Janani Suraksha Yojana Chiranjeevi Yojana Balshakha Yojna Dr

Janani Suraksha Yojana Chiranjeevi Yojana & Balshakha Yojna Dr. A. M. Kadri Associate Professor Community Medicine 1
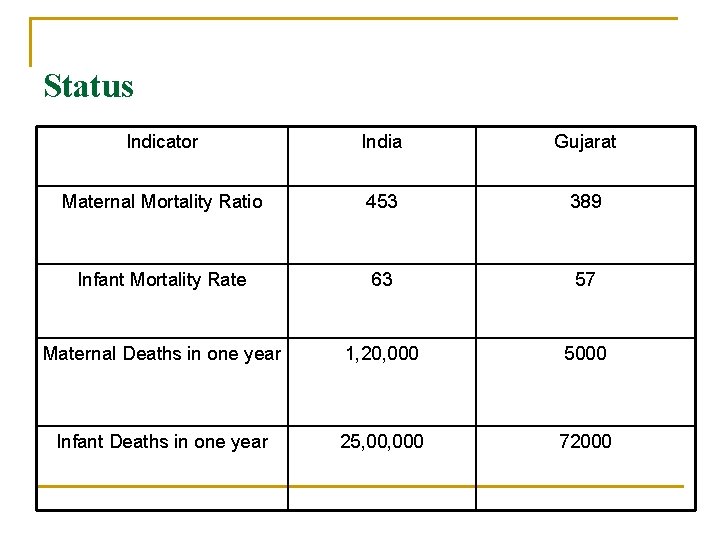
Status Indicator India Gujarat Maternal Mortality Ratio 453 389 Infant Mortality Rate 63 57 Maternal Deaths in one year 1, 20, 000 5000 Infant Deaths in one year 25, 000 72000

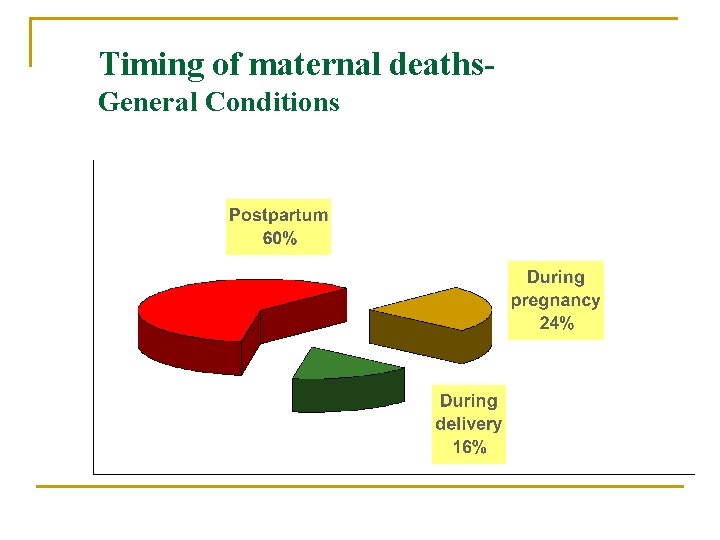
Timing of maternal deaths. General Conditions

Time from onset of complication to death n n n PPH APH Ruptured uterus Eclampsia Obstructed labor Sepsis 2 hour 1 day 2 days 1 day 6 days

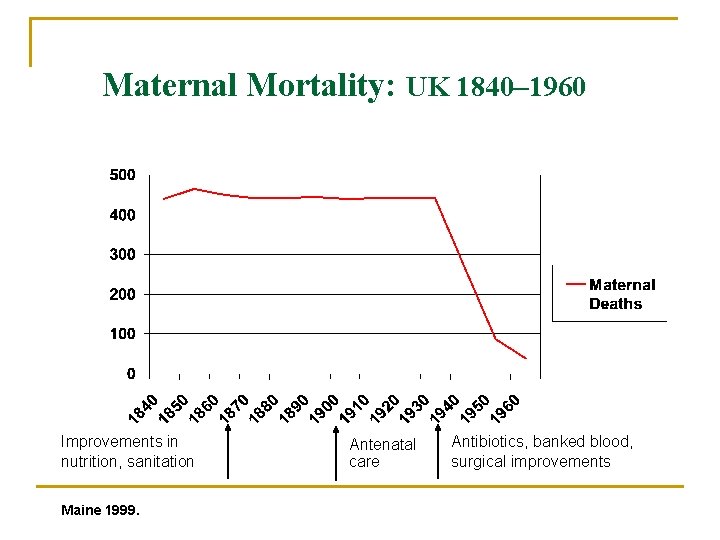
Maternal Mortality: UK 1840– 1960 Improvements in nutrition, sanitation Maine 1999. Antenatal care Antibiotics, banked blood, surgical improvements

Three Delays Responsible for Maternal Deaths 1. Delay in deciding to seek care (Individual & family) § Lack of understanding of complications § Gender issues, Low status of women § Socio-cultural barriers to seeking care § Poor economic conditions of the family 2. Delay in reaching care ( Community & System) § Lack or underutilization of transport funds § Non availability of referral transport in remote places § Lack of communication network 3. Delay in receiving care (System) § Poor facilities, personnel and Supplies § Poorly trained personnel with indifferent attitude

n Goals of National Population policy – q q n Interventions to increase institutional deliveries q q n Reduce MMR to less than 100 per 100000 livebirths by the year 2010. Increase proportion of institutional deliveries to 80% by 2010. JSY Chiranjeevi yojana Proportion of Home delivery (47%) in Gujarat. 9

Goals for different policies n n NRHM (By 2012) – 100/100000 livebirths. RCH II Goals – 150/100000 livebirths. National Population Policy 2000 (By 2012) 100/100000 livebirths Millennium development Goals – Reduction by 3/4 th by 2015. 10

Janani Suraksha Yojana n n Centrally sponsored scheme Safe motherhood intervention under umbrella of National Rural Health Mission (NRHM). Launched on 12 th April, 2005. Objective : q Reducing maternal and neonatal mortality by promoting institutional delivery among the poor pregnant women. 11

Implementation of JSY n All the states are divided in two categories. q Low Performing states ( LPS) (10) n q Accredited social health activitist (ASHA) is the link between government and poor preganant women. High Performing states (HPS) (Gujarat is one of them). n AWW and/ or TBA can act as link. 12

Activities under JSY n Role of ASHA or other link worker q q q Identification of beneficiary, Provision of at least three ANC check ups including TT, IFA tablets. Identification of Institute (Private or government). Counselling for institutional delivery. Escorting the beneficiary women Etc. 13

Activities under JSY (Continued) n Tracking of each preganancy – q n Beneficary should have a JSY card. Eligibility for Cash Assistance : q q q LPS – All preganant women delivering in govt. or accredited private hospital. HPS – BPL, aged 19 years and above. LPS & HPS- All SC and ST women delivering in govt. or accredited private hospital. LPS- for all deliveries. HPS – for first two births Dr. Hitesh M Shah 14
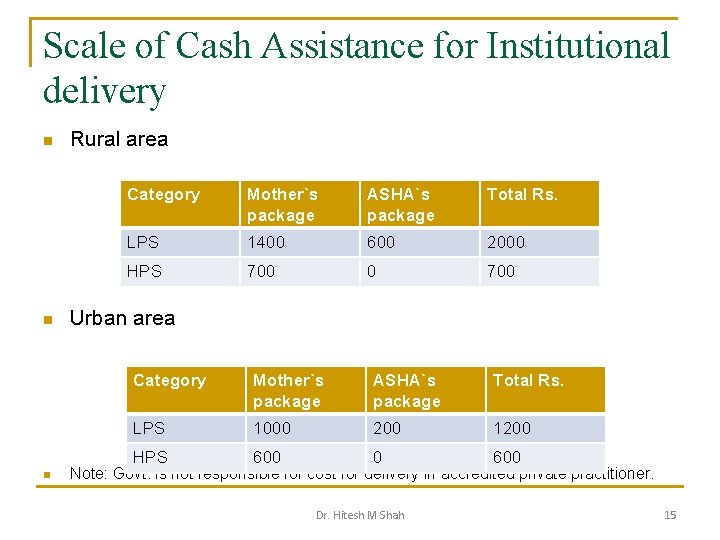
Scale of Cash Assistance for Institutional delivery n n n Rural area Category Mother`s package ASHA`s package Total Rs. LPS 1400 600 2000 HPS 700 0 700 Urban area Category Mother`s package ASHA`s package Total Rs. LPS 1000 200 1200 HPS 600 0 600 Note: Govt. is not responsible for cost for delivery in accredited private practitioner. Dr. Hitesh M Shah 15

Subsidizing cost of LSCS or obstetric complications n In Govt. set up – free of cost. n If govt. specialist are not available – Rs. 1500/- per delivery for hiring specialist. 16

Assistance for Home delivery n In LPS and HPS- BPL, aged 19 years and above, preferring to deliver at home should receive a cash benefit of Rs. 500/-. This assistance is up to 2 live births. 17

Chiranjeevi scheme n n It is a state government scheme. Objective : q q q To reduce maternal mortality ratio and Infant mortality rate. To increase the institutional deliveries. To involve the private practitioner to reduce MMR. 18

Broad Issues n n n Non - availability of O & G specialists Accessibility of services-Tribal and urban slums Poor utilization of servicesn n Low felt need of health & medical services Lack of user friendly & quality public health services Costly private health and medical services No health insurance coverage

Chiranjeevi scheme n n Initiated in December 2005 as a pilot scheme in five backward districts (BK, SK, Dahod, panchmahal and Kutch) to all BPL families. Now it is implemented throughout state. 20
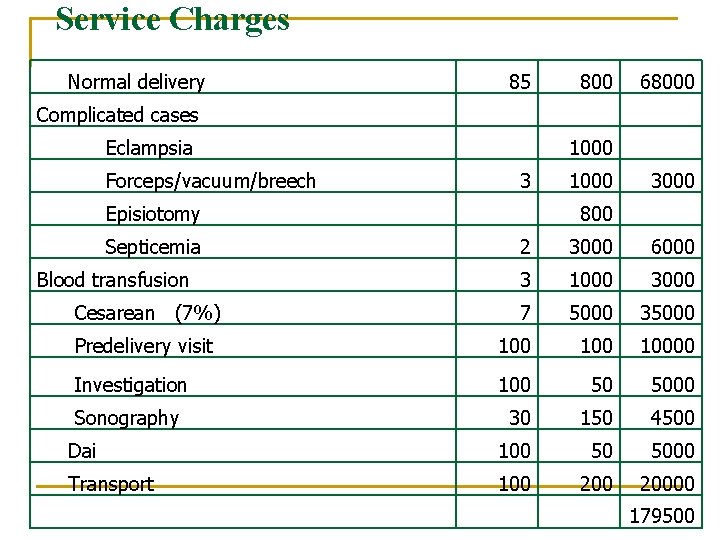
Service Charges Normal delivery 85 800 68000 Complicated cases Eclampsia Forceps/vacuum/breech 1000 3 Episiotomy Septicemia 1000 3000 800 2 3000 6000 3 1000 3000 7 5000 35000 Predelivery visit 100 10000 Investigation 100 50 5000 Sonography 30 150 4500 Dai 100 50 5000 Transport 100 20000 Blood transfusion Cesarean (7%) 179500
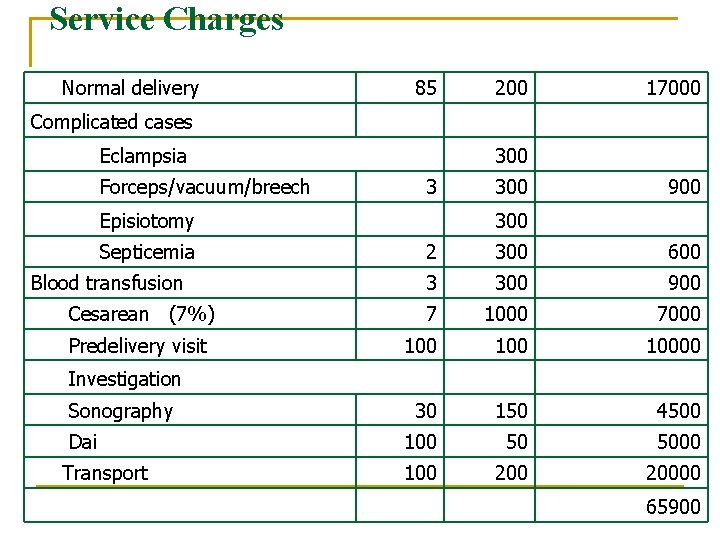
Service Charges Normal delivery 85 200 17000 Complicated cases Eclampsia Forceps/vacuum/breech 300 3 Episiotomy Septicemia Blood transfusion Cesarean (7%) Predelivery visit 300 900 300 2 300 600 3 300 900 7 1000 7000 100 10000 30 150 4500 100 50 5000 100 20000 Investigation Sonography Dai Transport 65900

Compensation of private practitioner – scheme II n If private practitioner provides services in government set up – the package for 100 deliveries is Rs. 65900 (Rs. 659/ delivery). 23

Bal Sakha Yojana n Need & Rationale : n High IMR : 50 /1000 LB to 30/1000 60% of them occurred during neonatal period. 2/3 of neonatal death during first week. Lack of pediatric doctors in Govt. Hosp Good network of Pvt Gynec & Pedia doctors. n n 24

Major features q q q q Part – 1 : Care During first 48 hours of life Part – 2 : Care for children up to 5 years BPL children will be covered. An Mo. U with Private Gynec & Pedia Doctors for 100 cases will be done. Rs. 1, 68, 000 & Rs. 1, 75, 000 for part I & part II respectively Money will be provided in advance. Additional support of Rs. 25, 000 for ventilator purchase on coverage of 500 children

Major features q q q q Part – 1 : Care During first 48 hours of life Part – 2 : Care for children up to 1 year BPL children will be covered. Mo. U with Private Gynec & Pedia Doctors for 100 cases will be done. Rs. 1, 68, 000 & Rs. 1, 75, 000 for part I & part II respectively Money will be provided in advance. Additional support of Rs. 25, 000 for ventilator purchase on coverage of 500 children

Major features – For Part : 1 q q q Cost is calculated based on the 100 cases. For all cases Gynecologist has to keep mother for two days and provide PNC care. Gynecologist has to ensure, BF in first half an hour of birth, Vit-K, 0 BCG & Polio & Kanagaru care Affiliated Pediatric doctor has to visit newborn for two times in 48 hours Based on the pattern it was presumed that out of 100 cases 20 will be required ENBC- 2 care & 5 will be required ENBC – 3 care. ENBC- 2 care to be provided at affiliated doctor’s Hospitals & For ENBC – 3 cases to be referred to Tertiary Care hospital.

Major features – For Part : 2 q q Cost is calculated based on the 100 cases. Consultation charges for all the case is considered. Out of 100 cost for hospitalization is calculated for 25 case based on the scientific evidences. Referral rate to tertiary care is considered 5% and for such cases additional Transport support is created.
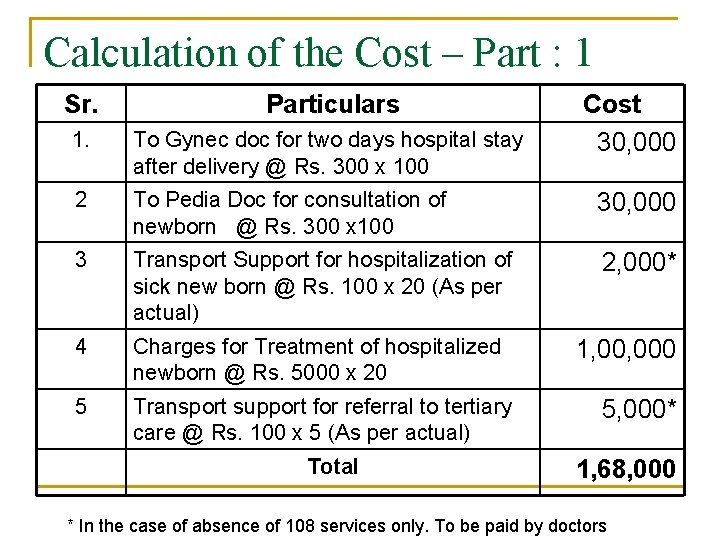
Calculation of the Cost – Part : 1 Sr. Particulars 1. To Gynec doc for two days hospital stay after delivery @ Rs. 300 x 100 2 To Pedia Doc for consultation of newborn @ Rs. 300 x 100 30, 000 3 Transport Support for hospitalization of sick new born @ Rs. 100 x 20 (As per actual) 2, 000* 4 Charges for Treatment of hospitalized newborn @ Rs. 5000 x 20 5 Transport support for referral to tertiary care @ Rs. 100 x 5 (As per actual) Total Cost 30, 000 1, 000 5, 000* 1, 68, 000 * In the case of absence of 108 services only. To be paid by doctors
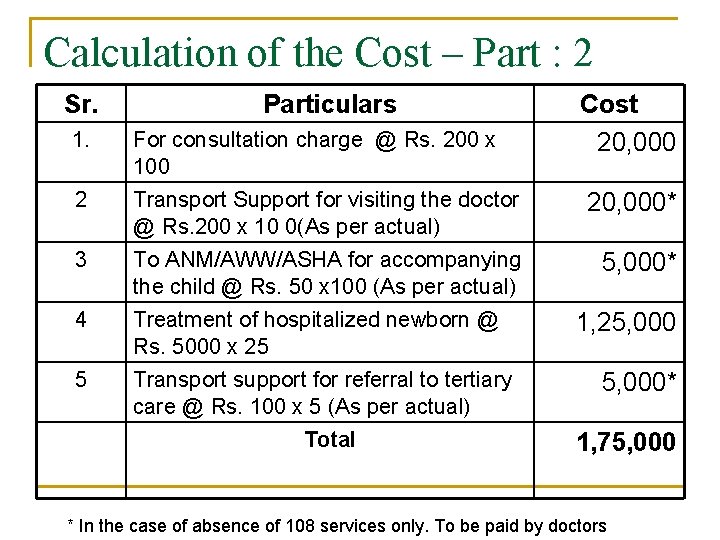
Calculation of the Cost – Part : 2 Sr. Particulars Cost 20, 000 1. For consultation charge @ Rs. 200 x 100 2 Transport Support for visiting the doctor @ Rs. 200 x 10 0(As per actual) 20, 000* 3 To ANM/AWW/ASHA for accompanying the child @ Rs. 50 x 100 (As per actual) 5, 000* 4 Treatment of hospitalized newborn @ Rs. 5000 x 25 5 Transport support for referral to tertiary care @ Rs. 100 x 5 (As per actual) Total 1, 25, 000* 1, 75, 000 * In the case of absence of 108 services only. To be paid by doctors

Thank you 31
- Slides: 31