Ischemic heart Disease Dr Rehab F Gwada Objectives
Ischemic heart Disease Dr. Rehab F. Gwada

Objectives of the Lecture • The student at the end of this lecture will be able Ø To define Ischemic heart disease (IHD)& identify associated risk factors according to scientific rational Ø To describe its causes &pathogenesis. Ø To differentiate between angina &AMI. Ø To explain sign & symptoms associated with IHD Ø to diagnose IHD according to scientific base. Ø To describe the strategies of management in patient with IHD according to scientific protocol.

Ischemic heart disease Definition Ischemic heart disease (IHD), or myocardial ischemia, or coronary artery disease is a disease characterized by reduced blood supply of the heart muscle, as a results of coronary artery narrowing or blocked usually due to atherosclerosis. • Partially blocked it causes angina. • Fully blocked it causes myocardial infarction or a heart attack
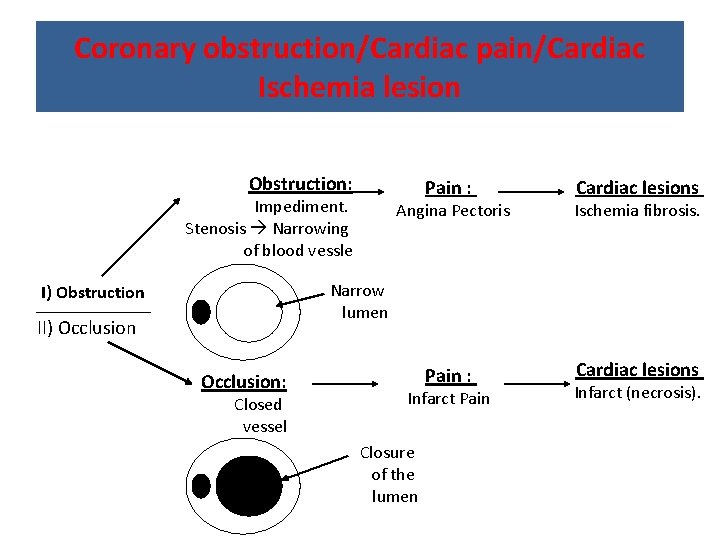
Coronary obstruction/Cardiac pain/Cardiac Ischemia lesion Obstruction: Pain : Impediment. Stenosis Narrowing of blood vessle Cardiac lesions Angina Pectoris Ischemia fibrosis. Pain : Cardiac lesions Narrow lumen I) Obstruction II) Occlusion: Closed vessel Infarct Pain Closure of the lumen Infarct (necrosis).
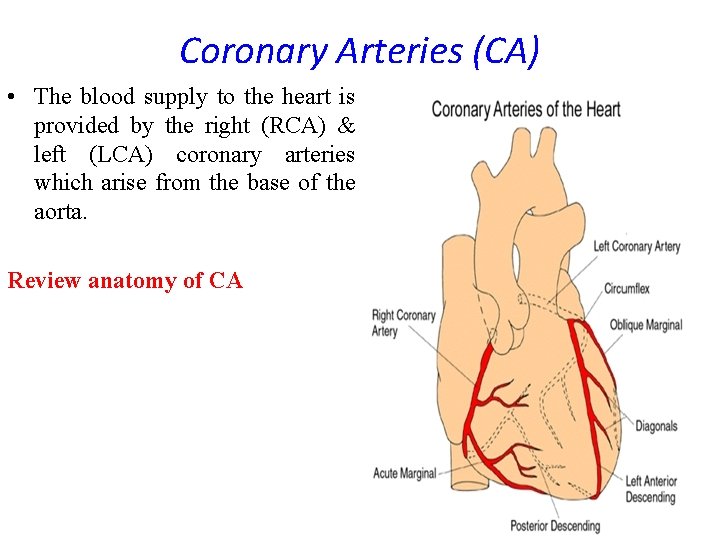
Coronary Arteries (CA) • The blood supply to the heart is provided by the right (RCA) & left (LCA) coronary arteries which arise from the base of the aorta. Review anatomy of CA

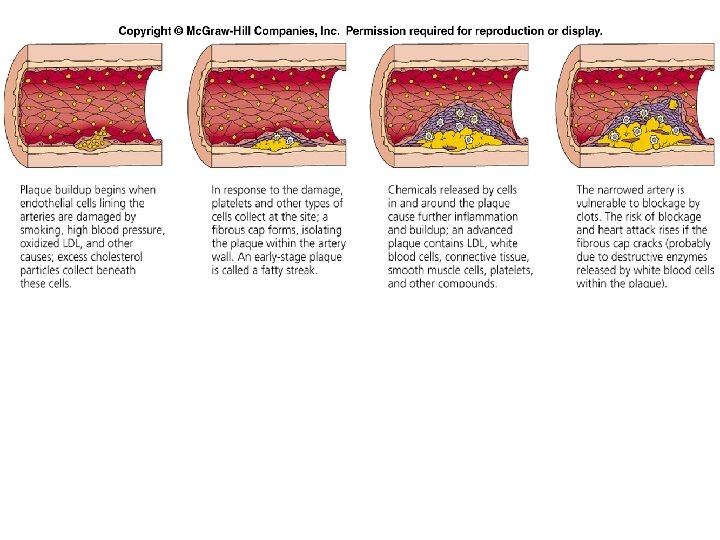
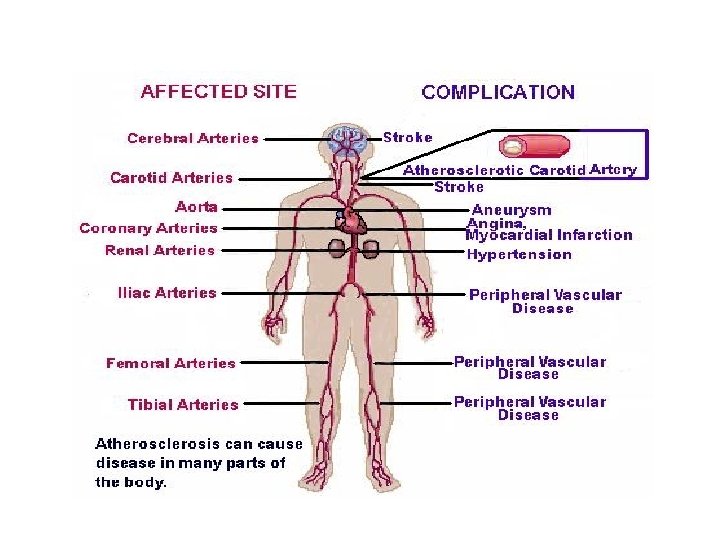
Atherosclerosis • Atherosclerosis is a slow, progressive disease which begins in childhood and takes decades to advance. • In which patchy deposits of fatty material(atherosclerotic plaque) develop in wall of arteries leading to reduced blood flow. • Plaque (the build-up of lipid/cholesterol, calcium fibrin, cell debris) in the artery wall forms as a response to injury to the endothelium in the artery wall.

Atherosclerosis Factors may injury endothelium cells lining the arteries : ü high BP ü elevated cholesterol and triglycerides(LDL) ü cigarette smoking
8

Presentation of Ischemic heart disease • Depending on the degree & character of the obstruction IHD results in : – Asymptomatic(silent) – angina (stable &unstable) – MI – Heart failure. – Arrhythmias – sudden cardiac death

Angina • Angina pectoris (chest pain on exertion, in cold weather or emotional situations). • It may be radiating • Association : sweating , dizziness, may be dyspnea (due to LVF) • NB: Silent ischemia : Dyspnea, fatigue & dizziness with no pain

Signs (during attack) Usually no abnormal finding • A positive Levine sign: the patient's fist clenched over the sternum when describing the pain. • Pallor, tachycardia & hypertension (sec. to sympathetic stimulation) • S 1: weak • S 2: reversed splitting • S 3: due to LVF • Murmur : due to papillary Ms. dysfunction

myocardial infarction ü myocardial infarction due to sudden , complete cessation of blood supply. ü new onset, intensification, nocturnal, prolonged chest pain unrelieved by rest ü IT associated with evidence of acute heart damage. & difficulty breathing ü need intervention. ü Most deaths from heart attacks occur within 2 hours from the onset of symptoms
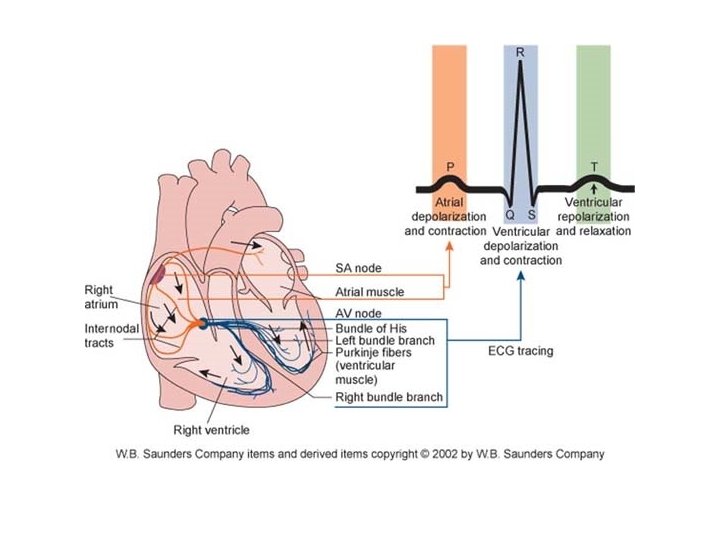
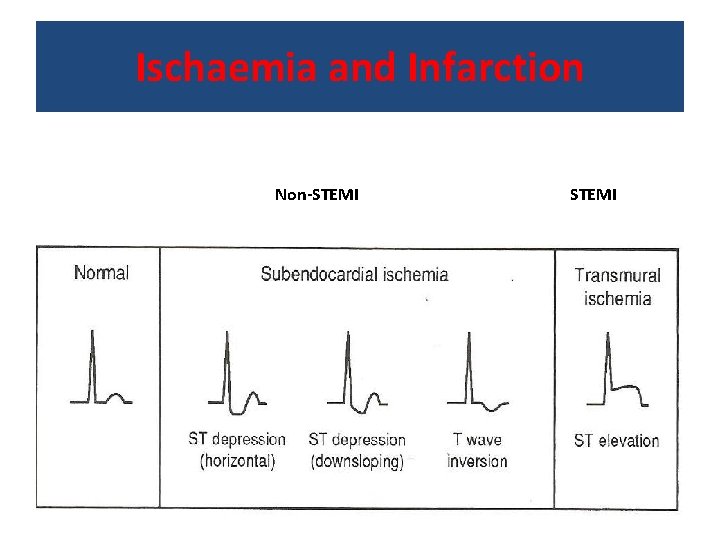
Ischaemia and Infarction Non-STEMI

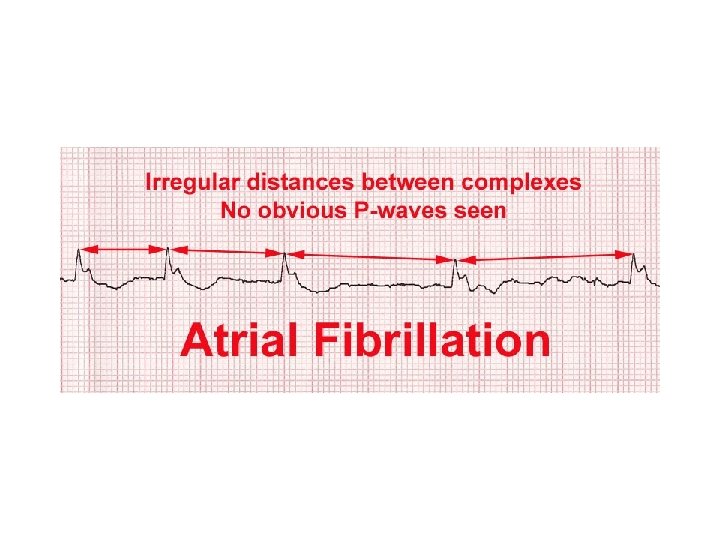
Arrhythmia • Arrhythmia: is an abnormality in the heart's rhythm or rate • All types may occur ü Tachycardia: Fast heartbeat > 100 beats/min in the absence of exercise or anxiety ü Brachycardia: Slow heartbeat < 60 beats/min ü Atrial flutter ü rapid, regular atrial rhythm ü ~ 300 beats/min ü Atrial fibrillation ü rapid, irregular atrial rhythm ü decreased CO ü Ventricular fibrillation – extremely rapid & irregular ü Premature Atrial Contractions (PAC) – Extra contraction or ectopic beats of atria
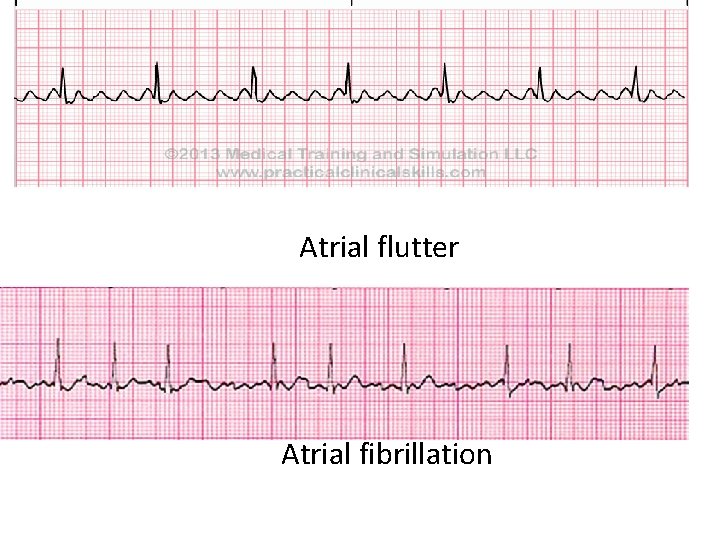
Atrial flutter Atrial fibrillation

Arrhythmia ü Premature ventricular contraction: Contraction of the ventricles, that occurs earlier than usual because of abnormal electrical activity of the ventricles. The premature contraction is followed by a pause; the contraction following the pause is usually more forceful than normal. These more forceful contractions are frequently perceived as palpitations. • http: //www. cardiachealth. org/premature-atrialcontractions-pacs • https: //www. youtube. com/watch? v=y. Ilw. Ht. Dszf 0&list= PLh. Suwhf. Ecqes 7 ABCcafdt 2 Lhyo. Y 0 hdm 0 p

Heart Failure • Heart unable to pump sufficient blood to meet metabolic needs of body • Endpoint for – – – coronary atherosclerosis(most common cause) HTN valve disease cardiomyopathy congenital cardiac malformation

Heart Failure(CHF) ü In LT ventricular failure, low CO causes systemic hypoperfusion & pulmonary venous congestion ü RT ventricular failure causes systemic venous congestion
Cardiac Arrest • Cessation of all activity in the heart • No conduction of impulses (flat line) • May occur : – Arrhythmia Ventricular fibrillation – Excessive vagal nerve stimulation (decreases heart) – Drug toxicity – Insufficient oxygen to maintain heart tissue – Massive Acute infarct • Blood flow to heart and brain must be maintained to resuscitate

Risk Factors for Ischemic Heart Disease • Age: – Male > 45 years – Female > 55 years or premature menopause without estrogen replacement therapy • Family History • Sex – male> female

Risk Factors for Ischemic Heart Disease • Hypertension – Appears to weaken the artery wall at points of high pressure leading to injury and invasion of cholesterol. • Cigarette Smoking – It reduces high-density lipoproteins& increase BP & HR.

Risk Factors for Ischemic Heart Disease o Diabetes o Inactivity o Sedentary person has double risk for developing CHD as a person who is active. o Obesity

Risk Factors for Ischemic Heart Disease • Abnormal Blood Lipids The recommended level of LDL & HDL cholesterol for adults is less than 100 mg/dl & 60 mg/dl or more respectively. Normal level of total cholesterol for adults is less than 200 mg/deciliter. The National Cholesterol Education Program recommends that all adults, beginning at age 20, have their lipoproteins measured at least once every 5 years. • LDL Cholesterol (low density lipoprotein) • HDL Cholesterol (high density lipoprotein)
Differential Diagnosis ü Dissecting aortic aneurysm ü Esophageal spasm. ü Musculoskletal chest pain

Diagnosis The nature of the symptoms. An electrocardiogram Coronary angiogram Stress testing An X-ray of the chest Cardiac enzymes {creatine kinase (CK), and troponin (T)}. • Echocardiogram • Blood tests may be performed. • • •

Strategies of Management • Depending on the symptoms and risk: Ø Modification of risk factors. • Medication can be given to control the blood flow to the heart. Ø Percutaneous coronary intervention(angioplasty) Ø Coronary artery bypass graft(CABG). Ø Rehabilitation

Thought question • In coronary heart disease patients , you prefer the resistance exercise, or moderate rhythmic aerobic exercise during rehabilitation program and why?

Management Treatment of coronary artery disease includes addressing "modifiable" risk factors. This includes • Suppression of cholesterol • Control of blood pressure, • Control of blood sugars (if diabetic), • Regular exercise alters blood fat levels by increase HDL • A healthy diet. ü increasing viscous (soluble) fiber intake which slows the rate at which food is broken down and nutrients like glucose are absorbed so it decreased risk of high blood cholesterol and diabetes. ü decreasing saturated & trans fat intake • Stop smoking

Cont. The role of physical therapy in MI , at the first 48 hours: ü To prevent the accumulation of secretions in the lung which may predispose to chest infection and complications ü Prevent stasis in the deep veins of the legs ü Improve the ventilation.

Quiz. • Sami is 56 years old and considers himself to be in good health. He has a family history of heart disease, stroke, and diabetes. He recently had a routine physical exam. He was told that his blood pressure was 130/85, his total cholesterol was 210 (LDL was 175 and HDL was 35), and his glucose levels were normal. He was also informed that his weight of 190 pounds made him about 10 pounds overweight. Sami's physician expressed some concern about the results of the exam. What finding is most likely the key cause of her concern? A. high cholesterol levels B. high blood pressure C. high weight D. high age

THANK YOU
- Slides: 34