Invasive Cervical Cancer Prof Dr Tawfik Abdel Salam

Invasive Cervical Cancer Prof. Dr. Tawfik Abdel Salam Prof. of OB/GYN Alexandria University

CANCER CERVIX INVASIV E CERVICAL CARCINOMA

Invasive Cervical Carcinoma Cervical carcinoma with disruption of the basement membrane and invasion of the subepithelial stroma of the cervix According to the depth of invasion and clinical profile two categories of invasive cancer are defined : 1. Microinvasive carcinoma : Pre-clinical invasive cancer 2. Clinical invasive carcinoma : Clinical malignant lesion of the cervix

CANCER CERVIX VE CERVICAL CARCINOMA EPIDEMIOLOGY INV

Epidemiology World-wide, cervical cancer remains the second most common genital cancer surpassed only by breast cancer Globally, the heaviest burden of cervical cancer is reported in Africa , south Asia and south America 80% of globally reported cases are in the third world and developing countries

Epidemiology Significant decline in the incidence of invasive cervical cancer in the past 2 -3 decades has been ascribed to the national screening programs for preinvasive disease (USA , Canada , UK) Most cases of invasive cervical cancer have been reported in women who have never been previously screened nor HPV -vaccinated

Epidemiology The peak incidence of invasive cervical cancer is reported in women in their 40 s The median age at diagnosis is 47 yrs This reflects the insidious nature of HPV infection which is contracted in early 20 s with subsequent carcinogenesis in women whose infection does not clear over 10– 15 yrs

CANCER CERVIX MICROINV ASIVE CARCINOMA

Micro-invasive Carcinoma Definition: Invasive cancer with a maximum depth of invasion less than 5 mm beneath the basement membrane Nomenclature: Preclinical invasive carcinoma Stage Ia cancer cervix (FIGO) Micro-carcinoma of the cervix Early stromal invasion Superficial squamous carcinoma of the cervix

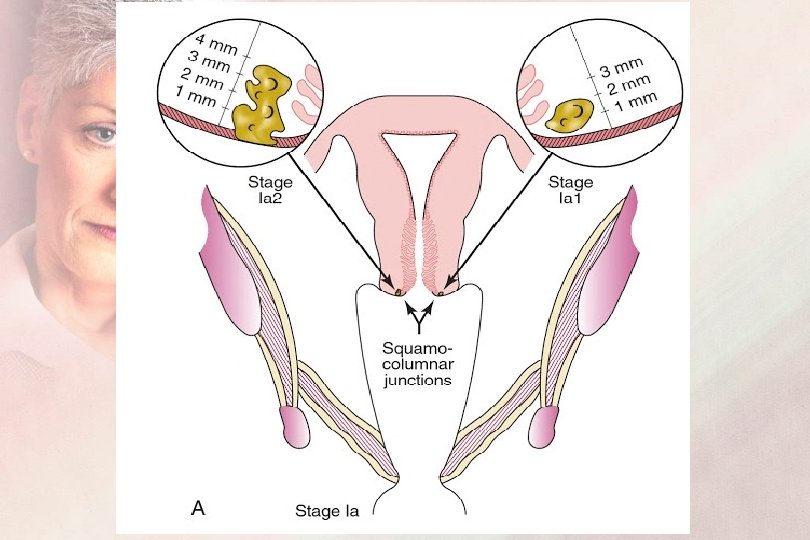
Micro-invasive Carcinoma Staging : FIGO Stage IA IA 1: Depth of invasion is less than 3 mm IA 2: Depth of invasion is ≥ 3 mm and less than 5 mm the more than 7 mm lateral extent has been omitted from definition of stage IB (FIGO staging 2019)

Micro-invasive Carcinoma Diagnosis : (the same work-up for CIN) : Preclinical: no symptoms – no clinical lesion Suspicious microinvasion : • Pap smear : - Severe dyskaryosis - Pleomorphism • Colposcopy : - Abnormal B. V. - Colour tone change - Loss of surface epithelium • Directed biopsy : Definitive diagnosis : Cervical Conization : precise depth of micro-invasion

Micro-invasive Carcinoma Treatment : Stage IA 1: 1. Therapeutic conization : (Fertility sparing) • Cold-knife cone • Laser excisional cone • LEEP cone - young patients desirous for future fertility - annual follow up is mandatory 2. Total Hysterectomy : (Standard treatment) - patients >40 yrs/completed family size - non-compliant patients for follow up

Micro-invasive Carcinoma Treatment : Stage IA 2 : 5% pelvic nodal metastases Modified Radical Hysterectomy : (Standard) • • Extrafascial Total Hysterectomy Resection of medial parts of parametrium Pelvic lymphadenectomy or SLN mapping Removal of upper 1/3 of the vagina Radical Trachelectomy : (fertility sparing) In young patients seeking future fertility Brachytherapy : Intracavitary and vaginal vault radium In high operative risk patients

CANCER CERVIX CLINICAL INVASIVE CERVICAL CARCINOMA

Clinical Invasive Carcinoma Invasive cervical carcinoma with malignant lesion of the cervix which can be demonstrated and diagnosed clinically It includes all FIGO stages more than stage IA FIGO Stages IB IVB

CANCER CERVIX VASIVE CERVICAL CARCINOMA PATHOLOGY
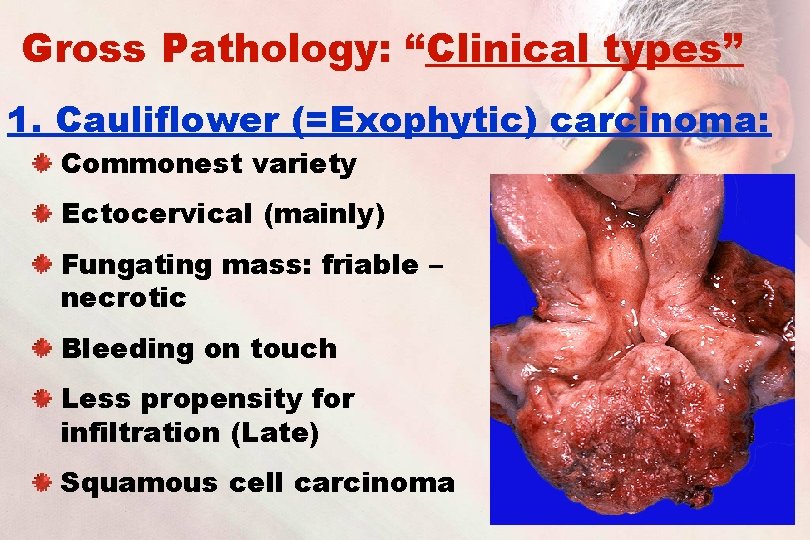
Gross Pathology: “Clinical types” 1. Cauliflower (=Exophytic) carcinoma: Commonest variety Ectocervical (mainly) Fungating mass: friable – necrotic Bleeding on touch Less propensity for infiltration (Late) Squamous cell carcinoma
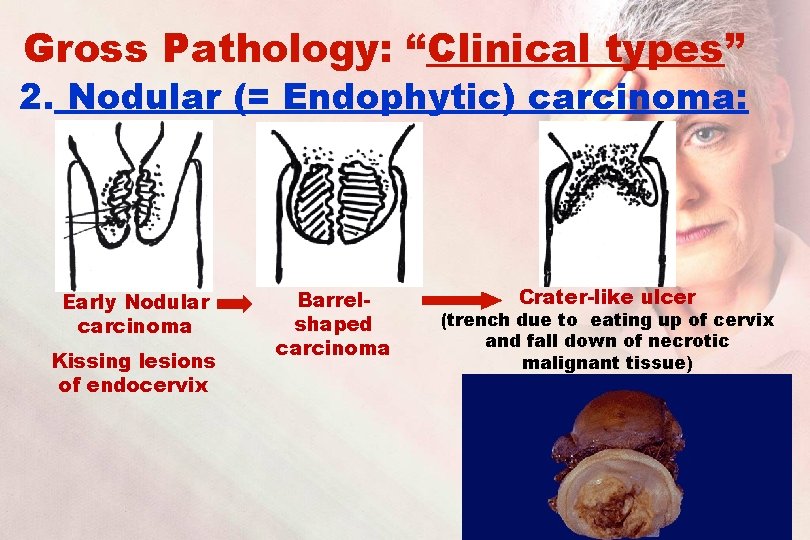
Gross Pathology: “Clinical types” 2. Nodular (= Endophytic) carcinoma: Early Nodular carcinoma Kissing lesions of endocervix Barrelshaped carcinoma Crater-like ulcer (trench due to eating up of cervix and fall down of necrotic malignant tissue)

Gross Pathology: “Clinical types” 2. Nodular (=Endophytic) carcinoma: Endocervical mainly Propensity for early infiltration of the stroma and L-V space (LVS) invasion Adenocarcinoma /squamous cell carcinoma Occult carcinoma : Hidden early endophytic carcinoma not apparent clinically - It can be diagnosed by ECC or Cone biopsy
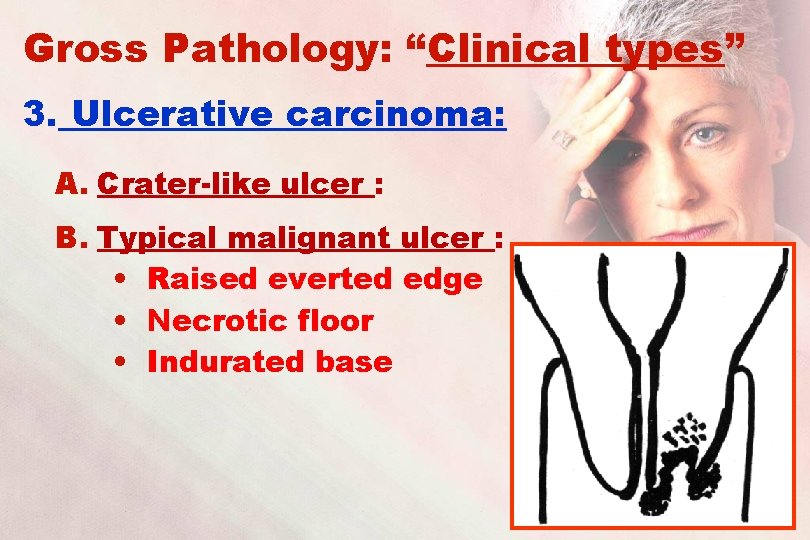
Gross Pathology: “Clinical types” 3. Ulcerative carcinoma: A. Crater-like ulcer : B. Typical malignant ulcer : • Raised everted edge • Necrotic floor • Indurated base

Gross Pathology: “Clinical types” 4. Malignant Polyp: Ecto or Endo-cervical Friable Necrotic – Ulcerated Bleeding on touch 5. Malignant plaque: Raised plaque Very rare – in older patients Good prognosis Behaves as Scirrhus cancer
Histopathology 1. Squamous cell carcinoma : Commonest (75 – 80%) According to grade of differentiation : A. Large cell keratinizing : • Well-differentiated • Keratin pearl formation in cell nests B. Large cell non-keratinizing : • Moderately differentiated • No keratin pearls C. Small cell non-keratinizing : • Poorly differentiated • Scanty cytoplasm + small nuclei

Histologic Grading Histologic grading of cervical squamous carcinoma is of value in : • Prognosis • Planning for therapy (radiosensitivity) Wentz-Reagan classification : most universally accepted system A. Keratinizing : B. Non-Keratinizing : - Large cell - Small cell

Histopathology 2. Adenocarcinoma: Pure : endocervical cell type Mixed : with squamous cell carcinoma 3. Adeno-squamous carcinoma: Less favourable prognosis than pure types 4. Clear cell carcinoma: Special type of adenocarcinoma with clear cytoplasm and excentric nucleus – It has a poor prognosis – common in DES-women

Routes of Spread 1. Direct invasion : the earliest and most important mode of spread- occurs in all directions and in all stages into : vagina, parametrium, ureters, bladder, rectum and pelvic wall 2. Lymphatic metastasis: most important for distant spread of malignancy 3. Haematogenous metastasis: extremely rare in late advanced cases 4. Transperitoneal implantation: during surgical extirpation of the tumour by radical hysterectomy
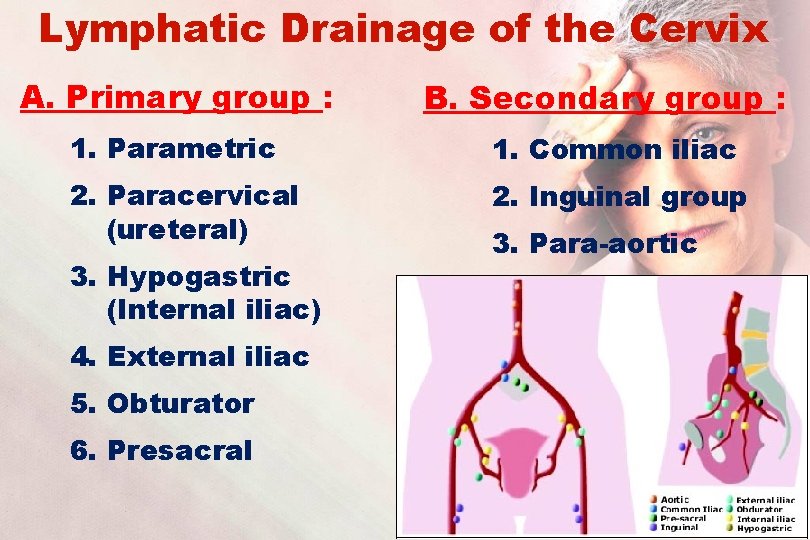
Lymphatic Drainage of the Cervix A. Primary group : B. Secondary group : 1. Parametric 1. Common iliac 2. Paracervical (ureteral) 2. Inguinal group 3. Hypogastric (Internal iliac) 4. External iliac 5. Obturator 6. Presacral 3. Para-aortic

Causes of Death in Cancer Cervix I- Renal failure : Bilateral ureteral infiltrationobstruction II- Massive Hemorrhage : Invasion-erosion of pelvic vessels III- Malignant Cachexia : Multiple organ failures due to metastases to vital organs IV- Iatrogenic Causes : Major complications of radical surgery and radio-chemotherapy

CANCER CERVIX VASIVE CERVICAL CARCINOMA CLINICAL PROFILE

Clinical Profile Classical clinical presentation of cervical carcinoma is specific and pathognomonic Symptoms: 1. Vaginal discharge: (Leucorrhoea) § Earliest symptom § Discharge is usually profuse, offensive, serosanguinous, mucopurulent or purulent 2. Contact Bleeding: (post-coital bleeding) § Commonest presenting symptom § § Common cause of death Less commonly : metrorrhagia - intermenstrual

Clinical Profile Symptoms: 3. Pain: • Late in advanced stages • mainly due to Infiltration of : ureter, bladder, rectum, pelvic wall or pelvic nerves • Pelvic side wall involvement (stage IIIB) presents with : a triad of flank pain, sciatic pain and leg swelling 4. Cachexia: • Advanced stages • Anorexia, pain, infection, anemia • Metastatic carcinoma ends fatally by multiple organ failures

Clinical Profile Clinical Signs: Diagnostic clinical criteria of malignant cervical lesion 1. Contact Bleeding : (Bleeding on touch) Commonest in cauliflower carcinoma 2. Friability : Krobac's test : probing breaking down 3. Necrosis : ± ulceration : Lesion usually has necrotic, ulcerated aspect 4. Indurated base : Induration may be due to malignant infiltration

Diagnosis § History : relevant risk factors § Symptomatology : specific § Pathognomonic signs : criteria of malignant cervical lesion § Cervical Biopsy : 1. Punch biopsy 2. 3. 4. 5. 4 -Quadrant biopsy (multiple punch) wedge biopsy Endocervical curettage Cone biopsy

CANCER CERVIX VASIVE CERVICAL CARCINOMA STAGING

Clinical Staging I – Clinical appraisal : Ø Ø § § § Examination under anesthesia Office Examination Speculum Examination Bimanual Examination Recto-vaginal Examination

Clinical Staging II – Conventional Radiology : § IVP § Barium Enema § Plain Chest Radiograph III – Endoscopy : § Cystoscopy § Proctosigmoidoscopy

Clinical Staging Revised FIGO Staging for Cervical Carcinoma 2019



FIGO Staging 2019 Sage I : Carcinoma is strictly confined to the Cervix IA : Micro-invasive Carcinoma IA 1 : Depth of invasion is less than 3 mm IA 2 : Depth of invasion is ≥ 3 mm and less than 5 mm

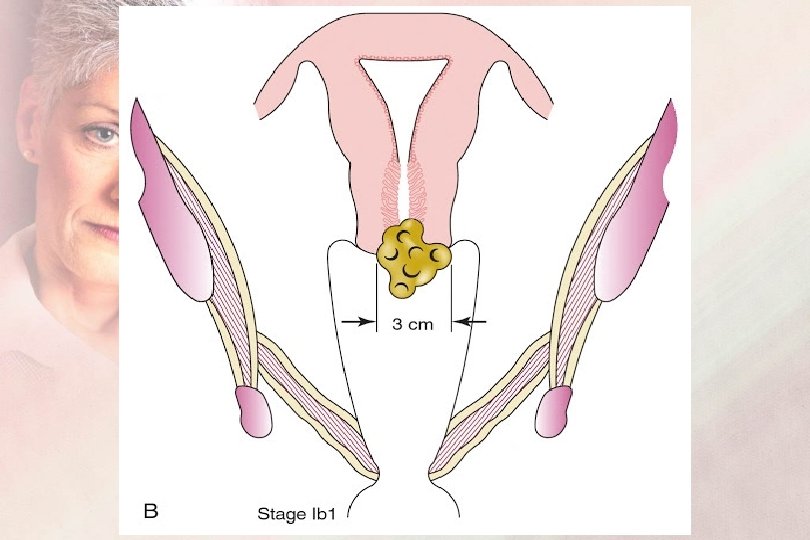
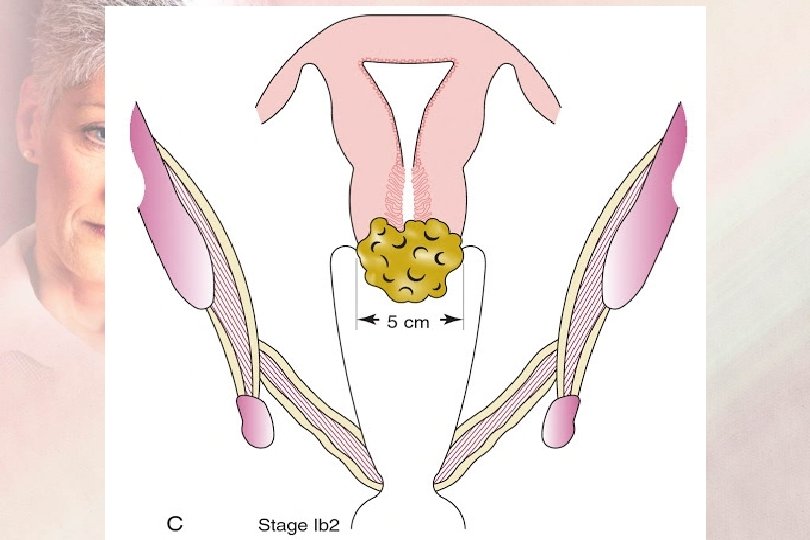
FIGO Staging 2019 Sage I : IB : Invasive lesion ≥ 5 mm depth or clinically visible lesion IB 1 : Carcinoma is less than 2 cm IB 2 : Carcinoma is ≥ 2 cm and less than 4 cm IB 3 : Carcinoma is ≥ 4 cm

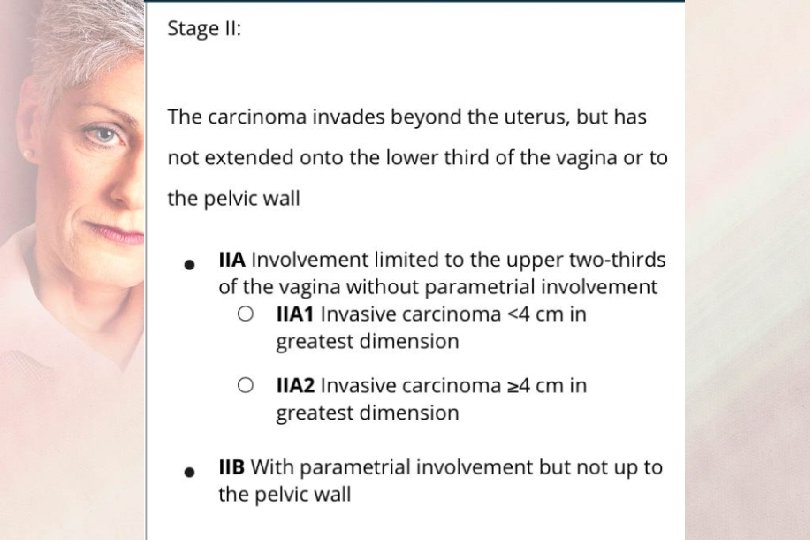
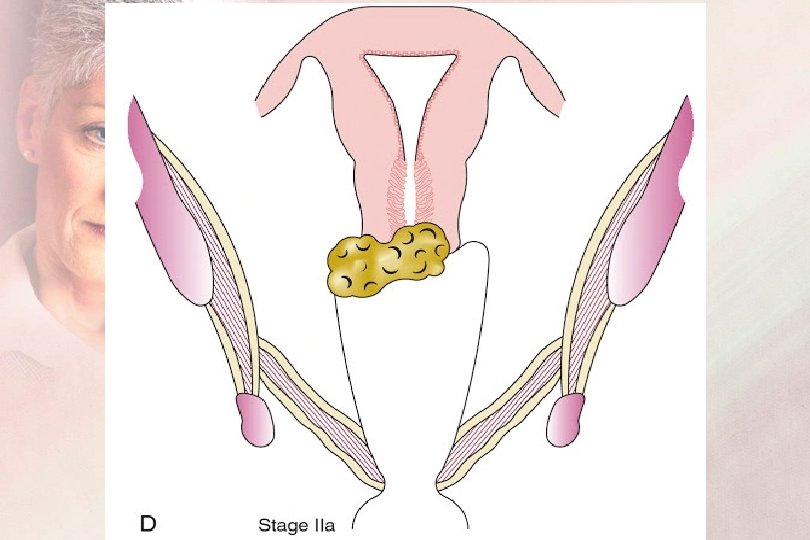
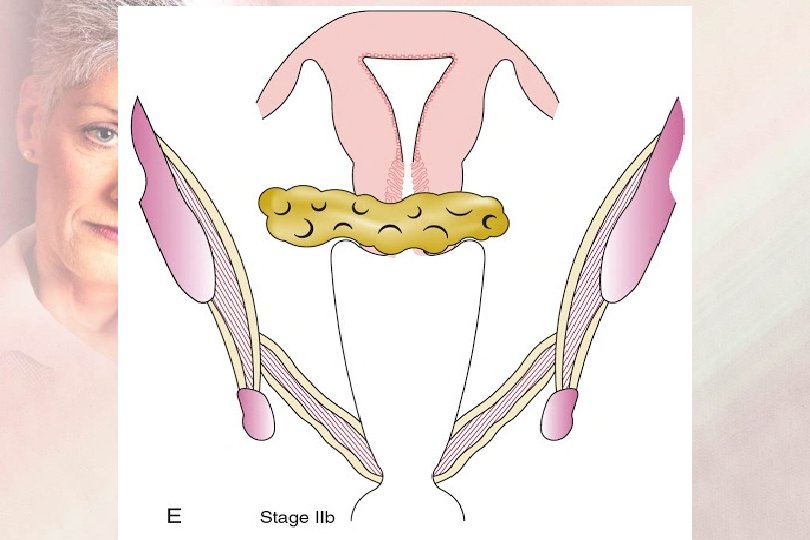
FIGO Staging 2019 Sage II : Carcinoma extends beyond the Cervix IIA : Extension to the upper 2/3 of the vagina IIA 1 : Carcinoma less than 4 cm IIA 2 : Carcinoma ≥ 4 cm IIB : Parametrial involvement

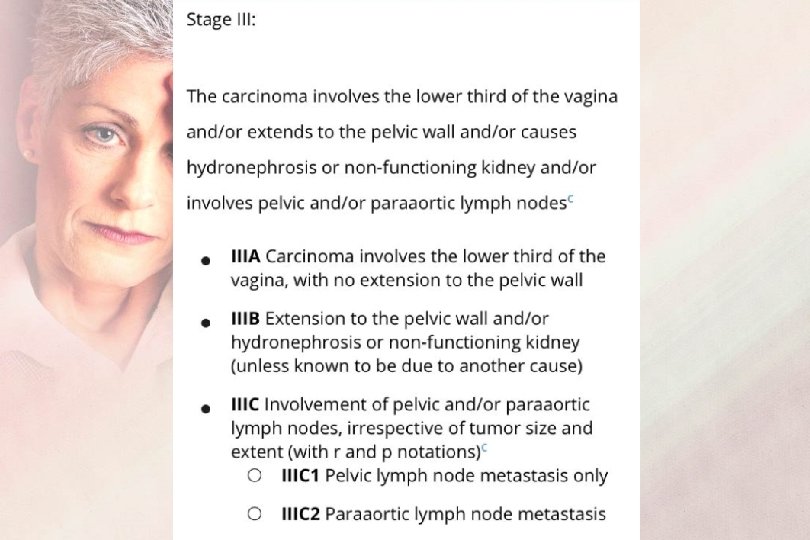
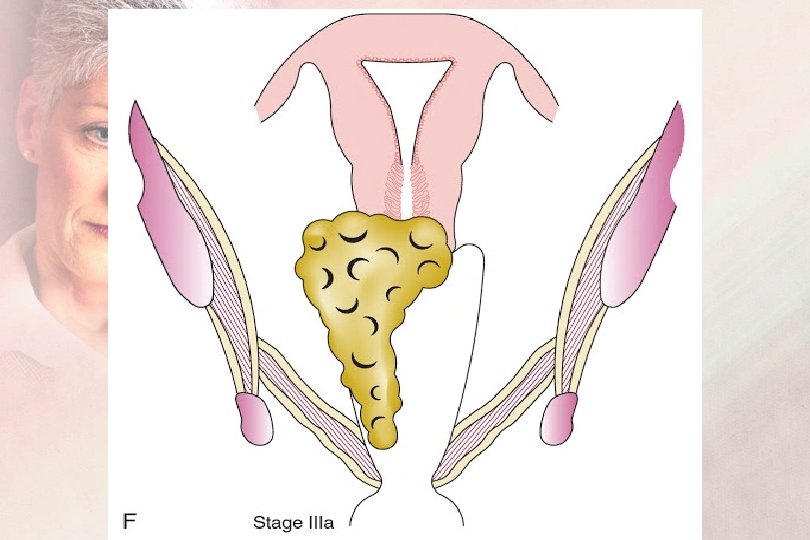
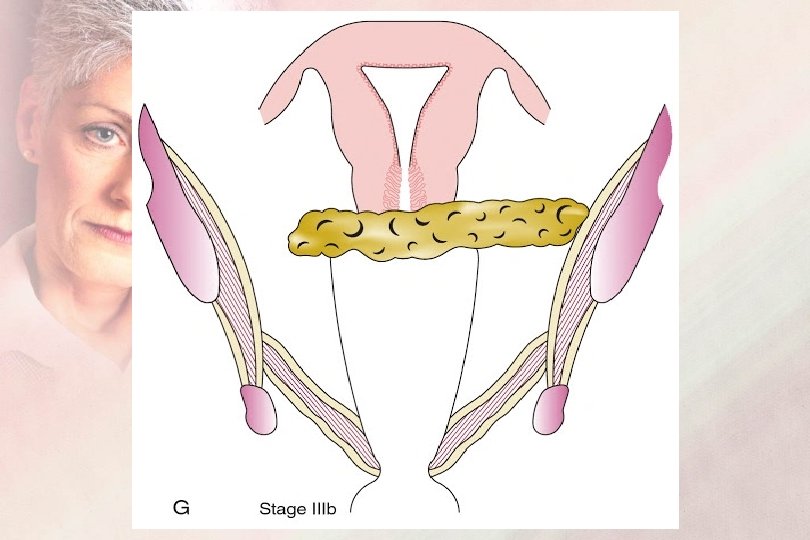
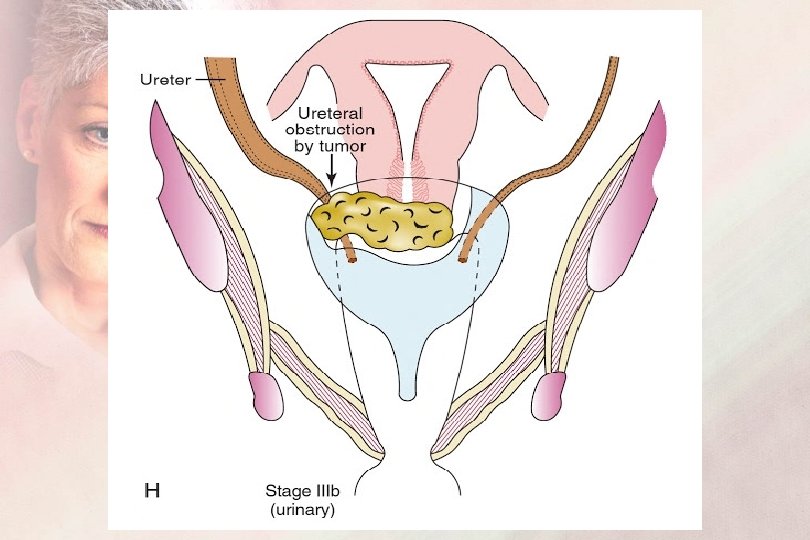
FIGO Staging 2019 Sage III : IIIA : Extension to the lower 1/3 of the vagina IIIB : Extension to the pelvic wall and/or hydronephrosis or non-functioning kidney IIIC : Nodal involvement IIIC 1: pelvic LN metastasis IIIC 2: paraaortic LN metastasis

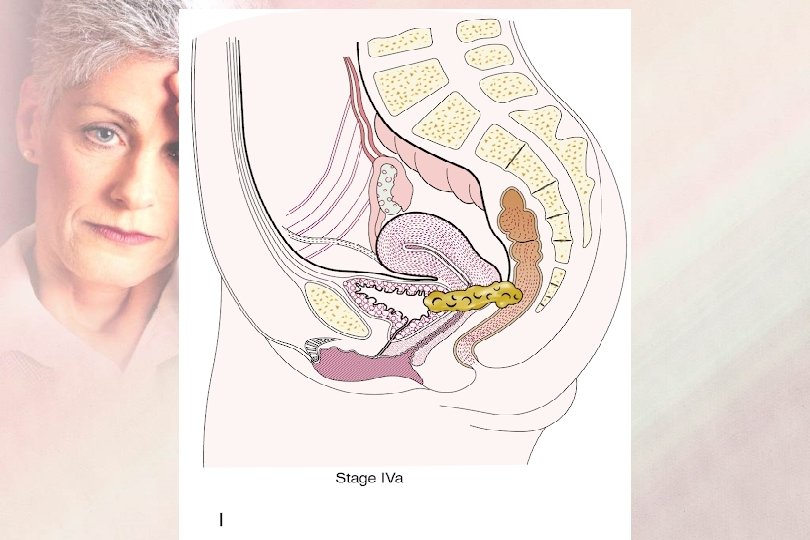
FIGO Staging 2019 Sage IV : Carcinoma extends beyond the true pelvis or invades the bladder and/or the rectal mucosa IVA : Invasion of the bladder and/ or the rectal mucosa IVB : Distant metastasis
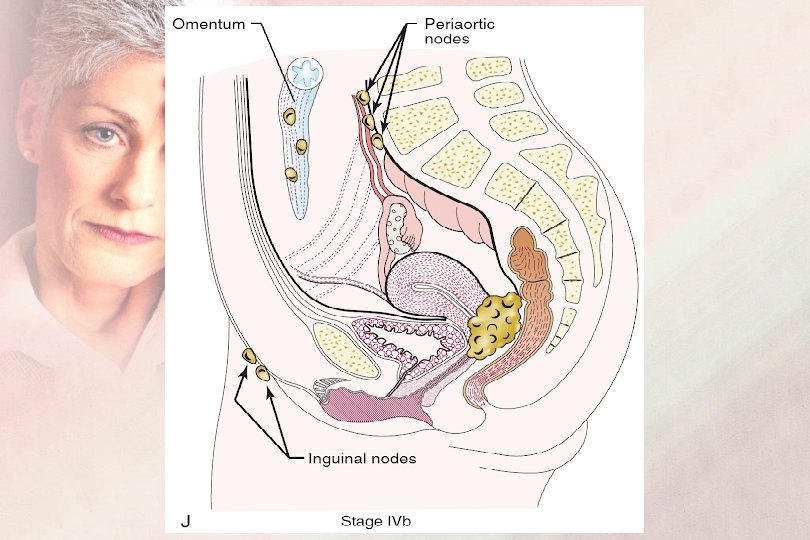

Pretreatment Evaluation of Cancer Cervix patient Objectives: Extent of disease (staging) Prognostic criteria Selection of treatment plan

Pretreatment Evaluation of Cancer Cervix Patient I. Hematological – Blood Chemistry: CBC Renal function : Urea – Creatinine Liver function : SGOT–SGPT–A/G ratio Blood sugar profile Lipid profile Coagulation studies Serum electrolytes Urine : analysis–microscopy–culture Tumour markers : ? CEA–CA 125–SCC

Pretreatment Evaluation of Cancer Cervix Patient II. Radiographic imaging : Conventional Radiology : § § § Chest X-rays Intravenous Urography (IVU) Barium Enema Ultrasonography (U/S) : § § Abdominal Pelvic

Pretreatment Evaluation of Cancer Cervix Patient II. Radiographic imaging: Computer Tomography (CT) : • Chest – Abdomen – Pelvis • Extent of pelvic disease • Nodal involvement • Distant metastases Magnetic Resonance Imaging (MRI) : • Superior to CT to delineate extent of pelvic disease and nodal involvement

Pretreatment Evaluation of Cancer Cervix Patient II. Radiographic imaging: Lymphangiography: (Optional) now replaced by MRI, CT and PET Isotope scans: (Optional) Positron Emission Tomography : (PET) scan and integrated PET-CT

Pretreatment Evaluation of Cancer Cervix Patient III. Endoscopic procedures : Cystoscopy : to exclude bladder mucosal invasion Procto-sigmoidoscopy : to exclude rectal or recto-sigmoid invasion

CANCER CERVIX VASIVE CERVICAL CARCINOMA TREATMENT

Treatment of Invasive Cancer Cervix Strategy Primary SURGERY Primary RADIOTHERAPY Combined Plan based on Stage Pre-treatment evaluation Histopathology Histologic grade
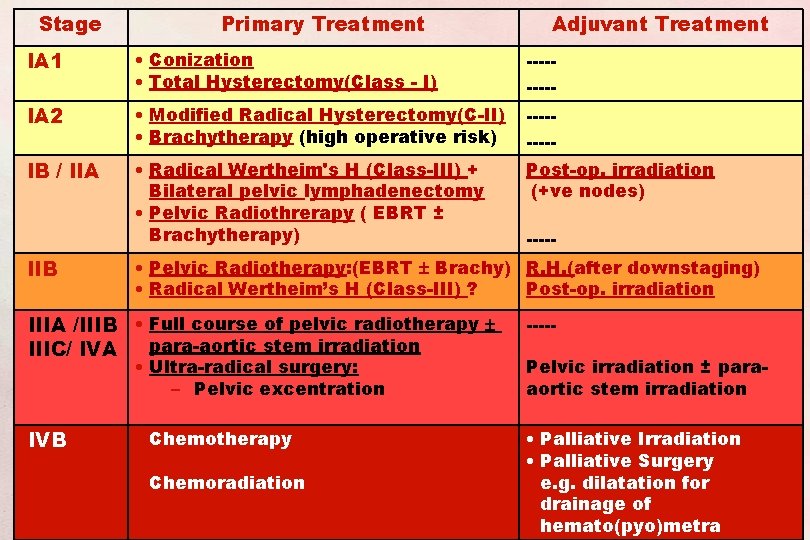
Stage Primary Treatment Adjuvant Treatment IA 1 • Conization • Total Hysterectomy(Class - I) ----- IA 2 • Modified Radical Hysterectomy(C-II) • Brachytherapy (high operative risk) ----- IB / IIA • Radical Wertheim's H (Class-III) + Bilateral pelvic lymphadenectomy • Pelvic Radiothrerapy ( EBRT ± Brachytherapy) Post-op. irradiation (+ve nodes) IIB • Pelvic Radiotherapy: (EBRT Brachy) R. H. (after downstaging) • Radical Wertheim’s H (Class-III) ? Post-op. irradiation IIIA /IIIB • Full course of pelvic radiotherapy para-aortic stem irradiation IIIC/ IVA IVB ----- • Ultra-radical surgery: – Pelvic excentration Pelvic irradiation ± paraaortic stem irradiation • Chemotherapy • Palliative Irradiation • Palliative Surgery e. g. dilatation for drainage of hemato(pyo)metra • Chemoradiation

CANCER CERVIX VASIVE CERVICAL CARCINOMA RADICAL HYSTERECTOMY
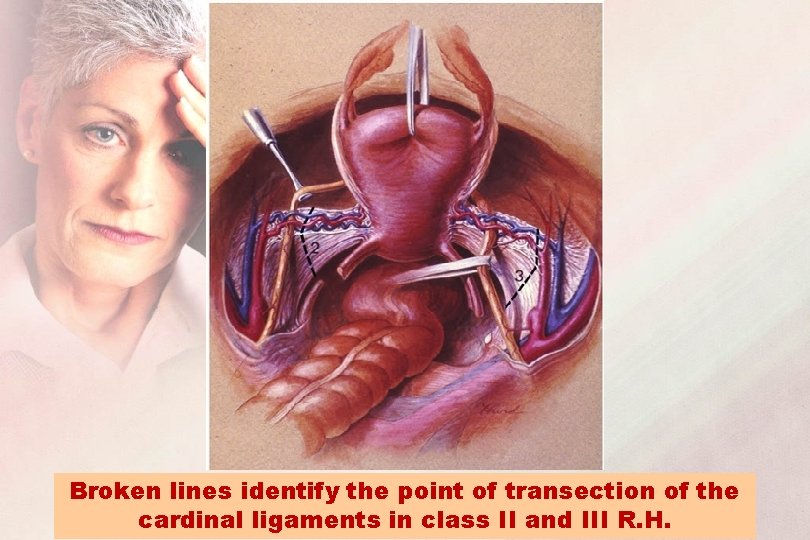
Broken lines identify the point of transection of the cardinal ligaments in class II and III R. H.
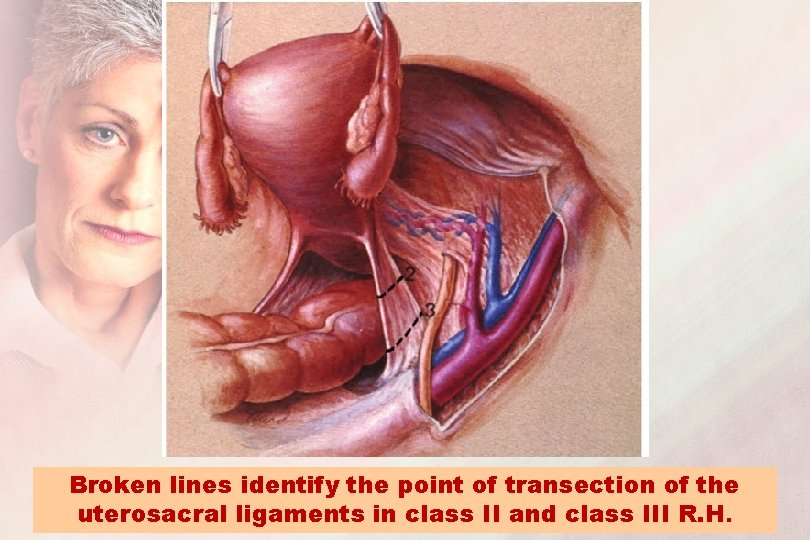
Broken lines identify the point of transection of the uterosacral ligaments in class II and class III R. H.
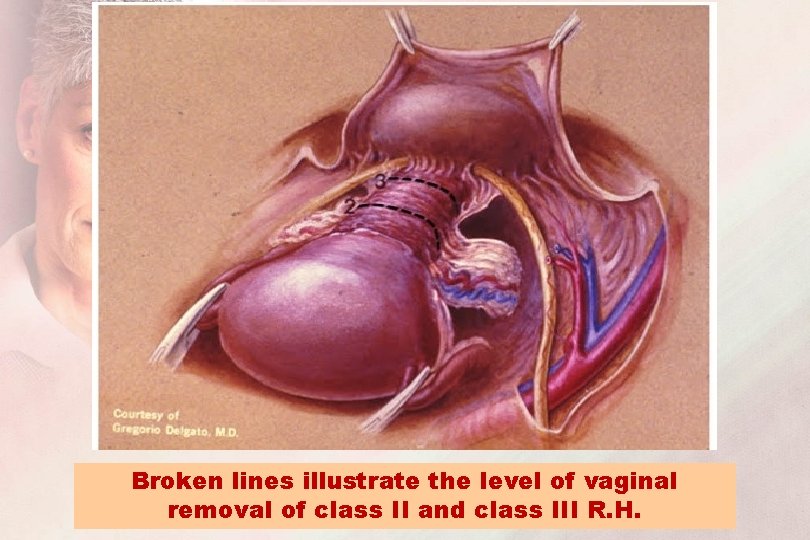
Broken lines illustrate the level of vaginal removal of class II and class III R. H.
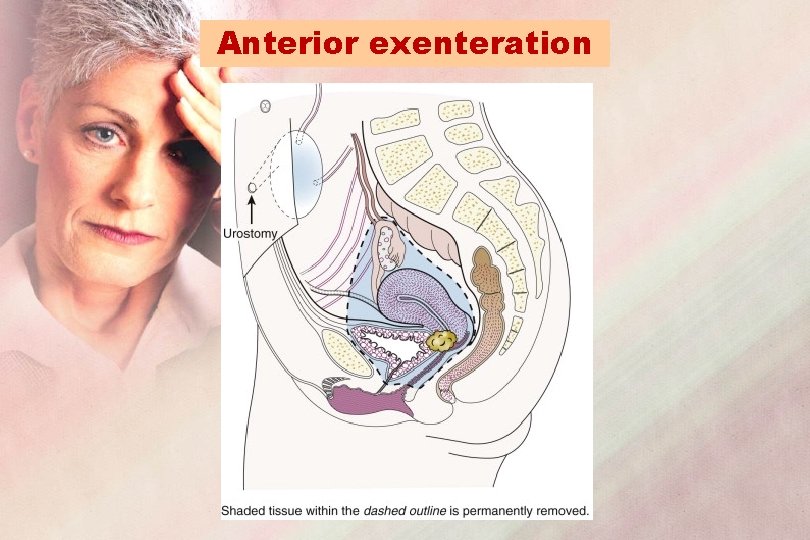
Anterior exenteration
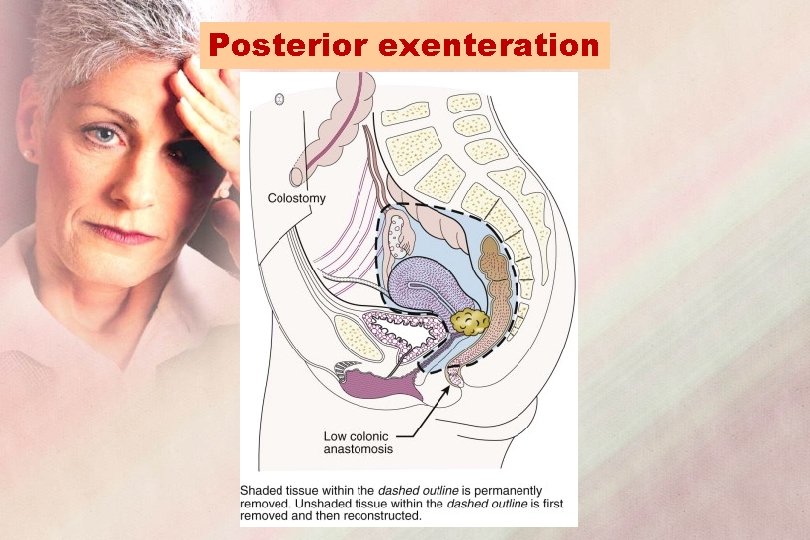
Posterior exenteration
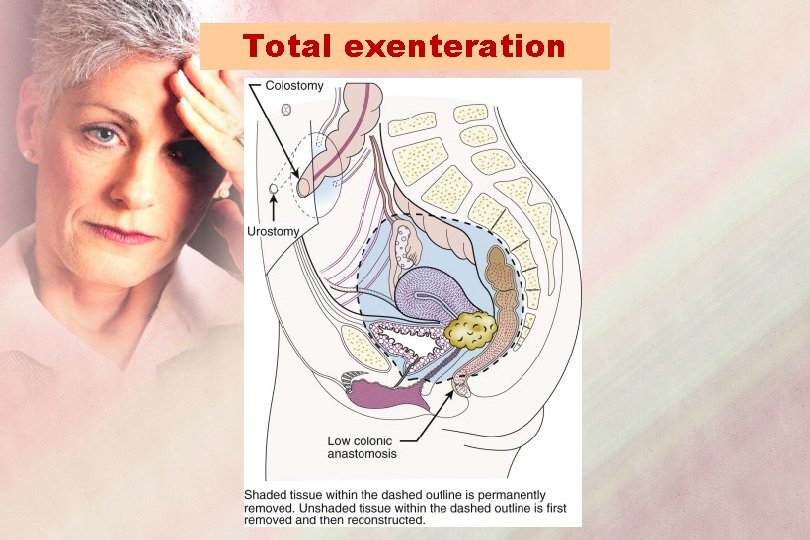
Total exenteration

Complications of R. H. § § § § Vesico-vaginal fistula Uretero-vaginal fistula Bladder atony Bowel obstruction Lymphocyst DVT / Pelvic VT Pulmonary Embolism 1% 2% 4% 1% 3% 2% 1%

CANCER CERVIX VASIVE CERVICAL CARCINOMA RADIOTHERAPY
Techniques of Radiotherapy I. Teletherapy: (External Irradiation) Radiation source is away from the patient i. e. external beam radiotherapy ( EBRT ) Dose : 6000 -8000 rads given fractionally 200 rads/day x 5 days/week for 6 weeks II. Brachytherapy: Radiation device is placed either within or close to the target e. g. intra-cavitary or vaginal vault radium implants
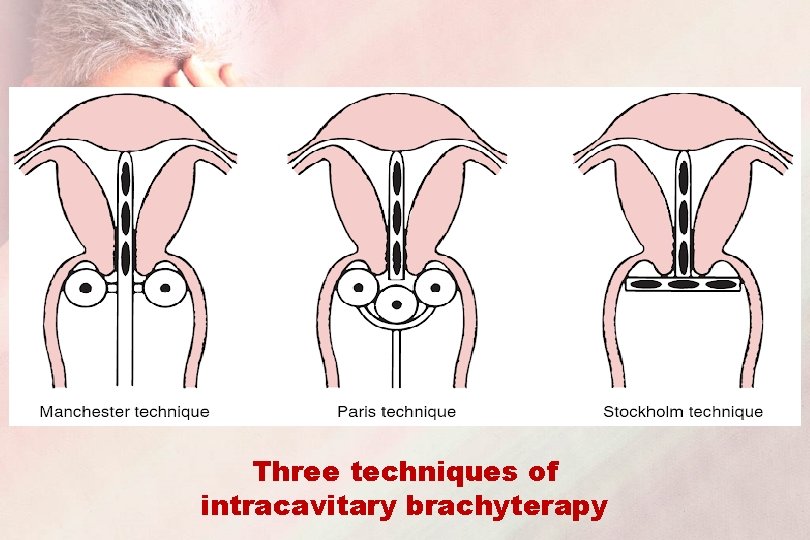
Three techniques of intracavitary brachyterapy

Overall Survival in treated Cancer Cervix IA IB II IVA / B 98% 89% 70% 40% 10 -20%

- Slides: 77