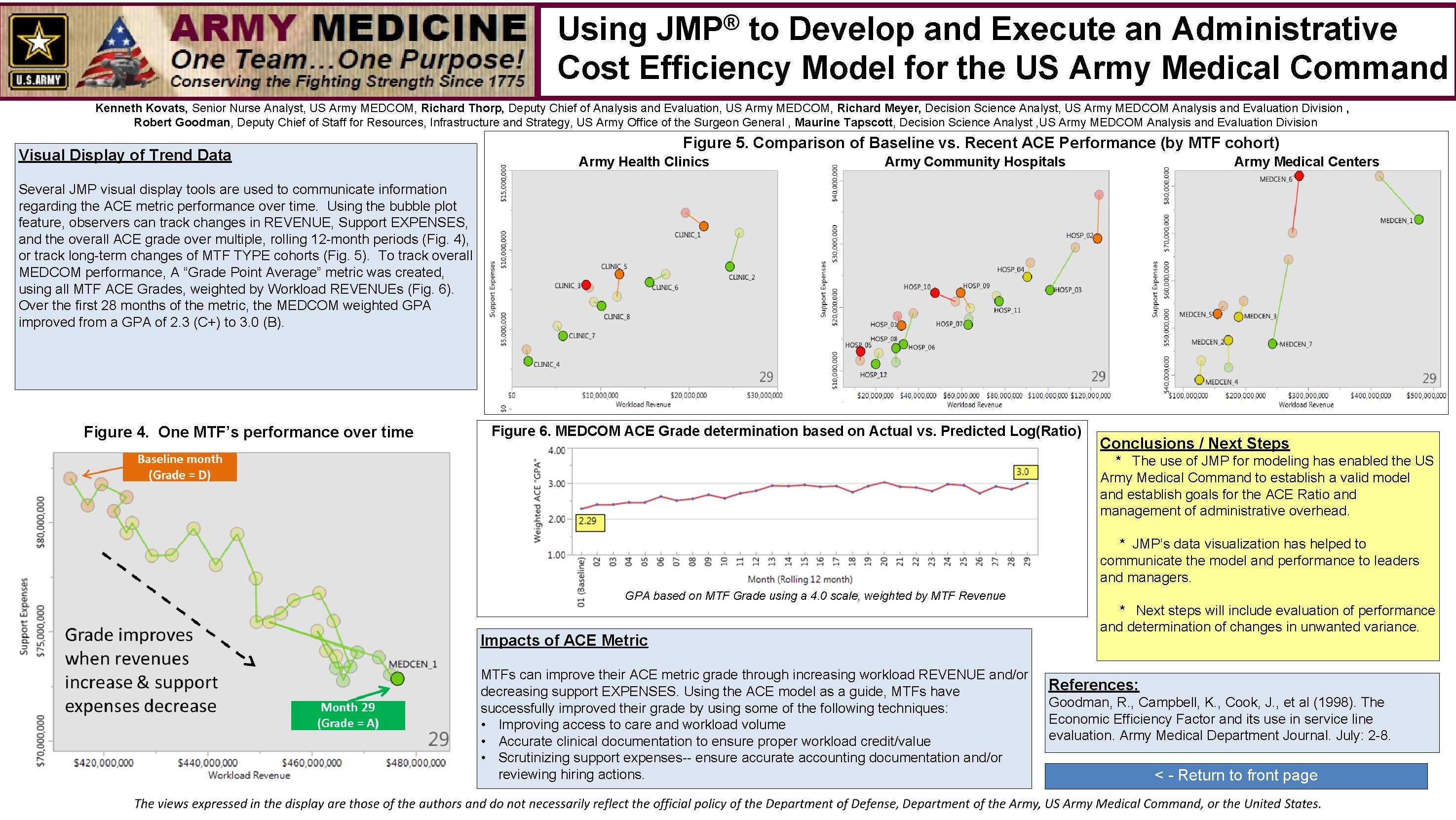
® JMP Using to Develop and Execute an Administrative Cost Efficiency Model for the US Army Medical Command Kenneth Kovats, Senior Nurse Analyst, US Army MEDCOM, Richard Thorp, Deputy Chief of Analysis and Evaluation, US Army MEDCOM, Richard Meyer, Decision Science Analyst, US Army MEDCOM Analysis and Evaluation Division , Robert Goodman, Deputy Chief of Staff for Resources, Infrastructure and Strategy, US Army Office of the Surgeon General , Maurine Tapscott, Decision Science Analyst , US Army MEDCOM Analysis and Evaluation Division Visual Display of Trend Data Figure 5. Comparison of Baseline vs. Recent ACE Performance (by MTF cohort) Army Health Clinics Army Community Hospitals Army Medical Centers Several JMP visual display tools are used to communicate information regarding the ACE metric performance over time. Using the bubble plot feature, observers can track changes in REVENUE, Support EXPENSES, and the overall ACE grade over multiple, rolling 12 -month periods (Fig. 4), or track long-term changes of MTF TYPE cohorts (Fig. 5). To track overall MEDCOM performance, A “Grade Point Average” metric was created, using all MTF ACE Grades, weighted by Workload REVENUEs (Fig. 6). Over the first 28 months of the metric, the MEDCOM weighted GPA improved from a GPA of 2. 3 (C+) to 3. 0 (B). Figure 4. One MTF’s performance over time Figure 6. MEDCOM ACE Grade determination based on Actual vs. Predicted Log(Ratio) Conclusions / Next Steps * The use of JMP for modeling has enabled the US Army Medical Command to establish a valid model and establish goals for the ACE Ratio and management of administrative overhead. * JMP’s data visualization has helped to communicate the model and performance to leaders and managers. GPA based on MTF Grade using a 4. 0 scale, weighted by MTF Revenue Impacts of ACE Metric MTFs can improve their ACE metric grade through increasing workload REVENUE and/or decreasing support EXPENSES. Using the ACE model as a guide, MTFs have successfully improved their grade by using some of the following techniques: • Improving access to care and workload volume • Accurate clinical documentation to ensure proper workload credit/value • Scrutinizing support expenses-- ensure accurate accounting documentation and/or reviewing hiring actions. * Next steps will include evaluation of performance and determination of changes in unwanted variance. References: Goodman, R. , Campbell, K. , Cook, J. , et al (1998). The Economic Efficiency Factor and its use in service line evaluation. Army Medical Department Journal. July: 2 -8. < - Return to front page