Ischemic Heart Disease IHD coronary Heart Disease Introduction



















- Slides: 23

Ischemic Heart Disease (IHD – coronary Heart Disease) Introduction to Primary Care: a course of the Center of Post Graduate Studies in FM PO Box 27121 – Riyadh 11417 Tel: 4912326 – Fax: 4970847 1 1

objectives: At the end of this session the trainee will be able to • be able to discuss the burden of IHD. • describe essential elements in history taking & examination • develop a differential diagnosis of chest pain. • describe appropriate diagnostic testing for chest pain. • discuss modifiable & non modifiable risk factors for cardiac disease. • describe the use of investigation in the evaluation of a patient with chest pain. • appropriatly use of specialty referral.

Prevalence of IHD • Heart diseases responsible for overal deaths in the Saudi population: – IHD : 17% – Hypertensive heart disease 9% – CVA : 4% 18 th scientific session of the Saudi Heart Association. 2007 http: //www. highbeam. com/doc/1 G 1 -158905180. html

History taking in CAD • Patient characteristics (Name, age, sex, occupation) • Pain (duration, location, intensity, nature, aggravating factors • Associated symptoms (Dyspnea, syncope…. etc) • Past history (HPN, DM, COPD. . ETC) • Family history (coronary artery disease , pneumothorax) • Drug history (antiangina, anti diabetic. . etc) • Life style (Diet, exercise, alcohol, smoking ) • Psychosocial (ICE, anxiety, stress )

What characteristics of the chest pain might make you more concerned for cardiac chest pain? • • • Location Associated Symptoms Quality Chronology Onset • • • Duration Intensity Exacerbating Relieving Situation

Physical Examination • General Examination – patient status: stable, notstable, inpain or not in pain. – Vital signs. – Obese or overweight. – Skin appearance. • Cardiovascular &respiratory system examination – BP, Pulse rate, JVP. – Chest : apex beat deviation, crepitations, decrease breath sounds. – Heart : 1 st & 2 nd heart sounds, gallop, friction rub. – Abdomen: tenderness, guadring….

Any exam findings that might help distinguish cardiac from non cardiac chest pain? • General Appearance – may suggest seriousness of symptoms. • Vital signs – marked difference in blood pressure between arms suggests aortic dissection • Palpate the chest wall – Hyperesthesia may be due to herpes zoster • Complete cardiac examination – pericardial rub – Ischemia may result in MI murmur, S 4 or S 3 • Determine if breath sounds are symmetric and if wheezes, crackles or evidence of consolidation

What would be the differential diagnosis for chest pain?

Life threatening Causes Non-life threatening Causes Cardiovascular(16%): • Myocardial infarct. • Angina. • Thoracic aortic dissection. Chest wall (33%): • Trauma • Fracture • Costo-chondritis. • Musculoskeletal. Pulmonary (5%): • Pulmonary embolus. • Pulmonary infarction. • Tension pneumothorax. • Pneumonia. • Pleurisy. • Gastrointistinal(20%): • Esophageal spasm • Esophagitis. • Gall bladder disease. • Peptic ulcer disease. • pancreatitis Psychatric (9%): • Anxiety. Spinal dysfunction: • Cervical disease. . . Infections (rare): • Herpes Zoster.

The risk factors for CAD • • • Age > 45 (male) and >55 (female). Smoking. Family history. Hyperlipidemia. Diabetes. Hypertension. Obesity. Sedentary life style. Anxiety. Drug addiction. Past History.

Any tests that might help in diagnosis? • History and Examination • ECG • Cardiac Enzymes • Chest x-ray. • Upper GI endoscopy.

Cont… • ECG üST elevation of > 1 mm or new Q in 2 leads – Sensitivity 45% üAbove + ST depression or T-wave inversion – Sensitivity 79% – False positive rate = 17% ü 20% of patients having an MI will have a normal ECG initally

Cont… Cardiac enzymes: • Troponin, CK, myoglobin – 88 -90% sensitive at 4 -6 hours – 95 -100% sensitive 8 -12 hours Source: Am Heart J 1998 Aug; 136(2): 237 -44


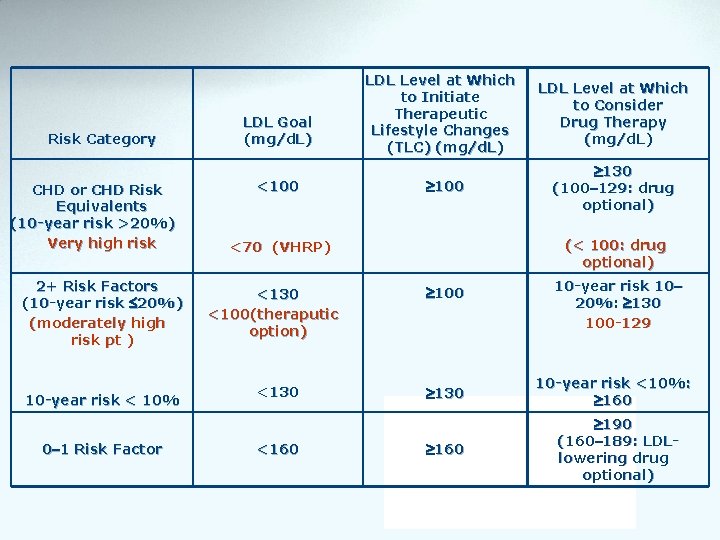
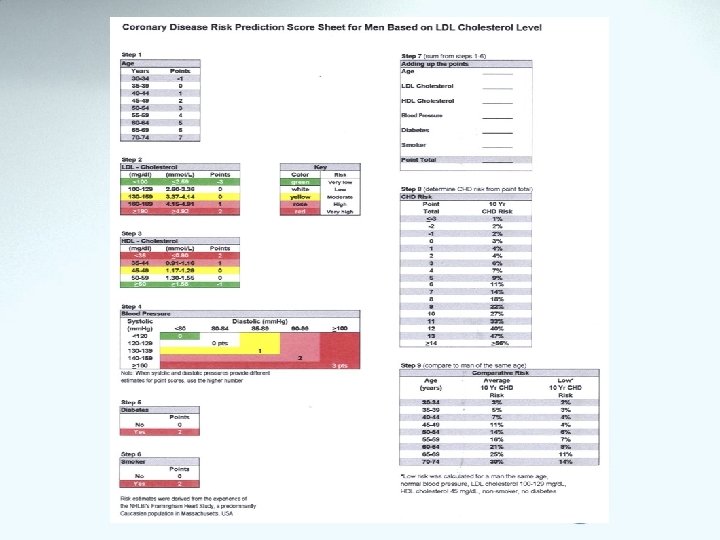
Risk Category CHD or CHD Risk Equivalents (10 -year risk >20%) Very high risk 2+ Risk Factors (10 -year risk 20%) (moderately high risk pt ) 10 -year risk < 10% 0– 1 Risk Factor LDL Goal (mg/d. L) <100 LDL Level at Which to Initiate Therapeutic Lifestyle Changes (TLC) (mg/d. L) 100 <130 <160 130 (100– 129: drug optional) (< 100: drug optional) <70 (VHRP) <130 <100(theraputic option) LDL Level at Which to Consider Drug Therapy (mg/d. L) 100 130 160 10 -year risk 10– 20%: 130 100 -129 10 -year risk <10%: 160 190 (160– 189: LDLlowering drug optional)

• Diabetes is regarded as a CHD Risk Equivalent • 10 -year risk for CHD 20% • High mortality with established CHD – High mortality with acute MI – High mortality post acute MI

Initial Approach • • ABC assessment 100% Oxygen Aspirine Nitroglycerine IV access Morphine Monitoring ECG quickly

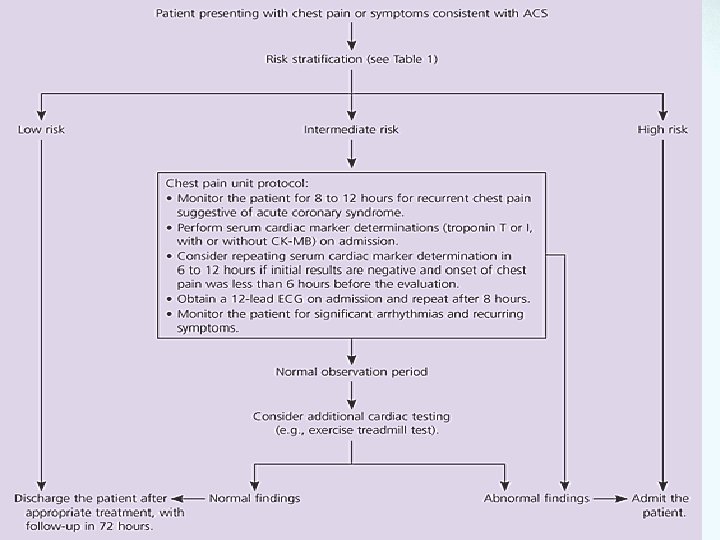
Action Plan

Action Plan Source: http: //www. aafp. org/afp/20050701/119. html

Referral Refer urgently all the serious conditions with chest pain: • • Cardiac causes. Esophageal spasm. Pulmonary embolism. Any other cases not responding to usual treatment.

Important Points • The likelihood of acute coronary syndrome (low, intermediate, high) should be determined in all patients who present with chest pain. • A 12 -lead ECG should be obtained within 10 minutes of presentation in patients with ongoing chest pain. • Cardiac markers (troponin T, troponin I, and/or creatine kinase. MB isoenzyme of creatine kinase) should be measured in any patient who has chest pain consistent with acute coronary syndrome. http: //www. aafp. org/afp/20050701/119. html

Important Points • A normal electrocardiogram does not rule out acute coronary syndrome. • When used by trained physicians, the Acute Cardiac Ischemia Time-Insensitive Predictive Instrument (a computerized, decision-making program built into the electrocardiogram machine) results in a significant reduction in hospital admissions of patients who do not have acute coronary syndrome. http: //www. aafp. org/afp/20050701/119. html
