Jacquie Campbell Site Director The West Lothian Frailty

Jacquie Campbell, Site Director The West Lothian Frailty Programme • Large scale improvement programme covering: o health care, Mental Health, social care, and all related sectors and provision across West Lothian processes and pathways quality cost available capacity skills / who does what where and when o o o

Led by West Lothian executive team and subject experts who will now: • • • Set the scene Give a background to Frailty Describe role development Describe a discharge example Discuss pathways and vision

Setting the scene: The West Lothian Pathways Collaborative (WELPACT) Dr. Karen Adamson Consultant Physician and Associate Director of Medical Education
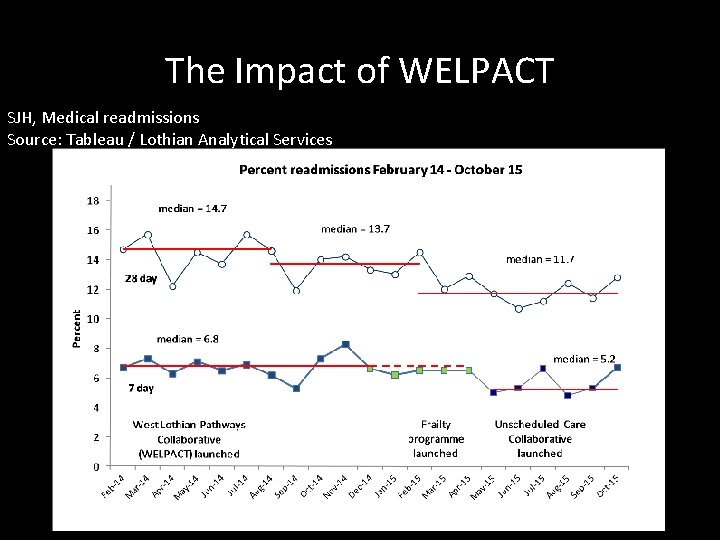
The Impact of WELPACT SJH, Medical readmissions Source: Tableau / Lothian Analytical Services

Key points for success: ü ü ü ü o o o Consultant engagement Consultant review of 474 cases Numbers of readmissions are incorporated on the daily print-outs MDTs led by a Geriatrician Discharge Hub implementation COPD Discharge Bundle KIS and ACP Communication, understanding and relationships across sector boundaries: WELPACT events Integration & Education Events (IEEs) Interface Group

Dr. Maria Corretge Consultant Physician and Geriatrician

Paradigm shift in Geriatric care • Previously… • Now • Discharge “when ready” • Weekly, long MDT • SW not integrated part of discharge planning • Early discharge • Rehabilitation and sometimes assessment to be completed in the community • Daily short huddles, shortened MDT • SW integrated in patient’s admission

Drivers to change in paradigm • • • Economic Hospital bed availability Demographic Social Human ? Medical – Evidence of intermediate care outside hospital

Frail Elderly: What are the standards • Quality standards: OPAH • Quantitative standards: Time waiting for rehabilitation or intermediate care Time spent in hospital as a delayed discharge Access to Comprehensive Geriatric Assessment

Rapid Elderly Assessment and Care in Hospital (REACH) Louise Mc. Kay
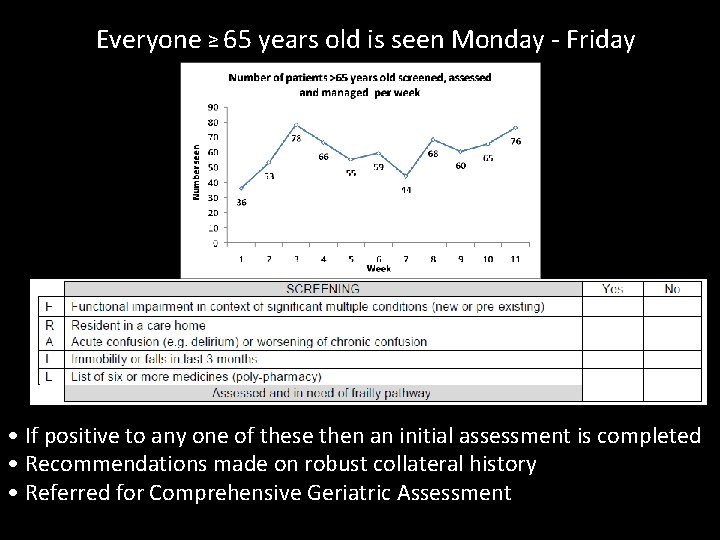
Everyone ≥ 65 years old is seen Monday - Friday • If positive to any one of these then an initial assessment is completed • Recommendations made on robust collateral history • Referred for Comprehensive Geriatric Assessment
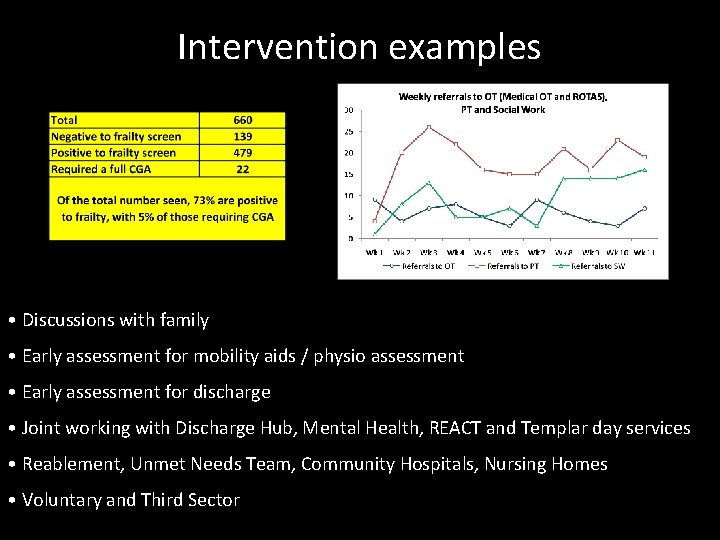
Intervention examples • Discussions with family • Early assessment for mobility aids / physio assessment • Early assessment for discharge • Joint working with Discharge Hub, Mental Health, REACT and Templar day services • Reablement, Unmet Needs Team, Community Hospitals, Nursing Homes • Voluntary and Third Sector
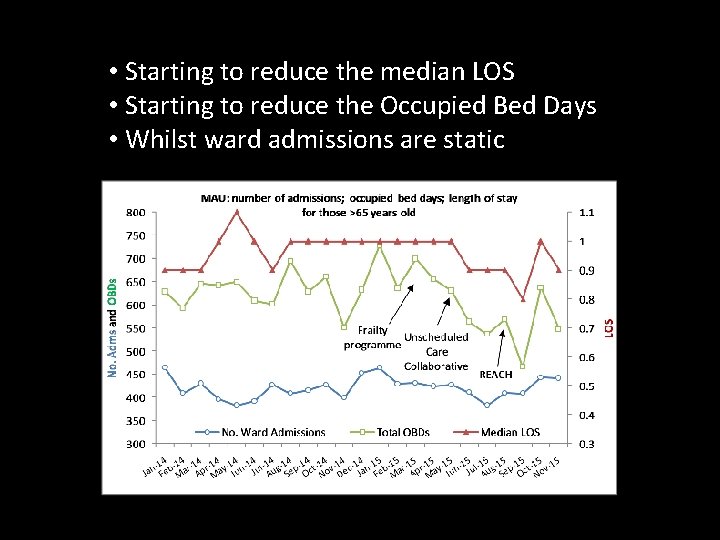
MAU data for those >65 yo • Starting to reduce the median LOS • Starting to reduce the Occupied Bed Days • Whilst ward admissions are static

Christine Owen

Dr. Jane Rimer Consultant Physician and Geriatrician
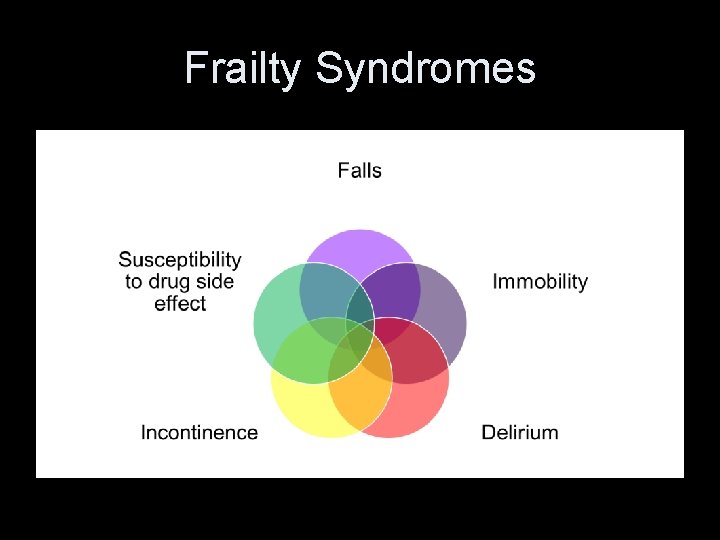
Frailty Syndromes
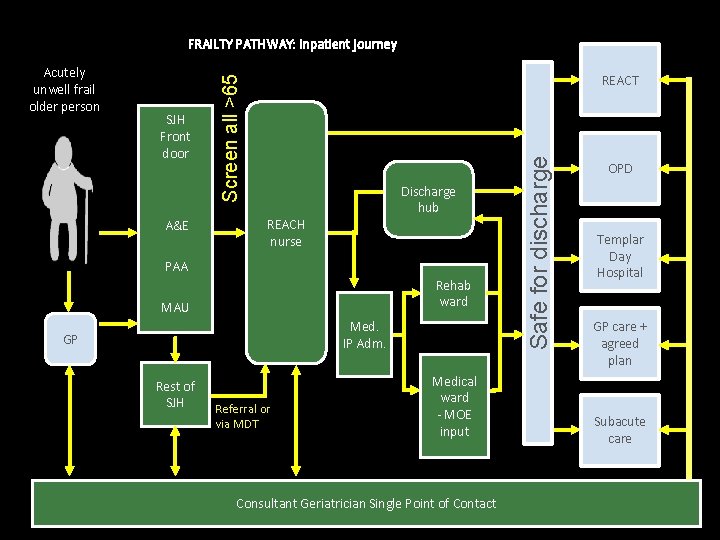
FRAILTY PATHWAY: Inpatient journey A&E Discharge hub REACH nurse PAA Rehab ward MAU Med. IP Adm. GP Rest of SJH Referral or via MDT Medical ward - MOE input Consultant Geriatrician Single Point of Contact Safe for discharge SJH Front door REACT Screen all >65 Acutely unwell frail older person OPD Templar Day Hospital GP care + agreed plan Subacute care
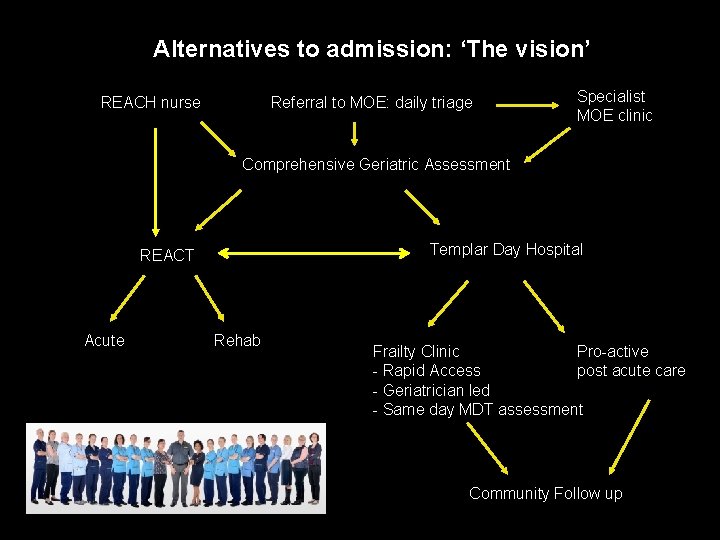
Alternatives to admission: ‘The vision’ REACH nurse Referral to MOE: daily triage Specialist MOE clinic Comprehensive Geriatric Assessment Templar Day Hospital REACT Acute Rehab Frailty Clinic Pro-active - Rapid Access post acute care - Geriatrician led - Same day MDT assessment Community Follow up
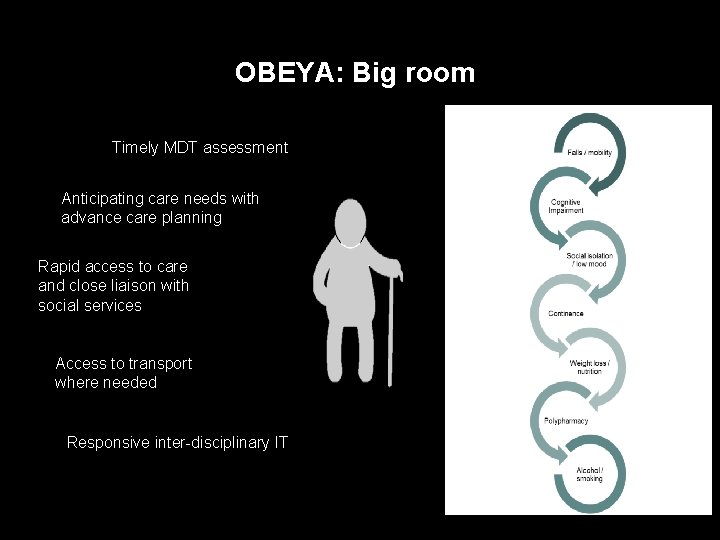
OBEYA: Big room Timely MDT assessment Anticipating care needs with advance care planning Rapid access to care and close liaison with social services Access to transport where needed Responsive inter-disciplinary IT

QUESTIONS
- Slides: 20