Ive never been a problem patient experiences of

“I’ve never been a problem patient”: experiences of end of life care Dr Jo Ashby, Dr Sam Wright and Amanda Clayson #EOLC 2018

The research (strand 3) • To learn and understand more around the complexities of delivering end-of-life care to people with alcohol and other drug problems • Qualitatively driven - talking to people with a life-limiting conditions/end of life and alcohol/other drug problems

Ethical/moral challenges • How do you ensure that people at the end of life have the opportunity to take part in research respectfully? • How to define ‘end of life’ especially for those who do not engage with ‘traditional processes’ can be more typical of substance users? – Moral positioning of substance users/misusers • How do you approach initial conversations and guide the interview itself? • How do you look after yourself as a researcher when doing the fieldwork?

Person-centred Evolving Method • A process – ongoing reflection on ethics and use of process consent approach specifically commensurate to this kind of research work • Much of the literature focuses on ethical categories – important but does not account for the fluidity of chronically/ terminally ill • Beginning with initial ‘conversations’ and follow-up discussions about possible options – being flexible /available • Open mindedness around data collection/interview schedule/questioning • Follow up interviews- a chance to ‘pick up where we left off’ • Involvement of family members/carers
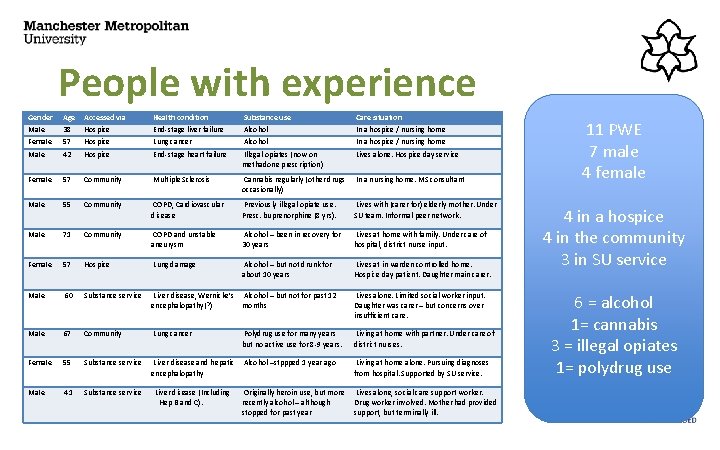
People with experience Gender Age Accessed via Health condition Substance use Care situation Male 38 Hospice End-stage liver failure Alcohol In a hospice / nursing home Female 57 Hospice Lung cancer Alcohol In a hospice / nursing home Male 42 Hospice End-stage heart failure Illegal opiates (now on methadone prescription) Lives alone. Hospice day service Female 57 Community Multiple Sclerosis Cannabis regularly (other drugs occasionally) In a nursing home. MS consultant Male 55 Community COPD, Cardiovascular disease Previously illegal opiate use. Presc. buprenorphine (8 yrs). Lives with (carer for) elderly mother. Under SU team. Informal peer network. Male 71 Community COPD and unstable aneurysm Alcohol – been in recovery for 30 years Lives at home with family. Under care of hospital, district nurse input. Female 57 Hospice Lung damage Alcohol – but not drunk for about 10 years Lives at in warden controlled home. Hospice day patient. Daughter main carer. Male 60 Substance service Liver disease, Wernicke’s Alcohol – but not for past 12 encephalopathy(? ) months Lives alone. Limited social worker input. Daughter was carer – but concerns over insufficient care. Male 67 Community Lung cancer Living at home with partner. Under care of district nurses. Female 55 Substance service Liver disease and hepatic Alcohol –stppped 1 year ago encephalopathy Male 41 Substance service Liver disease (Including Hep B and C). Polydrug use for many years but no active use for 8 -9 years. Living at home alone. Pursuing diagnoses from hospital. Supported by SU service. Originally heroin use, but more Lives alone, social care support worker. recently alcohol – although Drug worker involved. Mother had provided stopped for past year support, but terminally ill. 11 PWE 7 male 4 female 4 in a hospice 4 in the community 3 in SU service 6 = alcohol 1= cannabis 3 = illegal opiates 1= polydrug use

Current health and care Life-shortening condition 4 liver failure 3 COPD (and other comorbidities) 2 lung cancer 1 Heart failure 1 Multiple sclerosis Care situation 5 living alone 3 living with family (1 with partner; 1 with adult child and his partner; 1 with mother who he cares for) 2 temporarily hospice inpatients (awaiting move to nursing home) 1 residing in nursing home
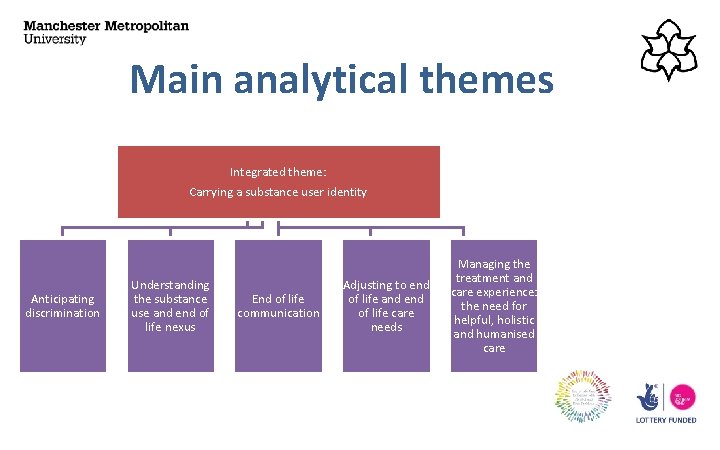
Main analytical themes Integrated theme: Carrying a substance user identity Anticipating discrimination Understanding the substance use and end of life nexus End of life communication Adjusting to end of life and end of life care needs Managing the treatment and care experience: the need for helpful, holistic and humanised care

Anticipation of discrimination (Jake, 71) Anticipation of discrimination was evident, carrying identity of drug user : thus it was important that Jake positioned himself as a ‘good patient’: ‘I’ve been in hospital a few times on and off over the years for all kinds of different things but as I say, I’ve never been a problem patient … on record, on my files as an IV user and yet they were giving me morphine … but the fact that I wasn’t abusing it, I wasn’t asking for it every two minutes … These look at me just like the next man … maybe the majority of them have no reason to have access to my file’

Perceived lack of compassion (Jake, 71) • 6 months later they told me about this place (hospice) and said “how do you feel about going there? ” … I was scratching my head thinking, “why do I need to go to a hospice? ” … the nurse explained, she said you know you’re very ill? ” and I’ve flippantly remarked, “no shit” … my heart is working at 14%, I know I’m ill”, she went, “no you’re really ill”, she went, “you could have as little as a year to three years to live” • I had this conversation with possibly half a dozen people at the hospital and at no time did anybody ever say, “the likelihood of you actually being here in ten years is next to zero” • It came across as almost flippantly mentioned but I think it was more a case of I think she presumed that I already knew.

Understanding substance use from end of life perspective: late presentation • ‘It pretty much all started about May this year, I was ill for about ten days with flu-like symptoms but I’m not a man-flu type person and this was quite severe. What had struck me down, there was other things like vomiting that made me think it wasn’t just flu. Just over a week and I went to a friend’s and said “do you mind if I stay for a few days? I’m really not feeling good”, I live on my own and I should put that in. I said “I’d just feel a bit better if there was somebody to keep an eye on me” and he said “yes”, obviously “stay as long as you like. ” Rob,

Barbara (57): Understanding her addiction • This is where the drink kicked in, • Took over because I could not cope, I didn’t know what to do • … my only way of dealing with it was drink, but I became dependent • But at that particular time, I didn’t know what alcohol dependency was, • I was like yes, I knew I’d got a drink problem but I wasn’t…, I wasn’t … • I didn’t go to the doctors because I didn’t think a doctor was needed, • I just had this dependency on alcohol because every time I stopped drinking, every time I got up in the morning, • I’d start to shake, “what the hell’s this” “what’s this? ”, and I’d have panic attacks and I’m thinking “what’s this” • I didn’t know what a panic was and so my coping mechanism was • “Ooh if I have a drink, the panic attack goes away” and that was how it started

Needing knowledge • After I’d had all my drains done and I’d been told I’d got cirrhosis, I didn’t really know much about cirrhosis, • The doctors told me “you’ve got ascites” • I thought, “what the hell is ascites? ” • I couldn’t spell it never mind know it at the time • And I was discharged from the hospital after two weeks of being drained. • … back to my dad said “ok I’ve got cirrhosis, I’ve been drained” • And within four weeks I was back in again because I was given no knowledge of diet, such as low salt, you can’t do this, you can’t do that • I didn’t pick up a drink but my stomach grew and I thought • “hang on a minute what’s going on here? ” • So I was back in again for another four weeks, where I had another two drains and I said to them look, • “I’m not leaving this hospital until somebody tells me what is going on”

To know me, you need to know my story … • • • I went to see the same gastroenterologist in 2014, my sister came with me and I always remember his words, He said “yes I remember you in 2008” He’s treated me as another person who just drank He didn’t know my background, he didn’t know I was abused mentally and physically. He didn’t know anything, but he just, he just saw a six stone alcoholic and that is all he could see There was no, no delving into my past And his words were in 2010, when I left, He said “we’ll discharge you now” he said, “but no doubt we’ll see you again in the future” Now how un-motivational is that?

‘They don’t judge me like that’ • I think in hospital, liver unit, they don’t have a liver unit, honestly, they only have a gastroenterology, • It’s horrible! It’s horrible to be spoken to like that! • Whereas the liver unit, they don’t look at you like that, you know, • I honestly don’t, I don’t drink, I haven’t had, I don’t touch the drink now for nearly a year but they don’t judge me like that, • They never have, they’ve looked at me as another patient. • But they, you know, they’ve never really said to me, “well, how did you start drinking in 2008? ” • It was just a bit of background that they were after

Emerging themes: Late presentation, unpredictable trajectories (1) Operating within a rigid treatment/healthcare system § Anticipation of negative attitudes / discrimination – leading to late presentation § Poor mobility / lack of confidence/knowledge in accessing services (appointments etc) § Passivity in patient role: unable to judge health priorities (2) Enhancing care needs § The need for compassion to effectively support – avoiding the ‘undeserving’ identity § The need for holistic approaches to address complex needs (i. e. SU and Palliative care) § Families ill-prepared to provide support; unlikely to seek help

Implications for policy and practice § Practice requires more compassionate care approaches to substance users § Beginning to ask: is more training around attitudes / understanding identity needed? § Practitioner training – deconstructing/reconstructing substance misusers? § Better and more effective lines of communication regarding end of life/ diagnosis/prognosis § Guidance to help communication with families/carers – how to tell children etc. § Flexibility in support/treatment – time, space and place need re-thinking in terms of adaptability / availability of services.

Summary • Complex interaction of multiple physical and mental health needs, selfidentity and social support In a context of: • Single-issue treatment pathways requiring high levels of understanding and assertiveness to identify different health needs and care priorities. • Holistic approaches needed for complex needs, communication; hospitals particularly perceived as poor • Without coordination, patients are vulnerable to poor (or in some cases non-existent) care.

Thank you • • Dr Jo Ashby Email: j. ashby@mmu. ac. uk Tel: 0161 247 2594 Twitter: @J 0 ashby @SUABMan. Met Professor Sarah Galvani Email: s. galvani@mmu. ac. uk Tel: 0161 247 2579 Twitter: @Sarah. Galvani @SUABMan. Met • Website: www. suab. com • •
- Slides: 18