Introduction to Pharmacodynamics Dr J Domenech 1 Objectives

Introduction to Pharmacodynamics Dr. J. Domenech 1

Objectives • Define the common terms related to Pharmacology. • Explain how drugs are named. • Explain the concepts of drugs in terms of pharmacokinetics, pharmacodynamics and pharmacotherapeutics. • Identify the common drug interactions. • Identify the common patient variables affecting drug action. • List the various routes of administration and the role of nurses in drug administration. 2

Definition of Pharmacology • is the study of drugs and its origin, chemical structure, preparation, administration, action, metabolism and excretion. • The study of drugs that alter functions of living organisms. 3

Implication of Pharmacology to Nursing – Responsible for drug administration – Responsible for the administration of medications that they direct others to give. – Ethical and legal responsibilities 4
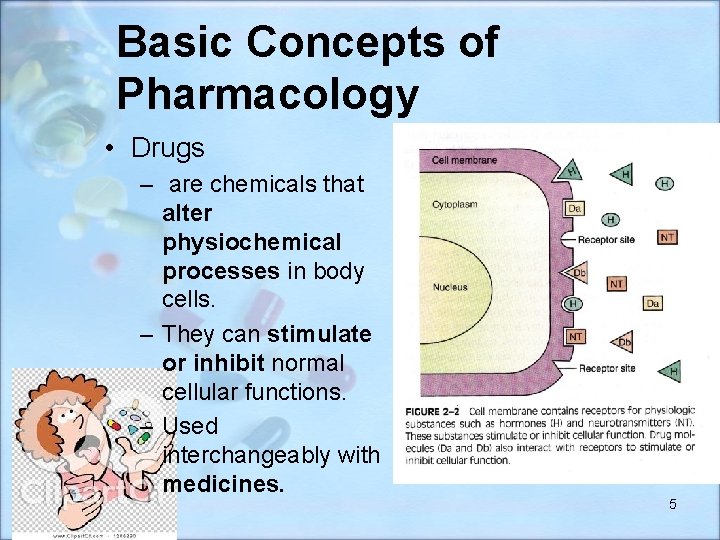
Basic Concepts of Pharmacology • Drugs – are chemicals that alter physiochemical processes in body cells. – They can stimulate or inhibit normal cellular functions. – Used interchangeably with medicines. 5

Drug Names 1. Generic or Nonproprietary Name: name approved by the Medical or Pharmaceutical Associations in the original country of manufacture and is adopted by all countries. e. g. Paracetamol 2. Brand name or trade name: name given by the manufacturer of the drug e. g. Adol or Panadol 3. Chemical name that describes the atomic or chemical strucuture 6
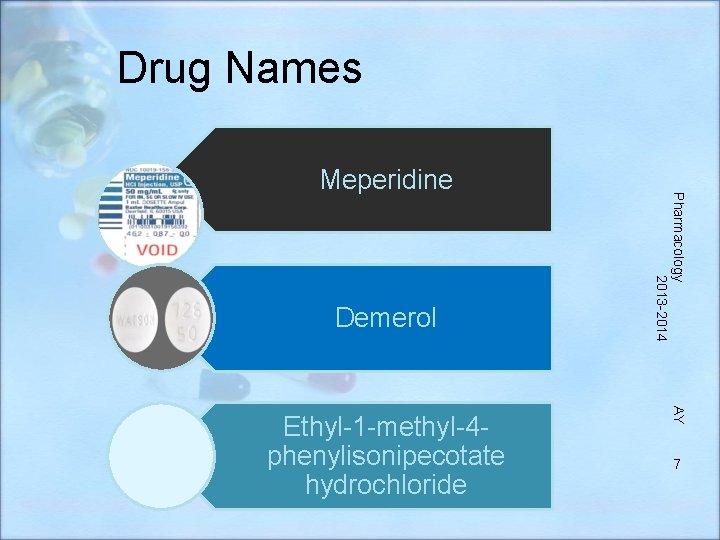
Drug Names Demerol AY Ethyl-1 -methyl-4 phenylisonipecotate hydrochloride Pharmacology 2013 -2014 Meperidine 7

Example Pharmacology 2013 -2014 AY 8

Exercise 1: Reading the Label Pharmacology 2013 -2014 AY 9

Pharmacokinetics 10

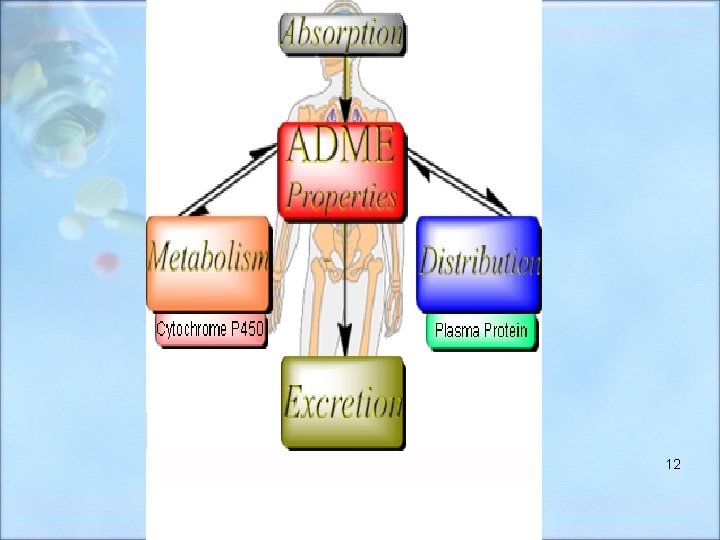
Pharmacokinetics-activities within the body • It includes: • Absorption • Distribution • Metabolism • Excretion 11
12
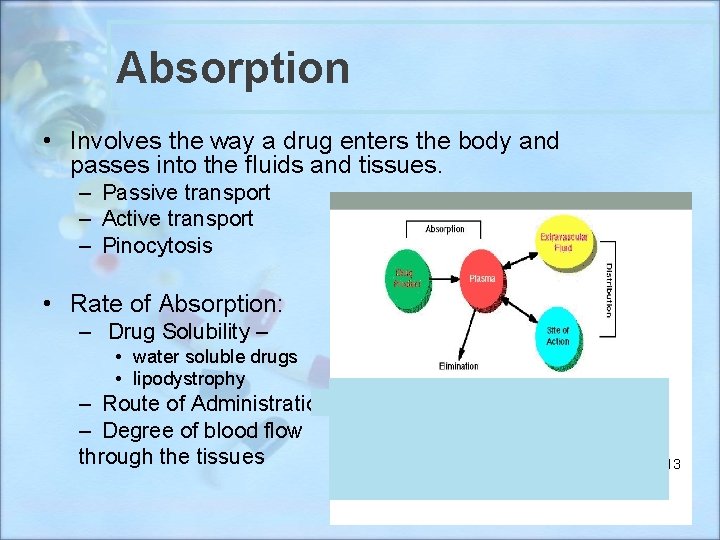
Absorption • Involves the way a drug enters the body and passes into the fluids and tissues. – Passive transport – Active transport – Pinocytosis • Rate of Absorption: – Drug Solubility – • water soluble drugs • lipodystrophy – Route of Administration – IV, IM, SC, Oral – Degree of blood flow through the tissues 13

Factors affecting Absorption – Drug Solubility – • water soluble drugs • lipodystrophy – Bioavailability- the extent to which active ingredients are absorbed and transported to sites of action. – p. H – Drug concentration – Circulation to site of absorption – Absorbing surface – Route of administration 14 – Presence of body conditions

Distribution • Is defined as the way the drug moves from the circulating body fluids to its site of action. Note: The greater the blood supply in a body organ, the faster the medication is absorbed – Therapeutic effect – certain blood level is maintained for the drugs to be effective. – Toxic effect - when blood level increase significantly over therapeutic level. 15

Bioavailability • is defined as the extent to which active ingredients are absorbed and transported to sites of action. • Factors 1. Drug solubility 2. Pharmaceutical formulation 3. p. H 4. Food 16
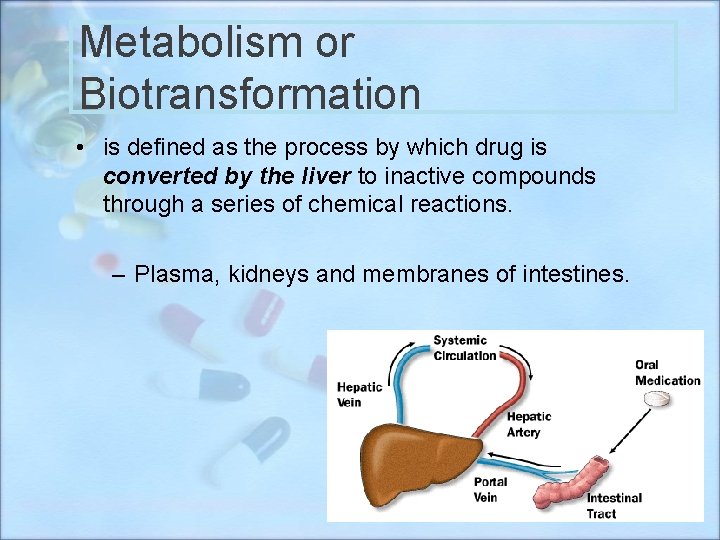
Metabolism or Biotransformation • is defined as the process by which drug is converted by the liver to inactive compounds through a series of chemical reactions. – Plasma, kidneys and membranes of intestines. 17
Excretion Pharmacology 2013 -2014 • Is the elimination of drugs from the body AY 18

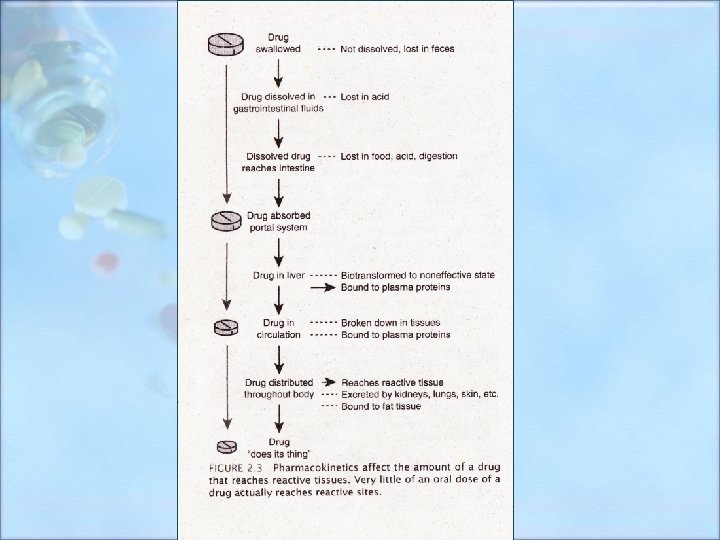
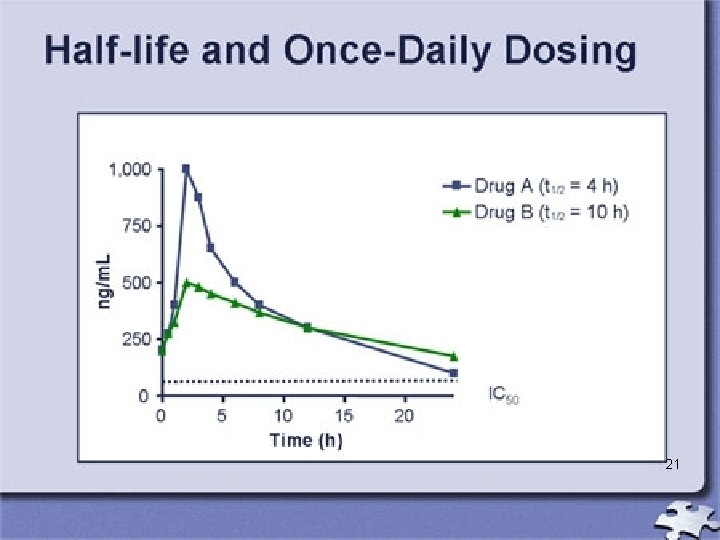
Half-life • Refers to the time required for the body to eliminate 50% of the drug. – It is important in planning the frequency of dosing. • Short half-life (2 -4 hours) : needs to be given frequently • Long half life: (21 -24 hours): requires less frequent dosing Note: It takes 5 to 6 half lives to eliminate approximately 98% of a the body drug from 19
21

Half-life • Liver and kidney disease patients may have problems of excreting a drug. • Difficulty in excreting a drug increases the half-life and increases the risk of toxicity. • Implication: may require frequent diagnostic tests and measuring renal and hepatic function. 22
Pharmacodynamics Drug Cellular Components Response/ Drug Effect 23

PHARMACODYNAMICS • Is the study of biochemical, and physiological and effect of drugs. • “what the drug does to the body” – Primary Effects - drug’s desired or therapeutic effect – Secondary Effects – all other effects whether desirable or undesirable. 24

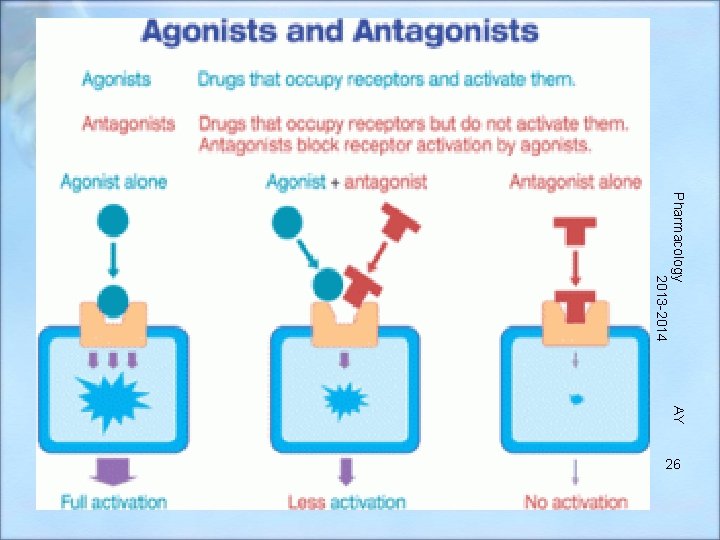
Drug Attachment • Medication chemically binds to specific sites called “receptor sites” – Agonist-chemical fits at receptor site well – Antagonist- a chemical blocks another chemical from getting to a receptor – Partial agonist - attach to the receptor but only produce a small effect Pharmacology AY 2013 -2014 25
Pharmacology 2013 -2014 AY 26

Basics of Drug Action • Desired action – the expected response of a medication • Side effects –known and frequently experienced, expected reaction to drug. • Adverse reaction –unexpected, unpredictable reactions that are not related too usual effects of a normal dose of the drug. 27
Drug Interaction • Takes place when one drug alters the action of another drug. • Some are helpful but often produce adverse effects. 28

Common Drug Interactions Pharmacology 2013 -2014 • Additive effect- takes place when 2 drugs are given together & double the effect is produced. Alcohol + aspirin= Pain relief AY 29

Common Drug Interactions – Protamine sulphate to counteract heparin toxicity Pharmacology 2013 -2014 • Antagonistic effect- takes place when 1 drug interferes with the action of another drug. AY 30

Common Drug Interactions • Displacement effect - takes place when 1 drug replaces another at the drug receptor site, increasing the effect of the 1 st drug. 31

Common Drug Interactions • Incompatibility –occurs when 2 drugs mixed together in a syringe produce a chemical reaction so they cannot be given. e. g. Protamine sulfate & vitamin K 32

Common Drug Interactions • Synergistic effect takes place when the effect of 2 drugs taken at the same time is greater than the sum of each drug given alone. AY E. g. combining diuretics & adrenergic blockers to lower the BP Pharmacology 2013 -2014 • Interference- occurs when 1 drug promotes the rapid excretion of another, thus reducing the activity of the 1 st. 33
age Body wt illness Pt. variables Cumulative effect Dependence Psychological overlay 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 34

Pharmacology 2013 -2014 Pharmacotherapeutics AY 35

Pharmacotherapeutics • Is defined as the use of drugs to treat diseases. Depends on: Severity § Urgency § Prognosis of patient’s condition § 36

Routes of Drug Administration

1: Enteral Medications • administered directly into the G. I. T. through the oral, nasogastric (NG) or rectal routes q. Advantages: q. Convenience for nurse & patient q. Most medications are available in oral route q. Inexpensive to make oral preparations q. Can be removed by gastric lavage or make to vomit 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 38

Disadvantages • cannot be administered to very nauseated/vomiting or unconscious persons • some loose their effectiveness if mixed with gastric secretions • onset of action may vary due to changes in absorption in the GIT 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 39

Forms of Oral Medication • Capsules-are gelatin containers that hold powder or liquid medicine. • Elixirs- clear liquids made up of drugs dissolved in alcohol & water with coloring & flavoring agents added. • Emulsions-are solutions that have small droplets of water & medication dispersed in oil, or oil & medication dispersed in water. 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 40

Forms of Oral Medication AY • Suspensions- are liquids w/ solid, insoluble drug particles dispersed throughout. Pharmacology 2013 -2014 • Lozenges- are medicines mixed with a hard sugar base to produce a small, hard preparation of various shapes & sizes. 41

Forms of Oral Medication • Syrups-are liquids w/ a high sugar content designed to disguise the bitter taste of a drug. Pediatric use. • Tablets-dried, powdered drugs compressed into small shapes. 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 42

2. Parenteral Administration • Reasons: 1. When the patient cannot take an oral medication 2. When the medication must be given quickly 3. When medication might be destroyed by gastric enzymes 4. When medication must be given at a controlled rate 5. When the medication is not available in an enteral form. 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 43

Parenteral Medications • INTRAMUSCULAR – 90 ° – Provides faster medication absorption because of muscle’s greater vascularity • SUBCUTANEOUS- 45 ° – Placing medications in the loose connective tissue under the dermis • INTRADERMAL- 15 ° 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 44

Other Routes of Administration • Topical administration – skin – – – Cleanse Soften Disinfect Lubricate E. g. clotrimazole –cream dermatophytosis – atropine- eye-dilate the pupil • Transdermal route nitroglycerin (skin patch) systemic vasodilation in angina 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 45
Other Routes of Administration • Inhalation – provides rapid delivery of drugs to a large area of mucus membranes & tissues of the respiratory system. – Anesthesia – Bronchodilators • Intranasal – desmopressin for diabetes insipidus – Calcitonin- a peptide hormone for tx of osteoporosis 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 46

Other Routes of Administration • Intrathecal injection- introduction of hypodermic needle into the subarachnoid space for the purpose of instilling a material for diffusion throughout the spinal fluid. • Intraventricular- space into the ventricle – Both gains access to the CSF e. g. amphotericin B –in meningitis 6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 47

6/15/2021 Pharmacology Unit 1 Class Session 1 Pharmacology 48

Ms. Maria Jose
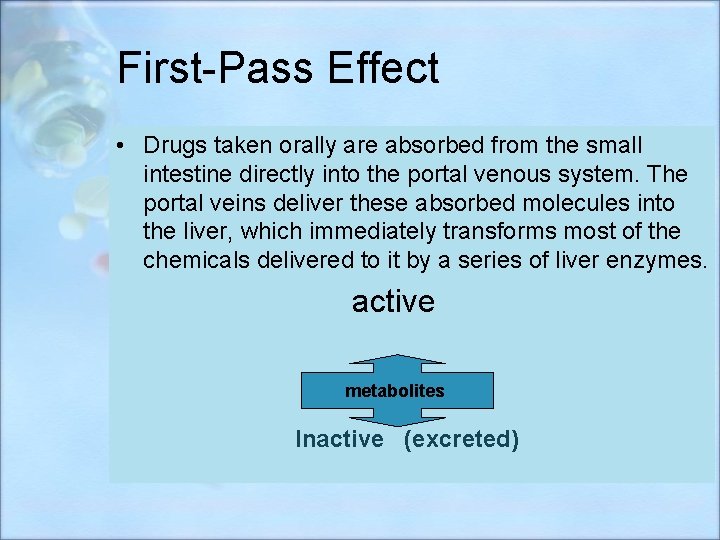
First-Pass Effect • Drugs taken orally are absorbed from the small intestine directly into the portal venous system. The portal veins deliver these absorbed molecules into the liver, which immediately transforms most of the chemicals delivered to it by a series of liver enzymes. active metabolites Inactive (excreted)

Protein Binding • Most drugs are bound to some extent to proteins in the blood to be carried into circulation. • The protein-drug complex is relatively large & cannot enter into capillaries & then into tissues to react. The drug must be freed from the protein’s binding site at the tissues.

Protein Binding • Tightly bound – released very slowly. these drugs have very long duration of action (not freed to be broken down or excreted) , slowly released into the reactive tissue. • Loosely bound – tend to act quickly and excreted quickly • Compete for protein binding sites – alters effectiveness or causing toxicity when 2 drugs are given together.

Half-Life • Half life of a drug is the time it takes for the amount of drug in the body to decrease to onehalf of the peak level it previously achieved. • e. g. – 20 mg of a drug with half-life of 2 hours, 10 mg of the drug will remain 2 hours after administration. Two hours later, 5 mg will be left (one-half of the previous level); in 2 more hours, only 2. 5 mg will remain.

Why to know half-life? – To determine the appropriate timing for a drug dose or – determining the duration of a drug’s effect on the body.

Determining the Impact of Half-Life on Drug Levels • A patient is taking a drug that has a halflife of 12 hours. You are trying to determine when a 50 -mg dose of the drug will be gone from the body. – In 12 hours, half of the 50 mg (25 mg) would be in the body – In another 12 hours (24 hours) half of 25 mg (12. 5 mg) would remain in the body.

Determining the Impact of Half-Life on Drug Levels – After 36 hours, half of 12. 5 mg (6. 25 mg) would remain – After 48 hours, half of the 6. 25 mg (3. 125 mg) would remain – After 60 hours, half of the 3. 125 mg (1. 56 mg) would remain – After 72 hours, half of the 1. 56 mg (0. 78 mg) would remain

Determining the Impact of Half-Life on Drug Levels – After 84 hours, half of the 0. 78 mg (0. 39 mg) would remain – Twelve more hours (for a total of 96 hours) would reduce the drug amount to 0. 195 mg – Finally, 12 more hours (108 hours) would reduce the amount of the drug into the body to 0. 097 mg, which is negligible – Therefore, it would take 4 ½ to 5 days to clear the drug from the body.


- Slides: 59