IRRITABLE BOWEL SYNDROME AN EVIDENCEBASED APPROACH Joel J

IRRITABLE BOWEL SYNDROME AN EVIDENCE-BASED APPROACH Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Medical School

Learning Objectives • To accurately and confidently diagnose IBS in daily clinical practice with a high degree of sensitivity and specificity • To learn to provide appropriate and detailed education to patients with regard to dietary strategies • To treat and minimize symptoms of diarrhea- and constipation-predominant IBS (IBS-D, IBS-C) • To highlight pharmacologic and complimentary/alternative medicine strategies to improve symptoms in patients with both IBS-D and IBS-C • To review of current evidence-based AGA guidelines for pharmacologic treatment of IBS-D and IBS-C

Epidemiology Burden of Illness and Misconceptions

Prevalence of IBS • 1 – 20% in North America and Europe, depending upon casefinding definition (e. g. , Manning criteria vs. Rome criteria)1 • When specifically using Rome III criteria, pooled prevalence in US is 7%2, 3 • Community-based data indicate that IBS-D and IBS-M subtypes are more prevalent than IBS-C, yet switching and overlap may occur between groups in > 25% of cases 2, 3 • IBS is 1. 5 times more common in women than in men, yet commonly overlooked in men despite growing evidence 2, 3 • True prevalence across subtypes (IBS-D, IBS-C, IBS-M) is actually unknown due to challenge in reporting and definitions 1. Saito YA, et al. Am J Gastroenterol. 2002; 97: 1910 -1915. 2. Andrews EB, et al. Aliment Pharmacol Ther. 2005; 22: 935 -942. 3. Hungin AP, et al. Aliment Pharmacol Ther. 2005; 21: 1365 -1375.

High Prevalence and Incidence • Common in Western Europe and North America; less common in Asia • Decrease in reporting in older patients (Are abnormal stools really abnormal? ) • Annual incidence in primary care = 0. 8% • Annual prevalence in primary care = 3 – 4% • Average 14 hours lost work productivity per 40 -hour week • 2 nd to GERD in burden of GI illness – $1. 6 billion – direct costs – $19. 2 billion – indirect costs Hungin AP, et al. Aliment Pharmacol Ther. 2005; 21: 1365 -1375.

Demographic Predictors • • • Age, gender, socioeconomic status Odds higher in women than men (OR = 1. 46) Recognized as key component of Gulf War syndrome Patients under age 50 are more commonly diagnosed 2 – 6% of patients are over 50 years of age Graded decrease in prevalence with increasing income – 8 – 16% in those making less than $20, 000/year – 3 – 5% in those making more than $75, 000/year 1. Andrews EB, et al. Aliment Pharmacol Ther. 2005; 22: 935 -942. 2. Hungin AP, et al. Aliment Pharmacol Ther. 2005; 21: 1365 -1375.

IBS Myths and Misconceptions • Misconceptions – Purely a psychological-based diagnosis – Unknown mechanism(s) – Difficult to diagnose/“diagnosis of exclusion” • Reality – IBS is a REAL disorder and multifactorial – Majority of patients do not have psychological comorbidities! – Serotonin implicated in pathogenesis – Diagnosis can be made accurately in primary care!
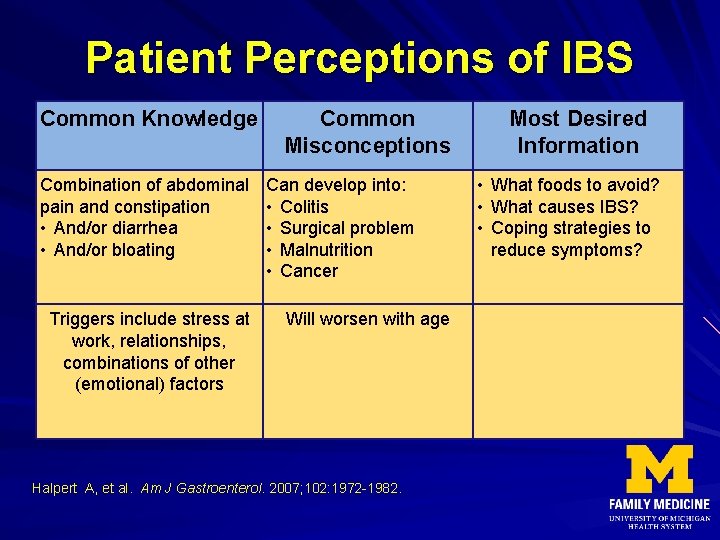
Patient Perceptions of IBS Common Knowledge Combination of abdominal pain and constipation • And/or diarrhea • And/or bloating Triggers include stress at work, relationships, combinations of other (emotional) factors Common Misconceptions Can develop into: • Colitis • Surgical problem • Malnutrition • Cancer Will worsen with age Halpert A, et al. Am J Gastroenterol. 2007; 102: 1972 -1982. Most Desired Information • What foods to avoid? • What causes IBS? • Coping strategies to reduce symptoms?

Primary Care Perceptions • 55 – 71% of PCPs identified stress or anxiety as causing or triggering IBS symptoms 1 • 45% of PCPs in UK defined IBS as a “nervous complaint” 2 • In 2 studies, 26% of PCPs in the Netherlands and 54% in the US believed that visceral hypersensitivity was an etiology of IBS 1, 3 – PCPs were significantly less likely than gastroenterologists to believe that visceral hypersensitivity plays a role in IBS, although the majority of PCPs believed that IBS is a disorder of both visceral hypersensitivity and gastrointestinal motility 1. Bijkerk CJ, et al. Can J Gastroenterol. 2003; 17: 363 -368. 2. Cox S, et al. BMC Fam Pract. 2004; 5: 22. 3. Lacy BE, et al. Scand J Gastroenterology. 2006; 41: 892 -902.

Health-Related Quality of Life • Patients with IBS have same physical HRQOL scores as patients with diabetes, and lower physical HRQOL scores than patients with depression and GERD 1, 2 • Psychological HRQOL scores are lower than patients with chronic renal failure, and can be so severe as to raise risk of suicidal behavior 3 1. El-Serag HB, et al. Aliment Pharmacol Ther. 2002; 16: 1171 -1185. 2. Gralnek IM, et al. Gastroenterology. 2000; 119: 654 -660. 3. Spiegel BMR, et al. Aliment Pharmacol Ther. 2007; 26: 183 -193.

Health-Related Quality of Life • IBS has an unquestionable negative impact on HRQOL in most patients • Failure to recognize this impact could undermine the physician-patient relationship and lead to dissatisfaction with care provided by the PCP • Imperative that PCPs: – Identify the predominant IBS symptom (C or D or M? ) – Gauge symptom severity – Understand the negative impact on HRQOL, especially relative to the psychological impact
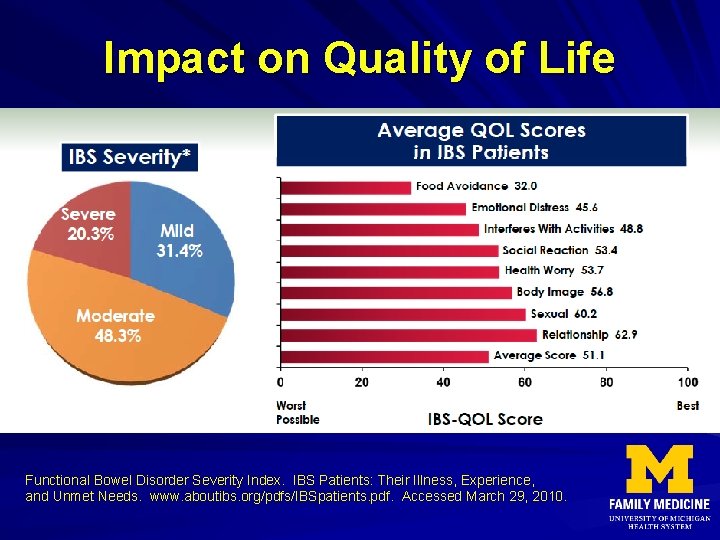
Impact on Quality of Life Functional Bowel Disorder Severity Index. IBS Patients: Their Illness, Experience, and Unmet Needs. www. aboutibs. org/pdfs/IBSpatients. pdf. Accessed March 29, 2010.

Other Associated Conditions • GI motility disorders – Dyspepsia, GERD, cyclic vomiting, gastroparesis, etc. • Psychiatric disorders – Anxiety, depression, somatoform disorders, PTSD • Chronic back pain • Fibromyalgia, chronic fatigue syndrome • Chronic headaches, “migraines” • Chronic pelvic pain – men and women • Functional urinary symptoms (e. g. , interstitial cystitis) • Dysmenorrhea • Sexual dysfunction

IBS and Symptom Overlap Frissora CL, Koch KL. Curr Gastroenterol Rep. 2005; 7: 264 -271.

Our Practices • Most cases of IBS are diagnosed by gastroenterology • Most research is done by gastroenterology • Most patients with all forms of IBS are managed by primary care! • Imperative that primary care has optimal understanding of perceptions and evidence behind diagnosis and treatment!

Diagnosis of Constipation-Related Functional GI Disorders
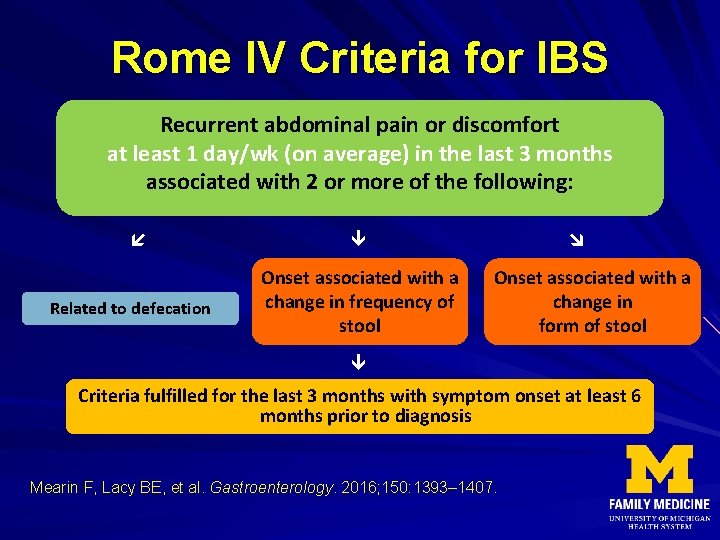
Rome IV Criteria for IBS Recurrent abdominal pain or discomfort at least 1 day/wk (on average) in the last 3 months associated with 2 or more of the following: Related to defecation Onset associated with a change in frequency of stool Onset associated with a change in form of stool Criteria fulfilled for the last 3 months with symptom onset at least 6 months prior to diagnosis Mearin F, Lacy BE, et al. Gastroenterology. 2016; 150: 1393– 1407.
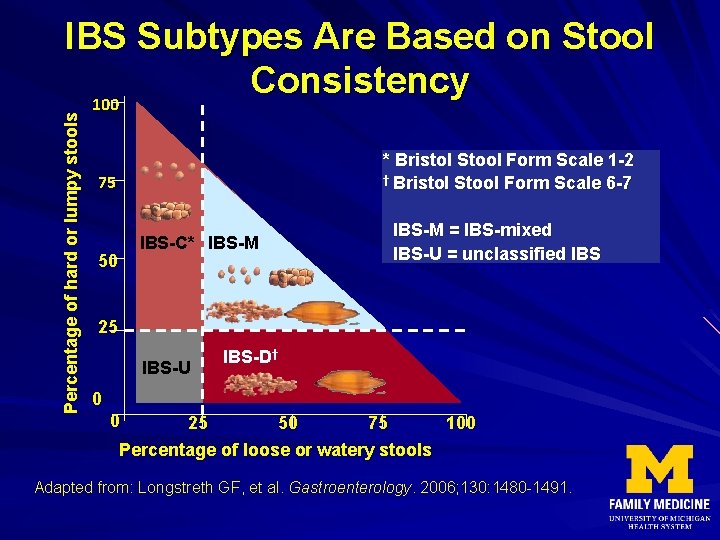
Percentage of hard or lumpy stools IBS Subtypes Are Based on Stool Consistency 100 * Bristol Stool Form Scale 1 -2 † Bristol Stool Form Scale 6 -7 75 IBS-C* IBS-M 50 IBS-M = IBS-mixed IBS-U = unclassified IBS 25 IBS-U IBS-D† 0 0 25 50 75 100 Percentage of loose or watery stools Adapted from: Longstreth GF, et al. Gastroenterology. 2006; 130: 1480 -1491.
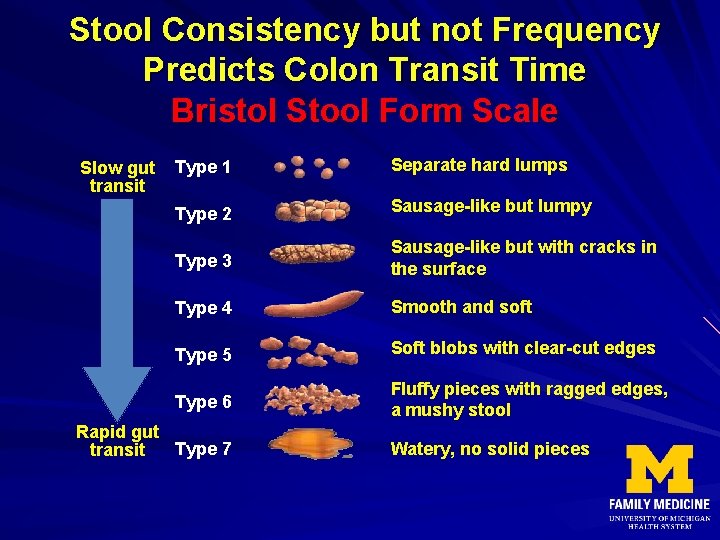
Stool Consistency but not Frequency Predicts Colon Transit Time Bristol Stool Form Scale Slow gut transit Type 1 Separate hard lumps Type 2 Sausage-like but lumpy Type 3 Sausage-like but with cracks in the surface Type 4 Smooth and soft Type 5 Soft blobs with clear-cut edges Type 6 Fluffy pieces with ragged edges, a mushy stool Rapid gut Type 7 transit Watery, no solid pieces

IBS-C vs. Chronic Constipation IBS-C CC Visceral Hypersensitivity Transit/Defecation = Pain

Subtypes of Constipation Slow-transit constipation 47% Dyssynergic defecation 59% IBS-C 58% Slow transit and IBS-C overlap in half of each group Recent SR found prevalence of STC to be 38%-80% Mertz H, et al. Am J Gastroenterol. 1999; 94: 609 -615. Rao SS, et al. Am J Gastroenterol. 2005; 100: 1605 -1615.
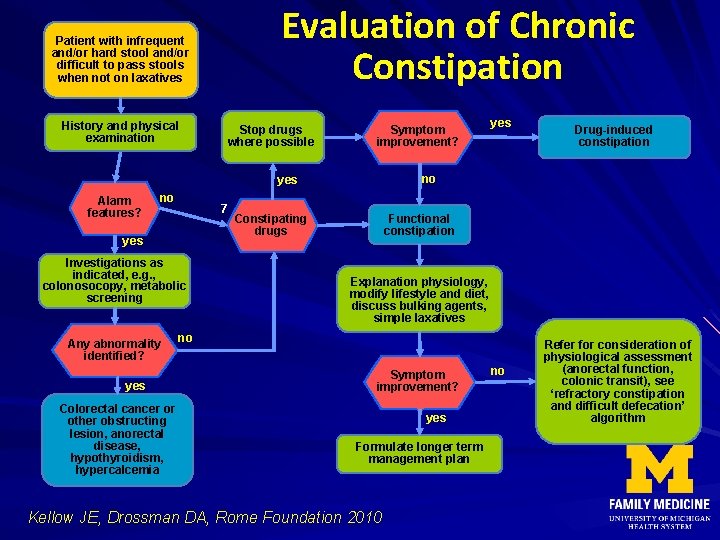
Evaluation of Chronic Constipation Patient with infrequent and/or hard stool and/or difficult to pass stools when not on laxatives History and physical examination Stop drugs where possible Symptom improvement? no 7 yes Investigations as indicated, e. g. , colonosocopy, metabolic screening Any abnormality identified? yes Colorectal cancer or other obstructing lesion, anorectal disease, hypothyroidism, hypercalcemia Drug-induced constipation no yes Alarm features? yes Constipating drugs Functional constipation Explanation physiology, modify lifestyle and diet, discuss bulking agents, simple laxatives no Symptom improvement? yes Formulate longer term management plan Kellow JE, Drossman DA, Rome Foundation 2010 no Refer for consideration of physiological assessment (anorectal function, colonic transit), see ‘refractory constipation and difficult defecation’ algorithm

Alarm Features for Chronic Constipation • Age > 50 years; > 45 years if African-American • New onset constipation in elderly • Severe symptoms not investigated • Rectal bleeding • Weight loss • Family history of organic GI disease • Palpable abdominal/rectal mass Paré P, et al. Can J Gastroenterol. 2007; 21(suppl B): 3 B– 22 B. Investigate and treat appropriately; colonoscopy may be indicated

When to Refer to a Specialist? • Warning Signs or Alarm Features • New onset of symptoms over age 50 • Rectal bleeding/bloody stools • Weight loss • Family history of colon cancer or inflammatory bowel disease • Abnormal physical examination • Severe or progressive symptoms • Failure to improve with fiber or laxative therapies

Rome IV: Limited Diagnostic Tests • In the appropriate patient, consider – CBC, ESR or CRP, fecal calprotectin – Celiac serologies • All patients do not require testing • No role for colonoscopy in all patients Mearin F, Lacy BE, et al. Gastroenterology. 2016; 150: 1393– 1407.

Evolving Schema of Treatment for Constipation-Related Functional GI Disorders

Improving Patient-Physician Interactions • • Listen (It’s hard; don’t interrupt) Understand fears Review goals Set expectations – Short-term – Long-term • Develop a logical treatment plan together • Arrange for routine follow-up

Managing IBS: What Do Your Patients Want? • They want you to listen – Understand their history (symptoms, work, home) • Education about their condition – Address questions or concerns – Address uncertainty of IBS • Reassurance • A positive diagnosis – Review results with patients • Symptom improvement
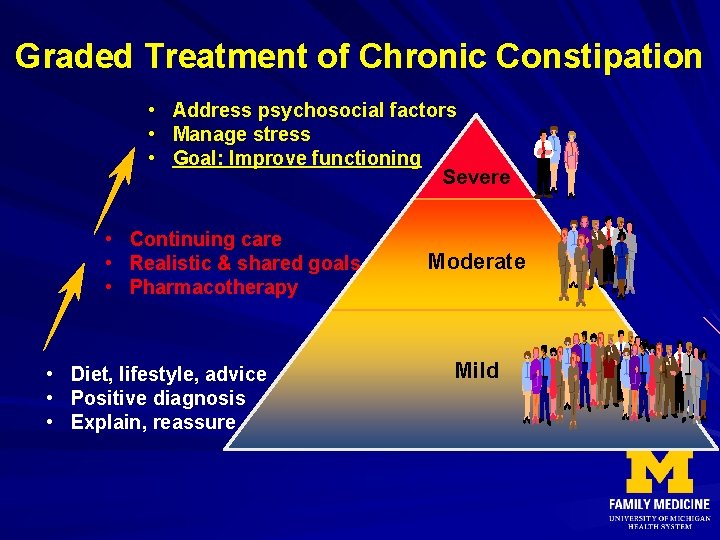
Graded Treatment of Chronic Constipation • Address psychosocial factors • Manage stress • Goal: Improve functioning Severe • Continuing care • Realistic & shared goals • Pharmacotherapy • Diet, lifestyle, advice • Positive diagnosis • Explain, reassure Moderate Mild

IBS & Low FODMAP Diet Quality of evidence: very low Shepherd SJ, et al. J Am Diet Assoc. 2006; 106: 1631 -1639. Shepherd SJ, et al. Clin Gastroenterol Hepatol. 2008; 6: 765 -771. Gibson PR, et al. J Gastroenterol Hepatol. 2010; 25: 252 -258.
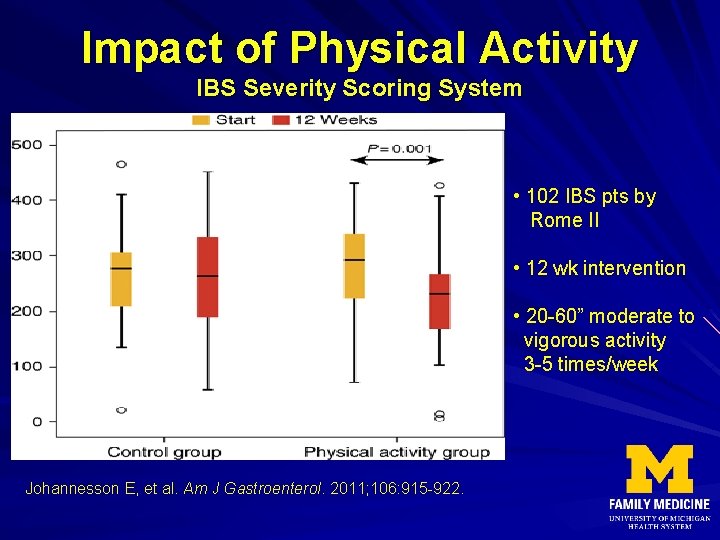
Impact of Physical Activity IBS Severity Scoring System • 102 IBS pts by Rome II • 12 wk intervention • 20 -60” moderate to vigorous activity 3 -5 times/week Johannesson E, et al. Am J Gastroenterol. 2011; 106: 915 -922.

Pharmacologic Treatments for IBS Modified from: Brandt LJ, et al. Am J Gastroenterol. 2009; 104(Suppl 1): S 1 -S 35.

Practical Advice on Fiber and Antispasmodics for IBS-C Fiber supplementation • Mild constipation symptoms • May or may not help with pain • Soluble probably better than insoluble • “Start low and titrate slow” • Gas and bloating are the main side effects Anti-spasmodics • For postprandial abdominal pain • Not effective for chronic abdominal pain • Avoid in the elderly Eswaran S, et al. Am J Gastroenterol. 2013; 108: 718 -727.

Fiber and Stool Softeners • Fiber and stool softeners (ducosate) are most useful in patients with mild, infrequent constipation • Best evidence for psyllium up to 25 grams/day • Their role in patients with significantly delayed colon transit or dyssynergia is limited • Fiber may worsen symptoms in patients with significantly delayed colon transit or dyssynergic defecation
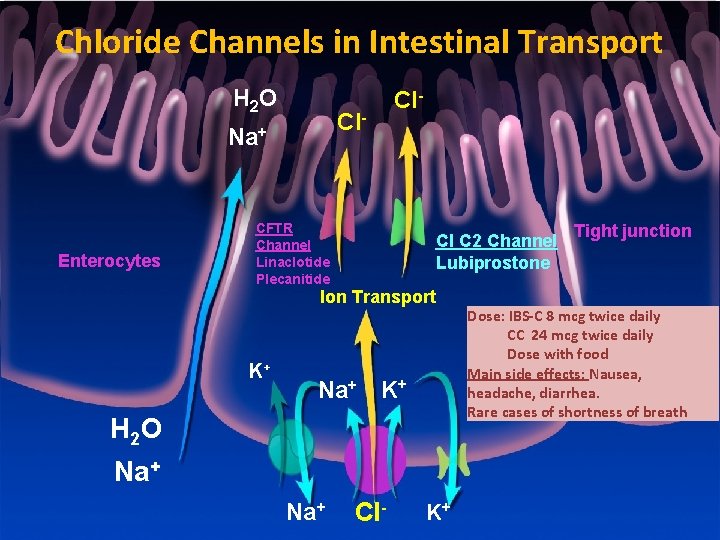
Chloride Channels in Intestinal Transport H 2 O Cl- Na+ Enterocytes Cl- CFTR Channel Linaclotide Plecanitide Cl C 2 Channel Lubiprostone Ion Transport K+ Na+ K+ H 2 O Na+ Cl- K+ Tight junction Dose: IBS-C 8 mcg twice daily CC 24 mcg twice daily Dose with food Main side effects: Nausea, headache, diarrhea. Rare cases of shortness of breath

Lubiprostone for IBS-C: Data From 2 Phase III Trials 50 % Overall 25 Responders * P=0. 001 • 12 -week treatment period • Overall responder = monthly responder for at least 2 of 3 months • Monthly responder = at least moderate relief for 4/4 weeks or significant relief for 2/4 weeks 17. 9 10. 1 0 Lubiprostone 8 mcg bid n=780 Drossman DA, et al. Aliment Pharmacol Ther. 2009; 29(3): 329 -341. Placebo n=387
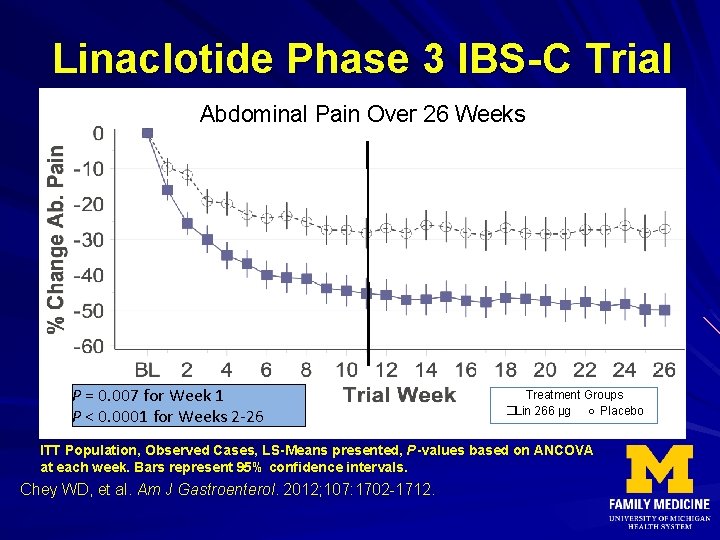
Linaclotide Phase 3 IBS-C Trial Abdominal Pain Over 26 Weeks P = 0. 007 for Week 1 P < 0. 0001 for Weeks 2 -26 Treatment Groups �Lin 266 µg ○ Placebo ITT Population, Observed Cases, LS-Means presented, P-values based on ANCOVA at each week. Bars represent 95% confidence intervals. Chey WD, et al. Am J Gastroenterol. 2012; 107: 1702 -1712.
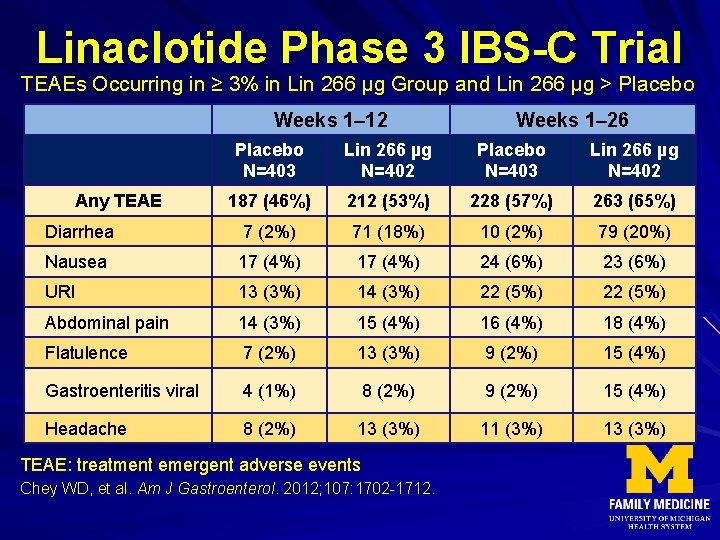
Linaclotide Phase 3 IBS-C Trial TEAEs Occurring in ≥ 3% in Lin 266 µg Group and Lin 266 µg > Placebo Weeks 1– 12 Weeks 1– 26 Placebo N=403 Lin 266 µg N=402 187 (46%) 212 (53%) 228 (57%) 263 (65%) Diarrhea 7 (2%) 71 (18%) 10 (2%) 79 (20%) Nausea 17 (4%) 24 (6%) 23 (6%) URI 13 (3%) 14 (3%) 22 (5%) Abdominal pain 14 (3%) 15 (4%) 16 (4%) 18 (4%) Flatulence 7 (2%) 13 (3%) 9 (2%) 15 (4%) Gastroenteritis viral 4 (1%) 8 (2%) 9 (2%) 15 (4%) Headache 8 (2%) 13 (3%) 11 (3%) 13 (3%) Any TEAE: treatment emergent adverse events Chey WD, et al. Am J Gastroenterol. 2012; 107: 1702 -1712.

Complementary and Alternative Treatments for Functional GI Disorders

Probiotics: Putative Mechanisms of Action • • • Competitive inhibition Barrier protection Immune effects Anti-inflammatory effects Production of various substances (enzymes, SCFA, bacteriocidal agents) • Ability to alter local p. H and physiology • Provides nutrition to colonocytes SCFA: short chain fatty acids Camilleri M. J Clin Gastroenterol. 2006; 40: 264 -269.

Probiotics and Constipation • B. lactis DN shortens colonic transit in healthy women and in the elderly 1 -3 – Observed only if live organisms used Probiotics Studied in Constipation 1, 2 – Most obvious if slow baseline colon transit • B. lactis DN-173 010 • L. rhamnosus, B. lactis, and inulin stimulate bowel motility 4 • E. coli Nissle 1917 • Data from 5 RCTs (n=377) suggest a favorable effect of treatment on defecation and stool consistency 3, 5 • Use should be considered investigational until further data are available 1. Marteau P, et al. Aliment Pharmacol Ther. 2002; 16: 587 -593. 2. Meance S, et al. Microb Ecol Health Dis. 2001; 13: 217 -222. 3. Quigley EMM. Best Pract Res Clin Gastroenterol. 2011; 25: 119 -126. 4. Lesniewska V, et al. Exp Phsyiol. 2006; 91: 229 -237. 5. Chmielewska A, Szajewska H. World J Gastroenterol. 2010; 16: 69 -75. • L. casei Shirota

Randomized Trial of Dried Plums for Chronic Constipation • Dried plums contain large amounts of fiber and sorbitol • 8 -week RCT single-blinded cross-over study examined treatment with dried plums (prunes, 50 g/day or 6 prunes) compared with psyllium (11 g/day fiber) taken BID – 40 patients with chronic constipation – Dried plums resulted in a greater improvement in constipation symptoms compared with psyllium • More CSBMs (3. 5 ± 0. 2 vs 2. 8 ± 0. 2, P = 0. 006) • Softer stools (3. 2 vs 2. 8 on the BSFS, P = 0. 02) • Overall constipation symptoms (both groups improved, NS) Attaluri A, et al. Aliment Pharmacol Ther. 2011; 33(7): 822 -828.

AGA Guideline for Pharmacologic Treatment of IBS • Multidisciplinary guideline development – Gastroenterologists – Epidemiologists – Primary Care – Patient Representative – Rigorous COI exclusions (NB: No one is paid!) • Clinical Practice and Quality Measures Committee – Guideline – Technical Review

AGA Guideline for Pharmacologic Treatment of IBS • GRADE Methodology – Grading of Recommendations Assessment, Development, and Evaluation System – High/Moderate/Low Quality Evidence – Strong/Conditional (Weak) Strength of Evidence • PICO – Patient Problem or Population – Intervention – Comparison – Outcome(s)

AGA Guideline for Pharmacologic Treatment of IBS 1. Use linactolide (over no drug tx) in IBS-C 1 1. - Strong recommendation; high quality evidence 2. Use lubiprostone (over no drug tx) in IBS-C 1 1. - Conditional recommendation; moderate quality evidence 3. Use laxatives [PEG] (over no drug tx) in IBS-C 1. - Conditional recommendation; low quality evidence 4. Use rifaximin (over no drug tx) in IBS-D 2 1. Conditional recommendation; moderate quality evidence 2. 1 Pts who value avoiding higher out-of-pocket costs may prefer alternate treatments 3. 2 Not approved by FDA, cost may be high, no evidence to support repetitive treatment Weinberg DS, Smalley W, Heidelbaugh JJ, Sultan S. American Gastroenterological Association Institute Guideline on the Pharmacological Management of Irritable Bowel Syndrome. Gastroenterology 2014; 147(5): 1146 -1148.

AGA Guideline for Pharmacologic Treatment of IBS 5. Use alosetron (over no drug tx) in IBS-D - Conditional recommendation; moderate evidence 6. Use loperamide (over no drug tx) in IBS-D - Conditional recommendation; very low quality evidence 7. Use TCAs (over no drug tx) in IBS - Conditional recommendation; low quality evidence 8. Do not use SSRIs for IBS patients - Conditional recommendation; low quality evidence 9. Use antispasmodics (over no drug tx) in IBS - Conditional recommendation; low quality evidence Weinberg DS, Smalley W, Heidelbaugh JJ, Sultan S. American Gastroenterological Association Institute Guideline on the Pharmacological Management of Irritable Bowel Syndrome. Gastroenterology 2014; 147(5): 1146 -1148.

SUMMARY • Constipation is a multi-symptom condition that must be appropriately defined in our respective patients • The main causes of constipation are slow colon transit and/or disordered defecation • *Diet and lifestyle changes can help with mild, moderate, or intermittent constipation symptoms and should always be tried first • Laxatives including osmotics, stimulants, and prosecretory agents, improve symptoms in many patients • Biofeedback and physical therapy are the preferred treatments for dyssynergic defecation and have modest results • When patients fail to respond to laxatives, diagnostic testing can help to determine the etiology of constipation symptoms • Gain skill in using newer agents, know when to refer to GI • A multi-disciplinary approach is optimal for severely affected patients

QUESTIONS ?
- Slides: 48