Invasive Pneumococcal Disease Streptococcus pneumoniae Clinical Syndromes Meningitis








- Slides: 16

Invasive Pneumococcal Disease Streptococcus pneumoniae

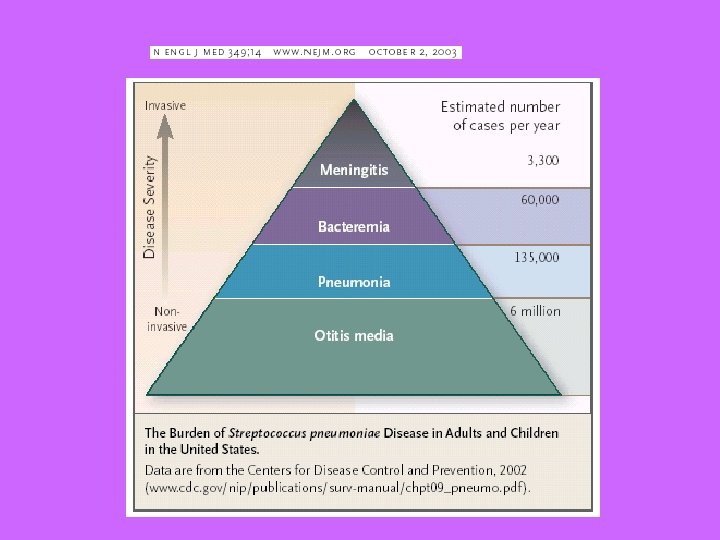
Clinical Syndromes • Meningitis: fever, headache, photophobia, nausea, vomiting, nuchal rigidity • Bacteremia: fever, chills, (+/-)mental status or behavioral changes • Pneumonia: fever, chills, productive cough, pleuritic chest pain • Otitis media: fever, ear pain, lack of appetite, irritability


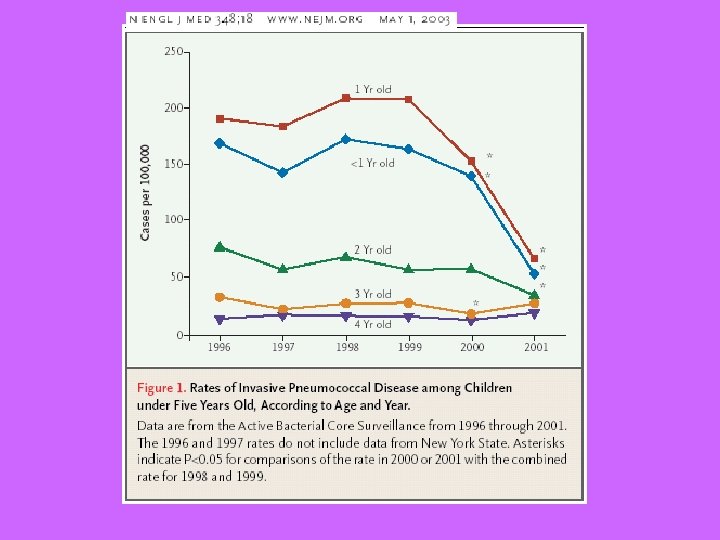
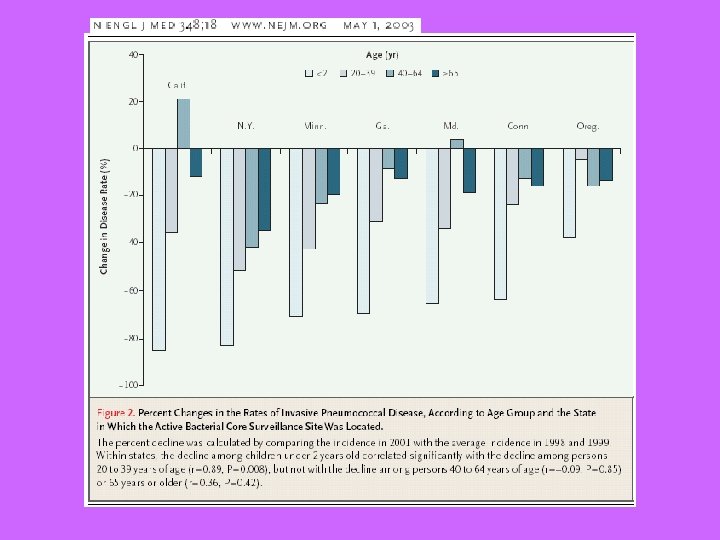
Conjugate Vaccine (2000) MMWR, 2000; 49 (No RR-9) • 7 serotypes of capsular polysaccharide (4, 9 V, 14, 19 F, 23 F, 18 C, 6 B) linked to a protein carrier • Recommended for: – Children < 23 months – Children 24 -59 months with • Sickle cell* or trait, beta-thalassemia, functional or anatomic asplenia* • HIV* • Chronic disease*, including chronic heart or lung disease, diabetes, or CSF leak; cochlear implant • Immunocompromising conditions* *revaccinate (23 -valent polysaccharide vaccine after age 2)

Polysaccharide vaccine (1983) MMWR, 1997; 46(No RR-8) • 23 polysaccharide antigens • Recommended for: – Persons > 65 years – Persons age 2 -64 with: • • • Chronic heart or lung disease or diabetes; cochlear implant Alcoholism, chronic liver disease or CSF leaks Functional or anatomic asplenia* Living in special environments or social settings Immunocompromising conditions* *revaccinate

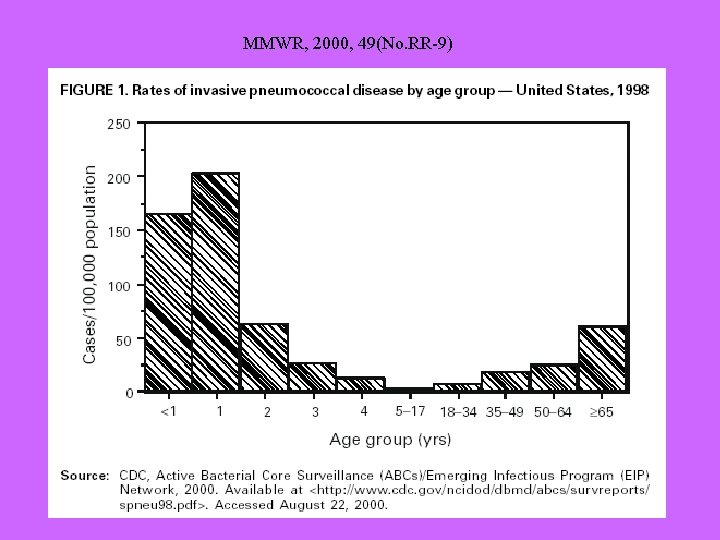
MMWR, 2000, 49(No. RR-9)



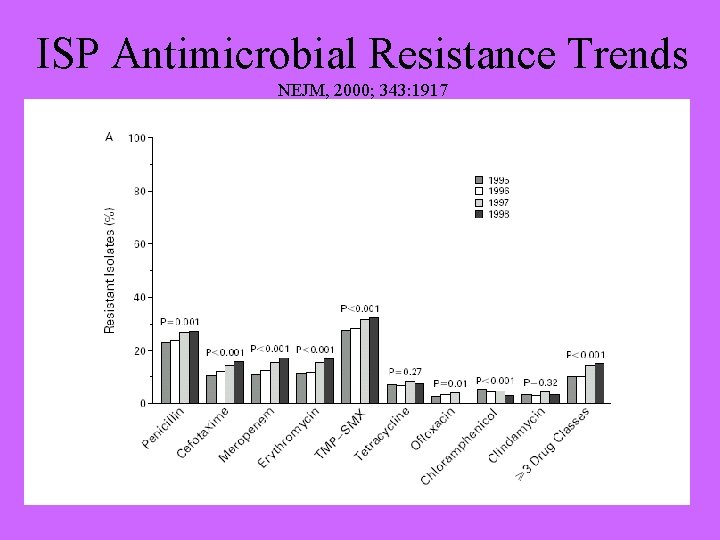
ISP Antimicrobial Resistance Trends NEJM, 2000; 343: 1917

Case Definition • Clinical description Streptococcus pneumoniae causes many clinical syndromes, depending on the site of infection (e. g. , acute otitis media, pneumonia, bacteremia, or meningitis). • Laboratory criteria for diagnosis Isolation of S. pneumoniae from a normally sterile site (e. g. , blood, cerebrospinal fluid, or, less commonly, joint, pleural, or pericardial fluid) • Case classification – Confirmed: a clinically compatible case caused by laboratory-confirmed culture of S. pneumoniae from a normally sterile site

Public Health Action • Confirm the case • Use the supplemental form to guide you in asking important questions: – What was the site of infection? – Did the case have underlying disease? – What is the immunization status of the case? • Attach laboratory results and antimicrobial susceptibility studies

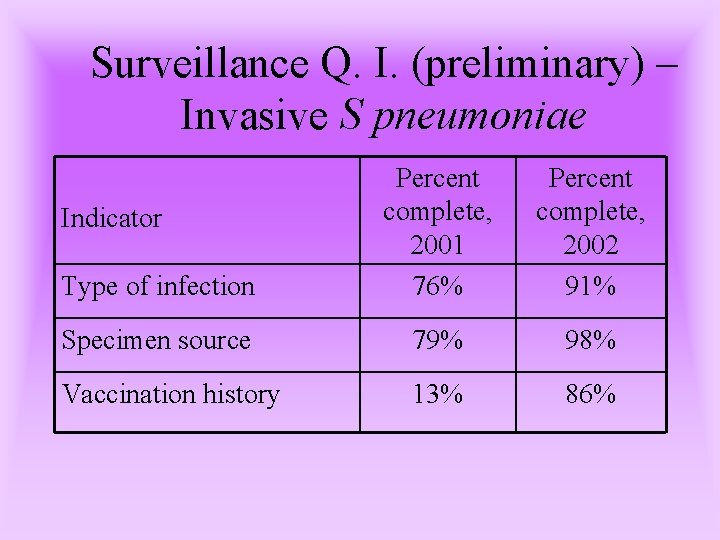
Surveillance Q. I. (preliminary) – Invasive S pneumoniae Type of infection Percent complete, 2001 76% Percent complete, 2002 91% Specimen source 79% 98% Vaccination history 13% 86% Indicator

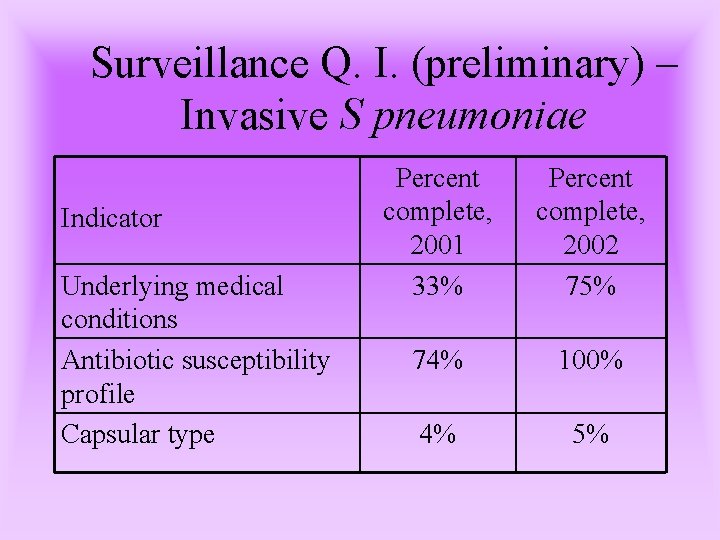
Surveillance Q. I. (preliminary) – Invasive S pneumoniae Indicator Underlying medical conditions Antibiotic susceptibility profile Capsular type Percent complete, 2001 33% Percent complete, 2002 75% 74% 100% 4% 5%

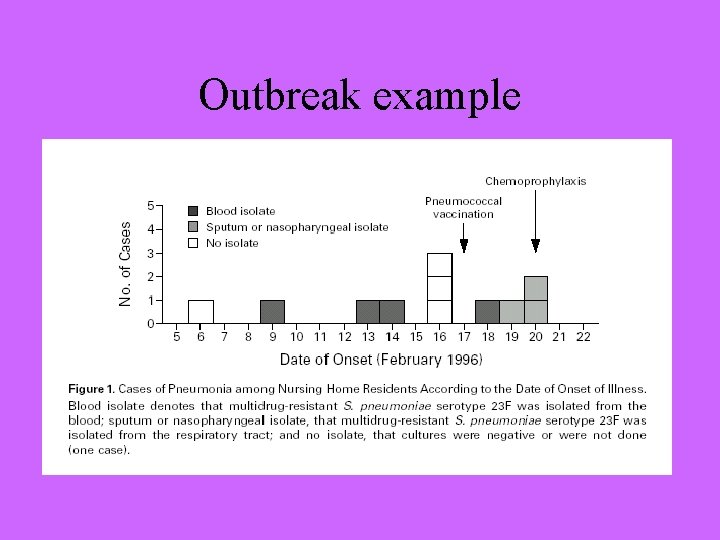
Outbreak example

Outbreak Example (2) • Pneumonia in 11 (13%) of 84 nursing home residents – 3 deaths • S pneumoniae serotype 23 F, – intermediate resistance to penicillin, cefotaxime; resistant to trimethoprim sulfamethoxazole and erythromycin; and sensitive only to vancomycin, rifampin and ofloxacin • 3 (4%) of residents had been vaccinated • 20 (27%) of 74 residents and 12 (17%) of 69 staff were colonized with the outbreak strain

ISP - Summary • Risk – Highest in the very young and the very old • Vaccine-preventable disease • Antimicrobial resistance increasing • Investigation: – – Site of infection Vaccination history Underlying disease Antimicrobial resistance profile