Introduction to your HRA Members since 2012 Members

Introduction to your HRA Members since 2012 Members since 2018 Members since 2006 Copyright © 2018 Health. Equity, Inc. All rights reserved.

Why HRAs? Save and win • Coverage for out-of-pocket costs • You don’t pay taxes on HRA funds • Contributions are free money, provided by your employer. There are no payroll deductions 2

Get started today! 1. Sign up • Enroll in the medical plan associated with your HRA • You will automatically be enrolled with an HRA 2. Use your funds • Your HRA will be deposited for your use during the plan year • Claims will be paid from your employer-funded account • Remember to save ALL receipts 3
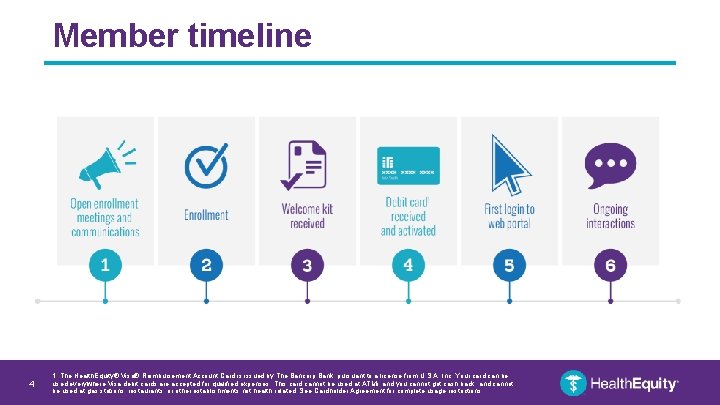
Member timeline 4 1. The Health. Equity® Visa® Reimbursement Account Card is issued by The Bancorp Bank, pursuant to a license from U. S. A. Inc. Your card can be used everywhere Visa debit cards are accepted for qualified expenses. This card cannot be used at ATMs and you cannot get cash back, and cannot be used at gas stations, restaurants, or other establishments not health related. See Cardholder Agreement for complete usage restrictions.
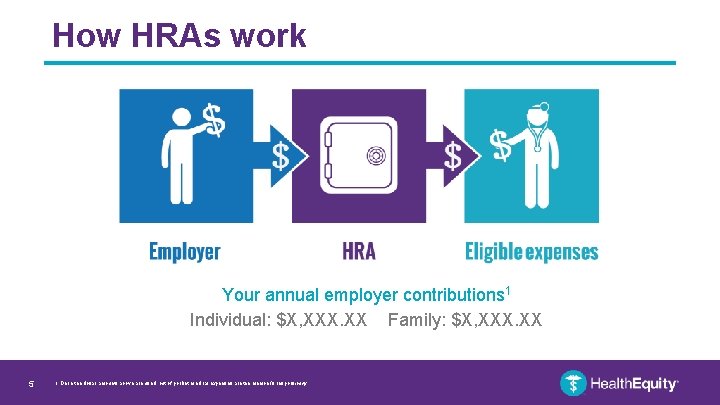
How HRAs work Your annual employer contributions 1 Individual: $X, XXX. XX Family: $X, XXX. XX 5 1. Once the dollar amounts above are used, out of pocket medical expenses are the member’s responsibility

Your HRA plan details • HRA plan type: {9 versions} • Coverage type: {Individual, family, etc. . } • HRA deductible: {Member pays first plans only} • Dates to incur expenses: • Dates to submit expenses: • Rollover: Y/N – $ amount or % • Claims/payments/substantiation: 6

Eligible expenses • Eligible services for family members covered under the medical plan • Medical co-pays, deductible, and coinsurance expenses • Prescriptions • Dental • Vision 7 In addition to restrictions imposed by law, your employer may limit what expenses are eligible for reimbursements. It is the member's responsibility to ensure eligibility requirements as well as if they are eligible for the plan and expenses submitted.
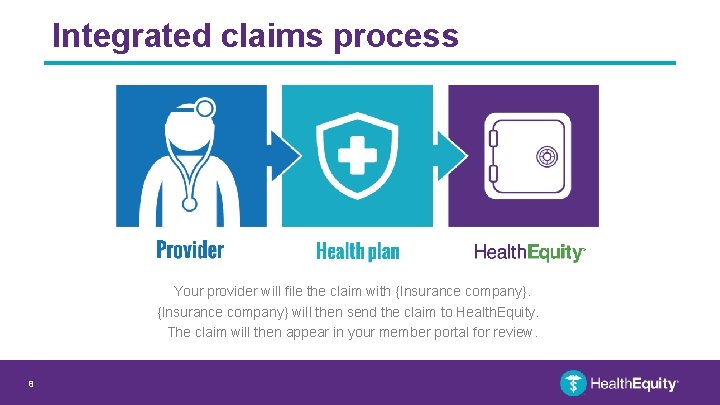
Integrated claims process Your provider will file the claim with {Insurance company} will then send the claim to Health. Equity. The claim will then appear in your member portal for review. 8

How HRAs work: Auto pay provider • Claims with eligible expenses out of the HRA are automatically paid from the account when Health. Equity receives them • A virtual payment is sent directly to the provider – Payments should process within 7 -10 business days • Payments can be tracked through the claims in your Health. Equity Member Portal • If your plan covers copays or prescription costs, those expenses will be reimbursed to you automatically – Free EFT reimbursements are recommended: 2 -3 business days – $2 paper fee per check reimbursement: 7 -10 business days 9
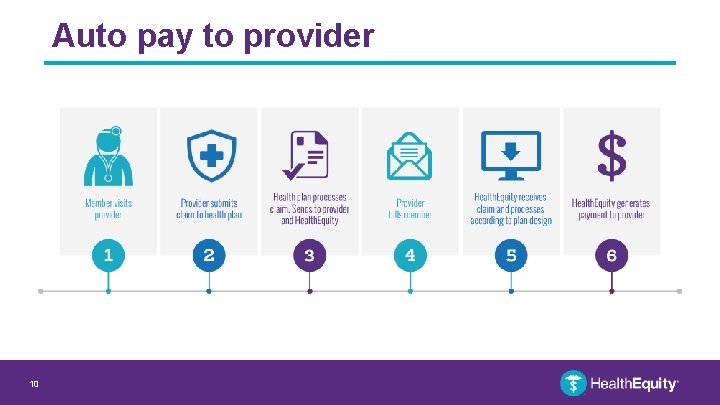
Auto pay to provider 10

How HRAs work: Auto pay member • Claims with eligible expenses out of the HRA are automatically paid to the member when Health. Equity receives the claim – Free EFT reimbursements are recommended: 2 -3 business days – $2 paper fee per check reimbursement: 7 -10 business days • Payments can be tracked through the claims in your Health. Equity Member Portal • The member is responsible to pay the provider for the expense out of pocket 11

Auto pay to member 12

How HRAs work: self-directed • Claim with eligible HRA expenses posts to the Health. Equity Member Portal • Member receives a bill from the provider • Member decides how they would like to pay the bill out of their HRA – Pay out of pocket and reimburse themselves • Free EFT reimbursements are recommended: 2 -3 business days • $2 paper fee per check reimbursement: 7 -10 business days – Pay provider from the claim online • Health. Equity will send a virtual payment directly to the provider • Payment should process within 7 -10 business days • Payments can be tracked through claims in your Health. Equity Member Portal 13

Use it or lose it • HRA funds do not always roll over from year to year • If not, you must use all HRA dollars within the plan year or forfeit them • Check with plan administrator for specific dates for reimbursements/documentation 14

Making payments online • Login to your account at My. Health. Equity. com • Go to Claims & Payments • Click on View All Claims • Locate your claim • Click ‘Pay Provider’ or ‘Reimburse Me’ 15

Using your debit card • When to use the card – At the pharmacy for a prescription – At the Doctor’s office for a copay • When to pay online/mobile app – When you get a bill from your doctor (amounts applied to your deductible and coinsurance) • Remember to save ALL receipts – Take a photo using the mobile app! – Upload to the documentation library in the member portal 16 The Health. Equity® Visa® Reimbursement Account Card is issued by The Bancorp Bank, pursuant to a license from U. S. A. Inc. Your card can be used everywhere Visa debit cards are accepted for qualified expenses. This card cannot be used at ATMs and you cannot get cash back, and cannot be used at gas stations, restaurants, or other establishments not health related. See Cardholder Agreement for complete usage restrictions.

Debit card: at the pharmacy 17

Documenting your purchases What is Substantiation? • The IRS requires that HRA funds be used for qualified expenses only • Substantiation is documentation that an expense is qualified When is this needed? • When you run your card and the transaction cannot be auto-substantiated or auto-matched to a claim How do I substantiate? • Manually match to a claim on the portal • Send in an EOB or itemized receipt 18 In addition to restrictions imposed by law, your employer may limit what expenses are eligible for reimbursements. It is the member's responsibility to ensure eligibility requirements as well as if they are eligible for the plan and expenses submitted.

Notification requests We will notify a member to provide substantiation by mail or email 19

Documentation that includes the following should be provided to substantiate: • Name of provider • Date(s) of service • Cost of service • Name of patient • Description of services What documentation is not sufficient? • Credit card receipts • Cancelled checks 20

Auto-substantiation In some instances card transactions can be auto-substantiated: • Transactions for copayments • At a pharmacy that is IIAS certified (Visit www. sig-is. org for a detailed list) 21

Claim matching Claims can be automatically matched to card transactions based on: • Amount • Medical code When will my claim not automatically match to my card transaction? • If you pay for more than one date of service at a time • If you pay a discounted or partial amount at the time of service or the card transaction name doesn’t match the name of the provider in the claim • If Health. Equity does not receive the claim from the health plan (Mental health, dental, or vision) 22

How to: card to claim matching 1. Click “Submit Documentation” 2. Select “Match to claim” 3. Choose a claim to match to the card swipe 4. Card transaction is updated to “Member Match” 5. Payable amount on claim reduced 23

Other options for providing substantiation documents: • Upload documentation directly to the debit card transaction from the member portal • Send documentation by mail, fax or email. Contact information is included in the substantiation letter • Health. Equity mobile app 1 24 1. Accounts must be activated via the Health. Equity website in order to use the mobile app.

Submitting a HIPAA form for dependents 25
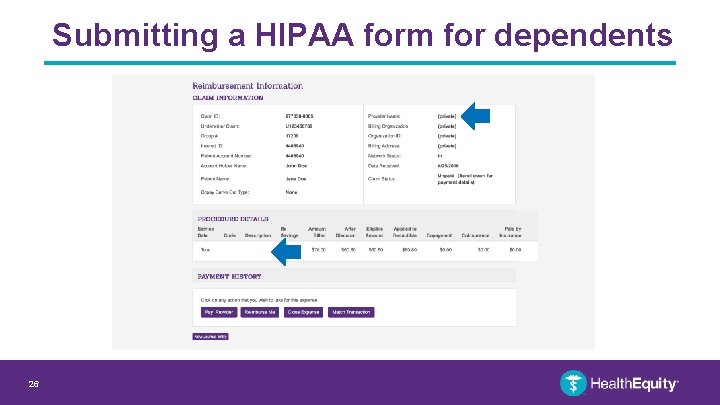
Submitting a HIPAA form for dependents 26
Mobile app Convenient, powerful tools: • On-the-go access for all account types • Take a photo of documentation with phone and link to claims and payments • Manage debit card transactions • View claims status • Manage claims Available for i. OS and Android 27 Accounts must be activated via the Health. Equity website in order to use the mobile app.

• Available around-the-clock, every day • Helpful support for members • Based in Salt Lake City 866. 346. 5800 Melissa Health. Equity team member

- Slides: 29