Introduction to Nephrology JENNIFER SMITH FNPS Objectives v

Introduction to Nephrology JENNIFER SMITH, FNP-S

Objectives v. Provide an overview of basic renal anatomy and physiology v. Discuss the growing epidemic of chronic kidney disease due to increased incidence of obesity, hypertension, and diabetes v. Define the stages of chronic kidney diseases and discuss associated complications such as: anemia of chronic kidney disease, secondary hyperparathyroidism, hypertension, cardiovascular disease, hyperkalemia, hyperphostphatemia, and bone disease v. Discuss management of chronic kidney disease v. Discuss other common kidney disorders that may lead to end-stage renal disease

The Kidney §Location- relatively high under lower ribs in the retroperitoneal space
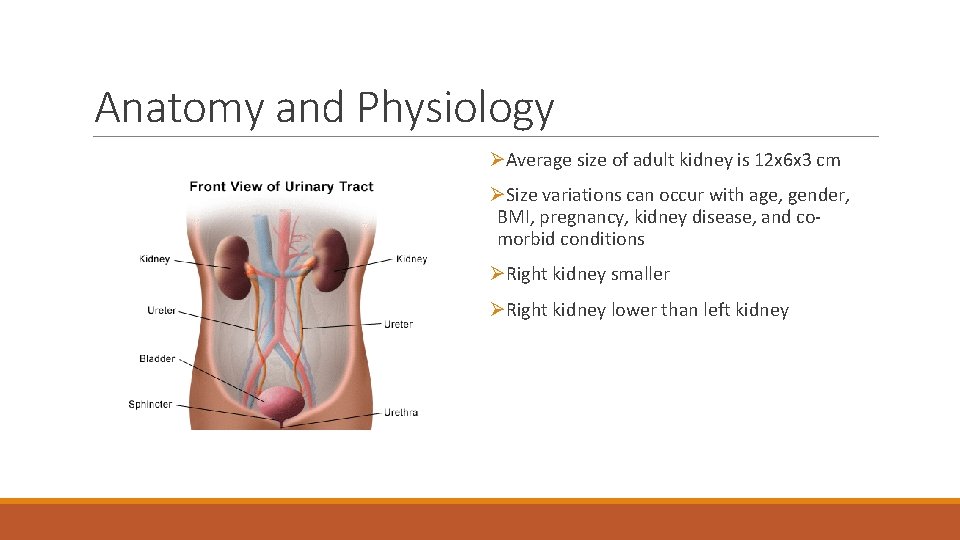
Anatomy and Physiology ØAverage size of adult kidney is 12 x 6 x 3 cm ØSize variations can occur with age, gender, BMI, pregnancy, kidney disease, and comorbid conditions ØRight kidney smaller ØRight kidney lower than left kidney
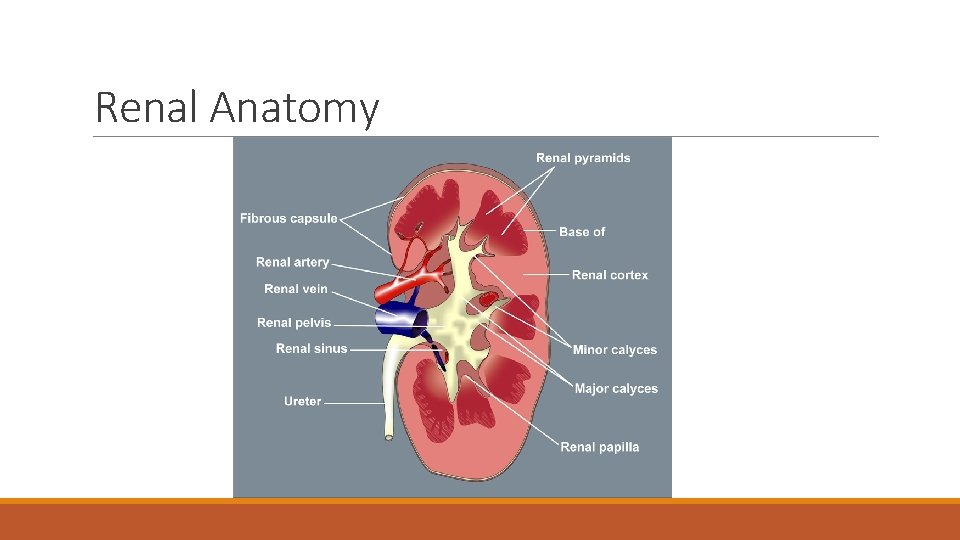
Renal Anatomy

Structure of Kidney v. Cortex-the outer layer of the kidney comprising the glomeruli, most of the proximal tubules, and some of the distal tubules v. Medulla-formed by 7 -9 cone shape pyramids which extend into the renal pelvis v. Renal Pelvis-flat funnel-like tube continuous with ureter as it leaves the hilus v. Calyces- subdivided into major and minor calyces ØMajor calyces- 2 or 3 branches off of renal pelvis ØMinor calyces- cup-shaped areas that enclose the papillae of the pyramids. Continuously collect urine draining from papillae, emptying it into the renal (Greenburg et al, 2009) pelvis

The Nephron v Functional unit of kidney v. Consisting of glomerulus and long tubule v. Approximately 1 million nephrons in each kidney v. Filters plasma->reabsorption and secretion->forms filtrate free of protein->regulates the filtrate to maintain fluid volume, electrolytes, and p. H (Greenburg et al, 2009)

The Nephron v. Glomerulus- tuft of capillaries surrounded by Bowman’s capsule. Together form the renal corpuscle. v. Tubules- segmented into proximal tubule, loop of Henle, distal tubule, and collecting tubules • Tubular Transport: ØProximal Tubule- active reabsorption of sodium ØLoop of Henle and distal tubule- concentration or dilution of urine ØCollecting Tubules- run through medullary pyramids (give them their striped appearance) (Greenburg et al, 2009)
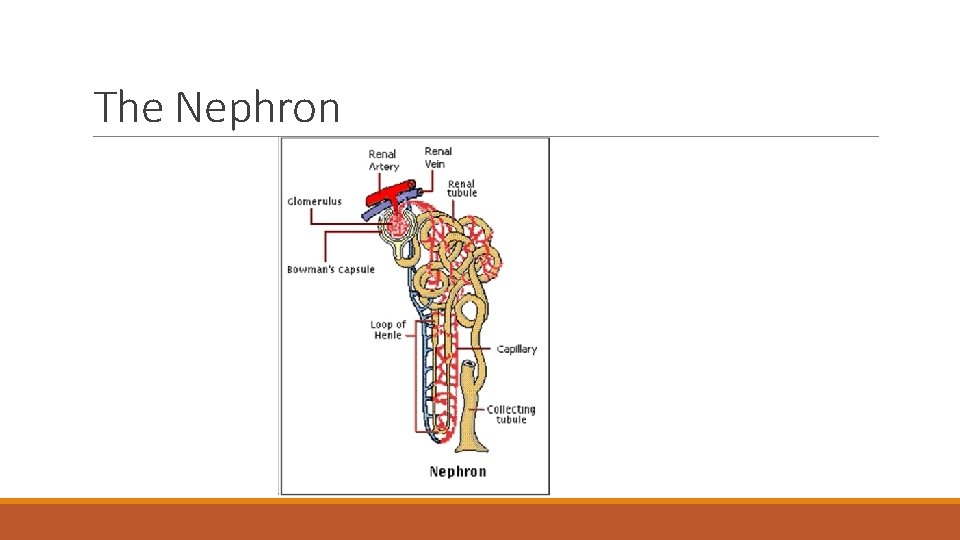
The Nephron
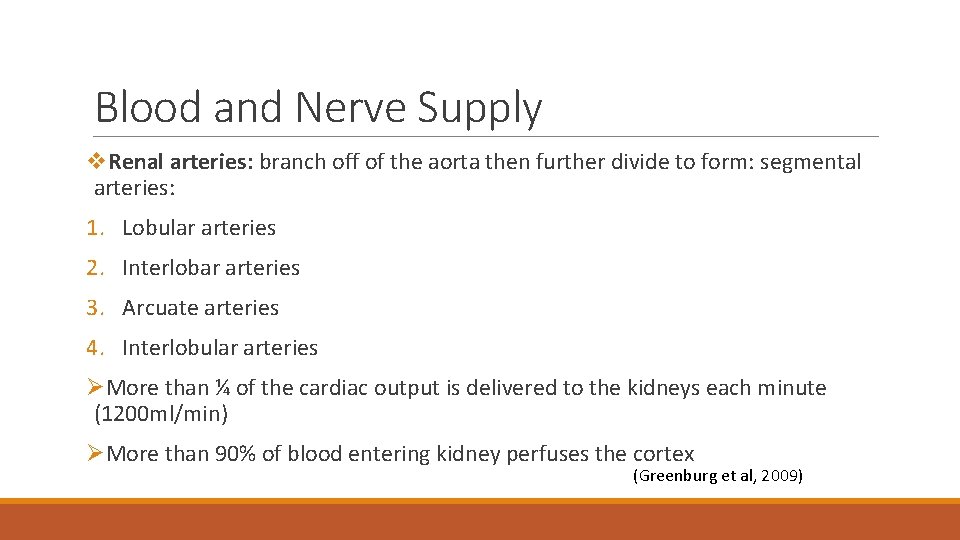
Blood and Nerve Supply v. Renal arteries: branch off of the aorta then further divide to form: segmental arteries: 1. Lobular arteries 2. Interlobar arteries 3. Arcuate arteries 4. Interlobular arteries ØMore than ¼ of the cardiac output is delivered to the kidneys each minute (1200 ml/min) ØMore than 90% of blood entering kidney perfuses the cortex (Greenburg et al, 2009)
Blood and Nerve Supply v. Renal Veins- trace pathway of arterial blood supply in reverse ØEmpty into the inferior vena cava ØLeft renal vein is about 2 x longer in order to extend to IVC in its position to right of vertebral column v. Renal Plexus-network of autonomic nerve fibers and ganglia. Supplied by sympathetic fibers from thoracic and lumbar splanchnic nerves v. Sympathetic fibers- vasomotor fibers that control renal blood flow by adjusting arteriolar diameters (Greenburg et al, 2009)
Functions of Kidney v. Maintenance of body fluids composition (fluid volume, osmolarity, electrolyte, and acid/base balance. v. Excretion of metabolic end products and foreign substances (i. e. urea, toxins, drugs). v. Production/secretion of enzymes and hormones (Greenburg et al, 2009)

Functions of Kidney v. Renal Hormones and Enzymes ØRenin- produced in juxtaglomerular apparatus. Catalyzes production of angiotensin which is important for sodium balance and blood pressure regulation ØErythropoietin- stimulates maturation of RBC’s in bone marrow Ø 1, 25 -Dihydroxyvitamin D 3 - most active form of Vitamin D 3, steroid hormone that helps the body regulate calcium/phosphorus balance (Greenburg et al, 2009)
Functions of Kidney Alterations in body fluid composition and fluid volume can impact: ØCardiac Output and Blood Pressure- dependent on optimal plasma volume ØEnzyme Function- most function best in narrow range of p. H and ion concentrations ØCell Membrane Potential- depends on potassium concentrations ØMembrane excitability- depends on calcium ion concentrations

Evaluation of Renal Function v. Glomerular Filtration Rate (GFR) v. Serum Creatinine, Blood Urea Nitrogen v. MAU/CR ratio Ø 30 -300 mg/dl microalbuminemia Ø>/= 300 mg/dl- macroalbuminemia v 24 hour urine collection

Glomerular Filtration Rate (GFR) v. GFR- amount of fluid filtered from blood into glomerular capsule each minute v. GFR- 180 L/day v. GFR controlled by: ØAuto-regulation (tubuloglomerular feedback) ØNeural regulation ØHormonal regulation- renal aldosterone angiotensin system

Screening v. DM- largest single cause of CKD in the U. S. ØInitial screening 5 years after diagnosis of Type I DM ØAT DIAGNOSIS of type II DM ØAnnually thereafter v. HTN v. Family history of CKD v. Autoimmune disorders
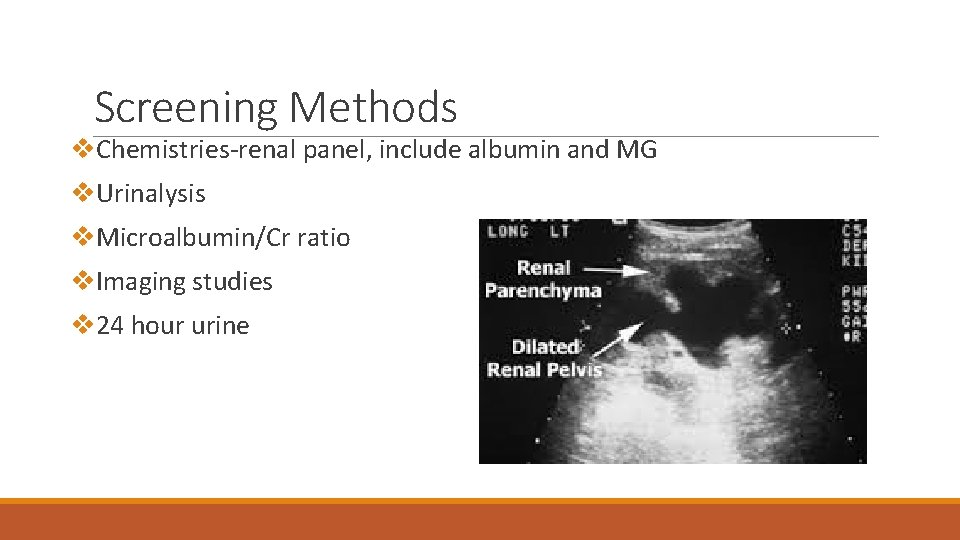
Screening Methods v. Chemistries-renal panel, include albumin and MG v. Urinalysis v. Microalbumin/Cr ratio v. Imaging studies v 24 hour urine
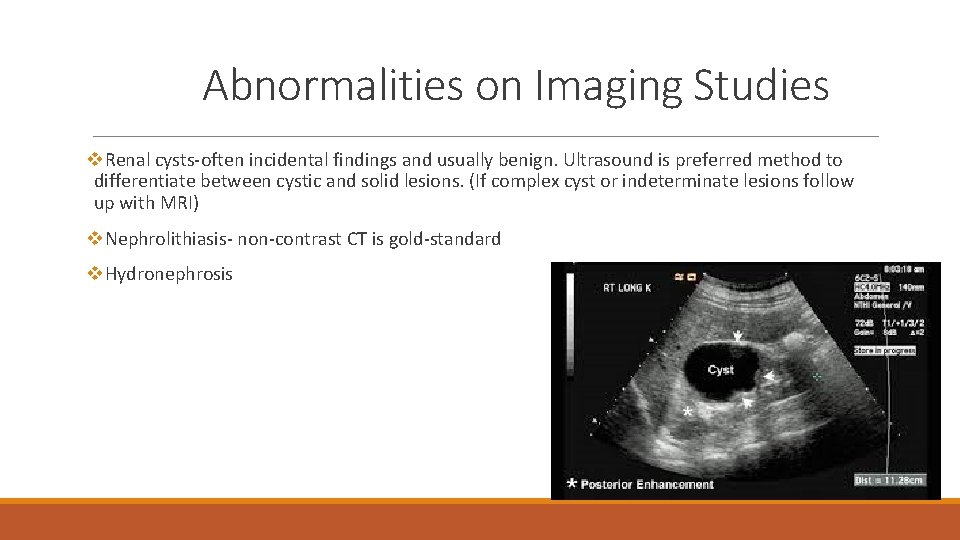
Abnormalities on Imaging Studies v. Renal cysts-often incidental findings and usually benign. Ultrasound is preferred method to differentiate between cystic and solid lesions. (If complex cyst or indeterminate lesions follow up with MRI) v. Nephrolithiasis- non-contrast CT is gold-standard v. Hydronephrosis

Chronic Kidney Disease v. CKD is defined as: ØKidney damage for 3 months or longer to include either structural or functional abnormalities With or without a decrease in GFR (as seen by pathology abnormalities, markers of kidney damage in blood or urine, or abnormalities on imaging studies). ØGFR of less than 60 ml/min for at least 3 months

Prevalence v 31 million in U. S. (16% of population) and rising v 1 in 10 adults have some level of CKD v. Majority of people with CKD are in Stage 1 -3 v. Incidence is increasing rapidly in those >65 v. ESRD expected to reach 2. 2 million by 2030 v. ESRD males > females v. Most people with CKD die before they are diagnoses, primarily of cardiovascular complications v. African Americans are 4 times more likely to develop CKD than Caucasians. (Domino, 2013)

Risk Factors v. Hypertension v. Systemic infections v. DM v. Low income/education v. Minority populations v. Autoimmune diseases (vasculitis, connective tissue disorder) v. Obesity v. Congenital anomalies v. Smoking v. Family history of CKD or transplant v. Age > 60 years v. Kidney stones v. Frequent urinary tract infections v. Exposure to certain drugs (i. e. NSAID) v. Cardiovascular disease v. Acute Kidney Injury v. Race v. Neoplasm v. Urinary Tract Obstruction v. Hyperlipidemia (Domino, 2013)
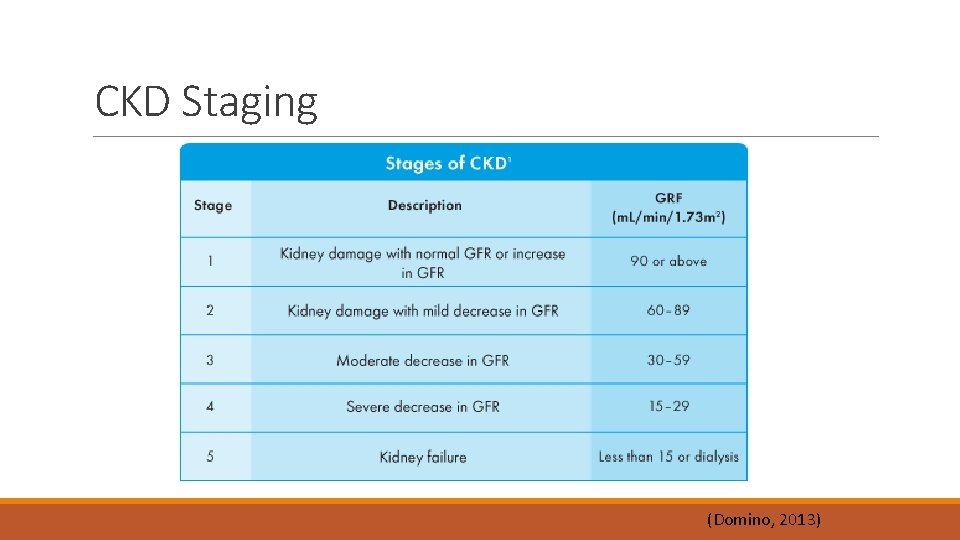
CKD Staging (Domino, 2013)

Clinical Findings of CKD by Stage I and II Stage IV Stage V • Asymptomatic, BUN/CR slightly elevated or normal, acid-base, fluid, and electrolyte balance is maintained through compensation of remaining nephrons • Usually asymptomatic, BUN/CR increased. Erythropoietin decreased and PTH levels are increased • Patient may have anemia, acidosis, hypocalcemia, hyperphosphatemia, and hyperkalemia • Fatigue, dysgeusia, anorexia, nausea, pruritus, asterixis, uremic breath

Associated Complications v. HTN v. Anemia v. Secondary Hyperparathyroidism (SHPT) v. Hyperkalemia v. Cardiovascular complications v. Bone disease (Greenburg et al, 2009)

Hypertension v. Can be cause or effect ØInappropriate sodium reabsorption leading to increased fluid volume is primary cause of HTN in CKD ØRAAS stimulation ØRenal Artery Stenosis ØVascular Calcifications

Managing HTN in CKD v. Goal is BP < 130/80 mm/Hg v. Many patients will require multiple drug classifications to control BP due to increased vascular resistance and increased fluid volume v. Uncontrolled HTN is key risk for progression of CKD v. An increase in BP of 20/10 mm. Hg doubles risk for cardiovascular disease (Greenburg et al, 2009)

Pharmacologic Management HTN in CKD v. ACE/ARB Ø“Reno protective” ØLowers intra-glomerular pressure and reduces proteinuria, slowing the progression of CKD ØMay see initial increase in s. Cr (less than 30% that returns to baseline within 2 months if acceptable) ØMonitor K level ØContraindicated in renal artery stenosis, uncontrolled hyperkalemia, pregnancy, history of angioedema ØNot unusual to see patients with CKD on several different classifications of medications (Collins, 2012)

Pharmacologic Management HTN v. Calcium Channel Blocker: ØDihydropyrodines-Amlodipine, Valsaartan §Increase intraglomerular pressure causing worsening of proteinuria if not used in combination with a ACE/ARB ØNon-Dihydropyrodines (Diltiazem, Verapamil) §If failing on ACE/ARB therapy, have been shown to reduce proteinuria v. Vasodilators (Hydralazine, Isosorbide) ØMay be useful in patients with known renal artery stenosis (Collins, 2012)

Pharmacology Continued v. Diuretics ØDiuretic resistance may be due to high sodium diet v. Loop Diuretics ØBest dosed BID for CKD III or higher ØMay take second dose 6 hours after 1 st dose ØMonitor serum K+ levels, may need replacement v. Thiazide Diuretics ØEffective in patients with GFR>30 ØMonitor uric acid level as may cause gout ØMonitor serum K+ levels (Collins, 2009)

Diuretics v. Most CKD patients require diuretics v. Enhances antihypertensive therapy v. Reduces tubular sodium reabsorption which in turn increases sodium excretion and lowers ECF volume, lowering BP v. Choice of diuretic depends on CKD stage, volume of fluid overload, and other individual patient factors v. Use potassium sparing diuretics with caution if GFR is less than 30, or if concomitant use of ACEI/ARB v. Don’t decrease diuretics due to increase BUN/Cr will fluctuate with fluid volume v. Don’t treat the lab, treat the patient! (Collins, 2009)

CKD in Pregnancy v. Renal function in CKD may deteriorate during pregnancy v. CR >1. 5 and hypertension are major risk factors of worsening renal function v. Increased risk of premature labor, preeclampsia, and/or fetal loss v. ACE inhibitors and ARBs are contraindicated v. Use diuretics with caution (Domino, 2009)
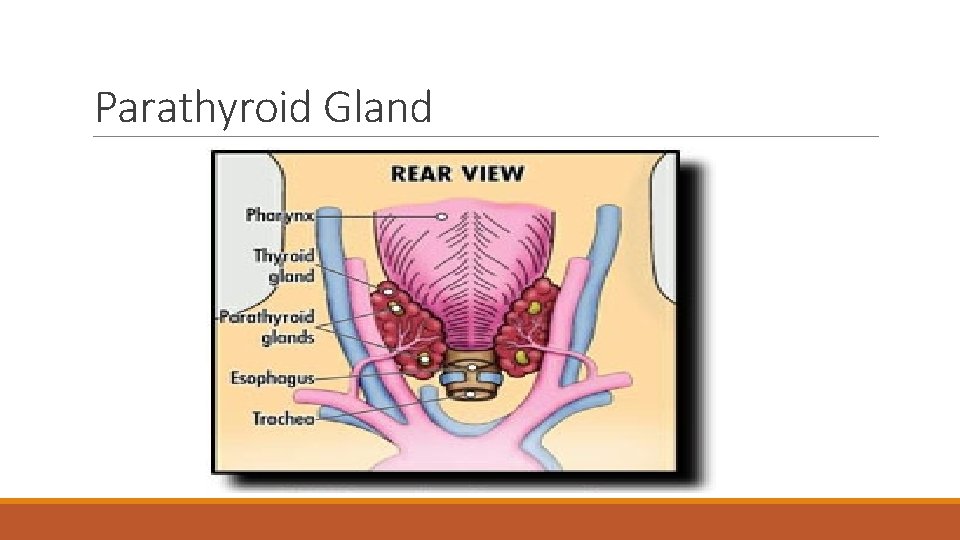
Parathyroid Gland

Secondary Hyperparathyroidism (SHPT) v. The parathyroid glands main function is to control calcium within the blood and bones v. Parathyroid glands atrophy due to constant stimuli in CKD (either hypocalcemia or hyperphosphatemia). v. Atrophied glands secrete PTH, causing serum levels to rise v. PTH stimulates conversion of active Vitamin D to increase calcium absorption from the GI tract v. Over time, elevated PTH leads to bone disease, vascular and soft tissue calcifications, decreased quality of life, amputations, and increased mortality (Greenberg et al, 2009)
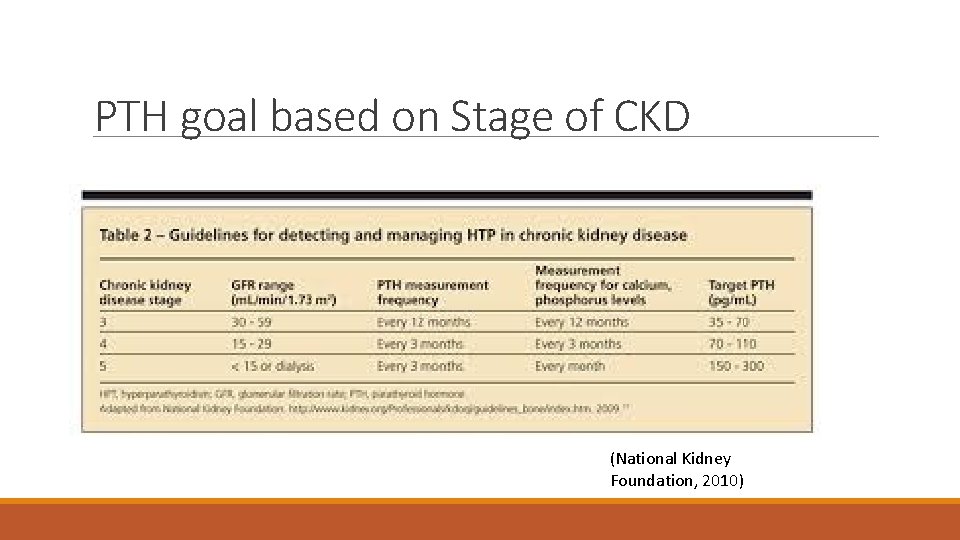
PTH goal based on Stage of CKD (National Kidney Foundation, 2010)

SHPT v. Monitoring ØIntact PTH levels ØCa and Phosphorus levels ØVitamin D 1, 25 level ØTreatment ØOral Calcitriol, Zemplar, Hectoral, Sensipar ØMay need Vitamin D replacement ØTreat hyperphosphatemia- if you control phosphorus you will control the parathyroid ØMay need parathyroidextomy

Hyperphosphatemia v. Increases cardiovascular risk factors v. Calcifications develop may result in bone deformities and amputations v. High levels of phosphorous cause Calcium to be pulled from bone v. Osteoporosis v. Bone pain v. Fractures
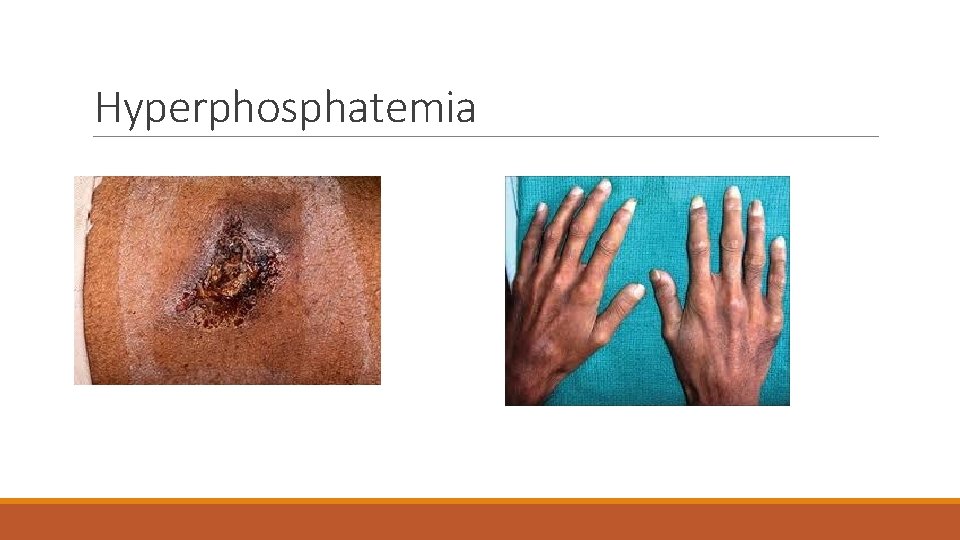
Hyperphosphatemia

Treatment for Hyperphosphatemia
Cardiovascular Complications in CKD v. Patients with CKD more likely to die from CVD v. Survival rate of MI patients with CKD are 53% compared to 36% v. Vascular calcifications common in patients with hyperphosphatemia and SHPT v. Cardio-renal syndrome v. Patients with CKD should have annual EKG, stress test on file

Hyperkalemia v. Decreased Renal Excretion ØAcute or chronic renal failure ØAldosterone deficiency (frequently associated with diabetic nephropathy, chronic interstitial nephritis, or obstructive uropathy) ØAdrenal Insufficiency (Addison’s disease) ØKidney diseased that impair distal tubule function (Sickle cell, Systemic Lupus Erythematosus) v. Abnormal Potassium Distribution ØInsulin deficiency ØB-Blockers ØMetabolic and Respiratory Acidosis v. Abnormal Potassium Release from Cells ØRhabdomyolysis ØTumor lysis syndrome (Greenburg et al, 2009)

Treatment Goals to Slow Progression of CKD ØControl blood pressure <130/80 or <140/80 in renal artery stenosis ØLow NA diet ØACE/ARB therapy ØDiuretics ØNondihydropyridine Calcium Channel Blockers ØOptimize control of DM (HGA 1 C <7. 5) ØControl dyslipidemia LDL goal <100 ØRestrict dietary protein ØLow phosphorous diet

Prescribing Considerations in CKD v. Dose adjust medications based on GFR (Metformin, Allopurinol, many antibiotics, etc) v. Avoid use of nephrotoxic drugs (NSAIDS, contrast dye, Bactrim) v. When treating DM with CKD less insulin may be required due to decreased gluconeogenesis v. Best to avoid 1 st generation sulfonylureas as they have increased risk for hypoglycemia due to decreased renal clearance v. Second generation sulfonylureas are preferred (Glipizide) v. As always start low and go slow! (Greenburg et al, 2009)

Drug-Induced Hyperkalemia v. Block Sodium Channel in the Distal Nephron v. Block Na+, K+-ATPase Activity in the Distal Nephron ØPotassium-sparing diuretics: amiloride, triamterene ØCyclosporine ØAntibiotics: trimethoprim, pentamidine v. Potassium Release from Injured Cells v. Block Aldosterone Production ØDrug-induced rhabdomyolysis (lovastatin, cocaine) ØACE inhibitors ØDrug induced tumor lysis syndrome(chemotherapy agents in leukemia's, high-grade lymphomas) ØARBs ØNSAIDS and COX-2 inhibitors ØHeparin ØTacrolimus ØDepolarizing paralytic agents (succinylcholine) v. Block Aldosterone Receptor ØSpironolactone ØEplerenone

NSAID’s v. Major cause of CKD v. Block Aldosterone Production v. Widespread use of these drugs are leading to increased cases of NSAID-induced nephropathy v. Not a problem if no renal impairment v. Avoid in CKD and transplant patients

Diabetic Nephropathy v. About 35% of patients with DM (Type I and Type II) will develop nephropathy after about 25 to 30 years v. Approximately 45% of dialysis patients have diabetic nephropathy as cause of ESRD v. However many type II patients die from CV disease before they reach ESRD v. May not be able to tell patient has kidney disease based on GFR v. Need to have a micro albumin urine test to determine level of proteinuria v. Need to be on ACE/ARB for renal protection
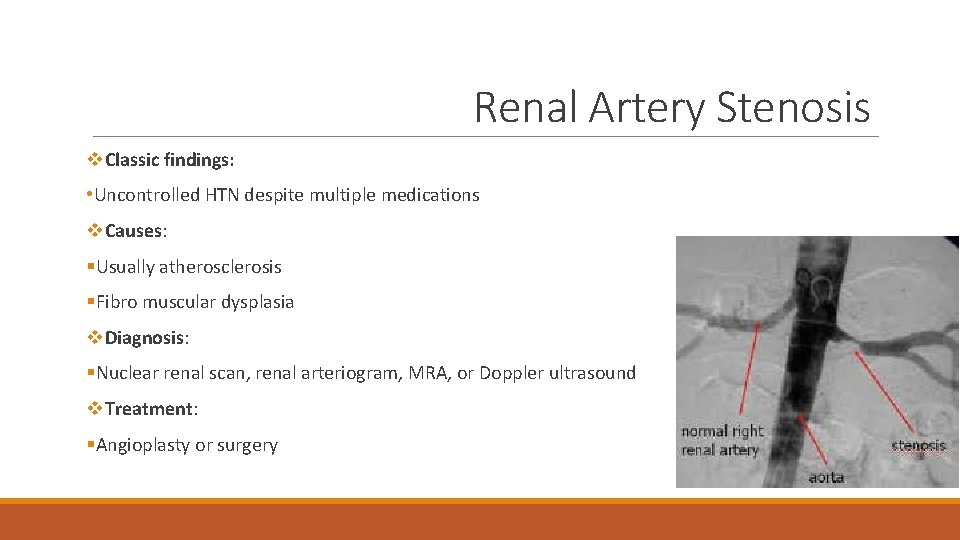
Renal Artery Stenosis v. Classic findings: • Uncontrolled HTN despite multiple medications v. Causes: §Usually atherosclerosis §Fibro muscular dysplasia v. Diagnosis: §Nuclear renal scan, renal arteriogram, MRA, or Doppler ultrasound v. Treatment: §Angioplasty or surgery

Obstructive Uropathy v. Obstruction can occur anywhere along urinary tract causing hydonephrosis ØRenal calculi ØBPH ØColon, cervical, or uterine cancer ØNeurogenic bladder v. Can be unilateral or bilateral v. Treatment ØResolve obstruction- may need stents ØTreat BPH ØFoley catheter or nephrostomy tubes

Autosomal Dominant Polycystic Kidney Disease v. Most common inherited kidney disease v. Affects 1 in 1000 people v. Systemic disease causing kidney, liver, pancreas, thyroid, and subarachnoid cysts and intracranial aneurysm v. Clinical hallmark sign is gradual and massive cystic enlargement of kidneys resulting in kidney failure v. May be present in childhood with symptoms usually beginning in middle age v. Symptoms can include abdominal pain, hematuria, nocturia, flank pain, and fatigue v. Diagnosis usually made by ultrasound v. Presence of enlarged kidneys with multiple cysts required for diagnosis
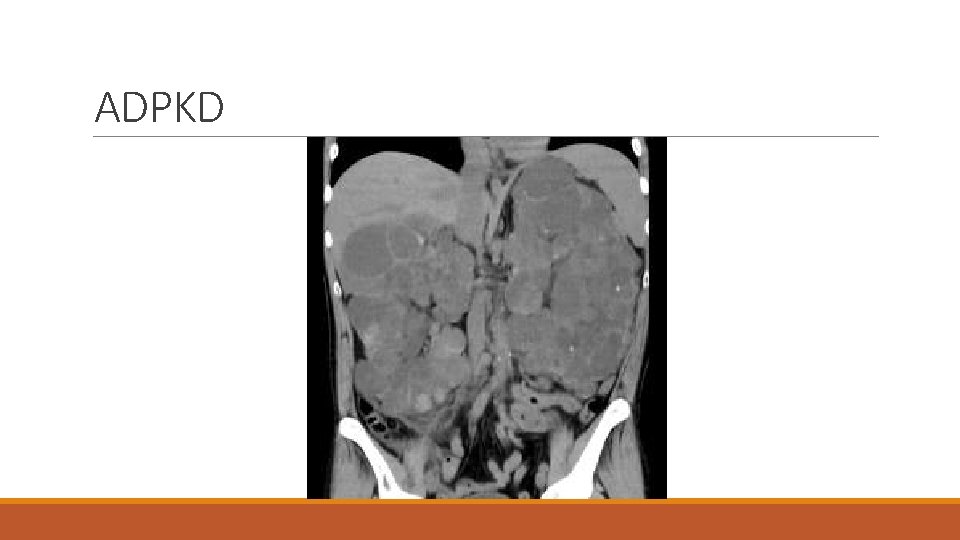
ADPKD
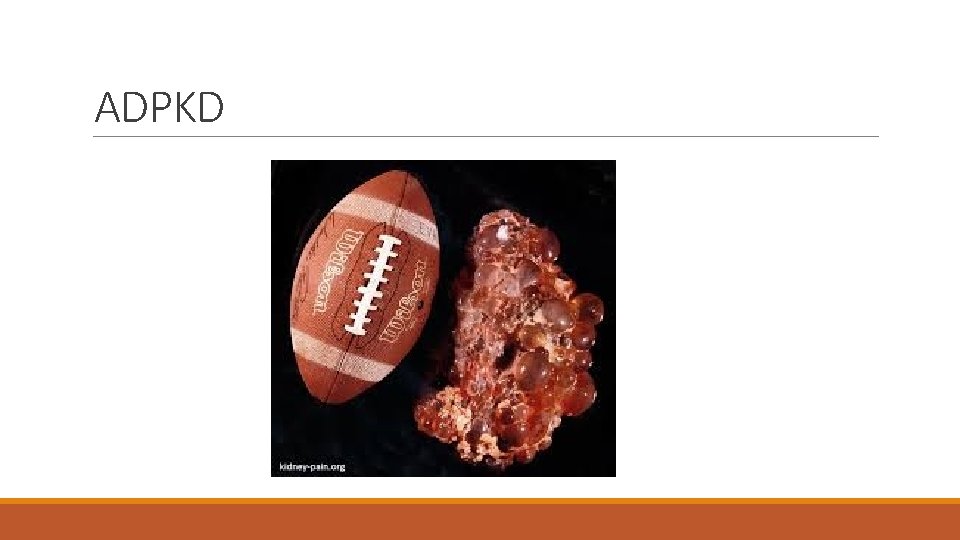
ADPKD

Hepatorenal Type II §Usually rapid decline in kidney function §Moderate steady decline in GFR §s. Cr may double in 2 weeks §Cirrhosis causes decrease in NA and water excretion, decreased renal perfusion and GFR §Occurs with acute hepatitis, bacterial infections, major surgery, or massive GI bleed §Decreased ability to excrete NA leads to ascites §Presence of ascites represents marked impairment or renal sodium handling
Cardio-Renal 1. Abrupt worsening of cardiac function leads to AKI 2. Chronic abnormalities in cardiac function causes progression of CKD 3. Abrupt worsening of renal function causes acute cardiac dysfunction (heart failure, arrhythmia, or ischemia) 4. CKD contributes to decreased cardiac function resulting in hypertrophy and increased risk of CVD 5. A systemic condition results in both cardiac and renal dysfuction

Aging and Renal Function v. Natural decline in GFR is 8 ml/min for every decade after 40 despite normal creatinine v. Renal blood flow declines by 10% per decade v. Renal mass decreased from 400 g to 300 g by age 90 v. All the above accelerated by: HTN, DM, lead exposure, smoking, atherosclerotic vascular disease, and male gender

Acute Kidney Injury v. Incidence increasing with the number of hospitalizations with AKI diagnosis rose from 3, 942 in 1996 to 23, 052 in 2008 v 5% to 30% of hospital ICU admissions v 25% of people develop while in the hospital v 50% of cases are iatrogenic v. Pre-renal- response to hypoperfusion->volume depetion, sepsis, heart failure, cirrhosis v. Intra-renal- conditions that affect parenchyma->acute tubular necrosis, acute interstitial nephritis, nephrotoxic medications v. Post-renal-obstruction of urinary outflow->BPH, renal calculi (Domino, 2013)

Nephrotic Syndrome v. Clinical syndrome characterized by massive proteinuria (>3 g/24 hrs) v. Associated with many types of kidney diseases such as minimal change disease, membranous glomerulopathy, diabetes, and amyloidosis v. Hypoalbuminemia v. Edema v. Hyperlipidemia v. Lipiduria v. May have fatigue, weight gain, anorexia, foamy urine v. Treatment involves addressing underlying cause and complications v. May need a kidney biopsy v. May require long-term immunosuppressant therapy (Domino, 2013)

End-Stage Renal Disease (ESRD) v. Cardiovascular disorders are leading cause of death for ESRD patients v. More than 50% of dialysis patients die from cardiovascular complications v. Risk of CV death is 50% higher in this population if patient also has DM v. Screen patients annually for CV disease with electrocardiogram, stress test v. Refer to cardiologist

Signs and Symptoms of ESRD v. Head-headaches, fatigue, and difficulty thinking v. Mouth- food may taste bad or like metal, foul smelling breath (like urine) v. Lungs-dyspnea caused by fluid or anemia v. Stomach- loss of appetite, nausea and vomiting v. Bladder- less or no urine. Some people still make urine but it is just fluid no waste products are removed v. Hands and feet- swelling v. Skin-build up of uremic wastes causes itching v. Blood vessels- high blood pressure failing kidneys can no longer keep pressure under control (Greenburg, 2009)
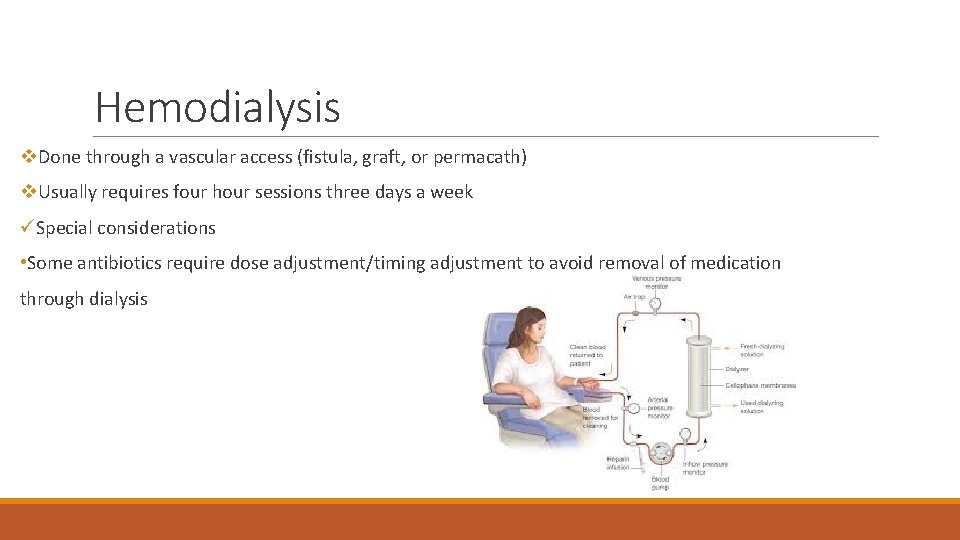
Hemodialysis v. Done through a vascular access (fistula, graft, or permacath) v. Usually requires four hour sessions three days a week üSpecial considerations • Some antibiotics require dose adjustment/timing adjustment to avoid removal of medication through dialysis

Peritoneal Dialysis v. Advantages v. Disadvantages §Convenient done at home §High Risk for peritonitis §Daily treatments more closely match natural renal functions §Requires compliance with aseptic technique §Patients have less fluid/dietary restrictions §Patients with history of multiple abdominal surgeries or hernia may not be candidates

Renal Transplant v. Evaluation process can start when GFR is <20 v. Many options are available such living relative, non-related living, and cadaver v. Requires extensive workup to be placed on list v. Compliance v. Requires immunosuppressant therapy v. Caution when prescribing/adjusting transplant patient’s medication

Burden of ESRD v. Economic costs v. Total Medicare costs for ESRD care in 2005 were $19. 3 billion v. Decreased quality of life v. Increased morbidity and mortality v. Complications associated with dialysis

Referral v. Electrolyte abnormalities v. Persistent proteinuria v. Uncontrolled HTN v. Elevated serum CR/decreased GFR –guidelines CR 1. 5 female, 2. 0 male v. Patient with known CKD that are likely to progress v. Don’t wait to refer to nephrologist when the patient needs dialysis v. Patients need to have dialysis access, education, and preparation

Collaboration v. CKD requires collaboration and coordination among many health care providers v. CKD stages I-III usually managed by PCP v. Nephrologist usually consulted when CKD III or other kidney disorder v. Dietician v. Cardiologist v. Vascular Surgeons v. Endocrinologist v. Social workers

Educational Resources v. National Kidney Foundation www. kidney. org v. American Nephrology Nurse’s Association http: //ww. annanurse. org v. Internet School of Nephrology http: //www. Ukidney. com v. International Society of Nephrology http: //www. theisn. org v. American Society of Nephrology http: //www. asn-online. org/

Questions § The number one cause of death in patients with ESRD: A. Complications from DM B. Septicemia D. Cardiovascular Disease E. Cancer § The functions of the kidney are: A. Production and secretion of enzymes and hormones B. Excretion of metabolic end products and foreign substances C. Maintenance of body fluid composition D. Both A & B E. All of the above § The best antibiotic choice for a 69 y/o female with a urinary tract infection A. Cipro 250 mg BID B. Bactrim DS 1 tablet BID C. Do not provide antibiotics wait for urine culture

References Claudio, R. , Haapio, M. , House, A. , Anavekar, N. , & Bellomi, R. (2008, November). Cardiorenal syndrome. Journal of American College of Cardiology, 52(19), 1527 -1539. Collins, T. (2012). Twelve things hospitalists need to know about nephrology. The Hospitalist. Retrieved February 7, 2014 from http: //the-hospitalist. org/details/article/3782901/12 Things Hospitalists Need to Know About Nephrology. html Deja Review Internal Medicine (2011). Mobasser, S. , Mc. Graw Hill Medical, New York Dunphy, L. , Winland Brown, J. , Porter, B. , & Thomas, D. (2011). Primary Care: The art and science of advanced practice nursing. 3 rd Edition. Philadelphia: F. A. Davis. ISBN 978 -0 -8036 -2255 -5. Domino, F. (2013). Griffith’s 5 Minute Clinical Consult. 19 th Ed. Lippincott Williams & Wilkins. Fibromuscular Dysplasia (n. d. ). Retrieved February 7, 2014 from http: //www. mayoclinic. com/ health/fibromuscular-dysplasia/DSO 1101. Greenburg, A. , Cheung, A. K. , Coffman, T. M. , Falk, R. J. , Jennette, J. C. (2009). Primer on kidney diseases. (5 th ed. ), Philadelphia, Saunders Elsevier National Kidney Foundation (2010). Nephrology essentials: chronic kidney disease. Retrieved February 8, 2014 from http: //www. kidney. org/professionals/CAP/neph. Essentials. cfm

References National Kidney Foundation (2012). Clinical Practice Guidelines for Chronic Kidney Disease Evaluation, Classification, and Stratification. National Kidney and Urologic Diseases Information Clearinghouse (2012). Retrieved February 10, 2014 from http: //www. nih. gov/kudiseases/pubs/kustats/#top Niels-Peter, B. , Farhat, A. , Syed, R. , Biyabani, Q. , Masood, A. , Imtiaz, R. (2012) Ultrasonographic renal size in individuals without known renal disease. Journal of Pakistan Medical Association.
- Slides: 68