Jane Bordner Rn BSN Instructor of Nursing HACC

Jane Bordner, Rn BSN Instructor of Nursing HACC Central Pennsylvania’s Community College Nursing 102 Fall 2012 Drugs Affecting the Nervous System

Nervous System Review • 2 Major divisions – CNS – PNS
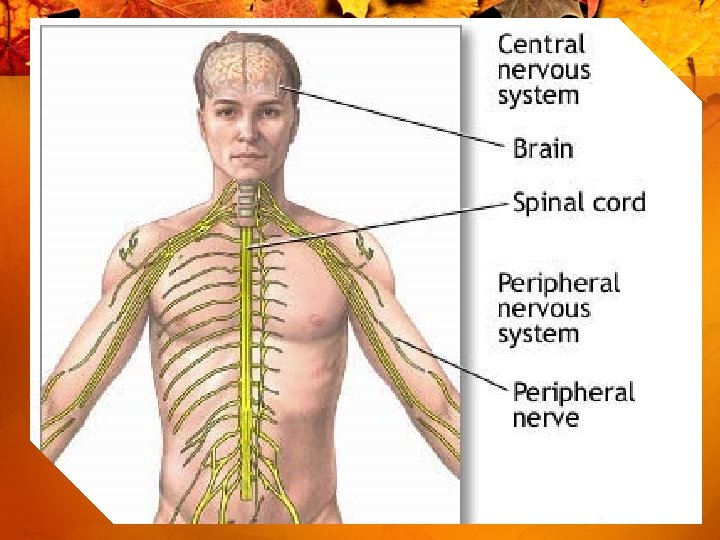

The Central and Autonomic Nervous Systems • Central nervous system (CNS) – Made up of brain and spinal cord – Receives signals from sensory receptors (vision, pressure, pain, cold, warmth, touch, smell)

The Central and Autonomic Nervous Systems • PNS • 2 Divisions – Somatic- voluntary-conscious control – Autonomic- involuntary-unconscious control • Sympathetic- fight or flight epinephrine/norepinephrine • Parasympathetic- rest or digest • acteylocholine • 2 Types of Nerves – Afferent – to the brain – Efferent-from sensory organs

The Central and Autonomic Nervous Systems (cont’d) • Peripheral nervous system – Afferent nerves—transmit signals to the spinal cord and brain – Efferent nerves—carry impulses from CNS to other parts of body.
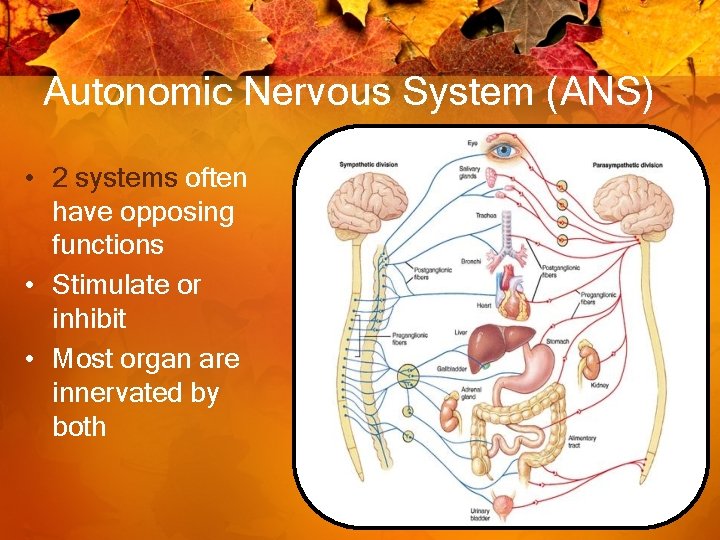
Autonomic Nervous System (ANS) • 2 systems often have opposing functions • Stimulate or inhibit • Most organ are innervated by both

Autonomic Nervous System • Sympathetic - Adrenergic • “Fight or Flight”
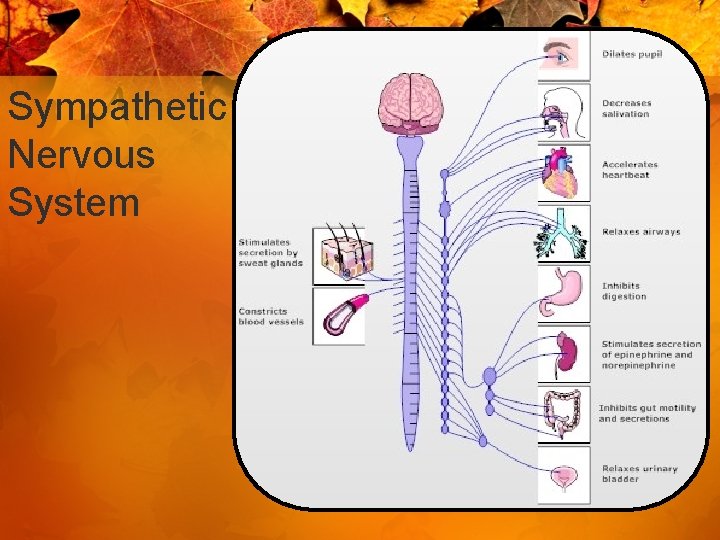
Sympathetic Nervous System

Autonomic Nervous System • Parasympathetic - Cholinergic • “Rest and Digest”
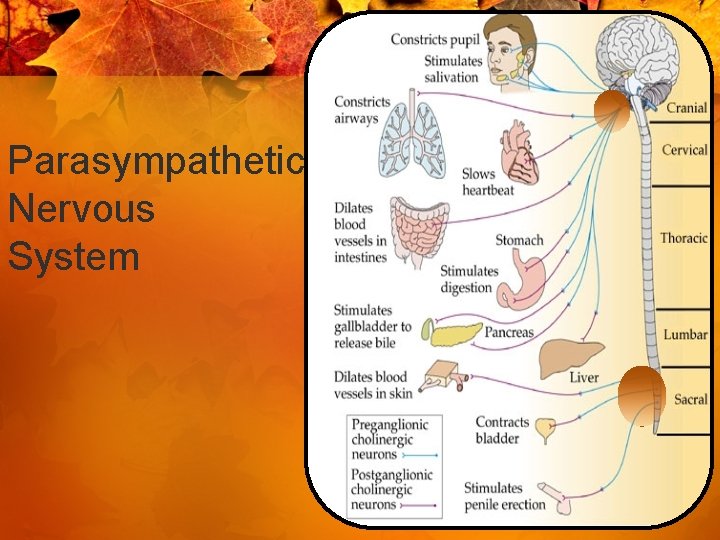
Parasympathetic Nervous System
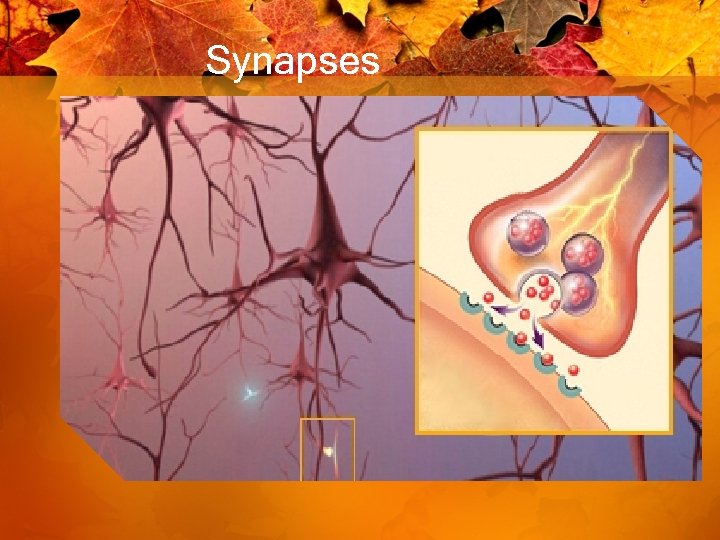
Synapses
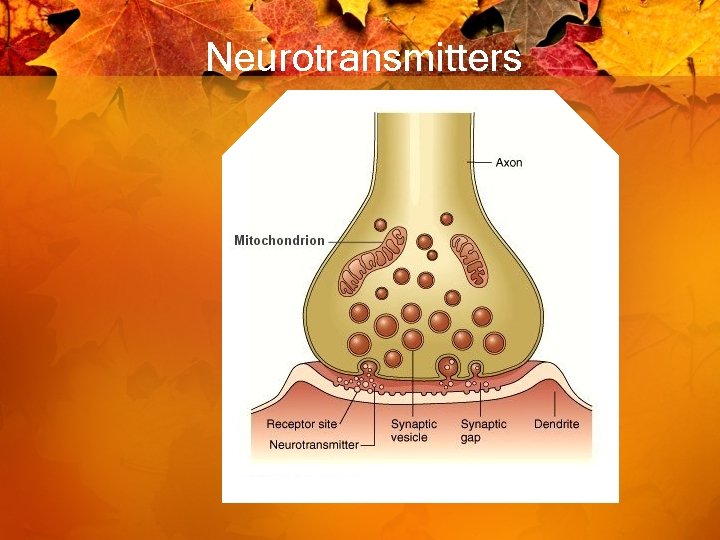
Neurotransmitters
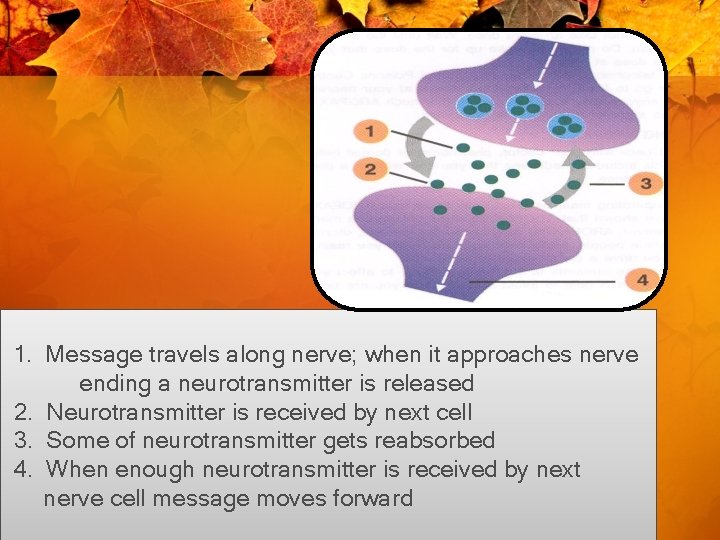
1. Message travels along nerve; when it approaches nerve ending a neurotransmitter is released 2. Neurotransmitter is received by next cell 3. Some of neurotransmitter gets reabsorbed 4. When enough neurotransmitter is received by next nerve cell message moves forward
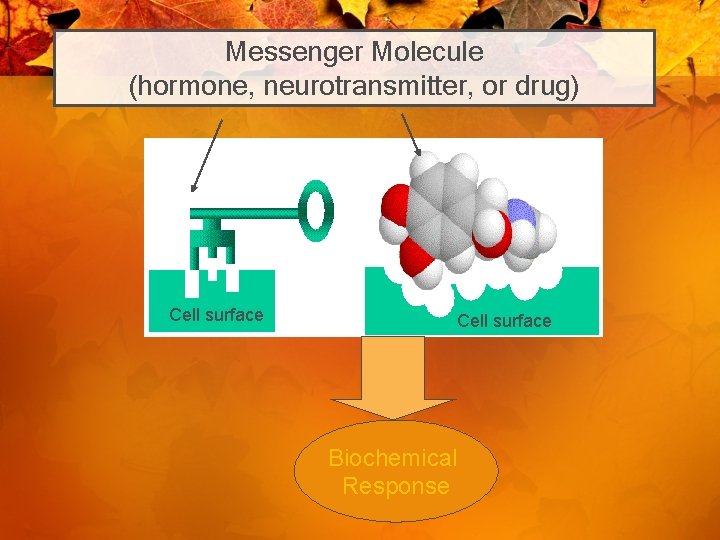
Messenger Molecule (hormone, neurotransmitter, or drug) Cell surface Biochemical Response

Sympathetic • Major Neurotransmitters (Catecholamines) – Epinephrine – Norepinephrine – Dopamine

Effects of Sympathetic System • • • Increase heart rate Relax bronchial smooth muscles Pupil dilation Increased metabolism Decreased GI motility Peripheral vasoconstriction

Neuroreceptors • Alpha 1: vasoconstriction of arterioles, relax bladder, eyes, liver • Alpha 2: skeletal blood vessels, pancreas • Beta 1: AV and SA node stimulation = increased heart rate and contraction strength • Beta 2: relaxes smooth muscle of bronchi and uterus • Dopaminergic

Sympathetic Neurotransmitters • Act on alpha, beta, or dopaminergic receptor sites • Example: – Alpha 1 receptors are found in peripheral blood vessels, when stimulated they cause peripheral vasoconstriction which leads to increased BP

Parasympathetic Activity • Major Neurotransmitter (Cholinergic) – Acetylcholine

Parasympathetic Neuroreceptors • Cholinergic receptors – Muscarinic • Both excitation and inhibition – Salivation – Lacrimation – Gastric acid secretion • Slow onset – Nicotinic • Excitation • Fast onset • Short duration

Parasympathetic Effects • • • Decrease heart rate Constrict bronchial smooth muscle Pupil constriction Increased GI motility Increased secretions Increased bladder tone
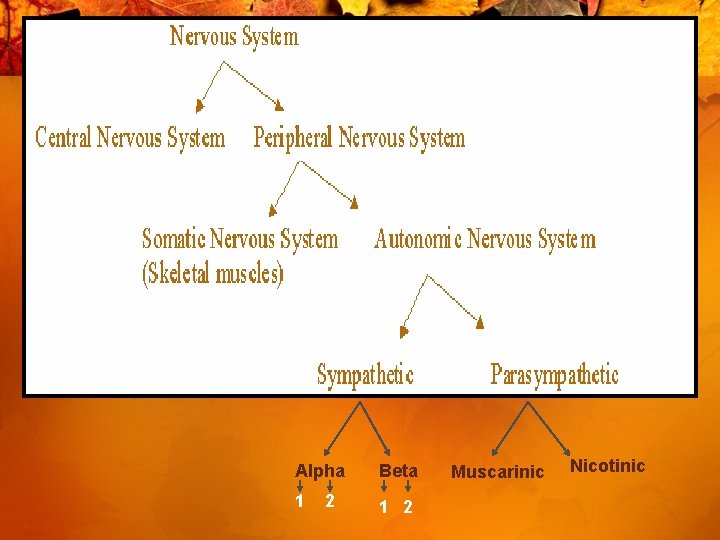
Alpha Beta 1 1 2 2 Muscarinic Nicotinic
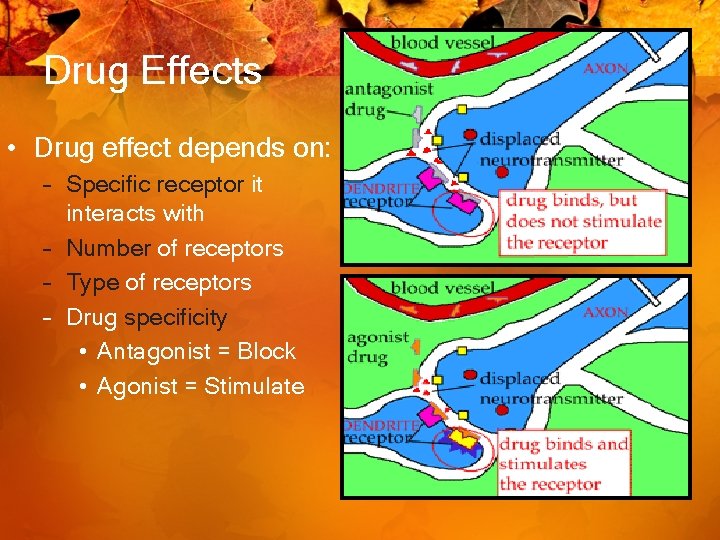
Drug Effects • Drug effect depends on: – Specific receptor it interacts with – Number of receptors – Type of receptors – Drug specificity • Antagonist = Block • Agonist = Stimulate

Drug Effects • Imitate neurotransmitters’ action • Block neurotransmitters’ action • Enhance or inhibit – – synthesis storage release breakdown

Drug Categories • ANS drugs are categorized by – Site of action – Effect – Receptor

Drug Categories • Sympathomimetics – Adrenergics • Sympatholytics – Adrenergic blockers • Parasympathomimetics – Cholinergics • Parasympatholytics – Cholinergic blockers

SYMPATHOMIMETICS AKA ADRENERGIC AGENTS

Sympathomimetics/ Adrenergic Agents • Catecholamines • Noncatecholamines • Primary Actions – – – Increase heart rate Increase BP Relax bronchial smooth muscle Relax GI tract Coronary artery vasodilation Peripheral vascular vasoconstriction

Catecholamines • Stimulate alpha and beta receptors • Mimic action of epinephrine, norepinephrine, and dopamine • Examples: – – dobutamine HCL (Dobutrex, Intropin, Dopastat ) Epinephrine (Adrenalin, Epi. Pen ) Norepinephrine (Levophed) isoproterenol HCL (Isuprel)

Catecholamines • Uses – Severe hypotensive crisis – Cardiac arrest – Anaphylactic shock • Special considerations – Destroyed by digestive enzymes

“Cat”echolamines • Side Effects – Severe throbbing headache – Dizziness – Anxiety – Fear – Palpitations – Hypertension

Noncatecholamines • • • Similar responses More receptor selective Slower acting Longer lasting Can be given PO Usually given SC or by inhaler

Noncatecholamines • Examples – – albuterol (Proventil) metaproterenol sulfate (Alupent) terbutaline (Brethine) phenylephrine HCL (Neo-Synephrine) • Uses – Bronchospasm (Asthma/Emphysema) – Nasal congestion – Preterm labor
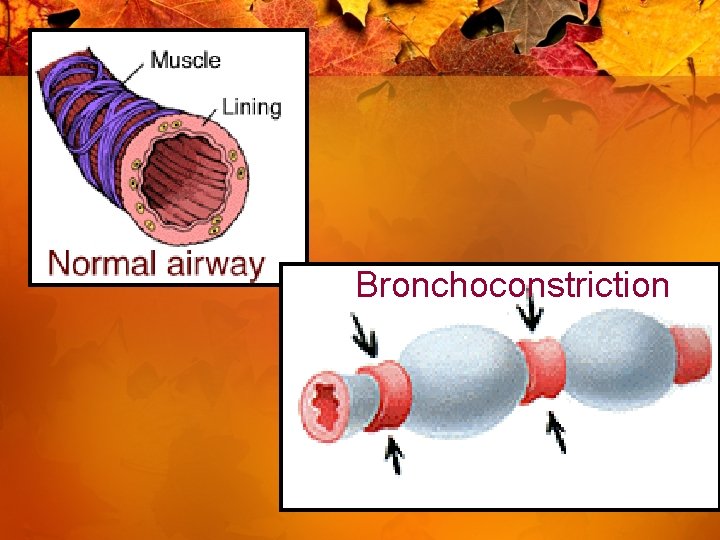
Bronchoconstriction

Noncatecholamines • Side Effects – – – Tachycardia Palpitations Tremors Hypertension Headache Anxiety

Adrenergic Agents • Nursing Measures – Monitor VS frequently – Monitor breath sounds – Monitor blood glucose in Diabetic

SYMPATHOLYTICS AKA ADRENERGIC BLOCKERS

Adrenergic Blocking Agents • AKA – Sympatholytics – Antiadrenergics • Antagonistic effect • Classified by site of action – Alpha Adrenergic Blockers – Beta Adrenergic Blockers

Alpha Adrenergic Blocking Agents • Action – Relax smooth muscle – Peripheral vasodilation • Uses – Antihypertensives – Vascular H/A – Raynaud’s Disease – Buerger’s Disease

Alpha Adrenergic Blocking Agents • Side Effects – – Hypotension Tachycardia Dizziness H/A • Nursing Actions – Postural BP – Teach to avoid caffeine

Alpha Adrenergic Blocking Agents • Examples – ergotamine tartrate (Ergostat) • Inhaler, PO or SL • Treat migraine H/A – phenoxybenzamine HCL (Dibenzyline) • Antihypertensive • Treat Raynaud’s Disease – doxazosin mesylate (Cardura) – prazosin HCL (Minipress) – terazosin (Hytrin) • Arteriole and venous vasodilation BP lower

Beta Adrenergic Blocking Agents • AKA – Beta Blockers • Most widely used group • Beta 1 receptors = heart • Beta 2 receptors = bronchi and blood vessels • Mixed = Nonselective blocking agents

Beta Adrenergic Blocking Agents • Effect – – Lower HR Decrease BP Constrict pupil Decrease production of aqueous humor • Uses – Cardiac Arrhythmias – HTN – Angina – Glaucoma

Beta Adrenergic Blocking Agents • Mixed – *labetalol (Normodyne) • Selective Beta-1 – esmolol (Brevibloc) – *metoprolol (Lopressor/Toprol XL/Betaloc ) – acebutolol (Sectral) – betaxolol (Kerlone) – bisoprolol (Zebeta) – *atenolol (Tenormin) • Non-selective Beta-1 and Beta-2 – – – *propranolol (Inderal) *nadolol (Corgard) pindolol (Visken) carteolol (Cartrol ) *sotalol (Betapace) Timolol (Blocadren/Timoptic ) – penbutolol (Levatol) * Most commonly used

Beta Adrenergic Blocking Agents • Treatment of Glaucoma – Decrease IOP by decreasing production of aqueous humor • betaxolol (Betoptic) • timolol maleate (Timoptic) • levobunolol HCL (Betagan) – Can cause systemic side effects

Beta Adrenergic Blocking Agents • Side Effects – – – Hypotension Bradycardia Dizziness Insomnia Wheezing and Bronchospasm

Beta Adrenergic Blocking Agents • Nursing Measures – Never give with antacid – Check apical pulse for one minute before administering – Closely monitor blood glucose in diabetic pt. – Teach pt. to not discontinue abruptly

PARASYMPATHOMIMETICS AKA CHOLINERGICS

Cholinergic Agents • AKA – Parasympathomimetic • Promotes/mimics – function of acetylcholine • Stimulate cholinergic receptors – nicotinic and muscarinic • Imitate parasympathetic effects

Cholinergic Agents • Uses – – – Glaucoma Paralytic ileus Urinary retention Diagnosis and treatment of Myasthenia Gravis (MG) Antidote for tricyclic antidepressant overdose Antidote for neuromuscular blocking agent overdose

Cholinergic Agents • Examples – pilocarpine HCL - treatment of glaucoma – bethanechol (Urecholine) – treatment of urinary retention and neurogenic bladder – neostigmine (Prostigmin), pyridostigmine (Mestinon) – diagnosis and treatment of MG

Cholinergic Agents • Side Effects – – – N/V/D Bradycardia Hypotension Increased salivation and sweating Bronchoconstriction = wheezing and SOA

Cholinergic Agents • Nursing Measures – Never given IM or IV – Antidote = Atropine sulfate (Cholinergic Blocker)

PARASYMPATHOLYTICS AKA CHOLINERGIC BLOCKERS

Cholinergic Blocking Agents • AKA: – Anticholinergics – Parasympatholytics • Actions – Compete with acetycholine at muscarinic receptor sites – antagonists

Cholinergic Blocking Agents • Effects – – Decreased GI motility Decreased secretions Relax bladder muscle Increased heart rate

Cholinergic Blocking Agents • Uses – – Parkinson’s Disease Preanesthesia Agents Cardiac Arrhythmias Spastic conditions of bowel and bladder

Cholinergic Blocking Agents • Examples – Atropine sulfate • Preanesthesic • Emergency treatment of brady arrythmias – glycopyrrolate (Robinul) • Preanesthesic – dicyclomine HCL (Bentyl) • Irritable bowel syndrome

Cholinergic Blocking Agents • Examples – oxybutynin (Ditropan) • Bladder spasms – propantheline (Pro-Banthine) • Peptic ulcer disease – benztropine mesylate (Cogentin) • Extrapyramidal symptoms of Parkinson’s

Cholinergic Blocking Agents • Side Effects – Mild • Dry mouth • Decreased sweating • Decreased bronchial secretions – Moderate • Decreased accommodation – Severe • Urinary retention • Severe constipation • Ileus

Cholinergic Blocking Agents • Overdose – – – Restlessness Disorientation Hallucinations Unconsciousness Death

Cholinergic Blocking Agents • Nursing Measures – Dose range is very small – Infants, children and elderly are more prone to side effects – Heatstroke is potential complication – NEVER give to patient with glaucoma – Used to decrease GI motility, give 30 minutes before meals – Watch for urinary retention

NEUROMUSCULAR BLOCKING AGENTS
Neuromuscular Blocking Agents • Relax skeletal muscles – Disrupt transmission of nerve impulses at neuromuscular junction • Clinical Uses – Relax muscles during surgery – Decrease muscle spasms during ECT – Manage ventilator patients

Neuromuscular Blocking Agents • Examples – – pancuronium bromide (Pavulon) doxacurium Cl (Nuromax) succinylcholine Cl (Anectine) vecuronium bromide (Norcuron)

Neuromuscular Blocking Agents • Side Effects – – – Excessive salivation Excessive bronchial secretions Bronchospasm Apnea Hypotension

Neuromuscular Blocking Agents • Nursing Measures – O 2 – Suction equipment – Artificial ventilation

Anti. Parkinson’s Medications

Parkinson’s Disease • Neurotransmitters – Dopamine ( inhibitory) – Acetylcholine (excitatory) • Types of parkinsoinsm – Primary (idiopathic) – Secondary (induced by head trauma, infection, tumors, or drug exposure

Parkinson’s Disease • Goal of treatment is minimization of symptoms • Individualized combination therapy • Therapy begins when symptoms interfere with the ability to function in daily life • All symptoms cannot be eliminated because of side effects involved

Parkinson’s Disease • Signs – Facial appearance – Psychological involvement • Symptoms – Motor function • Tremor • Dyskinesia, propulsive, uncontrolled movement • Bradykinesia, akinesia • Excessive salivation
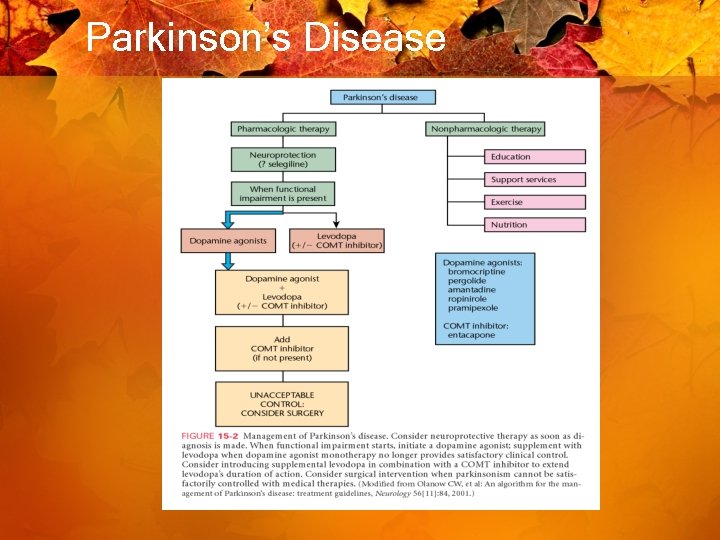
Parkinson’s Disease

Parkinson’s Disease • Dopamine agonists – – – Amantide hydrochloride Bromocriptine mesylate Carbidopa Pergolide mesylate Pramipexole Ropinirole

Parkinson’s Disease • Anticholinergic Agents – Cogentin ( Benztropine mesylate) – Akineton ( Biperiden hydrochloride) – Benadryl (diphenhydramine hydrochloride) – Banflex, Norflex (Orphenadrine citrate)

ANTICONVULSANT MEDICATIONS

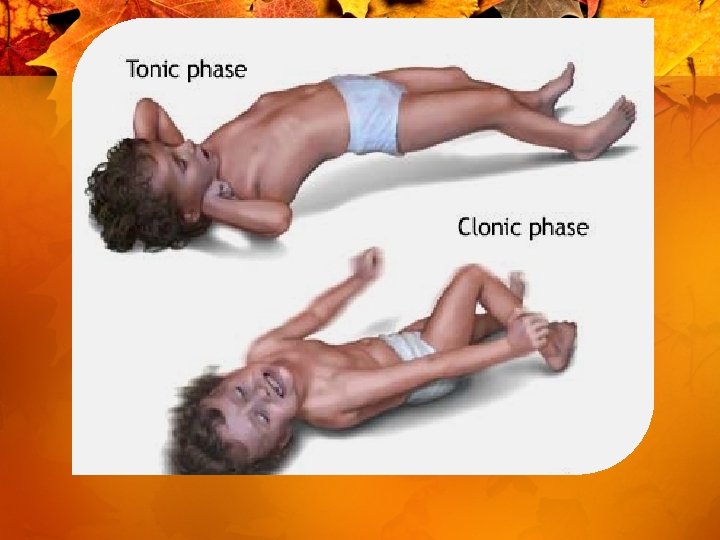
Types of seizures • Generalized – Tonic-Clonic (grand mal) – Myoclonic – Absence (petite mal) • Partial (localized) – Partial simple – Partial complex • Status Epilepticus

Anticonvulsant Therapy (cont’d) • Nurses may play an important role in diagnosis and treatment – Learn to take histories, describe seizures, record postictal behavior – Identify a care plan, have proper supplies, discuss with patient and family – Learn to assist patient during seizures, observe and record, discuss lifestyle and feelings with patient

Anticonvulsant Medications • Agents – – – Barbiturates Benzodiazepines Succinimides Hydantoins Miscellaneous Agents • Action – Increase seizure threshold – Regulate firing by inhibiting excitation or enhancing brains ability to inhibit its own excitation

Barbiturates • phenobarbital (Luminal) – Action • Increase seizure threshold • Prevent spread of electrical activity – Uses • Partial seizures • Generalized clonic tonic seizures

Barbiturates • Side Effects – Sedation – Nausea – Lethargy • Nursing Measures – Monitor therapeutic blood levels – Monitor effectiveness – Monitor degree of sedation

Benzodiazepines • Action – Enhance inhibitory effect – It is thought that they enhance the inhibitory effects of GABA in postsynaptic clefts between nerve cells • Drugs and Uses – diazepam (Valium) – acute status epilepticus ; IV – lorazepam (Ativan) – status epilepticus – clonazepam (Klonopin) – absence and myoclonic seizures – clorazepate (Tranxene) – adjunct treatment of partial seizures

Benzodiazepines • Side Effects – – Drowsiness Confusion Weakness Dizziness • Adverse Effects – Blood dyscrasias – Hepatotoxicity • Nursing Measures – Monitor CBC and LFT’s

Succinimides • Action – unknown • Uses – Absence seizures – Petit mal • Drugs – ethosuximide (Zarontin) – Methsuximide (Celontin) • Side Effects – GI upset – Sedation

Hydantoins • Action – Stabilizes nerve cells against hyperexcitability – Inhibits spread of seizure activity • Uses – Partial and generalized seizures • Drugs – phenytion (Dilantin) – fosphenytion (Cerebyx) – CAUTION: phenytoin (and diazepam) must be administered slowly, and not mixed with other medications in the same syringe

Hydantoins • Side Effects – – GI upset Sedation Confusion Gingival Hyperplasia • Adverse Effects – – Hyperglycemia Blood Dyscrasias Hepatotoxicity Rashes and pruritus

Hydantoins • Toxicity – – Nausea Sedation Lethargy Nystagmus

Hydantoins • Nursing Measures – Monitor CBC, LFT’s, Blood Glucose and Therapeutic Blood Levels – Good oral hygiene – Monitor effectiveness – Monitor for excessive sedation – Give with food – Give at same time each day

MISCELLANEOUS AGENTS

carbamzepine (Tegretol) – Action – Blocks up the reuptake of norepinephrine – Decreases release of norepinephrine and rate of dopamine and GABA turnover – Mechanisms of action as anticonvulsant are unknown • unknown – Uses • Generalized tonic-clonic seizures • Partial and mixed seizures • Often used with other agents – Side Effects • GI upset • Sedation • Edema

carbamazepine (Tegretol) • Adverse Effects – – – – Orthostatic hypotension Hypertension Dyspnea Edema Hepatotoxicity Blood Dyscrasias Rashes and pruritus

carbamazepine (Tegretol ) • Nursing Measures – Monitor CBC, LFT’s and therapeutic blood level – Monitor BP – Give with food – Monitor seizure activity – Monitor for excessive sedation

valproic acid (Depakote, Depakene – Action • May increase concentrations of GABA – Uses • Absence seizures • Combination seizures

valproic acid (Depakote, Depakene) • Side Effects • • • Abdominal pain Diarrhea Dizziness Drowsiness Unusual bleeding • Nursing Measures – CBC and platelet count before and 2 wks after start of therapy – LFT’s before and every 6 months – Can cause birth defects

gabapentin (Neurotin) • Uses – Partial seizures – In combination with other agents • Side Effects – Sedation – Confusion

Other Miscellaneous Agents • • lamotrigine (Lamictal) levetiracetam (Keppra) primidone (Mysoine) tiagabine (Gabatril) oxcarbazepine (Trileptal) topiramate (Topamax) zonisamide (Zonegran)

Anticonvulsant Medications • General Nursing Considerations – NEVER suddenly stop anticonvulsant therapy – SEDATION is MOST common reason for noncompliance with drug therapy – Driving • Must be seizure free for 6 months • Physicians required to report seizures to DOT

Alternative Therapy • Ketogenic Diet – – – – – Most successful in children Used for intractable epilepsy High fat, low CHO, low protein Limited fluids Mechanism of action unknown Nutritional supplementation of Ca+ and vitamins Monitor ketones with every void May not see response for 10 wks May gradually wean from diet after seizures controlled

Research • GABA – Discovered in 1950 • • Chemical that maintains balance in brain’s delivery system Nerve cells communicate by releasing neurotransmitters GABA halts messages Without GABA, system becomes overloaded and seizures occur • New drug vigabatrin (Sabril ) has chemical structure similar to GABA, ensuring GABA stays at level necessary to keep message delivery system functioning properly
- Slides: 101