IVUS Predictors of Late Stent Thrombosis Gary S

IVUS Predictors of Late Stent Thrombosis Gary S. Mintz, MD Cardiovascular Research Foundation

Disclosure Statement of Financial Interest Within the past 12 months, I have had a financial interest/arrangement or affiliation with the organization(s) listed below. Affiliation/Financial Relationship • Grant/Research Support • Consulting Fees/Honoraria • Consulting Fees/Honoraria Company • Volcano • Boston. Scientific • Terumo • Prescient • Light. Lab

Predictors of DES Thrombosis & Restenosis DES Thrombosis Underexpansion DES Restenosis • Fujii et al. J Am Coll Cardiol • Sonoda et al. J Am Coll Cardiol 2005; 45: 995 -8) 2004; 43: 1959 -63 • Okabe et al. , Am J Cardiol. • Hong et al. Eur Heart J 2007; 100: 615 -20 2006; 27: 1305 -10 • Liu et al. JACC Cardiovasc • Doi et al. JACC Cardiovasc Interv. 2009; 2: 428 -34 Interv. 2009; 2: 1269 -75 • Fujii et al. Circulation 2004; 109: 1085 -1088 • Rathore et al. Eurointervention 2009; 5: 349 -54 Edge problems (geographic miss, secondary lesions, large plaque burden, etc) • Fujii et al. J Am Coll Cardiol • Sakurai et al. Am J Cardiol 2005; 45: 995 -8) 2005; 96: 1251 -3 • Okabe et al. , Am J Cardiol. • Liu et al. Am J Cardiol 2007; 100: 615 -20 2009; 103: 501 -6 • Liu et al. JACC Cardiovasc • Costa et al, Am J Cardiol, Interv. 2009; 2: 428 -34 2008; 101: 1704 -11
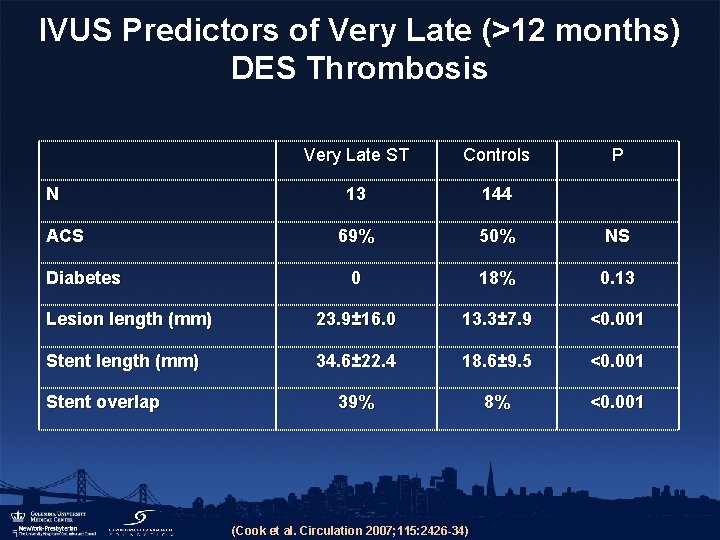
IVUS Predictors of Very Late (>12 months) DES Thrombosis Very Late ST Controls 13 144 69% 50% NS 0 18% 0. 13 Lesion length (mm) 23. 9± 16. 0 13. 3± 7. 9 <0. 001 Stent length (mm) 34. 6± 22. 4 18. 6± 9. 5 <0. 001 39% 8% <0. 001 N ACS Diabetes Stent overlap (Cook et al. Circulation 2007; 115: 2426 -34) P
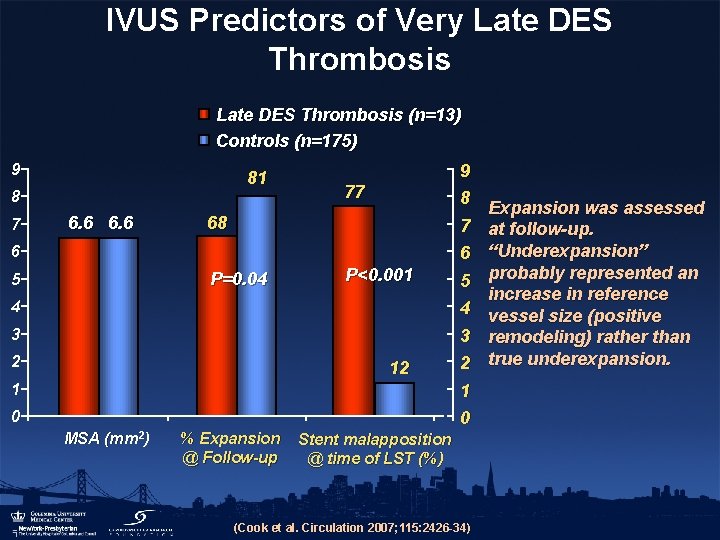
IVUS Predictors of Very Late DES Thrombosis (n=13) Controls (n=175) 9 81 8 7 6. 6 9 8 77 68 7 6 6 P=0. 04 5 P<0. 001 4 3 2 12 1 5 4 3 2 1 0 0 MSA (mm 2) % Expansion @ Follow-up Stent malapposition @ time of LST (%) (Cook et al. Circulation 2007; 115: 2426 -34) Expansion was assessed at follow-up. “Underexpansion” probably represented an increase in reference vessel size (positive remodeling) rather than true underexpansion.
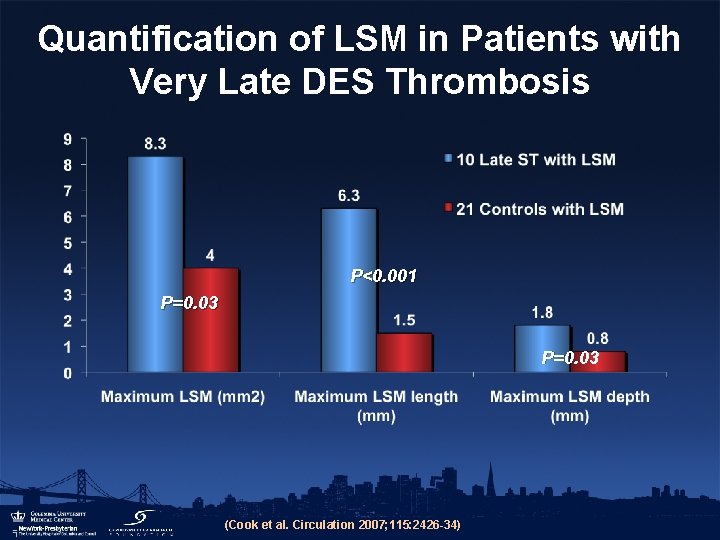
Quantification of LSM in Patients with Very Late DES Thrombosis P<0. 001 P=0. 03 (Cook et al. Circulation 2007; 115: 2426 -34)

Meta-Analysis of Late Stent Malapposition (LSM) Frequency • 17 studies with 4648 patients ¡ 2453 BMS and 2195 DES ¡ 4 SES, 4 PES, 1 EES, 2 ZES, 3 DES vs DES, and 3 BMS only • LSM more common in DES than BMS ¡ OR=2. 5, p=0. 02 when both RCT and observational studies were included ¡ OR=4. 4, p=0. 002 when only RCT were included ¡ SES > PES > ZES > EES (Hassan et al. Eur Heart J, in press)

Meta-Analysis of Very Late ST in LSM • 5 studies with 2080 patients ¡ 228 LSM and 1852 no LSM ¡ 3 Late ST (<12 mos), none in LSM ¡ 6 Very late ST (>12 mos), 4 in LSM • Risk of very late ST was higher in LSM patients (OR=6. 5, p=0. 02). • Based on the expected numbers of very late ST, 3 of 5 studies favored the relationship between LSM and very late ST. (Hassan et al. Eur Heart J, in press)
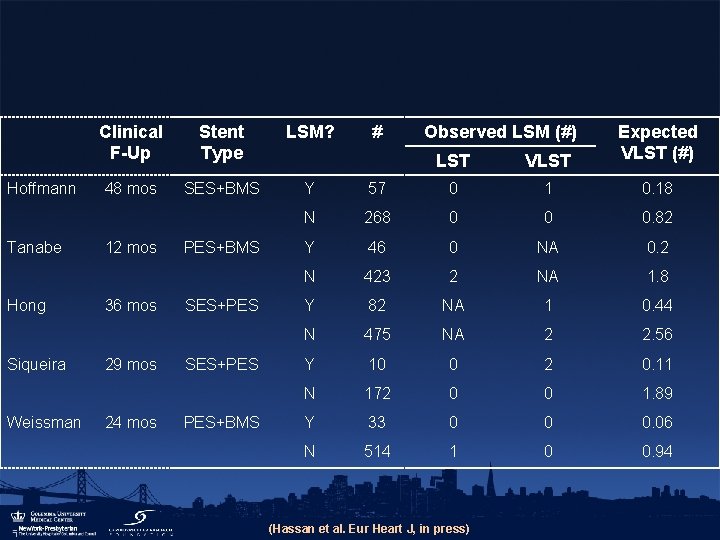
Hoffmann Tanabe Hong Siqueira Weissman Clinical F-Up Stent Type LSM? 48 mos SES+BMS Y 12 mos 36 mos 29 mos 24 mos PES+BMS SES+PES PES+BMS # Observed LSM (#) LST VLST Expected VLST (#) 57 0 1 0. 18 N 268 0 0 0. 82 Y 46 0 NA 0. 2 N 423 2 NA 1. 8 Y 82 NA 1 0. 44 N 475 NA 2 2. 56 Y 10 0 2 0. 11 N 172 0 0 1. 89 Y 33 0 0 0. 06 N 514 1 0 0. 94 (Hassan et al. Eur Heart J, in press)
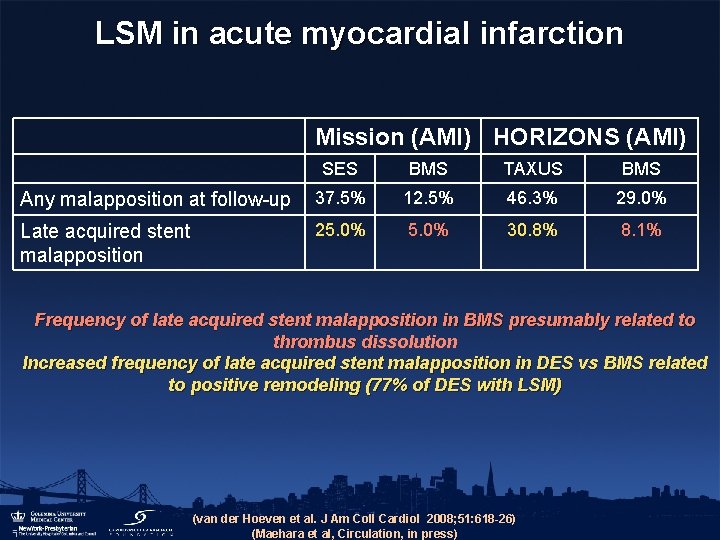

LSM in acute myocardial infarction Mission (AMI) HORIZONS (AMI) SES BMS TAXUS BMS Any malapposition at follow-up 37. 5% 12. 5% 46. 3% 29. 0% Late acquired stent malapposition 25. 0% 30. 8% 8. 1% Frequency of late acquired stent malapposition in BMS presumably related to thrombus dissolution Increased frequency of late acquired stent malapposition in DES vs BMS related to positive remodeling (77% of DES with LSM) (van der Hoeven et al. J Am Coll Cardiol 2008; 51: 618 -26) (Maehara et al, Circulation, in press)
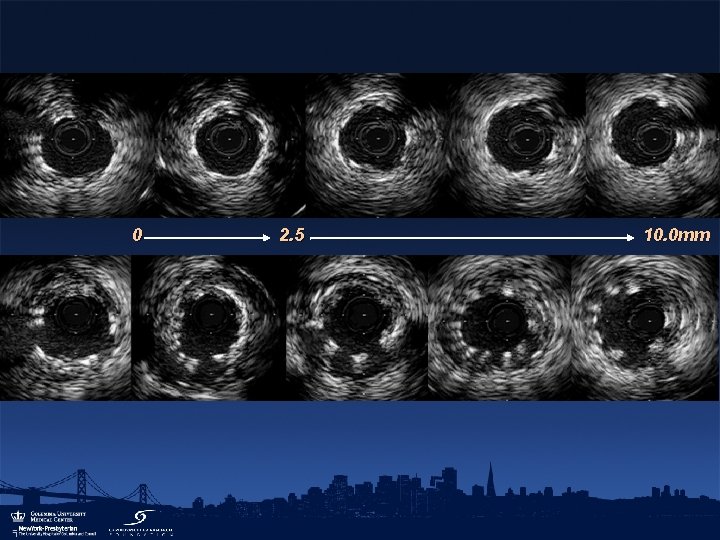
0 2. 5 10. 0 mm

0 3. 0 12. 0 mm
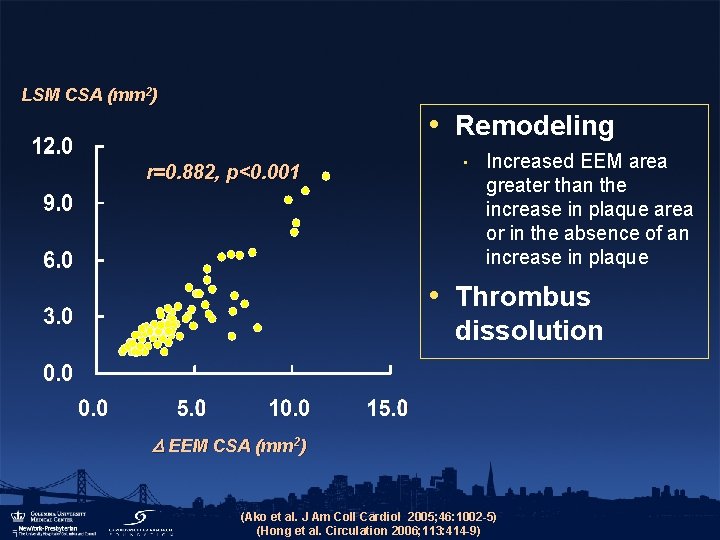
LSM CSA (mm 2) • Remodeling r=0. 882, p<0. 001 • Increased EEM area greater than the increase in plaque area or in the absence of an increase in plaque • Thrombus dissolution EEM CSA (mm 2) (Ako et al. J Am Coll Cardiol 2005; 46: 1002 -5) (Hong et al. Circulation 2006; 113: 414 -9)

Serial (post-stenting and 6 -month and 2 -year follow-up) IVUS analysis of LSM at Asan Medical Center • Among 250 patients with complete serial IVUS data, LSM was identified at 6 months in 19 (7. 6%). An additional 23 LSM were identified at 2 years. Because no LSM resolved between 6 months and 2 years, the LSM at 2 years was 12. 8%. • LSM noted at 6 months continued to increase from 6 months to 2 years and correlated to the ongoing increases in EEM. (Kang et al. unpublished)

Underexpansion is often lumped with malapposition - even by people who should know better

“We have shown that in humans delayed healing is common with current DES and that in those that thrombose, other factors, such as hypersensitivity reaction, bifurcating and ostial stenting, penetration of a necrotic core, stent malapposition, and restenosis, may also be important predictors of thrombosis. ” (Luscher et al. Circulation 2007; 115: 1051 -8)

Correlation of IVUS Findings With Aspirates in 28 Pts with Very Late DES Thrombosis • 28 pts with very late DES ST and 26 controls (7 spontaneous MI, 4 early BMS thrombosis, 5 late BMS thrombosis, and 10 early DES thrombosis). • LSM was present in 73% of very late DES ST segments. Maximal LSM area measured 6. 2± 2. 4 mm 2, and length measured 9. 4± 9. 5 mm. LSM area exceeded 5. 0 mm 2 in 5 of 8 segments (63%) • LSM area was associated with total eosinophil count (p=0. 008) WBCs p-ANOVA Eosinophils Spontaneous MI 291± 94 7± 10 Early ST-BMS 146± 117 1± 1 Early ST-DES 73± 117 Very late ST-BMS 84± 50 2± 3 Very late ST-DES 283± 149 20± 24 0. 0001 (Cook et al. Circulation 2009; 120: 391 -9) 1± 2 P-ANOVA 0. 038

IVUS analysis of 23 very late DES thrombosis cases at Asan Medical Center • LSM was observed in 17 DES patients (73. 9%) • Disease progression with neointimal rupture within the stent was observed in 10 DES patients (43. 5%) and reference segment plaque rupture in another 5 DES patients (21. 7%) • Only two very late DES thrombosis patients had neither of these findings (Lee et al. J Am Coll Cardiol, in press)
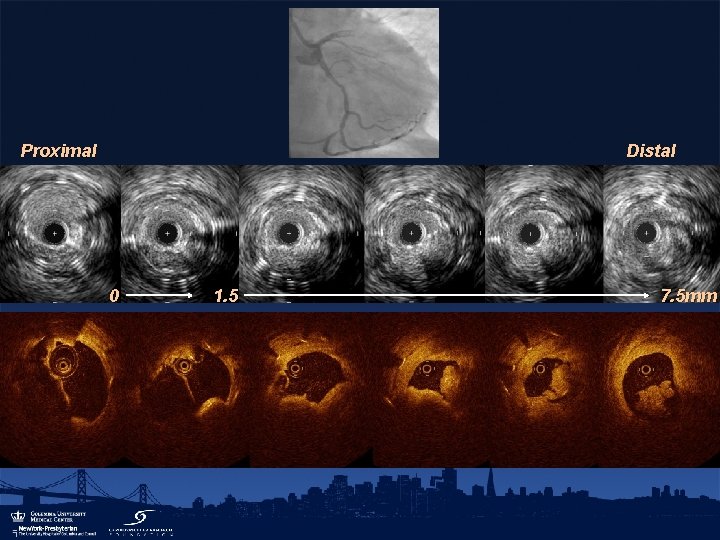
Proximal Distal 0 1. 5 7. 5 mm
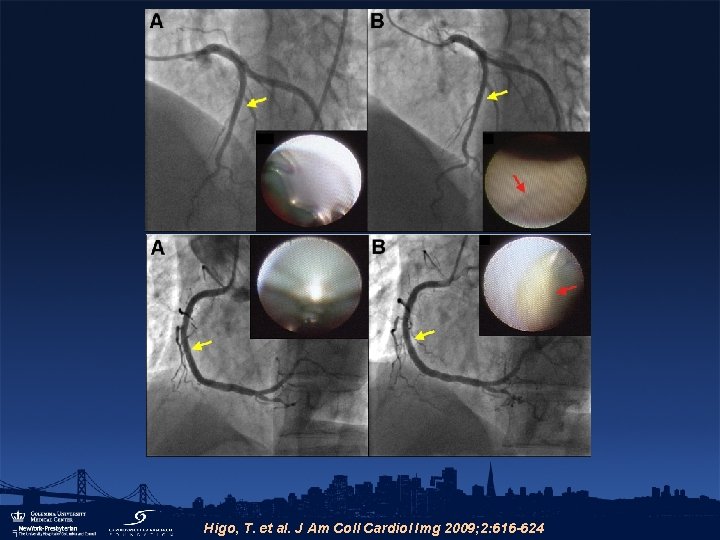
Higo, T. et al. J Am Coll Cardiol Img 2009; 2: 616 -624
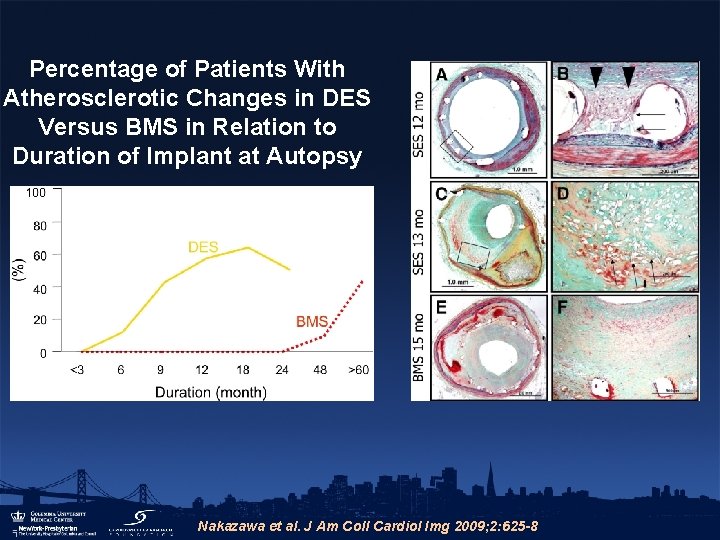
Percentage of Patients With Atherosclerotic Changes in DES Versus BMS in Relation to Duration of Implant at Autopsy Nakazawa et al. J Am Coll Cardiol Img 2009; 2: 625 -8
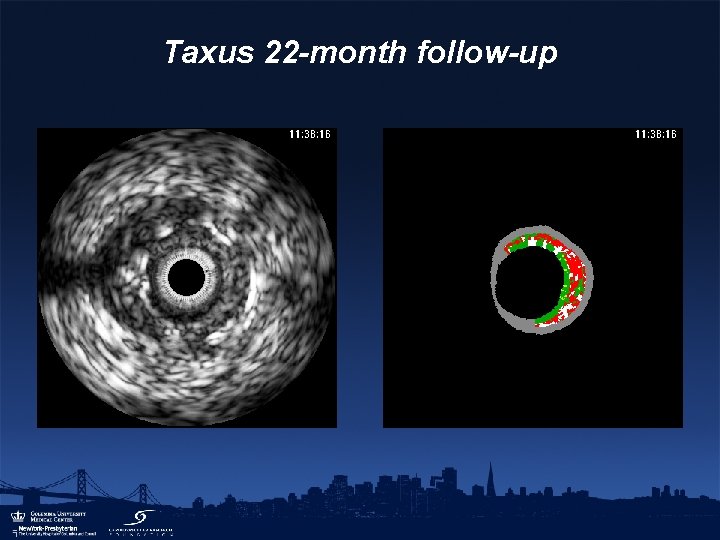
Taxus 22 -month follow-up

BMS 57 -month follow-up

1296 IVUS-guided, DES-treated lesions in 884 pts vs 1312 propensity-score-matched, angio -guided, DES-treated lesions in 884 pts IVUSguided Angioguided p MACE 2. 8% 5. 2% 0. 01 Stent thrombosis 0. 5% 1. 4% 0. 045 TLR 0. 7% 1. 7% 0. 045 MACE 14. 5% 16. 2% 0. 3 Definite stent thrombosis 0. 7% 2. 0% 0. 014 Probably stent thrombosis 4. 0% 5. 8% 0. 08 TLR 5. 1% 7. 2% 0. 06 0. 2% 0. 7% 0. 3 30 day 1 year Late definite stent thrombosis (Roy et al. Eur Heart J 2008; 29: 1851 -7)
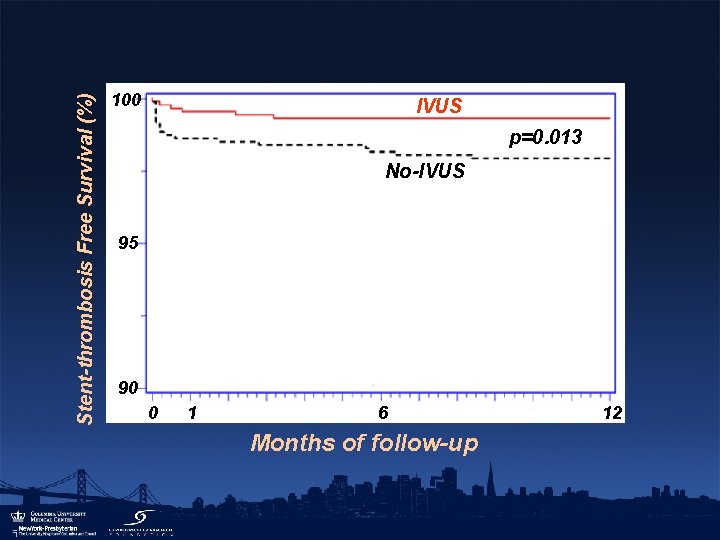
Stent-thrombosis Free Survival (%) 100 IVUS p=0. 013 No-IVUS 95 90 0 1 6 Months of follow-up 12
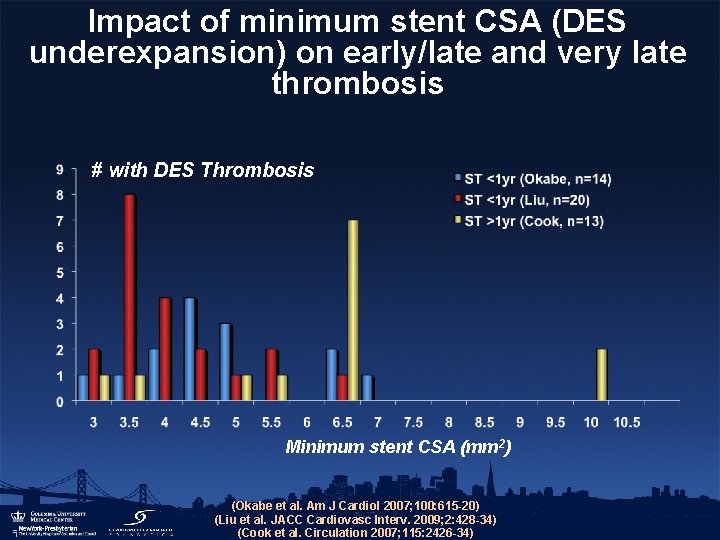
Impact of minimum stent CSA (DES underexpansion) on early/late and very late thrombosis # with DES Thrombosis Minimum stent CSA (mm 2) (Okabe et al. Am J Cardiol 2007; 100: 615 -20) (Liu et al. JACC Cardiovasc Interv. 2009; 2: 428 -34) (Cook et al. Circulation 2007; 115: 2426 -34)
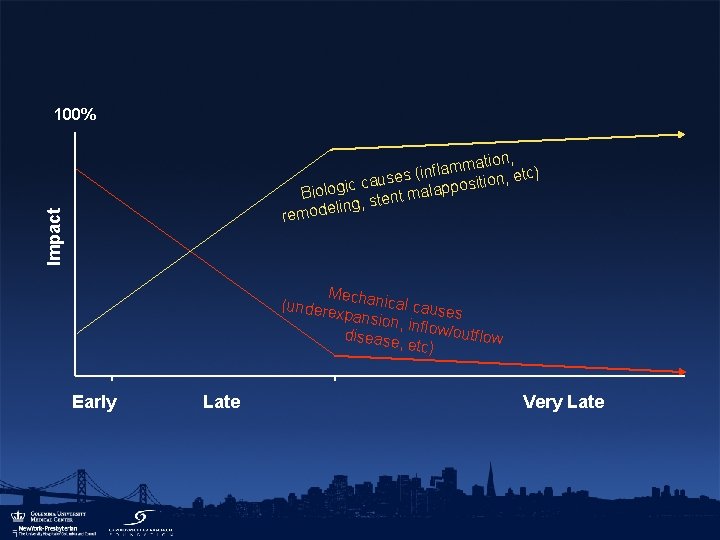
100% Impact tion, a m m a l f ses (in n, etc) u o i a t i c s c o i Biolog stent malapp ling, remode Mec (undere hanical causes xpansio n, in disease flow/outflow , etc) Early Late Very Late
- Slides: 27