Invasive Mechanical Ventilation Weaning Intolerance Indicators Box 16

Invasive Mechanical Ventilation � Weaning Intolerance Indicators (Box 16 -1) �Decreased LOC �SBP increased or decreased by 20 mm. Hg �DBP > 100 mm. Hg �HR increased by 20 beats/min �Resp. rate increase by 10/min (> 30 or < 10) �Use of accessory muscles �Pa. CO 2 increase of 5 -8 &/or p. H < 7. 3 �Sp. O 2 < 90% Copyright © 2004, Elsevier (USA). All rights reserved. Chapter 16

Noninvasive Mechanical Ventilation � Advantages �Decreased incidence of nosocomial pneumonia �Increased comfort �More efficient delivery of preset tidal volume � Nursing Management �Assessment and patient compliance �Properly fitted mask �Skin integrity �Head of bed elevated 45 degrees to prevent aspiration �Avoid sedation Chapter 13 -2 Copyright © 2004, Elsevier (USA). All rights reserved.

Acute Respiratory Failure � Description �Acute Respiratory Failure abbreviated as ARF �A clinical condition where the pulmonary system fails to maintain adequate gas exchange �Mortality �May rate of 22% - 75% be classified as: Type I or Type II �Type I: Low Pa. O 2 and Normal Pa. CO 2 �Type II: Low Pa. O 2 and High Pa. CO 2 Chapter 15 Copyright © 2004, Elsevier (USA). All rights reserved.

Acute Respiratory Failure(P. � Pathophysiology of Type I ARF �Hypoxemia is a hallmark sign caused by: Alveolar hypoventilation – ventilation to alveoli is insufficient d/t ↑ metabolic O 2 needs or ↓ ventilation (extrapulmonary disorders) Ventilation / Perfusion (V/Q) mismatching – blood, passing through under ventilated alveoli, leaves without adequate O 2 Intrapulmonary shunting – extreme form of V/Q mismatching; blood reaches the arterial system w/out participating in gas exchange Chapter 13 -4 Copyright © 2004, Elsevier (USA). All rights reserved.

Acute Respiratory Failure � Complications �If the hypoxemia (blood) is not corrected, it will lead to hypoxia within the body cells �Tissue hypoxia develops because of the oxygen demand / supply imbalance �Low tissue oxygen can lead to lactic acidosis and place organs at major risk Chapter 13 -5 Copyright © 2004, Elsevier (USA). All rights reserved.

Acute Respiratory Failure � Nursing Management- maximize oxygenation �Positioning Position patient to best match ventilation/ perfusion Place least affected area of lung in a dependent position (healthy lung down) gravity and perfusion If both lungs are equally affected, position with right (larger lung) down Reposition every 2 hours Chapter 13 -6 Copyright © 2004, Elsevier (USA). All rights reserved.

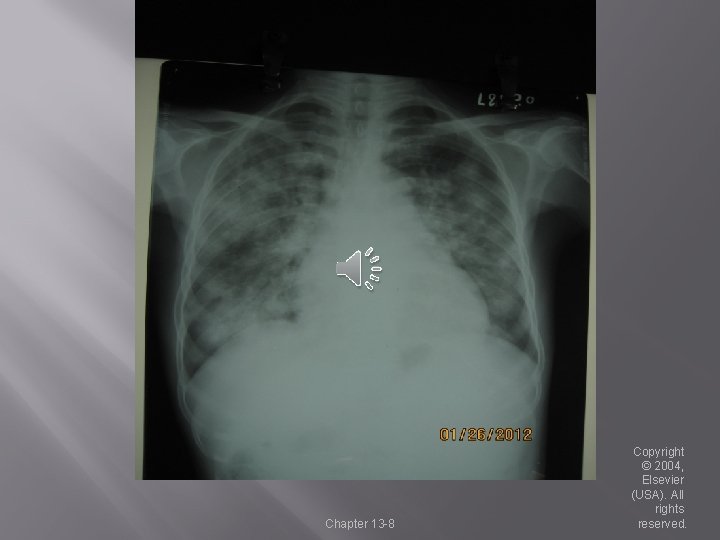
Acute Respiratory Distress Syndrome (ARDS) � Description � Acute in onset (severe form of ALI-Acute Lung Injury) � Alveolar collapse due to damage to surfactant producing Type II cells � Ratio of Pa. O 2 / FIO 2 equal or below <200 mm Hg Example: � Pa. O 2 of 80 mm Hg receiving 70% (0. 7) O 2 � 80 divided by 0. 7 = 114 mm Hg Bilateral infiltrates on chest x-ray-differs for pulmonary edema PAOP less or equal to 18 mm Hg PAOP = pulmonary artery occlusion pressure Chapter 13 -7 Copyright © 2004, Elsevier (USA). All rights reserved.
Chapter 13 -8 Copyright © 2004, Elsevier (USA). All rights reserved.
Chapter 13 -9 Copyright © 2004, Elsevier (USA). All rights reserved.

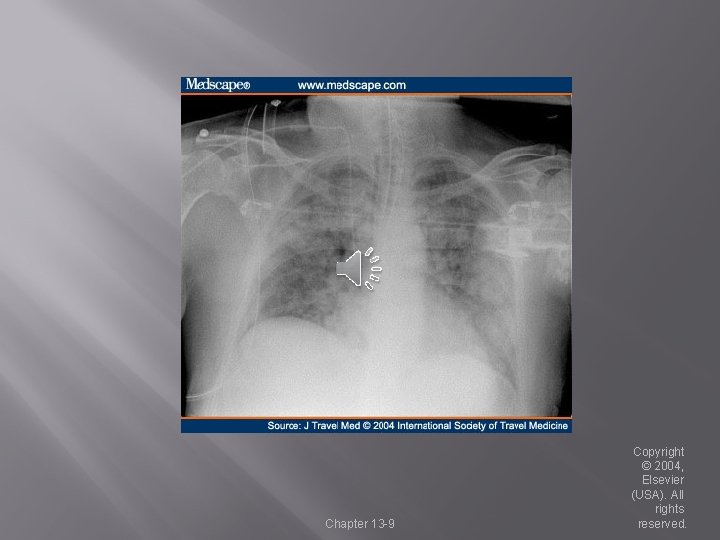
Acute Respiratory Distress Syndrome (ARDS) � Etiology (Box 15 -3) Pathophysiology Fig. 15 -1) p. 275 �Direct Injury Aspiration or inhalation injury Near-drowning Pneumonia �Indirect Injury Sepsis Severe pancreatitis Embolism – air, fat Shock Chapter 13 -10 Copyright © 2004, Elsevier (USA). All rights reserved.

Acute Respiratory Distress Syndrome (ARDS) � Medical Management �Ventilation Assist Control or SIMV (traditional methods) Permissive Hypercapnia �Smaller tidal volumes (5 - 8 ml/kg) Pressure Control Ventilation (PCV) �Maintain plateau pressure < 30 - 40 cm H 2 O Chapter 13 -11 Copyright © 2004, Elsevier (USA). All rights reserved.
Chapter 15 Copyright © 2004, Elsevier (USA). All rights reserved.

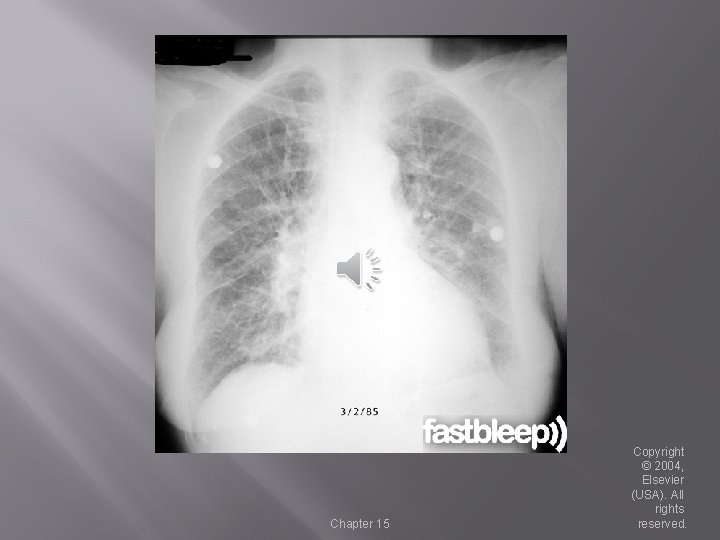
Pneumonia � Description �Acute inflammation of the lung �Caused by an infectious agent �Can lead to alveolar consolidation �May be classified by where or how contracted: Community acquired pneumonia (CAP) Hospital acquired pneumonia (HAP) Ventilator associated pneumonia (VAP) Chapter 15 Copyright © 2004, Elsevier (USA). All rights reserved.

Pulmonary Embolism (PE) � Etiology (Box 15 -3, p. 301) �Hypercoagulability �Venous stasis �Injury to vascular endothelium �Atrial fibrillation Chapter 13 -14 Copyright © 2004, Elsevier (USA). All rights reserved.

Status Asthmaticus � Description � Asthma a chronic obstructive airways disease with: Partially reversible airflow obstruction Airway inflammation Hyper-responsiveness to a variety of stimuli � Status asthmaticus is a SEVERE asthma attack that fails to respond to conventional therapy and can result in acute respiratory failure Chapter 1515 Copyright © 2004, Elsevier (USA). All rights reserved.
- Slides: 15