INTRODUCTION TO SCLERAL CONTACT LENSES Dr Desinee Drakulich






























- Slides: 48

INTRODUCTION TO SCLERAL CONTACT LENSES Dr. Desinee Drakulich O. D.

Disclaimer � I do not have any affiliations nor am I paid by any of the companies that are used in this presentation.

Outline for today’s class � � � Historical overview of scleral lens Detailed review of structure and design Detailed process of fitting � Introduction of sagittal depth � Peripheral curves � Edge lift � Diameter � Slit Lamp images � OCT images � Why and when we use scleral lenses � Advantages and Disadvantages � Comparing other RGPs

First Glass Scleral Contact Lens

Size Comparision

Size Comparision

Brief History of Scleral Lenses � � The scleral contact lens was the first contact described in medical literature. In 1888, Adolf Fick developed the first blown glass scleral contact. Also in 1888, Eugene Kalt started using blown glass scleral contacts for the treatment of keratoconus. In 1889, August Mueller made himself a ground glass scleral lens for his high myopia and used it for his doctorial dissertation.

Brief History of Scleral Lenses � � � Scleral CLs never really progressed much after that due to the poor oxygen permeability of glass. Re-introduced in 1900’s with the advent of PPMA material. More oxygen permeable than glass but still not great. Fenestration was added to try to increase oxygen permeability. Developers started making lenses small to allow the tear to flow under the CL and increase oxygen.

Brief History of Scleral Lenses � � � In 1970, scleral lens were re-introduced again in Rigid Gas Permeable materials. Lens were difficult to fit and intimidating due to there relative size. With the recent focus on Dry Eye Disease contact lens companies have began promoting scleral lenses as a suitable solution for dry eye patients who want to remain in contacts.

Oxygen PPMA Material RGP Material

Oxygen Permeability of Different Materials (Dk/t) � � � � Glass = 0 Dk/t PPMA = 0 Dk/t Boston EO = 31 -61 Dk/t Boston XO = 61 -100 Dk/t Fluoroperm 151 = 151 -200 Dk/t Air Optix Night and Day = 140 Dk/t Scleral Lenses = 10 - 36. 7 Dk/t in center 17. 4 – 62. 6 Dk/t in peripheries

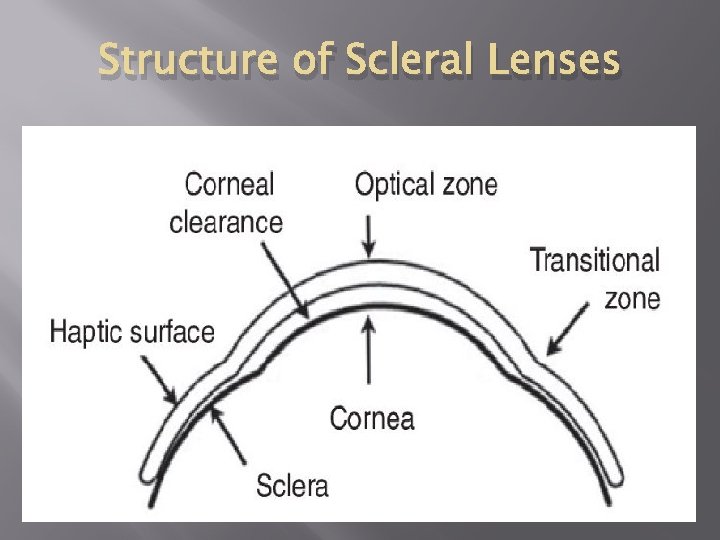
Structure of Scleral Lenses

Jupiter Scleral Lens � � � The Jupiter Scleral Lens has two designs – 15 mm diameter and the 18 mm diameter. Both are true scleral lenses, meaning they bear on the sclera and vault the cornea. Both have 5 curves organized in 3 zones

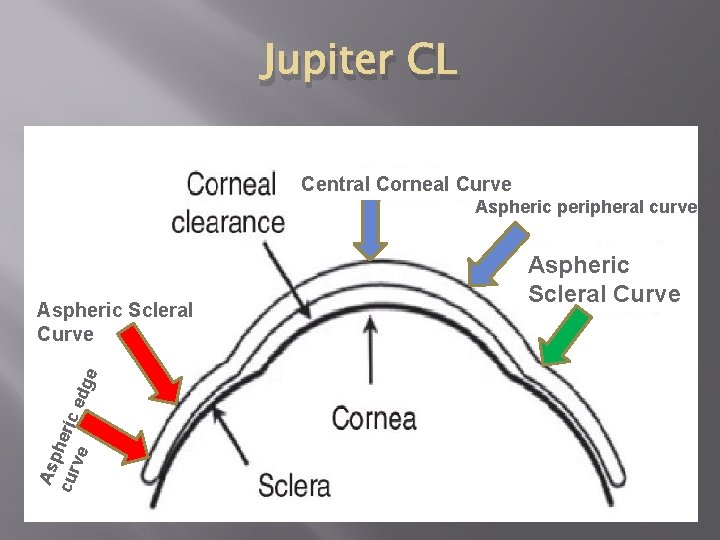
The 3 zones of the Jupiter CL � � � The Corneal Zone – the central corneal curve and the Aspheric peripheral corneal curve. The Limbal Zone – the Aspheric scleral curve. The Scleral Zone – the Aspheric scleral curve and the Aspheric edge curve.

Jupiter CL Central Corneal Curve Aspheric peripheral curve Asp cur heric ve edg e Aspheric Scleral Curve

3 Designs � � The Jupiter Standard – central and peripheral curves in Zone 1 are the SAME. The Jupiter Advanced Keratoconic – central curve STEEPER than peripheral curve. The Jupiter Reverse Geometry – central curve FLATTER than the peripheral curve. There is a fourth design – Toric Scleral Zone – front toric with double slab off ballasting.

Available Parameters � � � Base Curve – any Diameter – 13. 5 mm to 24. 0 mm BV power - +50. 00 D to -75. 00 D in 0. 25 steps Cylinder power - -0. 25 D to 15. 00 D in 0. 25 steps Axis – 1˚ to 180˚ in 1˚ steps Diagnostic lenses – 14 pre-designed lenses for each 3 configurations.

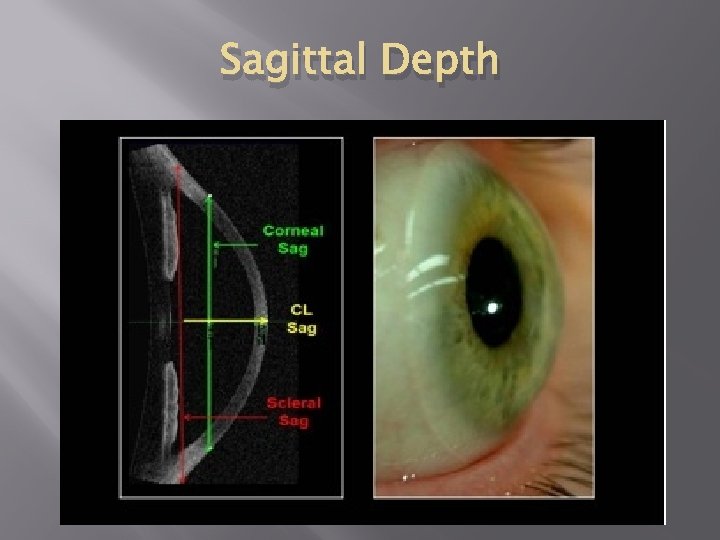
Fitting Process � � � Standard RGPs and Soft CLs rely heavily on Base Curve and Diameter to fit them properly. Scleral CLs rely heavily on Corneal Sagittal Depth and Diameter. With the use of an anterior segment OCT scan one can easily calculate the sagittal depth of the cornea and what the sagittal depth of the contact would be needed for that patient.

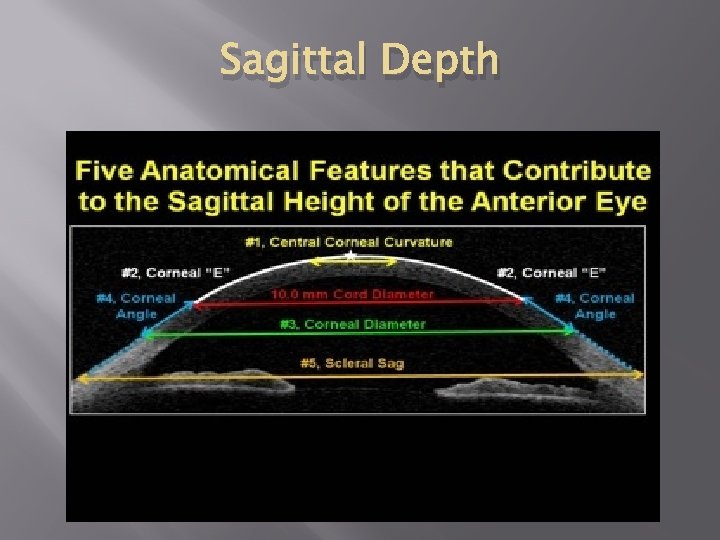
Sagittal Depth

Sagittal Depth

How Sagittal Depth Affects Corneal Diameter

Why is this important? � � When fitting you need to ensure adequate corneal clearance. What is adequate? For 18 mm design – 40 to 200 um For 15 mm design – 50 to 200 um

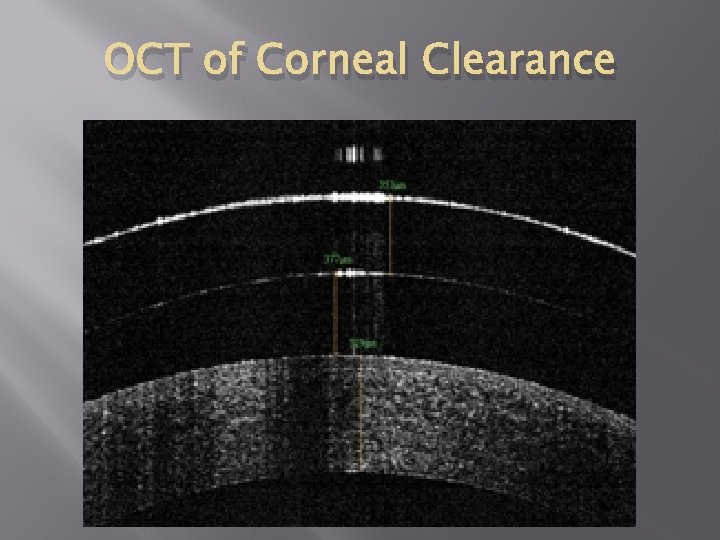
OCT of Corneal Clearance

What if you don’t have an OCT? � � An OCT makes fitting Scleral CLs easier; however it is not necessary. If you have the pachymetry reading of your patients cornea you can use that as a guide to estimate the corneal clearance of the scleral contact in the slit lamp. If clearance is too low you need to either increase sagittal depth by steeping the base curve or increasing the diameter. For example:

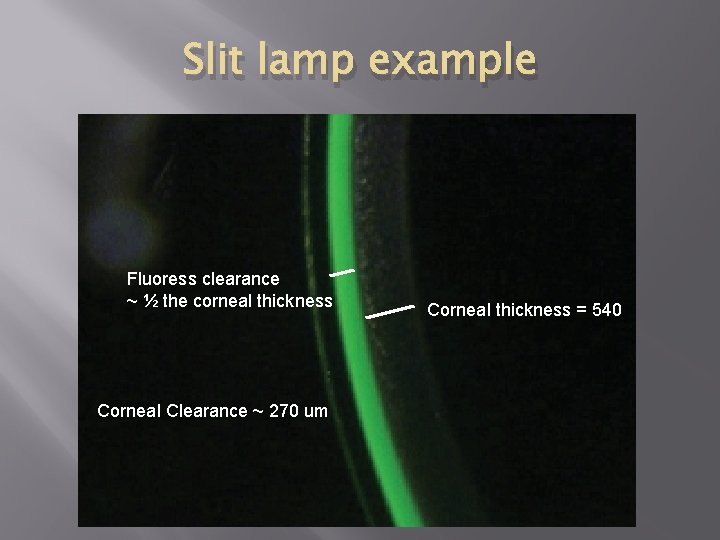
Slit lamp example Fluoress clearance ~ ½ the corneal thickness Corneal Clearance ~ 270 um Corneal thickness = 540

Where do you start? � � I always start steep and back down from there approximately 1. 00 D STEEPER than patients STEEPEST curvature. I have learned from me own fitting experience that it is important on initial fit that you leave about 400 um clearance. The reason for this is the scleral elasticity of every person is different. These lens can settle any where between 50 um to 250 um in a 4 h period and can continue to settle up to 8 h.

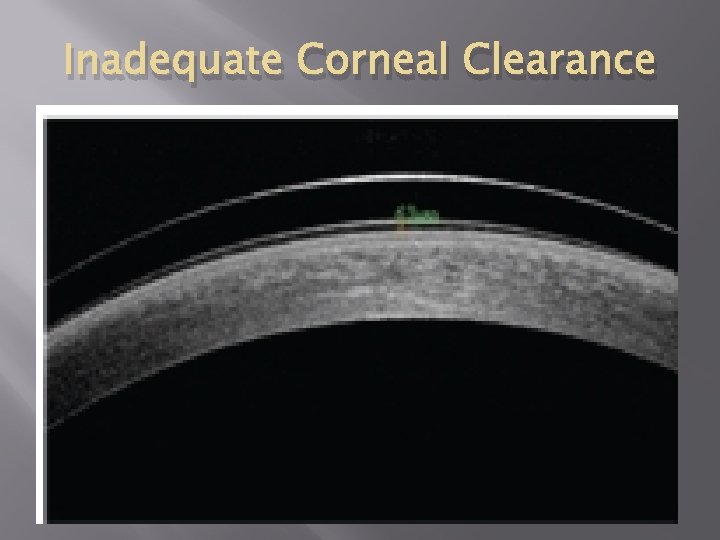
Inadequate Corneal Clearance

Excessive Corneal Clearance

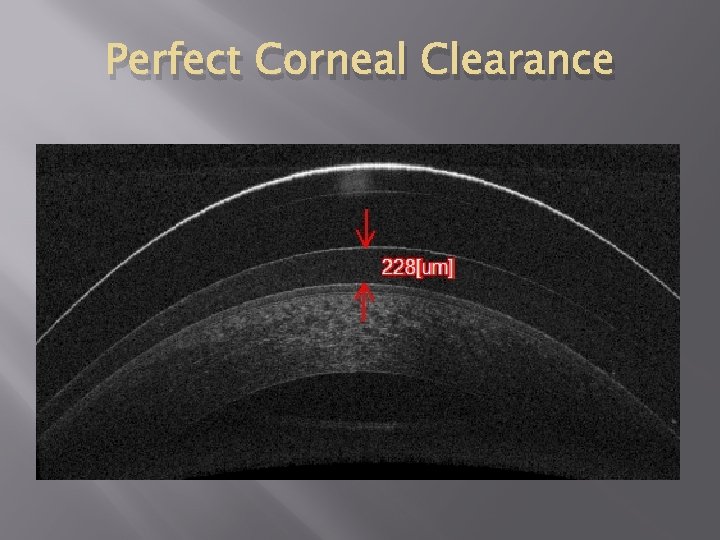
Perfect Corneal Clearance

What is next? � � Limbal clearance – complete and generous limbal clearance insures good tear circulation. If there is very little limbal clearance you must pick a large diameter lens. If there is too much limbal clearance large bubbles will form and a smaller diameter should be uses. Examples:

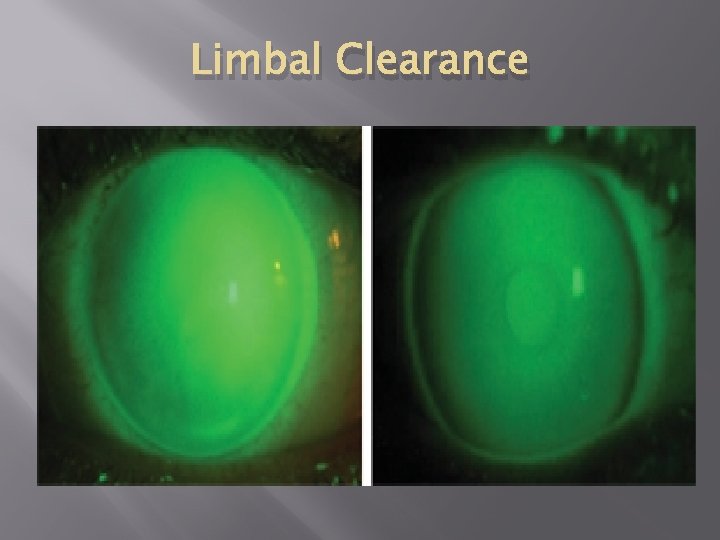
Limbal Clearance

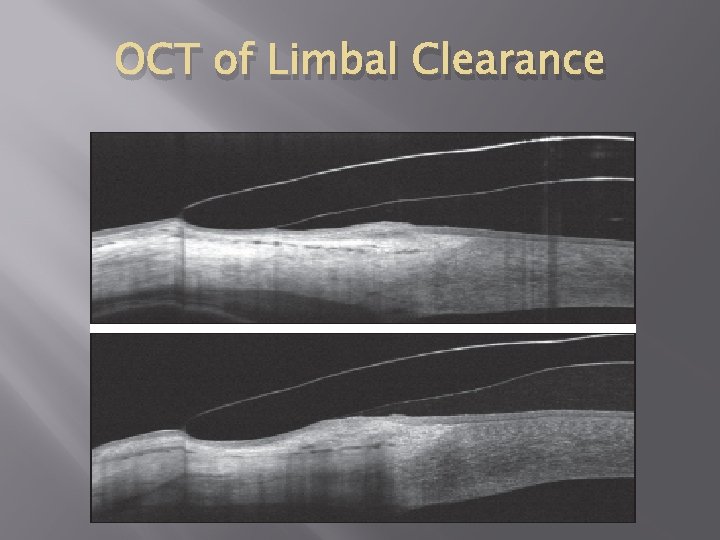
OCT of Limbal Clearance

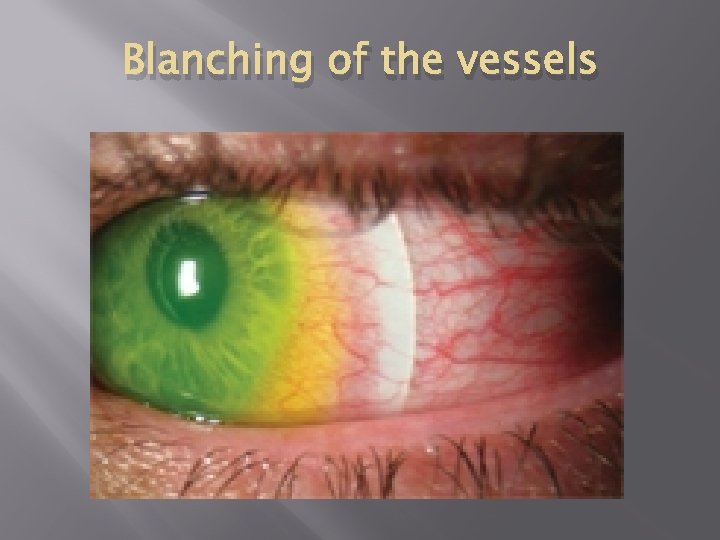
Next Step � � Peripheral Curves need to be adjusted to either tighten or loosen the fit of the CL. If the PCs are to tight this can lead to vessel blanching, hyperemia, difficulty removing the lens, fogging and discomfort for the patient. If the PCs are to loose seal off can not be maintained and the lens will not stay on the cornea. Examples:

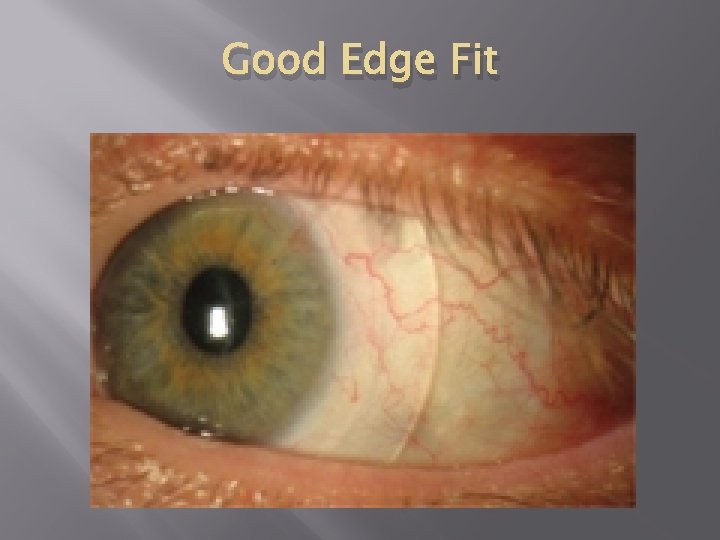
Good Edge Fit

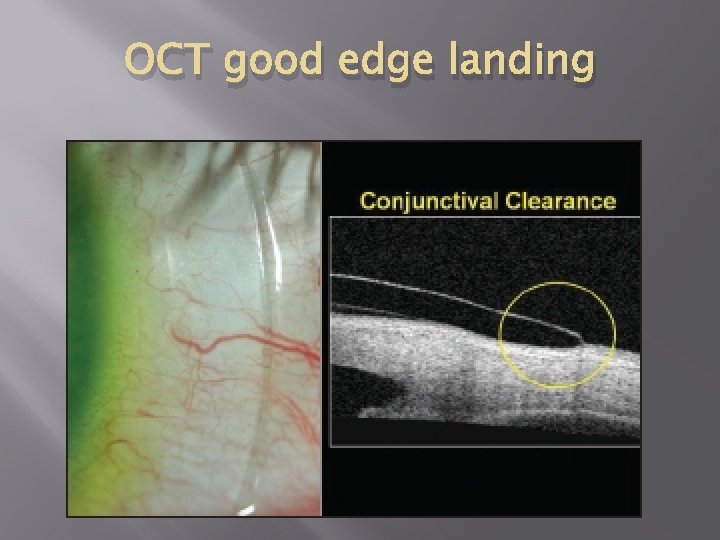
OCT good edge landing

Blanching of the vessels

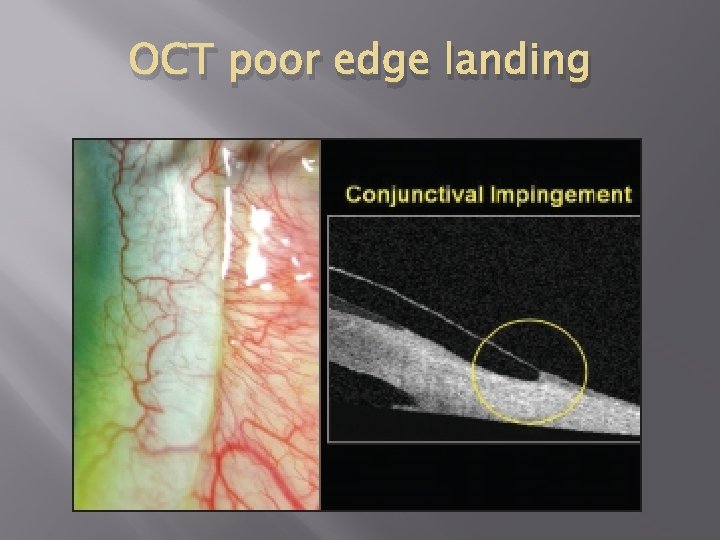
OCT poor edge landing

Why would we use Scleral Contacts � � � Dry Eye Ocular Surface disease Keratoconus High refractive error Irregular Corneas � Post Lasik � Post RK � Post PKP � Injury/Scarring

Dry Eye/Ocular Surface Disease � � Advantage – since the scleral contact is filled with preservative free saline the cornea is constantly bathed in fluid throughout the day. Advantage – since the scleral contact is vaulted over the cornea instead of touching the cornea it does not compromise the integrity of the corneal surface. Disadvantage – lenses are large and difficult to handle. Disadvantage – cost ~ 300 dollars per lens

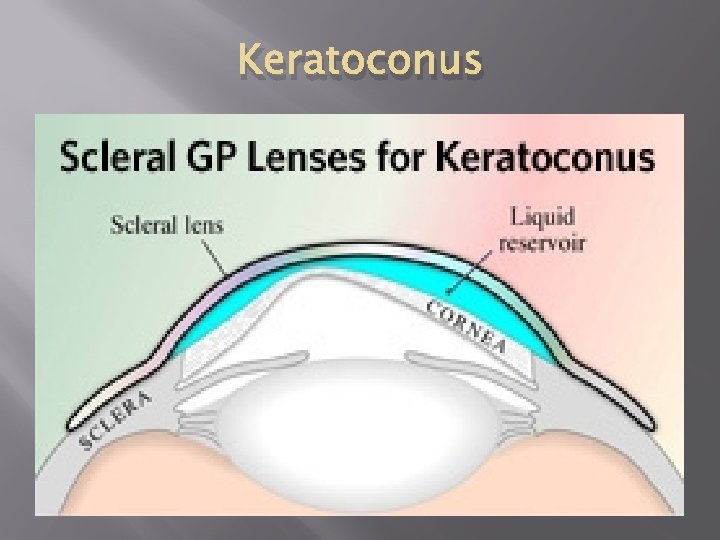
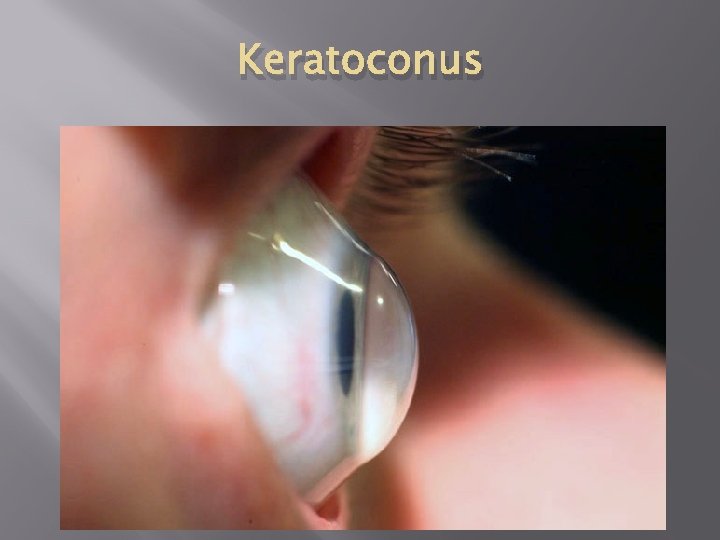
Keratoconus � � Keratoconus is a progressive thinning of the cornea secondary to the loss of the collagen fiber integrity. Thinning causes a bulging of the cornea resulting in an irregular corneal surface. Treatment for keratoconus: � Rigid Gas Permeable contacts � Hybrid Contacts (Duette) � Specialty Contacts (Rose K, Rose K 2 IC, Rose K Post) � Scleral Contacts � Surgery (Corneal Cross-linking, Intacs, PKP)

Keratoconus

Keratoconus

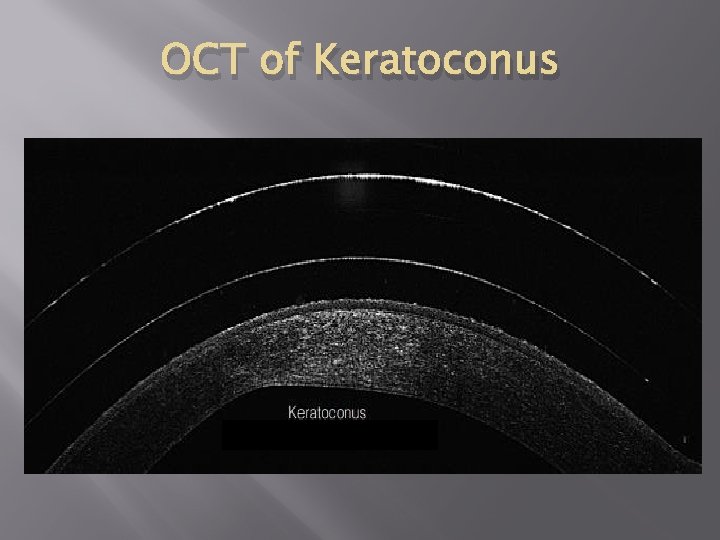
OCT of Keratoconus Keratocnusoooooo

Keratoconus � � Advantage – corneal vaulting reduce risk of corneal scarring since the lens does not touch the cornea. Advantage – excellent visual outcome even with advanced keratoconic patients. Disadvantage – difficult to handle Disadvantage - cost

High Refractive Error � Advantage – wide range of available powers � BV power - +50. 00 D to -75. 00 D in 0. 25 steps � Cylinder power - -0. 25 D to 15. 00 D in 0. 25 steps � Axis – 1˚ to 180˚ in 1˚ steps � � Disadvantage – difficult to handle Disadvantage - Cost

Post Surgerical � � � Advantage – wide range of powers Advantage – does not compromise corneal integrity Advantage – gives excellent visual outcome Disadvantage – difficult to handle Disadvantage - Cost

Summary � � � Scleral lenses are not difficult to fit if you follow some simple rules. Scleral lenses have improved materials and oxygen permeability to make them safe to fit. They can be a life saver for that difficult dry eye patient or irregular cornea. They are difficult to handle due to their large size They are no inexpensive, but worth it for the right patient.

Any Questions